
Allegra
| Contato
Página Inicial
Deidra Candice Crews, M.D.
- Associate Vice Chair for Diversity and Inclusion, Department of Medicine
- Associate Professor of Medicine
https://www.hopkinsmedicine.org/profiles/results/directory/profile/0018671/deidra-crews
The study excluded cancer diagnoses made within two years of the diverticulitis diagnosis to eliminate cancers whose onset probably pre-dated the diverticulitis allergy medicine ok for dogs allegra 180 mg order line. The authors identified an increased risk of left-sided colon cancer compared with patients with diverticulosis without history of diverticulitis (odds ratio 4 allergy symptoms 4 year old buy allegra 120 mg mastercard. The researchers hypothesised that the increased inflammation of diverticulitis could be responsible for the increased risk allergy testing reliability buy 180 mg allegra otc, or that the two diseases share a common developmental pathway though this seemed less likely allergy medicine 44-329 discount allegra 120 mg visa, as the presence of diverticulosis without diagnosis of diverticulitis did not increase the risk of colon cancer allergy symptoms dark circles under eyes 120 mg allegra order with visa. The researchers noted that the yield for routine colonoscopy after diverticulitis is low and suggested that only those exhibiting alarm symptoms be screened, though they acknowledge that the risk of forgoing routine screening in their patient population would have missed a diagnosis of colon cancer in 0. These data suggest that a colonoscopy after complicated disease is more important than after uncomplicated diverticulitis. At this point in time, there is insufficient high-quality evidence to disavow the current practice offollowing up an attack of acute diverticulitis with screening colonoscopy within six to eight weeks of resolution, though perhaps further research in this area will help delineate target populations that demonstrate a higher yield. Traditionally, diverticulitis in the young has been viewed as a more virulent process than in patients over age 50. A number of early studies seemed to demonstrate that surgery was required in up to 88% of younger patients experiencing their first bout of acute diverticulitis. Recent studies, however, suggest that the underlying problem in younger patients is not a more aggressive disease course but is in fact an issue of initial misdiagnosis or attention to symptoms, leading to less defined criteria in those who might need surgery. The most common incorrect diagnosis was appendicitis, which was initially misidentified in nine (75%) of the misdiagnosed patients. The researchers concluded that though 35% of this cohort of younger patients had emergency surgery, only 16% had received a correct preoperative diagnosis and in fact needed operative treatment. Of these, 16 patients (35%) had surgery during the initial admission, but only three patients (19%) had been accurately diagnosed preoperatively. The 30 patients (65%) who were treated nonoperatively had successful resolution of their diverticulitis with only one patient needing a drainage procedure further along their course. The researchers suggested that the young adult presenting with abdominal pain, low-grade fever and leukocytosis should be evaluated for diverticulitis, particularly if they are obese and male. If the sigmoid colon is redundant and crosses the midline, the discomfort of sigmoid diverticulitis can mimic appendicitis. Despite the growth in diverticulitis knowledge, substantial gaps remain in some critical areas. Patients remain confused regarding the role of diet, family history and optimal timing for surgery. The traditional understanding of diverticulitis as an episodic condition is now changing and more data suggest chronicity to the condition in some patients. In a time of growing attention to patient-centred outcomes, the value of colectomy for these patients needs to be better understood and refined. Further diverticulitis research will shed more light on potential triggers, the colonic biome, medical therapy and other treatment alternatives. Diverticular disease as a chronic illness: Evolving epidemiological and clinical insights. Changing views on diverticular disease: Impact of aging, obesity, diet, and microbiota. Diarrhea-Predominant Irritable Bowel Syndrome Is Associated With Diverticular Disease: A PopulationBased Study. Usefulness of colonic motility study in identifying patients at risk for complicated diverticular disease. Alterations in colonic motility and relationship to pain in colonic diverticulosis. Diverticular disease associated with inflammatory bowel disease-like colitis: A systematic review. Review of current classifications for diverticular disease and a translation into clinical practice. The management of acute complicated diverticulitis and the role of computed tomography. Longterm risk of acute diverticulitis among patients with incidental diverticulosis found during colonoscopy. A prospective study of alcohol, smoking, caffeine and the risk of symptomatic diverticular disease in men. Pathogenesis of multiple diverticula of the sigmoid colon in diverticular disease. Colonic haustral pattern in relation to pressure activity and presence of diverticula. Interstitial cells of Cajal, enteric nerves, and glial cells in colonic diverticular disease. The anatomy, pathology, and some clinical features of diverticulitis of the colon. Transit times of food in patients with diverticulosis or irritable colon syndrome and normal subjects. Assessment of small intestinal bacterial overgrowth in uncomplicated acute diverticulitis of the colon. Diverticular disease of the colon: New perspectives in symptom development and treatment. Diet and the faecal microflora of infants, children and adults in rural Nigeria and urban U. Lymphoid tissue and lymphoid-glandular complexes of the colon: relation to diverticulosis. Diverticular disease in younger patients is it clinically more complicated and related to obesity Concurrent drug use and the risk of perforated colonic diverticular diseases: A population-based case-control study. Yamada E, Inamori M, Watanabe S, Sato T, Tagri M, Uchida E, Tanida E, Izumi M, Takeshita K, Fujisawa N, Komatsu K, Hamanaka J, Kanesaki A, Matsuhashi N, Nakajima A. Constipation is not associated with colonic diverticula: A multicenter study in Japan Neurogastroenterol Motil. Higher serum levels of vitamin D are associated with a reduced risk of diverticulitis. Diverticular disease and migration the influence of acculturation to a Western lifestyle on diverticular disease. Heritability and familial aggregation of diverticular disease: A populationbased study of twins and siblings. Acromegaly is associated with an increased prevalence of colonic diverticula: A case-control study. The resultant inflammation is confined to the bowel wall and the surrounding pericolic fat or mesentery and is usually self-limiting. This is in contradistinction to acute complicated diverticulitis which by definition is diverticulitis associated with a bowel obstruction, phlegmon, abscess, fistula or a free perforation. Approximately 20% of patients with uncomplicated diverticulosis will develop acute diverticulitis. A primary muscle