
Diovan
| Contato
Página Inicial
Linnea S. Hauge PhD
- Assistant Professor and Educational Specialist, Department of Surgery,
- Department of Medical Education, University of Michigan Medical School, Ann
- Arbor, Michigan
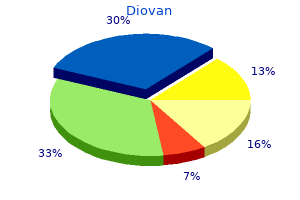
The interplay between the glucocorticoid receptor and nuclear factor-kappaB or activator protein-1: molecular mechanisms for gene repression blood pressure after eating cheap diovan 160 mg buy on-line. Repeat antenatal glucocorticoids for women at risk of preterm birth: a Cochrane Systematic Review blood pressure 6050 diovan 80 mg buy lowest price. Posttranslational modifications of proopiomelanocortin in vertebrates and their biological significance blood pressure chart resting diovan 40 mg low price. This page intentionally left blank 47 Chapter Endocrine Pancreas and Pharmacotherapy of Diabetes Mellitus and Hypoglycemia Alvin C arteria dorsalis scapulae generic diovan 40 mg line. Both genetic and environmental factors contribute to its pathogenesis blood pressure 50 over 70 diovan 160 mg buy line, which involves insufficient insulin secretion, reduced responsiveness to endogenous or exogenous insulin, increased glucose production, or abnormalities in fat and protein metabolism. The resulting hyperglycemia may lead to both acute symptoms and metabolic abnormalities. Major sources of the morbidity of diabetes are the chronic complications that arise from prolonged hyperglycemia, including retinopathy, neuropathy, nephropathy, and cardiovascular disease. These chronic complications can be mitigated in many patients by sustained control of the blood glucose and treatment of comorbidities such as hypertension and dyslipidemia (Nathan, 2014; Orchard et al. There are now a wide variety of treatment options for hyperglycemia that target different processes involved in glucose regulation or dysregulation (Nathan, 2015). Although the actions of insulin are of central importance, webs of interorgan communication via other hormones, nerves, local factors, and substrates also play vital roles. The pancreatic cell is central in this homeostatic process, adjusting the amount of insulin secreted very precisely to promote glucose uptake after meals and to regulate glucose output from the liver during fasting. The dominant regulation of hepatic glycogenolysis and gluconeogenesis is controlled by the pancreatic islet hormones insulin and glucagon. Insulin inhibits hepatic glucose production, and the decline of circulating insulin concentrations in the postabsorptive state (fasting) is permissive for higher rates of glucose output. Glucagon maintains blood glucose concentrations at physiological levels in the absence of exogenous carbohydrate (overnight and in between meals) by stimulating gluconeogenesis and glycogenolysis by the liver. Elevations of blood glucose are necessary for insulin release above basal levels, and other stimuli are relatively ineffective when plasma glucose is in the fasting range (4. Neural stimulation of insulin secretion occurs throughout the meal and contributes significantly to glucose tolerance. Arrival of nutrient chyme to the intestine leads to the release of insulinotropic peptides from specialized endocrine cells in the intestinal mucosa. Insulin secretion rates in healthy humans are highest in the early digestive phase of meals, preceding and limiting the peak in blood glucose. Some of the effects of insulin on the liver occur rapidly, within the first 20 min of meal ingestion, whereas stimulation of peripheral glucose uptake may require up to an hour to reach significant rates. In addition, catecholamines promote lipolysis, freeing fatty acids for oxidation in exercising muscle and glycerol for hepatic gluconeogenesis. This complex and highly regulated process involves the Golgi complex, the endoplasmic reticulum, and the secretory granules of the cell. The C-peptide is useful in assessment of cell secretion and to distinguish endogenous and exogenous hyperinsulinemia. Glucose, amino acids, fatty acids, and ketone bodies promote the secretion of insulin. Hepatic glucose production and lipolysis are inhibited, and total body glucose oxidation increases. The boldness of the arrows reflects relative intensity of action; a dashed line indicates little or no activity. In general, glucagon and insulin secretion are regulated in a reciprocal fashion; that is, the agents or processes that stimulate insulin secretion inhibit glucagon secretion. The effects of insulin on cell proliferation and differentiation occur over a longer period of time. The number of receptors varies from 40/cell on erythrocytes to 300,000/cell on adipocytes and hepatocytes. Insulin binding to the subunits releases this