
Diflucan
| Contato
Página Inicial
Edmond Bedrossian, DDS, FACS, FACOMS
- Assistant Professor, Dugoni School of Dentistry
- Director, Implant Training
- Department Oral Maxillofacial Residency Training Program
- Private Practice, San Francisco, California
Her chest x-ray shows pneumonia fungus gnats rid diflucan 200 mg purchase visa, and respiratory cultures are positive for Aspergillus fumigatus baking soda antifungal buy diflucan online pills. Itraconazole is the treatment of choice in patients with mild/moderate acute pulmonary histoplasmosis who have had symptoms for more than 1 month fungus games order genuine diflucan online. Micafungin fungus games buy diflucan without prescription, terbinafine antifungal jock itch spray order diflucan 100 mg online, and griseofulvin are not active for this type of infection. Anidulafungin alone Amphotericin B plus flucytosine Flucytosine alone Isavuconazole plus anidulafungin Correct answer = B. The treatment of choice for initial therapy for cryptococcal meningitis is the combination of 1240 amphotericin B and flucytosine. Flucytosine should not be given alone because of the rapid development of resistance. Oral fluconazole Topical miconazole Oral terbinafine Topical efinaconazole Correct answer = A. Terbinafine and efinaconazole are not used clinically for vulvovaginal candidiasis. Caspofungin is the only drug listed that requires a loading dose before starting the maintenance dosing. They lack both a cell wall and a cell membrane, and they do not carry out metabolic processes. Viruses use much of the metabolic machinery of the host, and few drugs are selective enough to prevent viral replication without injury to the infected host cells. Therapy for viral diseases is further complicated by the fact that clinical symptoms appear late in the course of the disease, at a time when most of the virus particles have replicated. At this stage of viral infection, administration of drugs that block viral replication has limited effectiveness in many cases. However, a few virus groups respond to available antiviral drugs, and some antiviral agents are useful as prophylactic agents. Mechanism of action Influenza viruses employ a specific neuraminidase that is inserted into the host cell membrane for the purpose of releasing newly formed virions. Oseltamivir and zanamivir selectively inhibit neuraminidase, thereby preventing the release of new virions and their spread from cell to cell. Pharmacokinetics Oseltamivir is an orally active prodrug that is rapidly hydrolyzed by the liver to its active form. Resistance Mutations of the neuraminidase enzyme have been identified in adults treated with either of the neuraminidase inhibitors. Due to widespread resistance, the adamantanes are not recommended in the United States for the treatment or prophylaxis of influenza A. Adverse effects Adverse effects of ribavirin include dose-dependent transient anemia. The aerosol may be safer, although respiratory function in infants can deteriorate quickly after initiation of aerosol treatment. Treatment of Hepatic Viral Infections the hepatitis viruses currently identified (A, B, C, D, and E) each have a pathogenesis, which specifically involves replication in and destruction of hepatocytes. Interferons Interferons are a family of naturally occurring, inducible glycoproteins that interfere with the ability of viruses to infect cells. In "pegylated" formulations, bis-monomethoxy polyethylene glycol has been covalently attached to interferon- to increase the size of the molecule. The principal dose-limiting toxicities are bone marrow suppression, severe fatigue and weight loss, neurotoxicity characterized by somnolence and behavioral disturbances, autoimmune disorders such as thyroiditis and, rarely, cardiovascular problems such as heart failure. Lamivudine must be phosphorylated by host cellular enzymes to the triphosphate (active) form. As with many nucleotide analogs, the intracellular half-life of the triphosphate is many hours longer than its plasma half-life. Adefovir is administered once daily and is renally excreted via glomerular filtration and tubular secretion. As with other agents, discontinuation of adefovir may result in severe exacerbation of hepatitis. Adefovir is no longer recommended in current hepatitis B guidelines due to lower efficacy compared to other agents. The drug is primarily excreted unchanged in the urine and dosage adjustments are needed in renal dysfunction. The polyprotein is then cleaved by cellular and viral proteases to yield structural and nonstructural proteins. With combination therapy, the agents are collectively able to suppress both wild-type and drug-resistant viral populations. For a summary of current guidelines and regimens recommended in specific scenarios, see Ribavirin, a guanosine analogue, improves viral clearance, decreases relapse rates, and improves rates of sustained virologic response when used in combination with other agents. The dose of ribavirin is always weight-based, and it is administered in two daily divided doses with food. Treatment of Herpes Virus Infections Herpes viruses are associated with a broad spectrum of diseases, for example, cold sores, viral encephalitis, and genital infections. The drugs that are effective against these viruses exert their actions during the acute phase of viral infections and are without effect during the latent phase. It is also given prophylactically to seropositive patients before bone marrow transplant and post-heart transplant to protect such individuals from herpetic infections. The monophosphate analog is converted to the di- and triphosphate forms by the host cell kinases. Adverse effects Adverse effects of acyclovir treatment depend on the route of administration. Transient renal dysfunction may occur at high doses or in a dehydrated patient receiving the drug intravenously. Slow elimination of the active intracellular metabolite permits prolonged dosage intervals and eliminates the permanent venous access needed for ganciclovir therapy. Instead, it is a pyrophosphate derivative and does not require activation by viral (or cellular) kinases. It is dispersed throughout the body, and greater than 10% enters the bone matrix, from which it slowly disperses. In addition, hypokalemia, hypo- and hyperphosphatemia, seizures, and arrhythmias have been reported. Mechanism of action Like acyclovir, ganciclovir is activated through conversion to the nucleoside triphosphate by viral and cellular enzymes. Like valacyclovir, valganciclovir has high oral bioavailability, because rapid hydrolysis in the intestine and liver after oral administration leads to high levels of ganciclovir. Ganciclovir is carcinogenic as well as teratogenic and carries a boxed warning for use in pregnancy. Penciclovir triphosphate has an intracellular half-life much longer than acyclovir triphosphate. Penciclovir is negligibly absorbed upon topical application and is well tolerated. There are five classes of antiretroviral drugs, each of which targets one of the four viral processes. Selection of the appropriate combination is based on 1) avoidance of the use of two agents of the same nucleoside analog; 2) avoidance of overlapping toxicities and genotypic and phenotypic characteristics of the virus; 3) patient factors, such as disease symptoms and concurrent illnesses; 4) impact of drug interactions; and 5) ease of adherence to the regimen. Cobicistat