
Arcoxia
| Contato
Página Inicial
Tracy L. Sprunger, PharmD, BCPS
- Associate Professor of Pharmacy Practice, Butler University College of Pharmacy and Health Sciences, Indianapolis, Indiana
http://www.usaprn.org/state-prn--school-contacts/indiana-2/tracy-l-sprunger-pharmd.html
Most antigens currently evaluated are cell surface associated arthritis in cats back order arcoxia 60 mg on-line, but cytoplasmic and nuclear antigens arthritis in back and stomach pain 90 mg arcoxia buy otc. A number of commercially available reagents are available for fixation and permeabilization of cells prior to the addition of antibodies to cytoplasmic and nuclear antigens treating arthritis of the big toe buy 120 mg arcoxia with mastercard. When both cell surface and cytoplasmic antigens are evaluated in the same assay arthritis in dogs what age generic 90 mg arcoxia mastercard, the surface staining is performed first arthritis of feet buy cheap arcoxia online. The cells then are fixed and permeabilized, followed by staining for cytoplasmic and nuclear 74 antigens. It is important to note that the permeabilization process introduces some amount of artifactual, background "shift" in antigen expression. Assessment of antigen expression in permeabilized cells must be performed using the level of expression of known positive and negative cellular populations as controls. Instrument Configuration and Quality Control Deciding upon the number of antigens to simultaneously evaluate is dependent on the model of flow cytometer used. Single-laser flow cytometers typically are used to evaluate three or four antigens simultaneously, in addition to the two light scatter properties of forward scatter (proportional to cell size) and side scatter (also known as orthogonal or 90-degree light scatter, which is proportional to cytoplasmic complexity and granularity). Although most clinical flow cytometry laboratories use six- or eight-color flow cytometry for leukemia and lymphoma immunophenotyping, 10-color machines are now commercially available for clinical use. The simultaneous assessment of such a large number of antigens minimizes the number of tubes that must be set up, and therefore is of particular benefit for the analysis of paucicellular specimens, while offering the potential for cost savings. On a less frequent basis, the linearity of detected fluorescence should be confirmed by using a series of microbeads with known fluorescence properties ranging from negative to very bright; in addition, acceptably low levels of cell carryover between specimens must be confirmed. Antibodies: Compensation and Panel Design Each fluorochrome has well-characterized absorption and emission spectra. Because the emission spectrum of each commonly used fluorochrome extends over a range of wavelengths (Table 2. Antibodies typically are used in defined combinations, or panels, to answer specific questions about specific cell populations. For example, most laboratories that perform leukemia and lymphoma immunophenotyping have an acute leukemia panel designed to distinguish acute myeloid leukemia from acute lymphoid leukemia and a lymphoma panel to distinguish benign from malignant lymphoid tissue. Although a detailed discussion of flow cytometric panel design is beyond the scope of this chapter, suffice it to say that a great deal of thought must go into panel design. At a minimum, antibody panels should measure a sufficient number of antigens to distinguish normal and benign from abnormal and neoplastic cell populations with a high degree of sensitivity and specificity. However, the quality of the flow cytometric data also depends on how antibodies are used in combination. Conversely, it may be unwise to use a bright fluorochrome to detect a strongly expressed antigen, because the bright fluorescence emission will likely create compensation problems due to spillover. When a specimen is received in the flow cytometry laboratory, it is important that the pathologist or flow cytometry technologist consider the underlying clinical question in deciding which panels to use. On the other hand, when the clinical question is much broader, for example, when ruling out a hematolymphoid neoplasm in the marrow of a patient with pancytopenia and no known malignancy, then a broader evaluation of the myeloid, lymphoid, and plasmacytic lineages is likely to be appropriate. When clinical concern exists for a lymphoproliferative disorder, then it is prudent to evaluate both the B cells and T cells, whenever possible. However, because B-cell lymphomas are much more common than T-cell lymphomas, if analysis is limited by a paucity of cells in the specimen, it is reasonable to rule out a B-cell malignancy before evaluating the T cells. In flow cytometry parlance, a particle of sufficient size to be detected is typically a cell, but is referred to as an "event". The number of events required for evaluation depends on both the purpose of the flow cytometric evaluation and the nature of the specimen. For example, if one is evaluating a lymph node that is replaced by lymphoma, acquisition of a relatively low number of events per tube of cells and antibodies. In most laboratories, if adequate cells are available, then at least 100,000 viable cells are routinely collected per tube. However, at least 500,000 cells will be collected to quantify stem cells in a specimen being evaluated for use in stem cell transplantation. Assuming that the presence of 50 cells would enable confident identification of a population, then the evaluation of 500,000 cells offers the ability to detect a population at a frequency of 1 in 10,000 cells, or 0. A potential artifact in the evaluation of flow cytometric data is carryover from one tube to the next, in which stained cells from previous specimens accumulate in the tubing of the instrument and are released in relatively small numbers as subsequent acquisition occurs. The hazard in carryover is that certain combinations of bound fluorochromes on the contaminating cells could lead to interpretation as a small abnormal cell population, suggesting the possibility of malignancy despite the fact that no such cell population truly exists in the specimen in question. Most clinical flow cytometers have manufacturer specifications guaranteeing no more than 1% carryover, and these instruments frequently demonstrate much less carryover in practice. One way to accomplish this is to run plain sheath fluid through the instrument between tubes and to monitor the data generated by such a procedure to ensure that no increase occurs in the number of cellular events beyond the usual background level for the instrument. In this process, greater and greater numbers of extraneous cellular events are excluded from the analysis in a sequential manner, to maximize the likelihood of identifying an abnormal cell population. The first step is exclusion of doublets (cohesive aggregates of cells and/or platelets). After excluding cellular aggregates, nonviable cells are excluded, which is necessary due to their nonspecific antibody binding. Nonviable cells have porous membranes that leak out cytoplasmic contents and nuclei that are shrunken, so these events are compact with low forward and side scatter. Forward versus side scatter gating also will exclude any residual, un-lysed erythrocytes, due to their small size and lack of granules. Aberrant antigen expression indicating a neoplastic population typically includes: An abnormal decrease in the expected level of expression of an antigen in the cells of interest, including complete loss of expression. Lastly, no studies have shown strong data indicating that finding an "abnormal" maturation pattern is predictive of transformation to a clinical neoplasm. Although some attempts have been made, no recommendations have been widely adopted. A critical fact that must always be taken into account is that flow cytometry findings are reported to the clinical team, who typically have little or no practical experience in flow cytometry. As such, the interpretation must be clear and precise, rid of extraneous, possibly misleading information. To indicate which populations were analyzed, and for billing purposes, a list of tested antigens must be included. The immunophenotype of each abnormal cell population, including the proportion of the total viable cells represented by each