
Betapace
| Contato
Página Inicial
Michael G. Ison, M.D., M.S.
- Assistant Professor
- Divisions of Infectious Diseases & Organ Transplantation
- Northwestern University Feinberg School of Medicine
- Medical Director
- Transplant & Immunocompromised Host
- Infectious Diseases Service
- Northwestern Memorial Hospital
- Chicago, Illinois
Just as cis-gender persons can be heterosexual blood pressure 44 betapace 40 mg order overnight delivery, homosexual blood pressure medication diuretic buy betapace 40 mg amex, or bisexual arteria umbilical unica pdf buy betapace australia, the same is true for transgender individuals arteria yugular funcion betapace 40 mg purchase fast delivery. Transgender females on estrogen may still produce sperm and may have the ability to impregnate partners blood pressure medication algorithm buy cheap betapace line. As such, they should be counseled on barrier methods for themselves and contraception for their partners. In addition, transgender men on testosterone who retain reproductive organs also remain at risk for pregnancy. Cervical cancer screening should follow current guidelines for patients who retain a cervix. Pap smears have an increased likelihood of insufficient tissue in transgender men, which is likely related to testosterone use. The patient should be counseled on the indications and reassured as to their control over the exam. Ovarian tissue and testicular tissue cryopreservation are experimental options that are currently being investigated under research protocols. Transgender females who use estrogen may have impairment of spermatogenesis and an absence of Leydig cells in the testis. Testosterone use may result in ovarian stromal hyperplasia and follicular atresia. Although some of the effects of gender-affirming hormone therapy appear partially reversible, the threshold for which fertility is impaired is unknown, and duration of use will likely be an important factor. However, adolescents may not feel qualified to make decisions on fertility or may not be able to consider the true impact. Although early discussion is desirable, it is not always possible to proceed with fertility preservation prior to initiating hormonal management. For transgender females, the act of sperm extraction or masturbation may also be distressing. Finally, the cost associated with available fertility preservation options may be prohibitive. This includes inquiring about gender identity or variance as part of routine clinical care. Statement on gender affirmative approach to care from the Pediatric Endocrine Society Special Interest Group on Transgender Health. Endocrine treatment of gender dysphoric/incongruent persons: An Endocrine Society clinical practice guideline. Supporting and caring for transgender and gender nonconforming youth in the urology practice. Injustice at Every Turn: A Report of the National Transgender Discrimination Survey. Estimating population size and demographic characteristics of lesbian, gay, bisexual and transgender youth in middle school. Standards of care for the health of transsexual, transgender and nonconforming people, version 7. Proceedings of the Working Group Session on Fertility Preservation for Individuals with Gender and Sex Diversity. Young adult psychological outcome after puberty suppression and gender reassignment. Combined hysterectomy and mastectomy surgery for transgender patients in an integrated health care setting. Transgender men who experienced pregnancy after female-to-male gender transitioning. Contraceptive use and pregnancy intentions among transgender men presenting to a clinic for sex workers and their families in San Francisco. Menstrual Manipulation for Adolescents with Physical and Developmental Disabilities. The response of the menstrual cycle to initiaton of hormonal therapy in transgender men. Femaleto-male patients have high prevalence of unsatisfactory paps compared to non-transgender females: Implications for cervical cancer screening. Transgender youth fertility attitudes questionnaire: Measure development in nonautistic and autistic transgender youth and their parents. Care providers have the unique opportunity to assist the teens and their families through this change. This article focuses on reproductive health in teenagers with special needs and addresses menstrual and hygiene issues, as well as specific concerns about sexual education, contraception, mood disorders, seizures, and abuse. The principle of any intervention is to provide the optimal and least harmful form of care and be evidence based where possible. Although it is challenging to try to teach all of these concepts in the setting of a brief office visit, it is suggested that providers attempt to assess the current knowledge base of each patient, then help the family and caregivers with information to continue educational efforts in the home setting, in conjunction with community-based resources. Sex education, including gender roles, social boundaries, and healthy sexual behaviors 3. These girls may have cognitive impairment and speech delays that would predictably make it hard for them to understand or communicate about the changes that occur with puberty and the menstrual cycle. Recommended content for education regarding puberty and menstrual hygiene is in Table 24. Using basic language when asking the initial questions will help to assess how much the patient understands. Whether the patient should be offered a confidential part of the interview, as is customary in adolescent encounters, is dependent on the degree of intellectual disability. Ask about home and school situations, and inquire about issues with menstrual hygiene, behaviors, mood changes, concerns about sexual activity, potential for coercion, abuse, or depression (common in all teens, around 11%). However, if the patient is adopted or lives in a group home, this information may be unknown. Menstrual and behavioral calendars can be very helpful to get written information on menstrual cycles and accompanying symptoms and behaviors. This makes it easier to establish a diagnosis and to aid in judging treatment efficacy. Common reasons for a reproductive health visit include anticipatory pubertal guidance, education, menstrual problems, including pain management, hygiene and menstrual control, cyclical behavioral concerns, or an evaluation for possible abuse or pregnancy. Basic anatomy and reproductive function General hygiene, mood changes, sexual feelings Explain menstrual flow Review hygiene-washing, changing pads, changing clothes and underwear 5. Family member models hygiene techniques level, sex education should include an explanation of the differences between boys and girls and the proper labeling of body parts. Emphasis is placed on the concept of "public and private" to reinforce acceptable patterns of conduct. We distinguish between public and private body parts, as well as public and private places. If the teen has a lot of