inhibits the metabolism of elvitegravir, thereby increasing its concentration in the plasma. Because of these mitochondrial toxicities, didanosine and stavudine are rarely used in current antiretroviral regimens. Sensitized individuals should never be rechallenged with abacavir because of rapidly appearing, severe reactions that may lead to death. Because cross-resistance and antagonism occur between agents of the same analog class (thymidine, cytosine, guanosine, and adenosine), concomitant use of agents with the same analog target is contraindicated (for example, zidovudine and stavudine are both analogs of thymidine and should not be used together). For example, efavirenz is safe to use in patients co-infected with tuberculosis because of its lower potential for drug interactions with rifamycins, and rilpivirine has the smallest tablet size, making it ideal for patients with difficulty swallowing. Delavirdine and nevirapine are rarely used due to toxicities and/or inferior antiviral efficacy. Due to their high genetic barrier to resistance, protease inhibitors are recommended in initial regimens in certain clinical situations (for example, patients with uncertain adherence or when resistance testing results are not yet available). Green background indicates years in which combination antiretroviral therapy came into common usage. Overview these potent agents have several common features that characterize their pharmacology. The inhibition prevents maturation of the viral particles and results in the production of noninfectious virions. Resistance Resistance occurs as an accumulation of stepwise mutations of the protease gene. Thus, unboosted atazanavir is contraindicated with concurrent use of proton pump inhibitors, and administration must be spaced apart from H2blockers and antacids. Enfuvirtide is a polypeptide that binds to gp41, preventing the conformational change. Enfuvirtide, in combination with other antiretroviral agents, is indicated for therapy of treatment-experienced patients with evidence of viral replication despite ongoing antiretroviral drug therapy. The drug has been associated with severe hepatotoxicity, which may be preceded by a fever or rash. The half-life of elvitegravir is 3 hours when administered alone, but increases to approximately 9 hours when boosted by cobicistat. Cobicistat may also cause elevations in serum creatinine due to inhibition of tubular creatinine secretion. Oseltamivir is the best choice since it is administered orally and not associated with resistance. Valacyclovir, famciclovir, penciclovir, and acyclovir are all indicated for herpes simplex virus infection. Integrase inhibitors Nonnucleoside reverse transcriptase inhibitors Protease inhibitors Entry inhibitors 1298 Correct answer = A. Integrase inhibitors bind to other positively charged ions, rendering them ineffective. As such, separation of doses of these agents from aluminum-, magnesium-, and calcium-containing antacids is recommended. His prescriber would like to change his therapy to elvitegravir/cobicistat/emtricitabine/tenofovir alafenamide. Which information should the prescriber provide to the patient that best summarizes the advantage of tenofovir alafenamide over tenofovir disoproxil fumarate Removal of food restrictions Fewer drug interactions Twice daily dosing Improved renal and bone safety profile Correct answer = D. Tenofovir alafenamide delivers the same active drug as tenofovir disoproxil fumarate, but with a lower incidence of renal and bone adverse effects. Both tenofovir-containing combinations are dosed once daily and should be taken with food. Which is the most appropriate information for the patient regarding use of a proton pump inhibitor during treatment with ledipasvir/sofosbuvir A proton pump inhibitor can be safely administered with ledipasvir/sofosbuvir without regard to timing of the dose or food intake. The patient should either stop using the proton pump inhibitor or take it with ledipasvir/sofosbuvir under fasted conditions. Overview It is estimated that over 25% of the population of the United States will face a diagnosis of cancer during their lifetime, with more than 1. However, in most cases, drug therapy will produce only a regression of the disease, and complications and/or relapse may eventually lead to death. Thus, the overall 5-year survival rate for cancer patients is about 68%, ranking cancer second only to cardiovascular disease as a cause of mortality. Principles of Cancer Chemotherapy Cancer chemotherapy strives to cause a lethal cytotoxic event or apoptosis in the cancer cells that can arrest the progression of tumor growth. Ideally, anticancer drugs should interfere only with cellular processes that are unique to malignant cells. Unfortunately, most traditional anticancer drugs do not specifically recognize neoplastic cells but, rather, affect all kinds of proliferating cells, both normal and abnormal. Therefore, almost all antitumor agents have a steep doseresponse curve for both therapeutic and toxic effects. While this strategy is showing great promise, adverse effects are also a concern and present as autoimmune toxicity, as compared to the myelosuppressive profile with traditional chemotherapy agents. Goals of treatment the ultimate goal of chemotherapy is a cure (that is, long-term, disease-free survival). If a cure is not attainable, then the goal becomes control of the disease (prevent the cancer from enlarging and spreading) to extend survival and maintain quality of life. Thus, the individual maintains a "near-normal" existence, with the cancer treated as a chronic disease. In advanced stages of cancer, the likelihood of controlling the cancer is low, and the goal is palliation (alleviation of symptoms and avoidance of life-threatening toxicity). This means that chemotherapeutic drugs may be used to relieve symptoms caused by the cancer and improve the quality of life, even though the drugs may not extend survival. The goal of treatment should always be kept in mind, as it often influences treatment decisions. Indications for treatment Chemotherapy is sometimes used when neoplasms are disseminated and are not amenable to surgery. Chemotherapy given prior to the surgical procedure in an attempt to shrink the cancer is referred to as neoadjuvant chemotherapy, and chemotherapy given in lower doses to assist in prolonging remission is known as maintenance chemotherapy. Tumor susceptibility and the growth cycle the fraction of tumor cells that are in the replicative cycle ("growth fraction") influences susceptibility to most cancer chemotherapeutic agents. However, the number of cells that are in various stages of the cycle may differ in normal and neoplastic tissues. Although the nonspecific drugs generally have greater toxicity in cycling cells, they are also useful against tumors that have a low percentage of replicating cells. This is due to a deficiency of nutrients and oxygen caused by inadequate vascularization and lack of blood circulation.
Colloidal Minerals. Diflucan.
- How does Colloidal Minerals work?
- Mineral deficiencies, low energy, diabetes, arthritis, reducing blood cell clumping, reversing early cataracts, turning gray hair dark again, flushing poisonous heavy metals from the body, improving general well being, reducing aches and pains, and other conditions.
- Are there safety concerns?
- Dosing considerations for Colloidal Minerals.
- What is Colloidal Minerals?
