
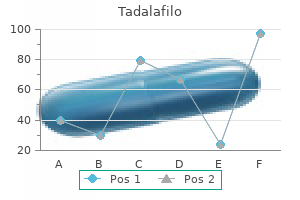
Tadalafilo
| Contato
Página Inicial
Juan Marcos Gonzalez, PhD
- Assistant Professor in Population Health Sciences
- Assistant Professor in Medicine
- Member of the Duke Clinical Research Institute
https://medicine.duke.edu/faculty/juan-marcos-gonzalez-phd
If there is a history of recent onset of green sputum production rather than white best erectile dysfunction pills treatment purchase tadalafilo with paypal, and clinical signs support a diagnosis of chest infection impotence 36 5 mg tadalafilo buy fast delivery, surgery should if possible be postponed and a course of antibiotics and physiotherapy commenced erectile dysfunction low testosterone treatment purchase tadalafilo in united states online. Reduced values compared to predicted values for age erectile dysfunction medicine bangladesh order tadalafilo overnight, height and sex indicate airflow obstruction impotence 22 year old buy tadalafilo us. Serial measurements are useful for monitoring disease progress and for demonstrating a response to bronchodilator therapy. Arterial blood gas analysis may be useful, and interpretation should be systematic. Look first at the pH value (acidosis or alkalosis) to determine the direction of the primary change. Although there may be partial compensation for the underlying abnormality, there is never full or over-compensation. If standard bicarbonate is raised, there is either a metabolic alkalosis or metabolic compensation for a respiratory acidosis. If the standard bicarbonate is low, there is a metabolic acidosis or metabolic compensation for a respiratory alkalosis. A negative base excess (a base deficit) indicates metabolic acidosis, so is found with a low standard bicarbonate; a positive base excess, which is found with a raised standard bicarbonate, indicates metabolic alkalosis. Although mean systemic diastolic and systolic arterial pressure rise with increasing age, hypertension is defined by arbitrarily set levels. However, the evidence for what level of blood pressure constitutes a risk for anaesthesia and how great that risk is remains unclear. There is no evidence that patients with stage 1 (140159 mmHg systolic and 9099 mmHg diastolic) and stage 2 (160179 mmHg systolic and 100109 mmHg diastolic) hypertension in the absence of target organ damage have increased perioperative cardiovascular risk (Hartle et al. If these values are not available in the preoperative assessment clinic blood pressures, then blood pressures below 180 mmHg systolic and 110 mmHg diastolic are acceptable. It is also unclear whether or not control of hypertension prior to elective surgery will reduce perioperative complications, morbidity and mortality. The emphasis on managing the patient perioperatively is focused on the management of cardiovascular risk rather than precise blood pressure values. Isolated systolic hypertension is most prevalent in the elderly population and is a significant risk factor for stroke as well as cardiovascular morbidity in this group. Additionally, the level of sympathetic nervous system activity is high, resulting in a greater than normal response to any stimulus. In a hypertensive patient there is a much greater fall than normal in systemic arterial pressure on induction of anaesthesia, due to a fall in cardiac output resulting from decreases in both heart rate and stroke volume. Importantly, there is an increased risk of postoperative myocardial infarction in hypertensive patients. At preoperative assessment the anaesthetist should look for evidence of any of these conditions and for end-organ damage due to hypertension. Serum urea, electrolytes and creatinine may reveal renal impairment, and serum glucose may show diabetes. Chest x-ray may reveal left ventricular enlargement, and distended upper pulmonary lobe veins indicate left ventricular failure. Drug treatment Usual antihypertensive therapy should be continued on the day of surgery. Antihypertensive agents tend to potentiate the hypotensive effects of general anaesthesia. Thiazide diuretics are a common first-line treatment for hypertension, particularly in the elderly. Despite their advantages during anaesthesia (depression of the cardiovascular response to laryngoscopy and to surgical stimulation), -blockers may cause problems: bradycardia, atrioventricular block, decreased myocardial contractility, bronchoconstriction and altered response to inotropes. If -blockers are stopped preoperatively, hypertension, arrhythmias and myocardial ischaemia are increased intraoperatively, as is postoperative myocardial ischaemia. Sedative premedication is often prescribed for hypertensive patients to reduce endogenous catecholamine levels that may exacerbate the hypertension. The rate of progression of individual plaques within any patient is variable, and this explains why, although peripheral vascular and cerebrovascular disease will often coexist with coronary artery disease, the patient may be asymptomatic of these other conditions. A guide to the severity of angina is the exertion necessary to precipitate an attack. The distance that is regularly walked on the flat before an attack occurs should be elicited in the history. It may be that angina is only occasional, such as when climbing more than one flight of stairs or in very cold weather. If angina is precipitated by minimal exertion or is even occurring at rest (unstable angina), the patient has severe myocardial insufficiency and anaesthesia may present problems. If elective surgery is proposed, this should be cancelled and the patient investigated further with a view to cardiac intervention. Perioperative assessment of cardiac risk the Goldman cardiac risk index was one of the earlier multifactorial scoring systems designed to predict clinical risk, but despite various modifications and the introduction of alternative scoring systems, overall predictive accuracy has remained disappointingly limited. However, much of the work supports the likelihood that certain factors consistently reduce perioperative cardiac morbidity and mortality. These include preoperative optimisation of cardiac status, aggressive invasive monitoring and prompt treatment of intraoperative haemodynamic disturbance. This is almost always due to atheroma, although rarely other disease processes may be responsible. These plaques grow and evolve with time, decreasing blood flow through a vessel and possibly occluding it. Chapter 1: Preoperative management 13 perioperative cardiac management in patients undergoing non-cardiac surgery, building on earlier guidelines from the American College of Cardiology and the American Heart Association. The guidelines integrate clinical risk factors and functional capacity with the risk for cardiac events of the planned surgical procedure when evaluating patients preoperatively. Cardiovascular risk is defined in terms of myocardial infarction, heart failure and death. An algorithmic process is used to identify patients who might benefit from further investigation (such as echocardiography and radionuclide scanning) or therapeutic intervention. In other words, patients with cardiac disease awaiting elective surgery can be considered on a more individual basis with respect to their perioperative risk. Sinus tachycardia has several common causes such as anxiety, pyrexia, cardiac failure and anaemia. Atrial tachyarrhythmias should be controlled preoperatively with digoxin or