
Sotalol
| Contato
Página Inicial
Andrew R. Banker, DDS, MD
- Assistant Professor
- Department of Oral and Maxillofacial Surgery
- Louisiana State University Health Sciences Center
- Shreveport, Louisiana
If the cornea becomes dry pulse pressure of 100 sotalol 40 mg mastercard, thinning of the cornea will result in loss of surface epithelium and cause a dellen formation hypertension jnc 40 mg sotalol buy, which can be seen on slit-lamp examination with fluorescein uptake blood pressure and anxiety discount sotalol 40 mg buy on line. Ophthalmic antibiotic ointment arrhythmia in 7 year old buy genuine sotalol on-line, patching blood pressure drops after eating 40 mg sotalol order visa, and drainage of the chemosis will be required to correct the mechanics. Dryness and exposure lead to desiccation of nonkeratinized mucosal epithelium on the surface of the conjunctiva. A cyclic relationship of chemosis causing conjunctival prolapse and chemosis-induced lagophthalmos requires intervention for treatment. Chemosis associated with lid malposition or chronic chemosis resulting from abnormal eyelid closure biomechanics requires surgical correction of eyelid position and function before the chemosis can be resolved. Furthermore, when blepharoplasty is combined with a face-lift or midface-lift procedure, there is increased periorbital edema, thereby increasing the risk for chemosis. There continues to be a need to define the structural damage that may occur to lymphatic channels draining the conjunctiva Chapter 17 · Management of Chemosis 471 during blepharoplasty from a skin-muscle flap and lateral canthal dissection. Therefore chemosis is found after transcutaneous lower blepharoplasty as well as transconjunctival lower blepharoplasty. The incidence of chemosis is the same, whether a canthopexy or canthoplasty is performed. There does not appear to be a significant increase in long-term chemosis despite the use of routine lateral canthal support. If the chemosis appears to be mild and additional surgery such as a face lift is planned, ophthalmic ointment can be liberally applied during surgery; then a moistened eye pad can be taped to the closed eyes using a Steri-Strip from the forehead to the cheek. Patients will be able to open their eyelids enough to see during the first 7 days after surgery. The interim marginal temporary tarsorrhaphy suture is removed on postoperative day 7, along with other blepharoplasty sutures that require removal. For more severe cases of chemosis that are recognized at the time of surgery, 6-0 plain catgut suture can be used within the fornix to plicate the loose conjunctiva and prevent outward herniation. D, A one-snip conjunctivotomy is performed, with drainage of the chemosis fluid either intraoperatively or postoperatively. Continued use of ophthalmic ointment and patching the eye closed at night, with Steri-Strips applied to help support the lower eyelid, will shorten the recovery period. This conservative technique corrects chemosis by restabilizing the conjunctival vasculature and reducing inflammation. In some mild cases, the chemosis can be immediately corrected during the office visit. Patients are instructed to continue to use the eyedrops, combined with patching the eyelids for 24 hours if possible; otherwise, at night. The eyepatch must be done properly to completely close the eyelids without irritating the cornea with the patch. Moderate chemosis is similarly treated with the addition of systemic antiinflammatory medications such as methylprednisolone (Medrol Dosepak) and a mild compressive wrap (Ace bandage) to create increased pressure to promote lymphatic drainage. For severe chemosis, if the conjunctiva impairs the ability of the eyelids to close causing chemosis-induced lagophthalmos, drainage with conjunctivotomy can be performed in the office. The one-snip conjunc- Chapter 17 · Management of Chemosis 475 tivotomy is then performed, draining as much of the edema as possible, followed by Neo-Synephrine 2. Systemic antiinflammatory medications should be considered along with patching for at least 2 to 3 days. B, Ophthalmic ointment and oval eye pads are applied, and the eyelids are taped closed with generous use of tape from the forehead to the cheek. A cycle of dryness and conjunctival irritation begins, resulting in an exposed dry cornea that can result in a dellen sign on slit-lamp examination and adjacent chemosis. Epithelial irritation will begin with fluorescein staining of the cornea indicating further irritation and inflammation which may stimulate chronic chemosis. If there does not appear to be chronic red inflammation, antiinflammatory medications will not be helpful. Another cause of chronic chemosis is abnormal eyelid biomechanics that inhibit normal eyelid closure. Although there may be no obvious evidence of lower lid malposition, chemosis may be from upper and lower eyelid dysfunctional closure biomechanics, which has been described as fishmouthing. Chronic cases of chemosis require early diagnosis and intervention, with surgical correction of malposition, lagophthalmos, eyelid closure problems, or lower lid laxity. B, Correction of chronic chemosis with drill-hole canthoplasty and restoration of normal eyelid closure. B, Alternatively, lidocaine without epinephrine may be used as a local anesthetic and to billow the chemosis. C, Phenylephrine is used after a conjunctivotomy to cause constriction of the chemosis, then ophthalmic antibiotic ointment is applied. However, because almost all cases resolve over time, it can be considered swelling of the periorbital region, which occurs after 100% of blepharoplasties. Persistent chemosis becomes a complication when soft tissue bruising and swelling has subsided, yet the clear or yellow conjunctiva remains obvious. There are no risks associated with chemosis; however, it is an annoying complication after blepharoplasty, because it is certainly unaesthetic and clearly makes the patient feel that healing is delayed or problematic. Conjunctivochalasis is a predetermining factor of chemosis, and patients should be prepared for this. If chemosis is present in the operating room, a temporary lateral tarsorrhaphy suture for a week or two is used to keep the conjunctiva covered and prevent drying, which is the main cause of chemosis. Secondary causes may be surgical disruption of lymphatics or reaction to preservatives in eyedrops. Assuming the lower lid position is normal and there is no lagophthalmos, chemosis is generally self-limiting. Liberal use of preservative-free over-the-counter eyedrops such as GenTeal during the daytime and lubricating ointment at night is recommended. If there is chemosis-induced lagophthalmos, a conjunctivotomy can be performed in the office and will immediately cure the patient. Presented at the Fifth Annual Oculoplastic Symposium of the Southeastern Society of Plastic Surgery, Atlanta, Jan 2012. Sentinel node biopsy in patients with conjunctival and eyelid cancers: experience in 17 patients. The histopathology of experimental dry spots and dellen in the rabbit cornea: a light microscopy and scanning and transmission electron microscope study. Postoperative chemosis after cosmetic eyelid surgery: surgical management with conjunctivoplasty. The comprehensive management of chemosis following cosmetic lower lid blepharoplasty. Kosowski Key Points · the periorbital region, like the rest of the face, can be rejuvenated and improved with nonsurgical treatments. Understanding the layers of the skin and how the skin reacts to different topical treatments provides the key to individualized management. Younger and younger patients are requesting regular, small, nonsurgical treatments from plastic surgeons with the intent of delaying or possibly avoiding future surgical intervention. For a new practice, offering a larger menu of nonsurgical rejuvenation options can be a great way to expand the patient base and increase supplemental income. In this chapter, we introduce chemical peeling, mechanical and energetic dermabrasion and skin resurfacing, and general skin care, and we discuss how to expand their use in the modern plastic surgery practice. These cells become more superficial within the layers of the skin as they mature, and they ultimately die and slough from the surface. The remaining minor cell types of the skin are melanocytes, which produce melanin for pigment and ultraviolet ray protection; antigen-presenting Langerhans cells or dendritic cells; and somatosensory Merkel cells. An extracellular lattice of lipids surrounds and organizes these cells into four distinct layers (five in the glabrous skin of the hands and the soles). The outermost layer, which is the stratum corneum, is composed of terminally differentiated and cornified keratinocytes (corneocytes). This layer is constantly turned over as a result of the shedding and regeneration of the deeper layers. The next layer, the stratum granulosum, contains live keratinocytes that appear granular because of the keratohyalin granules within the cytoplasm of its cells; this is the layer that is chiefly responsible for extracellular lipid production. Keratinization begins in the stratum spinosum, and the stratum basale can be thought of as the "stem cell layer" of keratinocytes. The reticular dermis is composed of more densely packed collagen than the reticular layer, and it is the deepest layer of the dermis. The patient is asked to describe his or her concerns, problem areas, and goals to determine whether a surgical or nonsurgical modality would be preferable. Skin care that includes a basic regimen should be customized for each patient to prevent further sun damage and age-related changes and to begin the process