inhibition and allows transphosphorylation of one subunit by the other and autophosphorylation at specific sites from the juxtamembrane region to the intracellular tail of the receptor. The binding of insulin to its plasma membrane receptor activates a cascade of downstream signaling events. Following the facilitated diffusion into cells along a concentration gradient, glucose is phosphorylated to G6P by hexokinases. These include the following: · Normal glucose homeostasis: fasting plasma glucose < 5. Although hyperglycemia is common to all forms of diabetes, the pathogenic mechanisms leading to diabetes are quite distinct. A number of interventions, including pharmacological agents and lifestyle modification, are effective. Screening for Diabetes and Categories of Increased Risk of Diabetes Many individuals with type 2 diabetes are asymptomatic at the time of diagnosis, and diabetes is often found on routine blood testing for non glucose-related reasons. The concordance of type 1 diabetes in genetically identical twins is 40%60%, indicating a significant genetic component. However, there likely is a critical interaction of genetics and an environmental or infectious agent. The initiating or triggering stimulus for the autoimmune process is not known, but most favor exposure to viruses (enterovirus, etc. The cell destruction occurs over a period of months to years and when more than 80% of the cells are destroyed, hyperglycemia ensues and the clinical diagnosis of type 1 diabetes is made. Most patients report several weeks of polyuria and polydipsia, fatigue, and often abrupt and significant weight loss. Type 1 diabetes -cell destruction, usually leading to absolute insulin deficiency A. Endocrinopathies-acromegaly, Cushing syndrome, glucagonoma, pheochromocytoma, hyperthyroidism, somatostatinoma, aldosteronoma E. Gestational diabetes mellitus Pathogenesis of Type 2 Diabetes the type 2 diabetes condition is best thought of as a heterogeneous syndrome of dysregulated glucose homeostasis associated with impaired insulin secretion and action. Overweight or obesity is a common correlate of type 2 diabetes that occurs in about 80% of affected individuals. For the vast majority of persons developing type 2 diabetes, there is no clear inciting incident; rather, the condition is thought to develop gradually over years, with progression through an identifiable prediabetic stage. Type 2 diabetes results when there is insufficient insulin action to maintain plasma glucose levels in the normal range. Insulin action is the composite effect of plasma insulin concentrations (determined by islet cell function) and insulin sensitivity of key target tissues (liver, skeletal muscle, and adipose tissue). Graphs show data from nondiabetic individuals (blue lines) and from individuals with diabetes (red lines), comparing postprandial insulin and glucagon secretion and hepatic glucose production, and comparing the sensitivities of muscle glucose use and adipocyte lipolysis to insulin. This results in delayed secretion of insufficient amounts of insulin, allowing the blood glucose to rise dramatically after meals, and failure to restrain liver glucose release during fasting. Progressive reduction of cell mass and function explains the natural history of type 2 diabetes in most patients who require steadily increasing therapy to maintain glucose control. Insulin Resistance Insulin sensitivity is measured as the amount of glucose cleared from the blood in response to a fixed dose of insulin. Insulin sensitivity is affected by many factors, including age, body weight, physical activity levels, illness, and medications. The sensitivity of humans to the effects of insulin administration is inversely related to the amount of fat stored in the abdominal cavity; more visceral adiposity leads to more insulin resistance. Enlarged collections of adipose tissue, visceral or otherwise, are often infiltrated with macrophages and can become sites of chronic inflammation. Sedentary persons are more insulin resistant than active ones, and physical training can improve insulin sensitivity. Physical activity can decrease the risk of developing diabetes and improve glycemic control in persons who have diabetes. These mutations affect insulin receptor number, ligand binding, receptor phosphorylation, and trafficking. Insulin sensitivity is under genetic control, but it is unclear whether insulin-resistant individuals have mutations in specific components of the insulin signaling cascade or whether they have a complement of signaling effectors that operate at the lower range of normal. Abnormal secretion of the islet hormones-insufficient insulin and excessive glucagon-accounts for a significant portion