amiodarone therapy. Complete heart block, any form of bifascicular block and sick sinus syndrome require preoperative pacing. Echocardiography uses ultrasound to study blood flow, the structure of the heart and the movement of valves and cardiac muscle. Ventricular volumes, ejection fraction and gradients across valves can be estimated. The ejection fraction is particularly useful: it is normally over 60%; if it is less than 40% serious problems associated with anaesthesia should be anticipated. Seventy per cent of patients with cardiomegaly have an ejection fraction of less than 50%. Radionuclide scanning provides a relatively noninvasive means of accurately assessing myocardial function. In blood pool scanning 99technetium-labelled red blood cells are injected intravenously and then both the amount of blood in the heart at each stage of the cardiac cycle and the shape of the cardiac chambers can be determined. This technique also uses 99technetium, which is taken up into the acutely infarcted myocardial tissue thus revealing the position and extent of the damage. It is taken up by normal myocardium, so areas that are not being perfused show on the scan as perfusion defects. A coronary Other cardiac investigations Chapter 1: Preoperative management 15 vasodilator, such as dipyridamole, may then be given. A fixed perfusion defect indicates scar tissue while a reperfusion defect indicates ischaemia. Reperfusion defects are more significant because ischaemia may develop perioperatively, whereas a fixed perfusion defect cannot deteriorate. However, most modern units require a cautious approach to the use of magnets, which may expose a programmable unit to the risk of being re-set in a variable fashion. Preoperative assessment should be directed to determining the indication for the device, the type of unit and its characteristics. Chest x-ray will help identify the pulse generator siting and lead placement and number. With pacemakers, magnet response will vary between models and programmed settings. Energy can also be induced into heart lead systems causing tissue heating at lead tips through high-frequency currents. However, where the procedure will be close to the implant and where the use of diathermy is likely, then risk of malfunction is increased. Valvular heart disease the availability of echocardiography today means that any patient with suspected valve disease should be properly investigated and a diagnosis made prior to anaesthesia. Unfortunately, patients with significant valve disease may still present for emergency surgery. Any patient with a heart valve lesion, including replacement valves, requires prophylactic antibiotics for dental, genitourinary, obstetric, gynaecological and gastrointestinal procedures. Aortic stenosis the symptoms of aortic stenosis occur late and include angina, syncope, dyspnoea and sudden death. On chest x-ray, left ventricular enlargement may not be evident and the aortic valve may be calcified. Echocardiography determines the gradient across the valve and will provide information on ventricular function. If the valve gradient is greater than 50 mmHg, angioplasty or valve replacement should be considered. The main anaesthesia-related problems are fixed cardiac output, ventricular arrhythmias and incipient cardiac failure. Clinical signs include a collapsing pulse, left ventricular enlargement and an early diastolic murmur. Problems with respect to anaesthesia are poor myocardial reserve and cardiac failure. Mitral stenosis Symptoms of mitral stenosis are dyspnoea, tiredness and haemoptysis. Mitral stenosis may be complicated by systemic embolism or pulmonary hypertension. On chest x-ray there may be left atrial enlargement and pulmonary venous congestion. Hypothyroidism (normochromic) Low-grade haemolytic anaemia with high reticulocyte count Mitral regurgitation Progressive dyspnoea and tiredness are common symptoms of mitral regurgitation. Left ventricular enlargement and a pansystolic murmur are the predominant clinical signs. Chest x-ray demonstrates left-sided enlargement of the heart, particularly atrial enlargement, and indications of pulmonary oedema may be seen. Haematological disease Anaemia A patient is considered anaemic if the haemoglobin is below the normal range and polycythaemic if it is above the normal range. In children the range varies: a child is considered to be anaemic if the haemoglobin value is less than 18 g dL1 at birth, less than 9 g dL1 at 3 months, less than 11 g dL1 from 6 months to 6 years, and less than 12 g dL1 from 6 to 12 years. The causes of anaemia are blood loss, inadequate production of erythrocytes and excessive destruction of erythrocytes. Iron deficiency is the most common cause of anaemia, but the cause is often multifactorial. Those patients in whom anaemia should be suspected include all females of child-bearing age (due to menstrual loss), the elderly (due to poor diet and other diseases) and all patients who are undergoing gastrointestinal or gynaecological surgery (due to blood loss). If severely anaemic, symptoms may include tiredness and dyspnoea Tricuspid valve lesions Tricuspid stenosis is usually associated with mitral and aortic valve disease. Anaesthesia-related problems are usually due to the accompanying other valve disease rather than to the tricuspid lesion itself. Pulmonary regurgitation is rare, and most often secondary to pulmonary hypertension. Chapter 1: Preoperative management 19 on exertion, and in the elderly angina, heart failure and confusion may be precipitated. A full blood count also provides the platelet count (raised in acute blood loss and acute inflammation) and the white cell count (raised in infection). A differential white cell count distinguishes between neutrophilia (bacterial infection, inflammation) and lymphocytosis (viral infection). If the platelet count, white cell count and haemoglobin are all low, this indicates marrow aplasia or infiltration. Abnormalities which may be detected on examination of the blood film include a raised reticulocyte count (haemolytic anaemia, continued bleeding), sickle cells or malarial parasites. Of most relevance to anaesthesia is a decrease in the oxygen-carrying capacity of the blood. Although anaemia decreases blood viscosity and hence improves blood flow, with a consequent increase in oxygen delivery to the tissues, once the haemoglobin is less than 10 g dL1 the increase in blood flow no longer compensates for the decreased oxygen-carrying capacity. Some authorities consider a haemoglobin value of greater than 8 g dL1, rather than 10 g dL1, acceptable for anaesthesia. A secondary anaemia-related problem is the fact that cardiac output increases in order to maintain oxygen flux. In some patients this leads to cardiac failure, and in all patients cardiac reserve is decreased, reducing the ability to compensate for the myocardial depressant effects of anaesthesia. It is important to remember that cyanosis is only evident clinically when the level of deoxyhaemoglobin equals or exceeds 5 g dL1. Hence blood transfusion in an anaemic patient immediately prior to anaesthesia confers minimal advantage and may lead to fluid overload. Blood should be transfused to achieve a haemoglobin > 10 g dL1 and a haematocrit > 0. Administration of oxygen therapy will increase oxygen delivery by ensuring maximal saturation of the available haemoglobin and an increase in the dissolved oxygen in blood.