abnormal population should be reported in a free-text format. Descriptions of the fluorescence intensities of diagnostically relevant antigens are useful, especially considering that many reports are used as a basis for detecting residual disease after therapy. The addition of key two-dimensional histograms to the report can provide a snapshot of a neoplastic immunophenotype that can be of great help in assessing residual disease when subsequent specimens are received. The analysis and interpretation should be directed toward the clinical query or prior diagnosis. It should begin with a binary statement of positive or negative, followed by statements citing which cell populations were analyzed. If positive, the percentage of total cells should be cited along with the most salient immunophenotypic properties. Although specimens are sometimes received for the evaluation of other immune abnormalities, any interpretation of the results should be performed with great caution. The rosette test is still the most widely used screening test in the United States. Still, flow cytometry can be useful in confirming that a myeloid population is neoplastic when diagnostic features are not known or are pending evaluation. What follows is a concise description of flow cytometry for clinically relevant purposes in myeloid neoplasms. Aside from subtle abnormalities like abnormally dim or abnormally bright expression of expected antigens, detection of aberrant antigen expression is useful and important. Again, dim/partial expression is not significant, but uniform expression by a distinct, discrete myeloid population is typically indicative of a neoplasm. Diagnostic criteria for myeloid neoplasms in which the neoplastic cells are mature. The use of flow cytometry in such diseases is limited to the assessment of blasts in the event that a blast crisis has been diagnosed by clinical and morphologic findings. Also, cases with "abnormal maturation patterns" in which diagnostic criteria are not met are not found to have an increased future risk for development of a myeloid neoplasm. Also important is the general lack of lymphoid antigen expression (although some lymphoid antigens may be aberrantly expressed by neoplastic blasts). Acute biphenotypic leukemia is rare, and coexpression of markers for all three lineages is extremely rare. In cases in which surface antigen evaluation is ambiguous for lineage, cytoplasmic antigen evaluation frequently is helpful. Because no well-defined immunophenotype exists in mixed phenotype acute leukemia, these cases must be evaluated on a case-by-case basis. Finally, both mixed phenotype acute leukemia and acute bilineal leukemia should be distinguished from undifferentiated acute leukemia. These neoplasms are defined by lymphoblast morphology and confirmed by immunophenotype. Whereas a population of some sIg+ and some sIg+ reactive B cells is called polytypic, a neoplastic population with only sIg+ or sIg+ is called "monotypic. For example, an sIgk+ lymphoma may exist in a specimen with a relatively large number of nonneoplastic B cells; because the background B cells have a normal:, the overall ratio may be skewed only slightly or not at all, depending on the size of the neoplastic population. In such cases, permeabilizing the cells and assessing cytoplasmic immunoglobulin light chain expression often shows clear monotypic expression. Whereas the process of B-cell ontogenic maturation is limited to peripheral lymphoid organs, T-cell populations are highly plastic at all sites. Also, temporary "abnormal" T-cell populations commonly arise during immune reactions and can be seen in numerous clinical scenarios in patients with different kinds of illnesses. Because any clinically relevant neoplasm is an abnormal growth, diagnosis of a neoplasm must be based upon demonstration of an expanded population. Although it involves skin and marrow, because it is typically leukemic, a blood sample usually is submitted for diagnosis. Because most patients are asymptomatic, a definitive diagnosis is not usually required. The diagnosis of lymphoma is typically easy to make on the basis of a large population of circulating and/or infiltrative, markedly atypical lymphoid cells. For these reasons, bone marrow core biopsy immunostaining is the best and most accurate technique for analysis of myeloma (see below). Because "junk" and dead cells typically fall on that line, in general, populations of cells in that location would be assumed to be "background," not representing true expression. An important concept that should be emphasized is that, consequent to the action of therapeutic drugs, often, the immunophenotype of the cancer cells changes after therapy. In others, there are subtle changes, like a decrease or increase in the level of expression of an antigen. In some cases, the changes are relatively dramatic, prompting reversion to genetic analysis, to prove the relationship to the prior cancer. The methods described are proprietary, requiring specific, nonstandard processing machinery, reagents, and cytometers; as such, the published methods for circulating tumor cell detection cannot be performed in a 90 standard laboratory. After the collection, the photographed events are visually examined by a technologist, who decides whether the "positive event" is actually a tumor cell. Moreover, its use seems to be waning and there are questions about the efficacy of the information. The advantages are cost savings due to the use of far less reagents and labor savings due to not having to maintain the flow cytometry apparatus. The downside is that, because the aliquots in the wells are so small, the number of cells analyzed is far less. Still, for most specimens, laser scanning cytometry works well for diagnostic purposes. The reasons for such limited use are not known, but may be due to resistance to change platforms and/or to a lack of effective marketing from laser scanning cytometry manufacturers. Although some practitioners are adept at analysis of maturation patterns for diagnostic purposes and have supported its use since the late 1990s, this technique has never found widespread acceptance for diagnostic purposes or been included in any well accepted scheme for diagnostic criteria. Unlike solid organs, in which most of the cells in a biopsy are tumor cells, in hematopoietic lesions, the cells of interest are admixed with large populations of background cells. For most purposes, a skilled practitioner can find a population of interest on one slide, then look at another slide and discern whether the second antigen is expressed by the population of interest, by inference from the spatial location in the tissue. In t(11;14), the Ig heavy chain gene regulatory elements on chromosome 14 cause massive overexpression of cyclin D1 by acting on the translocated gene. By contrast, the extra copy of cyclin D1 in hyperdiploidy, due to an extra copy of chromosome 11, causes only mild overexpression by a gene-dosage effect. Counting can be performed with an ocular grid or by taking a photomicrograph and counting on the screen. It is a tertiary, molecular conformation, the -pleated sheet, that may be composed of any of several different protein building blocks, most commonly Ig light chains. As such, diagnosis remains dependent on demonstrating amyloid by staining with Congo red, a solution containing red crystals that are of the perfect size to deposit into the deep groves of the -pleated sheet. Although seeing that there are dark red, extracellular deposits by regular light microscopy generally indicates amyloid, it must be confirmed by demonstrating birefringence, the property of rotating the plane of polarized light. Positive amyloid birefringence when viewing a slide by polarized light is classically apple green, but may also be of other colors. Mass Spectrometry for Amyloid Diagnosis the advantage of this technique is that it can identify the type of protein making up an amyloid deposit. Because therapy is markedly different for amyloidosis of different protein types, this is very important. However, it should be emphasized that, due to technical limitations, mass spectrometry cannot be used to diagnose amyloid. Mass spectrometry can only be used to determine the protein composition of amyloid once a deposit has already been identified by Congo red staining.
