
Amaryl
| Contato
Página Inicial
Joseph J. Quinlan, MD
- Professor
- Department of Anesthesiology
- University of Pittsburgh
- Chief Anesthesiologist
- University of Pittsburgh Medical Center?resbyterian
- Pittsburgh, Pennsylvania
These findings have led others to rely on automated syringe-infusion systems to improve precision and reliability with syringe-coupled cannulas diabetes diet type 1 recipes purchase amaryl 1 mg. With multiple or prolonged injections diabetes type 1 causes and symptoms 2 mg amaryl fast delivery, cells in suspension begin to settle under the influence of gravity blood sugar yeast infection cheap 2 mg amaryl with visa, creating a gradient of cellular density diabetes mellitus uptodate generic amaryl 4 mg visa. Depending on the viscosity of the carrier media diabetes insipidus guidelines endocrine society 1 mg amaryl purchase free shipping, up to threefold difference in cell concentration between the first and last fractions administered have been reported. In addition to eliminating potential dead space, this integrated plungercatheter design allows small, precise delivery of the cellular suspension (1. With each catheter deployment, the surgeon delivers the entire cell dose which has been preloaded in the catheter, thus avoiding dose variability due to sedimentation in the delivery device. Together, these design elements allow for the delivery of cells to a wide range of 3D "patterns" in anatomically complex target regions via a single transcortical penetration. In this iteration, polyether ether ketone, nylon, and nickel titanium are used to construct the outer guide tube, inner guide tube, and plunger, respectively. Using an established neurosurgical work flow,28,31,32 multiple deposits of human embryonic stem cell-derived dopaminergic neuronal precursor cells were safely implanted into the striatum of live swine without hemorrhage or adverse events. Studies have established that multiple small stem cell engraftments are superior in incorporating the cells into host neuronal circuitry. However, the optimal cell dosage and distance between engraftments have yet to be determined and may differ based on target region and disease process. Cell delivery strategies and device selection should similarly be tailored to the neuroanatomic region of interest. For small, well-defined brain regions, a straight cannula may be sufficient for cell delivery; meanwhile, larger or more complex brain regions may require newer radial delivery strategies. Further innovations, such as the simultaneous use of multiple delivery catheters very small in diameter (<50 m), may overcome some of the remaining limitations. Initial targeting also remains dependent on placement of a rigid linear guide cannula. When eloquent neural structures and/or regional vascular anatomy prohibit a linear trajectory, suboptimal catheter placement may be unavoidable. In such scenarios, the development of "steerable" or more flexible guide cannulas may be beneficial. With increasing complexity of delivery strategies and devices, parallel efforts are also needed to develop computer algorithms to optimally seed complex 3D structures with small cell engraftments. Finally, delivery strategies will also need to account for the migratory properties of the injected cells. Adjuvant strategies to biologically harness such cellular properties remain important areas of future research. As our understanding of the biology underlying cell-based therapeutics continues to advance in the decades to come, continued research into the devices and surgical aspects of this therapeutic strategy will help ensure that delivery platforms no longer present a critical bottleneck to clinical translation. Devices for cell transplantation into the central nervous system: design considerations and emerging technologies. Neurosurgical techniques for disruption of the blood-brain barrier for glioblastoma treatment. Local and reversible blood-brain barrier disruption by noninvasive focused ultrasound at frequencies suitable for trans-skull sonications. Intracerebroventricular delivery as a safe, long-term route of drug administration. Therapeutic effects of human umbilical cord blood-derived mesenchymal stem cells after intrathecal administration by lumbar puncture in a rat model of cerebral ischemia. Implantation site and lesion topology determine efficacy of a human neural stem cell line in a rat model of chronic stroke. Preclinical evaluation of a novel intracerebral microinjection instrument permitting electrophysiologically guided delivery of therapeutics. Improved graft survival and striatal reinnervation by microtransplantation of fetal nigral cell suspensions in the rat Parkinson model. Comparison of different needle diameters and flow rates on bone marrow mononuclear stem cell viability: an ex vivo experimental study. Improving viability of stem cells during syringe needle flow through the design of hydrogel cell carriers. Cellular transplantation for the nervous system: impact of time after preparation on cell viability and survival. Injection parameters affect cell viability and implant volumes in automated cell delivery for the brain. Intracerebral cell implantation: preparation and characterization of cell suspensions. Magnetic resonance imaging-guided delivery of neural stem cells into the basal ganglia of nonhuman primates reveals a pulsatile mode of cell dispersion. Radially branched deployment for more efficient cell transplantation at the scale of the human brain. Comparison of deep brain stimulation lead targeting accuracy and procedure duration between 1. Comparison of accuracy and precision between frame-based and frameless stereotactic navigation for deep brain stimulation electrode implantation. Analysis of stereotactic accuracy in patients undergoing deep brain stimulation using nexframe and the leksell frame. Hemorrhage detection and incidence during magnetic resonanceguided deep brain stimulator implantations. An optimized system for interventional magnetic resonance imaging-guided stereotactic surgery: preliminary evaluation of targeting accuracy. Manual vs automated delivery of cells for transplantation: accuracy, reproducibility, and impact on viability. Ischemic central necrosis in pockets of transplanted myoblasts in nonhuman primates: implications for cell-transplantation strategies. Intramyocardial microdepot injection increases the efficacy of skeletal myoblast transplantation. A microtransplantation approach for cell suspension grafting in the rat Parkinson model: a detailed account of the methodology. Efficacy of and morbidity associated with stereoelectroencephalography using computerized tomography-or magnetic resonance imaging-guided electrode implantation. A systematic review and meta-analysis of stereo-electroencephalography-related complications. Risk factors for hemorrhage during microelectrode-guided deep brain stimulator implantation for movement disorders. Feasibility of three-dimensional placement of human therapeutic stem cells using the intracerebral microinjection instrument. Interventional magnetic resonance imaging-guided cell transplantation into the brain with radially branched deployment. Safety and function of a new