selfstimulation in public places, it can be taught that in private places that same behavior can be acceptable. Explain about good touch in contrast to bad or inappropriate touch, and in this context, introduce the issues of personal space and boundaries. Try to outline very specifically appropriate behaviors and appropriate responses to interactions with other people. It can be difficult to assess the ability of the patient to consent to sexual activity. Discuss with caregivers and patient, alone if possible, if there are any active issues related to sexual activity or consent. One basic strategy used to teach impaired individuals appropriate social boundaries is the "circles technique" described by Champagne and Walker-Hirsch. Family is in the closest circle and strangers the farthest away, helping them understand social boundaries, distance, and touch. These boundaries may seem somewhat obvious to usually developing children but must be specifically reinforced for children and teens with cognitive impairment. Sexual abuse Unfortunately, many characteristics associated with developmental disability predispose individuals to sexual abuse: physical challenges, reliance on adults or caregivers for assistance with many activities of daily living, learned compliance, affectionate or loving nature, and decreased communication skills. Estimates of sexual abuse range from 25% to nearly 83% in national statistics, but clearly rates of sexual assault are higher among persons with disabilities. A few studies demonstrate that women with mild to moderate mental delay can acquire skills for sexual abuse prevention. One study of sexually abused women with intellectual disability found that greater than 50% had not received any sexual education. Simple accurate anatomy Appropriate social boundaries Public and private body parts and behaviors Sexual identity-gender roles and socialization Sexual activities-intercourse, masturbation, and alternative sensual activities 6. Healthy relationships, abuse, and protective measures from exploitation model described by Krents and Adkins. Teaching this concept requires repetition, modeling, and generalization to use the technique in a variety of settings. Clinicians should recognize that children with disabilities are at increased risk of sexual abuse and should advocate for appropriate sex education. In addition, we need to be vigilant in looking for physical signs, like unexplained bruising and symptoms or changes in behavior that may be indications of sexual abuse in those patients who may not be able to communicate details of their abuse. Fortunately, these examinations are only indicated for specific circumstances, like vaginal discharge, vulvar pain, or concern about trauma. Increased rates of sexual assault and difficulty obtaining an accurate sexual history make continued cervical screening recommended in the adult population. If a vulvar/pelvic examination is necessary, there are some specific aspects to address (Table 24. Positioning the legs for an internal exam may require extra assistance, due to physical handicaps. Use a Huffman speculum (narrow, but long) as opposed to a pediatric speculum, which is narrow, but often too short to visualize the cervix of a postmenarchal girl. Bimanual exam, if indicated, with one finger in the vagina, can be difficult due to cooperation of the client, body position like scoliosis, and very tight rectus muscles. Sedation for exams has been used in some clinic settings, but if a thorough evaluation is strongly indicated to rule out suspected pathology, an ultrasound or an exam under anesthesia is much more helpful and less traumatizing. The most recent recommendations are two injections 612 months apart in children 914 years old; after the 15th birthday, a total of three injections is currently recommended. Bleeding irregularities are common in all teens, with 85% of all cycles anovulatory during the first year after menarche. Women with epilepsy have an increased incidence of reproductive endocrine disorders, including irregular menstrual cycles, anovulatory cycles, amenorrhea, and oligomenorrhea. Thyroid disease, which can lead to subsequent disturbance of the cycle, is more prevalent in women with Down syndrome. Bleeding is only considered medically unhealthy if it leads to anemia or if it is very sparse. For heavy bleeding, leading to anemia, consider anovulation, poor food intake (leading to iron deficiency), or bleeding Table 24. Usually wear a white coat to clearly establish the professional nature of the caregiver. Allow the patient as much control over the exam as possible by having her touch the instruments and assist, if possible. Adjust the positions: Frog-leg position V-position Elevate legs without abduction of the hips Side position. Very sparse cycles, due to anovulation, can lead to endometrial concerns long term. Does the bleeding negatively affect the patient and her daily activities or her family and caregivers The families of children with disabilities can have a very delicate balance of caring for their girls, and menstrual cycles may disturb that. The issues may include menstrual hygiene, like accidents with bleeding due to removal of pads out of the underwear by the teens or getting menstrual blood on their hands. If there is a concern for abuse, either within the surroundings or because the patient cannot be monitored closely enough or is unable to understand appropriate boundaries, the care provider should assist with evaluation of a potentially unsafe situation and also address contraception needs. This can be to decrease heaviness of flow, relieve pain or symptoms, provide contraception, or achieve amenorrhea. A method causing unpredictable bleeding may be less desirable than infrequent but predictable withdrawal bleeding. There may be some troublesome spotting that can be addressed by taking two pills for several days or allowing periodic withdrawal bleeds. Higher doses of oral norethindrone, medroxyprogesterone acetate, and megestrol have been used with complete suppression of the cycles. Side effects of these medications include mild weight gain and mood changes, with megestrol increasing appetite as well. Although the studies have mixed results, there appears to be some weight gain noted with Depo-Provera, especially in overweight girls, but with large individual variations. If a teenager gains significantly in the first year of use, the method of menstrual suppression may need to be revised. Although the issue of wheelchair use and bone density has not been researched extensively, decreased bone density has been found in several small subpopulations. Surgery, like hysterectomy or endometrial ablation, for cessation of normal menses is usually not recommended. Long-acting reversible methods are preferred with the caveats outlined in the previous section. Discuss emergency contraception with adolescents, as they may have an unplanned sexual encounter.