abnormality is the most consistent and therefore diagnostic features of diverticular disease. The degree of muscle thickening correlates well with the macroscopic appearance of the disease. There is a tendency for the thickness of the colonic wall and the amount of elastic tissue to increase with age. Elastin seems to play an important role in the pathogenesis of diverticular disease. Symptoms include pain, commonly in the left lower quadrant, but occasionally in the suprapubic region or the right lower quadrant if the sigmoid colon is redundant. It is constant and approximately one-third of the patients have had at least one episode of similar pain. Nausea and vomiting are often associated with an ileus but may also indicate a mechanical bowel obstruction. Examination typically reveals localised tenderness and may include peritoneal signs such as focal guarding and rebound tenderness. The presence of diffuse peritonitis or a rigid abdomen suggests complicated disease. Appropriate laboratory investigations include a complete blood count, electrolytes and urinalysis. Although diverticula may be distributed throughout the colon, the muscle thickening is almost invariably confined to the sigmoid. Characteristically, diverticula are found between the mesentery and the two anti-mesenteric taeniae. The arcade penetrates the longitudinal muscle before it reaches the anti-mesenteric taeniae. The point of vascular penetration results in an area of weakness which corresponds to the primary site of diverticula. A pulsion diverticulum consists of mucus membrane and muscularis mucosa which projects through the circular and longitudinal muscle of bowel wall. The common differential diagnosis includes colorectal cancer, acute appendicitis, inflammatory bowel disease, infectious colitis, ischaemic colitis, bowel obstruction, urinary tract infection or stones and other acute gynaecologic conditions including pelvic inflammatory disease. It is very accurate with a sensitivity and specificity of 98% and 99%, respectively, and a low false positive rate. Immunocompromised patients may not mount a normal inflammatory response and may have only extraluminal gas in isolation without the typical findings of diverticulitis. Although ultrasound has a diagnostic accuracy as high as 97%, it is operator-dependent and may be difficult to perform in patients with abdominal pain. In general, the higher the disease stage, the more likely surgery will be required. Uncomplicated disease is classified as 60 80 40 Time to recurrence (months) 100 48. In the absence of sepsis or signs of generalised peritonitis, patients with free air can be treated non-operatively and observed. However, there is a growing body of evidence that each patient requires evaluation on an individual basis and that within the disease spectrum, a subset of patients may not require either antibiotics or dietary restriction and many can be treated in an outpatient setting. Inpatient Recent studies suggest that outpatient treatment is safe, effective and appropriate for many cases of acute uncomplicated diverticulitis. All patients received the first dose of antibiotics intravenously in the emergency room. There was no difference in the response to treatment Management 987 between the groups. The overall healthcare costs were three times greater in the inpatient setting with no differences observed in the quality of life between the two groups. Antibiotics In general, antibiotics have been viewed as essential for the management of all cases of acute diverticulitis. Despite the traditional view that the pathophysiology is an infectious process, to date there have been no direct studies concerning the microbiology of acute uncomplicated diverticulitis. Moreover, most clinical studies examine antibiotic usage in complicated diverticulitis that requires either surgical or radiologic intervention with extrapolation to uncomplicated disease. Additional indirect evidence comes from antibiotic treatment of acute intestinal perforations secondary to other gastrointestinal pathology which may or may not be applicable. With the increasing incidence of antibiotic-resistant bacteria and the rise in iatrogenic infections such as Clostridium difficile, the necessity of antibiotics for all patients with uncomplicated diverticulitis has been questioned. Patients in the antibiotic arm received one of three options: a second or third generation cephalosporin intravenously in conjunction with metronidazole or a carbapenem antibiotic or piperacillin/tazobactam. Upon clinical improvement, patients in the antibiotic arm were switched to oral ciprofloxacin or cefadroxil combined with metronidazole for a combined total duration of seven days of intravenous and oral coverage. Data from these two trials suggest that the use of antibiotics does not reduce the duration of symptoms in acute uncomplicated diverticulitis. However, the results were not statistically significant and were imprecise with wide confidence intervals. Patients with clinical signs of sepsis and with significant co-morbidities as well as immunocompromised patients were excluded from both trials. Based on best evidence, withholding antibiotic treatment should be limited to reliable, good risk patients with uncomplicated disease without signs of sepsis or generalised peritonitis who are easily observed and followed. Patients who do not fall into this category should be treated with a course of antibiotics. Clearly, additional primary data is needed and this recommendation may change as additional evidence becomes available. Antibiotics should be chosen based on the known bacterial groups associated with diverticulitis and must include broad activity against enterobacteriaciae, enteric anaerobes, some activity against Staphylococcus sp. Dual agent therapy is also effective and can include a third-generation cephalosporin or a fluoroquinolone in combination with metronidazole. Surprisingly, there is very little evidence regarding the timing of step down to oral therapy. There is a growing realisation that patients receive antibiotics for much longer than is necessary, contributing to the emergence of resistant bacterial species. Provided there is clinical improvement with resolution of symptoms in a patient who is not immunocompromised, antibiotics should be limited to a total of four to seven days. Patients who develop complicated disease may require an extended course of antibiotics as outlined in Chapter 49. Clinical Course Up to 90% of patients with acute uncomplicated diverticulitis will respond to non-operative management, many in the outpatient setting. Any increase in fever, pain or an inability to tolerate oral intake requires urgent reassessment by the medical team and may be an indication for hospitalisation. Inpatients who deteriorate or fail to improve over 48 to 72 hours of optimal management should be reassessed for the development of complicated acute diverticulitis. Depending on the clinical picture, these patients may require reimaging to assess for the development of an abscess with subsequent percutaneous drainage if indicated. Patients who suffer an acute clinical deterioration or develop an irreversible complication may require an urgent laparotomy.