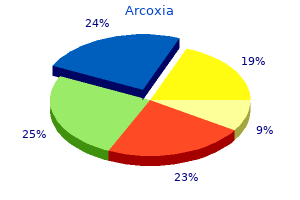
The speculum should remain in place so that both hands can be removed arthritis medication gold order 60 mg arcoxia free shipping, making it possible for the examiner to handle other equipment arthritis in young dogs uk buy arcoxia once a day. Inspect the cervix for color chinese medicine arthritis diet arcoxia 120 mg with amex, position crippling arthritis definition arcoxia 120 mg buy line, size arthritis in fingers uk cheap 90 mg arcoxia overnight delivery, surface characteristics, shape of the os, and discharge. The cervix is remarkable for the vast variety of shapes, sizes, and appearances that are within the range of health. Symmetric, circumscribed erythema around the os is a normal finding caused by exposing, or everting, the columnar epithelium lining of the endocervical canal. This eversion results from pressure of the speculum blades against the anterior and posterior fornices. Knowledge of cervical anatomy is important to document normal findings versus abnormalities, including presence of the squamocolumnar junction, ectropion, and transformation zone based on age, phase of the menstrual cycle, pregnancy, menarche, menopause, and malignancy. The most common position of the cervix is posterior, indicating an anteverted uterus. The cervix should be located in the midline; significant deviation may indicate a pelvic mass or adhesions. The diameter of the cervix is approximately 2 to 3 cm, and its length is approximately 3 cm. Nulliparous Parous Stellate 118 Chapter 6: Gynecologic History and Physical Examination the surface should be smooth. Nabothian cysts may be seen as small white or yellow, raised areas; these retention cysts of endocervical glands are a normal variation (see Chapter 26). Note any friable tissue, a strawberry appearance, abnormal coloration such as a blue or purple tinge, granular areas, or red or white patchy areas. Note any discharge, and determine if its source is vaginal, which is far more common than a cervical origin. Normal vaginal discharge is odorless, creamy or clear, and thick or thin, depending on time in the menstrual cycle. Three types of specimens are frequently collected at this point in the speculum examination: cervical cells for cytology screening; a vaginal or endocervical sample for gonorrhea, chlamydia, and trichomoniasis testing; and vaginal secretions for microscopy (see the chapter appendices for information on these procedures). In some laboratories, the same cervical sample is used for cytology screening and gonorrhea, chlamydia, and trichomoniasis testing. If separate cervical samples are collected for these tests, the optimal order for collecting these specimens is unknown because no evidence exists to guide this choice. Vaginal swabs are the preferred specimen type for such testing, even when a full pelvic examination is performed (Papp, Schachter, Gaydos, & Van Der Pol, 2014). To begin removing a metal speculum, loosen the screw on the thumbpiece, but press on it to keep the blades open as the speculum is withdrawn from around the cervix. If using a plastic speculum, press on the thumbpiece to release it from the notch that has kept the anterior blade open. Once the cervix is no longer within the speculum blades, release most of the pressure on the thumbpiece, and rotate the speculum back to the oblique angle. Depending on the vaginal anatomy, the cervix may not release easily from within the blades. If this occurs, use the speculum handle as a lever and gently lift and lower the speculum body while slowly retracting the blades, until the cervix releases. The pulling and compression of the cervix into the vaginal canal as the speculum is removed often causes significant discomfort at this point of the examination if not given careful attention and patience. Vaginal mucosa should be almost the same color as the cervix, and the surface should be moist and smooth or rugated. Taking care not to pinch the vaginal mucosa, quickly and completely withdraw the speculum in an upward direction, but with downward pressure, similar to that used during insertion. This maneuver provides the most comfort for the woman, and avoids unintentional and unnecessary pressure against the urethra and suprapubic bone. As with the speculum examination, the bimanual component of the examination is included for specific clinical reasons. This examination is not required annually for pelvic health screening for asymptomatic women, nor is it a necessary component of every examination for symptomatic evaluation if there is no concern or symptom for which an internal examination would provide further information. The bimanual examination, as with all components of any examination, should be used intentionally and to garner specific information and assist in overall health determination. Remove the glove from one hand, and lubricate the index and middle fingers of the gloved hand. Generally the dominant hand is gloved and used for the internal examination, but this is a clinician preference. Using the thumb and fourth finger, separate the labia to visualize the vaginal introitus. Place the index and third fingers just inside the vaginal orifice, press downward and encourage the woman to relax her perineum as much as possible, and gently insert the fingers, maintaining posterior pressure, to the posterior fornix. As the examination continues, be careful of where the thumb of the examining hand is resting. Avoid touching the clitoris or the underlying clitoral body, which is usually very sensitive. Once the hand is rotated superiorly, consciously extend the thumb as far laterally as possible to avoid unconsciously folding it medially and inadvertently resting it on the clitoris during the examination. Locate and palpate the end of the cervix with the palmar surface of the examining fingers, then run the examining fingers around the circumference of the cervix to feel the size, length, shape, and consistency. A nonpregnant cervix will be firm, like the tip of the nose, while during pregnancy it is softer. Assess for cervical motion tenderness by grasping the cervix gently between the examining fingers, moving it from side to side once, and observing the woman for any expression of pain or discomfort. Begin palpation of the uterus by placing the ungloved hand on the abdomen, halfway between the umbilicus and the pubis at the midline. Palms should be facing each other, with one internally on the 120 Chapter 6: Gynecologic History and Physical Examination anterior vaginal wall and the other externally on the abdomen. Slowly slide the abdominal hand down toward the pubis, pressing downward and forward with the flat surface of all four fingers. This combination of abdominal and vaginal pressure will feel as if the two hands are pressing against each other. The uterus is relatively mobile, usually inclines forward at about 45°, and is essentially flat. If the uterus cannot be palpated with the maneuver described in step 5, keeping the hand palm-up, place the vaginal fingers together in the posterior fornix with the abdominal hand at the pubis. With the vaginal fingers turned upward, press up against the cervix moving it inward. If the uterus still is not palpated, move the vaginal fingers to the sides of the cervix, one on each side, pressing the cervix inward as far as possible. Then move one finger on top