
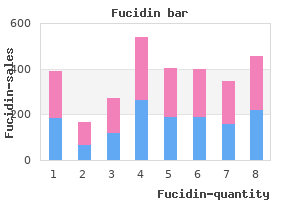
Fucidin
| Contato
Página Inicial
Neha S. Pandit, PharmD, AAHIVP, BCPS
- Associate Professor, Department of Pharmacy Practice, University of Maryland School of Pharmacy, Baltimore, Maryland
Cutaneous adverse events and gemifloxacin: observations from the clinical trial program antibiotic joint replacement cheap fucidin 10 gm buy. Use of fluoroquinolones in pediatrics: consensus report of an International Society of Chemotherapy commission bacteria zone buy discount fucidin 10 gm line. Increased risk of Achilles tendon rupture with quinolone antibacterial use antibiotic resistant bacteria in meat quality fucidin 10 gm, especially in elderly patients taking oral corticosteroids antibiotics for uti shot buy fucidin 10 gm with amex. Quinolone-related Achilles tendinopathy in heart transplant patients: incidence and risk factors antibiotics for sinus infection diarrhea 10 gm fucidin purchase otc. Fluoroquinolones cause changes in extracellular matrix, signalling proteins, metalloproteinases and caspase-3 in cultured human tendon cells. A randomized trial comparing the cardiac rhythm safety of moxifloxacin vs levofloxacin in elderly patients hospitalized with community-acquired pneumonia. Pregnancy outcome following gestational exposure to fluoroquinolones: a multicenter prospective controlled study. Comparative in vitro activities of nemonoxacin, doripenem, tigecycline and 16 other antimicrobials against Nocardia brasiliensis, Nocardia asteroides and unusual Nocardia species. In vitro and in vivo activities of novel fluoroquinolones alone and in combination with clarithromycin against clinically isolated Mycobacterium avium complex strains in Japan. Barber and Amar Safdar During the past 6 decades, introduction of effective antimicrobial drugs has enormously improved global public health. The oral analogue has extremely limited bioavailability when given via the enteral route. Table 35-1 provides in vitro activity of surotomycin and vancomycin against lower intestinal microbiota, which are now widely considered to be critical for sustaining local gut homeostasis. However, in patients given vancomycin, 125 mg four times daily, a significant reduction in these bacterial counts occurred 10 and 14 days after treatment commenced. Similarly, patients treated with 250 mg surotomycin twice daily had a high (n = 44/66; 66. The limited treatment options are underscored by the fact that colitis caused by Clostridium difficile is the second most common cause of hospital-acquired colitis. Amid clusters, outbreaks, and epidemics, the increased frequency of infection accompanied by the emergence of hypervirulent C. In contrast, all hamsters that died during the study had detectable toxins A or B. The interim study results in the published meeting abstract did not indicate adverse events, other than a mention of no clinically important differences in serious toxicity among the three groups. Differences in relapse rates and timing of recurrence favored the 250-mg twice-daily arm of surotomycin. Historically, relapse rates among patients treated with oral vancomycin or metronidazole are approximately 20% to 30%. Plazomicin (Achaogen, San Francisco), a next-generation aminoglycoside hailed as a "neoglycoside," is derived from the aminoglycoside sisomicin, which was the parent compound from which 400 derivatives were evaluated. Development of drug resistance to amikacin and tobramycin among clinical gram-negative bacteria isolates has been less often observed compared with antipseudomonal penicillins, advanced-generation cephalosporins, monobactams, and carbapenems, along with the markedly improved ototoxicity profile of the major aminoglycosides in clinical use. Two phase I randomized, double-blind, placebo-controlled clinical trials examined the pharmacokinetics, safety, and tolerability of plazomicin intravenous injection in healthy adults. The second study included 8 individuals between age 18 and 65 years, in whom the maximum tolerated dose from the first phase I study (15 mg/kg once daily) was assessed for a treatment duration of 5 days. Ototoxicity was measured by pure tone audiometry, with bone conduction and otoacoustic emission evaluated before, at the end of, and 3 and 6 months after treatment. Electronystagmography was also performed at similar intervals to assess vestibular function. Mild-to-moderate headache, tinnitus, dizziness, and somnolence were common adverse events, albeit they were transient and resolved rapidly. Tinnitus had occurred in two patients at higher doses, although both subjects retained normal cochlear and vestibular function. The plazomicin/levofloxacin randomization was 2: 1, and the median ages were 39 and 43 years, respectively. Serious adverse events related to the study drug were observed in 1 patient treated with levofloxacin and in a single patient given plazomicin who developed unilateral permanent tinnitus. In the modified intent-to-treat population, microbiologic eradication rates for plazomicin and levofloxacin were 76. Four strains exhibited drug-resistant phenotypes, including 3 with the Ant(2)-Ia and 1 with the Acc(6)-Ib aminoglycoside