clinical intracerebral microinjection instrument for stem cells and therapeutics examined in the Gottingen minipig. Such approaches include gene augmentation to replace the mutant gene, or gene knockdown to inhibit expression of a dominantly acting disease gene. Therapeutic modalities also include going after the mutant protein, either by replacing it. Recently, gene editing has been added to the toolbox of methodologies to reduce the disease gene burden. This modality offers the flexibility to edit, replace, and modify specific loci in the genome with simplicity and ease in the laboratory, which makes it a useful tool to knockout and knock-in genes, to activate or silence gene expression, and to create model systems. Indels can create frameshift mutations and downstream premature stop codons, leading to inactivation of the target gene. For this, a mutated, dead Cas9 (dCas9) that lacks enzymatic endonuclease activity is used. This enhanced gene regulation is achieved with effector protein domains fused to dCas9 to recruit epigenetic modifying factors. These latter approaches, if delivered via nonviral means, require repeated treatments, and both can be prone to high off-target effects and cytotoxicity. On-target specificity was improved by engineering an enhanced Cas9 and a high-fidelity Cas9; both were associated with reduced offtargeting. In this scenario, Cas9 is expressed by two expression systems that can be induced to dimerize, and has editing activity similar to that of wild-type SpCas9. Alzheimer disease is a major cause of morbidity and mortality in elderly individuals. Although this may reduce immune responses to the bacterial nuclease, further testing is required to determine the extent to which this also may alleviate unintended editing. Furthermore, the mice showed a delay in disease onset, more surviving neurons at end stage, and increased survival. However, repeated dosing or sustained expression from vector systems will be required, raising the specter of off-targeting or immune responses to the foreign Cas proteins. The technology opens a new door in biomedical research for drug discovery, uncovering disease mechanisms, and personalized medicine and therapeutics. Two alternative pathways of double-strand break repair that are kinetically separable and independently modulated. Obligate ligation-gated recombination (ObLiGaRe): custom-designed nuclease-mediated targeted integration through nonhomologous end joining. A protein-tagging system for signal amplification in gene expression and fluorescence imaging. Efficient genome editing in the mouse brain by local delivery of engineered Cas9 ribonucleoprotein complexes. Treatment of autosomal dominant hearing loss by in vivo delivery of genome editing agents. In vivo evaluation of candidate allele-specific mutant huntingtin gene silencing antisense oligonucleotides. A split-Cas9 architecture for inducible genome editing and transcription modulation. Progress in the genetics of polygenic brain disorders: significant new challenges for neurobiology. In vivo genome editing improves muscle function in a mouse model of Duchenne muscular dystrophy. It comprises a microvascular endothelium, extracellular matrix, and neuroglial structures. Lacking fenestrations, these cells restrict paracellular transport of large hydrophilic compounds. This leads to tightly regulated and limited transcellular transport of substances needed for brain functioning. This barrier also contains peptidases that inactivate proteins, as well as intracellular enzymes that inactivate neuroactive and neurotoxic substances. Interestingly, in comparison to their systemic counterpart, cerebral endothelial cells also possess a greater concentration of mitochondria to provide the energy needed for the maintenance of the barrier integrity as well as active transport. Molecules with low solubility require facilitated transport, relying on mechanisms such as ion channels, specific transporters, energydependent pumps, or receptor-mediated endocytosis for transportation. For example, the chemotherapy agent carboplatin is efficacious systemically against lung cancer and in vitro for glioblastoma, but is ineffective in humans with glioblastoma. For example, aged mice that underwent traumatic brain injury have been shown to have significantly slower repair of the barrier compared with younger mice. However, this alteration in permeability is highly variable and dependent on tumor type and size. Additionally, the core of a malignant brain tumor is often leaky, whereas the brain adjacent to the tumor has variable barrier integrity. The sink effect refers to the distribution of drug concentration-highest in the center of the lesion, with progressively decreasing concentration toward the periphery of the lesion. These alterations have significant implications for understanding disease pathology and progression as well as for optimizing drug-delivery strategies. This technique uses a sublethal pulsed electric field to disrupt the endothelial membrane, allowing uptake of chemotherapeutic agents. Irreversible electroporation is achieved via the use of a series of electric pulses delivered through needle electrodes; these pulses induce a nonthermal focal ablation to the target. The mechanisms of action of this therapy are twofold: it exerts an antimicrotubule effect, and it creates a nonthermal ablative property of the electric field, which occurs as the pulse frequency increases, causing dielectric losses and developing friction between rapidly oscillating molecules. In vivo studies of two different glioma cell lines showed additional increased cytotoxicity by >50% for 1 ng/mL concentrations of either bleomycin or carboplatin at electric fields! Their usual diameter (110 m) allows them to pass through the capillary networks of the tissue exposed to the ultrasound, and the ultrasound wave causes microbubbles to expand and contract in the capillaries. The bubble oscillations also prompt the surrounding fluid to flow (a process known as microstreaming), thereby creating large shear forces around the bubbles as well. Above a certain threshold, the bubble oscillations become so large that the inertia of the surrounding fluid causes the bubbles to collapse. Since 2006, when ophthalmic artery chemosurgery for retinoblastoma was introduced, enucleation rates have decreased from over 95% to <10% at Memorial Sloan Kettering Cancer Center in New York City. Intrathecal/intraventricular Drug Delivery Like other approaches, the intrathecal/intraventricular route is an alternative way to bypass the physical barriers of the brain. The drug therefore achieves a higher concentration in the brain compared to the extravascular concentration. The major disadvantage of the intrathecal/intraventricular approach is the risk of causing a subependymal astrogliatic reaction due to the high drug exposure at the ependymal surface of brain. The drug concentration in the brain relies on the diffusion phenomenon, which determines how much of the drug penetrates the brain from the administration site. Diffusion decreases logarithmically with each millimeter of brain tissue; that is, from the injection site to the ependymal surface of the brain.
