
Prednisolone
| Contato
Página Inicial
James R. Ouellette DO
- Assistant Professor of Surgery/Associate Program Director, Division of Surgical
- Oncology, Hepatobiliary and Pancreatic Surgery Program, Wright State University
- Boonshoft School of Medicine, Dayton, Ohio
Histopathologically allergy medicine isn't working order prednisolone 20 mg without prescription, there is photoreceptor degeneration allergy choices generic prednisolone 10 mg mastercard, atrophy of the outer nuclear layer allergy mask cheap prednisolone online visa, and melanin deposits within the inner nuclear layer allergy symptoms cough buy cheap prednisolone 40 mg line. Ultrastructurally in the inner collagenous portion of Bruch membrane allergy treatment 197 purchase cheap prednisolone on line, numerous lipofuscin granules, vesicular bodies, and crystalline material are seen. Irene Maumenee Widespread atrophic change with choroidal vessel visibility is evident in this patient with Alagille syndrome. It is characterized by intestinal lipid malabsorption with low serum cholesterol, vitamin A and E deficiency, and absent plasma betalipoproteins. Systemic findings include acanthocytosis (crenation of red blood cells), neuropathy, and cerebellar dysfunction (Friedreich-type spinal cerebellar ataxia). The ocular findings include a pigmentary retinopathy that may resemble retinitis punctata albescens or the more typical retinitis pigmentosa. The retinal changes are presumed to be due to a deficiency of vitamin A, and the clinical course of the retinal degeneration resembles that seen in vitamin A deficiency with rod function deteriorating earlier than cone function. Treatment with a low-fat diet and large doses of supplements of the fat-soluble vitamins A, E, and K may slow progression. A broad angioid streak is present superotemporally in the right eye and finer branching streaks are seen in the same area of the left eye (arrows). Scott Sneed In this patient with BassenKornzweig syndrome, diffuse peripheral chorioretinal atrophy and pigment epithelial hyperplasia is noted. Irene Maumenee this patient with BassenKornzweig syndrome has a prominent angioid streak (arrows) with chorioretinal atrophy around the disc and otherwise a relatively normal fundus. Clinically it is characterized by neonatal growth retardation, impaired development of the nervous system, hearing loss, premature aging, cachexia, and characteristic facies and multiple ocular problems. Anterior segment manifestations include severe tear film deficiency leading to exposure keratopathy and early cataract. A "salt and pepper" type pigmentary retinal degeneration can be documented in over 60% of patients and is considered one of the hallmarks of the disease. In some cases a retinitis pigmentosa-type picture has been described with peripheral bone spicules, vascular attenuation, and optic atrophy. Optic atrophy is prominent in association with retinal vascular attenuation in this 9-year-old female. It is characterized by early onset of extrapyramidal motor signs, dysarthria, rigidity, choreoathetosis, epilepsy, and dementia with a rapidly progressive course leading to death in early adulthood. It has been classified clinically into three forms each with a different age of onset and rate of progression. Patients with retinal findings tend to have an earlier onset of disease that is more rapidly progressive, leading to death in late childhood. Histopathologically, there is absence of photoreceptors and atrophy of the plexiform and outer nuclear layers but the inner retinal layers are normal. Acanthocytosis and a pigmentary retinal degeneration were also noted and the latter occurs in about one-quarter of these patients. Retinal flecks are often seen in the peripheral fundus, as is evident in the photo on the left. This patient with HallervordenSpatz disease shows severe optic atrophy and attenuated retinal vessels with a pigmentary retinopathy. These are characteristic of the disorder, implicating the presence of lipofuscin in the central portion of the lesion. It is characterized by distal amyotrophia, atrophy of the corpus callosum, progressive spasticity affecting primarily the lower limbs, cognitive impairment, and maculopathy. Fundus findings are phenotypically similar to Stargardt disease or pattern dystrophy, but with distinct differences. These may be seen dramatically with fundus autofluorescence where they exhibit central hyperautofluorescence surrounded by a hypoautofluorescent halo. With fluorescein angiography, the lesions block fluorescence centrally with a hyperfluorescent halo in late phase. The central portion of the lesions exhibits late staining with indocyanine green angiography. The lesions on fluorescein angiography are dark with borders of hyperfluorescence. The disorder is genetically heterogeneous and typically inherited in an autosomal dominant manner with variable penetrance and many of the subtypes are a result of trinucleotide expansions. While at least 30 distinct subtypes have been described, types 1, 2, 3, 6, and 7 represent approximately 80% of diagnoses. Patients may present with progressive color and sometimes severe visual acuity deficits. There is a total loss of outer segments and total loss of inner segments with a reduction in the outer nuclear layer. Congenital syphilis can cause an asymmetric pigmentary retinopathy with or without pigment spicules and associated peripheral vision loss in patients with other stigmata of this syndrome including saddle-shaped nose, peg shaped teeth, and interstitial keratitis. Peripheral visual field constriction or an annular scotoma, like that seen in retinitis pigmentosa, may also be seen as is noted in the right eye of this syphilitic patient (third row). The facial photograph illustrates peg-shaped teeth with blunting of the incisors characteristic of congenital syphillis. Patients manifest various degrees of hypopigmentation in the iris and fundus with associated reduced vision, large refractive errors, nystagmus, strabismus, and foveal hypoplasia. Misrouting of the optic nerves and increased decussating axonal fibers occur at the chiasm. Ocular findings include iris transillumination defects and a hypopigmented fundus with enhanced