Source: http://www.rxlist.com/script/main/art.asp?articlekey=96421
Thus fungus dandruff purchase diflucan us, the absorption rates were considered exceedingly low fungus gnats on orchids diflucan 200 mg purchase overnight delivery, especially when compared with orally administered aspirin fungus we eat purchase 200 mg diflucan overnight delivery, and of dubious dependability (2) fungus resistant grass purchase diflucan master card. Because of the possibility of chemical and/or physical interactions between the medicinal agent and the suppository base fungus gnats damage plants order generic diflucan pills, which may affect the stability and/or bioavailability of the drug, the absence of any drug interaction between the two agents should be ascertained before or during formulation. Morphine sulfate in slow-release suppositories is prepared by compounding pharmacists. The base includes a material such as alginic acid, which will prolong the release of the drug over several hours (1). Of course, one of the first requisites for a suppository base is that it should remain solid at room temperature but soften, melt, or dissolve readily at body temperature so that the drug is fully available soon after insertion. Fat-soluble drugs seem to be released more readily from bases of glycerinated gelatin or polyethylene glycol, both of which dissolve slowly in body fluids. Particle Size For undissolved drugs in a suppository, the size of the drug particle will influence its rate of dissolution and its availability for absorption. As indicated many times previously, the smaller the particle, the greater the surface area, the more readily the dissolution of the particle and the greater the chance for rapid absorption. Nature of the Base As indicated earlier, the base must be capable of melting, softening, or dissolving to release its drug for absorption. Also, if the base irritates the mucous membranes of the rectum, it may initiate a colonic response and prompt a bowel movement, eliminating the prospect of complete drug release and absorption. Fatty or Oleaginous Bases Fatty bases are perhaps the most frequently employed suppository bases, principally because cocoa butter is a member of this group of substances. Among the other fatty or oleaginous materials used in suppository bases are many hydrogenated fatty acids of vegetable oils, such as palm kernel oil and cottonseed oil. Also, fatbased compounds containing compounds of glycerin with the highermolecular-weight fatty acids, such as palmitic and stearic acids, may be found in fatty bases. Such compounds, such as glyceryl monostearate and glyceryl monopalmitate, are examples of this type of agent. Some bases are prepared with the fatty materials emulsified or with an emulsifying agent present to prompt emulsification when the suppository makes contact with the aqueous body fluids. At room temperature, it is a yellowish-white solid having a faint, agreeable chocolate-like odor. However, because of its triglyceride content, cocoa butter exhibits marked polymorphism, or existence in several crystalline forms. Because of this, when cocoa butter is hastily or carelessly melted at a temperature greatly exceeding the minimum required temperature and is then quickly chilled, the result is a metastable crystalline form (alpha crystals) with a melting point much lower than that of the original cocoa butter. In fact, the melting point may be so low that the cocoa butter will not solidify at room temperature. If the melting point is low enough that it is not feasible to prepare a solid suppository using cocoa butter alone as the base, solidifying agents like cetyl esters wax (about 20%) or beeswax (about 4%) may be melted with the cocoa butter to compensate for the softening effect of the added substance. However, the addition of hardening agents must not be so excessive as to prevent the base from melting in the body, nor must the waxy material interfere with the therapeutic agent in any way so as to alter the efficacy of the product. Other bases in this category include commercial products such as Fattibase (triglycerides from palm, palm kernel, and coconut oils with selfemulsifying glyceryl monostearate and polyoxyl stearate), the Wecobee bases (triglycerides derived from coconut oil) and Witepsol bases (triglycerides of saturated fatty acids C12C18 with varied portions of the corresponding partial glycerides). A glycerinated gelatin base is most frequently used in preparation of vaginal suppositories, with which prolonged local action of the medicinal agent is usually desired. Because glycerinated gelatinbased suppositories have a tendency to absorb moisture as a result of the hygroscopic nature of glycerin, they must be protected from atmospheric moisture if they are to maintain their shape and consistency. Also as a result of the hygroscopicity of the glycerin, the suppository may have a dehydrating effect and irritate the tissues upon insertion. The water in the formula for the suppositories minimizes this action; however, if necessary, the suppositories may be moistened with water prior to insertion to reduce the initial tendency of the base to draw water from the mucous membranes and irritate the tissues. Urethral suppositories may be prepared from a glycerinated gelatin base of a formula somewhat different from the one indicated earlier. Urethral suppositories of glycerinated gelatin are much more easily inserted than those with a cocoa butter base owing to the brittleness of cocoa butter and its rapid softening at body temperature. Melting ranges for the polyethylene glycols follow: 300 400 600 1000 1450 3350 4600 6000 8000 15°C 18°C 4°C 8°C 20°C 25°C 37°C 40°C 43°C 46°C 54°C 58°C 57°C 61°C 56°C 63°C 60°C 63°C Various combinations of these polyethylene glycols may be combined by fusion, using two or more of the various types to achieve a suppository base of the desired consistency and characteristics. This property permits a slower release of the medication from the base once the suppository has been inserted, and permits convenient storage of these suppositories without need for refrigeration and without danger of their softening excessively in warm weather. Further, their solid nature permits slow insertion without fear that they will melt in the fingertips (as cocoa butter suppositories sometimes do). Polyethylene glycol suppositories that do not contain at least 20% water should be dipped in water just before use to avoid irritation of the mucous membranes after insertion. Miscellaneous Bases In the miscellaneous group of bases are mixtures of oleaginous and water-soluble or water-miscible materials. Some are preformed emulsions, generally of the water-in-oil type, or they may be capable of dispersing in aqueous fluids. One of these substances is polyoxyl 40 stearate, a surface-active agent that is employed in a number of commercial suppository bases. Other surface-active agents useful in the preparation of suppository bases also fall into this broad grouping. Mixtures of many fatty bases (including cocoa butter) with emulsifying agents capable of forming water-in-oil emulsions have been prepared. The method most frequently employed both on a small scale and on an industrial scale is molding. Other molds, such as those most commonly found in the community pharmacy, are capable of producing 6, 12, or more suppositories in a single operation. Molds in common use today are made from stainless steel, aluminum, brass, or plastic. The molds, which separate into sections, generally longitudinally, are opened for cleaning before and after preparation of a batch of suppositories, closed when the melt is poured, and opened Suppository Molds Commercially available molds can produce individual or large numbers of suppositories of various shapes and sizes. Although satisfactory reusable and disposable molds are commercially available for preparation of rectal, vaginal, and urethral suppositories, if necessary, temporary molds may be successfully formed by pressing heavy aluminum foil about an object having the shape of the desired suppository, then carefully removing the object and filling the shaped foil with the melt. The first step in calibration of a mold is to prepare molded suppositories from base material alone. After removal from the mold, the suppositories are weighed and the total weight and average weight of each suppository are recorded (for the particular base used). In determining the amount of base to be incorporated with the medicaments, the pharmacist must be certain that the required amount of drug is provided in each suppository. If the added amounts of medicaments