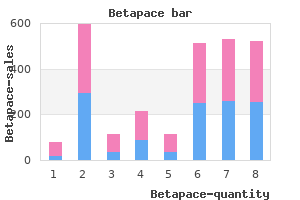
Timing of surgery is controversial and can be performed during the newborn period or after the patient undergoes puberty when the hymen is well estrogenized blood pressure levels of athletes buy 40 mg betapace with visa, thus avoiding stricture arrhythmia medscape 40 mg betapace for sale. The hymenal tissue is then resected with careful attention being paid to avoid the vaginal wall blood pressure medication when pregnant cheap betapace 40 mg buy online, as this could cause more bleeding or pain hypertension with diabetes buy betapace with a mastercard. The risk of stenosis is very low blood pressure and age buy generic betapace 40 mg on line, and postoperative vaginal dilation is not routinely recommended. Class U0: Normal uterus U1: Dysmorphic uterus U2: Septate uterus U3: Bicorporeal uterus U4: Hemi-uterus U5: Aplastic uterus C0 C1 C2 C3 C4 V0 V1 V2 V3 V4 Anatomic findings Normal uterine cavity a. Without rudimentary cavity Normal cervix Septate cervix Double normal cervix Unilateral cervical aplasia Cervical aplasia Normal vagina Longitudinal nonobstructing vaginal septum Longitudinal obstructing vaginal septum Transverse vaginal septum and/or imperforate hymen Vaginal aplasia Table 6. Transverse vaginal septum the upper vagina is derived entirely from the Müllerian ducts, and incomplete canalization or abnormality of the vaginal plate may result in a septum. Perforate septums allow for menstrual outflow, and patients may only present with difficulty inserting a tampon or with intercourse, as well as during routine obstetric or gynecologic examination. The location is determined by measuring the distance between the vaginal introitus and the distal end of the septum and is classified as low (<3 cm), mid (36 cm), or high (>6 cm). Mid to high or thick septums are associated with more complex surgeries and may require a combined abdominal and vaginal approach. These surgeries are associated with a high rate of reobstruction requiring repeat surgery, and in extreme cases, hysterectomy. Often, preoperative dilation is utilized to increase the length of the distal vagina and thin the septum. The anterior and posterior leaflets are then cut circumferentially, flush with the vaginal wall. For thick septums where the need for an interposition graft or injury to bowel or bladder is high, a team approach with urology, plastic surgery, and/ or colorectal surgery may be warranted. One review suggested a mid to high septum was directly correlated with infertility, possibly due to increased risk of prolonged (a) Vaginal mucosal flap of outer portion of vagina obstruction and damage caused by hematosalpinx or endometriosis. The distal septal mucosa is incised with an "X" to create four triangular leaflets (ad). The proximal mucosa is then incised with a "+" to create four additional distinct leaflets (14). The introitus is dissected below the urethra, and the areolar space between the urethra and rectum is bluntly dissected until the bulging vagina is encountered. The vagina is then grasped, dissected from the surrounding tissues, and "pulled through" to the introitus. It is important to ascertain the distance from the hematocolpos to the introitus, as a distance of greater than 3 cm is associated with greater stricture rate. Distal mucosa at the vaginal dimple is noted and incised horizontally with a scalpel. Thick connective tissue is then dissected both sharply and bluntly to the level of the proximal mucosa. This anomaly is rare with true incidence unknown but estimated to be 1:80,000, and the classical treatment has been by total hysterectomy27; while this does definitely relieve symptoms of obstruction, it renders the patient irreversibly infertile. The procedure is accomplished by laparotomy, dissection of the anterior space, followed by modified vaginal pull-through, and finally, catheterization of the uterine cavity and attachment of the neovagina to the uterine body. This procedure, however, is associated with significant morbidity, including stenosis and severe infection. To date, four pregnancies have been reported, and all have delivered preterm via cesarean section. If there is vaginal agenesis associated with cervical agenesis, the vagina can be lengthened preoperatively through dilation. Vaginal reconstruction can also be performed with skin, buccal, or bowel graft, as in the case of thick transverse septum or agenesis. This anomaly is thought to be a result of abnormal development of the caudal portion of the Wolffian duct, resulting in ipsilateral renal agenesis. If a communication is observed, a Foley catheter may be inserted into the obstructed hemivagina and used as a guide for resection. When the anatomy is not clear, a spinal needle can be inserted under ultrasound guidance to identify the correct hemivaginal space Patients with obstructive anomalies with menses generally present with dysmenorrhea or worsening pelvic pain following menarche. Although they may be seen in the office, many patients will present with severe pain and an acute abdomen in the emergency department. Due to the presence of menses, diagnosis is often delayed by 35 months; however, cases of delay of up to 20 years have been described. These cases often present later as pain is periodically relieved, and are accompanied by a history of irregular menses, chronic brown and malodorous vaginal discharge, or with pyocolpos or pyometra. When the horn is not communicating, it may become distended with menstrual products, causing severe abdominal pain. While a noncommunicating horn generally presents early due to abdominal pain, a communicating horn may take several years to diagnose. Obstructed vagina can be drained with a spinal needle to allow for clear visualization of the anatomy. A horizontal incision is then made along the obstructed vaginal sidewall, and septum excision is carried out circumferentially (dotted line). Two cervixes are clearly noted and right hemivagina obstruction completely resolved. Some experts endorse placing a vaginal mold or stent postoperatively; however, this is not universally practiced. Long-term prognosis Complete resolution of pain symptoms, endometriosis, and obstruction can be expected after vaginal septum excision. Pregnancy rates are fair, and infertility has been noted in 5%15% of these patients, consistent with the general population. Delivery method has been largely based on provider preference, but overall, half of deliveries are accomplished vaginally and half by cesarean section. Histologically, the obstructed vaginal mucosa approaches mature squamous epithelium; however, it continues to remain abnormal even after several years. In the literature, cases of severe infection and sepsis have been documented, disastrously resulting in hemi- or total hysterectomy. About 13% of patients will require surgery for urinary obstruction to alleviate renal impact. Patients who present with nonobstructive longitudinal vaginal septums often have presenting symptoms that may be complaints of difficulty placing a tampon or pain with intercourse; however, some may present during the course of a routine pelvic exam. It is important when there is a complete duplication that Pap smears of both cervixes be collected. When the septum is associated with discomfort, these can be resected in the operating room with Bovie cautery or the LigaSure device. Once the septum is resected, the mucosa can be approximated with absorbable suture. Diagnosis is usually made by hysteroscopy or hysterosalpingogram in the adult patient, often due to infertility. A uterine septum may cause implantation failure or recurrent miscarriage, and in these cases, septoplasty by operative hysteroscopy is indicated. Rarely, a Thompkins or Jones metroplasty may be indicated for complex intrauterine anomalies; however, these