visualization of the underlying choroid. Histopathologic sectioning through the center of the macula shows a lack of foveal differentiation. Unique systemic syndromes that include various degrees of albinism as a feature are HermanskyPudlak and ChédiakHigashi. HermanskyPudlak syndrome is a rare autosomal recessive disorder with oculocutaneous albinism, bleeding related to poor platelet aggregation, lysosomal ceroid accumulation in a variety of tissues, pulmonary fibrosis, granulomatous enteropathic disease, and renal failure. ChédiakHigashi syndrome is characterized by partial oculocutaneous albinism, impaired bacteriolysis due to failure of phagolysosome formation, neutropenia, abnormal susceptibility to infection, and lymphomatous disease. The histopathological serial sectioning through the center of the macula in a patient with ocular albinism shows a lack of foveal differentiation. Jeffrey Shakin Transillumination of the globe and gross examination also show absence of substantial pigment. Findings include vision loss, nystagmus, iris transillumination defects, hypopigmented fundus with easily visible choroidal vessels, and foveal hypoplasia. With fluorescein angiography, areas of normal pigmentation will block fluorescence adjacent to areas of increased transmission from the choroid through less pigmented areas. This patient with ocular albinism demonstrates the characteristic hypopigmented fundus. There is enhanced visualization of the choroidal circulation through the depigmented pigment epithelial layer. There is no evidence of pigmentation, prominent choroidal vessels are easily visible clinically, and there is poor differentiation of the fovea. This is a 2-year-old patient with ocular albinism, showing widespread hypopigmentation and an indistinct foveal depression. A pale fundus like this may sometimes be confused with other pediatric fundus anomalies and abnormalities. This is the so-called "mud-slung" fundus with alternating areas of hypo- and hyperpigmentation throughout the fundus from the central foveal area to the far periphery. Migrating pigment spicules and vascular attenuation are not prominent features of this class of disease. The disease follows a well-characterized course of progression with onset in the first to second decade of life. Fundus examination early in the disease course reveals "salt and pepper" pigmentary retinopathy involving the midperiphery and posterior pole, with patchy areas of pigment loss giving the underlying fundus a metallic sheen. Diffuse choroidal atrophy ensues, beginning in the midperiphery and extending toward the macula, which leaves scattered small areas of intact choriocapillaris in the central macula and periphery. Rarely carrier females may demonstrate diffuse chorioretinal atrophy similar to affected male patients. This is thought to be a result of random inactivation of the wild type X chromosome in the female carrier, a genetic phenomenon known as lyonization. Histopathologically, extensive choroidal atrophy is seen in male patients with choroideremia. Note the pallor to the fundus, which is diffusely atrophic surrounding the posterior pole. The fluorescein angiogram shows diffuse loss of the choriocapillaris, except for a preserved central hyperfluorescent island. A ring of perifoveal pigment epithelial and choriocapillaris atrophy is noted in the middle row of color photos. Jim Tiedeman the histopathology images from a patient with choroideremia reveal loss of the choroid, retinal pigment epithelium, and outer retinal areas. The fluorescein angiograms from a different patient show a similar stellate preservation in the macula. Presumably, this pattern may relate to conformity to the lobular architectural structure of the choriocapillaris. Fluorescein angiogram and autofluorescence (third row) of her son shows diffuse chorioretinal atrophy. Patients generally present with nyctalopia, high myopia, and astigmatism within the first decade of life with subsequent development of posterior subcapsular cataracts by the second decade. Slowly progressive constriction of visual fields and eventual loss of central visual acuity continue into the fourth to fifth decades. Initially, circular, sharply demarcated regions of chorioretinal atrophy with hyperpigmented margins in the midperiphery are seen that slowly enlarge and coalesce in a "scalloped" pattern, spreading anteriorly and posteriorly, and eventually encroaching into the macula. Leakage at the margins of healthy and affected tissue, with hyperfluorescence within the gyrate lesions, may be seen on fluorescein angiography. Early impaired scotopic and photopic responses are seen on electrophysiologic testing, and these become extinguished as the disease progresses. These patients usually have no muscular symptoms, but may show impaired performance when speed or acute strength is required. The disease progresses to almost complete loss of type 2 fibers, but the progression of muscular abnormalities is slower than the chorioretinal degeneration. Treatment for gyrate atrophy has been aimed toward reducing plasma ornithine levels. In patients with a pyridoxine-responsive form of gyrate atrophy, supplementation with pyridoxine has been shown to reduce ornithine levels. Diets restricted in arginine (the precursor of ornithine) have been shown to delay the progression of visual deficits, although patients may demonstrate continued chorioretinal deterioration. Like choroideremia, the atrophic lesions start in the midperiphery and then extend in both directions, anteriorly and posteriorly. On light microscopy, there is a clearly distinguishable junction between unaffected and affected areas on these phase contrast and light microscopy photographs (arrows). There is also an absence of the choroid and outer retinal layers in the affected area. The image below is her young daughter, who also has gyrate atrophy at a very early stage, a product of consanguinity between the above patient and her father. Associated ocular findings include elongated spindles extending from the ciliary body to the central position on the lens capsule, best appreciated with transillumination. The large choroidal vessels are well visualized within these areas due to atrophy