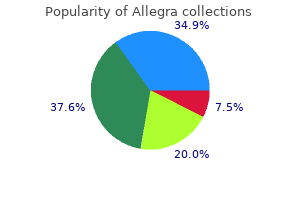
Many patients with rectal cancer express an explicit wish to avoid a definitive stoma allergy shots nausea buy cheap allegra 120 mg on line. Very low and intersphincteric anastomoses for distal rectal cancer can avoid a definitive stoma allergy symptoms 3 months discount allegra 180 mg otc, but the functional outcome is often poor allergy medicine gluten free 180 mg allegra with visa. The concern about the oncological risk of organ preservation is that some local regrowths may not be amenable to salvage surgery and that some regrowths could be the source of metastases allergy symptoms when it rains cheap 120 mg allegra with mastercard. Although the available studies described below generally suggest that this risk is small with adequate selection and follow-up allergy testing tampa 180 mg allegra for sale, the exact risk in different clinical situations is not yet well established. This should be communicated clearly with patients who are considered candidates for organ preservation and should be balanced against the possible benefits of the approach. In this tradeoff decision process for an individual patient there are broadly two types of considerations. The second type of considerations are more subjective and concern quality of life issues such as disturbed body image with a colostomy, impaired anorectal function in distal anastomoses, urogenital dysfunction, etc. Although there is an increasing interest in organ preservation strategies, especially from the patient community, there are still many unanswered questions. Although there is some overlap, the studies fall into three main categories: (1) patients with a more advanced tumour with an accepted indication for neoadjuvant chemotherapy who show a very good clinical response at restaging and who enter a watch-and-wait (W&W) programme; (2) patients with a smaller tumour that could well be treated with surgery alone, but who are treated with chemoradiation with the explicit aim of organ preservation, often with incorporation of a local excision and (3) patients with a very high operative risk or who refuse surgery. Watch-and-Wait After the pioneering paper by Angelita Habr-Gama from Sao Paulo in 20044 on a watch-and-wait strategy for clinical complete responders, a number of other positive reports have been published. There is a large variation in treatment protocols: radiation dose, number of fractions, inclusion of boost, concomitant chemotherapy combinations and consolidation chemotherapy. Some of the papers describe the complete population that received chemoradiation whereas other papers only describe the complete responders, and it is therefore difficult to estimate the exact percentage of patients that might benefit from a W&W policy. Patients with distal tumours are generally very motivated for organ preservation because they are facing a rectal amputation or a very low anastomosis with the risk of a poor function. Another important issue in comparing the different series is the proportion of smaller tumours. Whereas the majority of patients in most series are T3 tumours, half of the patients in the prospective study of Appelt et al. In this study, chemoradiation is given with the specific aim of organ preservation. The oncological concern of W&W is undetected residual disease in either the bowel wall or lymph nodes that could lead to a regrowth that is not amenable to salvage surgery and that could be the source of metastases. This cannot, however, be considered as absolute proof because the series are relatively small and there is no method other than a randomised comparison that can completely exclude bias. To avoid those types of local regrowths, some studies have included only clinically N0 patients. There are, however, patients who decline completion surgery, and the series of Pucciarelli and Verseveld show that the majority do not recur locally. Further differentiation between pT2 low-risk (G12/ L0/V0) versus pT2 high risk (G34/L1/V1) can also be helpful in deciding the optimal treatment for an individual patient. Radiotherapy as Definitive Treatment for Inoperable Patients There are patients with rectal cancer who are not candidates for surgical resection, either because they are medically unfit or the tumour is technically unresectable. Some series report on the results of radiotherapy as definitive treatment, which are summarised in Table 39. The series all have different proportions of medically unfit patients, unresectable tumours and patients refusing surgery, and are therefore difficult to compare. Generally, better local control rates are obtained with higher doses of radiotherapy. According to the series from Princess Margaret Hospital in Toronto, a 30% local control rate is obtained for mobile or partially fixed tumours, whilst in more advanced lesions the results are more disappointing. In the older series often radiotherapy alone was used, whereas at present, chemoradiation is more often used in patients who can tolerate it, with higher response rates and a prolonged local control. Some series with relatively small tumours report a higher local control rate in the range of 70%. The conclusion is that radiotherapy alone as a definitive treatment has a high failure rate in larger tumours and can only be considered in patients with relative or absolute contraindications for surgery. The success rate is higher with higher doses of radiotherapy, with chemoradiation and with smaller tumours. With the recent interest in organ preservation and response assessment, this interval has been challenged. If residual tumour is overlooked and a false diagnosis of (near) complete response is made, patients are at risk for local regrowth. Restaging modalities have therefore been a subject of investigation and are constantly evolving. When the nodes have become smaller, it is more difficult to rule out remaining nodal metastases. Lymph node specific contrast agents could offer some help, but this is still investigational. Biopsies unfortunately have a limited clinical value for ruling out residual cancer due to sampling errors. The main disadvantage is that there is a higher complication rate than in non-irradiated patients, with a painful slow healing ulcer as one of the more troublesome complications. It is clear that in patients who have a true complete response, a local excision is of no benefit to the patient. Although at present there is not enough data to define the exact roles of W&W and local excision in organ preservation, it is clear that they are complementary. In addition to the standard follow-up after treatment of rectal cancer aimed at detection of metastases, follow-up in an organ preservation programme is also aimed at early detection of local regrowth. The vast majority of local regrowths after W&W are located intraluminally and occur within 1218 months. A substantial number of these regrowths occur in the surrounding lymph nodes, and imaging is essential for early detection and treatment. Comparing serial images provides a powerful tool for early detection of a regrowth. The best follow-up schedule is yet to be determined and should take into account the higher incidence of regrowth in the first one to two years. At endoscopy, only the rectum is examined with a flexible sigmoidoscope, without sedation and without oral bowel preparation. However, alternative treatment options can be considered in various situations, such as a high operative risk or patient preference to avoid major surgery with the risk of a poor functional outcome and/or a definitive colostomy. Patients who have been treated initially with an organ preservation approach are sometimes reluctant to give up this approach. For an isolated luminal regrowth after W&W, there is the alternative option of a local excision or endoluminal radiotherapy. The W&W series show that with adequate