of dysregulated hepatic glucose metabolism in type 2 diabetes. Increased concentrations of glucagon, especially in conjunction with hepatic insulin resistance, can lead to excessive hepatic gluconeogenesis and glycogenolysis and abnormally high fasting glucose concentrations. Despite ineffective insulin effects on hepatic glucose metabolism, the lipogenic effects of insulin in the 870 liver are maintained and even accentuated by fasting hyperinsulinemia. This contributes to hepatic steatosis and further worsening of insulin resistance. Chronic diseases of the pancreas, such as pancreatitis or cystic fibrosis, or endocrinopathies such as acromegaly and Cushing disease (see Table 472) can cause diabetes. A number of medications promote hyperglycemia or lead to diabetes by impairing either insulin secretion or insulin action (Table 473). Glycemic control is assessed using both short-term (blood glucose selfmonitoring; continuous glucose monitoring) and long-term (A1c, fructosamine) metrics. A1c reflects glycemic control over the prior 3 months, whereas measures of glycosylated serum proteins or albumin (fructosamine) reflect glycemic control over the preceding 2 weeks. The treatment goals should be individualized to the patient and take into account factors such as risk of hypoglycemia, life expectancy, age, other medical conditions, duration of diabetes, and advanced macrovascular/microvascular complications of diabetes (Cahn et al. These require hospitalization for insulin administration, rehydration with intravenous fluids, and careful monitoring of electrolytes and metabolic parameters. Microvascular complications occur only in individuals with diabetes and include retinopathy, nephropathy, and neuropathy, which are specific to diabetes. The mechanisms by which long-standing hyperglycemia causes end-organ complications are unclear. There is now compelling evidence that metabolic surgery can prevent or even reverse type 2 diabetes, with clinical trials showing greater efficacy than medical management (Rubino et al. Within the short-acting acting category, it is common to distinguish the very rapid-acting insulins (aspart, glulisine, lispro) from regular insulin. The first approach is based on formulations that slow the absorption following subcutaneous injection. There is wide variability in the kinetics of insulin action amongst individuals and even with repeated doses in the same individual. Native or regular insulin mole- cules associate as hexamers in aqueous solution at a neutral pH, and this aggregation slows absorption following subcutaneous injection. Goals should be individualized for each patient and may be different for certain patient populations (lower or higher). Subcutaneous administration of insulin delivered into the peripheral circulation can lead to near-normal glycemia but differs from physiological secretion of insulin in two major ways: · the absorption kinetics do not reproduce the rapid rise and decline of endogenous insulin in response to changes in blood glucose. Thus, the portal/peripheral insulin concentration is not physiological, and this may alter the influence of insulin on hepatic metabolism. When used to treat glycemia after meals, the short-acting analogues have lower rates of hypoglycemia and modestly improved A1c levels compared to regular insulin. Unlike regular insulin, lispro dissociates into monomers almost instantaneously following injection. Insulin aspart is formed by the replacement of proline at B28 with aspartic acid, reducing self-association. Like lispro, insulin aspart dissociates rapidly into monomers following injection. Insulin glulisine is formed when glutamic acid replaces lysine at B29 and lysine replaces asparagine at B3; these substitutions result in a reduction in self-association and rapid dissociation into active monomers. This produces a cloudy or whitish solution in contrast to the clear appearance of other insulin solutions. Two arginine residues are added to the C terminus of the B chain, and an asparagine molecule in position 21 on the A chain is replaced with glycine. When injected into the neutral pH of the subcutaneous space, aggregation occurs, resulting in prolonged, predictable, absorption from the injection site. Insulin detemir is an insulin analogue modified by the addition of a saturated fatty acid to the amino group of LysB29, yielding a myristoylated insulin. When insulin detemir is injected subcutaneously, it binds to albumin via its fatty acid chain. Insulin degludec is a modified insulin with one amino acid deleted (threonine at position B30) and is conjugated to hexadecanedioic acid via -l-glutamyl spacer at the amino acid lysine at position B29. Altering Asp3B to Lys and Lys29B