of the overlying tissues. Note the fluorescein angiogram that shows a well circumscribed geographic window defect early with late staining due to central atrophy. The very late angiogram shows staining of visible sclera and the silhouette of larger choroidal vessels. There is no leakage into the extrachoroidal tissue because of the absence of the choriocapillaris. This patient with central areolar choroidal dystrophy has a larger, ovoid, symmetrical atrophic maculopathy. There are multiple areas of more pronounced atrophy, which include the choriocapillaris within the ovoid zone. These atrophic areas are more clearly evident on the fundus autofluorescence image where patchy areas of hypoautofluorescence are present (arrows). Posterior polar central choroidal dystrophy may start as a focal degenerative process in the central macula, but the area of atrophy may expand. At first, there may be patchy or zonal atrophy, followed by confluency as the entire process expands to the temporal vascular arcades and the disc and beyond. The annular zone of atrophy has scalloped and indistinct margins, again with some preservation of the choriocapillaris at the junction with the normal choroid. The fluorescein angiogram again shows a fringe of choriocapillaris hyperfluorescence concentric to the posterior pole and central macular region. The fundus autofluorescence reveals hypoautofluorescence in areas of chorioretinal atrophy with islands of sparing in the central macula where there is preserved pigment epithelium. They are all associated with systemic manifestations, most frequently renal disorders. It is characterized by numerous glistening, yellow, crystalline deposits distributed throughout the fundus and, in some cases, the superficial cornea near the limbus and the lens capsule. Patients may develop progressive nyctalopia, constriction of visual fields and decreased visual acuity progressing to legal blindness in the sixth decade. Clinical manifestations of Bietti crystalline corneoretinal dystrophy are seen in these images. Crystalline deposition in the cornea is usually in the middle stroma near the limbus. The patient also had crystal deposits in the cornea seen here on slit lamp examination (right). This disorder is characterized by continuous, high urinary oxalate excretion with progressive bilateral oxalate urolithiasis, nephrocalcinosis, and chronic renal failure in childhood or early adulthood.
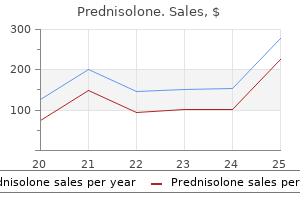
This needle is exchanged for a micropuncture set with which the definitive calyceal puncture is made under direct ultrasound visualisation allergy over the counter generic prednisolone 10 mg. Once urine is aspirated allergy upset stomach prednisolone 5 mg buy, dilute contrast is injected to confirm calyceal position with fluoroscopy allergy medicine and blood pressure discount prednisolone 10 mg buy line. This should be done prior to the insertion of a guidewire and sheath to ensure a secure and satisfactory position allergy symptoms hives 10 mg prednisolone with amex. A vascular catheter commonly a Cobra or biliary manipulation catheter is used to provide stability and facilitate bridging of any stenosis and entry into the bladder allergy juniper generic 5 mg prednisolone with visa. When the position in the bladder is confirmed with contrast fluoroscopically, a peelaway sheath may be inserted over a support wire to lie in the mid ureter place; this supports the insertion and positioning of the stent. A double J stent is then advanced over a stiff wire to sit with the distal loop in the bladder. Once safe position in the bladder is confirmed, the proximal loop is formed in the renal pelvis and contrast is instilled to ensure patency. The latter are similar to a retrograde stenting as they are related to the stent itself, which are ubiquitous irrespective of the route of placement. The majority of complications are the former and may be further considered as systemic or local and minor or major, dependent on requirement for further treatment [10]. This results from bacterial translocation from renal pelvis to systemic circulation due to increased pressure in an infected system during puncture, contrast injection, and wire manipulation [11]. The reported rate of post nephrostomy insertion fever has been reported at between 21 [12] and 100% [13]. The rate of sepsis, however, is relatively small and has been reported in 13% of all patients post percutaneous nephrostomy, increasing to 79% in patients with preexisting pyonephrosis in one review [10]. To reduce this risk, over distension of the collecting system should be avoided during contrast injection. Evidence also suggests that the routine administration of 500 mg of oral ciprofloxacin 1 hour prior to nephrostomy insertion significantly reduces complications and is cost effective [9]. It stands to reason that a similar protocol for antegrade stenting would be effective but local microbiology protocols should be consulted. Bleeding is the major local complication of percutaneous renal puncture and may occur from parenchymal or, if a high approach is taken, intercostal vessels. Venous bleeding is normally selflimiting but may be ameliorated by upsizing the catheter to cause tamponade. In fact, some degree of venous bleeding is reported in up to 95% of cases but is a minor complication that rarely requires intervention [10]. It arises either from branches of the renal artery or intercostal vessels if a high approach is taken. Depending on the severity, the Role of the Interventional Radiologist in Managing Ureteric Obstruction 59 this may require transfusion, embolization, and rarely, open surgical management. The risk of bleeding correlates directly with the size of tract, and as such, a smaller sheath will carry a lower bleeding risk. The longterm complications of arterial injury include arteriovenous fistula formation, perirenal/retroperitoneal hematoma, and pseudoaneurysms. Although these are rare, they may be significant and should be considered in a patient who deteriorates following intervention [11]. The overall rate of bleeding complications requiring transfusion or other intervention is reported at 1 to 4% [10]. Less common local complications of