Hydrocephalus needs to be treated urgently if the infant is symptomatic (poor feeding diabetic neuropathy treatment order amaryl with amex, vomiting diabetes hypoglycemia definition order generic amaryl, lethargy) or is manifesting symptoms of the Chiari malformation in the face of untreated hydrocephalus (stridor diabete o que pode comer purchase amaryl in india, frequent apnea spells) diabetes type 2 symptoms purchase line amaryl. A pregnant woman is undergoing an amniocentesis during a scheduled prenatal visit diabetes definition and types best amaryl 4 mg. With this modality, myelomeningocele may be detected during scanning of the fetal head for subtle changes in the cranial and cerebellar configurations. Infants may display lethargy, lack of interest in their surroundings, and poor feeding. In older children and adolescents, other common findings include headache, visual disturbance, abnormal gait, poor coordination, and papilledema. Prenatal maternal factors such as intrauterine exposure to alcohol, isotretinoin, valproic acid, and carbamazepine; hyperthermia; diabetes; obesity; and folate deficiency may increase the risk of giving birth to a child with myelomeningocele. The patient began suffering seizures as a child, and, despite being compliant on two anticonvulsant agents, he continues to suffer tonic-clonic episodes almost daily. The medications have interfered with his ability to study, and he would like to gain more independence and autonomy. Epilepsy can be a significantly disabling disease, especially in severe forms such as those categorized as "drug-resistant," a term used in patients on two well-tolerated, appropriately chosen antiepileptic drugs who fail to achieve a sustained seizure freedom. Surgically treated epilepsies include mesial temporal lobe epilepsy (most common type of surgery-treated epilepsy) and neocortical epilepsy, which are both treated with temporal lobectomy. Sturge-Weber syndrome and large congenital hemispheric strokes can be treated by hemispherectomy. Hemispherectomy is usually performed in children with severe epilepsy who are constantly disabled by the disease. While it can eliminate the seizures, many are left with hemiparesis and speech difficulties. Corpus callosotomy can be a palliative treatment for atonic seizures in patients with Lenox-Gastaut syndrome where the anterior two-thirds of the corpus callosum is resected. Drop attacks carry a risk of injury, and corpus callosotomy has been shown to reduce falls by 70%. The main targets of preoperative testing in patients with planned resection epilepsy surgery are (1) precise localization of the epileptic focus and (2) documentation of baseline cognitive function. Identification of the dominant hemisphere and speech and language dominance for temporal and some frontal lobe resections is essential to delineate the eloquent cortices to avoid causing postoperative deficits. In this test, amobarbital or other anesthetic agents can be selectively injected into the carotid artery supplying one side of the brain to temporarily disrupt the function of this side while the patient is awake in order detect hemisphere dominance and speech and language zones and thus predict the possibility of postoperative memory deterioration. Once the patient is back to baseline mental status, the same procedure is repeated on the contralateral side. Electrocortocography electrodes placed directly on the brain surface to record cortical activity. The cortical surface between the electrodes is accessible for surgical manipulation in this type of electrodes. But the recorded signal quality can be potentially degraded by travel from the cortex through the dura and bony structures to reach the scalp electrodes. There are two types of electrodes used: one type consists of arrays of evenly spaced electrodes imbedded in strips of silicone plastic; the space between these electrodes is not accessible for surgical manipulation due to the presence of the 148 · Strip electrodes allow recording and surgical access or manipulation. It is important to remind the patient that he will be awakened during a certain point during the procedure to test the integrity of his neurological and cognitive function. Giving the patient an insight about the intraoperative situation will help build rapport and mutual trust between the patient and the anesthesia team. A comprehensive preoperative medical evaluation of the patient is essential, with emphasis placed on associated comorbidities in a patient with underlying medical conditions associated with epilepsy. Tuberous sclerosis can be associated with cardiac arrhythmia as well as renal dysfunction, and Von Recklinghausen disease can be associated with atlantoaxial instability, increased sensitivity to neuromuscular blocking agents, and pulmonary hypertension. Chronic use of those anticonvulsants known to be enzymes inducers can alter the metabolism of opioids and cause unpredicted kinetics for muscle relaxants. If the patient will have an entirely awake procedure, the Foley catheter can sometimes be avoided to avoid unnecessary discomfort while providing conservative use of fluids. Antiepileptic agents can be taken the morning of the surgery after discussion with the neurosurgeon and neurologist. Motivated, mature, cooperative patients can be ideal candidates for awake craniotomy, but patients who suffer from psychiatric disease, developmental delay, or are merely uncooperative are unlikely to tolerate it successfully. In some centers, the subdural grids are placed up to a week before planned resection, and the patient is monitored for seizure activity and localization of the epileptogenic zone. This requires a full craniotomy and is an opportunity to evaluate the patient and appreciate his response to anesthetics and surgical stimulus. The anesthetic regimen must be tailored to allow for rapid emergence and neurological evaluation. Initially, methohexital was the drug used for pharmacological activation, but etomidate at a dose of 0. Most techniques allow the patient to be sleeping or heavily sedated during the maximum stimulatory stages of the procedure that include performing a "scalp block," applying the pins for head immobilization, incision, and removal of the bone flap. The patient is then allowed to awaken as brain mapping and demarcation of the epileptogenic zone is achieved. Once fully conscious, speech and memory testing is performed while areas are stimulated to determine if a seizure occurs or if speech is affected. The surgeon may proceed with resection with the patient awake or determine that it is safe to resume unconsciousness. The preferred agents for this technique include remifentanil, propofol, and often dexmedetomidine, which may be utilized throughout the testing in young patients. It is essential to be prepared for more common problems such as respiratory depression, nausea, and vomiting. The newer agents and the addition of propofol help to decrease the incidence of nausea. A supraglottic airway should be readily available for airway rescue and control if needed and has proved successful when needed in this scenario. Additionally, the surgeon can irrigate the brain with cold water, which may also stop the seizure. Nausea should be treated aggressively and the patient carefully monitored