to Glu produces an insulin (glulisine) with a more rapid onset and a shorter duration of action. Substituting Gly for Asn21A and lengthening the B chain by adding Arg31 and Arg32 produces a derivative (glargine) with reduced solubility at pH 7. Deleting Thr30B and adding a myristoyl group to the -amino group of Lys29B (detemir) enhances reversible binding to albumin, thereby slowing transport across vascular endothelium to tissues and providing prolonged action. Inhaled insulin (Afrezza) is formulated for inhalation using a manufacturer-specific device (Leahy, 2015). Jet injector systems that enable patients to receive subcutaneous insulin injections without a needle are available. Intravenous infusions of insulin are useful in patients with ketoacidosis or when requirements for insulin may change rapidly, such as during the perioperative period, during labor and delivery, and in intensive care situations. Short-acting insulins are the only form of the hormone used in subcutaneous insulin infusion devices. Insulin infusion devices provide a constant basal infusion of insulin and have the option of different infusion rates during the day and night to help avoid the rise in blood glucose that occurs just prior to awakening from sleep (the dawn phenomenon) and bolus injections that are programmed according to the size and nature of a meal. Pump insulin infusion devices can produce a more physiological profile of insulin replacement during exercise (where insulin production is decreased) and thus less hypoglycemia than traditional subcutaneous insulin injections provide. The technology for combining an insulin infusion device and continuous glucose monitoring is rapidly evolving with algorithms that alter the infusion rate (Thabit and Hovorka, 2016). Insulin administered as a single daily dose of long-acting insulin, alone or in combination with short-acting insulin, is rarely sufficient to achieve euglycemia. More complex regimens that include multiple injections of long-acting or short-acting insulin are needed to reach this goal. In all patients, careful monitoring of therapeutic end points directs the insulin dose used.
This remarkable period of discovery linked the Nobel Prize of von Euler in 1970 to that of Bergström blood pressure lowering diovan 80 mg purchase with amex, Samuelsson pulse jet pressure purchase diovan overnight, and Vane in 1982 heart attack 2o13 diovan 80 mg purchase online. However blood pressure medicine order diovan 80 mg visa, this distinction is not absolute; both enzymes may contribute to the generation of autoregulatory and homeostatic prostanoids during physiologic and pathophysiologic processes pulse pressure under 25 buy diovan with american express. Isoprostanes correlate with cardiovascular risk factors, and increased levels are found in a large number of clinical conditions (Milne et al. Inhibitors of Eicosanoid Biosynthesis by synthases, expressed in a relatively cell-specific fashion. The enzymes require a fatty acid substrate with two cis double bonds separated by a methylene group. Physiological Actions and Pharmacological Effects the widespread biosynthesis and myriad pharmacological actions of eicosanoids are reflected in their complex physiology and pathophysiology. Because of their short t1/2, prostanoids act locally and generally are considered not to affect systemic vascular tone directly. In the intact animal, however, increased force of contraction and increased heart rate are, in large measure, a reflex consequence of a fall in total peripheral resistance. The renal vasculature is resistant to this constrictor action, but the mesenteric vasculature is not. The total biosynthesis of TxA2, as determined by excretion of its urinary metabolites, is augmented in clinical syndromes of platelet activation, including unstable angina, myocardial infarction, and stroke. They also induce cytokine generation in eosinophils, mast cells, and dendritic cells. TxA2, generated at low levels in the normal kidney, has potent vasoconstrictor effects that reduce renal blood flow and glomerular filtration rate. Bartter syndrome is an autosomal recessive trait that manifests as hypokalemic metabolic alkalosis. Other effects include stimulation of steroid production by the adrenals, stimulation of insulin release, and thyrotropin-like effects on the thyroid. Prostanoids have a short t1/2 in the circulation, and their systemic administration produces significant adverse effects. Nonetheless, several prostanoids are of clinical utility in the following situations. Inhibitors and Antagonists Eye Prostaglandin F2 induces constriction of the iris sphincter muscle, but its overall effect in the eye is to decrease intraocular pressure by increasing