are slight, they may be considered to be negligible, and no deduction from the total volume of base may be deemed necessary. The total volume of these materials is subtracted from the volume of the mold, and the appropriate amount of base is added. Because the bases are solid at room temperature, the volume of base may be converted to weight from the density of the material. For example, if 12 mL of cocoa butter is required to fill a suppository mold and if the medicaments in the formula have a collective volume of 2. However, no material that might irritate the mucous membranes should be employed as a mold lubricant. Similarly, any added medicinal agent alters the density of the base, and the weight of the resulting suppository differs from that of those prepared with base material alone. The pharmacist should calibrate each suppository mold for the usual base (generally cocoa butter and a polyethylene glycol base) so as to prepare medicated suppositories each having the proper quantity of medicaments. After adjusting for the preparation of an extra suppository or two, the calculated amount is weighed. Another method for determination of the amount of base in the preparation of medicated suppositories requires the following steps: (a) weigh the active ingredient for the preparation of a single suppository; (b) dissolve it or mix it (depending on its solubility in the base) with a portion of melted base insufficient to fill one cavity of the mold, and add the mixture to a cavity; (c) add additional melted base to the cavity to fill it completely; (d) allow the suppository to congeal and harden; and (e) remove the suppository from the mold and weigh it. The weight of the active ingredients subtracted from the weight of the suppository yields the weight of the base. A third method is to place all of the required medicaments for the preparation of the total number of suppositories (including one extra) in a calibrated beaker, add a portion of the melted base, and incorporate the drug substances. Then add sufficient melted base to reach the required volume of mixture based on the original calibration of the volume of the mold. Obviously, if a suppository mold of less than 2 g is used, the powder volume may need to be considered. The density factors of various bases and drugs need to be known to determine the proper weights of the ingredients to be used. If the density factor of a base is not known, it is simply calculated as the ratio of the blank weight of the base and cocoa butter. Three methods of calculating the quantity of base that the active medication will occupy and the quantities of ingredients required are illustrated here: (a) dosage replacement factor, (b) density factor, and (c) occupied volume methods. Melt the suppository base and incorporate the medication, mix, pour into molds, cool, trim, and remove from the molds. Determine the density factor as follows: Density factor = where A is the average weight of blank, B is the weight of medication per suppository, and C is the average weight of medicated suppository. The average weight of the cocoa butter blank is 2 g and the average weight of the medicated suppository is 1. Divide the total weight of active drug required for the total number of suppositories by the ratio obtained in step 3. Multiply the weight of active drug per suppository times the number of suppositories to be prepared to obtain the quantity of active drug required. Using the determination of occupied volume method, prepare the requested suppositories. Preparing and Pouring the Melt Using the least possible heat, the weighed suppository base material is melted, generally over a water bath, because not a great deal of heat is required. A porcelain casserole, that is, a dish with a pouring lip and a handle, is perhaps the best utensil, because it later permits convenient pouring of the melt into the cavities of the mold. After incorporation, this material is stirred into the remaining base, which has been allowed to cool almost to its congealing point. Any volatile materials or heat-labile substances should be incorporated at this point with thorough stirring. The melt is poured carefully and continuously into each cavity of the mold, which has been previously equilibrated to room temperature. The excessive material may form a continuous ribbon along the top of the mold above the cavities. When solidified, the excess material is evenly scraped off of the top of the mold with a spatula warmed by dipping into a beaker of warm water; this will make a smooth surface on the back of the suppository during trimming. When the suppositories are hard, the mold is removed from the refrigerator and allowed to come to room temperature. Then the sections of the mold are separated, and the suppositories are dislodged, with pressure being exerted principally on their ends and only if needed on the tips. In preparation for compression into the molds, the base and the other formulative ingredients are combined by thorough mixing, the friction of the process softening the base into a pastelike consistency. Heating the mortar in warm water (then drying it) greatly facilitates the softening of the base and the mixing. On a large scale, a similar process may be used, employing mechanical kneading mixers and a warm mixing vessel. Compression is especially suited for making suppositories that contain heat-labile medicinal substances or a great deal of substances that are insoluble in the base. In contrast to the molding method, compression permits no likelihood of insoluble matter settling during manufacture. The disadvantage to compression is that the special suppository machine is required and there is some limitation as to the shapes of suppositories that can be made. In preparing suppositories with the compression machine, the suppository mass is placed in a cylinder; the cylinder is closed; pressure is applied from one end, mechanically or by turning a wheel; and the mass is forced out of the other end into the mold or die. When the die is filled with the mass, a movable end plate at the back of the die is removed, and when additional pressure is applied to the mass in the cylinder, the formed suppositories are ejected. The end plate is returned and the process is repeated until all of the mass has been used. It is possible to prepare suppositories of uniform circumference by extrusion through a perforated plate and by cutting the extruded mass to the desired length. Base: glycerin, glyceryl monopalmitate, glyceryl monostearate, hydrogenated fatty acids of coconut and palm kernel oils Pruritus ani, inflamed hemorrhoids, other inflammatory conditions of the anorectum. Base: glycerin, monopalmitate, glyceryl monostearate, hydrogenated fatty acids of coconut and palm kernel oils Antihistamine, antiemetic, sedative: used to manage allergic conditions; preoperative or postoperative sedation or nausea and vomiting; motion sickness. As noted earlier, drugs like aspirin given for pain, ergotamine tartrate for treating migraine headaches, theophylline as a smooth muscle relaxant in treating asthma, and chlorpromazine and prochlorperazine, which act as antiemetics and tranquilizers, are intended to be absorbed into the general circulation to provide systemic effects. Many commercial hemorrhoidal suppositories contain a number of medicinal agents, including astringents, protectives, anesthetics, lubricants, and others, intended to relieve the discomfort of the condition. Cathartic suppositories are contact-type agents that act directly on the colonic mucosa to produce normal peristalsis. Suppositories of bisacodyl are usually effective within 15 minutes to an hour, and glycerin suppositories usually within a few minutes following insertion. Some commercially prepared suppositories are available for both adult and pediatric use. Pediatric suppositories are more narrow and pencil-shaped than the typical bullet-shaped adult suppository. Then the sodium stearate is dissolved with stirring in the hot glycerin, the purified water added, and the mixture immediately poured into the suppository mold. The sodium stearate, a soap, is the solidifying agent and may also contribute to the laxative action. The pharmacist should relate several helpful items of information about the proper use of suppositories. Glycerinated gelatin or polyethylene glycol suppositories should be moistened with water to enhance lubrication. If the polyethylene glycol suppository formulation does not contain at least 20% water, dipping it into water just prior to insertion prevents moisture from being drawn from rectal tissues and decreases irritation.