Heparin reduces platelet aggregation secondary to the reduction in thrombin (a potent platelet aggregator) impotence stress discount tadalafilo 20 mg on line. The drug is metabolised in the liver erectile dysfunction related to prostate buy tadalafilo us, kidney and reticuloendothelial system by heparinases that desulphate the mucopolysaccharide residues and hydrolyse the links between them erectile dysfunction books tadalafilo 2.5 mg line. They may be used in extracorporeal dialysis circuits erectile dysfunction prevalence purchase 10 mg tadalafilo mastercard, and have been used in cardiopulmonary bypass erectile dysfunction vascular causes purchase tadalafilo mastercard. Peak anti-Xa activity is achieved within 34 hours after subcutaneous injection and activity has halved after 12 hours. This occurs because the negative charge of the heparin is attracted to the positive charges of the protamine. Protamine (in excess) has anticoagulant activity, although this effect is not as powerful as that of heparin. It has a volume of distribution of 40100 mg kg1 and is bound to antithrombin, albumin, fibrinogen and proteases. Increase in acute-phase proteins (during acute illness) can significantly alter the clinical effect. Heparin also binds to platelet and endothelial protein, reducing Activated factor X inhibitors Examples apixaban, fondaparinux, rivaroxaban Apixaban, fondaparinux and rivaroxaban act by inhibiting factor Xa. These drugs share the potential for causing active bleeding and are not easily monitored by laboratory tests. Like the factor Xa inhibitors, these drugs may cause active bleeding and are not easily monitored. Calcium chelating agents Calcium is an essential cofactor in the coagulation system. However, this is technically difficult and the delay in doing so may remove any benefit. Some of these agents require heparin and/or aspirin to prevent reformation of thrombus. They may reduce levels of plasminogen, 2-antiplasmin, 2-macroglobulin and C1-esterase inhibitor. Anistreplase is a ready-combined complex of plasminogen and streptokinase that is blocked by an anisoyl group. Once in the body the anisoyl group leaves the complex, which produces plasmin and so activates fibrinolysis. Streptokinase induces an immune response that produces antibodies to the drug, limiting its useful duration to 6 days. Patients frequently have antibodies to protein from previous exposure to the Streptococcus. Plasminogen activators are used to destroy clots in the following situations: r Venous thrombosis r Pulmonary embolus r Retinal thrombosis r Myocardial infarction the drugs may also remove clot formed in response to haemorrhage, so bleeding from other sites is a risk. In Examples aprotinin, tranexamic acid the fibrinolytic inhibitors act by inhibiting the enzymatic activity of plasmin on fibrin. They are used to prevent the breakdown of fibrin clot when excessive bleeding during surgery is a risk. Uses include the reduction of blood loss during surgery in haemophiliacs, in cardiac surgery, and in thrombolytic overdose. Aprotinin is a polypeptide and inhibitor of proteolytic enzymes in general, but specifically it is used for its action on plasmin and kallikrein. It is useful in upper gastrointestinal haemorrhage and in surgery in haemophiliacs, and it can be administered orally or intravenously. More importantly, endothelial cells generate new cyclo-oxygenase, whereas platelets are unable to do so. Aspirin is not specific for platelet cyclo-oxygenase, but this is more readily inactivated than the endothelial cyclo-oxygenase responsible for prostacyclin production. Aspirin should be stopped 710 days before surgery to allow regeneration of normally functioning platelets. Prostacyclin Synthetic prostacyclin (epoprostenol) inhibits platelet aggregation and dissipates platelet aggregates. It can be used in haemodialysis, but must be given as an infusion because of a short half-life (about 3 minutes). Prostacyclin is also a potent vasodilator, so patients should be observed for hypotension, flushing and headaches. These are reduced by broadspectrum antibiotics and are deficient in the newborn (haemorrhagic disease of the newborn). This may be useful to decrease surgical oozing in mild haemophilia, and in cases of massive transfusion, when clotting factors are reduced. P2Y12 inhibitors Platelet action Ethamsylate reduces capillary bleeding, probably by correcting abnormal platelet adhesion. P2Y12 inhibitors: differences in properties and mechanisms of action and potential consequences for clinical use. After treatment has commenced, the duration of therapy must be determined and regularly reassessed, together with the need to modify the antibiotic(s) in terms of both type and dose, depending on the clinical condition of the patient and laboratory results. The cell wall comprises N-acetyl glucosamine, acetyl muramic acid and a polypeptide, which form multiple cross-links. The cell wall can range from several molecular layers thick in Gramnegative bacteria to 100 layers in the Gram-positive organisms. Antimicrobials that inhibit cell wall synthesis cause the growing cell to burst, and so are normally bactericidal. Antibacterial drugs targeting the cell wall cannot affect eukaryotic cells by this mechanism. Patient factors r Age r Weight r Renal function r Hepatic function r Antimicrobial allergy r Immune deficiency or suppression r Pregnancy r Significant medical conditions r Site of infection r Severity of infection r Prophylaxis or treatment required Organism factors r Virulence r Predicted microbe population r Predicted antimicrobial susceptibility Drug factors r Spectrum of antimicrobial activity r Route of administration r Pharmacokinetics r Synergy or antagonism with other antimicrobial agents r Toxicity profile r Interactions with non-antimicrobial compounds r Local antibiotic prescribing policies Cell membrane permeability Drugs that selectively interfere with cell membrane permeability are active against bacterial and fungal cells. Selectivity is conferred by targeting components of bacterial or fungal cell membranes that are not found in the host. Negatively charged lipids are abundant in the cell membranes of Gram-negative bacteria and are the target of polymyxins such as colistin and polymyxin B. Imidazoles and triazoles interfere with sterol synthesis, and toxicity occurs with higher doses. Polyenes such as amphotericin and nystatin bind to the fungal sterols and open pores in the membrane, leading to destruction of the molecular composition of the cytoplasm. Antimicrobial therapy in renal failure Most antibiotics or their metabolites are renally excreted. Accumulation of potentially toxic compounds may therefore arise unless careful monitoring and dose adjustments are performed. Protein synthesis Where bacterial and human ribosomes differ, they can be targeted by antibiotics. Mechanisms of action Antimicrobials work by interfering with bacterial or fungal cellular functions. They target structures and functions specific to the target microbe or those that have an alternative metabolic pathway in human cells. These mechanisms target four groups of microbial sites: r Cell wall r Cell membrane r Protein synthesis r Nucleic acid synthesis Mechanisms of resistance Bacteria, viruses and fungi can all mutate, and