modifying enzyme. In vitro synergy was demonstrated among most bacterial strains: plazomicin plus imipenem-cilastatin showed the least synergy (68%), whereas 92% of the isolates tested showed synergy for the plazomicin plus piperacillin-tazobactam combination. Plazomicin in combination with piperacillin-tazobactam appears promising and needs clinical validation to assess efficacy for treatment of P. In addition, plazomicin is being investigated for treating Yersinia pestis and Francisella tularensis infections in the setting of biological warfare. Its role would be in combination with a known antibacterial agent, such as piperacillin or a third-generation cephalosporin, just as tazobactam or clavulanic acid was combined with piperacillin or amoxicillin, respectively. Combining avibactam with various -lactam antibiotics restores antibacterial activity against class A and class C producing organisms. This has been shown with piperacillin, aztreonam, ceftazidime, ceftriaxone, cefpodoxime, and cefixime. The combination of avibactam with ceftazidime has been shown to be effective against ceftazidime-resistant enterobacterial strains producing class A and class C -lactamases. Administered every 8 hours, ceftazidime-avibactam, 500 mg/125 mg, was compared with imipenem-cilastatin, 500 mg every 6 hours for complicated urinary tract infections, including pyelonephritis in hospitalized adults, aged 18 to 90 years. After 4 days, patients in either arm were allowed to switch to oral ciprofloxacin, 500 mg twice daily for 14 days, as clinically indicated. Patients having a permanent indwelling catheter, ureteral reflux or obstruction of the urinary tract, intrarenal or perinephric abscess, ileal loop, or nephrostomy were excluded from this study. Sixty-four patients were clinically evaluable: 28 with ceftazidimeavibactam and 36 patients with imipenem-cilastatin. Among microbiologically evaluable patients with ceftazidime-resistant uropathogens, 85. The small number of patients (n = 6/7) in the microbiologically evaluable population was an important limitation of this study. Site of infection, infection/disease severity, and surgical procedures were also comparable. Patients with multiple microorganisms isolated in culture samples and when an organism was resistant to the study drug could be continued in the study at the discretion of the investigator. The clinically evaluable patients needed confirmation of complicated intra-abdominal infection by operative findings and received a minimum of 5 days of study drugs. In the ceftazidime-avibactammetronidazole arm, 87 were clinically evaluable and 68 were microbiologically evaluable; whereas 90 and 67 patients, respectively, were in these categories in the meropenem-placebo treatment arm. Patients with no pathogen isolated before treatment commenced or those with organisms resistant to study drugs were excluded from evaluation of microbiologic response. Treatment with ceftazidime-avibactammetronidazole resulted in clinical and microbiologic response in 25 (96. The limitations of this study were the limited number of subjects, especially the small population of critically ill patients. The rates and occurrences of adverse events and serious adverse events were comparable in both groups. Nausea, vomiting, abdominal pain, and elevated hepatic enzymes were common adverse events, occurring in greater than 5% of patients in each group. Gastrointestinal toxicity was higher in patients treated with ceftazidimeavibactam-metronidazole, although this was not significantly increased compared with patients given meropenem without metronidazole. In 1 patient, elevated liver enzymes were regarded as a sign of serious toxicity caused by ceftazidime-avibactam-metronidazole. In preliminary clinical trials, avibactam appears promising and holds the potential to salvage existing broad-spectrum -lactam antibiotics, to which resistance has emerged among common gram-negative bacteria. There was an option to start these antibiotics orally, and doses used were omadacycline, 200 mg daily, versus linezolid, 600 mg twice daily. Aztreonam could be added in patients given linezolid for added gram-negative coverage. This multicenter trial, which is being conducted in the United States, includes patients with wound infections and cellulitis, and 20% had major abscesses. Intravenous treatment was anticipated to last for 4 to 7 days, and maximal duration of therapy was 14 days. Sixty patients in whom omadacycline was given and 67 patients treated with linezolid were evaluable, clinical responses at the end of treatment were 98. Both these parameters were comparable for the disease state and in patients with microbiologically proven infection versus infections in which no bacterial pathogen was identified. For all pathogens among the microbiologically evaluable population, eradication rates were 95. There were two nonspecified adverse events, resulting in discontinuation of omadacycline, whereas in linezolid-treated patients, there were no treatment disruptions caused by adverse events. It also possesses a fluorine, giving solithromycin an additional third binding site with the bacterial ribosome and perhaps