for intracranial bleeding. The team approach and communication among specialties can often provide the best outcome for patients. Epilepsy can occur at any stage in life, and modalities must be utilized that produce the most benefit and cause the least harm. Three-dimensional angiography is not necessary for delineation of structures for epilepsy surgery. Complications of vagal nerve stimulators can include: a) Tinnitus b) Tachycardia c) Intractable vomiting d) Voice changes Correct Answer: d. Patients frequently experience hoarseness and coughing from stimulation of the recurrent laryngeal nerve and sensation of a constricted throat. While Moyamoya disease can present with a seizure, it is primarily a vascular abnormality; however, a large number of patients experience seizures with SturgeWeber syndrome, tuberous sclerosis, and Lennox-Gastaut syndrome. The function of the "Wada test" is: a) To rule out a vascular lesion causing seizures b) To determine the hemispheric dominance c) A measure of cognitive function d) To localize the epileptogenic focus Correct Answer: b. The "Wada test" establishes cerebral language and memory representation of each hemisphere to determine which side of the brain is responsible for vital cognitive functions. A decompressive craniectomy is performed to allow the brain to expand, whereas the others are specific procedures to treat epilepsy. Methohexital (along with etomidate and ketamine) is known to activate seizure activity when administered to patients with epilepsy. The opioids have minimal effect, and volatile agents are generally depressive with the exception of sevoflurane at high doses. While there are variations in the technique for awake craniotomy, having adequate and long-acting local anesthetic and a satisfactory regimen for sedation is necessary for success. In addition, patient selection, good positioning, and good surgical technique are essential. A patient is starting to become anxious and agitated after prolonged testing during an awake procedure and begins shaking violently. This difficult situation can often be mitigated with a small dose of sedative and also stopping the procedure for a moment to calm the patient. It is important to observe the patient carefully for signs of oversedation and note recovery of consciousness. Psychiatric and medical comorbidity and quality of life outcomes in childhood-onset epilepsy. Determinants of health-related quality of life in pharmacoresistant epilepsy: results from a large multicenter study of consecutively enrolled patients using validated quantitative assessments. Long-term seizure outcomes following epilepsy surgery: a systematic review and meta analysis. Is vagus nerve stimulation a treatment option for patients with drug-resistant idiopathic generalized epilepsy The anesthetic considerations of intraoperative electrocorticography during epilepsy surgery. Etomidate accurately localizes the epileptic area in patients with temporal lobe epilepsy. A retrospective analysis of a remifentanil/propofol general anesthetic for craniotomy before awake functional brain mapping. On physical examination, he has a resting tremor, muscular rigidity, and bradykinesia. The main objective is to modulate the function of such structures in order to achieve a reversible, adjustable, and therapeutic or clinically beneficial effect. Levodopa is a precursor to dopamine that can cross the bloodbrain barrier (unlike peripherally administered dopamine). Carbidopa inhibits dopa decarboxylase, preventing conversion of levodopa into dopamine and therefore allows more levodopa to cross into the brain to then be converted to dopamine. Additionally, this also reduces the peripheral side effects of dopamine such as nausea, vomiting, and postural hypotension. The surgery can be performed in a single stage, with implantation of the brain leads and the pulse generator in the chest in the same day. The last part is usually performed a few days or weeks after brain electrode placement in an attempt to minimize the risk associated with two back-toback procedures in patients who are commonly elderly and have multiple comorbidities. Most commonly, the patient is positioned supine or in semi-sitting position with the stereotactic frame attached to the bed. Another test performed during the procedure is to verify that the lead is inserted in an adequate location using macrostimulation testing. It has been reported that propofol affects the background neuronal discharges and patterns during recording. Propofol may have an impact on macrostimulation testing considering that it can provoke dyskinesia. This 2-agonist has the advantage of being easily titratable, it possesses an analgesic effect, and it produces minimal respiratory depression. Comorbidities such as chronic pain and respiratory and cardiovascular disorders 3. In this approach, the patient is under moderate/deep sedation during the initial portion of the surgery such as positioning, local infiltration of the skin, burr hole, opening of the meninges, and cannula insertion. At this point, patient should be awakened to cooperate with neurological assessment. The benefit of sedating the patient with shortacting agents such as propofol and/or dexmedetomidine is that they are easily titratable and have a predictable pharmacokinetic profile facilitating the process of intraoperative emergence. It has been speculated that the intraoperative use of -blockers could interfere with the macrostimulation testing but there is not enough data to support it. The calculated coordinates to the specific target are then transferred to the stereotactic frame and arc. In this step, the pulse generator is implanted, typically in the chest, and connected to the brain leads by tunneling extension cables through the scalp and subcutaneously on the side of the neck. The main hardware complications include migration of the leads, erosion of the subcutaneous portions · 19. Stimulation-related adverse effects are reversible with programing and/or drug adjustments. Animal stereotactic surgery was first described by Horsley and Clarke in 1908,23 when they reported the method for accurate insertion of a needle or electrode into the brain of a monkey. Human stereotactic surgery was started more than 30 years later with SpiegelWycis. The main hypothesis is that the electrical stimulation of the targeted area modulates the basal ganglia and thalamocortical network and improves the symptoms of the disease. For other parts of the procedure, the patient may be deeply sedated or under general anesthesia. The most commonly used anesthetic drugs in our institution are propofol and dexmedetomidine. Ideally, patients undergoing surgery should have their implantable neurological devices checked preoperatively. In emergent surgical procedures, all the surgical staff should be aware of the device and the potential impact of the electromagnetic interference such as: 1. Dexmedetomidine has the advantage of being easily titratable, possesses analgesic effect, and produces minimal respiratory depression. The overall benefits of this procedure are better quality of life and improvement of motor symptoms such as tremor, rigidity, dyskinesia, and offon fluctuations.
Buy amaryl discount. La médication dans le traitement du diabète de type 2.