of photoaging treatment. Similarly, the patient should be asked about his or her current skin care regimen, level of sun exposure, and use of sunscreen. Although the use of tretinoin is common, it is often used alone rather than in combination with the other skin care products that are necessary to provide optimal results. This is also important information to have if a chemical peel is planned, because the use of tretinoin may predispose the patient to a deeper peel than would occur in a patient who had never used it. Because hormone replacement therapy and oral contraceptives predispose patients to hyperpigmentation, they should be discontinued 3 to 6 months before skin rejuvenation therapy, if possible. Hormones can be safely used throughout nonsurgical and surgical treatments, as long as proper skin care is also used to prevent the risk of hyperpigmentation. If a patient discontinues hormone replacement therapy, it can be resumed 3 to 6 months after treatment with minimal risk of dyspigmentation. If the patient has a history of oral herpetic infection, prophylaxis with acyclovir is necessary before and after any surgical or nonsurgical procedure. A common regimen includes acyclovir (Zovirax; 200 mg three times daily) for 2 days before the procedure and for 2 weeks after treatment or until reepithelialization has occurred. Valacyclovir (Valtrex; 500 mg twice daily) or famciclovir (Famvir; 250 mg twice daily) can also be used. Doctors should be able to rely on their nurses to discuss the importance and proper use of skin care products. Patients who are new to skin care will not be consistent with a complex routine; they should be given essential products that offer predictable results. Patients will also need step-by-step instructions on how much of each product to use and when to use it. Chapter 18 · Nonsurgical Periorbital Rejuvenation 487 There are four products that make up what we consider to be essential skin care: 1. Tretinoin (Retin-A): this product is used in the evening for the stimulation of basal cell turnover to reverse and prevent aging. Vitamin C: this antioxidant is applied in the morning to protect the skin and prevent photoaging. Hydroquinone: this product is used in both the morning and the evening to decrease melanin production, which prevents and reverses sun damage. Sunscreen: Sunscreen with a sun protection factor of 15 or higher prevents photoaging and protects the skin when it is applied each morning. Other products can enhance the effects of these four, but the first goals are simplicity and patient compliance. Aging-related skin changes are caused by many factors that have the same results: cellular photodamage and abnormal cell growth with dyspigmentation. Skin aging and sun damage are the products of two processes: (1) intrinsic or chronologic aging, which is mainly genetic, and (2) extrinsic aging from environmental stressors such as sun exposure, smoking, systemic toxins, and free radical damage. Skin damage caused by the sun and the environment can be stopped and reversed over time. Patients must understand that sun damage is the result of decades of cumulative photoaging. Physicians need to provide patients with the tools and routines that will improve overall skin health. If a practice is new to skin care or perhaps considering starting a skin care line, the products discussed in this chapter provide a good foundation. The four essential products that we recommend have been scientifically proven to reverse and prevent damage and to protect the skin when they are of the appropriate prescription grade and strength. Retin-A Tretinoin is topical vitamin A, and it is most commonly marketed as Retin-A. Retin-A has been used clinically for the past 50 years for the treatment of acne and photoaging. This improves the appearance of the skin by reducing fine lines, wrinkles, and sunspots, and it brightens and evens the overall complexion of the skin. Photodamage involves fine and coarse wrinkles, mottled pigment, uneven skin tone, and rough skin texture. Several factors must be addressed to improve the effects of photodamage on the skin. Clinical studies involving histologic data have reported significant improvement as evidenced by increased epidermal thickness; a more compact stratum corneum; a decrease in the amount of melanin being produced, with a concomitant decrease in sun-induced hyperpigmentation; and the organization of collagen, increased fibroblast growth, procollagen synthesis, and elastin fibers. Retin-A has also been shown to cause molecular changes in the skin by increasing the level of keratolytic activity, inhibiting the production of matrix metalloproteinase, and stimulating collagen synthesis. Significant clinical and histologic experimental evidence supports the use of Retin-A for the reversal of photoaging. The ideal strength of Retin-A should be individualized for each patient, with a gradual increase in the frequency, strength, and amount of application. Patients should be careful to follow physician recommendations when beginning a round of treatment.
Flaps are not compulsory and the inferior position angles the Jones tube below the middle turbinate and toward the septum without direct end-to-end contact with the septal mucosa prehypertension mayo clinic purchase sotalol american express, which can cause distal obstruction pulse pressure pv loop purchase sotalol without a prescription. C arrhythmia emedicine purchase sotalol master card, the anterior middle turbinate is partially removed at the time of Jones tube placement if it obstructs the correct position of the tube blood pressure for athletes 40 mg sotalol buy with amex, and intranasal clamping of the tip of the middle turbinate is done useless eaters hypertension zip buy cheap sotalol 40 mg on line, followed by direct excision with Bovie cautery. This can be done with the use of a nasal speculum for visualization and does not require endoscopic assistance. If the anterior tip of the middle turbinate lies at the level of the surgical ostium, a partial middle turbinectomy should be performed. Local anesthetic with epinephrine is injected into the anterior portion of the turbinate. The soft tissue anterior tip blocking the entrance of the Jones tube is clamped and excised with the Bovie set on coagulation. This also takes advantage of gravity and capillary action to maximize efficient tear drainage. Chapter 39 · Lacrimal System and Treatment of Epiphora 1145 the tip of a 14-gauge intravenous Teflon-sheathed needle is positioned in the medial canthus 2 mm behind the skin-mucosal junction and angled 35 degrees medially and downward. The needle is pushed through the medial canthal tissues into the lacrimal sac and through the surgical ostium. This can initially be created with a needle guide, followed by straight iris scissors, a Beaver blade, or a Tooke corneal knife to enlarge the tract. The trajectory of Jones tube placement should be downward and inward to position the tube so it will drain properly with gravity and blinking. F, Once the length and diameter are determined, a straight Jones tube can be inserted, using a small lacrimal probe as a guide. The position is verified as downward and inward with the proximal funnel rotated slightly outward at the most dependent position of the inferior fornix to drain the tears. The length of the Jones tube should extend well into the nose without touching the septum. Initially, the collar size should be as large as can be tolerated without rubbing on the eye. As the tube becomes well seated, it is not unusual to need a shorter length or smaller collar size. Straight tubes are commonly used, but we prefer angled tubes to be able to avoid the middle turbinate. A spectrum of tube sizes should be available in Pyrex glass, as well as tubes with collared holes for suturing the tube to the fornix. Tubes with Porex polymer collars are also used; this will prevent movement or expulsion of the tube by formation of tissue ingrowth, which will hold the tube in place. Once the tube is in position, it should be fixed in place during the healing period to avoid postoperative dislodgement. A common method is to pass a suture of braided nylon 4-0 Mersilene through the tube and suture this to the inner canthus. This photograph shows a straight Jones tube with a Mersilene suture looped through the tube and tied at the flange for suturing to the canthus. Alternatively, newer tubes have a small hole in the flange that allows the tube to be sutured into proper position and prevent displacement. I, Once the Jones tube is properly placed through the rhinostomy with the Mersilene sutures in place, the flange can be seated within the area of the excised caruncle and sutured in place until healing has occurred. The suture can be easily and completely removed after 2 to 3 months of normal healing. The loop should not be too loose, because it is prone to being accidentally caught and can be pulled. This is less ideal than the tubes, which have a direct suture hole or a sleeve of Medpor to minimize displacement. K, this Jones tube has a small sleeve of Medpor at the waist of the flange that allows friction and tissue ingrowth for theoretical decrease in long-term tube malposition. Canine bites commonly have been reported to involve avulsion of the canalicular system and puncta, often with no ocular injury. This boy sustained a dog bite to the inner canthus that damaged his proximal canaliculi, resulting in no lacrimal drainage, but the canalicular damage was completely corrected with positioning of a Jones tube. B, A closeup side view of the child showing proper positioning of the Jones tube in the inner canthus, with minimal visibility and no contact with the ocular