the aqueous humor outflow. Apnea is observed in about 10% of neonates treated, particularly those who weigh less than 2 kg at birth. Treprostinil (t1/2 ~ 4 h) may be delivered by continuous subcutaneous or intravenous infusion. Prostaglandin E1 (alprostadil), given as an intracavernous Pulmonary Hypertension. Benveniste and his coworkers characterized the factor as a polar lipid and named it platelet-activating factor. When given intravenously, it causes hemorrhagic erosions of the gastric mucosa that extend into the submucosa. Platelet-activating factor decreases renal blood flow, glomerular filtration rate, urine volume, and excretion of Na+ without changes in systemic hemodynamics. Coronary blood flow is decreased at higher doses by the formation of intravascular aggregates of platelets or the formation of TxA2. However, the evidence of its importance as an endogenous mediator remains to be established. The pharmacology of the cytochrome P450 epoxygenase/ soluble epoxide hydrolase axis in the vasculature and cardiovascular disease. Lipoxygenase and leukotriene pathways: biochemistry, biology, and roles in disease. Platelet-activating factor, a pleiotrophic mediator of physiological and pathological processes. In 1859, Kolbe synthesized salicylic acid, and by 1874, it was being produced industrially. Hoffmann came across the earlier work of the French chemist Gerhardt, who had acetylated salicylic acid in 1853, apparently ameliorating its adverse effect profile, but without improving its efficacy, and therefore abandoned the project. It was introduced into medicine in 1886 under the name antifebrin by Cahn and Hepp, who had discovered its antipyretic action accidentally. It was introduced into therapy in 1887 and was extensively employed in analgesic mixtures until it was implicated in analgesic abuse nephropathy, hemolytic anemia, and bladder cancer; it was withdrawn in the 1980s. It can be evoked by noxious agents, infections, and physical injuries, which release damage- and pathogen-associated molecules that are recognized by cells charged with immune surveillance (Tang et al. The inflammatory response is characterized mechanistically by · transient local vasodilation and increased capillary permeability; · infiltration of leukocytes and phagocytic cells; and · resolution with or without tissue degeneration and fibrosis. Several biological anti-inflammatory therapeutics target these cytokines or their signaling pathways (see Chapter 35). The concentrations of many of these factors are increased in the synovia of patients with inflammatory arthritis. Nonsteroid drug selectivities for cyclooxygenase-1 rather than cyclooxygenase-2 are associated with human gastrointestinal toxicity: a full in vitro analysis. Pain Nociceptors, peripheral terminals of primary afferent fibers that sense pain, can be activated by various stimuli, such as heat, acids, or pressure. However, both enzymes contribute to the generation of autoregulatory and homeostatic prostanoids with important functions in normal physiology (see Chapter 37). This triggers the hypothalamus to elevate body temperature by promoting an increase in heat generation and a decrease in heat loss. They also accumulate in sites of inflammation, where the pH is lower, potentially confounding the relationship between plasma concentrations and duration of drug effect. However, such a partial platelet function also may predispose noncompliant patients on low-dose aspirin for antiplatelet therapy to thrombotic events. The unique sensitivity of platelets to inhibition by low doses of aspirin is related to their presystemic inhibition in the portal circulation before aspirin is deacetylated to salicylate on first pass through the liver (Pedersen and FitzGerald, 1984). Most coxibs have been either restricted in their use or withdrawn from the market in view of their adverse cardiovascular risk profile (Grosser et al. Aspirin begins to acetylate platelets within minutes of reaching the presystemic circulation (Pedersen and FitzGerald, 1984). In some cases, such as the propionic acid derivatives naproxen and ketoprofen, the glucuronide metabolites can hydrolyze back to form the active parent drug when the metabolite is not removed efficiently due to renal insufficiency or competition for renal excretion with other drugs. It is the permanent suppression of platelet TxA2 formation that is thought to underlie the cardioprotective effect of aspirin. Treatment with indomethacin, combined with potassium repletion and spironolactone, is associated with improvement in the biochemical derangements and symptoms. Large doses of niacin (nicotinic acid) effectively lower serum cholesterol levels, reduce low-density lipoprotein, and