and the other beneath the cervix, continuing to press inward, while pressing down with the abdominal fingers. Confirm the location of the uterus as midline, regardless of its anterior, midposition, or posterior position. This examination should not cause pain, although a sensation of pressure is common. Continue the bimanual examination by palpating the ovaries and surrounding area, called the adnexae. This term refers to the areas lateral to the uterus, which are taken up by the broad ligaments, as well as to the structures located there. At the same time, with the abdominal hand, sweep the flat surface of the fingers deeply inward and obliquely down toward the pubis. Often normal ovaries are difficult to palpate because they are small, sometimes positioned deep in the pelvis, or obscured by the presence of abdominal adipose tissue or tense abdominal muscles. If the ovaries are palpable, this examination usually causes momentary moderate pain when the ovaries are located. However, palpable ovaries in postmenopausal women are reason for concern and require follow-up. If the ovaries are not felt after thorough palpation with one or two sweeps, the examination is normal in the absence of any clinical signs or symptoms, and does not require repeating or further pressure or palpation. Once the adnexal examination is completed, remove the intravaginal fingers, and take off and discard the examination glove. Give her a moment to adjust her position and become comfortable, and then offer her tissues to wipe excess secretions and lubricant. Rectovaginal Examination this part of the pelvic examination allows palpation to a depth of an additional 2. Such an examination is perhaps most useful if the uterus is retroflexed or retroverted. It is usually an uncomfortable examination, but once mastered, can be very rapidly completed. Many clinicians omit this examination because the vaginal examination allows for sufficient palpation of gynecologic organs and because digital rectal examination to collect a stool sample for fecal occult blood testing is an unacceptable screening strategy for colorectal cancer screening (Levin et al. Especially in asymptomatic women, this examination may be eliminated as part of routine screening and health maintenance. Pelvic sidewall practitioners continue to utilize this examination for women who may experience difficult vaginal examinations, for pediatric pelvic examination, or for those women for whom an evaluation for a rectovaginal fistula is necessary. Learning to perform a gentle rectal examination is an important skill for any clinician, though it should be utilized sparingly and with full consent from the individual. Before beginning, tell the woman that the rectum and vagina will be briefly examined. Inform her that this may be uncomfortable and may also cause a sensation similar to that of having a bowel movement. Put an examination glove on one hand, and lubricate the index and third fingertips with water-soluble gel. Place the third finger against the anus, ask the woman to bear down, and insert this finger into the rectum just past the sphincter. Palpate the anorectal junction and rotate the examining finger to sweep over the anterior and then posterior rectum that can be reached above the sphincter. Now also insert the index finger of the examining hand into the vagina as far as it will go. The posterior surface of the uterus should be palpable, especially if it is retroverted. If the findings of the adnexal examination were questionable, repeat that examination as described previously. Gently remove the examining fingers, inspect for secretions, and prepare a specimen for fecal occult blood testing if indicated. If the clinician is not sure of the implications of the finding, it is reasonable to say so, but also assure the woman that consultation with another health professional will be sought promptly, and that a more complete explanation and plan will be forthcoming. Encourage women to voice their concerns, questions, and reactions to the examination. Discuss ways the woman may contact the provider after the examination with any recollected health history, new questions, or follow-up needs. Clinicians should balance medically accurate documentation of the physical examination and recommendations with more personal information. The effect of vaginal speculum lubrication on the rate of unsatisfactory cervical cytology diagnosis. The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Lubrication of the vaginal introitus and speculum does not affect Papanicolaou smears. The role of gel application in decreasing pain during speculum examination and its effects on Papanicolaou smear results. Female genital mutilation/ cutting: A statistical overview and exploration of the dynamics of change. For many years, specimens were collected using a special wooden spatula (Ayer spatula), sometimes in conjunction with a cotton-tipped swab. The conventional method of preparing the sample for cytology is the Papanicolaou (Pap) smear, which entails applying the specimen to a glass slide. Limitations of this method of specimen collection and preparation are well documented. They include not obtaining sufficient endocervical cells for adequate laboratory cytologic evaluation; unavoidably leaving much of the cellular sample on the collection device when transferring the materials to the glass slide; and obscured detection of abnormal cells due to the presence of blood, mucus, air-drying, or other artifacts on the slide. Newer specimen collection devices and liquid-based preparation methods have been developed to try to overcome these limitations and improve cervical cytology screening. Endocervical brushes plus spatulas, brooms, and extended-tip spatulas are all effective. Liquid-based methods for cervical cytology screening (ThinPrep, SurePath) allow for more complete removal of cellular material by rinsing the sampling devices in a liquid medium. Cells for cytologic examination are removed from the medium via a filtering process that minimizes the presence of obscuring artifacts. A disadvantage of liquid-based methods is their higher cost compared to the conventional (Pap) cytology method. Additionally, liquid-based cytology is not considered diagnostic for trichomoniasis. These considerations, and the failure of scientific evidence to establish clear superiority of one 126 Appendix 6-A: Cervical Cytology Screening 127 method over the other, have led multiple organizations to recommend that use of conventional cytology or liquid-based cervical cytology is acceptable (American College of Obstetricians and Gynecologists, 2012, reaffirmed 2015; Saslow et al. Procedures for both conventional and liquid-based methods for cervical cytology screening using the different specimen collection devices are described in the next section. Assemble the necessary materials: a labeled container for one or two standard microscope slides, slides, spatula, endocervical brush, and canister of fixative. Tell the woman the Pap smear will be performed and she may feel slight pressure or discomfort, which is caused primarily from the contact of the sampling devices with the endocervix. Visualize the cervix, using the speculum examination procedure described in this chapter. Turn the spatula over, and spread the secretions from the second side of the spatula onto the slide.