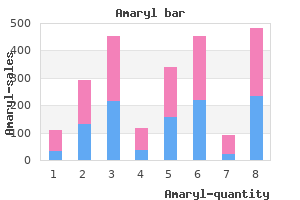
Epispadias is rare (1 in 120 diabetic diet foods buy 4 mg amaryl visa,000 male births) and is characterized by a urethral orifice on the dorsal aspect of the penis diabetes test online australia purchase amaryl 1 mg. It is thought to occur from a defective migration of the genital tubercle primordia to the cloacal membrane early in development (fifth week) diabetes mellitus type 2 wikipedia free encyclopedia order amaryl 4 mg free shipping. Glanular hypospadias Penile hypospadias Penoscrotal hypospadias (with chordee) Scrotal hypospadias (bifid scrotum diabetes pills vs insulin buy amaryl with american express, chordee) Complete epispadias Penile epispadias Chapter 5 Pelvis and Perineum 281 5 Clinical Focus 5-26 Uterine Anomalies Incomplete fusion of the distal paramesonephric (müllerian) ducts can lead to septation of the uterus or partial or complete duplication of the uterus (bicornuate uterus) diabetes symptoms type 1 adults amaryl 1 mg buy cheap. If only one paramesonephric duct persists and develops, a unicornuate uterus results. These conditions seem to be transmitted by a polygenic or multifactorial pattern and carry a higher risk for recurrent spontaneous abortions (15-25%), premature labor, uterine pain, breech or transverse deliveries, and dysmenorrhea. Complete septum (with double uterus and double vagina) Partial septum Rudimentary second vagina (without external opening, forming cyst) Bicornuate uterus with complete septum (double cervix) Double uterus Bicornuate uterus Septate uterus Partial septum Unicornuate uterus 282 Chapter 5 Pelvis and Perineum Clinical Focus 5-27 Male Circumcision (Newborn) Male circumcision is the removal of the foreskin of the penis. Generally, this is not a medically indicated procedure but is done at the request of the parents or because of a religious preference. All circumcision techniques begin with the undiapered newborn restrained on an infant (papoose) board. Placement of the bell through the baseplate may be facilitated by reaching through the opening with a hemostat. The stem of the bell is placed into the top of the clamp and the thumb screw gently tightened. Clinical Focus Available Online 5-28 Ovarian Tumors Additional figures available online (see inside front cover for details). Risk factors include a family history of ovarian cancer, high-fat diet, age, nulliparity, early menarche, late menopause, white race, and higher socioeconomic status. Papillary serous cystadenocarcinoma Uterus Clear cell carcinoma of ovary Pelvic mass (up to 30 cm) partially cystic 40% bilateral predominately Papillary projections Challenge Yourself Questions 1. Cancer of the uterine cervix reaches an advanced stage and disseminates anteriorly. Which of the following structures is most likely to be involved in the spread of the tumor Ultrasound examination reveals that she has a bicornuate uterus with a complete septum and double cervix. A 41-year-old woman presents in the clinic with a uterine prolapse (cervix at introitus) in which the cervix is visible at the vaginal opening. Which of the following structures is the most important support structure of the uterus Which of the following lymph nodes will be the first to harbor disseminated ovarian cancer cells A 69-year-old man with a history of atherosclerotic disease and heavy smoking tells his physician that he is "impotent. A 73-year-old woman is admitted to the hospital with significant abdominal ascites. When she sits upright on the side of her bed, the intraperitoneal fluid accumulates in her pelvis. Which of the following sites represents the lowest extent of the female abdominopelvic cavity where this fluid will collect Vesicouterine pouch Multiple-choice and short-answer review questions available online; see inside front cover for details. A male driver has sustained severe trauma to the pelvic region in a motor vehicle crash, resulting in a tearing of the prostatomembranous urethral junction (a tear just superior to the external urethral sphincter). After an automobile crash the teenage male driver presents to the emergency department with pelvic fractures and paralysis of his urinary bladder. During surgery deep within the pelvis, the surgeon clamps the transverse cervical (cardinal) ligaments and the uterine arteries to provide hemostasis for a female patient. Which of the following structures lies close to these structures and must be preserved Sexual arousal and orgasm employ a coordinated regulatory effort mediated by somatic and autonomic nerves, as well as by endocrine and central nervous system input. During male ejaculation, which of the following nerves contract the internal urethral sphincter and prevent the semen from entering the urinary bladder The dissemination of cancer cells from the left testis would enter the testicular veins and then first enter which of the following veins A forensic pathologist is asked to characterize the bony pelvis of an unidentified and largely decomposed human body. For each of the descriptions below (14-20), select the muscle from the list (A-M) that is most closely associated. Contraction of this muscle expels the last few drops of urine from the male urethra. An abscess in the ischioanal fossa is limited in its spread superiorly by this muscle. Anterior rami of S2-S4 exit the anterior sacral foramina and then pass directly over (superficial to) this muscle. Trauma to the L1-L2 sympathetic outflow would result in the inability to contract this muscle. During pelvic surgery, the surgeon notices that the inferior gluteal artery and internal pudendal artery are leaving the pelvis just inferior to the piriformis muscle as they are headed for the gluteal region. Surgeons operating in the perineal region must be cognizant of this structure, because it is the anchor point for many of the perineal structures. During a pelvic examination, the gynecologist feels a pulse adjacent to the vaginal fornix. An ultrasound examination of a 16-year-old girl shows that she has a double uterus. Failure of which of the following developmental events is responsible for this condition A 20-year-old male college student with testicular pain and swelling is seen in the university health clinic. Which of the following conditions is most likely the cause of the swelling and inflammation Which of the following lymph node collections is most likely to be involved first in the spread of this tumor During a difficult delivery, the physician decides to perform a posterolateral episiotomy to enlarge the vaginal opening. Which of the following structures will be completely or partially incised during this procedure During surgery to remove an ovary and its associated lymphatics, the surgeon must be particularly mindful of the close anatomical approximation of which of the following nerves Rupture of the male urethra can lead to the extravasation of urine into various pelvic or perineal spaces. In the retroperitoneum of the lower pelvis For each of the questions below (31-37), select one vessel from the list (A-L) that best fits the structure described. This vessel usually passes between the lumbosacral trunk and the first sacral nerve. The urinary bladder is directly anterior to the uterine cervix, lying just deep to the vesicouterine pouch. Incomplete fusion of the distal paramesonephric (müllerian) ducts can lead to septation of the uterus, resulting in a partial or