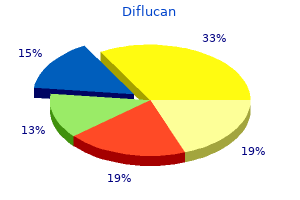
Similar to the proximal convoluted tubules (1) antifungal lacquer buy diflucan uk, the distal convoluted tubules (2 fungus gnats bug zapper buy diflucan 100 mg cheap, 4) show deep basal and lateral cell membrane infoldings and interdigitations anti yeast remedies buy diflucan 50 mg lowest price. The medullary rays include the following three types of tubules: straight (descending) segments of the proximal tubules (14) antifungal wipes diflucan 50 mg buy, straight (ascending) segments of the distal tubules (6) antifungal kit amazon buy generic diflucan 400 mg, and collecting tubules (12). The straight (descending) segments of the 703 proximal tubules (14) are very similar to the proximal convoluted tubules (1), and the straight (ascending) segments of the distal tubules (6) are similar to distal convoluted tubules (2, 4). The collecting tubules (12) in the cortex are distinct because of their lightly stained cuboidal cells and distinct cell membranes. The medulla contains only straight portions of the tubules and the segments of the loop of Henle (thick and thin descending segments and thin and thick ascending segments). The thin segments of the loops of Henle (15) are lined with a simple squamous epithelium and resemble the capillaries (13). The distinguishing features of the thin loops of Henle (15) are the thicker epithelial lining and the absence of blood cells in their lumina. Also visible in the cortex are the interlobular blood vessels (3) and the larger interlobar vein and artery (7). The interlobular blood vessels (3) give rise to the afferent glomerular arteriole (11) that enters the glomerular capsule (5b) at the vascular pole (8) and forms the capillary tuft of the glomerulus (5a). These cells are also attached to the capillaries and perform several important functions. Mesangial cells synthesize the extracellular matrix and provide structural support for the glomerular capillaries. As the blood is filtered through the glomerular 705 capillaries, numerous proteinaceous macromolecules are trapped in the glomerular basement membrane and filtration slit diaphragms. Mesangial cells function as macrophages in the intraglomerular regions by removing the trapped material from filtration slits and glomerular basal membrane, thus preventing its clogging and keeping the glomerular filter free of debris. They also phagocytose antigenantibody complexes and produce several interleukins in response to glomerular injury or damage. Mesangial cells are also contractile and regulate glomerular blood flow and pressure changes in the vascular pole region, between the afferent and efferent arterioles. Here, they are called the extraglomerular mesangial cells, also called lacis cells, and form part of the juxtaglomerular apparatus. The kidneys also produce urine, which is formed by three main functions: (1) filtration of blood in the glomeruli, (2) reabsorption of nutrients and other valuable substances from the ultrafiltrate that enters the proximal and distal convoluted tubules, and (3) secretion, or excretion, of metabolic waste products or unwanted chemicals or substances into the filtrate that become urine. Approximately 99% of the glomerular ultrafiltrate produced by the kidneys is reabsorbed into the system; the remaining 1% of the filtrate is voided as urine. In addition, kidneys have endocrine functions by producing hormones erythropoietin and renin. Endothelial cells of the peritubular capillary network in the renal cortex produce the glycoprotein hormone erythropoietin, which is a growth factor that stimulates erythrocyte production in red bone marrow in response to hypoxia, a decrease in oxygen concentration in blood or tissues. Renin is produced by kidney cells to regulate blood pressure and to maintain proper filtration pressure in the glomeruli. As the ultrafiltrate from 706 nephrons passes through the uriniferous and collecting tubules of the kidneys, it undergoes significant changes in its content and volume producing concentrated urine, containing metabolic waste products. The cells of the proximal convoluted tubules show deep infoldings of the basal cell membrane, between which are located elongated mitochondria and lateral membrane interdigitations with neighboring cells. These features are characteristic of cells involved in active transport of molecules and electrolytes from the filtrate across the cell membrane into the interstitium. Reabsorption that is both active and passive of most of the substances from the glomerular filtrate takes place in the proximal convoluted tubules, which receive the glomerular ultrafiltrate from the capsular (urinary) space of the Bowman capsule. As the glomerular filtrate enters the proximal convoluted tubules, all glucose, proteins, and amino acids; almost all carbohydrates; and about 75% to 85% of water and sodium chloride ions are absorbed from the glomerular filtrate into the surrounding interstitium and peritubular capillaries. The presence of long and closely spaced microvilli (brush border) on proximal convoluted tubule cells greatly increases the surface area and facilitates absorption of the filtered material. In addition, the proximal convoluted tubules secrete certain metabolites, hydrogen, ammonia, dyes, and drugs such as penicillin from the body into the glomerular filtrate. The metabolic waste products urea and uric acid remain in the filtrate of the proximal convoluted tubules and are eliminated from the body in the urine. Loops of Henle the descending and ascending loops of Henle of the juxtaglomerular nephrons are long, extend deep into the medulla, and have different permeabilities and different functions. As a result, hypertonic urine is produced in the tubules by an osmotic gradient in the surrounding interstitium from the cortex of the kidney to the tips of the renal papillae. Sodium chloride and urea are transported and concentrated in the interstitial tissue of the kidney medulla by means of a complex countercurrent multiplier system, which creates a high interstitial osmolarity deep in the medulla. The descending loop of Henle is permeable to water but much less to sodium chloride, whereas the thin ascending limb is permeable to sodium 707 chloride but not to water. The hypertonicity (high osmotic pressure) of the extracellular fluid in the medulla interstitium removes water from the glomerular filtrate as it flows through the descending thin tubules, thereby increasing its sodium and chloride concentration. In the ascending thin limb, water remains behind, whereas sodium chloride leaves the fluid and is concentrated in the interstitium. The countercurrent flow of ultrafiltrate in the descending and ascending thin loops of Henle produces a gradient of osmolarity in the interstitium of the medulla. The water that enters the interstitium is then removed by the countercurrent blood flow in the capillary loops of the vasa recta, thus maintaining the osmotic concentration gradient in the medulla, resulting in water conservation and urine concentration. These capillary loops are permeable to water and take up the water from the medullary interstitium to return it to the systemic circulation. Distal Convoluted Tubules the distal convoluted tubules are shorter, less convoluted than the proximal tubules, and less frequently observed in the cortex and near the renal corpuscles. In comparison with the proximal convoluted tubules, the distal convoluted tubules do not exhibit brush borders, the cells are smaller, and more nuclei are seen per tubule. The basolateral membranes of distal convoluted tubule cells also show increased cell membrane interdigitations and elongated mitochondria within these infoldings. The distal convoluted tubules actively reabsorb sodium ions from the tubular filtrate and excrete hydrogen, potassium, and ammonium ions into the tubular fluid. The excretion of hydrogen ions is connected with the absorption of bicarbonate ions and increasing the acidification of urine. Sodium reabsorption in the distal convoluted tubules is controlled by the hormone aldosterone secreted by