percutaneous renal puncture include pleural complications of pneumothorax, hydrothorax, or hemothorax with reported rates of 0. Urinoma formation following percutaneous puncture is a further recognized local complication with a reported rate of 0. Complications relating to transcolonic puncture are uncommon but have been reported [16]. Local complications related to stent insertion are similar to those with a retrograde approach and include bladder irritation, pain, hematuria, infections, stent displacement, and blockage. These complications are not specific to antegrade stenting and are discussed in detail elsewhere. These figures are comparable to the reported complication rate of retrograde stent insertion at 5. The Glidex Hydrogel Coating on stent requires activation by soaking in sterile water or saline prior to use. The suture at the proximal end enables retraction to facilitate optimal positioning; this must be removed once appropriate placement is achieved. Midpole puncture may allow easier stent placement due to greater pushability particularly in the context of a distal ureteric stricture. Modern stents are almost exclusively double J in design and formed of polymeric material. Polymeric stents provide a largely biologically inert stent and are usually coated with a variety of substances to provide a hydrophilic coating and reduce the formation of biofilms. Polymeric stents do, however, have limitations in terms of strength to resist radial force and acting as a nidus for infection formation [20]. In a bid to overcome these problems, there is ongoing research into the development of both metallic ureteric stents, to provide greater radial force, and biodegradable stents, to reduce complications of stent encrusting and infection [21]. At present, no biodegradable antegrade stents are used in clinical practice and these will not be considered further. As discussed previously, antegrade stent insertion is most beneficial in the situation of external ureteric compression due to pelvic malignancy [5, 6] and as such the ability to withstand high radial force is especially desirable in stents placed via the antegrade route. Initial experience with metallic mesh stents was promising showing good patency rates in the treatment of malignant obstruction [22]. A more recent publication demonstrated a primary patency rate at 18 months of 54% but showed that placement of these stents did not result in adequate correction of renal failure to allow chemotherapy, the intended aim, in 21% of recipients [23]. Experience with newer covered metallic stents placed via the antegrade approach has been more encouraging. Although this was not a randomized study and the numbers small, initial results are promising and further large trials are required. Initially, a percutaneous nephrostomy tube is inserted acutely to relieve obstruction and after a delay the antegrade stent is inserted. These advances and increasing demand on interventional uroradiologists has led to research in to the utility of a onestage approach to antegrade ureteric stenting. Current small studies have suggested that the use of a onestage procedure in certain instances is both safe and cost effective. A onestage procedure should not be considered if there is obstruction complicated by acute sepsis or untreated renal failure [25]. Other studies have, however, demonstrated a lower clinical success rate with a one stage tubeless approach [17] and at present, the result of larger studies are awaited to inform daytoday practice. This has become known as the rendezvous procedure the Role of the Interventional Radiologist in Managing Ureteric Obstruction 63 and allows bidirectional traction to be applied across a stricture, as long as a wire can be passed across the lesion initially [26]. In patients with long length, mid ureteric, ischemic or radiationrelated strictures this approach has increased antegrade stent success from 78. The use of a buddy wire, which can be introduced via the peel away sheath, can aid stability in challenging anatomy and stenotic disease. Also, a staged approach to nephrostomy and stent insertion is frequently preferable in the emergent setting and while rarely an antegrade stent cannot be suitable advanced into a satisfactory position, this is mostly overcome with the use of a rendezvous technique. Waisting of the distal 1/3rd of the balloon is noted at the level of the vesicoureteric junction. As such, antegrade stenting is considered the optimal initial approach in this patient group. The place of antegrade stenting in benign ureteric obstruction is uncertain and no large studies exist. The limited case numbers available suggest that antegrade stenting is a reasonable secondline treatment if the retrograde approach fails. In complex situations where retrograde or antegrade stenting alone are unlikely to succeed, a rendezvous procedure is an effective and established approach requiring close cooperation of both interventionalist and urologist. Ongoing research in to a onestage approach to antegrade ureteric stenting is required, but the available evidence suggests this is a costeffective and safe approach in malignant ureteric obstruction without concomitant sepsis or renal failure. The use of antegrade metallic stents has in the past shown varied results but newer covered metallic stents are a promising area of ongoing research for the treatment of malignant ureteric obstruction. Biodegradable antegrade stents are still under investigation but to date are not in regular clinical use. The Role of the Interventional Radiologist in Managing Ureteric Obstruction 65 Best treatment of ureteric obstruction requires close collaboration between both urologists and interventional radiologists. Robust guidelines governing optimal approach for stenting, preintervention optimization, and appropriate antibiotic prophylaxis should be encouraged and agreed on locally in the absence of national guidelines. Accordingly, complications associated with stone disease have increased over time as well. Obstructive pyelonephritis, the occurrence of urinary infection proximal to a site of ureteral obstruction, is considered a urologic emergency that requires prompt drainage of the kidney