indeed do so frequently. Antimicrobial agents exert a selective pressure on microbial populations favouring resistant mutants. Because of the speed at which microorganisms Chapter 42: Antimicrobial therapy 741 multiply (every 20 minutes in the case of Escherichia coli in optimal growth conditions), it can be seen that the opportunity for the development and spread of resistance is considerable. As well as spontaneous mutation within a bacterium, organisms may acquire resistance genes in a number of ways. Bacterial genes can be transferred at the time of bacterial conjugation or via bacterial viruses (bacteriophages). Once a resistance gene has emerged it may therefore be readily transmitted between bacteria of the same species. They vary in size, and some may contain a number of different resistance genes as well as genes coding for a range of virulence and bacterial survival factors. Transposons are genes which allow movement of genetic material attached to them from one bacterial chromosome to another or between bacterial chromosomes and plasmids. Hence a resistance gene that originally arose in a bacterial chromosome could move to a more mobile bacterial plasmid. There are about eight distinct mechanisms of resistance recognised, some of which may be combined within a single organism to increase the degree of resistance. This is usually the most efficient mechanism, and it tends to have the least negative impact on the bacterium. Resistance to -lactam antibiotics (see below) is largely a consequence of production of -lactamase enzymes by bacteria. Aminoglycoside-modifying enzymes (of which there are more than 30) are the next most prolific group, conferring resistance to gentamicin, tobramycin and sometimes amikacin. A similar mechanism confers penicillin resistance in some Streptococcus pneumoniae and Neisseria gonorrhoeae. Resistance to the macrolides is often due to altered bacterial ribosomal binding sites. Excess of binding sites in the bacterial cell wall is responsible for reduction in susceptibility to glycopeptides in Staphylococcus aureus (so-called vancomycin-intermediate S. The movement of hydrophilic molecules through the outer bacterial lipid membrane is via porin proteins, which form channels through which they can pass. Mutations to the genes encoding for porin proteins or their expression may therefore confer a degree of resistance by preventing the antibiotic molecules passing through these channels. Aminoglycoside, quinolone and carbapenem resistance in certain Gram-negative bacteria. Usually the resistance is low-level as molecules useful to the bacterium will also be blocked to some degree. However, when combined with active efflux (see below) the resistance will be greater. Active efflux is a common mechanism of resistance, which, when it is present in conjunction with reduced antibiotic permeability, may confer high-level resistance. Quinolones, macrolides, -lactams and tetracyclines may all be subject to this form of resistance. Penicillins Examples amoxicillin, benzylpenicillin, flucloxacillin, piperacillin, temocillin Beta-lactams this is the single largest group of antimicrobial agents presently available. Individuals with a history of anaphylaxis, urticaria or rash immediately after penicillin administration should not receive a penicillin or other -lactam, as there is a small risk of cross-hypersensitivity with cephalosporins and carbapenems. In very high doses with meningitis and renal impairment, penicillins and other -lactams may cause convulsions. Penicillins and cephalosporins show synergy with antibiotics acting on targets within the bacterial cell because the cell-wall changes increase the permeability of the cell to other compounds. Benzylpenicillin Benzylpenicillin is active against Gram-positive bacteria, most anaerobes and certain Gram-negative cocci (Neisseria spp. It is distributed widely, penetrating pleural, pericardial, peritoneal and synovial spaces, but not cerebrospinal fluid in the absence of meningeal inflammation. It is excreted mainly by tubular secretion in the kidney, with an elimination halflife of 30 minutes. Acquired resistance Bacteria exhibit resistance to -lactams by four mechanisms: r Enzymatic destruction of -lactam (-lactamases). These enzymes may be encoded for by genes present on either bacterial chromosomes or plasmids. Since 2010, there has been a rapid increase in metallo-lactamase enzymes, which are also often referred to as carbapenemases (although they also destroy other -lactam antibiotics). Note that the last two mechanisms may act in synergy in some bacteria (such as Pseudomonas) to increase the degree of resistance. It is active against bacteria covered by benzylpenicillin and several Gram-negative species, Haemophilus influenzae and most faecal streptococci (enterococci). Resistance is common and is usually due to -lactamase production by the bacterium. Amoxicillin is stable in gastric acid, and achieves good bioavailability after oral administration. Amoxicillin is the drug of choice for most acute lower respiratory tract infections acquired in the community, for sensitive strains of Neisseria gonorrhoeae, and for faecal streptococcal (enterococcal) infections. Chapter 42: Antimicrobial therapy 743 Flucloxacillin Flucloxacillin and related compounds (meticillin, cloxacillin) are unaffected by staphylococcal -lactamase but have a narrower spectrum of activity than benzylpenicillin. Flucloxacillin is well absorbed orally but high protein binding (95%) limits its diffusion into some compartments, notably cerebrospinal fluid. Flucloxacillin may rarely cause cholestatic jaundice and hepatitis, and it must be used with caution in patients with hepatic impairment. Because of the risk of cholestatic jaundice and hepatitis it must be used with caution (if at all) in patients with hepatic impairment. Cephalosporins Piperacillin and Tazocin Piperacillin is distinguished from amoxicillin mainly by its activity against Pseudomonas aeruginosa and related species. It is therefore now combined with a -lactamase inhibitor (tazobactam) to produce Tazocin. These drugs are sodium salts, and the high doses required to treat severe sepsis may cause sodium overload. They are mainly used for known or suspected Pseudomonas infections and, usually in combination with aminoglycosides, for the treatment of febrile neutropenic patients. Most -lactam antibiotics exhibit antibacterial synergy when given with aminoglycosides, and there is some evidence that they may also be synergistic against Gramnegative bacteria when given with quinolones. Examples cefixime, cefotaxime, cefpirome, ceftaroline, ceftazidime, ceftriaxone, cefuroxime, cephalexin these compounds are based on cephalosporin C, a fermentation product of Cephalosporium acremonium cultivated from a Sardinian sewage outfall in 1948. It is also moderately active against some enterobacteria (including Escherichia coli). Cephalexin is stable to gastric acid and almost completely absorbed when given by mouth, and 10% is protein-bound. Cephalexin occasionally causes hypersensitivity, diarrhoea and abdominal discomfort, and rarely Stevens Johnson syndrome. Cefuroxime Cefuroxime is more active than cephalexin against most of the Enterobacteriaceae, and has useful activity against Haemophilus influenzae.