complete duplication of the uterus. External iliac vein Inferior gluteal artery Internal pudendal artery Middle rectal vein Ovarian artery Pampiniform plexus of veins (G) (H) (I) (J) (K) (L) Prostatic venous plexus Superior gluteal artery Testicular artery Umbilical artery Uterine artery Vaginal veins Chapter 5 Pelvis and Perineum 287 5 3. The ovaries descend into the pelvis from their original embryonic origin from the abdominal urogenital ridge. Thus, the lymphatic drainage courses back to the aortic (lumbar) nodes (the same is true for the male testes). The internal pudendal arteries give rise to the arteries of the bulb of the penis and the corpora cavernosa, which supply the erectile tissues. The space between the rectum and uterus, called the rectouterine pouch (of Douglas), is the lowest point in the female abdominopelvic cavity in the upright position. Fluids within the cavity will eventually percolate down and collect in this space. This rupture occurs before the prostatic urethra is completely surrounded by the external urethral sphincter, so blood and urine would collect primarily in the subperitoneal space beneath the pelvic floor. Excessive fluids in this space will allow it to expand superiorly and stretch the peritoneal floor of the pelvis. The pelvic splanchnic nerves arise from the S2-S4 spinal nerves and convey the preganglionic parasympathetic fibers that innervate the urinary bladder. Those fibers destined to innervate the bladder enter the inferior hypogastric plexus of nerves and then enter the vesical plexus on the bladder wall where they synapse on their postganglionic parasympathetic neurons. While most of the listed structures do not drain to the inguinal nodes, some lymph can track along the broad ligament of the uterus and enter the inguinal nodes. First, one must eliminate the possibility of perineal cancer, cancer of the distal anal canal, and cancer of the lower limb before focusing on the uterus. The ureters pass just inferior to the uterine vessels ("water flows under the bridge") and must be identified before anything in this region is clamped and/or incised. The sacral splanchnic nerves convey preganglionic sympathetic fibers to the inferior hypogastric plexus, where they synapse and send postganglionic fibers to innervate the internal urethral sphincter at the neck of the male urinary bladder (females do not have an internal urethral sphincter). Most of the adaptations that differentiate the female from the male pelvis pertain to its relationship to childbirth. As the testis descends through the inguinal canal, it becomes covered by three layers of spermatic fascia. The middle spermatic fascia is the cremasteric fascia or muscle and is derived from the internal abdominal oblique muscle. The cremaster muscle is innervated by the genital branch of the genitofemoral nerve. The only smooth muscle in the list that is innervated by them, resulting in contraction, is the detrusor muscle of the bladder wall. Contraction of this muscle empties the urinary bladder and is under parasympathetic control. The levator ani is one of two muscles comprising the pelvic diaphragm (the other one is the coccygeus), and is itself really the amalgam of three separate but closely associated muscles (the puborectalis, pubococcygeus, and iliococcygeus) that is commonly referred to as the levator ani. Contraction of the bulbospongiosus muscle following voiding helps evacuate the remaining urine in the penile urethra. The levator ani muscle is the "roof" of the ischioanal fossa; it extends up the sides of the pelvic wall to contact the obturator internus muscle. This fossa is largely filled with fat; however, infections in this area can spread anteriorly, superior to the deep perineal pouch. They are joined by the anterior rami of L4-S1 from above to form the sciatic nerve (L4-S3), which then exits the pelvic cavity via the greater sciatic foramen and enters the gluteal region. This muscle contracts during ejaculation, thus preventing the semen from entering the urinary bladder. The piriformis muscle, the gluteal arteries and nerves (superior and inferior), the pudendal nerve, and the internal pudendal artery all pass through the greater sciatic foramen to reach the gluteal region. The perineal body, or central tendon of the perineum, is an important fibromuscular support region and an attachment point for the perineal muscles and the female urethrovaginalis complex. The uterine artery lies within the cardinal ligament at the inferior aspect of the broad ligament (mesometrium) and contacts the uterus near the cervix. The rectouterine pouch (of Douglas) is the lowest point in the female abdominopelvic cavity and is where the peritoneum reflects off of the anterior rectum and is continuous with the broad ligament of the uterus. When a person is in the upright position, fluid in the cavity will ultimately flow into this low point. Incomplete fusion of the lower or distal portion of the paramesonephric (müllerian) duct can lead to partial or complete duplication of the uterus (bicornuate uterus). One of the most common causes of scrotal enlargement is hydrocele (excessive serous fluid within the tunica vaginalis). This usually occurs because of an inflammatory process, trauma, or the presence of a tumor. A small pouch of the processus vaginalis called the tunica vaginalis persists and partially envelops the testis. It is a piece of parietal peritoneum that envelops a portion of the testis as it passes through the deep inguinal ring. Much of the lymphatic drainage of the pelvic viscera follows the venous drainage of the same structures. However, some lymph from the perineum and the vestibule of the vagina and lymph that courses along the round ligament of the uterus (which passes through the inguinal canal) also drains into the superficial inguinal nodes. Although episiotomies are not routinely performed in the United States today, there are occasions when it is necessary to enlarge the vaginal opening, either with a midline episiotomy or a posterolateral approach. In the posterolateral approach, the incision usually will bisect the most posterior portion of the bulbospongiosus muscle; this is preferable to incising the perineal body. The obturator nerve and usually the artery pass along the deep lateral aspect of the pelvic wall on their way to the obturator foramen. In this location, they are closer to the ovary and its vessels than any of the other nerves in the option list. Damage to the nerve will weaken the adductor muscles of the medial thigh, which the nerve innervates. The middle (and inferior) rectal veins and their branches are part of the caval system and anastomose with the branches of the superior rectal vein, a tributary of the inferior mesenteric vein, which is part of the portal venous drainage. The only vessel in the list that travels through both the greater and lesser sciatic foramina is the internal pudendal artery. Hemorrhoids are symptomatic varicose dilations of the submucosal veins that protrude into the anal canal (internal hemorrhoids) or extend through the anal opening (external hemorrhoids). These rectal veins are tributaries of the middle rectal veins from the internal iliac veins and from the inferior rectal veins draining into the internal pudendal veins. The umbilical artery arises from the internal iliac artery and courses toward the abdominal wall, where it becomes a ligament.