thereby expanding coverage against drug-resistant bacteria. Overall, it demonstrated substantial but varied activity against numerous bacterial isolates. Solithromycin is well distributed throughout the body and achieves high concentration in lung tissue, particularly the epithelial lining fluid, and alveolar macrophages where the concentrations are approximately 10 and 200 times the serum concentrations, respectively. Patients were randomized (1: 1 ratio) to oral solithromycin 800 mg followed by 400 mg daily, or to levofloxacin, 750 mg daily. In the intent-to-treat subset, continued clinical success or test of cure assessed 4 to 11 days after treatment ended was comparable for solithromycin (84. Similarly, microbiologic success in this subset was also not dissimilar among the group of patients given solithromycin (77. Early response success on day 3 after therapy commenced was defined as improvement in at least two cardinal symptoms of pneumonia and was comparable between the two groups: 72. Adverse events related to antimicrobials occurred more frequently in patients treated with levofloxacin (45. Common adverse events were mild-to-moderate gastrointestinal symptoms, such as nausea (1. In 6 patients, treatment was discontinued because of adverse events, and all 6 were receiving levofloxacin. Solithromycin demonstrated comparable efficacy and a favorable safety profile compared with levofloxacin for the treatment of mild to modestly severe community-acquired bacterial pneumonia. An important limitation of this investigational drug is in the coverage for vancomycin-resistant Enterococcus spp. Tedizolid inhibits bacterial translation at the 23S ribosome and demonstrates potent in vitro activity against a wide variety of gram-positive bacteria, including linezolid-resistant S. After a single 600-mg oral dose in healthy adult volunteers, 13% of unbound free drug had excellent distribution in interstitial fluid of adipose and skeletal muscle tissue, and the serum half-life was 8 hours. In 667 adult patients, efficacy and safety of 6-day tedizolid therapy was compared with a 10-day course of linezolid for the treatment of acute bacterial skin and skin-structure infection. The study compared 200 mg once-daily oral tedizolid with 600 mg oral linezolid administered twice daily. Early and sustained clinical response to tedizolid, 48 to 72 hours after initiation of therapy, was statistically noninferior to a 10-day course of linezolid: 79. Continued clinical response 1 to 2 weeks after the treatment ended was also comparable for tedizolid (85. Treatment-related adverse events were similar in each group; most were mild to moderate in severity. Instances of serotonin syndrome were not noted in either group, and it has been suggested that the short course of oxazolidinone therapy may have minimized potentially serious drug toxicity. Two patients in each group discontinued treatment; 3 patients had nausea, vomiting and diarrhea. Tedizolid may provide a treatment option for skin and skin-structure infection caused by linezolid nonsusceptible S. Economic incentives for industrysponsored new drug development are promoted by a relative ease in gaining market entry, as regulatory agencies recognize limited available options for cure of conditions such as cancer. Inhibits bacterial fatty acid biosynthesis, targeting the Fabl enzyme in staphylococci. Potent pneumococcal and atypical respiratory organism activity, including macrolide-resistant strains. Orally active agent demonstrating efficacy with minimal drug (dose) exposure, potentially improving patient tolerability in the treatment of drug-sensitive and drug-resistant Mtb. Reversibly binds to the 50S subunit of the bacterial ribosome, blocking protein synthesis, preventing bacterial growth and reproduction. Binds at two sites in the bacterial ribosome, compared with current macrolide agents that bind at one site. LpxC-1 is an inhibitor of LpxC, a deacetylase enzyme present in many gram-negative bacteria. Previously used only in veterinary medicine or topical use in humans because of toxicity (retapamulin, Altargo, Altabax; GlaxoSmithKline). Potent in vitro activity against common gram-positive skin organisms, including S. Also exhibits in vitro activity against a broad spectrum of gram-positive and gram-negative community respiratory pathogens, including Streptococcus pneumoniae, Moraxella catarrhalis, and Haemophilus influenzae, as well as atypical bacteria: Legionella pneumophila, Chlamydia pneumoniae, and Mycoplasma pneumoniae. Efficacy of plazomicin against Yersinia pestis in a murine-aerosol challenge latetreatment model. Proceedings of the 52nd Interscience Conference on Antimicrobial Agents and Chemotherapy 2012. Efficacy and safety of ceftazidime avibactam versus imipenem cilastatin in the treatment of complicated urinary tract infections including acute pyelonephritis in hospitalized adults: results of a prospective investigator-blinded randomized study. Presented at the Programs and Abstracts of the 46th Interscience Conference on Antimicrobial Agents and Chemotherapy. In vitro potency and spectrum of activity compared to 10 other antimicrobial compounds.