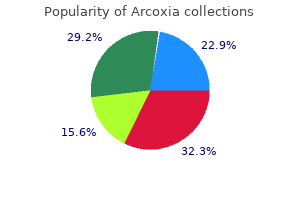
Management of invasive cancer is highly individualized and emphasis is on selecting the most conservative and appropriate treatment consistent with cure of the disease (Hacker et al rheumatoid arthritis lyme disease buy discount arcoxia. Localized wide excision involves removing the tumor and at least a 1-cm margin of normal tissue surrounding the tumor to limit recurrence arthritis diet mcdougall buy cheap arcoxia 120 mg online. Such surgery is the preferred intervention for women with early-stage vulvar cancer (American College of Obstetricians and Gynecologists arthritis pain suddenly worse 90 mg arcoxia order free shipping, 2011a; Hacker et al rheumatoid arthritis diet vegetarian order arcoxia overnight delivery. Lymph node exploration is recommended when higher-grade vulvar tumors are present or when diagnostic testing indicates cancer spread (Preti et al arthritis red feet buy 120 mg arcoxia free shipping. Because groin invasion of vulvar cancer carries a much higher mortality risk, appropriate lymph node management is the single most important factor in reducing mortality from earlystage vulvar cancer (Hacker et al. Sentinel node biopsy and dissection is the preferred method of lymph node evaluation and treatment. It carries less risk of wound breakdown and the lower-extremity lymphedema that is seen following more invasive inguinofemoral node dissection (Deppe et al. Chemotherapy and radiation treatment options for vulvar cancer have been limited to adjuvant use for locally advanced or metastatic disease, but both are being increasingly used in patients with earlier stages of the disease (Deppe et al. It can be used for single or multifocal lesions, although the risk of recurrence may be higher than with surgical wide excision. Emerging Evidence That May Change Management Research into the genetic and epigenetic changes that play a role in the carcinogenesis of vulvar cancer may lead to greater insight into the etiology of vulvar cancer, assist in predicting prognosis, and guide development of new targeted therapies (Trietsch et al. Identified characteristics and capabilities of cancer cells have been used to develop new cancer-fighting drugs that disrupt cellular signaling pathways or utilize cells of the immune system to modify cell functions affecting cancer growth and spread (Porth, 2015). Targeted therapy approaches are at the forefront of improving treatment and outcomes for all women who have gynecologic cancers. Women diagnosed with vulvar cancer require anticipatory education prior to treatment about the potential complications of any therapeutic option. Chronic lymphedema of the lower extremities may occur in patients who have undergone radical lymph node dissection, and may develop either early or late after treatment (Deppe et al. Lymphedema and surgically induced anatomic changes to the urinary meatus may cause the urinary stream to change direction, causing urine to "spray" rather than "stream. Regular (three times a week) use of vaginal dilators or regular sexual intercourse can help to stretch vaginal tissues and should be initiated before the vaginal introitus becomes stenotic. If introital stenosis occurs, the clinician may need to use a pediatric speculum for vaginal visualization, and insert only a single digit when palpating the vagina. Some degree of sexual dysfunction is almost always present with definitive treatment of vulvar cancer. In particular, problems with arousal, orgasm, vaginal dryness, and sexual relationship issues are commonplace. Vaginal dryness may be helped by the use of vaginal lubricants such as Astroglide or vaginal moisturizers such as Replens. It is also important to address the everpresent fear of recurrence of the disease or metastasis. Indeed, some women have attributed significant negative changes in their sexual relationship to the participation of a sexual partner in postoperative wound care. When diagnosed and treated early, vulvar cancer has a good prognosis, but unfortunately more than one-third of patients suffer from recurrent disease (American College of Obstetricians and Gynecologists, 2011a, reaffirmed 2014; Trietsch et al. Many patients can return to their primary care clinicians for follow-up after surgical recovery and resolution of any postoperative wound healing complications. Vulvar cancer is thought to have a relatively slow rate of progression, so women who have a good response to therapy and develop no new lesions at 6 and 12 months after treatment may be followed annually (American College of Obstetricians and Gynecologists, 2011a, reaffirmed 2014). A comprehensive history and physical examination are standard components of follow-up care. Every follow-up visit should focus on the history of any new vulvar lesion, bladder function, bowel function, bone pain, and lower-extremity lymphedema. Post treatment, all women should be taught how to perform a monthly self-examination of the vulva. Strict follow-up and rapid detection of suspicious lesions is important to minimize the need for repeated invasive treatments, which can have significant long-term physical and emotional effects (Preti et al. Worldwide, cervical cancer is the second most commonly diagnosed cancer and the third most common cause of death among women who live in low-resource countries (Bermudez et al. Approximately 12,900 new cases of cervical cancer and 4,100 deaths from cervical cancer were estimated to occur in the United States in 2015. Unfortunately, cervical cancer remains a disease of socioeconomic disparity in the United States. A review of the incidence of cervical cancer rates in the United States per 100,000 women from 1999 to 2011 identified the risk percentiles for women of different race and ethnicity as follows: Asian/ Pacific, 5. The risk for women who identify with Asian/ Pacific, American Indian/Alaska Native, or Hispanic ethnicity may well be underestimated due to a lack of a unified approach to understanding and accurately reporting race (U. This disparity in access to care and subsequent treatment is experienced on a global scale, with statistics indicating that 500,000 women in low- and middle-income countries are diagnosed annually with late-stage cervical cancer, making it the second largest cancer killer among women who are poor and belong to a minority group (Bermudez et al. Most women are infected shortly after beginning their first sexual Gynecologic Cancers 663 relationship, with the highest prevalence seen in women younger than 25 years. Types 6 and 11 are responsible for 90% to 100% of genital warts (condylomata acuminata) and low-grade cervical changes such as mild dysplasia. At the same time, these strains are frequently found to be the etiologic factor in minor lesions and mild dysplasia. Integration of the viral genome into the host cell genome is considered a hallmark of malignant transformation. The inactivation of these genes blocks apoptosis (programmed cell death) and induces chromosomal abnormalities (Gearhart et al. Cervical cancer is characterized by a welldefined premalignant phase that can be identified through cytologic examination of exfoliated cells (Pap test) and confirmed on histologic examination. Over time, the premalignant lesions can persist, regress, or progress to invasive malignancy. The premalignant changes almost always occur in the metaplastic epithelium at the squamocolumnar junction. The long natural history of this disease provides an opportunity to screen women for premalignant lesions, thereby preventing the lesions from evolving into cervical cancer. Adenocarcinoma, the second most common cervical cancer type, accounts for 10% to 12% of cervical cancer cases. An increase in the incidence of adenocarcinomas has been observed during the past 20 to 30 years: Among women younger than 35 years, the incidence more than doubled