are difficult surgeries to perform and are associated with increased risk of uterine rupture. The most common form is olated absence of the vagina and uterus, Type 1, or the typical form. Anomaly Any other anomaly No associated anomaly Uterine · Rudimentary · Hypoplastic with endometrium · Absent · Other Renal · Unilateral agenesis · Pelvic kidney · Horseshoe kidney · Duplicated system Skeletal · Scoliosis · Hip dysplasia · Caudal fusion of vertebrae · Klippel-Feil syndrome Cardiac Inguinal hernia Prevalence (%) 44. Mayer described the first patient in 1829, and the syndrome was later defined more precisely by von Rokitansky, Küster, and Hauser from 1910 to 1961. The differential diagnosis includes low Source: Adapted from data in Oppelt P et al. Skeletal anomalies are also found up to 20% of the time, so complete spinal x-ray can also be considered. These women are abruptly confronted with perceived loss of sexual function, as well as infertility, and each person becomes ready to discuss or pursue treatment at different times. It has been our practice to see patients multiple times over the course of 3 months from diagnosis in order to offer support and answer questions as patients are ready. Several case reviews have also shown that women have more successful outcomes in terms of vaginal creation and satisfying sexual function when they have regular access to physicians, nurses, psychosexual support, and physical therapy by trained professionals. Difficulties with continued sexual function are also higher among the surgery group, with almost half of these women indicating pain and inability to produce adequate lubrication. Complications after these surgeries are high, and include vaginal and introital stenosis, disfiguring scar formation, fistula, chronic pain, vaginal prolapse, and copious, malodorous discharge. In comparison, passive perineal dilation has been shown to be highly effective in creating a normal vaginal length, resulting in good sexual function, with very few complications (Table 6. Primary perineal dilation Primary or progressive vaginal dilation was first described by Frank in 1938. Patients and providers found this method to be difficult, because it was time consuming, required a private space and dedicated time, and could lead to muscle fatigue. In 1981, Ingram proposed an alternative form of dilation, involving progressive dilators on a bicycle seat. Since then, it has been concluded that dilation should occur when a patient is mentally and emotionally ready, in a fashion that she is comfortable with and has support for during its course. Often, surgery is not necessary, as the remnants are composed mainly of fibrous tissue. However, if active endometrium is noted, there is a high likelihood of menstrual obstruction and pain. In these cases, menstrual suppression should be offered, as well as removal of these dysplastic horns. Advantages · · · · · · · · Lower complication rate Good long-term functionality Noninvasive Epithelium histologically converts to vaginal tissue 96% functional success Vaginal approach to surgery Lower rate of prolapse 89. Food and Drug Administration · Associated with pain and need for long inpatient admission · Major abdominal surgery · Copious foul-smelling mucous discharge · · · · · · · · · · · · · · · · · 14% overall rate Injury to bladder or rectum Fistula Vaginal stenosis (9. It is important to note that many women achieve adequate vaginal length through dilation with attempted intercourse. It was also a long-held belief that successful dilation depended on a longer starting length of the vaginal pouch, of at least 23 cm. Surgical neovagina creation As previously discussed, rates of complications are higher with surgical management, and most procedures require postoperative dilation. Thus, most experts in the field agree that nonsurgical vaginal dilation should be first-line treatment for neovaginal creation. It is important to note that although many procedures have been performed, none has been noted to have superior outcomes, and each has unique risks and benefits (Table 6. McIndoe first described this procedure in 1938 as a noninvasive surgical approach to correction of vaginal agenesis. This stent is placed within the vaginal space, and the external tissue edge is sutured to the incision at the introitus. Patients have traditionally been maintained in-house on bedrest with a suprapubic tube, constipating agents, and venous thromboembolism prophylaxis to avoid disturbance of the graft. After 7 days, the stent was removed, and the patient was instructed to place a dilator at least two to three times per week. Given the smaller surface area that can be removed, multiple small slits are placed in the tissue in order to expand it over the mold. The space is created as previously described, and a mold is kept in place for 3 months until the vagina is fully covered with epithelium. Active perineal dilation: Vecchietti procedure the Vecchietti procedure was first described in 1965 as another noninvasive method of vaginal creation. This procedure entails the placement of an "olive" at the perineum, which is attached to sutures. Though originally described as an open approach, now currently laparoscopic, these sutures are advanced laterally anteriorly behind the peritoneum and finally through the abdominal wall. These sutures are then attached to a metal device that allows increasing tension in order to actively dilate the vagina. Autologous/membranous graft: Davydov procedure the Davydov or peritoneal advancement procedure was first described in 1933. The vaginal space is created as described in the McIndoe until the vaginal peritoneum is encountered, grasped, and pulled through to the introitus. Laparoscopically, the peritoneum is sutured closed with a purse-string suture with or without release of the peritoneum laterally (Video 6. Essentially, this procedure creates a pouch by incising the labia majora and perineal epithelium in a U-shape. Bowel vaginoplasty Bowel vaginoplasty was first described as early as 1892 by Sneguireff and made popular in the United States by Beck and Baldwin in the early 1900s. Though bowel vaginas can develop introital stenosis or complete stenosis if the blood supply is injured, these usually do not require immediate postoperative dilation. These can also be associated with neovaginal polyps, adenomas, and cancer and should be monitored with inspection. Finally, the posterior skin margins of the lower portion of the "U" are approximated at the midline in a similar manner, forming the external skin of the new pouch. Uterine transplant is still considered highly experimental and can only be obtained at hospitals enrolled in a clinical trial. These patients have high rates of concomitant Müllerian anomalies and require close follow-up with an adolescent gynecologist as they enter puberty. Since ovarian function is normal, patients can expect to undergo puberty as expected. No No No No Yes Yes Yes Yes Yes Yes No No No No No Yes No No No No Yes No Other malformations Testa Houston Menstruating Thrombosis/hysterectomy Menstruating Menstruating Menstruating Menstruating Infection/hysterectormy postoperative day 12 Hysterectomy postoperative day 14 Hysterectomy postoperative day 12 Hysterectomy postoperative day 6 Menstruating Menstruating Source: Compiled from data in Brännström M et al. Physical exam should be performed when the patient is ready after puberty to evaluate for scar tissue, introital stenosis, and adequacy of the vagina for sexual intercourse. Preconception evaluation is recommended to assess for uterine anomalies and provide appropriate counseling. Due to the complexity of surgical repair, women with a history of cloacal anomaly should deliver via cesarean section to avoid disruption of the vascular supply to repairs.