Bloodbrain barrier the bloodbrain barrier exists between the circulation and the interstitial fluid in the brain discount erectile dysfunction drugs tadalafilo 2.5 mg buy free shipping. It consists of the ultrafiltration barrier in the choroid plexuses and the barrier around cerebral capillaries impotence ka ilaj purchase tadalafilo with amex. The latter consists of capillary endothelium doctor for erectile dysfunction proven tadalafilo 2.5 mg, basement membrane and a fenestrated layer of astrocyte end feet erectile dysfunction papaverine injection cheap 2.5 mg tadalafilo with mastercard. Tight junctions erectile dysfunction and age 2.5 mg tadalafilo order with mastercard, impermeable to solutes, join capillary endothelial cells and form a basic component of the bloodbrain barrier. Water, carbon dioxide and oxygen diffuse freely across the bloodbrain barrier, but the transport of glucose, the principal brain substrate, and ionised molecules is controlled. The bloodbrain barrier has the following functions: r To provide tight control over ionic (H+, Na+, K+, Ca2+, Mg2+) concentrations in the interstitial fluid, because brain cells are extremely sensitive to ion changes. Cerebral oedema will thus be accompanied by a reduction in cerebral blood volume and compression of the ventricles. Vital centres respond by increasing systemic arterial blood pressure, slowing the heart rate and respiratory rate. The blood pressure response attempts to restore cerebral blood flow by restoring the cerebral perfusion pressure. These include: r Anaesthesia as required for surgical interventions on the urinary tract in malignancy, hydronephrosis and urolithiasis r Renal failure in the perioperative period (pre-renal, renal and post-renal) r Causes of sepsis involving the kidney and urinary tract (urinary tract infection, haemolytic uraemic syndrome) r Causes of renal failure after providing an anaesthetic for renal transplantation (arterial blood supply, venous drainage, bladder connections of the new kidney) Anatomy There are two kidneys, which are normally 1012 cm in length. They are enlarged in adult polycystic kidney disease but may be atrophic in chronic kidney disease. The upper pole is located under the eleventh and twelveth ribs in the retroperitoneum. The renal artery to each kidney divides into two upper branches which supply the anterior and posterior upper poles, and one lower branch which supplies the lower pole. From the glomerular capillaries, efferent arterioles transport blood to the peritubular capillaries and then to the venous circulation via the interlobular veins, arcuate veins, interlobar veins and renal veins. The transport of blood from glomerular capillaries to peritubular capillaries represents a portal system. The loop of Henle has two limbs, a descending limb and an ascending limb, which are parallel to each other running from the cortex to the renal medulla. The glomerular filter the function of a glomerulus is to produce an ultrafiltrate of the plasma. Mesangial cells are located between the capillaries, and these have a phagocytic and structural role. The capillary endothelium acts as a screen to prevent blood cells and platelets from coming into contact with the main filter, which is the basement membrane. It forms a continuous layer, and is the main filtration barrier allowing the passage of molecules according to their size, shape and charge. It consists of collagen and other glycoproteins, including large amounts of heparan sulphate proteoglycan, which is strongly negatively charged. Postganglionic sympathetic fibres are distributed to the afferent and efferent arterioles, the proximal and distal tubules and the juxtaglomerular apparatus. Parasympathetic efferents from the vagus nerve also supply the kidneys, but their function is uncertain. Renal nociceptive afferents enter the spinal cord at T1011 to give referred pain distributed over the flanks. The nephron Each kidney contains approximately a million functional units called nephrons, which are located in the cortex. The nephron consists of a knot of capillaries (the glomerulus) and a tubular system with a blind end. The glomerular ultrafiltrate has a composition echoing that of plasma, which is free from cells and particles of molecular weight > 70,000. Smaller molecules (< 7000) pass freely through the glomerular filter, but permeability to large molecules decreases with size and negative charge. From the distal tubule the filtrate enters the collecting duct system consisting of the cortical and medullary collecting ducts. It is in the collecting duct system that the degree of water reabsorption or excretion by the kidney is determined and ultimately extracellular fluid osmolarity is maintained. The majority of nephrons have glomeruli in the outer two-thirds of the cortex and possess short loops of Henle only passing a short distance into the medulla. Approximately 15% of nephrons have glomeruli in the inner third of the cortex (juxtamedullary nephrons), with long loops of Henle passing deeply into the medulla. The tubular system the tubular system of the nephron determines the final composition of the urine. It functions by actively or passively secreting and reabsorbing substances into the glomerular ultrafiltrate. The urogenital system the collecting ducts enter the renal papilla and calyces, in the medulla of each kidney. Formation of urine involves: r Filtration of plasma at the glomerulus r Reabsorption of the majority of the filtrate in Size of molecules filtered Charge of the basement membrane Hydrostatic pressure gradient Renal plasma flow Colloid osmotic pressure gradient Glomerular capillary coefficient Blood pressure Size of molecules for filtration the tubules r Secretion of additional waste products into the tubules Water and ions are filtered, whereas proteins such as albumin, of molecular weight 69,000, are not normally filtered. Ultrafiltration across glomerular capillaries occurs approximately 10 times more easily than in other capillary beds. The colloid osmotic pressure in the glomerular capillaries is dependent on the colloid osmotic pressure in the afferent arterioles, the filtration fraction and renal plasma flow. This tubuloglomerular feedback mechanism is driven not only by changes in blood pressure; it is primarily mediated by sodium chloride concentration at the macula densa. For instance, when there is an increase in the delivery of amino acids or glucose to the kidney, a rise in sodium reabsorption in the proximal tubule occurs owing to co-transportation. This process of autoregulation is mediated by: r the myogenic response of blood vessels, which constrict as a result of increases in blood pressure or dilate when blood pressure falls. The proximal tubule Here, effectively 100% of amino acids and 100% of glucose are reabsorbed. Reabsorption of urea occurs passively down its concentration gradient since the the tubular urea concentration tends to increase as sodium chloride and water are reabsorbed from the proximal tubule. The filtrate osmolarity remains similar to plasma, because Chapter 16: Renal physiology interstitium tubular lumen 351 glucose Na+ Na+ K+ tubule. The loops of Henle do not concentrate the tubular fluid within them, but manufacture a hypertonic interstitial fluid in the renal medulla by a countercurrent mechanism. Urine is then concentrated by osmosis from collecting ducts as they pass through the medulla. It consists of a descending limb which passes into the medulla and loops round to become the ascending limb which passes back into the cortex. This limb then continues as the distal the countercurrent mechanism A proposed mechanism for countercurrent multiplication was described by Wirz, Hargitay and Kuhn in 1951. The hypertonic interstitium in the renal medulla is produced by a small osmotic