surface. The patient should also be encouraged to aspirate water or saline solution through the tube daily on a long-term basis to prevent protein buildup. However, the surgeon must be willing to follow up on the patient over the long term. Commonly, conjunctival revision at the collar of the tube or change in links or position of the tube may be needed. Tube replacement may be as easy as placing a straight probe through the passageway as a guide for the replacement tube. In any case, care must be taken not to break the tube with manipulation, which would lead to subsequent difficulties. Drainage problems are usually avoided by proper placement of the tube in the nose. The tube should not be against the turbinate, septum, a polyp, or the lateral wall of the nose. A tube against solid tissue may migrate or not function, so the tube must be shortened, moved, or given clearance by resecting the offending nasal anatomy. Similarly, the tube should be protected with gentle finger pressure when the patient sneezes or gently blows his or her nose, since these actions can cause the tube to extrude. Occasionally, patients have done well with an epithelialized tract without the tube. Infection of the conjunctiva from the direct connection with the nose needs treatment as indicated. Various alternative tubes have been introduced, but we strongly advocate the Jones tube. The Thornton tube is a plastic tube placed down the nasolacrimal duct into the nose. The angled silicone Reinke tube passes from the caruncle into the nose through a dacryocystorhinostomy ostium. These tubes are being mentioned only to discourage their use because of their lower success rates. The patient is instructed to irrigate the tube daily by instilling several drops of saline solution into the medial cul-de-sac and inhaling deeply with the opposite nostril occluded. If the tube becomes occluded, it can be flushed with saline solution through a lacrimal cannula, and if necessary, cleaned by passing a No. If significant septal deviation is present, it should be corrected before lacrimal drainage surgery. The middle turbinate occasionally extends forward, and if not resected, there may be insufficient space for the tube. Lateral migration of the tube: this may be seen with a tube that is in contact with the septum or one that is too long. The tip of the tube should be resting at least 2 to 3 mm from the nasal septum to avoid obstruction of tear flow. Medial migration of the tube: Loss of the tube into the medial canthal tissues occurs from laxity of the tissues and poor support of the tube. Granuloma formation or conjunctival overgrowth: Conjunctival granulomas around the Pyrex tube can occur and may sometimes be so extensive as to completely obstruct drainage. Closure of the soft tissue opening: If possible, a lost tube should be replaced within 1 week. If the tube cannot be replaced, a new opening is created, as before, with a Teflon-sheathed intravenous needle, without the need for repeat dacryocystorhinostomy. Septal and turbinate swelling: Recurrent swelling should be treated with routine nasal decongestants to shrink the mucosal swelling. Indications include: · Patients with dacryocystitis who do not have epiphora · Patients with lacrimal sac tumors the usual presentation of lacrimal sac tumors is a firm lacrimal mass above the level of the medial canthal tendon, a chronic dacryocystitis that irrigates freely, or bloody tears or bloody reflux with irrigation. With epithelial tumors of the lacrimal sac, it is necessary to surgically excise the entire sac and nasolacrimal duct with burring of the bony canal. A simple dacryocystectomy may be performed under either local or general anesthesia. Lidocaine with epinephrine will aid hemostasis and is infiltrated around the lacrimal sac. The periosteum of the anterior lacrimal crest is incised and the periorbita and lacrimal sac are reflected laterally out of the lacrimal sac fossa. Subcutaneous tissue attachments to the sac are dissected, including the fibers of the inferior oblique muscle origin and the superior and inferior preseptal muscles, to mobilize the entire body and fundus of the lacrimal sac. Needle Bovie cautery or Westcott scissors are then used to excise the sac superiorly at the level of the common canaliculus and inferiorly to the level of the nasolacrimal duct as it enters the bony canal. The foregoing procedure is adequate to cure the patient with dacryocystitis without epiphora. If a tumor is suspected, a frozen-section biopsy of the lacrimal sac must be submitted. In the presence of an epithelial tumor of the lacrimal sac, the entire lacrimal sac and nasolacrimal duct must be excised. To drain transantrally, the bony nasolacrimal canal is visible as a prominence under the sinus mucosa. The bone is removed with bone-biting Kerrison forceps to expose the nasolacrimal duct, which is then removed in its entirety. This procedure has recently been modified using a transcanalicular miniature fiberoptic light source and a laser-assisted rhinostomy opening guided by a nasal endoscope. LacriMaL prObLeMs in the newbOrn Newborns have tear secretion at birth, and 96% to 98% have totally patent and functional lacrimal drainage systems. The 2% to 4% who do not have lacrimal drainage systems intact have a thin residual membrane at the distal end of the nasolacrimal duct that will dissolve spontaneously in 80% to 90% of patients within the first few months of life. Clinical manifestations of congenital nasolacrimal duct obstruction include the following: Amniocele Amniocele occurs in the newborn as a distension in the lacrimal sac. Amniotic fluid enters the sac and is retained by a nonpatent nasolacrimal duct and is trapped in the sac by the valve at the common canaliculus, the valve of Rosenmüller. Chapter 39 · Lacrimal System and Treatment of Epiphora 1153 Dacryocystitis (Acute Mucocele or Pyocele) Dacryocystitis also exhibits acute distension and inflammation in the lacrimal sac region and may occur in the neonatal period. Probing is necessary in newborns with acute dacryocystitis to establish drainage as soon as possible. Tearing and Mattering Newborns who have congenital dacryostenosis may not develop acute dacryocystitis with a mucocele or pyocele of the sac in the early neonatal period, but may simply have tearing with a chronic mucopurulent discharge that usually becomes manifest at 2 weeks of age. Topical antibiotics should be employed, and the parents must be instructed in the proper technique of lacrimal sac compression and massage. More than 90% of these cases will clear and become asymptomatic with conservative management. Under normal circumstances, children with mild to moderate symptoms of epiphora and lid crusting can be followed for the first year of life without serious sequelae. There is rarely any imperative reason to make probing mandatory at an early age (before 6 months of age). A number of studies have now confirmed that probing and silicone tube intubation in children older than 12 months have a very high success rate. An index finger is pressed over the common canaliculus to prevent regurgitation of material from the puncta. This finger is then stroked downward firmly to increase hydrostatic pressure within the lacrimal sac and nasolacrimal duct. Significant mucopurulent discharge is treated with a topical antibiotic ointment such as erythromycin. With medical management alone, more than 90% of congenital nasolacrimal duct obstructions will resolve within the first 12 months of life. Special "social" circumstances that may warrant lacrimal probing at an earlier age include chronic mucopurulent discharge (in which case, a daycare center may refuse to care for the child) and a 4- to 6-month-old who could be probed in the office setting. In children beyond 6 to 8 months of age, probing is generally performed under general anesthesia. The technique of probing consists of two equally important maneuvers: the passage of the lacrimal probe, and intranasal manipulation and irrigation. The probe is first introduced vertically into the punctum and ampulla and then rotated horizontally 90 degrees in the same plane, conforming to the bend in the first portion of the canaliculus. With lateral tension placed on the lid to prevent kinking of the canaliculus, the probe is then advanced until it touches against bony firmness, which means that it has reached the nasal wall of the lacrimal sac. The probe is then withdrawn slightly and rotated upward 90 de- 1154 Part V · Orbital and Lacrimal Surgery grees in the same plane, and then angulated to point 15 degrees posteriorly. It is then advanced down the nasolacrimal duct, through which it should slide easily. The probe will meet some resistance at the membranous obstruction at the distal end of the nasolacrimal duct, and a sudden "give" may occur as it pops the membrane. Attention is next directed to the undersurface of the inferior turbinate, which has previously been vasoconstricted with intranasal packing. A thin periosteal elevator is slid under the turbinate and rubbed against the probe, which has been passed down through the nasolacrimal duct. It should be noted that the probe in the lacrimal duct moves as it is touched and a metal-on-metal grating is felt and also heard ("see it, hear it, feel it"). If the turbinate is compressed over the probe, a twist of the periosteal elevator will infracture the turbinate and open the nasolacrimal duct. The probe and the periosteal elevator are then withdrawn and fluorescein-stained saline solution is irrigated into the punctum. It should travel easily down the canaliculus, lacrimal sac, and nasolacrimal duct and can be aspirated from the nasal cavity with suction apparatus.