Diseases
- Coleman Randall syndrome
- 3-methyl crotonyl-coa carboxylase deficiency
- Myeloperoxidase deficiency
- Ventricular extrasystoles perodactyly Robin sequence
- Stern Lubinsky Durrie syndrome
- Schinzel Giedion syndrome
- Chromosome 15q, tetrasomy
In a study comparing 2% chlorhexidine antimicrobial epoxy paint order fucidin online pills, povidone-iodine bacteria bacillus purchase fucidin with amex, and 70% alcohol for sterile skin preparation of central venous and arterial catheter sites antibiotic lock therapy cheap fucidin 10 gm buy online, the 2% chlorhexidine lowered rates of subsequent bloodstream infections significantly more than the other two preparations virus on macbook air buy cheap fucidin 10 gm line. Triclosan (2 antibiotics for acne nausea cheap fucidin 10 gm mastercard,4,4-trichloro-2-hydroxydiphenyl ether) is a synthetic bisphenol active against a broad range of gram-positive and gramnegative bacteria. It is a biocide that has been used extensively for many years in dental hygiene products and soaps and has been incorporated into plastic kitchenware products, toys, and tea towels. Povidone-iodine has been widely used for many years in preoperative skin preparation, preparation of skin for blood culture phlebotomy, certain catheter placements, hand scrubbing, and the treatment and prevention of skin infections. It has also been evaluated for its bioavailability in human nasal secretions, and has demonstrated rapid bactericidal activity and good bioavailability within the human nares. Alcohols are rapidly bactericidal, but older preparations were not widely adopted because of their transient antiseptic action, local irritation, and excessive drying, especially when associated with repeated use. Over the last 15 years, newer waterless, alcohol-based hand hygiene products have been brought to market in the United States. These products contain 70% alcohol as the active antiseptic ingredient, and also contain emollients to minimize or eliminate the drying or irritating side effects. Alcohol-based hand sanitizers also differ from older preparations in that their antiseptic action is far more prolonged. Because these products are waterless, and there is no need for a sink or paper towels, alcohol-based hand sanitizers can be made widely available in and around patient care areas, which encourages more widespread use. Current guidelines on hand hygiene recommend these products over soap and water as the preferred method for cleaning unsoiled hands before and after patient encounters. Its noteworthy properties include persistent activity on the When a wound leads to disruption of epidermal integrity. However, no antibacterial formulation has ever been proven to be efficacious in the prophylaxis of clean wounds because so few clean wounds become infected. To avoid the difficulties in performing a large randomized, controlled trial, a human skin infection model was developed to test the efficacy of topical antibiotic formulations in the prophylaxis of minor skin infections. Both neomycin and bacitracin were more effective in preventing infection with both S. Other investigators have also found that the use of either topical neomycinbacitracin-polymyxin ointment or bacitracin alone enhanced the epidermal healing of wounds11 and significantly reduced streptococcal skin colonization and the subsequent infection of small skin trauma in children. The use of topical antibacterials in superficial wounds for a few days, until the integrity of the epidermis is reestablished, has been recommended because the longer the epidermal barrier remains defective, the more likely it is that infection will occur. The use of topical antibacterials in chronic nonhealing, noninfected wounds, such as pressure ulcers, has been recommended by the U. However, there is no substantial evidence in the published medical literature that this goal has been achieved. None of the currently marketed topical antibacterials has been labeled for use specifically in the setting of chronic nonhealing wounds. Some patients with recurrent furuncles, carbuncles, and other skin and soft tissue infections caused by S. One randomized trial treated such patients with a 5-day course of intranasal mupirocin and then randomized half the patients to receive successive monthly therapy for 1 year and half to receive a placebo. The small size of the study precluded the authors from making definitive recommendations for the management of recurrent furunculosis and folliculitis in staphylococcal carriers. The results of this study provide support for the clinical practice of mupirocin maintenance therapy in patients with persistent S. Several studies have been performed in a variety of surgical patients to evaluate the effectiveness of preoperative decolonization with intranasal mupirocin, alone or in combination with other products, on the subsequent rate of postoperative surgical site infections. Currently, it is not considered cost-effective or efficacious when used for all surgeries, but many experts believe it has real benefits in specific surgical populations. In one recent randomized double-blind, placebo-controlled, multicenter trial, researchers screened more than 6700 patients, of whom 1270 were positive for nasal carriage of S. The first large randomized, controlled, multicenter trial looking at use of intranasal mupirocin versus placebo enrolled 4030 patients undergoing general, cardiothoracic, neurosurgical, and gynecologic surgical procedures. It has been suggested that the lack of a statistically significant outcome in this study resulted in part from the fact that the sample size calculation had 85% power to detect a relative reduction of 50% in the rate of S. Several additional studies have assessed the effectiveness of preoperative intranasal mupirocin therapy in a variety of surgical patients. In two open trials performed in patients undergoing open heart surgery, the patients were treated with preoperative intranasal mupirocin and compared with historical control subjects. Based on costeffectiveness