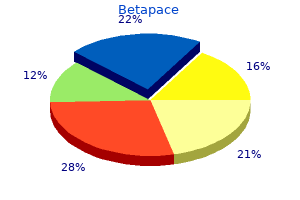
This degree of patience may relieve stress associated with the much anticipated visit and may go a long way to help establish a positive and interactive relationship hypertension in children order betapace 40 mg line. Imaging modalities such as ultrasound are useful for evaluating pelvic anatomy hypertension first aid purchase betapace 40 mg line, and in the setting of endometriosis high blood pressure medication valsartan buy betapace discount, may diagnose ovarian involvement (see Table 18 hypertension drug betapace 40 mg with amex. If she is unable to tolerate a vaginal probe blood pressure medication grapefruit juice order discount betapace line, excellent imaging can often be obtained with an abdominal probe with a full bladder. However, the absence of pelvic disease on ultrasound does not rule out the potential for peritoneal disease. Magnetic resonance imaging may be useful for detecting infiltrating lesions and can help guide the clinician for surgical intervention but is not absolutely necessary. If the suspicion for endometriosis is high, and surgery is indicated, it can be offered at any point in the evaluation. Endometriosis 221 Surgical characteristics Direct visualization of implants at time of surgery and histopathology do not always correlate, since atypical lesions may be difficult to assess without biopsy, and there is no standardized method used by all pathologists. These are often clear to colored, vesicular lesions superficially embedded on the peritoneal surface. These lesions are active prostaglandin producers, an attribute that substantiates the high rate of dysmenorrhea. Comparison of adolescent versus adult Adolescent Adult Secondary dysmenorrhea, moderate to severe, often accompanied by noncyclic chronic pelvic pain Black peritoneal Surgical Red, clear and/or implants, whitefindings vesicular appearing or nodular peritoneal implants; minimal fibrosis, dense adhesions that may fibrosis; smaller include rectosigmoid and less colon; ovarian adhesiogenic endometrioma more ovarian common with dense endometrioma adhesions to ovarian cortex Uncommon Variable, but more Deeply finding common; may be infiltrating difficult to identify if endometriosis inexperienced Rectovaginal or Other features Association with bladder lesions; outflow adenomyosis obstruction of reproductive tract Presenting symptoms Primary dysmenorrhea, severe, refractory to first-line medical therapy Source: See further Benagiano G et al. Treatment options Only after a comprehensive assessment that facilitates exclusion of other organic or functional causes of pain should the clinician provide endometriosis-targeted therapies. If empiric therapy is offered wantonly, therapy is more apt to fail, resulting in frustration and the possibility of distrust on behalf of the patient. Whether the early diagnosis and treatment of adolescents with endometriosis prevent disease progression or merely increase the number of interventions without affecting long-term outcomes is debatable. No one therapy has been proven substantially superior to the other, and most experts would agree that if pain is the main complaint, then reducing it to an acceptable level should be the goal. Even if treatment is deemed successful, many patients are not cured of their pain, and many will experience recurrent symptoms. Needless to say, the best management involves early evaluation and prompt intervention. Most treatment paradigms used in adolescents have been based on research focusing on adults, with a smaller percentage of the literature centering on this group. Although medical management is frequently used as first-line therapy, surgical intervention can be offered at any point in the evaluation or if advanced disease is clinically suspected. Various experts in the field differ in opinion with regard to the timing of surgical intervention, with opponents offering that one surgery at a young age may lead to several others by the time the patient has reached adulthood. Proponents feel that long-term medical therapy, which is often necessary to suppress symptoms, should not be considered until a surgical diagnosis is confirmed. Most nonsurgical remedies are composed of hormonal agents that suppress endometriotic growth, either directly or indirectly. If given continuously, patients may become amenorrheic and will experience less cyclic pain. Progestin-based medical treatments can also significantly reduce pain symptoms if used continuously. Since progestins inhibit estrogen and progesterone receptor synthesis, patients experience long periods of low estrogen production at a time when bone mineralization is high. Dienogest is an oral progestin now used as a monotherapy at a dose of 2 mg daily in patients with endometriosis. This medication is highly selective for the progesterone receptor, leading to strong progestational effects, moderate antigonadotrophic effects, and minimal androgenic, glucocorticoid, or mineralocorticoid effects. This prospective observational study evaluated the safety and efficacy of dienogest 2 mg daily in adolescents aged 1218 with clinically suspected or laparoscopically confirmed endometriosis. Results demonstrated that endometriosis-associated pain was substantially reduced and that the drug was very well tolerated during the 52-week trial. However, there was an associated decrease in lumbar bone mineral density with only a partial recovery after 6 months of treatment discontinuation. One must balance the benefits of decreased pain with the potential risks to bone health in each patient, and provide counseling in this regard. Patients should also be informed that dienogest has not been tested or approved as a contraceptive, so the concomitant use of barrier contraception is necessary in sexually active teenagers. Partial suppression can be achieved with a dose of 150 mg daily (for up to 24 months) and full suppression with a higher regimen of 200 mg twice daily (for up to 6 months). Addback therapy is recommended with use of the higher dosing to reduce the risk of bone loss. Elagolix should not be considered a contraceptive and estrogen-containing contraceptive options have been shown to reduce efficacy so consideration towards progestin-only options or barrier protection should be used if appropriate. Although androgens such as danazol have been shown to be equally effective in treating endometriosis-associated pain (and the only pharmacologic agents to show improvement in surgical scoring), the side effect profile that includes acne, hirsutism, and metabolic disturbances may be limiting in adolescent patients. These may prove beneficial as long-term options in that side effects are minimized while efficacy is spared. At this point, any patient offered such a drug should be done so under a formal study protocol. Surgery Surgical management of endometriosis is indicated for pain refractory to medical management, advanced disease with involvement of the bowel, ureters, or nerves, and associated subfertility (generally not a concern for this cohort). Conservative surgical management with laparoscopic excision or ablation of visible implants and restoration of pelvic anatomy can provide effective treatment of pain-related complaints. However, recurrence of disease is not uncommon, and there is no consensus as to when surgery should be offered. One trial demonstrated a significant reduction in pain, lasting up to 6 months, when compared to controls who underwent diagnostic laparoscopy (sham surgery). Although laparoscopic findings do not always correlate with the degree of symptoms, pain seems to correlate 224 Chronic pelvic pain and endometriosis well with