between 1970 and the mid-1980s. The process of squamous metaplasia occurs at the squamo-columnar junction, or transformation zone, where the more fragile columnar epithelial cells are replaced with hardier squamous epithelial cells. Squamous metaplasia is initiated by the eversion of the columnar epithelium onto the ectocervix, which occurs under the influence of estrogen Gynecologic Cancers 665 and its ensuing exposure to the acidic vaginal pH. Although metaplasia may arise throughout the reproductive years, it is most active during adolescence and first pregnancy. The age of greatest risk, however, is midlife, when the majority of cervical cancer diagnoses are made. Cofactors, such as smoking, are thought to play a contributing role in this evolution. Women who smoke cigarettes are twice as likely as nonsmokers to develop cervical cancer. Smoking exposes the body to many carcinogens that affect more than just the lungs, as carcinogens are absorbed by the lungs and carried in the bloodstream, thereby traveling throughout the body. Genetic Predisposition Studies suggest that women whose mother or sisters have had cervical cancer are more likely to develop the disease. Twin studies also suggest a familial susceptibility to cervical cancer is possible. Genetics, however, is estimated to affect less than 1% of cervical cancers (Boardman & Matthews, 2014). As many as 20% of patients who have invasive cervical cancer are asymptomatic when the disease is diagnosed. If symptoms do occur, the most commonly noted are abnormal vaginal bleeding, such as postmenopausal bleeding, irregular menses, heavy menstrual flow, painless heavy menstrual bleeding, or postcoital bleeding. An abnormal vaginal discharge that is odiferous, watery, purulent, or mucoid may also be present. Nutritional Status Diets low in fruits and vegetables have been identified as potential contributing factors in the development of cervical cancer. Such an inflammatory response is associated with the generation of free radicals, which are thought to play important roles in the initiation and progression of cancers. Free radicals directly Gynecologic Cancers 667 Physical Examination the physical examination should include a thorough pelvic, abdominal, inguinal lymph node, and rectal examination. In its earliest stages, a cancerous cervix cannot be distinguished from a normal cervix. As the disease progresses, the cervix may appear abnormal, with gross erosion, ulcers, or a mass that bleeds easily on contact. As the tumor enlarges, it grows by extending upward into the endometrial cavity, downward into the vagina, and laterally to the pelvic wall. Common sites for distant metastasis include the pelvic lymph nodes, liver, lungs, and bones (Boardman & Matthews, 2014). The triad findings of leg edema, pain, and hydronephrosis are indicative of spread to the pelvic wall (Boardman & Matthews, 2014). Diagnostic Testing Recommendations for cervical cancer screening have changed dramatically since 2012. The belief that routine Pap testing for precancerous lesions that has led to a dramatic decline in mortality rate from cervical cancer is now being balanced against data showing that 9 of 10 abnormal Pap tests will revert to normal even without treatment. Preventive Services Task Force (see Chapter 7) and American College of Obstetricians and Gynecologists. These guidelines recommend that screening for cervical cancer start at age 21 years. Screening should start at age 21 years with a routine Pap test and continue at 3-year intervals until the age of 29 years. An acceptable alternative for this age group is to complete a Pap test every 3 years. Women older than 65 years who have never had precancerous changes, who have never been diagnosed with cervical cancer, or who have had removal of the cervix and uterus with no evidence of precancerous or cancerous changes do not require further screening for cervical cancer. The debate over the efficacy of using a conventional versus liquid-based Pap test might be largely resolved in the United States, as automated liquid-based pap cytology has largely replaced conventional Pap smears. Most laboratories in the United States use the Bethesda System for reporting the results of cervical cytology. Satisfactory specimens require at least 5,000 squamous cells for a liquid-based preparation, with a minimum of 10 endocervical or squamous metaplastic cells. Unsatisfactory specimens include those in which more than 75% of the epithelial cells are obscured, which may occur due to inflammation or blood. The Bethesda System includes the general categories of "negative for intraepithelial 668 Chapter 27: Gynecologic Cancers lesion or malignancy," "epithelial cell abnormality," or "other," which may describe an unusual finding such as endometrial cells that might require further investigation. In this system, abnormalities of squamous cells and glandular cells are considered separately (see Table 27-3). This distinction is important because atypical glandular cells have an increased association with high-grade disease. Glandular cells are also specified according to cell type because treatment options may vary based on the type (Solomon et al. Table 27-3 provides a description of the Bethesda System for reporting cervical cytology results (Nayar & Wilbur, 2015). The terminology for histopathology has also changed during the last decade (Nayar & Wilbur, 2015). This term is used when the squamous cells do not appear completely normal but it is not possible to determine the cause of the abnormal cells. In advanced cases, cancer may spread to adjacent organs such as the bladder or rectum, or to distant sites in the body via the bloodstream and lymphatic channels. Testing can be done using a single vaginal or cervical swab (Hollier & Hensley, 2011). Women who have vulvovaginal candidiasis, bacterial vaginosis, or trichomoniasis can present with a variety of symptoms, including vaginal discharge, malodor, irritation, burning or itching, dysuria, and dyspareunia. Accurate Gynecologic Cancers 671 identification of the pathogen requires microscopic examination of vaginal secretions. Women with suspicious lesions on physical examination require referral regardless of the cytology results (Boardman & Mathews, 2014). A curette is inserted into the endocervical canal to remove tissue when the transformation zone is not visible. In this procedure, a cone-shaped tissue extending from the exocervix to the endocervical canal (including the transformation zone) is removed. The new evidencebased guidelines were influenced by the analysis of a large clinical database of 1. The guidelines assist clinicians in referral or management decisions for women who have abnormal cervical intraepithelial neoplasia or adenocarcinoma in situ results. Management Prevention Three human papillomavirus vaccines are now available that provide effective protection against cervical cancer (Table 27-5). The side effects most commonly reported have been pain, swelling and redness at the injection site, and systemic symptoms of headache and fever (McCormack, 2014; Stokley et al. Following administration of 67 million doses of Gardasil, 25,176 adverse event reports were recorded, with 92. There were 96 reports of death and 21 reports of ovarian failure, but none of these outcomes appeared to be causally related to Gardasil (Stokley et al. Nationally and internationally, reports have failed to show any causal association between vaccination and anaphylaxis, autoimmune and neurologic disease, and incidence of complex regional pain syndrome (Markowitz & Shimabukuro, 2015; McCormack, 2014). A post-surveillance general safety assessment of approximately 190,000 females from two large U. If the vaccination series schedule is interrupted, the woman does not need to restart it from the first dose (Markowitz & Shimabukuro, 2015; Petrosky et al.