analyses, it appears that it may be cost-effective to use preoperative intranasal mupirocin in patients undergoing cardiothoracic surgery. Results showed that both the screen-and-treat and treat-all strategies had both lower costs and greater benefits compared with the no-treatment strategy. The routine application of topical antiseptics to the skin before a surgical procedure is a standard practice. Currently, this alternative point of view is supported by only one published single-center trial. Patients may be told to bathe the evening before, morning of, or on several occasions before the planned surgical procedure. The benefit of bathing with any antiseptic preparation before surgery has no proven benefit, as concluded in a 2006 Cochrane Database System Review. In one prospective evaluation of 827 random catheter insertions in which three regimens of catheter care (neomycin-bacitracin-polymyxin at insertion and every 48 hours versus iodophor ointment at insertion and every 48 hours versus no ointment) were used, no differences in catheter-acquired sepsis (two patients in each group) or local inflammation (38. Chapter 37 TopicalAntibacterials ProphylaxisofVascular CatheterRelatedInfections the use of topical antibacterial agents to prevent vascular catheter related infections includes choice of appropriate skin site antiseptic preparation and the use of a topical agent applied to the catheter site as part of line site maintenance. In patients who undergo peritoneal dialysis, a few strategies have demonstrated efficacy in prophylaxis against exit site and tunnel infections. As discussed above, the use of intranasal mupirocin twice daily for 5 days for the treatment of S. In a prospective, open trial of intranasal mupirocin, peritoneal dialysis patients were treated with mupirocin when naris cultures were positive for S. Topical intranasal mupirocin also resulted in a significant decrease in the subsequent rates of S. The only randomized, doubleblind, placebo-controlled trial of monthly intranasal mupirocin was performed by the Mupirocin Study Group in nine centers throughout Europe. Of note, in a cost-effectiveness analysis, it was not cost-effective to use prophylactic topical intranasal mupirocin in chronic peritoneal dialysis patients. In a prospective, randomized study comparing oral rifampin with topical mupirocin applied daily to the exit site, the rates of infection were compared with those of historical control groups. In another prospective, controlled, historical study, in which a group of peritoneal dialysis patients were treated with topical mupirocin at the exit site three times weekly,46 there was a significant reduction in S. There were several smaller studies (none of which were randomized, placebo-controlled, or blinded) in which topical mupirocin was applied to the exit site either daily or three times weekly, and the results were similar with respect to decreased rates of peritoneal dialysis catheter related infections. As a result of the findings in these studies and despite the fact that there has not been a definitive, well-designed, large, multicenter, randomized, placebo-controlled trial to date, topical mupirocin has been advocated and prescribed at many centers in Europe and North America as part of the routine management of the peritoneal dialysis catheter. This practice has led to concerns about the long-term use of mupirocin and the emergence of resistance as well as concerns about changing the predominant pathogen associated with peritoneal dialysiscatheter infections from staphylococci to gram-negative bacteria. Compared with control subjects, the mupirocintreated patients had significantly fewer incidents of catheter-related bacteremia (7% vs. The incidence of bacteremia was statistically significantly higher in the control group compared with those treated with povidone-iodine-17% versus 2% incidence. The value of povidone-iodine ointment is likely real, and additional studies in which povidone-iodine ointment is used as part of catheter site care are needed. However, topical mupirocin at the exit site is currently recommended and preferred over intranasal mupirocin. In one study, intranasal mupirocin was used three times daily for 2 weeks after catheter insertion, followed by three times weekly as a maintenance regimen, versus placebo. The authors observed a significant decrease in nasal colonization in the mupirocin-treated group as well as a significant decrease in the rate of S. The prevention of infection in the burned patient is extremely difficult because burn wound sites are favorable for bacterial overgrowth, the epidermal barrier is often defective for extended periods, and the patients are in the hospital, where multiple antibiotic-resistant organisms are found. As a result of the pathogenesis and pathophysiology of the burn wound, the delivery of systemic antimicrobial therapy to the deepest, most severely ischemic areas of the wound cannot be relied on because gradient diffusion from the wound periphery is the sole means of access. Before the development of effective topical burn wound chemotherapy, burn wound sepsis was diagnosed as the principal cause of death in 60% of burn patients who died69; the use of mafenide acetate has reduced to 28% the incidence of burn wound sepsis as a cause of death. After administration, high antimicrobial concentrations are found on the wound surface, where the risk of bacterial contamination is the greatest. In patients with deep, extensive wounds, dense bacterial colonization, particularly by gram-positive cocci, often occurs within 24 hours; aerobic gram-negative bacilli typically appear within 3 to 7 days. If this initial bacterial colonization is not treated, deeper spread and ultimate systemic invasion of pathogenic bacteria can occur. Therefore, topical antibacterial therapy should be initiated as soon as possible to delay or prevent these processes. There is evidence that effective topical antibacterial therapy delays colonization of the burn wound for a variable period (measured in days, not