raise high-density lipoprotein (see Chapter 33). Epidemiological studies suggested that daily use of aspirin is associated with a 24% decrease in the incidence of colon cancer (Rothwell et al. Gastrointestinal (frequency 1/100,000 persons) characterized by hypokalemic, hypochloremic metabolic alkalosis with normal blood pressure and hyperplasia of the juxtaglomerular apparatus. These eicosanoids inhibit acid secretion by the stomach, enhance mucosal blood flow, and promote the secretion of cytoprotective mucus in the intestine. Analgesic nephropathy is a condition of Cardiovascular slowly progressive renal failure, decreased concentrating capacity of the renal tubule, and sterile pyuria. However, this use is associated with closure of the ductus arteriosus and impaired fetal circulation in utero, particularly in fetuses older than 32 weeks of gestation. Although less common in children, this cross sensitivity may occur in 10%25% of patients with asthma, nasal polyps, or chronic urticaria and in 1% of apparently healthy individuals. Aspirin Resistance All forms of treatment failure with aspirin have been collectively called aspirin resistance, but pharmacological resistance to aspirin is rare. Hepatotoxicity Liver injury occurs in 17% of adults with unintentional acetaminophen overdose (Blieden et al. By contrast, therapeutic dosing of diclofenac may be complicated by hepatotoxicity. Aspirin generally is avoided in pediatric populations Due to the possible association with Reye syndrome, aspirin and other salicylates are contraindicated in children and young adults less than 20 years of age with viral illnessassociated fever (Schrör, 2007). Acetaminophen and ibuprofen have not been implicated in Reye syndrome and are the agents of choice for antipyresis in children and youths. However, high doses of aspirin (30100 mg/kg/d) are used to treat children during the acute phase of Kawasaki disease, followed by low-dose antiplatelet therapy in the subacute phase. Therefore, acetaminophen dosing intervals need to be extended (812 h) or daily doses reduced to avoid accumulation and liver toxicity. For example, ibuprofen plasma concentrations are reduced and clearance increased (~80%) in children with cystic fibrosis. The reduction in serum albumin associated with these conditions causes an elevation of the free salicylate concentration, which may saturate renal excretion and result in salicylate accumulation to toxic levels. In this section, important characteristics of individual substances are discussed. Because aspirin is so available, the possibility of misuse and serious toxicity is underappreciated, and it remains a cause of fatal poisoning in children. Mechanism of Action the effects of aspirin are largely caused by its capacity to acetylate proteins, as described in Irreversible Cyclooxygenase Inhibition by Aspirin. Orally ingested salicylates are absorbed rapidly, partly from the stomach, but mostly from the upper small intestine. The rate of absorption is determined by disintegration and dissolution rates of the tablets administered, the pH at the mucosal surface, and gastric emptying time. Even though salicylate is more ionized as the pH is increased, a rise in pH also increases the solubility of salicylate and thus dissolution of the tablets. Rectal absorption of salicylate usually is slower than oral absorption and is incomplete and inconsistent. Salicylic acid is absorbed rapidly from the intact skin, especially when applied in oily liniments or ointments, and systemic poisoning has occurred from its application to large areas of skin. Enteric coating delays and reduces the bioavailability of aspirin by roughly half and renders absorption more variable in the presence of food (Bogentoft et al. This dose-dependent elimination is the result of the limited capacity of the liver to form salicyluric acid and the phenolic glucuronide, resulting in a larger proportion of unchanged drug being excreted in the urine at higher doses. Salicylate metabolism shows high intersubject variability due to the variable contribution of different metabolic pathways. Women frequently exhibit higher plasma concentrations, perhaps due to lower intrinsic esterase activity and gender differences in hepatic metabolism. Salicylate clearance is reduced and salicylate exposure is significantly increased in the elderly. The plasma concentration of salicylate is increased by conditions that decrease the glomerular filtration rate or reduce proximal tubule secretion, such as renal disease, or the presence of inhibitors that compete for the transport system. The total concentration of salicylate in plasma is therefore a relatively linear function of dose at lower concentrations. At higher