to prevent life threatening sepsis. According to data obtained from the Nationwide Inpatient Sample, hospital discharges associated with a diagnosis of renal or ureteral calculi and urinary tract infection/pyelonephritis increased by 96% between 1999 and 2009. Taking into account the increase in population, this represents a 12% increase in incidence per 100,000 U. Interestingly, despite a higher prevalence of nephrolithiasis in men than women, women were more than twice as likely to have infected urolithiasis than men (22. There are no randomized trials comparing surgical decompression with conservative management in patients with obstructive pyelonephritis. Only one older retrospective trial evaluated the outcome of 14 febrile patients with ureteral calculi in whom conservative therapy with fluid and antibiotics was initiated [12]. However, concern for pyonephrosis, the most feared and extreme form of obstructive pyelonephritis, which carries a high mortality rate and risk of renal loss, leads most practitioners to recommend prompt drainage of the collecting system in the setting of obstruction and infection. Indeed, data from the Nationwide Inpatient Sample from 2007 to 2009 revealed a higher mortality rate in patients with ureteral calculi and sepsis treated conservatively than with surgical decompression (19. Furthermore, this disparity in mortality rates is likely an underestimate because of selection bias, by which only less sick patients were likely selected for conservative management. Elevated white blood count, fever, and bacteriuria are generally accepted indicators of pyelonephritis, although the exact cutpoints defining abnormal parameters are not wellestablished. However, the optimal choice of drainage in the setting of obstruction and infection is controversial (Table 7. Proponents of nephrostomy drainage favor avoiding manipulation of the ureter and stone for fear of urinary extravasation or sepsis and cite the larger caliber nephrostomy tube, ability to directly monitor drainage and placement under intravenous sedation as advantages. On the other hand, stent advocates cite the lower serious complication rate with stent placement, greater comfort for patients with an internal drainage tube, and the ability of all urologists to perform the procedure. Retrograde stent placement is exclusively performed by urologists, most often in the operating room under general anesthesia using fluorosocopic guidance. Yossepowitch and colleagues prospectively evaluated 92 patients with ureteral obstruction, 61 of whom had intrinsic obstruction (from ureteral stones in 52, ureteropelvic junction obstruction in 5 and ureteral stricture in 4) [15]. Stent placement was successful in 94% of the patients with intrinsic obstruction and in 73% of the patients with extrinsic obstruction. On univariate analysis, the cause of obstruction, location of obstruction, and degree of hydronephrosis predicted the likelihood of successful stent insertion. Early complications of retrograde stent placement include sepsis, stent migration, and stent occlusion. The incidence of sepsis associated with stent placement in the absence of stone manipulation has not been well evaluated. Stent occlusion or failure increases with duration of stenting, but the likelihood of immediate stent failure in the setting of pyonephrosis or obstructive pyelonephritis has not been reported. The two groups were comparable with regard to preoperative patient and stone characteristics. Among the 21 patients randomized to stent placement, a 7Fr double pigtail stent was placed in 81% of patients and 6Fr stent in 19%. Because of no difference in efficacy between the two modalities, the authors concluded that the choice of drainage should be left to the discretion of the treating physician, taking into account stone size and location, subsequent planned definitive treatment modality and availability of operative room time and interventional radiologists. The primary outcome parameters in this trial included success of drainage, relief of accompanying symptoms, duration of tube drainage, and effect of diversion on quality of life. Both procedures were performed under local anesthesia or conscious sedation in all patients. Reasons for failure were enlarged prostate precluding access to the ureteral orifice and discomfort during stent insertion. No significant difference was reported for pain relief or quality of life between the two groups. Using the Nationwide Inpatient Sample (19992009), Sammon and associates identified 113,439 patients with infection and obstruction due to stones who underwent drainage of the kidney. They found no difference in the mean EuroQol and analogue pain scores between the two groups. Prompt drainage of the collection system under these circumstances is considered mandatory, even through in some cases infection may not subsequently be proven. The choice of drainage modality, percutaneous nephrostomy versus ureteral stent placement, has been debated, but no clear evidence demonstrates superiority of one modality over the other with regard to clinical parameters. Consequently, the choice of drainage modality is left to the discretion of the clinician and should take into account patient preference, availability of an operating room or interventional radiologist, the size and location of the stone, and the subsequent surgical plan for definitive treatment. Kidney stones: a global picture of prevalence, [3] Trinchieri A, Coppi F, Montanari E, Del Nero A, Zanetti G, Pisani E. Study on the prevalence and incidence of urolithiasis in Germany comparing the years 1979 vs. Temporal trends, practice patterns, and treatment outcomes for infected upper urinary tract stones in the United States. Surgical decompression is associated with decreased mortality in patients with sepsis and ureteral calculi. Emergency Management of Ureteric Obstruction 73 [14] Yoshimura K, Utsunomiya N, Ichioka K, Ueda N, Matsui Y, Terai A. Emergency [15] [16] [17] [18] [19] [20] [21] [22] [23] [24] [25] [26] [27] [28] [29] [30] [31] drainage for urosepsis associated with upper urinary tract calculi. Single centre review of radiologicallyguided percutaneous nephrostomies: a report of 273 procedures.