weeks), maintains the bacterial density of the wound at lower levels than those which could otherwise be achieved and for appreciable intervals (measured in weeks), and tends to result in a relatively homogeneous and less diverse wound flora than that which would otherwise be expected. Ideally, the agent should penetrate the eschar, but because it may be absorbed, it must have low toxicity70; the agent must also remain active in the presence of serum and necrotic debris. Furthermore, with the increasing use of cultured skin grafts in the therapeutic approach to the burned patient, topical antibacterials may be required to prevent microbial colonization and the destruction of grafts containing cultured skin cells. The successful use of topical agents prevents the bacterial conversion of superficial burns to deeper injury, results in the spontaneous healing of wounds that initially appeared clinically to be of full thickness, and decreases the frequency of episodes of systemic sepsis. There is a role for topical agents in the management of one specific type of pyoderma-impetigo. Impetigo is a superficial infection of the skin caused by group A streptococci (see Chapter 199), S. One of the goals of antimicrobial therapy in impetigo is to prevent the spread of infection to uninvolved skin. However, topical therapy may be used early in infection, when the number of lesions is small and there is a reasonable chance that these agents will be scrupulously and skillfully applied. Retapamulin, a newer topical antibacterial, has been approved for use in adults and children 9 months of age and older. Retapamulin administered twice daily for 5 days was compared with placebo or fusidic acid in two separate double-blind, randomized trials in patients with impetigo. Topical antibacterial agents may have some efficacy in the therapy for secondary types of pyoderma, although the available studies generally did not include control groups. Because topical antibacterials can lower the bacterial colony counts in acute dermatitis, the use of these agents in combination with topical glucocorticoids is a logical treatment regimen. The rash of erythrasma is commonly found in intertriginous areas that include axillae, inframammary areas, the interspaces of toes, and intergluteal and crural folds. Once the diagnosis is confirmed, systemic antibacterial therapy with erythromycin is usually prescribed as first-line therapy. Most experts recommend the addition of a topical agent to systemic therapy in patients with intertriginous area involvement and the exclusive use of topical therapy in those patients intolerant of the recommended active systemic therapies. Topically administered erythromycin, tetracycline, and chloramphenicol have all been evaluated and found not to be effective in the treatment of erythrasma. The etiology of rosacea remains somewhat controversial and is considered to be multifactorial, depending on the phase of disease. Helicobacter pylori has been implicated as a potential causative factor by some authorities, and the Demodex mite has been implicated as a significant contributing factor of papulopustular rosacea. Numerous randomized, controlled trials have been published that confirm the tolerability and superior efficacy of topical metronidazole. Topical clindamycin, retinoids, and azelaic acid in a 20% cream formulation have all also been identified as acceptable topical alternatives in the management of rosacea. Topical azelaic acid, a dicarboxylic acid derivative that is bacteriostatic for P. A randomized 10-week trial comparing the efficacy of erythromycin (3%)benzoyl peroxide (5%) gel with that of erythromycin (4%)zinc (1. Additional studies have also demonstrated the efficacy of the combination formulation of benzoyl peroxide with erythromycin, and this regimen is considered one of the most effective in the treatment of acne. The combination formulation of 1% clindamycin and 5% benzoyl peroxide gel has been marketed and evaluated for its effectiveness in the treatment of acne vulgaris. Both patient and physician assessments at the end of the study indicated that global improvement was significantly greater with clindamycinbenzoyl peroxide than with benzoyl peroxide alone and similar to that identified with erythromycinbenzoyl peroxide. Therefore, the clindamycinbenzoyl peroxide and erythromycinbenzoyl peroxide formulations are equally efficacious and can both be considered first-line topical therapies in the treatment of acne vulgaris. The blocked follicles become an ideal anaerobic culture medium filled with nutrients in the form of lipid substrates; P. Benzoyl peroxide exerts its effects by bacteriostatic activity on the proliferation of P. Oxygen is liberated when the drug is decomposed by cysteine in the skin, and bacterial proteins are thus oxidized. After 2 weeks of daily application, a 10% benzoyl peroxide preparation reduces concentrations of free fatty acids by about 50% and P. Topical antibiotics are used almost universally by dermatologists for the treatment of acne vulgaris. It has also been used in the prevention of dialysis catheter infections and in the prevention of surgical site infections as discussed above. Whether inpatient decolonization should be attempted only in the setting of outbreaks or more universally is also undecided. Attempts to control hospital outbreaks have included methods to eradicate nasal carriage of staphylococci by means of systemic antimicrobial agents with or without topical treatment; however, recolonization is frequent, and the development of resistance has been reported. EliminationofStaphylococcus aureus NasalCarriage 459 A systematic review of this subject was published by Ammerlaan and colleagues in 2009. Of these, 13 studies evaluated mupirocin, with either placebo or active comparator arms. In summary, short-term nasal application of mupirocin was shown to be effective at eradicating S. This compares with an estimated success rate from oral antibiotic administration of 60% 1 week after treatment and 50% after longer follow-up.