Thereafter blood pressure 60 over 0 order sotalol pills in toronto, white cell count blood pressure for elderly sotalol 40 mg purchase overnight delivery, platelet count and liver function tests should be performed every 23 months blood pressure medication side effects cough sotalol 40 mg for sale. Under these circumstances blood pressure numbers close together sotalol 40 mg order otc, patients can be given a combination of low-dose thiopurine pulse pressure 46 generic 40 mg sotalol visa. Methotrexate acts predominantly by inhibiting the enzymes that metabolize folic acid. Although not yet proven to be effective in ulcerative colitis in formal clinical trials, methotrexate is used in many centers for patients with colitis who are intolerant of or refractory to thiopurines. As with other immunosuppressive agents, there is an increase in opportunistic infections and bone marrow depression. These side effects are reduced by coadministration of folic acid, which does not compromise the therapeutic effectiveness of methotrexate. As with thiopurines, the risk of bone marrow depression necessitates twice-weekly blood counts for the first 2 months, and thereafter every 3 months. Folic acid should also be coadministered at a dose of 15 mg/day, except on the day when methotrexate is taken. Liver biopsy is probably unnecessary, except in those with persistently abnormal © 2016 Health Press Ltd. Unexplained shortness of breath or coughing necessitates a chest X-ray, blood gas and lung function tests, particularly measurement of carbon monoxide diffusing capacity. Pregnancy and conception should be avoided within 6 months of the treatment of either partner, because methotrexate is teratogenic. Coadministration of other antifolate agents, such as trimethoprimsulfamethoxazole, may increase the toxic effects of methotrexate on the bone marrow, as may non-steroidal anti-inflammatory drugs, penicillin, old age and renal impairment. To reduce the risk of hepatotoxicity, methotrexate should not be prescribed to patients who drink more than seven units of alcohol per week, are substantially overweight or have diabetes mellitus. Ciclosporin (cyclosporine) is a fungus-derived cyclic undecapeptide useful in steroid-refractory acute severe ulcerative colitis. Intravenous therapy is usually given initially, and replaced after a few days with the oral preparation (Neoral). Close monitoring of whole blood concentrations is used to adjust ciclosporin dosage. The target levels depend on the method used for analysis and on the route of administration Table 5. Because ciclosporin is metabolized via the cytochrome P450 enzyme system, grapefruit juice and drugs that inhibit this enzyme system should be taken with caution. However, drugs that induce the cytochrome P450 system decrease blood levels of ciclosporin (see Table 5. The most serious side effects are: · opportunistic infections (in 20% of patients) such as Pneumocystis carinii pneumonia, for which coadministration of prophylactic trimethoprimsulfamethoxazole may be advisable · renal impairment, including a 20% reduction in glomerular filtration rate in most patients and, in 25%, an interstitial nephritis that is not 70 always reversible when treatment stops © 2016 Health Press Ltd. Its use demands frequent monitoring of ciclosporin blood levels and serum biochemistry. Tacrolimus is another oral macrolide immunosuppressant derived originally from a bacterium and widely used in transplant medicine. Its side effects, which resemble those of ciclosporin, include induction of diabetes mellitus. Use of tacrolimus requires careful monitoring of drug levels, blood sugar and renal function. Infliximab is usually administered using an induction regimen of infusions at 0, 2 and 6 weeks, followed by regular infusions at intervals of 8 weeks, each infusion being given over 12 hours. The standard dose is 5 mg/kg per infusion, and the cost is about $2400/£1200/2000 per infusion, depending on body weight. Adalimumab is given by subcutaneous injection at induction doses of 160 and 80 mg every 2 weeks; subsequent injections of 40 mg are given every other week, although patients who lose their initial response need to increase to 40 mg every week. Dosing is weight dependent: for patients over 80 kg, 200 mg is given at 0 weeks, 100 mg at 2 and 4 weeks, followed by 100 mg every 4 weeks; for patients less than 80 kg, the loading dose is the same, followed by a maintenance dose of 50 mg every 4 weeks. These agents are of moderate efficacy in refractory outpatient ulcerative colitis, and infliximab has been shown to halve the colectomy rate in inpatients with steroid-refractory acute severe colitis (see Chapter 7). Common side effects associated with the infusion of infliximab include headache, rash, nausea and fever (see Table 5. However, antihistamines, adrenaline and corticosteroids should be on hand when infusions are given in case of anaphylaxis. Infusions should therefore be carried out in hospitals with full resuscitation facilities available, although they are routinely performed on an outpatient basis. These may reduce the efficacy of infliximab and can cause a delayed serum-sickness-like reaction, characterized by myalgia, arthralgia, rash and fever. This reaction 76 responds to prednisolone and analgesics but may contraindicate further © 2016 Health Press Ltd. Neurological complications include aseptic meningitis and irreversible demyelination. Most of these relate to the potential side effects of the treatment described above. In patients losing response to these drugs, many centers now offer tests that measure drug levels and antibodies to them, which can help to guide decisions about further treatment (see pages 1256). By blocking this interaction, vedolizumab reduces migration of pro-inflammatory lymphocytes into the gut mucosa. Vedolizumab is given as 300-mg 30-minute intravenous infusions at 0, 2 and 6 weeks and then every 8 weeks thereafter. Like infliximab, vedolizumab can occasionally induce acute infusion reactions and should therefore be given in healthcare settings where full resuscitation facilities are available; reactions should be treated as for infliximab reactions (see pages 767). The commonest side effects of vedolizumab are nasopharyngitis, headache and arthralgia. However, clinical experience over the 5 years since it was first used in patients suggests that vedolizumab may be a safer option, probably because its mechanism of action is focused on the gut through its antagonism of the 47 integrin. However, a test to measure drug levels or antibodies in patients who lose response to vedolizumab is not yet available. Because of the complexity of their manufacture, biosimilars are not structurally identical to the product that they imitate (although they are similar): neither their efficacy nor their safety is necessarily the same as that of the parent molecule. Remsima, Inflectra) are now being introduced in many parts of the world, and this usage, because of its cost © 2016 Health Press Ltd. A further consequence of the emergence of biosimilars is that all biological drugs will need to be identified by their proprietary (brand) names rather than their generic names. New therapeutic approaches the trend toward an increasing repertoire of immunomodulatory agents is set to continue. Over the next few years, several options are likely to reach the bedside, particularly for patients with disease refractory to current treatments. The most likely candidates are ustekinumab (as mentioned above), tofacitinib and mongersen (each an oral intracellular messenger inhibitor), and stem cell transplantation. In addition, several factors conspire to limit the long-term efficacy of a single therapeutic agent and create a risk of inflammatory escape with disease relapse. Such factors include the redundancy or synergistic action of inflammatory mediators, the up-regulation of various receptors in inflamed tissue, and cross-talk among different signaling cascades. This has prompted the clinical development of bispecific antibodies, which combine the specificities of two antibodies for simultaneous activity at two therapeutic targets. The emphasis on suppressing or modifying the host response may shift toward modifying the microbiome. Although this will prompt greater use of fecal microbial transplantation, considerations of safety and disease heterogeneity are likely to mandate an understanding of the minimal microbiota required for transplantation, which may vary according to the disease subset. The former applies to adjunctive therapies, while the latter applies to treatments that are used instead of standard management. The combined term comprises a heterogeneous range of diagnostic and therapeutic procedures, ranging from traditional practices such as 82 acupuncture, traditional Chinese medicine, homeopathy and herbal © 2016 Health Press Ltd. Recent surveys have shown that up to 50% of people