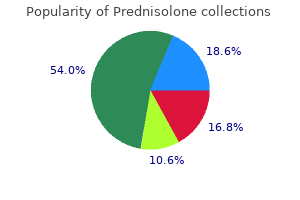
Three double-blind studies (The French Clozapine Parkinson Study Group 1999; Jones and Stoukides 1992; the Parkinson Study Group 1999; Pollak et al allergy symptoms of amoxicillin purchase prednisolone now. Moreover allergy testing wiki cheap prednisolone 10 mg on-line, these doses were not associated with an increase in tremor and rigidity allergy forecast paris france order prednisolone from india. Schizophrenia in Children and Adolescents Two randomized controlled trials from the National Institute of Mental Health have evaluated the effectiveness of clozapine in childhood-onset schizophrenia allergy vs sensitivity vs intolerance order prednisolone 40 mg without a prescription. Although there were substantial differences favoring clozapine cat allergy symptoms yahoo prednisolone 40 mg overnight delivery, the differences were statistically significant only for negative symptoms. The small sample (n=12 for clozapine and n=13 for olanzapine) was a limiting factor for obtaining statistical significance. Nevertheless, these studies suggest an important role for clozapine in younger patients with schizophrenia with refractory symptoms. Augmentation Strategies in Partial Responders to Clozapine A number of studies have evaluated augmentation strategies for individuals who are partial responders to clozapine. The most-studied antipsychotics added to clozapine were risperidone and aripiprazole, and the most-studied mood stabilizer was lamotrigine. Although some of the studies reported positive findings, none of the strategies was viewed as having adequate empirical support. Augmentation with electroconvulsive therapy has been shown to be more promising, with a recent prospective, randomized study demonstrating a 50% response rate in patients treated with clozapine who received electroconvulsive therapy compared with those who received only clozapine (Petrides et al. Maintenance Therapy in Schizophrenia Clozapine use has largely been confined to patients with treatment-refractory schizophrenia. As a result, clozapine has not been studied in traditional relapse prevention designs in which patients who are stable are randomly assigned to either clozapine or a comparator. Patients taking clozapine experienced fewer relapses and rehospitalizations than they did in the year prior to being changed to clozapine. A study in the state hospitals in Connecticut compared patients who were assigned to clozapine with patients who were maintained on their usual antipsychotics (Essock et al. Although clozapine did not result in a greater likelihood of hospital discharge, patients who were treated with clozapine had a higher likelihood of remaining in the community following discharge. This finding supports the observation that clozapine is associated with a reduced risk of relapse compared with conventional antipsychotics. Department of Veterans Affairs Cooperative Studies Program compared haloperidol and clozapine in patients with treatmentrefractory schizophrenia (Rosenheck et al. This study was not designed as a relapse prevention trial but rather as a comparison of the two agents in individuals who were poor responders to conventional therapy. However, the 1-year study is somewhat informative about the usefulness of the two drugs in patients living in the community. Fifty-seven percent of the patients taking clozapine completed the study, compared with only 28% of the patients taking haloperidol (P<0. In addition, clozapine-treated patients had fewer mean days of hospitalization (143. Other Indications Clozapine may also help patients with polydipsia-hyponatremia syndrome (Canuso and Goldman 1999). Patients with this syndrome tend to intoxicate themselves through excessive water drinking, and the resultant hyponatremia may result in seizures. Side Effects and Toxicology Hematological Effects the side effects of clozapine make it one of the most challenging medications for psychiatrists to prescribe. The main factor that limits its use is the potential serious side effect of agranulocytosis. In 1975, there were 17 cases of agranulocytosis in Finland, and widespread use of the medication for the treatment of schizophrenia was temporarily halted (Amsler et al. Agranulocytosis is a potentially lethal side effect that occurs in less than 1% of patients treated in the United States (Alvir et al. In a review of the morbidity and mortality of clozapine-treated patients (Honigfeld et al. When clozapine treatment is discontinued upon identification of marked leukopenia, patients usually recover within 1424 days and without any longterm consequences. However, rechallenging patients who have experienced agranulocytosis almost always leads to recurrence of the problem. In nine patients who were known to be rechallenged, the average time to onset of the second episode was 10 weeks shorter (14 weeks) than for the first episode (24 weeks) (Safferman et al. Cardiac Effects Well-known side effects of clozapine on the cardiovascular system include tachycardia, bradycardia, syncope, and orthostatic hypotension. Tachycardia is thought to be attributable to the anticholinergic activity of the medication at the M2 receptor, leading to vagal nerve inhibition, hypotension is due to adrenergic blockade, and bradycardia is thought to be neurally mediated reflex bradycardia, also known as the vasovagal response. The forms of cardiovascular toxicity that are of greatest concern, however, are clozapineassociated myocarditis and cardiomyopathy. In January 2002, Novartis reported that there had been 213 cases of