Intraductal papillomas without atypia that are solitary and less than 1 cm in size are generally not removed rheumatoid arthritis va disability order 60 mg arcoxia with visa, but women who have multiple papillomas or a single papilloma 1 cm or larger are treated with duct excision (Cuneo arthritis pain relief lotion order arcoxia online now, Dash arthritis in feet big toe arcoxia 120 mg buy without prescription, Wilke arthritis zone diet discount arcoxia 60 mg visa, Horton arthritis in neck dizziness buy arcoxia master card, & Koontz, 2012). Mammary duct ectasia can be managed expectantly (because it is associated with a benign process), or it can be surgically treated with removal of the subareolar duct system if imaging shows focal thickening of the duct wall (Ferris-James, Iuanow, Mehta, Shaheen, & Slanetz, 2012) or if symptoms are severe. If breast cancer is diagnosed, appropriate management should be initiated according to the disease stage, as is discussed in the breast cancer section later in this chapter. Fortunately, most breast masses are benign; however, malignancy must always be considered in the evaluation of a breast mass. The likelihood of malignancy increases with age and risk factors for breast cancer, which are detailed in the breast cancer section later in this chapter. Incidence, Etiology, and Clinical Presentation the most common benign breast masses are fibroadenomas and cysts. Lipomas, fat necroses, phyllodes tumors, hamartomas, and galactoceles may also be encountered. Fibroadenomas, which are composed of dense epithelial and fibroblastic tissue, are usually nontender, encapsulated, round, movable, and firm. Their incidence decreases with increasing age, but they still account for 12% of masses in menopausal women (Pearlman & Griffin, 2010). Multiple fibroadenomas occur in 10% to 15% of cases (Vashi, Hooley, Butler, Geisel, & Philpotts, 2013). A proposed etiology for formation of these masses is the effect of estrogen on susceptible tissue (Vashi et al. Cysts are fluid-filled masses that are most commonly found in women aged 35 to 50 years (Berg, Sechtin, Marques, & Zhang, 2010). Although many of these lesions can be dismissed as benign simple cysts requiring intervention only for symptomatic relief, complex cystic and solid masses require biopsy. A lipoma is an area of fatty tissue that may occur in the breast or other areas of the body, including the arms, legs, and abdomen. Lipomas typically occur in the later reproductive years (Grobmeyer, Copeland, Simpson, & Page, 2009). Fat necrosis is usually the result of trauma to the breast, whether as a result of external force against the tissue. These typically large and fast-growing masses account for fewer than 1% of all breast neoplasms. Phyllodes tumors, which can range from a benign mass to a sarcoma, are usually seen in women aged 30 to 50 years (Pearlman & Griffin, 2010). Hamartomas are composed of glandular tissue, fat, and fibrous connective tissue; the average age at presentation for these masses is 45 years (Sevim et al. They result from duct dilation and often have an inflammatory component (Vashi et al. Assessment A woman may present with a breast mass found on self-examination, or a mass may be discovered on clinical breast examination. History If the woman found the mass, determine when she first noticed it and any changes she has observed since that time. Ask about other breast symptoms, such as mastalgia or nipple discharge, and determine whether the woman has a history of any type of breast disease or surgery. Physical Examination Perform a comprehensive breast examination, including inspection and palpation with the woman in both the upright and supine positions, and evaluation of the lymph nodes. If a mass is palpable, identify the size (in centimeters), the shape, and the consistency or texture. Determine whether the mass is discrete (well-delineated, distinct edges) or poorly differentiated, tender to palpation, and mobile or fixed. Ultrasound helps to distinguish a cystic mass from a solid mass, but is not as accurate as tissue sampling. Mammography can be used to detect nonpalpable abnormalities if a woman is of appropriate screening age or has a solid mass. Palpable breast masses may not be visible with diagnostic imaging tests, however, so these tests cannot rule out malignancy. Biopsy is required to definitively ascertain whether a mass is solid versus cystic, and benign versus malignant. If cytologic evaluation does not yield definitive findings, a more invasive method of tissue sampling (Table 15-3) is required to rule out breast cancer or determine the type of tumor if the mass is benign (Kerlikowske, Smith-Bindman, Ljung, & Grady, 2003). Differential Diagnoses In addition to the types of breast masses already discussed, differential diagnoses for breast masses include fibrocystic changes, infection or abscess, and malignancy. Women with fibrocystic breast tissue may present with a perceived mass, although these changes are typically associated with nodularity or thickening rather than formation of a discrete mass. These cysts seem to be more prevalent in cigarette smokers and can be intermittently chronic. A fibroadenoma that has been definitively diagnosed by cytologic or histologic analysis does not need to be removed. Instead, it can be expectantly managed and removed only if the mass becomes enlarged, such as doubling in size or becoming 4 cm or larger (Hubbard, Cagle, Davis, Kaups, & Kodama, 2015). Fibroadenomas usually decrease in size postmenopausally, and many resolve completely (Hubbard et al. Management of cysts is based on symptoms, with these sac-like structures sometimes requiring incision and drainage. Complicated cysts will need biopsy of the debris to rule out atypia or malignancy. Excision of a lipoma is not required if a breast mass is consistent with lipoma on clinical Breast Conditions 367 examination and tissue sampling, and there are no suspicious findings at the site on mammography and ultrasound. Excisional biopsy is recommended for suspected phyllodes tumor, and typically a wide margin of normal surrounding tissue is also removed due to the tendency for such masses to recur (Pearlman & Griffin, 2010). Hamartomas may require excision for diagnosis, but otherwise do not have to be removed and may be expectantly managed. Aspiration of a galactocele allows for diagnosis and appropriate treatment (Vashi et al. When benign breast masses are managed expectantly, the woman should be advised to report any new symptoms and encouraged to follow up with her clinician for examinations and diagnostic testing as recommended. From the Halsted radical mastectomy of the 1890s to breast-sparing surgery in conjunction with other treatment modalities, the management of breast cancer has changed dramatically over time. With increased public awareness and earlier detection, comprehensive treatment can be initiated promptly for this disease process. The risk increases gradually with age, from 1 in 227 for women ages 30 to 39 to 1 in 28 for women ages 60 to 69 (National Cancer Institute, 2012). Breast cancer is the second leading cause of cancer deaths in women, after lung cancer (Centers for Disease Control and Prevention, 2014). Special Considerations Adolescents In approximately two-thirds of adolescents presenting with a breast mass, the diagnosis is a fibroadenoma. Mammography is not indicated, and aspiration for diagnostic purposes can be avoided (Giess et al. Breast cancer in women younger than age 20 is very rare (American Cancer Society, 2015). Etiology Two aspects of breast cancer are especially challenging: Many of the risk factors are nonmodifiable, and most women with breast cancer (85%) have no identifiable risk factors other than age (Fritz & Speroff, 2011). In fact, fewer than 10% of women with breast cancer have an identified germline mutation that puts them at known risk for this disease (Petrucelli, Daly, & Feldman, 2013). In normal cells, these