in the Western world use complementary therapies, most commonly herbal remedies. While it is unlikely that therapies such as reflexology will have direct adverse effects, the same cannot be said of herbal therapies: adverse effects have included fatal liver toxicity as well as irreversible renal failure. The interaction of herbal therapies with conventional drugs needs further clarification. Perhaps more importantly, complementary and alternative therapies may be associated with indirect adverse effects. For example, patients who initially consult an alternative practitioner may suffer from misdiagnosis, while others may delay or forego appropriate conventional options in favor of ineffective unconventional ones. There is an urgent need for further scientific assessment of the benefits and dangers of complementary therapies. Herbal preparations, in particular, should require licensing by an independent national body in order to improve their quality and safety, while claims of effect should be validated by controlled trials. The general public, pharmacists and doctors need to be aware of the direct and indirect risks associated with the use of complementary therapies. The possibility of serious side effects, including infection and malignancy, needs to be borne in mind for all patients on these treatments. It acts by reducing the recruitment of pro-inflammatory lymphocytes to the gut mucosa. Treatment of ulcerative colitis with a humanized antibody to the alpha4beta7 integrin. Infliximab as rescue therapy in severe to moderately severe ulcerative colitis: a randomized, placebocontrolled study. Fecal microbiota transplantation induces remission in patients with active ulcerative colitis in a randomized controlled trial. Adalimumab induction therapy for Crohn disease previously treated with infliximab: a randomized trial. Azathioprine and 6-mercaptopurine for maintenance of remission in ulcerative colitis. The aims of the antiinflammatory and immunomodulatory treatments used are to induce and then maintain full clinical and endoscopic remission Table 6. It should be high quality, safe, given as close as possible to where patients live and responsive to their needs. Indeed, an integrated service, in which the patient is assessed and supported psychosocially as well as medically from diagnosis, is increasingly advocated. They should offer: · continuity of care · appropriate clinical, endoscopic and laboratory monitoring of the disease and its treatment · rapid access for patients in relapse · psychological assessment and support · a computerized patient database providing opportunities for clinical audit and research · training for doctors and nurses. Sick inpatients who are malnourished often need enteral and occasionally total parenteral nutrition. Iron and folic acid supplements are often needed, as are appropriate drugs for incipient or established osteoporosis (see Chapter 3). Antidiarrheal (loperamide, codeine phosphate, diphenoxylate), opioid analgesic, antispasmodic and anticholinergic drugs should be avoided in active colitis as they may provoke acute colonic dilation. As soon as it is suspected that a patient may need immunomodulatory or biological therapy, their serology for previous infections should be checked (see Table 4. Second European evidence-based consensus on the prevention, diagnosis and management of opportunistic infections in inflammatory bowel disease. Knowledge of the extent of disease is particularly important in relation to the feasibility of effective topical therapy, while the severity of the attack defines not only the optimal type and route of therapy, but also whether the patient can be safely treated as an outpatient or needs urgent hospital admission. Immediate admission is required for those with acute severe attacks of ulcerative colitis, defined primarily by clinical features (see Chapter 2). These include six or more bloody diarrheal stools daily, pyrexia and tachycardia (more than 90 beats/minute). Such patients will usually be systemically unwell, may be anemic and may have lost weight; very ill patients may have abdominal tenderness and/or distension. Since the initial attack of ulcerative colitis is more dangerous than subsequent ones, the threshold for admission should be lowered in those presenting for the first time with bloody diarrhea. These patients should be admitted immediately to a gastroenterology ward for close joint medical, surgical and nursing care Table 7. Early involvement of the nutrition team and of a stoma therapist in those who may need surgery is important. Establishing the diagnosis, extent of disease and its severity requires a carefully targeted history and appropriate investigations (see Chapter 4) in those presenting for the first time. In patients with established ulcerative colitis, these procedures are required to exclude infection and to assess disease extent (if not already known) and severity. In patients with established ulcerative colitis, direct questions about stool frequency, consistency and urgency, overt blood content, abdominal pain, malaise, fever and weight loss indicate the severity of the attack. The differential diagnosis may also need evaluation in those presenting with bloody diarrhea for the first time (see Table 4. Abrupt onset with fever, vomiting, epidemic or contact history and/or recent foreign travel suggests infective colitis, even in those with pre-existing ulcerative colitis. In patients presenting for the first time, non-smoking or recent cessation of smoking increases the likelihood of ulcerative colitis, while previous abdominal or pelvic irradiation make radiation colitis a strong possibility. Ischemic colitis usually shows sudden onset in older people with other features of vascular disease, and often causes marked abdominal pain as well as bloody diarrhea. Blood tests are better for establishing the activity of ulcerative colitis than for making the diagnosis or identifying its extent (see Chapter 4). The best laboratory measures of disease activity in ulcerative colitis are hemoglobin, platelet count, C-reactive protein and serum albumin. For recent travellers, serology as well as stool samples should be requested (for amebiasis, strongyloidiasis and schistosomiasis). Serum magnesium and cholesterol should be checked in case ciclosporin (cyclosporine) is needed (see Chapter 5).

Inset arteria gastrica sinistra purchase sotalol 40 mg with mastercard, Higher magnification of individual cancer cells with hyperchromatic dark nuclei hypertension goals purchase sotalol 40 mg without a prescription. B arrhythmia or anxiety order sotalol paypal, A cluster of poorly differentiated cancer cells with somewhat elongated nuclei hypertension first line purchase sotalol cheap online, pronounced atypia blood pressure medication dizzy spells generic 40 mg sotalol otc, and brisk mitotic activity in a case of small cell carcinoma metastatic to bone. C and D, Groups of loosely arranged cells forming small follicular structures characteristic of thyroid cancer. Inset, Higher magnification of thyroid follicular cancer cells with visible nucleoli. A, An axial computed tomography scan of the spine shows several osteoblastic foci of metastatic carcinoma within the vertebral body. B, Radioisotope scan shows increased uptake in widespread metastases throughout the skeleton. C, Microscopic features of metastatic poorly differentiated adenocarcinoma filling the intertrabecular spaces associated with reactive bone formation. A, Anteroposterior radiograph shows a blastic metastatic focus from an esophageal adenocarcinoma. B and C, Coronal and axial computed tomography scans highlight the blastic reaction to the metastatic deposits within the medullary cavity as well as periosteal reaction. D, Microscopic features of metastatic, moderately differentiated adenocarcinoma that originated in the esophagus. A and B, Large sheets of colonic carcinoma cells showing overlapping nuclei and focal peripheral palisading. Note that individual nuclei of tumor cells vary in size and contain coarse chromatin with prominent irregular nucleoli. C and D, Metastatic ductal breast carcinoma of the breast with cells arranged in loose clusters. Inset, Details of nuclear morphology with coarse chromatin and prominent irregular nucleoli (A-D, ×400; Insets, ×600) (A-D and insets, hematoxylin-eosin). A and B, Axial computed tomography scans show foci of metastatic carcinoma adjacent to the sacroiliac joint and within the iliac wing. C and D, Microscopically, this poorly differentiated adenocarcinoma had foci with signet-ring cell features similar to the primary tumor within the breast (C, ×200; D, ×400) (C and D, hematoxylin-eosin). Differentiation between ductal and lobular carcinoma in bone aspirates is rarely possible. Aspirates from metastatic lobular carcinoma are characterized by the presence of relatively small, oval cells with eccentric, fairly