follow-up and early detection, local regrowths are mostly amenable to salvage treatment with good outcome. With a good follow-up, regrowths are detected when small and only rarely extend to the Functional Outcome and Quality of Life 793 39 (a) (b) (c) (d) (e) (f) 39. There is one report that describes more fibrosis with a longer interval, without an increased risk for complications. For patients with a high operative risk, or patients who desperately want to avoid a definitive colostomy, local luminal regrowths can be treated with a repeated local excision or endocavitary radiotherapy, accepting a higher repeated recurrence rate. In some patients, it is decided not to treat a local regrowth because of widespread metastatic disease, high co-morbidity, old age or patient choice. After low anterior resection, deterioration of bowel function is common, especially after neoadjuvant chemoradiotherapy. Reportedly, up to 75% of patients experience severe dysfunction 794 Chapter 39 Organ Preservation in Rectal Cancer on a long-term basis. Although functional problems can occur after organ preservation strategies, because of the long-term radiotherapy effects, the few available data suggest that compared to a low anterior resection, patients report significantly less change in bowel habit, less incontinence and a lower defaecation frequency. There is a need for better data on the functional outcome of organ preservation strategies. Studies with a total dose of 5560 Gy show organ preservation rates of more than 50%. Prediction of Response Many studies have reported baseline clinical variables that are associated with a higher incidence of complete response, such as lower T stage, lower N stage, small tumour volume, etc. The baseline prediction is of little value for patients who have a more advanced tumour with an accepted indication for neo-adjuvant therapy. For patients with smaller tumours that can be treated with surgery alone but who also have a higher chance of a complete response to chemoradiation, the prediction at primary presentation, however, is potentially highly interesting. With the combination of variables obtained from clinical data, tumour biopsies and radiological images, a good predictive model could support a more rational treatment choice that maximises oncological and functional outcome and minimises the use of futile radiotherapy. In patients who already have received chemoradiation and who show a very good response and patients who are facing a rectal amputation, a randomised trial will be more difficult to run. Many of these patients express a strong preference to avoid major surgery and/or a definitive colostomy. The next best level of evidence consists of large well-documented prospective cohort studies. Combining data of centres that practice watch-and-wait into a large database, such as the International Watch and Wait Database, provides an opportunity to study and compare real-world differences in assessment, follow up and outcome. Because of the high interest by patients in preserving quality and function, we suggest that the surgical community should cautiously move ahead and offer the option of organ preservation to patients in a controlled setting and combine this with reporting the outcome. This can be achieved by setting up a prospective organ preservation protocol with standardised assessment and follow up in centres that add their data to a large multicentre database. This will provide high-quality information on the benefits and risks whilst offering patients an improved quality of life. Apart from increasing the interval, there are two main ways to increase the response rate: intensifying radiotherapy and adding systemic therapy. As in many other tumours there is a doseresponse relationship for rectal cancer, and a significant increase of response is expected with doses higher than the currently used 4550. Low anterior resection syndrome score: Development and validation of a symptom-based scoring system for bowel dysfunction after low anterior resection for rectal cancer. Operative versus nonoperative treatment for stage 0 distal rectal cancer following chemoradiation therapy: Long-term results. Wait-and-see policy for clinical complete responders after chemoradiation for rectal cancer. Nonoperative management of rectal cancer with complete clinical response after neoadjuvant therapy. High-dose chemoradiotherapy and watchful waiting for distal rectal cancer: A prospective observational study. Watch-and-wait approach versus surgical resection after chemoradiotherapy for patients with rectal cancer (the OnCoRe project): A propensity-score matched cohort analysis. Long-term outcome of an organ preservation program after neoadjuvant treatment for rectal cancer. Predictors of pathologic complete response following neoadjuvant chemoradiotherapy for rectal 15. Comparative analysis of late functional outcome following preoperative radiation therapy or chemoradiotherapy and surgery or surgery alone in rectal cancer. Long-term outcome in patients with a pathological complete response after chemoradiation for rectal cancer: A pooled analysis of individual patient data. Wait-and-see or radical surgery for rectal cancer patients with a clinical complete response after neoadjuvant chemoradiotherapy: A cohort study. Surveillance after neoadjuvant therapy in advanced rectal cancer with complete clinical response can have comparable outcomes to total mesorectal excision. Transanal endoscopic microsurgery for residual rectal cancer after neoadjuvant chemoradiation therapy is associated with significant immediate pain and hospital readmission rates. Primary radical external beam radiotherapy of rectal adenocarcinoma: Long term outcome of 271 patients. Treatment of rectal adenocarcinoma with endocavitary and external beam radiotherapy: Results for 199 patients with localized tumors. Increasing the interval between neoadjuvant chemoradiotherapy and surgery in rectal cancer: A meta-analysis of published studies. Assessment of clinical complete response after chemoradiation for rectal cancer with digital rectal examination, endoscopy, and mri: Selection for organsaving treatment. Comparison of magnetic resonance imaging and histopathological response to chemoradiotherapy in locally advanced rectal cancer. Low anterior resection syndrome and quality of life: An international multicenter study. Radiation dose-response model for locally advanced rectal cancer after preoperative chemoradiation therapy. Watch and wait approach following extended neoadjuvant chemoradiation for distal rectal cancer: Are we getting closer to anal cancer management Role of biopsies in patients with residual rectal cancer following neoadjuvant chemoradiation after downsizing: Can they rule out persisting cancer Long-term follow-up features on rectal mri during a wait-and-see approach after a clinical complete response in patients with rectal cancer treated with chemoradiotherapy. Seventy percent of patients present with limited disease, whereas 30% present with locally advanced or distant metastatic disease. The liver is the main metastatic site, and 15%25% of all colorectal cancer patients present with synchronous liver metastases. The peritoneum is the second common metastatic site for colorectal cancer with 30%40% of patients affected. Ten to twenty percent of all patients with colorectal cancer develop pulmonary metastases. Noteworthy, lymph node metastases of the common or external iliac vessels or the aorta are considered distant metastases, too. Overall median survival in patients with metastatic colorectal disease is reported as up to 30 months; therefore, this situation poses a challenge to the interdisciplinary team caring for these patients. Synchronous metastases are usually diagnosed at time of diagnosis of the primary cancer; however, occasionally they lead to the diagnosis.