myocarditis, 85% of which occurred at recommended dosages of clozapine within the first 2 months of therapy (Novartis 2002). The presence of eosinophilia in many of the reported cases indicates that an immunoglobulin E (IgE)mediated hypersensitivity reaction may be involved (Kilian et al. Novartis (2002) also reported 178 cases of clozapine-associated cardiomyopathy, 80% of which were in patients younger than 50 years. Almost 20% of the incidents resulted in death, an alarming figure that may reflect delay in diagnosis and treatment. A later review spanning the years 1970 through 2004, however, indicated that overall the rate of potentially fatal cardiomyopathy or myocarditis was between 0. The detection of cardiac toxicity is challenging, because its manifestations (tachycardia, fatigue, and orthostatic hypotension) are frequently observed in clozapine-treated patients, particularly when alterations in dosage are made (Lieberman and Safferman 1992). The poor specificity of signs for cardiac toxicity demands that patients with any personal or family history of heart disease be identified, and the threshold for medical evaluation of patients developing respiratory and cardiovascular symptoms must be low (Wooltorton 2002). Therefore, we recommend monitoring of erythrocyte sedimentation rate and/or C-reactive protein, eosinophil count, and troponins on a weekly basis for the first 4 weeks of therapy (Freudenreich and McEvoy 2016). For hypotension caused by clozapine, we also recommend a slow upward titration of the medication and monitoring of orthostatic vital signs during the first weeks of therapy. Patients should be educated about the risk of orthostatic hypotension and should be taught to rise slowly from supine positions. Concomitant treatment with -blocking agents may be necessary for persistent tachycardia. However, the use of -blockers may exacerbate the hypotensive effects of clozapine and should be used cautiously. Metabolic Effects Weight Gain Weight gain has been observed in both premarketing and postmarketing trials of clozapine (Henderson 2001; Simpson and Varga 1974; Wirshing et al. The weight gain observed with clozapine seems to occur for a prolonged period of time-up to 40 weeks. In one naturalistic study, Henderson (2001) observed patients in a clozapine clinic for 5 years and noted weight gain occurring for up to 46 months in some patients. The numbers of patients assessed in the analyses were small, with only 45 patients in the clozapine group, 17 in the olanzapine group, 14 in the quetiapine group, and 14 in the risperidone group. Although the differences in weight gain among these agents were not statistically significant, they were interesting, with patients taking clozapine gaining a mean of 0. Diabetes the weight gain observed with clozapine can place patients at risk for significant health problems. Numerous case reports have linked clozapine with new-onset diabetes (Wirshing et al. Patients treated with clozapine should be routinely screened for diabetes and other metabolic abnormalities, including raised lipid levels. Reports and clinical experience suggest that in a case of antipsychotic-associated diabetes or diabetic ketoacidosis, discontinuation of the antipsychotic agent may result in reversal of the hyperglycemia and diabetes. During clozapine therapy, we recommend monitoring fasting glucose, cholesterol, and lipids at baseline and every 6 months thereafter. Prevention of weight gain with clozapine, through nutrition and diet counseling, is recommended. Screening questions by physicians that we find useful include the following: "Have you noticed if your belt or pants size has changed In 2004, in response to growing concern that the majority of antipsychotic medications may be associated with weight gain and other metabolic changes, the American Diabetes Association and other groups published a set of guidelines for monitoring weight, glucose, and lipids (American Diabetes Association et al. Also in 2004, a very comprehensive literature review was conducted by Marder et al. Labeling changes were made for all antipsychotic medications, including clozapine, regarding these metabolic risk factors. Seizures A well-known side effect of clozapine treatment is the risk for seizures, which are thought to occur in 5%10% of patients treated with this medication (Welch et al. The cause of seizures is unclear, but it is generally thought that rapid escalations in dosage and possibly high plasma levels of clozapine may account for the development of seizures (Klimke and Klieser 1995). Clozapine-associated seizures occur most often at dosages greater than 600 mg/day. The relationship between clozapine plasma levels and seizures is somewhat inconsistent in the literature (Simpson and Cooper 1978; Vailleau et al. The anticonvulsant agents sodium valproate, gabapentin, and topiramate have been used successfully to treat clozapine-induced seizures (Navarro et al. Topiramate has an advantage over sodium valproate in that it is associated with very little weight gain. In cases in our clinic where patients have developed seizures while taking clozapine, we institute rapid loading with anticonvulsant medication and temporarily discontinue the clozapine treatment. We then slowly reintroduce and retitrate the clozapine once the patient is taking an adequate dose of anticonvulsant medication. Constipation can be a difficult but important side effect to manage in severely mentally ill individuals, who may not complain about the problem until a medical emergency, such as acute bowel obstruction, occurs. We