the adrenal cortex. Aldosterone hormone induces cells of the distal convoluted tubules to actively absorb sodium and chloride ions from the filtrate and transport them into the interstitium. From the interstitium, sodium chloride ions are quickly absorbed by the peritubular capillaries and returned back to the systemic circulation, thereby decreasing sodium loss in urine. These functions of the distal convoluted tubules are vital for maintaining the proper acidbase balance of body fluids and blood. In the middle is the renal corpuscle with glomerular capillaries (5), parietal (8a) and visceral (8b) layers (epithelium) of the glomerular (Bowman) capsule (8), and the capsular space (10) around the glomerulus. Surrounding the renal corpuscle are the proximal convoluted tubules (7) with brush borders and acidophilic cells. These tubules are distinguished from the distal convoluted tubules (1, 6) that exhibit smaller and less intensely stained cells that lack the brush borders. In contrast to the convoluted tubules, the cuboidal cells of the collecting tubule (11) exhibit pale cytoplasm and distinct cell outlines. Each renal corpuscle exhibits a vascular pole where the afferent glomerular arteriole (4) enters and the efferent glomerular arteriole exits the renal corpuscle. Inside the renal corpuscle, the glomerular arteriole forms a network of glomerular capillaries (5). Here, the capsular space (10) becomes continuous with the lumen of the proximal convoluted tubule (7). The plane of section through both the vascular and urinary poles is only occasionally seen in the kidney cortex. This illustration shows the glomerular arteriole (4) on one end and the urinary pole (9) at the opposite end of the renal corpuscle. At the vascular pole, modified epithelioid cells with cytoplasmic granules replace the smooth muscle cells in the tunica media of the afferent glomerular arteriole (4). In the adjacent distal convoluted tubule, the cells next to the juxtaglomerular cells (3) are narrow and more columnar and exhibit a more compact cell arrangement. The juxtaglomerular cells (3) in the afferent glomerular arteriole (4) and the macula densa (2) cells in the distal convoluted tubule form the juxtaglomerular apparatus. The renal corpuscle consists of the glomerulus (1) and the glomerular capsule (2) with a parietal layer (2a) and a visceral layer (2b). Between these layers is the capsular space (5), with podocytes (4, 7) located on the surface of the visceral layer (2b). At the vascular pole of the renal corpuscle, blood vessels enter and leave the renal corpuscle. The juxtaglomerular apparatus (3) consists of modified smooth muscle cells of the afferent arteriole in the vascular pole, the juxtaglomerular cells (3a), and the macula densa (3b) of the distal convoluted tubule (6, 9). Surrounding the renal corpuscle are the darker-staining proximal convoluted tubules (8) and the distal convoluted tubules (6, 9). Juxtaglomerular cells are modified smooth muscle cells located in the wall of the afferent arteriole of the vascular pole of the renal corpuscle before it penetrates the glomerular capsule to form the glomerulus. The cytoplasm of juxtaglomerular cells contains membrane-bound secretory granules of the enzyme renin, which is synthesized, stored, and released into the bloodstream when needed. Opposite the afferent arteriole is the macula densa, a group of modified distal convoluted tubule cells that form a dense cluster. The macula densa cells and juxtaglomerular cells are close to each other and are separated only by a thin basement membrane allowing the juxtaglomerular cells and the macula densa closer integration of their functions. The main function of the juxtaglomerular apparatus is to maintain the necessary blood pressure, blood flow, and proper glomerular filtration in the kidney. The juxtaglomerular cells monitor the systemic blood pressure by responding to stretching in the walls of the afferent arterioles. A decrease in the blood pressure results in a decreased glomerular filtrate and decreased sodium ion concentration in the filtrate as it flows past the macula densa. A decrease in systemic blood pressure or in sodium concentration in the filtrate induces the juxtaglomerular cells to release the enzyme renin into the bloodstream. Aldosterone influences some cells of distal convoluted tubules, but mainly the cells of the collecting ducts to increase their reabsorption of sodium and chloride ions from the glomerular filtrate. Water follows sodium chloride by osmosis and increases fluid volume in the circulatory system raising the systemic blood pressure, increasing glomerular filtration rate, and decreasing the secretion of renin by juxtaglomerular cells. Aldosterone also facilitates the elimination of potassium and hydrogen ions and is an essential hormone for maintaining electrolyte balance in the body. The very long and closely packed microvilli (1) that line the apices are recognized as the brush border in the light microscopic images. The apices also exhibit a number of clear pinocytotic vesicles (6) and densestaining lysosomes (2, 5). Note that the cytoplasm of these cells is packed with mitochondria (4, 7) that provide the energy to transport the nutrients from the ultrafiltrate. The long and closely packed microvilli (1, 6) of the brush border extend into the lumen. A tight junctional complex (3) is visible as a dark strip near the base of the microvilli or the apical region of the cell. However, individual cell boundaries in the proximal tubules are not seen because of the complex interdigitations of the lateral cell walls. Also visible in the apical cytoplasm are numerous dense-staining lysosomes (4, 8), which will break down the substances that are brought into the cytoplasm by the pinocytotic vesicles (2, 7). The apical cytoplasm also exhibits numerous mitochondria (5) and a section of the nucleus (9). The flattened cell body of the podocyte (6) extends thicker primary processes (1, 3) that surround the capillary walls. The primary processes (1, 3) give rise to the smaller pedicles (2, 7), which interdigitate with pedicles from other podocytes around the capillaries. Also visible are remnants of proteinaceous debris (4) that became lodged in the filtration slits (5) during blood filtration. Surrounding the podocytes in the renal corpuscle is 714 the dark-appearing capsular space that would contain the glomerular filtrate in a functioning kidney. The nucleus (3) and cytoplasm of the podocyte (11) are separated from the adjacent basement membrane of the capillary (13). The larger primary process of the podocyte (12) extends from the podocyte cytoplasm (11) to surround the wall of the capillary. The smaller pedicles (2, 5) from the primary process of the podocyte (12) are attached to the basement membrane of the capillary (13). Separating the podocyte (3, 11) from the capillaries and adjacent podocytes is the clear capsular space (4). In the lumen of the capillary (6, 8) are the nucleus of an endothelial cell (10) 715 and sections of an erythrocyte (7) and a leukocyte (9). In the lumen of the capillary (6, 8) are also visible tiny fenestrations in the endothelium (arrowheads). The papillary ducts (3) exhibit large diameters and wide lumina and are lined with tall, pale-staining columnar cells. Also present in the papilla are the straight (ascending) segments of the distal tubules (7, 10) and the straight (descending) segments of the proximal tubules (1, 6, 11). The straight segments in the medulla are very similar to the convoluted tubules in the cortex. Interspersed among the ascending (7, 10) and descending straight tubules (1, 6, 11) are the transverse sections of the thin segments of the loop of Henle (5, 8) that resemble the capillaries (4, 9) or small venules (2). The capillaries (4, 9) and the small venules (2) differ from the thin segments of the loop of Henle (5, 8) by thinner walls and by blood cells in their lumina. The connective tissue (12) surrounding the tubules is more abundant in the 716 papillary region of the kidney, and the papillary ducts (3) are spaced further apart.