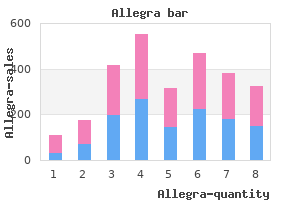
It has to be accepted that there is some selection bias when using historical comparisons allergy forecast milwaukee generic allegra 180 mg on line. Nevertheless allergy treatment clinic cheap allegra uk, 5-year survival rates after pulmonary metastasectomy for colorectal cancer have not improved over the last 20 years allergy testing guildford generic 120 mg allegra with amex, with 5-year overall survival of 39%68% after metastasectomy allergy symptoms scratchy throat order allegra 180 mg online, suggesting that modern chemotherapeutic agents have not greatly influenced the course of disease in these patients allergy symptoms alcohol 120 mg allegra order with amex. Currently, the first randomised trial comparing the outcome of patients with pulmonary metastases of colorectal cancer after metastasectomy vs. In a retrospective analysis the five-year overall survival after pulmonary metastasectomy was 45. The major problem after pulmonary metastasectomy is the pulmonary recurrence with reported rates of 44%66%. Complete resection of pulmonary metastases should be functionally possible and complete tumour resection obtained. Even with cases of simultaneous liver metastases, curative surgery is still possible. In the case of synchronous liver and pulmonary metastases, transdiaphragmatic resections is feasible. Whilst authors emphasise the advantage of reduced invasiveness with the transdiaphragmatic approach, there is a higher risk of biliary complications, which can lead to a fatal outcome. However, the appearance of hilar or mediastinal lymph node metastases has a negative impact on patient survival. Authors reported five-year overall survival of 45%50% for patients without lymph node metastases vs. A retrospective analysis during simultaneous lymph node dissection or lymph node sampling in colorectal pulmonary metastasectomy showed a 20. Consequent, routine lymph node dissection is generally advised during pulmonary metastasectomy. Wedge Resection Negative resection margins after resection of colorectal lung metastases are essential for disease-free survival and overall survival. Anatomic resection is not superior to wedge resection as long as a R0 resection can be obtained. Thoracotomy Another question is the technical approach of pulmonary metastasectomy. Authors report a median overall survival rate of 57% and a disease-free survival rate of 36% at three years. Clinical score for predicting recurrence after hepatic resection for metastatic colorectal cancer: Analysis of 1001 consecutive cases. Surgical management of patients with colorectal cancer and simultaneous liver and lung metastases. Cytoreductive surgery combined with perioperative intraperitoneal chemotherapy for the management of peritoneal carcinomatosis from colorectal 5. Resection margin and survival in 2368 patients undergoing hepatic resection for metastatic colorectal cancer: Surgical technique or biologic surrogate Margin status remains an important determinant of survival after surgical resection of colorectal liver metastases in the era of modern chemotherapy. The effect of a primary tumour resection on the progression of synchronous colorectal liver metastases: An exploratory study. The liver-first approach to the management of colorectal cancer with synchronous 3. Synchronous colorectal liver metastasis: A network meta-analysis review comparing classical, combined, and liver-first surgical strategies. Kinetic growth rate after portal vein embolization predicts posthepatectomy outcomes: Toward zero liver-related mortality in patients with colorectal liver metastases and small future liver remnant. Two-stage hepatectomy versus 1-stage resection combined with radiofrequency for bilobar colorectal metastases: A casematched analysis of surgical and oncological outcomes. Cost-utility analysis of operative versus non-operative treatment for colorectal liver metastases. Primary tumor resection in colorectal cancer with unresectable synchronous metastases: A review. Update on the prevention of local recurrence and peritoneal metastases in patients with colorectal cancer. Surgical management of peritoneal carcinosis: Diagnosis, prevention and treatment. Complete cytoreductive surgery plus intraperitoneal chemohyperthermia with oxaliplatin for peritoneal carcinomatosis of colorectal origin. Survival of patients with colorectal peritoneal metastases is affected by treatment disparities among hospitals of diagnosis: A nationwide population-based study. Peritoneal colorectal carcinomatosis treated with surgery and perioperative intraperitoneal chemotherapy: Retrospective analysis of 523 patients from a multicentric French study. Cytoreductive surgery and hyperthermic intraperitoneal chemotherapy in the management of peritoneal surface malignancies of colonic origin: A consensus statement. Revised guidelines for second-look surgery in patients with colon and rectal cancer. Risk-reducing laparoscopic cytoreductive surgery and hyperthermic intraperitoneal chemotherapy for low-grade appendiceal mucinous neoplasm: Early outcomes and technique. Intraoperative hyperthermic versus postoperative normothermic intraperitoneal chemotherapy for colonic peritoneal carcinomatosis: A case-control study. Role of hyperthermic intraoperative peritoneal chemotherapy in the management of peritoneal metastases. Metastatic colorectal cancer: Survival comparison of hepatic resection versus cytoreductive surgery and hyperthermic intraperitoneal chemotherapy. Comparison of prognostic scores for patients with colorectal cancer peritoneal metastases treated with cytoreductive surgery and hyperthermic intraperitoneal chemotherapy. Hyperthermic intraperitoneal chemotherapy using a combination of mitomycin C,5-fluorouracil, and oxaliplatin in patients at high risk of colorectal peritoneal metastasis: A Phase I clinical study. Cytoreductive surgery and hyperthermic intraperitoneal chemotherapy for peritoneal carcinomatosis from colorectal and gastrointestinal origin shows acceptable morbidity and high survival. Melphalan: A promising agent in patients undergoing cytoreductive surgery and hyperthermic intraperitoneal chemotherapy. Hyperthermic intraperitoneal chemotherapy with melphalan: A summary of clinical and pharmacological data in 34 patients. Closed abdomen hyperthermic intraperitoneal chemotherapy with irinotecan and mitomycin C: A phase I study. Phase I and pharmacological studies of adriamycin administered intraperitoneally to patients with ovarian cancer. Progression following neoadjuvant systemic chemotherapy may not be a contraindication to a curative approach for colorectal carcinomatosis. Evaluation of the cost-effectiveness of cytoreductive surgery and hyperthermic intraperitoneal chemotherapy (peritonectomy) at the St George Hospital peritoneal surface malignancy program. Long-term results of lung metastasectomy: Prognostic analyses based on 5206 cases. Resection of pulmonary metastases from colon and rectal cancer: Factors to predict survival differ regarding to the origin of the primary tumor. Recognition and treatment of organ dysfunction following therapy is another important component of follow-up. As the rationale of a follow-up program is difficult to argue against, the possible