concentrations, however, as metabolic pathways of disposition become saturated, small increments in dose can disproportionately increase plasma salicylate concentration. The analgesic-antipyretic dose of aspirin for adults is 325 1000 mg orally every 46 h. The anti-inflammatory doses of aspirin, as might be given in rheumatic fever, range from 4 to 8 g/d in divided doses. The rectal administration of aspirin suppositories may be preferred in infants or when the oral route is unavailable. After absorption, salicylates are distributed throughout most body tissues and transcellular fluids, primarily by pH-dependent processes. Hypoalbuminemia, as may occur in rheumatoid arthritis, is associated with a proportionately higher level of free salicylate in the plasma. Aspirin is bound to a more limited extent; however, it acetylates human plasma albumin in vivo by reaction with the -amino group of lysine and may change the binding of other drugs to albumin. Aspirin also acetylates other plasma and tissue proteins, but there is no evidence that this contributes to clinical efficacy or adverse events. Mesalamine is available as a rectal enema for treatment of mild-to-moderate ulcerative colitis, proctitis, and proctosigmoiditis and as a rectal suppository for the treatment of active ulcerative proctitis. Sulfasalazine (salicylazosulfapyridine) contains mesalamine linked covalently to sulfapyridine, and balsalazide contains mesalamine linked to the inert carrier molecule 4-aminobenzoyl-alanine. Sulfasalazine and olsalazine have been used in the treatment of rheumatoid arthritis and ankylosing spondylitis. Methyl salicylate (oil of wintergreen) is a common ingredient of ointments and deep-heating liniments used in the management of musculoskeletal pain; it also is available in herbal medicines and as a flavoring agent. Mesalamine (5-aminosalicylic acid) is a salicylate that is accompanied by increased Na+ and K+ excretion; plasma bicarbonate is thus lowered, and blood pH returns toward normal. Low-dose aspirin (100 mg daily) lowers car- diovascular risk and is recommended for the prevention of myocardial infarction and stroke in patients at elevated risk (see Cardioprotection section) (Patrono, 2015). At high therapeutic doses (3 g daily), salt and water retention can lead to an increase (20%) in circulating plasma volume and decreased hematocrit (via a dilutional effect). There is a tendency for the peripheral vessels to dilate because of a direct effect on vascular smooth muscle. Those with carditis or compromised cardiac function may not have sufficient cardiac reserve to meet the increased demands, and congestive cardiac failure and pulmonary edema can occur. High doses of salicylates can produce noncardiogenic pulmonary edema, particularly in older patients who ingest salicylates regularly over a prolonged period. Respiratory rate and depth increases, the Pco2 falls, and respiratory alkalosis ensues. Therapeutic doses of salicylate produce definite changes in the acid-base balance and electrolyte pattern. Gastroscopic examination of aspirin-treated subjects often reveals discrete ulcerative and hemorrhagic lesions of the gastric mucosa; in many cases, multiple hemorrhagic lesions with sharply demarcated areas of focal necrosis are observed.
160 mg diovan visa. Eye Pressure Test.
Syndromes
- Loss of bowel and bladder function
- If your blood cells stick together when mixed with anti-Rh serum, you have type Rh-positive blood.
- Complex regional pain syndrome
- Several x-rays of the gallbladder
- Red and white blood cell counts
- Phenytoin or other medications to prevent or treat seizures
- Abdominal x-ray
- Tell your doctor if you have a cold, flu, fever, or other sickness before your surgery.
- Fever and chills
References
- Celdran A, Bazire P, Garcia-Urena MA, et al: H-hernioplasty: A tension-free repair for umbilical hernia. Br J Surg 82:371, 1995.
- Cai S, Hong TS, Goldberg SI, et al. Updated long-term outcomes and prognostic factors for patients with unresectable locally advanced pancreatic cancer treated with intraoperative radiotherapy at the Massachusetts General Hospital, 1978 to 2010.
- Covino BG: Pharmacology of local anesthetic agents. Br J Anaesth 58:701-716, 1986.
- Arrabal-Martin M, Fernandez-Rodriguez A, Arrabal-Polo MA, et al: Extracorporeal renal lithotripsy: evolution of residual lithiasis treated with thiazides, Urology 68:956n959, 2006.
- Christensen R, Voepel-Lewis T, Lewis I, et al; American Heart Association's Get with the Guidelines-Resuscitation: Pediatric cardiopulmonary arrest in the post anesthesia care unit: analysis of data from the American Heart Association Get with the Guidelines-Resuscitation registry, Paediatr Anaesth 23:517-523, 2013.