If a recipient is considered to be at risk of syphilis transmission from the donor antimicrobial jiu jitsu gi best order for fucidin, prophylactic treatment should be given (2 antibiotic resistance documentary order fucidin 10 gm mastercard. However antibiotic weight loss buy fucidin without a prescription, this possibility should be borne in mind when assessing donors from areas where fungal infections are endemic antimicrobial quiet collar sink baffle order 10 gm fucidin amex. Toxoplasma gondii antibiotic pneumonia buy 10 gm fucidin with amex, Coccidioidomycosis, Strongyloides stercoralis, Trypanosoma cruzi (the causative agent of Chagas disease) and malaria can be transmitted by a renal transplant (21). In most of the reported cases, transmission has been from living unrelated donor transplantation taking place abroad. In this area, up to 8% recipients may develop infection, usually in the first year following transplantation. Infection with Strongyloides stercoralis results from skin penetration by larvae and thus may after walking in soil with faecal contamination. Adult worms can live for up to 5 years, and autoinfection is an important source of prolonged infection even when the individual is no longer living in an endemic area. Symptomatic infection with Strongyloides is more common in the immunocompromised (27). We suggest screening the following groups: those who were born or lived in tropical or subtropical countries where sanitation conditions are poor, those with unexplained eosinophilia and travel to an endemic area and those with a prior history of Strongyloides infection. If positive, an opinion from a Consultant with appropriate expertise should be sought. Donation may proceed after treatment of the donor with an appropriate agent, such as ivermectin. Other infections are either transmitted rarely (occasional case report) or may be considered a possible risk but there have been no reports of donor derived infection. Circumstances requiring an individual assessment, taking into consideration the level of risk or exposure, expected benefit of transplantation and the availability of alternative donors include: history of blood transfusion since 1980; history of receipt of dura mater graft; and history of receipt of human pituitary derived growth hormone or gonadotrophin. Should there be any uncertainties concerning potential risk, the advice of a Consultant with appropriate expertise in infectious diseases, microbiology, virology or hepatology should be sought, to maintain the health and safety of both donor and recipient. Transmission of tropical and geographically restricted infections during solid-organ transplantation. Clinical Practice Guideline on the evaluation and follow-up care of living kidney donors. Risks of transplanting kidneys from hepatitis B surface antigen-negative, hepatitis B core antibody-positive donors. Infection and cancer screening in potential living donors: best practices to protect the donor and recipient. Cytomegalovirus infection after organ transplantation: an update with special emphasis on renal transplantation. Guidelines for the prevention and management of cytomegalovirus disease after solid organ transplantation. Transmission of human herpesvirus 8 infection from renal transplant donors to recipients. Tuberculosis in solid organ transplant candidates and recipients: current and future challenges. Donor-derived Trypanosoma cruzi infection in solid organ recipients in the United States, 2001-2011. Full counselling of donor and recipient is required along with access to appropriate long-term donor follow up. The lifetime risk of recurrent kidney stones is an important consideration in evaluating the suitability for kidney donation. However, data relating to risk of further stone episodes are available for people who present with a symptomatic kidney stone (overall 50% chance of developing a further stone within 5 years) and a risk prediction tool exists (1). Risk prediction tools do not yet exist for asymptomatic stone formers, but 1 stone at presentation confers an increased risk of metabolic risk factors and future stone episodes (1). In symptomatic patients who undergo metabolic evaluation (who may be a selected group), a metabolic abnormality. The remaining 25% of stones are composed of uric acid, pure calcium phosphate, cysteine or struvite (magnesium ammonium phosphate, also called infection stones) (2,4). Uric acid stones are often associated with a history of gout, ileostomy, diarrhoea or with the metabolic syndrome, in all of which the urine is acidic. Calcium phosphate stones may occur with hypercalciuria and are the predominant stone type formed by patients with a low urinary citrate and distal renal tubular acidosis. Cystine stones are always associated with cystinuria and people with these stones should not donate a kidney. Infection stones are commonly associated with an anatomical abnormality and people with these stones should not donate a kidney unless the anatomical abnormality is easily correctable. Small stones usually pass spontaneously but can occasionally cause ureteric obstruction leading to acute renal failure in patients with a single kidney. However, for the general population, the evidence that treating small asymptomatic stones is superior to simply observing them is mixed (6), with about 25% becoming symptomatic in 5 years and 3% developing painless silent obstruction (7). Upper or middle pole stones are more likely to become symptomatic and also to pass spontaneously. It is recognised that the natural history of small asymptomatic stones detected during a donor work-up may be very different to stones presenting with clinical features or described in the existing urological literature. A recent study of 1,957 potential kidney donors evaluated at the Mayo Clinic from 2000 to 2008 reported that 3% had past symptomatic stones, while 11% had radiographic stones detected on screening (11). In this study, asymptomatic stone formers were not characterised by older age, male gender, hypertension, obesity, metabolic syndrome, abnormal kidney function, hyperuricaemia, hypercalcaemia or hypophosphataemia. One conclusion is that asymptomatic stone formers may lack the co-morbidities found in symptomatic stone formers and that different mechanisms may be involved in asymptomatic versus symptomatic stone formation. On balance, it is likely that the risks of recurrent stone formation are low in asymptomatic potential kidney donors. However, in the absence of a reliable evidence base, a degree of caution is warranted. Large or staghorn stones can commonly lead to chronic renal damage (2) and are usually associated with infection or a significant metabolic abnormality and people with these stones should not be considered as donors. In transplant recipients, the long-term risks associated with a small stone transferred from the donor kidney appear low (6,7). If a probable stone is identified on imaging, a urological and radiological review should be undertaken. The number, size, position and density of the potential stones should be considered; as should the presence of any underlying structural renal abnormality. Biochemical Assessment A full metabolic and imaging screen should be carried