benefit is much more debatable since evidence of benefit is often lacking, and decisions often rely on common sense, tradition and available resources. In the absence of absolute evidence, most organisations responsible for the surveillance of cancer treatment have agreed-upon algorithms and guidelines. Introduction of screening programs for colorectal cancer has changed the disease by finding smaller cancers in a less-advanced stage. At the other end of the spectrum, more extensive resection with multi-organ enbloc resection now can be performed. This increasing diversity in treatments argue for a follow-up program that should be tailored to the individual. The stage of the disease is a determining factor when it comes to setting up a surveillance program. It is important to balance patient preferences, heath status, co-morbidity, age, willingness to comply and the ability of the patient to undergo aggressive retreatment if recurrence is identified. Surveillance could also harm the patient by adding unnecessary examinations and operations with no benefit to the patient survival and by inducing psychological stress related to the numerous investigations involved. It is necessary to document that the institution fulfil recommended national standards with mortality and morbidity rates that are within an acceptable level and that the quality of the surgical specimens,5,6 the radiology and the pathology adhere to best practice. At the post-operative multidisciplinary pathology conference, valuable feedback on preoperative staging, treatment planning and surgical quality can be achieved. Furthermore, separation between inpatient and outpatient care may set up barriers for collecting and sharing of data. Through national registers it is possible to benchmark between departments by specified key 831 832 Chapter 41 Follow-Up and Post-Operative Sequelae in Colorectal Cancer indicators for best practice. It is important that these data should be of maximal quality to inform for further decision-making and strategic planning. From an institutional and societal perspective, health economic aspects are also important. Fixed budgets force the need for prioritisation of resources, such as access to investigations and outpatient clinics. There is a need to find a balance between the potential benefits or harm to the asymptomatic patient with no spread of the disease as well as to symptomatic patients with suspected recurrence or treatable side effects. By early detection of either a local recurrence or a distant metastasis, the chance of cure is likely to be more favourable since the critical window of opportunity for re-intervention remains open for curative treatment. In case of inoperable disease, early detection can also lead to early introduction of third-line chemotherapy with significantly improved quality of life (QoL) in the remaining life years. It is generally accepted that follow-up should be most intensive during the first two years since 60%80% of recurrences occur within that timeframe (Table 41. Extending the program beyond five years is usually not recommended since less than 10% of recurrences happen that late, and the benefit of surveillance is then diluted. This visit allows for detection of early treatment complication, such as wound infection, pain, impaired nutritional status, stoma problems, psychological sequelae, recovery of basic organ functions and return to normal life. The focus should be on rehabilitation, and action should be taken to ensure that the primary healthcare system can support the patient. General health should be assessed, and any persistent organ dysfunction such as bowel, bladder and sexual dysfunction should be explored and investigated. A second aim is to discuss the staging and pathology report with the patient so as to plan possible adjuvant therapy and agree on the future surveillance. The potential benefit of added visits in the oncological outpatient clinic fall outside of the scope of this chapter. Afterwards colonoscopy performed every 3 to 5 years for the duration of the patient active life. Rehabilitation 833 Intraluminal Recurrent Disease Following restorative surgery for rectal cancer or after local excision, a rectal examination and proctosigmoidoscopy will be scheduled to detect a possible extraluminal local recurrence or the rare anastomotic recurrence. Metachronous cancer and synchronous adenomatous polyps should be excluded by colonoscopy preoperatively, but if this is not possible preoperatively, colonoscopy should be done within six months post-operatively. The rate of metachronous cancer is low (<2%),17 but the risk of a second cancer is up to 8%. The risk of developing metachronous adenomatous polyps is between 30% and 56%1 or higher in a cancer surveillance cohort in comparison to patients with adenomatous polyp alone in the general population. Early detection will increase the critical window of opportunity for intervention. It is fair to predict that in the future there will be a collection of biomarkers that can be used as initial surveillance, and additional imaging techniques will then follow. Previously, chest X-rays and abdominal ultrasonography were used, but the benefit of crosssectional imaging has made these techniques obsolete. However, every cancer patient treated with curative intent has to face the fear of recurrence in the remaining life span. Other patients report increased fear of recurrence due to the repeated visits, resulting in depression and anxiety. The gastrointestinal sequelae of treatment have a significant negative impact on rehabilitation, social activities and QoL on cancer survivors. This calls for a re-thinking of the follow-up strategy with improved focus on late morbidity and rehabilitation. These issues should be highlighted at the preoperative information and counselling of patients. Once identified, the functional problems should be addressed in collaboration with the patient. It may be difficult to select only one answer, as we know that for some patients symptoms vary from day to day. We would kindly ask you to choose one answer which best describes your daily life. No, never Yes, less than once per week Yes, at least once per week No, never Yes, less than once per week Yes, at least once per week 0 9 11 0 11 16 Q. Several efforts to restore reservoir function have been made in the form of coloplasty, side-to-end anastomosis and J-pouch. The main benefits of these modifications are in the first one to two years but seems to diminish thereafter. Anal sphincter manometry has failed to show any significant change in anal sphincter function related to surgical or oncological treatment. In general, the sympathetic nerves inhibit peristalsis, whereas the parasympathetic nerves promote peristalsis. After rectal resection, the bowel proximal to the anastomosis is without parasympathetic (and to some extent without sympathetic) extrinsic innervation due to central vessel ligation causing damage to the sympathetic supply from the superior hypogastric plexus in the front of the aorta. Therefore, it is of importance to select patients who will actually benefit from radiotherapy. In the longer term, radiation causes ischaemic and fibrotic changes as well as initial mucosal inflammation.