Neither is superior; endovascular treatment is preferred for large aneurysms diabetes diet dogs buy generic amaryl online, hyperventilation is not necessary diabete association discount amaryl 1 mg buy on line, and hypotension could be hazardous diabetes signs of diabetes purchase genuine amaryl on line. A patient undergoing endovascular aneurysm suddenly becomes hypertensive to 180/100 diabetes insipidus bun order amaryl without a prescription, what could be happening Multidisciplinary consensus on assessment of unruptured intracranial aneurysms: proposal of an international research group managing diabetes through diet and exercise buy 1 mg amaryl. Current perspectives in imaging modalities for the assessment of unruptured intracranial aneurysms: a comparative analysis and review. Implementation of intraoperative neurophysiological monitoring during endovascular procedures in the central nervous system. Intracranial aneurysms treated with Guglielmi detachable coils: midterm clinical results in a consecutive series of 100 patients. Frequency of intensive care unit admission after elective interventional neuroradiological procedures under general anesthesia in a tertiary care hospital. Anaesthetic management for endovascular treatment of unruptured intracranial aneurysms. Sevoflurane for interventional neuroradiology procedures is associated with more rapid early recovery than propofol. The optimal depth for interventional neuroradiology: comparisons between light anesthesia and deep anesthesia. Risk factors for angiographic recurrence after treatment of unruptured intracranial aneurysms: outcomes from a series of 178 unruptured aneurysms treated by regular coiling or surgery. He is a vigorous person who lives alone, exercises regularly, and works part-time as a librarian. According to the next of kin, he was well the previous evening, approximately 12 hours ago. A general anesthetic versus a trial of mild to moderate sedation should be considered. After thorough consideration, the patient is intubated using 120 mg propofol and 50 mg rocuronium. The patient is extubated at the end of the procedure, and his neurological function is assessed in the postanesthesia recovery unit, showing no deficits. When one of the branches of the circle of Willis is occluded, there is an immediate deficit of oxygen supply to the area of the brain irrigated by the obstructed vessel. The symptoms are severe and include hemiplegia, neglect, and, if the dominant hemisphere is affected, aphasia and sometimes agitation; the patient may be obtunded and have dysphagia. Despite the symptoms, many patients have sufficient collateral circulation to keep most of the ischemic brain viable. The restrictions minimize the You reach the neurointerventionalist, who emphatically states that she needs you to help with the procedure as soon as the patient arrives. Presumably, he woke up with a stroke, and it is impossible to precisely ascertain how long ago it occurred. The procedure is indicated for patients who were functionally independent at baseline. Stroke is the leading cause of severe disability; the annual number of strokes is projected Table 9. Up to 87% of all strokes are ischemic, and the most devastating ones occur when a large intracranial vessel is occluded, usually by a thrombotic embolus originating either in the heart or aorta. Since the time the stroke occurred is unknown (so-called wake-up stroke), the issue at hand is whether there still is salvageable brain tissue as treatment of infarcted brain tissue is futile. A patient suspected of an acute stroke must have one of these imaging modalities as soon as possible. Even if he or she is found to have a lot of salvageable brain, penumbral tissue dies off as a function of time. Rapid recanalization of the occluded vessel and reperfusion of the viable brain is always a top priority. In an uncooperative, aphasic, or obtunded patient, airway examination may be impossible. This intervention is a true emergency, and risks associated with anesthetic management include the consequences of a rapid, often incomplete assessment. Oxygen supplementation is indicated only if SpO2 is lower than 94%1; the target should not result in hyperoxia. A single, gentle pass may be appropriate to decrease agitation due to bladder distension. Although initially derived from early retrospective data, the lowest acceptable value has long been considered 140 mm Hg. In In a case of acute stroke, anesthetic technique for the interventional treatment may vary widely considering either a general anesthetic or a mild to moderate sedation for the patient treated. For similar reasons, avoidance of hyperventilation and hyperoxia is probably beneficial. Their effectiveness in recanalization of cerebral vessels was established in 2012. Such a device, once deployed as a stent, restores partial flow in the target vessel and traps portions of the clot in its cells. The stent retriever can be withdrawn and reinserted until reperfusion is satisfactory. In addition, there was no involvement of anesthesiologists in either the trials or the resulting papers. Two practice workflow and anesthesia surveys from the United States and Scandinavia were published in 2017. Dexmedetomidine and propofol may both cause hypotension, but dexmedetomidine use requires higher doses of vasopressors. A small dose of fentanyl before deployment of the stent retriever and each withdrawal is helpful. They will be institutionspecific as they draw on the available resources and expertise. Early extubation and strict adherence to neurological protocols restricting oral intake until competent swallowing is demonstrated prevents postoperative pneumonia and improves stroke outcomes. Depressed consciousness, agitation, and risk of aspiration require general anesthesia with endotracheal intubation. Cooperative patients may be managed with local anesthesia only or with mild sedation. These findings are preliminary and may not be generalizable to all centers and all practice types. In light of the newest studies, intraarterial (endovascular) treatment (thrombectomy) for acute ischemic stroke can be performed until 24 hours after stroke onset. Select the most appropriate statement: a) False, the cutoff for treatment is 6 hours. Hypotension is a highly undesirable hemodynamic change, which may be responsible for poor neurological outcomes. Although seizures are a known complication of reperfusion after carotid endarterectomy, in the setting of acute ischemic stroke intracerebral hemorrhage is the most feared and life and function-threatening complication. Because of disruption of the blood-brain barrier in areas that were ischemic, hemorrhage is likely. There is recognition that hypocapnia may contribute to the poorer neurological outcomes associated with general anesthesia; one of the modifiable elements of management which may contribute to hypoperfusion of the ischemic areas of the brain is hypocapnia. All the randomized controlled trials focused on maintaining normoventilation and general anesthesia did not result in worsened neurological outcomes. This is a routine value that neurologists always obtain as part of the basic stroke work-up. In the randomized controlled trials comparing general anesthesia and sedation for stroke, many patients were excluded from randomization because of vomiting, agitation or impending respiratory compromise. The