monotonous hyperchromatic nuclei. Some of these cells contain a large vacuole with central inclusion of condensed mucous material. In the rare cases without this history, the disease should be suspected in women of the appropriate age group. In fact, for such malignancies, solitary or multiple skeletal metastases are frequently an integral component of the clinical picture at presentation, especially when the primary tumor remains occult. Even if they are not evident at presentation, skeletal metastases eventually develop later during the course of the disease in this group of tumors. Carcinoma of the Prostate Carcinoma of the prostate is one of the most common human cancers, accounting for nearly 25% of all malignancies in males, and is a model for epithelial malignancy that is likely to metastasize to bone. In rare instances, massive sclerotic metastases can develop within major portions of the skeleton and are associated with pronounced periosteal new bone formation. In typical cases, the unique morphologic characteristics of well-developed small glands of prostate carcinoma are easy to recognize in metastases. The small cell carcinomas of the prostate are microscopically indistinguishable from other small cell carcinomas, such as those of lung origin. In such cases, the metastatic foci predominantly consist of sclerotic bone with scattered small clusters of tumor cells. It is postulated that prostate carcinoma stimulates new bone production by secretion of several ubiquitous kinins and pro-osteoblastic factors that drive osteoblast differentiation and bone formation. Treated prostate carcinoma can be very inconspicuous; that is, the tumor cells can mimic nonneoplastic cells such as histiocytes. In such cases, documentation of the epithelial nature of these cells with epithelial markers such as cytokeratin can aid the diagnosis. In addition to radiotherapy and bisphosphonates, a variety of radiopharmaceuticals have recently been identified to specifically treat prostate carcinoma bone metastases by homing in on bone lesions while limiting local toxicity, thus providing both palliative and survival benefits. Cancer cells have no distinguishing features and are usually large with cytoplasmic borders and nuclei with clearly visible large nucleoli. Cytologic preparations from well or moderately differentiated prostate cancer may contain recognizable microglandular structures that resemble small rosettelike formations with nuclei at the periphery and a center formed by amorphous cytoplasmic material. Carcinoma of the Kidney Renal cell carcinoma is a prototype of a tumor that frequently presents as a skeletal (often solitary) metastasis with a clinically occult primary tumor. Note that nuclei of tumor cells are uniform in size and display only minimal atypia. Inset, Higher magnification of tumor cells showing details of nuclear morphology, which contain prominent nucleoli and evenly distributed chromatin. C and D, Metastatic clear cell carcinoma of the kidney shows loosely arranged clusters of tumor cells with ill-defined clear and finely granular cytoplasm. Note mild atypia of tumor cells characterized by the presence of round to oval nuclei with clearly visible nucleoli (A-D, ×400; Inset A, ×600; Inset D, ×400) (A-D and insets, hematoxylin-eosin. Renal cell carcinomas are known to metastasize to unusual distant sites such as the skin, tongue, eye, heart muscle, acral skeleton, and breast. Renal cell carcinomas preferentially metastasize to the femur, humerus, pelvis, and spine; although osteoblastic lesions have been described,128 the vast majority are lytic. Approximately 10% of renal cell carcinomas dedifferentiate into high-grade spindle-cell or pleomorphic sarcomatoid carcinoma. Some of these lesions can have features suggesting an undifferentiated spindle-cell or pleomorphic sarcoma, and can be misdiagnosed as primary bone lesions. Review of clinical data and identification of the epithelial nature of cells with appropriate immunohistochemical markers are helpful for classifying the lesion as a metastasis. Cytologic preparations from the metastatic sarcomatoid variant of renal cell carcinoma show malignant spindle and pleomorphic cells arranged in large sheets, small clusters, or singly that may be very misleading. Nuclei show pronounced atypia characterized by irregular chromatin clumping and prominent nucleoli. In general, the cytologic features of metastatic sarcomatoid carcinoma are indistinguishable from those of primary malignant fibrous tumors of bone. Immunohistochemical stains for keratin and vimentin, combined with a clinical history of primary renal carcinoma, are helpful to establish the correct diagnosis. Welldifferentiated thyroid carcinoma can present clinically as skeletal metastases (either solitary or multiple lesions) with an occult primary tumor. Thyroid carcinomas that affect younger individuals and children are more aggressive and have a higher propensity to metastasize to the skeleton and lungs, although age greater than 55 years is a strong predictor of death following disseminated disease. Aspirates from metastatic thyroid follicular carcinoma show a uniform population of small cells lying singly in three-dimensional clusters, sometimes forming follicles with central colloid. Intranuclear cytoplasmic inclusions and nuclear "creases" are commonly seen in the spherical nuclei. Colloid can be seen as an amorphous substance dispersed in a background of the smear or can be present inside the core follicles. Cytologic features of metastatic thyroid follicular cell carcinoma are very distinctive and permit the identification of thyroid origin in the majority of cases. Carcinoma of the Pancreas Carcinoma of the pancreas is known for its poor prognosis. The lesion is low signal intensity on T1-weighted images (A) and high-signal intensity on T2-weighted images (B). C, An axial computed tomography scan shows the large lesion in the right ilium as well as a second lesion near the left sacroiliac joint. A, Anteroposterior radiograph shows a solitary lytic lesion in the proximal humeral diaphysis. B, Radioisotope scan shows a solitary focus of uptake corresponding to the lesion seen in A. C and D, Microscopically, the lesion is composed of nests of clear cells with intervening fine capillaries, typical of renal cell carcinoma (C, ×100; D, ×400) (C and D, hematoxylin-eosin). C, Gross photograph of bisected rib shows intramedullary gray-tan lesion with cortical disruption. D, Photomicrograph shows characteristic follicular growth pattern with colloid of metastatic follicular variant of papillary carcinoma of thyroid. A and B, Low power photomicrographs show a predominantly spindle-cell neoplasm with abundant collagenous stroma, interpreted on limited needle biopsy as undifferentiated carcinoma. C, the sarcomatoid component adjacent to a focus with overt epithelial differentiation. D, the epithelial component resembles the follicular variant of papillary carcinoma. Melanoma most commonly metastasizes to regional lymph nodes, but skeletal metastases also occur, most often involving axial sites such as the ribs, jaw, pelvis, and spine; appendicular metastases are encountered less frequently. Tumor cells can vary from epithelioid to spindled in appearance, and may or may not contain melanin pigment. While establishing a diagnosis of metastatic melanoma is not difficult in the setting of a known primary cutaneous tumor, the diagnosis can be extremely challenging when the primary lesion has either not been identified or has undergone regression. In the setting of an unknown primary tumor, metastatic melanoma must be distinguished from poorly differentiated carcinoma; amelanotic tumors may also be mistaken for poorly differentiated carcinoma or even sarcomas when predominately spindled in appearance. Patients with appendicular metastases seem to have slightly better survival than those with axial metastases, owing in part to a shorter interval to metastasis for the axial lesions. In addition, they more often involve the appendicular skeleton compared with the axial skeletal involvement seen in adults. Rhabdomyosarcoma, neuroblastoma, and clear cell sarcoma of the kidney are the three most notable examples of pediatric malignancies that have a particularly high propensity for metastasizing to the skeleton, a feature that represents an integral part of the clinical behavior of these tumors. Rhabdomyosarcoma Rhabdomyosarcoma can be classified into several different subtypes. Embryonal and alveolar rhabdomyosarcoma are seen mainly in the pediatric population, whereas pleomorphic rhabdomyosarcoma, a relatively rare tumor, occurs mainly in the adult population. One subtype of embryonal rhabdomyosarcoma that affects adolescents and is more frequently located in the spermatic cord is the spindlecell variant. Overall, the head and neck region, genitourinary organs, and soft tissue of the extremities are the most