are less inclined to recommend treatments involving bulking agents, particularly in the setting of poor fluid intake. Other Side Effects Sedation is one of the most common and difficult side effects of clozapine to manage. Patients with sedation often do not want their dosages increased and will complain of sedation as one of the most annoying consequences of clozapine treatment (Angermeyer et al. In our experience, sedation is usually the limiting factor controlling both the rate at which the dose of clozapine can be increased and the maximum dosage the patient can tolerate. There have been several reports of respiratory arrest or depression during the early stages of treatment with clozapine (Novartis 2002). Two of the patients who experienced respiratory arrest were concomitantly taking benzodiazepines. Sialorrhea is a commonly reported side effect of clozapine (occurring in over 50% of patients) that can be problematic for patients. The etiology of sialorrhea is unclear, but the condition does not seem to be caused by the dopamine blockade. Case series and small pilot studies indicate that treating sialorrhea with antiadrenergic agents, such as the clonidine patch, or anticholinergic agents, such as benztropine and intranasal ipratropium bromide, or atropine ophthalmic drops administered sublingually, may be successful (Calderon et al. We generally recommend that patients sleep with a towel on their pillow, as this side effect seems to be most bothersome during the night. Unfortunately, the use of concomitant antiadrenergic or anticholinergic agents adds to the potential side-effect burdens of hypotension and constipation, respectively. Neuroleptic malignant syndrome, a syndrome of unknown etiology that includes hyperthermia, autonomic instability, and severe rigidity, has been reported in several patients treated with clozapine (Anderson and Powers 1991). The etiology of neuroleptic malignant syndrome that occurs in the context of clozapine use, as well as that occurring with use of conventional antipsychotics, remains unclear. Hepatotoxicity has been reported with clozapine, especially in the setting of polypharmacy (Macfarlane et al. Asymptomatic elevation of transaminase levels was observed most commonly, affecting between 30% and 50% of patients treated with clozapine. Although serious toxicity is rare, prescribers of clozapine should be aware of its hepatotoxic potential. Sexual side effects, including priapism and impotence, have been reported with clozapine. Urinary retention and bladder dysfunction can also result from treatment with clozapine. Although this daunting array of side effects-along with the management of the risk of agranulocytosis-makes the treatment of patients with clozapine complex, it is common for patients to report a sense of relief from the dysphoric moods they experienced while taking conventional antipsychotics. Discontinuation and Reinitiation (Rechallenge) As summarized in their 2013 review, Nielsen et al. Seizures should not be an absolute contraindication to clozapine treatment, because they may be managed by initiation of an anticonvulsant either prophylactically prior to initiation of clozapine or by stabilization of seizures prior to initiation of clozapine. If and when a clinician opts to restart clozapine in any patient, regardless of the circumstance, they must begin at 12. If the patient has not experienced adverse effects from clozapine in the past, the reinitiation dose may be titrated upward more rapidly than their initial titration. Cytochrome-related problems can be avoided by monitoring clozapine plasma levels while gradually increasing clozapine from a low starting dose. Conclusion Clozapine maintains an important place in the treatment of severe psychosis. Side effects, including agranulocytosis, cardiomyopathy, seizures, sedation, and weight gain, make it the most difficult antipsychotic to prescribe. For this reason, clozapine should be reserved for patients who have not responded to one or more other antipsychotics. On the whole, however, this very effective treatment is underutilized in most communities. References Alawami M, Wasywich C, Cicovic A, Kenedi C: A systematic review of clozapine induced cardiomyopathy.
5 mg prednisolone purchase otc. THE LIST - GLUTEN INTOLERANCE CURED! TRUTESTER.COM.
References
- Kasakov L, Burnstock G: The use of the slowly degradable analog, alpha, beta-methylene ATP, to produce desentitisation of the P2-purinoceptor: effect on non-adrenergic, non-cholinergic responses of the guinea-pig urinary bladder, Eur J Pharmacol 86:291, 1982.
- Ohshima H, Bartsch H. Chronic infections and inflammatory processes as cancer risk factors: possible role of nitric oxide in carcinogenesis. Mutat Res 1994;305(2):253-64.
- Lichtenstein IL, Shore JM: Simplified repair of femoral and recurrent inguinal hernias by a iplugi technique. Am J Surg 128:439, 1974.
- Salonia A, Eardley I, Giuliano F, et al: European Association of Urology guidelines on priapism, Eur Urol 65:480n489, 2014.
- Villablanca AC, McDonald JM, Rutledge JC. Smoking and cardiovascular disease. Clin Chest Med 2000; 21:159.
- Liang BA, Zivin JA. Empirical characteristics of litigation involving tissue plasminogen activator and ischemic stroke. Ann Emerg Med. 2008;52(2):160-164.
- Abs R, Verhelst J, Maiter D, et al. Cabergoline in the treatment of acromegaly: a study in 64 patients. J Clin Endocrinol Metab 1998; 83(2):374-378.
- Ha JW, Chung N, Chang BC, et al: Acute mitral regurgitation due to leaflet tear after balloon valvotomy, Circulation 98(19):2095-2097, 1998.