the depth of peritoneal invasion. Although a small percentage of patients will undergo reoperation due to recurrent symptoms and disease, adhesion formation and altered surgical planes may increase morbidity upon each return to the operating suite. Ovarian endometriomas are a form of deep disease that originates from the encapsulation of endometrial tissue between the ovarian cortex and the posterior leaf of the parametrium. For this reason, some experts suggest using postoperative hormonal suppression to prevent the recurrence of endometriomas. A retrospective cohort study published in 2017 demonstrated that long-term treatment with cyclic oral contraceptives can be effective in this respect. Appendectomy should be considered in patients undergoing laparoscopic surgery for suspected endometriosis, especially if complaining of right-sided pain or if the appendix appears grossly involved. Up to 50% of appendiceal specimens will yield abnormal pathology, but the effect on pain and future adverse outcomes is difficult to assess. Young age appears to be a profound risk factor for recurrent disease, particularly for ovarian endometrioma formation. In clinical practice, symptomatology should be the driving force for offering therapy and is most appropriate from a care-pathway perspective. In prevalence studies targeting adolescent females, only a relatively small percentage of patients underwent repeat laparoscopy, but the majority of these patients had surgically confirmed recurrence. Long-term follow-up allowed for the capacity of some of these women to conceive, which included 13 successful pregnancies, a success rate of approximately 72%. References 225 · · · · · · · · · repercussions of delays that contribute to long-standing morbidity. Functional pelvic pain, or that which has no easily identified source, should be assessed for in any young patient presenting with chronic complaints. Musculoskeletal disorders of the pelvic floor are often overlooked and do not respond to most medical or surgical options, but they may be elicited in up to 20% of such patients. A multidisciplinary evaluation should be undertaken in any adolescent presenting with chronic pain, especially prior to initiating therapy. Avoiding delays in effective treatment and limiting undue risks are crucial to caring for this young cohort. Ancillary imaging studies may be useful for targeting therapy but are not absolutely indicated other than to rule out other pathology. Most diagnostic and treatment paradigms used to treat adolescents have been derived from those used in adults, but new and effective, mainly progestin-based therapies have come to market in recent years. Side-effect profiles of any agents should be thoroughly addressed with the patient and her parents, especially those that may impact bone mineralization. Conservative surgery may be used to diagnose and treat endometriosis but is limited by recurrent disease that commonly affects young patients. Aggressive resection of endometriosis may provide more long-standing relief from pain and may reduce the need to perform repeat surgeries. Big picture of endometriosis helps provide guidance on approach to teens: Comparative historical data show endometriosis starting younger, is more severe. Classification of chronic pain: Descriptions of chronic pain syndromes and definitions of pain terms. Chronic pelvic pain: Prevalence, health-related quality of life an economic correlates. Transcutaneous electrical nerve stimulation and acupuncture for primary dysmenorrhoea. Neurological factors in chronic pelvic pain: Trigger points and the abdominal pelvic pain syndrome. Pelvic floor rehabilitation in the female according to the integral theory of female urinary incontinence. Sacral neuromodulation as an effective treatment for refractory pelvic floor dysfunction. Efficacy of static magnetic field therapy in chronic pelvic pain: Double-blind pilot study. Zullo F, Palomba S, Zupi E, Russo T, Morelli M, Sena T, Pellicano M, Mastrantonio P. Long-term effectiveness of presacral neurectomy for the treatment of severe dysmenorrhea due to endometriosis. Laparoscopic appendectomy in women without identifiable pathology undergoing laparoscopy for chronic pelvic pain. A randomized clinical trial to compare two different approaches to women with chronic pelvic pain. Chiropractic care for women with chronic pelvic pain: A prospective single-group intervention study. Long-term efficacy of lowdose tricyclic antidepressants for children with functional gastrointestinal disorders. Prevalence of endometriosis in adolescent girls with chronic pelvic pain not responding to conventional therapy. Long-term fertility after laparoscopy for endometriosis-associated pelvic pain in young adult women. Dysmenorrhea, absenteeism from school, and symptoms suspicious for endometriosis in adolescents. The development of the implantation theory for the origin of peritoneal endometriosis. Serum and peritoneal fluid immunological markers in adolescent girls with chronic pelvic pain. Suggestive evidence that pelvic endometriosis is a progressive disease, whereas deeply infiltrating endometriosis is associated with pelvic pain. Progesterone response in neonatal endometrium is key to future reproductive health in adolescents. A prospective study of body size during childhood and early adulthood and the incidence of endometriosis. Diagnosis of pelvic endometriosis with use of macroscopic versus histologic findings. Endometriosis in premenarcheal girls who do not have an associated obstructive anomaly. Prevalence of endometriosis diagnosed by laparoscopy in adolescents with dysmenorrhea or chronic pelvic pain: A systematic review. A selective cyclooxygenase-2 inhibitor suppresses the growth of endometriosis xenografts via antiangiogenic activity in severe combined immunodeficiency mice. A dose-ranging study to determine the efficacy and safety of 1, 2, and 4 mg of dienogest daily for endometriosis. Petraglia F, Hornung D, Seitz C, Faustmann T, Gerlinger C, Luisi S, Lazzeri L, Strowitzki T. Reduced pelvic pain in women with endometriosis: Efficacy of long-term dienogest treatment. Dienogest is as effective as leuprolide acetate in treating the painful symptoms of endometriosis: A 24-week, randomized, multicentre, open-label trial. A levonorgestrel-releasing intrauterine system for the treatment of dysmenorrhea associated with endometriosis: A pilot study. Levonorgestrel-releasing intrauterine device used for dysmenorrhea: Five-year literature review. Adolescents and long-acting reversible contraception: Implants and intrauterine devices. Lupron depot (leuprolide acetate for depot suspension) in the treatment of endometriosis: A randomized, placebo-controlled, double-blind study. Timing of peak bone mass in Caucasian females and its implication for the prevention of osteoporosis: Inference from a cross-sectional model. The use of gonadotropin releasing hormone analogues in adolescent and young patients with endometriosis. Hormonal add-back therapy for females treated with gonadotropin-releasing hormone agonist for endometriosis: A randomized controlled trial. Follow-up report on a randomized controlled trial of laser laparoscopy in the treatment of pelvic pain associated with minimal to mild endometriosis. Determinants of long-term clinically detected 228 Chronic pelvic pain and endometriosis 83. The effects and effectiveness of laparoscopic excision of endometriosis: a prospective study with 25 year follow-up.
Syndromes
- Increased hair (hypertrichosis)
- Children: 19 to 47
- Fortified milk and dairy products (cheese, yogurt, butter, and cream)
- Put safety latches on cabinets that a child should not open.