genes help prevent cancer by making proteins that keep the cells from growing abnormally. If a woman inherits a mutated copy of either gene from a parent, she has Pregnant or Breastfeeding Women Evaluation of palpable findings in pregnant and lactating women is complicated by the complex breast parenchyma. Nevertheless, appropriate diagnostic imaging and breast tissue sampling should not be deferred, with the exception of mammography- this modality is not generally used during pregnancy because physiologic changes in the breast result in poor sensitivity for such imaging (Vashi et al. Fibroadenomas may increase in size and become symptomatic during pregnancy (Amin et al. Masses in postmenopausal women are presumed to be malignant until proven otherwise (Vaidya & Joseph, 2014). These mutations are also associated with an increased risk of developing ovarian cancer. Given the growing knowledge base about genetic influences on the development of breast cancer, the genetic counselor has a significant role working in collaboration with the healthcare team in the care of women with breast cancer (Moyer & U. Other potential risk factors for breast cancer include cigarette smoking and shift work, particularly at night (American Cancer Society, 2015). Studies have yielded conflicting results about other putative risk factors, such as diet, vitamin intake, and chemicals in the environment (American Cancer Society, 2015), and research in this area is ongoing. Conversely, breastfeeding is a protective factor against developing breast cancer. This effect increases with longer duration of lactation, especially at least 1 year (Collaborative Group on Hormonal Factors in Breast Cancer, 2002). Moderate or vigorous physical activity for at least 4 hours per week is also associated with reduced breast cancer risk, with the average relative risk reduction being 30% to 40% (National Cancer Institute, 2015a). Maintaining a normal weight protects against breast cancer as well (American Cancer Society, 2015). Breast Conditions 369 Pathophysiology Breast cancer develops when erratic cell growth and proliferation occur in the breast tissue. Which hormones are most critical in the development of breast cancer and why a large percentage of women who develop breast cancer have no identified risk factors remain unclear (National Cancer Institute, 2015a). While the discovery of pertinent genetic factors has clarified the predisposition toward developing breast cancer in some women, a significant amount of ongoing research is dedicated to further elucidating the development of this disease. Invasive Breast Cancer Invasive or infiltrating ductal carcinoma is the most common malignancy of the breast. Invasive ductal carcinoma usually presents as a discrete, solid mass, with malignant cells escaping the confines of the ducts and infiltrating the breast parenchyma. The most common sites of metastatic spread of such cancer are the lymph nodes, bones, liver, and lungs (Price, 2009). Invasive or infiltrating lobular carcinoma is less common and may also present as a discrete mass. The mass may be characterized only by thickening or induration, with margins that are diffuse and ill defined, both on physical examination and on mammogram. Invasive lobular carcinoma is more frequently characterized by bilateral involvement than other types of breast cancer; it is associated with unusual spread of metastases, including carcinomatous meningitis, intra-abdominal metastases with intestinal and ureteral obstruction, and metastases to the uterus and ovaries (Dillon, Guidi, & Schnitt, 2010). Clinical Presentation and Types of Breast Cancer Breast cancer may be detected by identification of a palpable lesion or by screening mammography. It is important to note that pain (or lack thereof) does not indicate the presence or the absence of breast cancer (American Cancer Society, 2015); nevertheless, pain is not usually a sign of breast cancer (Vaidya & Joseph, 2014). Breast cancer is further classified based on whether it originated in the ducts or lobules. This condition is usually diagnosed in association with microcalcifications seen on mammography; it is rare to find a palpable mass in such cases. Controversy exists regarding whether the nipple involvement arises from infiltration from an underlying breast tumor or is a separate process involving the nipple epidermis. Assessment History the initial history for a woman with a breast mass is the same as that described in the earlier section on benign breast masses. Breast Conditions 371 about symptoms of metastases such as bone pain, arthralgias, cough, jaundice, abdominal pain, headaches, visual disturbances, malaise, loss of appetite, weight loss, fever, and fatigue. Clinicians should remain vigilant for symptoms of metastasis in any woman with a history of breast cancer. Physical Examination the clinician should perform a comprehensive breast examination when breast cancer is suspected. A suspicious lesion is usually hard, is painless, and has irregular borders that may be immobile and fixed to the skin or surrounding breast tissue. Palpate for the axillary, cervical, and supraclavicular lymph nodes-enlargement of any of these nodes is suspicious. Examination of the lungs, abdomen, and neurologic system should also be performed to detect signs of metastasis. Further Assessment When Breast Cancer Is Diagnosed Several factors guide appropriate treatment options and serve as prognostic indicators when breast cancer is diagnosed. A well-differentiated tumor has a more favorable prognosis than a poorly differentiated lesion (Chang & Hilsenbeck, 2010; Yamamoto et al. The status of the axillary lymph nodes is critical in determining treatment options for women with invasive breast cancer. For women who have early-stage tumors less than 5 cm in size and no palpable axillary lymph nodes, sentinel node Diagnostic Testing Diagnostic testing for breast cancer includes both imaging studies and tissue sampling. Mammography can identify breast cancers that are too small to palpate on physical examination, and can detect both benign and malignant calcifications. Benign calcifications are typically characterized by their large, coarse, and scattered appearance. With digital mammography as well as tomosynthesis, a wider range of tissue contrast can be seen; subtle contrast differences can be amplified with these technologies, and the images are immediately available. Mammography can also identify masses that ultrasound can then further characterize as solid or fluid filled. Solid masses require further intervention or follow-up, whereas simple fluid-filled cysts generally do not. With this technique, dye is injected into the region surrounding the tumor to identify the first node draining the breast. This node, which is termed the sentinel axillary node, is then removed (Cowher et al. Additional tests are performed if there is evidence of advanced cancer (stage 3 or 4) to detect metastases. These tests routinely include a complete blood count, liver function tests, and a chest radiograph.
Order arcoxia 120 mg otc. How to know if my dog has arthritis and what to do.
References
- Mueller EW, Bouchard BA. The use of extended-interval aminoglycoside dosing strategies for the treatment of moderate-to-severe infections encountered in critically ill surgical patients. Surg Infect (Larchmt). 2009;10:563-570.
- Hakki M, Riddell SR, Storek J, et al. Immune reconstitution to cytomegalovirus after allogeneic hematopoietic stem cell transplantation: impact of host factors, drug therapy, and subclinical reactivation. Blood. 2003:102(8):3060-3067.
- Denes FT, Tavares A, Cocuzza M, et al: Gonadal function and reproductive system anatomy in post puberal prune belly syndrome patients, J Urol 197:e863, 2017.
- Bourin M, Chenu F, Ripoll N, David DJ. A proposal of decision tree to screen putative antidepressants using forced swim and tail suspension tests. Behav Brain Res. 2005;164:266-269.