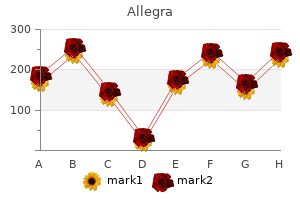
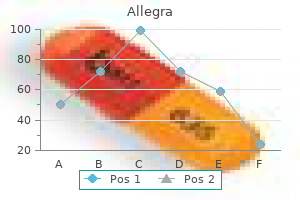
This approach is generally advocated to exclude the presence of a malignancy or an alternative diagnosis such as ischaemic colitis or inflammatory bowel disease allergy symptoms grass buy allegra with american express. This approach is encouraged in order to avoid potential conversion of a sealed microperforation into a free perforation allergy symptoms medication order 180 mg allegra mastercard. Others have demonstrated that colonoscopy during an acute episode of diverticulitis can be safe allergy symptoms versus sinus symptoms buy allegra online now. Even when optical examination of the colon is performed in the acute setting allergy shots lower immune system allegra 120 mg purchase otc, a significant number of the procedures cannot be completed medisana medinose nasal allergy treatment 45030 cheap allegra 180 mg without prescription. The presence of air in the urinary bladder in the absence of instrumentation is considered diagnostic. Patients who develop fistulas generally do not need emergent intervention as the abscess has decompressed. Colovesical fistulas are the most common (65%), followed by other types of fistulas including colovaginal, coloenteric, colouterine and colocutaneous fistulas. Patients often present with prominent urinary symptoms including polymicrobial urinary tract infections, pneumaturia and faecaluria. If performed, cystoscopy shows inflammation generally at the dome of the bladder and, on occasion, vegetable material in the urine. Colovesical fistulas may also be associated with locally advanced bladder or primary colon cancer. Cystoscopy and colonoscopy may be appropriate to exclude a malignancy under appropriate clinical circumstances. The surgical principles for treatment of colovesical fistulas due to diverticular disease include resection of the affected segment of colon, almost always the sigmoid. Management of complicated diverticular disease is dependent on the particular presentation of the disease. Treatment of the complications of diverticulitis may range from treatment with bowel rest and parenteral antibiotics to emergent exploratory laparotomy. We will review the treatment options for each of the complications of diverticulitis separately. In some cases, the precise site of the fistula cannot be determined because of the associated phlegmon and abscess, and pinching it off the bladder is sufficient treatment in most cases. A primary anastomosis between the descending colon and the upper rectum can usually be performed safely. On occasion, non-operative management may be used for colovesical fistulas especially if the symptoms are minor and the patient has medical co-morbidities conferring a significant operative risk. However, if non-operative treatment is advised, patients must be warned about the potential lethal threat of urosepsis. Often, women have seen a gynaecologist initially for evaluation of a vaginal discharge sometimes with gas. A single stage sigmoid resection with primary anastomosis can generally be performed, pinching off the site of the fistula from the top of the vaginal vault and interposing omentum. Diverticular Abscess Diverticular abscess occurs in approximately 10% to 25% of patients with acute diverticulitis. In women, an abscess associated with a diverticula phlegmon may involve the adenexa resulting in tubo-ovarian abscess. Traditionally, patients with diverticulitis and an associated abscess were treated by antibiotics and percutaneous drainage followed by interval elective sigmoid resection. This approach was based on the observation that over 40% will develop recurrent sepsis. Abscesses less than 4 cm in size often resolve with intravenous antibiotics alone without the need for further procedures. A recent review suggested 20% to 30% of diverticular abscesses were amenable to percutaneous drainage and the failure rate of percutaneous drainage was 20% to 30%. If the abscess is not accessible by this route, a transgluteal, transperineal or transrectal route may be employed. Transabdominal drainage tends to be better tolerated when compared to other access routes. In patients with simple unilocular abscesses, successful drainage is achieved in approximately 80%. Patients with more complex abscesses associated with loculations or fistula or when drainage route transverses normal organs are associated with a higher failure rate. The decision to perform a sigmoid resection following successful drainage of a diverticular abscess should be approached on a case by case basis. Whilst 40% to 50% of patients admitted with diverticular abscesses respond to conservative treatment, sigmoid resection is recommended for selected patients particularly those who present at a young age, those with complex or larger abscesses, those with recurrent symptoms and those that develop a fistula especially a colocutaneous fistula. Retroperitoneal abscess in particular appears to be associated with recurrence of diverticulitis (Hazard ratio of 4. These diverticula affect men and women equally and most but not all are found in the sigmoid colon. The average diameter is 13 cm but diverticula as large as 40 cm have been reported. One proposed mechanism is that the giant colonic diverticulum is simply a large abscess cavity that continues to communicate with the colon. Another proposed theory is that the diverticulum becomes massive because of a ball-valve mechanism allowing air into but not out of the diverticulum. Some have suggested air becomes trapped in the diverticulum as a result of gas forming micro-organisms without obstruction at the neck of the diverticulum. It is not essential to remove the entire cavity; however, resection of the affected colon is essential. Nevertheless, these patients typically are systemically ill and require a large amount of healthcare resources. Whilst large bowel obstruction is most commonly associated with obstructing colon cancer, approximately 10% of large bowel obstructions are attributable to diverticular disease. The small bowel can also become adherent to a focus of inflamed colonic tissue leading to small bowel obstruction. The approach to management depends on whether the obstruction is partial or complete. Patients with a partial obstruction that resolves with bowel rest, intravenous hydration and antibiotics may be able to undergo elective resection. In some patients, treatment of the acute inflammatory phlegmon allows the obstruction to resolve. Endoscopic or radiologic evaluation can then be performed and elective resection planned. In the past, persistence of obstruction after treatment with antibiotics typically required sigmoid resection and end colostomy. However, reversal of the Hartmann procedure may be technically difficult with an increased risk of anastomotic leakage necessitating a covering stoma. Whilst the Hartmann resection is still an excellent option in selected patients, other options include: a) sigmoid resection with primary anastomosis with or without a diverting proximal stoma (usually a loop ileostomy), b) on table lavage and primary anastomosis or c) colonic stenting placement followed by semielective sigmoid resection. On table lavage is a technique which allows clearing of the faecal-laden, obstructed colon before a potential anastomosis. A foley catheter attached to warm irrigation fluid is introduced through the appendix. If surgically absent, the catheter may be placed through a caecotomy or