- Sodium level in the blood
- Fatigue
- Vicodin ES
- Sarcoidosis
Biopsy revealed severe heart attack recovery discount betapace 40 mg with amex, acute ileitis arrhythmia natural cure order betapace 40 mg line, occurring only during inflammatory episodes arterial nicking quality 40 mg betapace, with resolution during clinical remission hyperextension knee buy online betapace. Disease is responsive to prednisone blood pressure medication young age 40 mg betapace buy otc, but infliximab and methotrexate may lead to steroid-sparing remission. However, both cause highly variable clinical manifestations, each with their own wide spectrum of disease. More severe anomalies including agenesis of the corpus callosum, and skeletal and renal anomalies are also commonly observed. Aphthous ulcerations are severe, painful, and recurrent, affecting the oral and genital mucosa, often with subsequent scarring. The inflammatory manifestations are thought to be secondary to gene dosage effects, but candidate genes remain to be identified. Corticosteroids, methotrexate, hydroxychloroquine, colchicine, tocilizumab, azathioprine, and thalidomide have been utilized in patients with one-third to one-half of patients experiencing symptomatic improvement. Cytokine targeted therapy, namely, anakinra, infliximab, or tocilizumab, was used in a subset of patients with fair response. Familial cold autoinflammatory syndrome: phenotype and genotype of an autosomal dominant periodic fever. An autoinflammatory disease with deficiency of the interleukin-1-receptor antagonist. Chronic cutaneous pustulosis due to a 175-kb deletion on chromosome 2q13: excellent response to anakinra. Genome-wide linkage scan for psoriasis susceptibility loci in multiplex Tunisian families. Gene for familial psoriasis susceptibility mapped to the distal end of human chromosome 17q. Mutations in proteasome subunit beta type 8 cause chronic atypical neutrophilic dermatosis with lipodystrophy and elevated temperature with evidence of genetic and phenotypic heterogeneity. Proteasome-associated autoinflammatory syndromes: advances in pathogeneses, clinical presentations, diagnosis, and management. A morphological, histochemical, immunohistochemical, and ultrastructural study of 10 cases. H syndrome: 5 new cases from the United States with novel features and responses to therapy. Faisalabad histiocytosis mimics Rosai-Dorfman disease: brothers with lymphadenopathy, intrauterine fractures, short stature, and sensorineural deafness. The H syndrome: a genodermatosis characterized by indurated, hyperpigmented, and hypertrichotic skin with systemic manifestations. Congenital poikiloderma with traumatic bulla formation and progressive cutaneous atrophy. Kindler surprise: mutations in a novel actin-associated protein cause Kindler syndrome. Kindler syndrome complicated by squamous cell carcinoma of the hard palate: successful treatment with highdose radiation therapy and granulocyte-macrophage colony-stimulating factor. Mucocutaneous lesions and recurrent fevers in patients with trisomy 8 mosaicism and chromosome 8 duplication [abstract]. Myelodysplastic syndrome with trisomy 8 associated with Behcet syndrome: an immunologic link to a karyotypic abnormality. Inflammatory disorders associated with trisomy 8-myelodysplastic syndromes: french retrospective casecontrol study. Chapter 32 Mendelian disorders of immunity related to an upregulation of type I interferon Marie-Louise Fremonda and Yanick J. A hallmark of these diseases is their high associated morbidity and early mortality, associated with an apparent lack of response to conventional immunosuppressive therapies. Phenotypic variability within the same genotype, and even in the same family, is seen frequently, and non-penetrance can also be observed. Below, we present a clinical and pathogenic overview of these conditions (see also Table 32. A better understanding of pathogenesis has led to the development of directed therapies in some contexts. Mendelian disorders of immunity related to an upregulation of type I interferon Chapter 32 753 represents the first of the described Mendelian type I interferonopathies. Importantly, disparity in clinical phenotype is sometimes observed even within the same family, thereby highlighting the role of modifying factors. Age at onset is difficult to set precisely; however, most patients experience the onset of disease during the first year of life: the earliest presentations being neonatal, thereby clearly implying in utero pathology in some cases. The oldest developed symptoms at five years of age (with the subacute onset of dystonia). Typically, patients are left with limb spasticity, dystonic posturing of the limbs, truncal hypotonia and poor head control. Epileptic seizures are reported in around 40% of patients, but are usually relatively easily controlled. A number of children have been noted to demonstrate a marked startle reaction to sudden noise. The lack of retinal changes and hearing loss are useful differentiating features from congenital infection. Where death occurs, this seems usually not to be due to a regressive process but secondary to the consequences of neurological damage incurred during the initial disease episode. Some patients are known to have lived beyond the age of 15 years, and rare patients are still alive at more than 30 years of age. The lesions most typically develop after the first year of life and are seen especially on the toes and fingers, and sometimes on the outer helix of the ears. Frequently, the feet and hands are also reported to be very cold, even in the absence of overt chilblains. The lesions probably result from an inflammatory vasculopathy, so that biopsy most typically reveals a lymphocytic vasculitis with, occasionally, the deposition of immunoglobulin and complement in vessel walls. These cells then signal to hematopoietic cells, leading to T cell-dependent inflammation and a disease-relevant autoantibody response. However, pulmonary symptoms can be insidious,53 thereby indicating the need for a careful screening - including an assessment of pulmonary functions (lung volumes, diffusing capacity of the lungs for carbon monoxide, and 6-min walking test) and chest computed tomography scan. However, the severe lung disease was poorly responsive to treatment, warranting further therapeutic strategies. A total of 12 individuals have been so far reported,92e99 presenting with distinct phenotypes encompassing apparently isolated hereditary hearing loss,93 late-onset neurological features with congenital hearing loss,98 and severe fixed or progressive early-onset encephalopathy with mitochondrial respiratory chain deficiency. Other prominent features include persistent periorbital erythema and edema, finger or toe swelling, joint contractures, hepatomegaly and splenomegaly, lymphadenopathy with anemia, progressive lipodystrophy, failure to thrive, inflammation affecting the muscle and different other organs. This disease is rare (less than 40 patients reported so far) and characterized by variable expression and clinical nonpenetrance. Interstitial lung disease can also be observed, resulting in fibrosis and end-stage respiratory failure. Arthritis is