procedure is performed on a horizontal table with the head restrained, greatly increasing the risk of aspiration if vomiting occurs. Society for Neuroscience in Anesthesiology and Critical Care Expert Consensus Statement: anesthetic management of endovascular treatment of acute ischemic stroke. Anesthetic management and outcome in patients during endovascular therapy for acute stroke. Type of anesthesia and differences in clinical outcome after intra-arterial treatment for ischemic stroke. Effect of general anesthesia on functional outcome in patients with anterior circulation ischaemic stroke having endovascular thrombectomy versus standard care: a meta-analysis of individual patient data. Anesthesia practices for endovascular therapy of acute ischemic stroke: a Nordic survey. Wide variability in prethrombectomy workflow practices in the United States: a multicenter survey. Safety and hemodynamic profile of Propofol and Dexmedetomidine anesthesia during intra-arterial acute stroke therapy. Even small decreases in blood pressure during conscious sedation affect clinical outcome after stroke thrombectomy: an analysis of ischemic thresholds. Effect of conscious sedation vs general anesthesia on early neurological improvement among patients with ischemic stroke undergoing endovascular thrombectomy: a randomized controlled trial. General anesthesia versus conscious sedation for endovascular treatment of acute ischemic stroke: the AnStroke Trial (anesthesia during stroke). Effect of general anesthesia and conscious sedation during endovascular therapy on infarct growth and clinical outcomes in acute ischemic stroke: a randomized controlled trial. The daughter reports at least two previous occasions during the past 6 months when her mother suddenly felt "weak" and out of balance but that the symptoms disappeared shortly after their onset. The procedure proves difficult, and the neurosurgeon decides that open surgery is required. Microvascular anastomoses, on the other hand, are low-flow bypasses, also known as "indirect. Direct bypass retains a high patency rate at the added risk of hyperperfusion syndrome. As such, avoiding sharp spikes or drops in hemodynamics at induction, intubation, and surgical incision is a must. This can ensure early detection of hypotension in patients at risk of ischemia from reduced perfusion and hypertension in patients with aneurysms at risk for rupture. In addition, central venous access should be considered in patients with comorbidities, especially those anticipated to require vasopressor administration. The benefit here is twofold: the clinician can estimate the extent of local involvement as well as establish a baseline of symptoms against which all postoperative assessments will be compared. Alternatively, these patients may be otherwise healthy and in their early stages of life. Medical management of co-existing diseases (cardiovascular, pulmonary, endocrine, or otherwise) should be maintained per institutional guidelines. A multidisciplinary team is ideal in dealing with the ramifications of individual diseases and can ensure a safer process overall. Preoperative workup should include all the investigations normally recommended for a craniotomy. While the neurosurgery team operates on the cranium, the 80 · Anesthesia supplies Proposed setup of the operating room equipment. If the bypass is being done to circumvent an aneurysm, a gradual and slow induction is required to avoid severe hypotension or hypertension and rapid changes in aneurysmal transmural pressure which may lead to rupture and fatal bleeding. Typical drugs used include phenylephrine and ephedrine to treat hypotension, and barbiturates, opioids, blockers, or a combination of those to treat hypertension. Attention should be given to patients with comorbid conditions such as coronary artery disease or heart failure where coronary perfusion is crucial and episodes of severe or prolonged hypotension may precipitate myocardial injury. The existence of systolic and/or diastolic dysfunction necessitates careful titration of anesthetic agents with cardiodepressive effects, such as propofol and inhalational agents. Maintenance of general anesthesia should aim at achieving a steady state of hemodynamics as rapidly as possible. The use of an inhalational agent coupled with continuous short-acting analgesia with or without barbiturates can be an option. A continuous infusion of a neuromuscular blocking agent is also considered routine in several centers. A temporary clip is sometimes placed on a major feeding artery during anastomosis and can cause a dramatic decrease in blood flow to an area as large as an entire hemisphere. The surgeon will try to minimize the time spent during the temporary clip phase, but a few seconds may be enough to induce considerable damage. Hyperventilation may cause vasoconstriction, thus normocarbia is encouraged in these procedures. Too low Risk of complications Ischemia High risk Bleeding Moderate risk Lowest risk Blood pressure Blood pressure management and the risk of complications during surgery. Ideal hemodynamic management aims at maintaining blood pressure in the safe zone and avoids the risks of bleeding or ischemia with hypertension and hypotension, respectively. The lowest risk zone revolves around a theoretical blood pressure range that is set based on patient characteristics and surgical findings. A severe drop in blood pressure greatly increases the risk of hypoperfusion and brain ischemia, whereas a sharp increase in blood pressure predisposes to bleeding and worse outcomes. Any acute change in mentation or abrupt development of symptoms warrant emergent evaluation by the caregiver team. Hence, these patients are placed in high-acuity monitoring areas (such as a neurointensive care unit). Decreasing cerebral blood flow would lead to ischemia, especially in the penumbra. The following is false regarding Moyamoya disease: a) Risk is increased with family history. Moyamoya (Japanese for "puff of smoke") is a progressive arterial stenosis leading to the formation of multiple thin collaterals. It is more commonly seen in families of affected individuals, although any condition that leads to neovascularization could potentially give rise to a similar picture. The most common presenting symptom in the pediatric age group is cerebral ischemia, while bleeding is the more common presenting symptom in adults.
References
- Hillbom M, Kaste M. Ethanol intoxication: A risk factor for ischemic brain infarction. Stroke 1983;14:694.
- Steinhubl SR, Talley JD, Braden GA, et al: Point-of-care measured platelet inhibition correlates with a reduced risk of an adverse cardiac event after percutaneous coronary intervention: Results of the GOLD (AU-Assessing Ultegra) multicenter study, Circulation 103:2572, 2001.
- Frankenschmidt, A., Heisler, M. Fetotoxicity and teratogenesis of SWL treatment in the rabbit. J Endourol 1998; 12:15-21.
- Mine N, Yamamoto S, Saito N, et al. CBP501-calmodulin binding contributes to sensitizing tumor cells to CDDP and BLM. Mol Cancer Therapy 2011;10:1929-38.
- Magos AL, Boumas N, Sinha R, Lo L, Richardson RE. Transvaginal endoscopic oophorectomy. Am J Obstet Gynecol. 1995;172:123-4.
- Omoto R, Kyo S, Matsumura M, et al: Bi-plane color transesophageal Doppler echocardiography (color TEE): Its advantages and limitations, Int J Card Imaging 4:57-58, 1989.