pressure difference between the ascending and descending limbs of the loops. This small difference is then multiplied into a large longitudinal gradient by the countercurrent arrangement. This limb produces an increase in the surrounding interstitium by the extrusion of sodium and accompanying ions. Consequently, the osmolality of the medullary interstitium is increased and the osmolality of the fluid in the ascending limb is decreased. The fluid within the descending limb will therefore come to osmotic equilibrium with the interstitium. In effect, then, we can consider the transport of NaCl out of the ascending limb as being directed into the descending limb. The remaining 75% of nephrons (cortical nephrons) have short loops of Henle which barely reach the medulla, and these nephrons do not make a significant contribution to the manufacture of medullary hypertonicity. However, the collecting tubules of all the nephrons (both cortical and juxtamedullary) pass through the medulla. Thus only the long-looped nephrons, which form 25% of the total, produce the medullary gradient that concentrates the urine produced by all the nephrons. Functionally the distal tubule is a segment of the nephron in which the tubule cells undergo transition from the distal tubule ascending-limb-of-Henle-type cells to collecting-tubuletype cells. The walls of the ascending-limb-of-Henle-type cells have only a very low and essentially constant permeability to water. The collecting tubules have cortical and medullary sections, each section having somewhat different properties. The osmolarity of the tubular fluid is controlled, and may become high if there is increased water reabsorption and low if there is increased water clearance. Chapter 16: Renal physiology 353 Tubular transport Transport of substances, ions and water takes place between the tubular filtrate and the peritubular capillaries. The difference between reabsorption and secretion lies in the direction of transport. Rates of tubular reabsorption Transport mechanisms for some substances and in some parts of the tubular system may become saturated, resulting in a maximum reabsorption rate called the transport maximum. An example is the transport maximum for glucose in the proximal tubule in diabetic patients, when the filtered glucose cannot be reabsorbed completely and an excess appears in the urine. Similarly there is a maximum value for the reabsorption of sodium in the distal tubule. Alternatively a maximum value for reabsorption may not occur, as in the case of sodium transport in the proximal tubule. This transport mechanism does not appear to reach saturation, but continues to increase as the sodium load increases. The transport mechanism here is dependent on the electrochemical gradient of sodium and time. Sodium is actively pumped out of the tubular cell into the interstitium, thus lowering its concentration and creating a negative charge. These substances undergo secondary active transport as they move against a concentration gradient. Peritubular capillary reabsorption Water reabsorption There is no active water reabsorption. Water reabsorption in the nephron follows solute absorption and can be both transcellular and paracellular. The overall reabsorption rate is 124 mL minÀ1, just less than the glomerular filtration rate of 125 mL minÀ1. This physiological mechanism occurs because: r A rise in glomerular filtration rate or a reduction in plasma flow. This process acts to ensure that the distal tubule, cortical collecting tubule and medullary collecting duct receive a relatively constant volume of filtrate. However, this mechanism is attenuated by high blood pressure, which leads to an increase in peritubular capillary hydrostatic pressure, which decreases peritubular reabsorption. Filtration fraction is the ratio of glomerular filtration rate to renal plasma flow, and so it may be estimated by measurement of these factors. In clinical practice, glomerular filtration rate is the most useful measure for quantifying renal function. In such a case, the mass of the substance filtered per unit time is equal to the mass of substance excreted per unit time in the urine. The substance not only has to be filtered but must also be secreted, since glomerular filtration accounts for only 20% of renal plasma flow. Assuming complete clearance, the mass of substance cleared from plasma per unit time is equal to the mass of the substance excreted in the urine per unit time. The measured value would have to be divided by 90% to avoid underestimating true renal plasma flow. Renal plasma flow Mesangiocapillary glomerulonephritis Diffuse proliferative glomerulonephritis Crescentic glomerulonephritis Renal control of extracellular osmolarity the clearance of any substance excreted by the kidney is the volume of plasma which is cleared of the substance in unit time. Thus the units of clearance are those of volume per unit time (usually mL minÀ1) In fact clearance only represents a theoretical volume of plasma, since no aliquot of plasma is completely cleared of any substance during its passage through the kidney. There is a gradient of osmolarity, increasing from outer medulla to inner medulla. This environment is created by the juxtamedullary nephrons, which have long loops of Henle and which represent 25% of all nephrons. The arrangement of the peritubular blood supply of the medulla, called vasa recta, prevents solute loss and hence dilution. Sodium chloride the high concentration of sodium chloride in the medulla originates from the active transport of sodium out of the tubular lumen by the thick ascending limb of the loop of Henle. This process generates an electrochemical gradient for co-transport of sodium from the luminal side of the tubular cells via sodiumpotassium-chloride and also sodiumhydrogen co-transporters, and establishes a small osmotic gradient of 200 mOsm LÀ1, between the fluid in the tubular lumen and that in the medullary interstitium. This concentrated plasma then passes through the ascending vasa recta, gradually becoming less concentrated as water enters from the decreasingly hyperosmolar interstitium, and solute returns to the interstitium. Urea Urea accounts for approximately 40% of the total osmolarity of 1200 Osm LÀ1 in the inner medullary interstitium. The collecting ducts help to maintain the hyperosmolarity of the medullary interstitium by recirculating urea. The urea is then returned from the collecting ducts to the interstitium by facilitated diffusion. As the filtrate flows from distal tubule to cortical collecting tubule and medullary collecting duct, water is reabsorbed into an increasingly hyperosmolar medulla for reuptake into the circulation via the peritubular capillaries. It is also detected in the third ventricle at the subfornical organ and the organum vasculosum of the lamina terminalis. Vasa recta the countercurrent exchange performed by the vasa recta involves the movement of solute and water across the capillary membrane as plasma flows in opposite directions in each limb of the vasa recta, and provides the blood supply to the medulla without disturbing the osmolarity gradient necessary for urine formation. Plasma from the efferent arterioles flows from outer medulla to inner medulla in the descending limbs of the vasa recta, and then from inner medulla to outer medulla in the ascending limbs of the vasa recta. Control of body sodium content is a vital function of the kidneys, since it is a major determinant of body fluid volume. Humans are able to conserve sodium (Na+) very effectively, and urinary losses can be less than 1 mmol LÀ1. However, maximal sodium reabsorption can increase the excretion of K+ and H+, and so may disturb acidbase balance. Changes in Na+ excretion are normally brought about by changes in tubular reabsorption.