frequently affected sites. The alveolar variant of rhabdomyosarcoma, which more commonly arises in the extremities, has a poorer prognosis than either embryonal rhabdomyosarcoma or fusion-negative alveolar rhabdomyosarcomas193 (see below). Rhabdomyosarcoma is a highly aggressive neoplasm; however, modern multimodality treatment regimens have significantly improved 5-year survival to greater than 70%, and 5-year survival for embryonal rhabdomyosarcoma approaches 90%. Many rhabdomyosarcomas have clearly recognizable rhabdomyoblastic microscopic features and can be diagnosed with the aid of appropriate immunostains and Text continued on p. A, Lateral radiograph of the knee shows subtle disruption of the posterior femoral cortex in the region of the lateral femoral condyle. B, Sagittal computed tomography scan more clearly shows a radiolucent lesion in the distal femur with destruction of the posterior metaphyseal cortex. A, Aspirates from metastatic melanoma showing large epithelioid cells with eccentric nuclei. B, Metastatic neuroblastoma showing poorly differentiated small cells in a background of delicate fibrillar matrix. C and D, Aspirate of metastatic alveolar rhabdomyosarcoma showing dispersed rhabdoid cells with oval cytoplasm. A, Aspirates of melanoma showing epithelioid cells with dense eosinophilic cytoplasm and eccentric nuclei. C and D, Crowded sheets of epithelial cells with high nuclear size variability among tumor cells. A, Blowout destructive lytic lesion of second left rib (arrows) confirmed by microscopic analysis to be metastatic carcinoma of thyroid. B, Computed tomogram of lesion in A documents destructive low-signal lesion in proximal portion of second left rib (arrows). These features suggest that this metastatic carcinoma most likely contains a secondary aneurysmal bone cyst component, which was confirmed microscopically. C, Anteroposterior radiograph of pelvis of a 9-year-old child shows multiple sclerotic foci that represent widespread skeletal metastases of medulloblastoma. Rhabdomyosarcoma must be differentiated from a variety of other hematologic and nonhematologic round-cell malignancies. Diffuse involvement of bone with a permeative growth pattern similar to that seen in other small cell malignancies may be seen with alveolar rhabdomyosarcoma,182 and pediatric patients typically undergo bone marrow biopsy as a component of their staging studies. Rhabdomyosarcoma is another example of a neoplasm for which molecular techniques can be used as an adjunct in diagnosis. Alveolar rhabdomyosarcoma shows consistent chromosomal translocation t(2;13)(q35;q14), and less commonly t(1;13)(p36;q1 4). The presence of larger cells with abundant eosinophilic cytoplasm containing fibrils or showing cross-striations indicates rhabdomyoblastic differentiation. However, rhabdomyoblasts displaying unequivocal cross-striation are difficult to find and, in most cases, immunohistochemical stains are necessary to classify the lesion. Neuroblastoma serves as an example of a tumor for which molecular studies can not only aid the diagnosis, but are also of prognostic value. Low-risk neuroblastomas are characterized by hyperdiploidy or near triploidy, particularly in patients younger than age 1. Formation of rosettes composed of spherically arranged nuclei with a fibrillar center may also be present, but this is a rather rare finding in cytologic preparations. Clear cell sarcoma of the kidney has a strong propensity to metastasize to the skeleton. A unique translocation-t(10;17)(q22;p13)-has been identified in clear cell sarcoma164,183,184,186,187; however, the molecular characteristics of the breakpoints have not been defined. Aspirates from metastatic clear cell sarcoma of the kidney are usually cellular and show a large population of pleomorphic sarcomatous cells. Deep nuclear indentations and nuclear grooves, as well as a granular cytoplasm, are characteristic features.
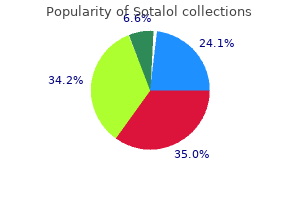
Inset blood pressure chart 14 year old buy generic sotalol, Axial computed tomography scan showing a metastatic neuroblastoma deposit within the calvarium (A prehypertension causes and treatment discount sotalol 40 mg otc, ×200; B blood pressure 50 over 70 discount 40 mg sotalol fast delivery, ×400) (A and B blood pressure chart over a day best order for sotalol, hematoxylin-eosin) blood pressure medication osteoporosis buy sotalol with a visa. A and B, Solid proliferation of round primitive cells with clear cytoplasm is characteristic of this tumor (A, ×200; B, ×400) (A and B, hematoxylin-eosin). Hiratsuka S, Watanabe A, Aburatani H, et al: Tumour-mediated upregulation of chemoattractants and recruitment of myeloid cells predetermines lung metastasis. Peters S, Meylan E: Targeting receptor activator of nuclear factor- B as a new therapy for bone metastasis in non-small cell lung cancer. Borak J: Relationship between the clinical and roentgenological findings in bone metastases. Norman A, Ulin R: A comparative study of periosteal new-bone response in metastatic bone tumors (solitary) and primary sarcomas. Wu Y, Li P, Zhang H, et al: Diagnostic value of fluorine 18 fluorodeoxyglucose positron emission tomography/computed tomography for the detection of metastases in non-small-cell lung cancer patients. Blastic M, Plavecz E, Zalatnai A: Pancreatic carcinomas in a 60-year, institute-based autopsy material with special emphasis of metastatic pattern. Bubendorf L, Schopfer A, Wagner U, et al: Metastatic patterns of prostate cancer: an autopsy study of 1589 patients. Farooki A, Leung V, Tala H, et al: Skeletal-related events due to bone metastases from differentiated thyroid cancer. Fottner A, Szalantzy M, Wirthmann L, et al: Bone metastases from renal cell carcinoma: patient survival after surgical treatment. Henriksson C, Haraldsson G, Aldenborg F, et al: Skeletal metastases in 102 patients evaluated before surgery for renal cell carcinoma. Ibayashi K, Ando M, Gotoh E: Regression of pulmonary and multiple skeletal metastases from renal cell carcinoma by nephrectomy and alpha-interferon therapy: a case report. Inci S, Akbay A, Bertan V, et al: Solitary skull metastasis from occult thyroid carcinoma. Ito Y, Kudo T, Kobayashi K, et al: Prognostic factors for recurrence of papillary thyroid carcinoma in the lymph nodes, lung, and bone: analysis of 5768 patients with an average 10-year follow-up. Kasagi K, Takeuchi R, Miyamoto S, et al: Metastatic thyroid cancer presenting as thyrotoxicosis: report of three cases. Kerbl K, Pauer W: Spontaneous regression of osseous metastasis in renal cell carcinoma. Koranda P, Ryznar V, Dockal M, et al: Papillary adenocarcinoma of the thyroid gland metastasizing into the epidural space of the upper thoracic spine, without vertebral involvement: case report. Kosuda S, Yokoyama H, Katayama M, et al: Technetium-99m tetrofosmin and technetium-99m sestamibi imaging of multiple Skeletal Metastases in Selected Common Neoplasms 54. Ezra E, Vardy S, Rose G: Metastatic colon adenocarcinoma of the orbit with intraneural extension from the brow to the brainstem. Katoh M, Unakami M, Hara M, et al: Bone metastasis from colorectal cancer in autopsy cases. Nozue M, Oshiro Y, Kurata M, et al: Treatment and prognosis in colorectal cancer patients with bone metastasis. Pauzner R, Istomin V, Segal-Lieberman G, et al: Bilateral patellar metastases as the clinical presentation of bronchogenic adenocarcinoma. Santini D, Tampellini M, Vincenzi B, et al: Natural history of bone metastasis in colorectal cancer: final results of a large Italian bone metastases study. Urvoy P, Mestdagh H, Butin E, et al: Patellar metastasis from a large bowel adenocarcinoma. Nakajima T, Suzuki M, Ando S, et al: Spontaneous regression of bone metastasis from renal cell carcinoma: a case report. Ozaki O, Kitagawa W, Koshiishi H, et al: Thyroid carcinoma metastasized to the sternum: resection of the sternum and reconstruction with acrylic resin. Schlumberger M, Challeton C, De Vathaire F, et al: Radioactive iodine treatment and external radiotherapy for lung and bone metastases from thyroid carcinoma. Sesenna E, Tullio A, Piazza P: Treatment of craniofacial metastasis of a renal adenocarcinoma: report of case and review of literature. Szendroi A, Dinya E, Kardos M, et al: Prognostic factors and survival of renal clear cell carcinoma patients with bone metastases. Takashi M, Takagi Y, Sakata T, et al: Surgical treatment of renal cell carcinoma metastases: prognostic significance. Van Poppel H, Baert L: Nephrectomy for metastatic renal cell carcinoma and surgery for distant metastases. Woodward E, Jagdev S, McParland L, et al: Skeletal complications and survival in renal cell carcinoma patients with bone metastases. Yamasoba T, Kikuchi S, Sugasawa M, et al: Occult follicular carcinoma metastasizing to the sinonasal tract. Zohar Y, Strauss M: Occult distant metastases of well-differentiated thyroid carcinoma. Benard J: Genetic alterations associated with metastatic dissemination and chemoresistance in neuroblastoma. Nishida Y, Tsukushi S, Urakawa H, et al: High incidence of regional and in-transit lymph node metastasis in patients with alveolar rhabdomyosarcoma. Seidal T, Mark J, Hagmar B, et al: Alveolar rhabdomyosarcoma: a cytogenetic and correlated cytological and histological study. Sotelo-Avila C, Gonzalez-Crussi F, Sadowinski S, et al: Clear cell sarcoma of the kidney: a clinicopathologic study of 21 patients with long-term follow-up evaluation. Sridhar S, Al-Moallem B, Kamal H, et al: New insights into the genetics of neuroblastoma. Tonelli R, McIntyre A, Camerin C, et al: Antitumor activity of sustained N-myc reduction in rhabdomyosarcomas and transcriptional block by antigene therapy. Turc-Carel C, Lizard-Nacol S, Justrabo E, et al: Consistent chromosomal translocation in alveolar rhabdomyosarcoma. Wang-Wuu S, Soukup S, Ballard E, et al: Chromosomal analysis of 16 human rhabdomyosarcomas. Whang-Peng J, Knutsen T, Theil K, et al: Cytogenetic studies in subgroups of rhabdomyosarcoma. Hayashi Y, Kanda N, Inaba T, et al: Cytogenetic findings and prognosis in neuroblastoma with emphasis on marker chromosome 1. Kaneko Y, Kanda N, Maseki N, et al: Different karyotypic patterns in early and advanced stage neuroblastomas. Many of the nodules subsequently become detached from the synovial membrane and float in the joint. The process typically involves the synovium diffusely, has a high propensity for recurrences, and may severely compromise the function of a joint. The peak incidence is in the fifth decade of life, but the age range varies widely from the first to seventh decades. Male patients are predominantly affected, and the male-tofemale ratio is approximately 2: 1. Synovial chondromatosis preferentially involves the major weight-bearing joints, but any joint may be involved. A few cases involve joints of the shoulder and acral skeleton, the intervertebral facet joint, and the temporomandibular joint. Clinical Symptoms the clinical presentation consists of pain, swelling, and limitation of motion. The patient may have a history of symptoms lasting several months to several decades, but usually symptoms have persisted for several years, with the average being 5 years. Superimposition of enchondral ossification is associated with the development of linear calcifications. These structures correspond to well-developed ossified nodules that are composed of a shell of bone with a central area mimicking a medullary cavity. In such cases, there is extensive involvement of tendons, multiple joints, or both tendons and joints in the same anatomic region. A and B, Lateral (A) and anteroposterior (B) radiographs of foot and ankle show long-standing synovial chondromatosis involving tendon sheaths. Note extensive involvement of extraarticular synovium of tendons and eggshell pattern of mineralization with central lucency in some of the nodules. B, Computed tomogram documents multifocal calcification in periarticular soft tissue. C, Specimen radiograph of resected synovial pad with multifocal calcified nodules representing areas of cartilaginous metaplasia. A, Sagittal magnetic resonance image shows high signal in loose bodies with areas of signal void representing mineralization of cartilage and bone matrix. B, Lateral radiograph of knee shows cartilaginous and bony loose bodies in knee joint below patella; joint space is preserved. Each cartilage nodule ranges in size from a small focus (<1 mm) that requires a magnifying glass to be seen to a larger lesion measuring more than 1 cm in diameter. In addition to individual nodules focally, larger cartilaginous areas represent coalescent smaller nodules of cartilage. These larger cartilaginous masses have multinodular (granular) surfaces, and their multifocal origin can still be seen on cut surface. Occasionally in long-standing cases, the adjacent bursae or tendons may be involved. On the basis of gross features, synovial chondromatosis can be divided into two forms: diffuse and localized. The diffuse form is characterized by multiple nodules that involve almost the entire synovium of the joint. In rare cases a nodular form of synovial chondromatosis can have a configuration of a polypoid pedunculated mass protruding into the joint space. In typical cases the cartilage cells form loose clusters, but a uniform distribution of cartilage cells can also be seen. The microscopic features of cartilage atypia may be compatible with those seen in grade 1 and 2 chondrosarcomas if taken out of context of a metaplastic synovial condition. These features should not be considered as indicative of malignant transformation and cannot be correlated with a more aggressive clinical behavior of the disease. The development of cartilage nodules in this metaplastic process is somewhat similar to normal phases of cartilage development. However, the majority of patients have a long history of symptoms when they are first seen. The earliest phases of synovial cartilage metaplasia are most frequently seen in smaller joints, such as the temporomandibular joint or the small joints of the acral skeleton, in patients with a short history of symptoms. In the earliest stages of synovial chondromatosis, small islands of cartilage cells with chondroblastic features form. Lateral radiograph shows popcornlike calcification in cartilaginous loose bodies and in synovium above posterior aspect of calcaneus and overlying the distal end of tibia, fibula, and talus. Note enlargement of tarsal sinus and thinning of neck of talus secondary to pressure of intraarticular bodies. T1-weighted images typically show a punctate signal void in the lesion involving the joint capsule. However, T2-weighted images show signal enhancement and may show the lesion to have a multinodular architecture. At the other end of the spectrum are longlasting lesions that present as a consolidated, heavily calcified mass. Note enlargement of acetabular fossa and calcified intrasynovial cartilaginous bodies characteristic of localized synovial chondrometaplasia. A and B, Computed tomogram of skull shows involvement of temporomandibular joint by synovial chondromatosis. Note expansion of joint and areas of signal void within joint and in thickened synovium. A, Plain radiograph of wrist and hand shows soft tissue calcifications in wrist joint overlying triquetrum, hamate, and distal end of ulna (arrows). B, Lateral view of wrist (same case as A) shows soft tissue calcified bodies that are both dorsal and volar in location (arrows). A, Anteroposterior radiograph of foot shows soft tissue calcification between first and second metatarsals with ringlike and punctate appearance. B, Oblique radiograph shows soft tissue calcifications representing loose cartilaginous bodies in tendon sheath. A and B, Synovectomy specimen in case of diffuse synovial chondromatosis of knee joint. C and D, Loose cartilaginous bodies and synovial membrane from two cases of synovial chondromatosis that diffusely involved knee joint. A, Localized synovial chondromatosis presents as conglomerate of individual cartilage nodules. B, Pedunculated polypoid lesion of knee joint is composed of individual cartilage nodules and interlacing synovial membrane. C, Radiograph of shoulder showing a conglomerate of individual mineralized nodules with punctate and ringlike calcification patterns. D, Central calcification in metaplastic chondroid nodule of synovium in knee joint. A, Low power photomicrograph of cross section through synovium of knee joint in synovial chondromatosis. B, Medium power photomicrograph of typical chondroid metaplastic nodules in synovium of knee joint. C, Low power photomicrograph of synovium with conversion of cartilage nodules to bone. A, Ill defined nodules composed of chondroblastic cells in the synovial membrane representing early phases of synovial chondromatosis.
Sotalol 40 mg buy overnight delivery. Setting Up Pressure Transducer.
References
- Barbash GI, Friedman B, Glied SA, et al: Factors associated with adoption of robotic surgical technology in US hospitals and relationship to radical prostatectomy procedure volume, Ann Surg 259(1):1n6, 2014.
- Gosalbez R Jr, Gousse AE: Reconstruction and undiversion of the short or severely dilated ureter: the antireflux ileal nipple revisited, J Urol 159:530n534, 1998.
- Jacobs MA, Avellino AM, Shurtleff D, et al: Reinnervating the penis in spina bifida patients in the United States: ilioinguinal-to-dorsal-penile neurorrhaphy in two cases, J Sex Med 10(10):2593n2597, 2013.
- Bradham RR, Sealy WC, Young WG Jr. Chronic middle lobe infection. Factors responsible for its development. Ann Thorac Surg 1966;2:612-6.
- Coca SG, Yusuf B, Shlipak MG, Garg AX, Parikh CR. Long-term risk of mortality and other adverse outcomes after acute kidney injury: a systematic review and meta-analysis. Am J Kidney Dis. Jun 2009;53(6):961-973.