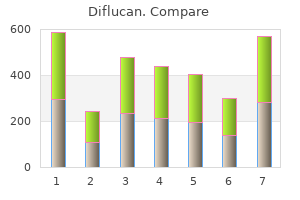
A digestive enzyme zeta antifungal generic diflucan 400 mg with amex, salivary amylase fungus ball purchase cheap diflucan online, mainly produced by the serous acini antifungal rosacea cheap 200 mg diflucan mastercard, initiates the 534 breakdown of starch into smaller carbohydrates during the time that food is in the oral cavity antifungal cream cvs generic diflucan 150 mg buy on line. Saliva also controls bacterial flora in the oral cavity and protects it against oral pathogens fungus quest ni no kuni order 50 mg diflucan overnight delivery. The bacterial enzyme, lysozyme, secreted by serous cells hydrolyzes cell walls of bacteria and inhibits their growth in the oral cavity. In addition, saliva contains salivary antibodies primarily immunoglobulin A, produced by the plasma cells located in the connective tissue of salivary glands. Salivary acinar cells secrete a protein component that binds to and transports the immunoglobulins from plasma cells in the connective tissue into saliva. The antibodies then form complexes with antigens and assist in immunologic defense against oral bacteria. As saliva flows through the duct system of salivary glands, the salivary ducts modify its ionic content by selective transport, resorption, or secretions of ions. The striated ducts actively reabsorb sodium and chloride ions from saliva, whereas potassium and bicarbonate ions, the buffering ions produced in the striated ducts, are added to the salivary secretions, forming a hypotonic saliva. The numerous infoldings of the basal cell membrane or striations in the striated ducts contain elongated mitochondria that provide the necessary energy for fluid and electrolyte transports across the cell membranes. The striated ducts of each lobule drain into interlobular or excretory ducts that eventually form the main duct for each gland, which ultimately empties its contents into the oral cavity. Intercalated ducts in salivary glands modify the saliva that passes through them by: A. Striated ducts in salivary glands modify the saliva that passes through them by: A. Although starch is in the oral cavity, amylase breaks it down before it is swallowed. The contractile myoepithelial cells surround the secretory acini and, by contracting, cause expulsion of the secretory products into the excretory ducts. The proteins secreted by acinar cells bind to and transport immunoglobulins from plasma cells into saliva. It includes the esophagus, stomach, small intestine (duodenum, jejunum, and ileum), large intestine (colon), and rectum. The wall of the digestive tube shows four distinct layers that represent the basic histologic organization of the entire tract. These layers are the mucosa, submucosa, muscularis externa, and serosa (or adventitia). Because the digestive tract performs different functions during the digestive processes, the morphology of these layers exhibits variations. These are primarily evident in the epithelium and indicate the specific functions for each section of the tract. Mucosa the mucosa is the innermost layer of the digestive tube that consists of a lining epithelium and glands that extend into the underlying layer of loose connective tissue called the lamina propria. A thin inner circular and an outer longitudinal layer of smooth muscle, called the muscularis mucosae, form the outer boundary of the mucosa. It consists of dense irregular connective tissue with numerous blood and lymph vessels and a submucosal (Meissner) nerve plexus that contains postganglionic parasympathetic neurons. The neurons and axons of the submucosal nerve plexus control the motility of the mucosa and secretory activities of mucosal glands. In the initial portion of 546 the small intestine, the duodenum, the submucosa contains numerous branched mucous glands. Muscularis Externa the muscularis externa is a thick, smooth muscle layer located inferior to submucosa. Except for the large intestine, this contains an inner layer of circular smooth muscle and an outer layer of longitudinal smooth muscle. Situated between the two smooth muscle layers are connective tissue and another nerve plexus called the myenteric (Auerbach) nerve plexus. This plexus also contains postganglionic parasympathetic neurons and controls the motility of smooth muscles in the muscularis externa. Serosa the serosa is the outermost layer of the abdominal portion of the esophagus, stomach, and small intestine and is continuous with the mesentery and the lining of the abdominal cavity. The serosa is a serous membrane of simple squamous epithelium called mesothelium and a thin underlying loose connective tissue that surrounds the visceral organs. If mesothelium covers the visceral organs, the organs are intraperitoneal and the outermost layer is called serosa. Serosa also covers ascending and descending colon only on the anterior and lateral surfaces. The posterior surfaces of the colon are bound to the posterior abdominal body wall and are not covered by the mesothelium or suspended by a mesentery. Adventitia When the digestive tube is not covered by mesothelium, it lies outside the peritoneal cavity and is called retroperitoneal. Here, the outermost layer of the organ adheres to the body wall and consists only of a connective tissue called adventitia. The characteristic features of each layer of the digestive tube and their functions are discussed in detail with illustration of the different parts of the digestive tract. After descending the thoracic cavity, the esophagus penetrates the muscular diaphragm with a short section present in the abdominal cavity before terminating at the stomach. In the thoracic cavity, the esophagus is surrounded by the connective tissue adventitia. In the abdominal cavity, a simple squamous mesothelium covers the outermost wall of the short segment of the esophagus, forming the serosa. The esophageal lumen is lined with a moist, nonkeratinized stratified squamous epithelium. An empty esophagus exhibits numerous but temporary longitudinal folds of mucosa in its lumen that are due to the contractions of the esophageal muscles. The wall of the esophagus contains two types of glands that secrete mucus; however, they are located in different parts of the organ. In the lamina propria of the proximal and distal parts of the esophagus near the stomach are the esophageal cardiac glands because they resemble the mucous glands located in the cardiac region of the stomach. In the submucosa are the esophageal glands proper that are scattered along the entire length of the esophagus. The mucus from these glands lubricates the lumen of the esophagus, protects the mucosa, and facilitates smooth passage of food material (bolus) through the esophagus to the stomach. The outer wall of the esophagus, the muscularis externa, contains both skeletal and smooth muscles fibers. In the upper third of the esophagus, both layers of the muscularis externa contain striated skeletal muscle fibers. In the middle third of the esophagus, the muscularis externa contains a mixture of both skeletal and smooth muscle fibers, whereas in the lower third of the esophagus, both layers are smooth muscle fibers. In this illustration, the upper portion of the esophagus has been sectioned in a transverse plane. The mucosa (1) of the esophagus consists an inner lining of nonkeratinized stratified squamous epithelium (1a); an underlying thin layer of fine connective tissue, the lamina propria (1b); and a layer of longitudinal smooth muscle fibers, the muscularis mucosae (1c), shown in transverse plane. The connective tissue papillae (9) of the lamina propria (1b) indent the epithelium (1a). Found in the lamina propria (1b) are small blood vessels (8), diffuse lymphatic tissue, and a small lymphatic nodule (7). The mucous acini of esophageal glands proper (2) are in the submucosa (3) at intervals throughout the length