Syndromes
- Chemotherapy
- Irritability
- 30% severe carbon monoxide poisoning present
- Recurrent or unnoticed injury to the hand
- Shellfish, fish, nuts, eggs, milk, and other foods
- You have pain in the thighs and buttocks that does not go away
Glycosuria which has been detected on routine urine testing performed preoperatively may often be the first indication that a patient has diabetes top erectile dysfunction doctor quality tadalafilo 10 mg. As there is individual variation in the renal threshold for glucose youth erectile dysfunction treatment discount tadalafilo online, diagnosis should be confirmed by examining blood glucose erectile dysfunction normal age purchase tadalafilo 5 mg amex. The diagnosis of diabetes mellitus may be made from a random blood glucose of > 11 erectile dysfunction doctors charlotte trusted 2.5 mg tadalafilo. If the patient is known to have diabetes erectile dysfunction non prescription drugs generic 5 mg tadalafilo with mastercard, control may be assessed from measurement of glycosylated haemoglobin (HbA1c), as this reflects blood glucose control over the previous 68 weeks. An elevated preoperative HbA1c is associated with adverse outcomes, but there is insufficient evidence to recommend an upper limit prior to elective surgery. The risks of proceeding when control is suboptimal should be balanced against the urgency of the procedure. An upper limit between 64 and 75 mmol mol1 is acceptable, depending on individual circumstances. Postponement of surgery and referral to the local diabetes specialist team may be appropriate. The long-term complications of diabetes are equally likely in both type 1 and type 2, and are related to the duration of the disease and the effectiveness of blood sugar control. Complications are due to disease of both large blood vessels (atheroma) and small blood vessels (microangiopathy). Atheroma causes the same pathological changes as in non-diabetic patients, but the disease occurs earlier and is both more extensive and more severe. Diabetic microangiopathy is the cause of diabetic nephropathy, retinopathy and neuropathy. Diabetes is a common cause of autonomic neuropathy, which can be detected at the bedside by demonstrating postural hypotension. Diabetic patients frequently present for surgery for the complications of their disease, and preoperative assessment must include screening for evidence of other complications. Serum urea, electrolytes and creatinine should be performed to assess renal function. While some type 2 diabetics are managed by diet alone, most will require one or more oral hypoglycaemic drugs as well as diet, and around a third will end up on insulin. A variety of different types of oral hypoglycaemic drugs can be used, most of which depend on the presence of some endogenous insulin. The commonly used sulphonylureas include glibenclamide, gliclazide and tolbutamide. Metformin is the only available biguanide and is often used in conjunction with a sulphonylurea. Hypoglycaemia is very unusual with metformin, although it may cause lactic acidosis. Acarbose inhibits intestinal -glucosidases, delaying the digestion and absorption of starch and sucrose. The two main types of insulin preparation are unmodified, rapid-onset, short-acting (soluble) insulin and modified, delayed-onset, intermediate- or long-acting insulin. It may involve twice-daily or multiple injections of a combination of short- and longer-acting insulins before meals and at bedtime. Soluble insulin is the only form which can be given intravenously as well as subcutaneously and it is used for perioperative control of blood glucose. The management of diabetic patients presenting for surgery, including which drugs should be omitted on the day of surgery to prevent hypoglycaemia, is covered in Chapter 5. E Have you ever taken a drink in the morning to steady your nerves or ease a hangover A score greater than 2 prompts a more targeted history, examination and investigation pertaining to alcoholrelated disease. History and examination should focus on the possible cardiac and neurological manifestations of alcohol-related disease. In particular, evidence of cardiac failure and rhythm disturbance should be sought. Pre-existing neuropathies need to be noted and carefully documented, particularly in patients likely to be undergoing regional anaesthesia. Investigation should include baseline blood investigations along with liver function tests and coagulation studies. Further haematological investigation may be indicated following a full blood count. An echocardiogram may be indicated if there are concerns regarding ventricular function. Most hospitals will have local guidelines as to the management of these patients, some of whom may require a benzodiazepine, typically chlordiazepoxide. Obesity Obesity continues to challenge us perioperatively and can represent a considerable anaesthetic and surgical risk. Obese patients comprise a high-risk group not just in terms of their practical anaesthesia management but also because of their associated comorbidities. Careful, targeted preoperative assessment enables us to address such comorbidities in order to guide perioperative management and evaluate risk. Obese patients are particularly at risk in terms of cardiorespiratory disease, metabolic disease and thromboembolism. Alcohol-related disease As alcohol misuse increases as a social problem, so does the prevalence of alcohol-related disease. While alcoholic liver disease may be the most obvious manifestation, there are many other potential associated conditions. These include cardiac disease such as cardiomyopathy and rhythm disturbances, haematological abnormalities, and metabolic disturbance. Cardiac disease Hyperlipidaemia is common in obese patients and may underlie ischaemic heart disease. It poses a series of questions regarding sleeping habits and determines likelihood of falling asleep during various activities in the daytime, such as while sitting reading or watching television, and reported snoring or apnoea. Thus a risk assessment may be carried out very easily in the preoperative assessment clinic using the questionnaire along with a history of snoring or sleep apnoea. A glycosylated haemoglobin will give an indication as to adequacy of blood sugar control. Some preoperative assessment clinics are able to arrange for specialist dietary advice, although time does not always allow for this. History-taking can be challenging in terms of establishing functional tolerance in these patients. Immobility due to obesity in itself can make it difficult to elicit symptoms such as angina and breathlessness which might normally alert us to cardiac ischaemia or cardiac failure. Cardiopulmonary exercise testing may be helpful in assessing functional capacity but, again, obesity in itself may hamper such investigations. Venous thromboembolism A venous thromboembolism risk assessment is now a routine part of the preoperative preparation process. It is important that obese patients receive prophylaxis appropriate to their weight and the planned surgical procedure. Respiratory disease Pre-existing respiratory disease in obese patients carries significant additional risk, both for anaesthesia itself and postoperatively. A baseline assessment for patients with chronic obstructive airways disease may be indicated in the form of pulmonary function testing. This will provide information regarding reversibility and may indicate the need for