ileostomy. Corrugated anaesthesia tubing is placed through the distal colon and secured with umbilical tape. The technique may be used in selected patients who are haemodynamically stable and in whom there is minimal contamination. Whilst the need for mechanical bowel preparation has been called into question for elective colon resection, this claim has not been critically evaluated in patients with bowel obstruction. There were no anastomotic leaks in this series but there was a significant (18%) incidence of wound infection. A number of authors have demonstrated that treatment of acute colonic obstruction with self-expanding metal stents is a viable option particularly in patients with obstructing colon cancer. In a series of 104 procedures from one centre, eight patients had obstruction from a benign aetiology. From a technical standpoint, stenting a diverticular stricture which is potentially longer or more angulated may be more difficult than stenting a 49 49. Arrow shows a retrograde injection of contrast within the rectum which is unable to pass the obstruction. Colonic stenting in benign disease remains a controversial procedure and should be embarked upon with caution. The objective is to remove the affected segment of colon whilst minimising damage to adjacent anatomical structures. An additional consideration is the restoration of intestinal continuity depending on clinical circumstances. The sigmoid colon is mobilised and proximal and distal points selected for resection. The proximal resection margin should be in soft pliable bowel and it is not necessary to resect all proximal diverticula. The distal resection margin is the proximal rectum as anastomosis to the distal sigmoid is associated with a higher risk of recurrent diverticulitis. One study suggested an inframesenteric dissection with preservation of the inferior mesenteric artery decreased the incidence of anastomotic leak. Faecal diversion with can be considered in a number of clinical circumstances but these are beyond the scope of this chapter. Patients are usually maintained with a urinary catheter for several days post-operatively. We advise a check cystogram to ensure healing of the bladder repair before urinary catheter removal. Although they do not prevent ureteral injuries, they permit easy recognition and repair of such injuries. Minimally Invasive Colectomy the advent of laparoscopic surgery has ushered in a new era in the surgical management of diverticular disease. In the last decade, increasing numbers of resections for diverticular disease have been performed laparoscopically. Conventional laparoscopic techniques allow the surgeon to perform all the major portions of the case, including the anastomosis through small 5 or 12 mm trocars. The dissection can be carried out in a medial to lateral or lateral to medial approach. The sigmoid colon can then be mobilised up to the level of the splenic flexure by sweeping down the attachments of the left colonic mesocolon to gerotas fascia and retroperitoneum. It may be necessary to mobilise the splenic flexure to perform a tension-free anastomosis, and there is evidence that suggests the incidence of splenic injury is lower with a laparoscopic approach. Alternatively, the anastomosis can be fashioned through the specimen extraction site. Use of the extraction site in cases of fistulas or abscesses often allows the laparoscopic completion of colectomies in patients with severe disease without conversion. Nonetheless, there is a wide range of published conversion rates as demonstrated in Table 49. The colon can be mobilised from a lateral to medial or medial to lateral approach. The specimen is typically extracted through a periumbilical vertical incision and the anastomosis performed in an intracorporeal fashion. Often patients may have suffered with chronic inflammation for a long period of time. Although the rectum is not primarily involved with diverticulitis, inflammation of the proximal rectum may be encountered from the diverticular phlegmon or from an associated pelvic abscess or diverticular perforation. In such cases, based on sound surgical judgement and specific intraoperative factors, primary anastomosis potentially to the mid rectum with proximal faecal diversion may be performed. It is our practice to infiltrate the bladder with a methylene blue solution to look for evidence of a sizeable defect in the bladder wall. If there is one present, then it typically is repaired with two layers of absorbable suture. No differences were noted when comparing complications, mortality, length of stay or oral feeding. These authors demonstrated no difference in anastomotic leak rates and intraoperative complications. It should be noted, however, that patients with complicated disease underwent conversion to open procedures more frequently (23% vs. Although patients in the laparoscopic group recovered bowel function more quickly (3. Whilst many of the current treatment methods have been used for the greater part of a century, their mode of application continues to evolve. As in all inflammatory conditions, the initial goal of therapy is to control infection. Once this is done, the surgeon is left with a variety of treatment algorithms and options which must be individualized for each patient. Prospective evaluation of hand-assisted laparoscopic techniques demonstrate that although operative times are similar to conventional laparoscopic surgery, conversions are less frequent (0% vs. The Norfolk Surgical Group demonstrated that ileus and length of stay were less in patients who had their sigmoid colectomy completed laparoscopically. Acute left colonic diverticulitis: A prospective analysis of 226 consecutive cases. Colonic diverticulitis: Impact of imaging on surgical management A prospective study of 542 patients. Long-term follow-up after an initial episode of diverticulitis: What are the predictors of recurrence Elective resection versus observation after nonoperative management of complicated diverticulitis with abscess: A systematic review and meta-analysis.
180 mg allegra order with visa. Celiac Disease vs. Gluten Intolerance.
References
- Mohr DN, Silverstein MD, Heit JA, et al: The venous stasis syndrome after deep venous thromboembolism or pulmonary embolism: A population-based study, Mayo Clin Proc 75:1249, 2000.
- Delaney KM, Reddy SH, Dayama A, et al: Risk factors associated with bladder and urethral injuries in female children with pelvic fractures: an analysis of the National Trauma Data Bank, J Trauma Acute Care Surg 80(3):472n476, 2016.
- Rogers TR. Optimal use of existing and new antifungal drugs. Curr Opin Crit Care. 2001;7(4):238-241.
- Adamek, H.E., Jakobs, R., Buttmann, A., Adamek, M.U., Schneider, A.R., Riemann, J.F. Long term follow up of patients with chronic pancreatitis and pancreatic stones treated with extracorporeal shock wave lithotripsy. Gut 1999;45:402-405.
- Maehama T, Dixon JE. The tumor suppressor, PTEN/MMAC1, dephosphorylates the lipid second messenger, phosphatidylinositol 3,4,5-trisphosphate. J Biol Chem 1998;273(22):13375-13378.
- Sansone GR, Frengley JD. Impact of HAART on causes of death of persons with late-stage AIDS. J Urban Health 2000; 77:166.
- Trachtman H, Christen E, Cnaan A, et al. Urinary neutrophil gelatinase-associated lipocalcin in D+HUS: a novel marker of renal injury. Pediatr Nephrol. 2006;21:989-994.
- Rabkin CS, Janz S, Lash A, et al. Monoclonal origin of multicentric Kaposi's sarcoma lesions. N Engl J Med 1997;336(14):988-93.