of the esophagus. The excretory ducts (10) of these glands (2) pass through the muscularis mucosae (1c) and the lamina propria (1b) to open into the esophageal lumen. The dark-staining ductal epithelium of the glands merges with the stratified squamous surface epithelium (1a) of the esophagus. Located inferior to the submucosa (3) is the muscularis externa (4), composed of two muscle layers, an inner circular muscle layer (4a) and the outer longitudinal muscle layer (4b), whose muscle fibers are shown here sectioned in a transverse plane. A thin layer of connective tissue (13) lies between the inner circular muscle layer (4a) and the outer longitudinal muscle layer (4b). In humans, the muscularis externa (4) in the upper third of the esophagus consists of striated skeletal muscles. In the middle third of the esophagus, the inner circular layer (4a) and the outer longitudinal layer (4b) exhibit a mixture of both smooth muscle and skeletal muscle fibers. The adventitia (5) consists of a loose connective tissue layer that blends with the adventitia of the trachea and the surrounding structures. Adipose tissue (14), large blood vessels, an artery and a vein (15), and nerve fibers (6) are numerous in the connective tissue of the adventitia (5). In the submucosa (7) are adipose cells and mucous acini of esophageal glands proper (6) and their excretory ducts (5). The muscularis externa consists of an inner circular layer 552 (10) and an outer longitudinal layer (14) of skeletal muscles, separated by connective tissue (11). The outermost layer is the connective tissue adventitia (8) with adipose tissue, nerves (13), a vein (9), and an artery (12). As in the upper esophagus, the mucosa (1) of the lower esophagus consists of stratified squamous nonkeratinized epithelium (1a), the connective tissue lamina propria (1b), and a smooth muscle layer muscularis mucosae (1c) (transverse section). Also visible are the connective tissue papillae (2) that indent the epithelium (1a) and a lymphatic nodule (3). The submucosa (6) contains mucous acini of the esophageal glands proper (5), their excretory ducts (4), and adipose tissue (7). The major differences between the upper and lower esophagus are seen in the next two layers. The muscularis externa (10) in the lower esophagus consists of smooth muscle layers, an inner circular muscle layer (10a) and an outer longitudinal muscle layer (10b). The outermost layer of the lower esophagus is the serosa (8) or visceral peritoneum. Serosa (8) consists of a connective tissue layer lined with a simple squamous layer mesothelium. In contrast, the connective tissue adventitia surrounds the esophagus in the thoracic 553 region. The smooth muscle fibers of the muscularis mucosae (9) exhibit a longitudinal orientation, and the fibers of the inner circular muscle layer are cut in a transverse section. The connective tissue lamina propria (8) contains numerous blood vessels, aggregates of lymphocytes, and a small lymphatic nodule (2). Connective tissue papillae (1) from the lamina propria (8) indent the surface epithelium (7). The muscularis mucosae (9) is illustrated as bundles of smooth muscle fibers sectioned in a longitudinal plane. The underlying submucosa (3, 10) contains mucous acini of esophageal glands proper (4). Small excretory ducts (11) from these glands (4), lined with a simple epithelium, join the larger excretory ducts with stratified epithelium. One of the excretory ducts joins the stratified squamous epithelium (7) of the esophageal lumen. In the submucosa (3, 10) are blood vessels (12), nerves (5), and adipose cells (6). The inner circular muscle layer (13 in the muscularis externa) consists of skeletal muscle that is illustrated in a transverse plane at the bottom of the figure. The mucosa consists of a thick but nonkeratinized stratified squamous epithelium (1), a connective tissue lamina propria (2), and a thin strip of smooth muscle muscularis mucosae (3). Below the muscularis mucosae are the esophageal glands in the submucosa, and closer to the stomach are the esophageal cardiac glands in the lamina propria. For this function, the lumen of the esophagus is lined with a protective nonkeratinized stratified squamous epithelium. The esophageal cardiac glands are in the lamina propria of the upper and lower regions of the esophagus and exhibit morphology similar to those found in the cardia of the stomach, where the esophagus terminates. Both types of glands produce mucus to lubricate the esophageal lumen and protect it during the passage of ingested solid material. The swallowed material is moved from one end of the esophagus to the other by strong muscular contractions called peristalsis. At the lower end of the esophagus, a muscular gastroesophageal sphincter constricts the lumen and prevents the regurgitation of swallowed material into the esophagus. The nonkeratinized stratified squamous epithelium (1) of the 556 esophagus abruptly changes to simple columnar, mucus-secreting gastric epithelium (10) of the cardiac region of the stomach. At the esophagealstomach junction, the esophageal glands proper (7) may be seen in the submucosa (8) with their excretory ducts (4, 6) coursing through the muscularis mucosae (5) and the lamina propria (2) of the esophagus into its lumen. In the lamina propria (2) of the esophagus near the stomach junction are the esophageal cardiac glands (3). The lamina propria of the esophagus (2) continues into the lamina propria of the stomach (12), where it is filled with glands (16, 17) and diffuse lymphatic tissue. The lamina propria of the stomach (12) is penetrated by shallow gastric pits (11) into which empty the gastric glands (16, 17). The simple tubular cardiac glands (17) are limited to the transition region, the cardia of the stomach, and are lined with pale-staining, mucus-secreting columnar cells. Below the cardiac region of the stomach are the simple tubular gastric glands (16), some showing basal branching. In contrast to the cardiac glands (17), the gastric glands (16) contain four cell types: the pale-staining mucous neck cells (13); large, eosinophilic parietal cells (14); basophilic chief or zymogenic cells (15); and several endocrine cells (not illustrated), collectively called the enteroendocrine cells. The muscularis mucosae of the esophagus (5) also continue with the muscularis mucosae of the stomach (18). In the esophagus, the muscularis mucosae (5) are usually a single layer of longitudinal smooth muscle fibers, whereas in the stomach, a second layer of the inner circular layer of smooth muscle is added. The submucosa (8, 19) and the muscularis externa (9, 21) of the esophagus are continuous with those of the stomach. Blood vessels (20) are found in the submucosa (8, 19) from which smaller blood vessels are distributed to other regions of the stomach.
150 mg diflucan order with mastercard. FURminator Deshedding Shampoo and Conditioner Review.
References
- World Health Organization. Programs and ProjectsóLeprosy Elimination. WHO 2008 [cited 11-12-2008]. Available at: http://www.who.int/lep/en/. Gasink LB, Seymour C, Blumberg EA, et al. An uncommon presentation of an uncommon disease: leprosy in a heart transplant recipient. J Heart Lung Transplant. 2006;25(7):854-856.
- Mehmood F, et al. Live three-dimensional transthoracic echocardiographic assessment of left atrial tumors. Echocardiography 2005;22(2):137-143.
- Yoshimoto H, Yano H, Kobayushi K, et al. Increased proliferative activity of osteoblasts in congenital hemifacial hypertrophy. Plast Reconstr Surg 1998;102:1605-1610.
- ACC: Report of the American College of Cardiology/AHA task force on practice guidelines (Committee on perioperative cardiovascular evaluation for noncardiac surgery), Anesth Analg 82:854, 1996.
- Lerman BB, Belardinelli L: Cardiac electrophysiology of adenosine, basic and clinical concepts, Circulation 83:1499, 1991.