a formal assessment by a respiratory physician. It must be remembered that these patients have considerably reduced respiratory reserve and will potentially desaturate rapidly in the anaesthetic room during induction of anaesthesia, and indeed in the operating theatre when supine. Regional anaesthesia often provides a solution regarding anaesthesia for obese patients. History and examination regarding issues which might preclude central neuraxial blockade are important, along with consideration of possible contraindications. Early liaison with the anaesthetist and theatre staff will ensure that optimal, timely preparation can be put in place for such patients. Increasingly, morbidly obese patients are presenting for surgery having already undergone bariatric surgery. It may be necessary for intervention by the bariatric surgery team prior to the non-bariatric surgery. Some units advise elective deflation prior to general anaesthesia and surgery, although this is by no means always the case and will depend upon the nature of the surgical procedure. Most of these patients will have been provided with a contact number, and liaison with the bariatric surgery unit is generally encouraged to discuss the need for deflation. Concurrent medication Concurrent medication may interact with drugs administered during anaesthesia. Furthermore, the surgical procedure itself may be affected by, or indeed affect, such medication. For this reason it is important that careful consideration is given to preoperative drug management. Alternatively, anaesthetic technique may have to be modified to minimise the risk of adverse interaction. Examples of drugs that should be continued are anticonvulsants, most cardiovascular drugs (antihypertensives, antianginals, antiarrhythmics), bronchodilators, corticosteroids and antiparkinsonian drugs. It is seldom necessary to stop drugs preoperatively, but a number of possible exceptions are worthy of discussion. Warfarin should be stopped several days preoperatively and the patient heparinised. To minimise the risk of thromboembolism oral contraceptives and hormone replacement therapy are often stopped several weeks before surgery. Most drugs that have been stopped preoperatively can be restarted when oral intake resumes. Should this be delayed, alternative routes of administration may have to be sought. It is occasionally necessary to modify dose and formulation of a drug perioperatively, as is the case with corticosteroid therapy. Adrenal suppression has not been reported with prednisolone doses below 5 mg daily. Patients on higher doses undergoing major surgery will require additional corticosteroid support administered as intravenous hydrocortisone. Stopping these drugs 3 weeks prior to anaesthesia, to allow resynthesis of the enzyme, is no longer considered necessary, but anaesthetic technique may need to be modified. Tricyclic antidepressants competitively block noradrenaline reuptake by postganglionic sympathetic nerve endings. Patients taking these drugs are hence more sensitive to catecholamines, so sympathomimetics may cause hypertension and arrhythmias. Similarly, heparin administration should be delayed for a period of 6 hours following central nerve blockade. Increasingly, patients with cardiac and peripheral or cerebral vascular disease present for surgery while taking clopidogrel, a potent platelet antagonist. This must be noted at preoperative assessment, as withdrawal is frequently required prior to anaesthesia and surgery. Anaesthetic risk relates mainly to regional anaesthetic techniques and the possibility of vertebral canal haematoma following epidural or spinal anaesthesia. While platelet antagonists should generally be stopped at least 7 days before elective surgery, the underlying reason for their use must be considered. This is particularly the case for patients taking clopidogrel following percutaneous coronary artery stenting within the last 12 months. Chapter 1: Preoperative management 27 When aspirin is prescribed for secondary prevention in cardiac and cerebrovascular disease preoperative stoppage is rarely necessary for non-neurosurgical procedures. Most hospitals have guidelines in place regarding perioperative aspirin management, and these should be sought if preoperative stoppage is being considered. These drugs may not be declared by patients and should be actively sought at preoperative assessment. A number of such drugs are associated with complications such as bleeding, stroke and myocardial infarction, as well as interaction with more conventional drugs. Garlic is a platelet inhibitor with potentially beneficial effects on blood pressure as well as serum lipid and cholesterol levels. There may be increased bleeding risk, particularly if it is taken along with more conventional platelet antagonists. Effects are believed to be mediated by hypericin and hyperforin and result in the inhibition of serotonin, noradrenaline and dopamine reuptake. A central serotonin syndrome can be precipitated, characterised by autonomic, neuromuscular and cognitive effects. Enzyme induction is an important feature of this drug and may affect many of the drugs used during anaesthesia. These patients may be dehydrated and possibly hypovolaemic due to gastrointestinal losses or to third space losses into the gut. Inappropriate intravenous fluid therapy on a surgical ward may have exacerbated the problems. Fluid and electrolyte disturbances should be corrected prior to theatre, and preoperative chest physiotherapy may be useful. A nasogastric tube should be inserted before induction of anaesthesia in an attempt to empty the stomach and decrease the risk of perioperative regurgitation and aspiration. Acute abdominal emergencies All patients with an acute abdomen from whatever cause are at increased risk of regurgitation of stomach contents, and so a nasogastric tube should be inserted prior to theatre. Guidelines for pre-operative cardiac risk assessment and perioperative cardiac management in non-cardiac surgery. Concurrent surgical disease Intestinal obstruction Patients with intestinal obstruction often have electrolyte disturbances due to vomiting or, in the case of incomplete obstruction, diarrhoea. The measurement of adult blood pressure and management of hypertension before elective surgery: Joint Guidelines from the Association of Anaesthetists of Great Britain and Ireland and the British Hypertension Society.
Order tadalafilo american express. Got Diabetes and Erectile Dysfunction? Go Vegan!.
References
- Segura, J.W., Preminger, G.W., Assimos, D.G. et al. Ureteral Stones Clinical Guidelines Panel summary report on the management of ureteral calculi. The American Urological Association. J Urol 1997;158:1915-1921.
- Suffredini AF, et al. The cardiovascular response of normal humans to the administration of endotoxin. N Engl J Med. 1989;321:280-287.
- Keim DR, Hernandez RJ, Sullivan DB. Serial magnetic resonance imaging in juvenile dermatomyositis. Arthritis Rheum. 1991;34:1580-1584.
- Fernando HC, Santos RS, Benfield JR, et al. Lobar and sublobar resection with and without brachytherapy for small stage IA non-small cell lung cancer. J Thorac Cardiovasc Surg 2005; 129: 261-267.
- Rassweiler JJ, Subotic S, Feist-Schwenk M, et al: Minimally invasive treatment of ureteropelvic junction obstruction: long-term experience with an algorithm for laser endopyelotomy and laparoscopic retroperitoneal pyeloplasty, J Urol 177:1000, 2007.