frequent, affecting the knees and the interphalangeal joints of the hands, and can be associated with autoantibodies (antinuclear and anti-neutrophil cytoplasmic antibodies, and rheumatoid factor). Osteonecrosis and severe erosive bone lesions have been documented in several patients. C1q deficiency Complement deficiencies are comprehensively described in Chapter 42. Different mutations occurring throughout the three chains of C1q have been described. Thus, a disturbance of phagocytosis of apoptotic cells could result in an excess of endogenous immunostimulatory nucleic acids. In the C1q knock-out mouse, maintenance of B cell tolerance is compromised, contributing to autoantibody secretion. These lesions predominantly develop within long bones, but may also occur in other areas of endochondral growth, such as the iliac crest. Severity varies, but slow progression during childhood is reported and is due to the location of the lesions within the growing metaphyses. Neurological involvement most typically includes intracranial calcification, particularly involving the basal ganglia, white-grey matter junction, dentate nuclei of the cerebellum and the pons, with or without white matter involvement. These imaging features can be associated with a variable degree of neurological dysfunction, most typically mild to moderate developmental delay, spasticity and epilepsy. In many cases, calcification is seen in a periventricular distribution highly suggestive of congenital infection. Additionally, intracranial calcification may only become evident over a period of Mendelian disorders of immunity related to an upregulation of type I interferon Chapter 32 763 months. However, some patients show marked fronto-temporal white matter involvement with cyst formation. Cerebral atrophy is present in the majority of severely affected children and some demonstrate marked brainstem and cerebellar shrinkage also. The cerebral vasculopathy can be both occlusive, with terminal carotid occlusion and basal collaterals reminiscent of moyamoya syndrome, and aneurysmal. Consequent intracerebral hemorrhage can be seen, and has been fatal in several cases. Post-mortem examination of one patient suggested that the arteriopathy was inflammatory in origin. Obvious issues relate to spasticity, dystonia, feeding, seizure control and the development of scoliosis. Neither classical immunosuppressive nor vasodilator therapy are definitely useful therapeutically for the chilblain lesions. Specific management of type I interferonopathies Deciphering mechanisms involved in the pathogenesis of the type I interferonopathies, and more generally in nucleic acid driven inflammation, can help to define targeted therapies. In line with the nucleic acid hypothesis, three general approaches to therapy might be delineated: 1. Favoring the degradation of self nucleic acids Therapeutic approaches enhancing the removal of nucleic acids are not currently available. Blocking downstream signaling this third strategy is currently the most developed in clinical trials and case reports. Self-awareness: nucleic acid-driven inflammation and the type I interferonopathies. A progressive familial encephalopathy in infancy with calcifications of the basal ganglia and chronic cerebrospinal fluid lymphocytosis. Intrathecal synthesis of interferon-alpha in infants with progressive familial encephalopathy. Mutations in genes encoding ribonuclease H2 subunits cause AicardiGoutières syndrome and mimic congenital viral brain infection. An unusual syndrome of widened medullary cavities of the metacarpals and phalanges, aortic calcification and abnormal dentition. Expanding the phenotypic spectrum of lupus erythematosus in AicardiGoutières syndrome. Asp18Asn mutation can cause variable neurological symptoms in a family with Aicardi-Goutieres syndrome/familial chilblain lupus. Autoimmunity initiates in nonhematopoietic cells and progresses via lymphocytes in an interferon-dependent autoimmune disease. Mendelian disorders of immunity related to an upregulation of type I interferon Chapter 32 767 42. Jeremiah N, Neven B, Gentili M, Callebaut I, Maschalidi S, Stolzenberg M-C, et al. Stimulator of interferon genes-associated vasculopathy with onset in infancy: a mimic of childhood granulomatosis with polyangiitis. Picard C, Thouvenin G, Kannengiesser C, Dubus J-C, Jeremiah N, Rieux-Laucat F, et al. Failure to thrive, interstitial lung disease, and progressive digital necrosis with onset in infancy. Detection of interferon alpha protein reveals differential levels and cellular sources in disease. X-linked reticulate pigmentary disorder with systemic manifestations: report of a third family and literature review. X-linked reticulate pigmentary disorder with systemic manifestations: a new family and review of the literature. Exome sequencing in 32 patients with anophthalmia/microphthalmia and developmental eye defects. Sato R, Arai-Ichinoi N, Kikuchi A, Matsuhashi T, Numata-Uematsu Y, Uematsu M, et al. Mendelian disorders of immunity related to an upregulation of type I interferon Chapter 32 769 102. Mutations in proteasome subunit b type 8 cause chronic atypical neutrophilic dermatosis with lipodystrophy and elevated temperature with evidence of genetic and phenotypic heterogeneity. C1q inhibits immune complex-induced interferon-alpha production in plasmacytoid dendritic cells: a novel link between C1q deficiency and systemic lupus erythematosus pathogenesis. Possible heterogeneity in spondyloenchondrodysplasia: quadriparesis, basal ganglia calcifications, and chondrocyte inclusions. Spondyloenchondrodysplasia with spasticity, cerebral calcifications, and immune dysregulation: clinical and radiographic delineation of a pleiotropic disorder. Tartrate-resistant acid phosphatase deficiency in the predisposition to systemic lupus erythematosus. Clinical, radiological and possible pathological overlap of cystic leukoencephalopathy without megalencephaly and Aicardi-Goutières syndrome.
Purchase betapace online now. High Blood Pressure - Causes Symptoms and Treatment Options.
References
- Kidner TB, Yoon J, Faries MB, et al. Preoperative imaging of pulmonary metastases in patients with melanoma: implications for minimally invasive techniques. Arch Surg 2012;147(9):871-874.
- Stahl R, Jain SK, Lutz J, et al. Osteoarthritis of the knee at 3.
- Waller FT, Tanabe CT, Paxton HD. Treatment of elevated intracranial pressure with dimethyl sulfoxide. Ann N Y Acad Sci. 1983;411:286-292.
- Ratjen F, Munck A, Kho P, et al. Treatment of early Pseudomonas aeruginosa infection in patients with cystic fibrosis: the ELITE Trial. Thorax 2010; 65: 286-291.
- Gloviczki P, Cambria RA, Rhee RY, et al: Surgical technique and preliminary results of endoscopic subfascial division of perforating veins, J Vasc Surg 23(3):517-523, 1996.
- Okumura MJ, Ong T, Dawson D, et al: Improving transition from paediatric to adult cystic fibrosis care: programme implementation and evaluation, BMJ Qual Saf 23(Suppl 1):i64ni72, 2014.
- Feeley L, Quinn CM. Columnar cell lesions of the breast. Histopathology. 2008;52(1):11-19.
- Parada MT, Alba A, Sepulveda C. Early and late infections in lung transplantation patients. Transplant Proc 2010;42:333-5.