out before donation on potential donors with a history of stone disease or radiological evidence of a current stone. This screen should include 24-hour urine collections for calcium, oxalate, citrate and urate, and early morning pH assessment. This will require two separate urine collections as calcium, oxalate and citrate analyses require an acidified collection, whereas electrolytes, urate and pH are measured in a plain urine collection. A pH measurement on an early morning urine sample is useful, together with a qualitative cystine screen for cystinuria (8), followed, if positive, by a 24-hour collection for cystine concentration. A metabolic screen (urine and plasma biochemistry) may also be indicated in potential donors with a significant family history of stone disease or with significant risk factors for the development of stones. In patients with previous calculus disease, where a stone has been retrieved, biochemical stone analysis is also of value. If a significant and uncorrectable metabolic abnormality is identified then kidney donation is contra-indicated (9). However, donation may be considered in potential donors with minor or correctable metabolic abnormalities. Donation may be considered where factors that have previously put the patient at risk of stone formation. It is recommended that advice is obtained from a clinician with a specific interest in this field. A history of a previous infection-related (struvite) or cystine renal stone is generally considered a contraindication to donation. In potential donors who have a history of previous stones but no metabolic abnormality, proceeding with donation should be considered providing the number, size and frequency of previous stones has been low. Potential donors found to have small stone(s) on imaging, or cases where there is uncertainty as to whether there is a true calculus or parenchymal calcification, may be suitable to donate. Both need to be aware of the limited data regarding long-term outcomes in these circumstances (10). The smaller the stone bulk and the older the potential donor, the lower is risk associated with proceeding to donation. If donation proceeds, it is preferable to remove the kidney containing the suspected calculus. However, it is relatively straight forward, with urological input and modern flexible ureterorenoscopes, to inspect the collecting system and remove any confirmed stones ex vivo, before implanting the donor kidney (15,16). Leaving the donor with a single kidney containing a possible small stone is undesirable, but may be considered in exceptional circumstances. Full counselling of the donor is required in this situation and appropriate close long-term follow-up of the donor is necessary. People with bilateral kidney stones should in general not be considered as kidney donors. This situation both suggests an inherent metabolic or anatomical abnormality and would leave the individual with a single kidney containing a stone placing them at significant risk of a future stone event in a solitary kidney. Donors who have a past history of stones and those who have donated a stonebearing kidney should be counselled about symptoms of renal/ureteric colic and anuria and information should be provided regarding the availability of local urological expertise. Donors should also be advised to maintain a high fluid intake for life (at least 2. The natural history of nonobstructing asymptomatic renal stones managed with active surveillance. Prevalence and early outcome of donor graft lithiasis in living renal transplants at the Mayo Clinic. The evaluation of living renal transplant donors: clinical practice guidelines: Ad Hoc Clinical Practice Guidelines Subcommittee of the Patient Care and Education Committee of the American Society of Transplant Physicians. Clinical characteristics of potential kidney donors with asymptomatic kidney stones. A report of the Amsterdam Forum on the care of the live kidney donor: data and medical guidelines: Council of the Transplantation Society. Ex vivo ureteroscopic treatment of calculi in donor kidneys at renal transplantation. Incidental renal stones in potential live kidney donors: prevalence, assessment and donation, including role of ex vivo ureteroscopy. All donors should have a full blood count and clotting screen as part of their assessment. In addition, the risks of general anaesthetic are much greater in this population. In addition, visible and non-visible haematuria are well described, often as a result of papillary necrosis. Careful screening for the presence of existing renal involvement is required, with particular attention to a history of macroscopic haematuria. There have been a few reports of minor tubular dysfunction in some patients with thalassaemia trait but there is no other reported association with renal disease (6). Other haemoglobin variants Other haemoglobinopathies may be encountered when screening donors of nonnorthern European heritage and in general should not pose a problem with kidney donation except where they form part of a compound heterozygote with Hb S. Such patients behave like patients with sickle cell disease and therefore should not be accepted as living kidney donors. Red cell membrane disorders these include hereditary spherocytosis and hereditary eliptocytosis, inherited haemolytic anaemias of variable severity. Renal function is not significantly impaired in these conditions and organ donation is acceptable in mild forms where treatment has not been required. However, such a decision has to be taken with great care and following discussion with the donor and their haematologist. Although the risk of disease transmission is considered negligible, the potential recipient should also be counselled re a potential increased risk associated with donation. As such there is a theoretical possibility of carry-over in a donor kidney to the recipient. However, those receiving bridging anticoagulation are more likely to have bleeding complications. These data should inform discussion with potential donors in this category and may represent a relative contraindication to donation but, in general, the risks should be discussed with a haematologist. Association of sickle cell trait with chronic kidney disease and albuminuria in African Americans. Perioperative management of antithrombotic therapy: antithrombotic therapy and prevention of thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Bleeding, recurrent venous thromboembolism, and mortality risks during warfarin interruption for invasive procedures. This may aid diagnosis for the recipient, clarify any mode of inheritance and identify at risk relatives. The diagnosis of many familial renal diseases still relies on a high index of suspicion coupled with biochemical, radiological and histological investigations. It may also be revealed only through a detailed pedigree, which must be obtained for all individuals with renal disease who are being considered for transplantation. In such cases, confirmation of all diagnoses within the family is essential to identify whether there is a clinically significant genetic predisposition to renal disease that may be relevant to potential donation (3). However, in most cases the family history is due to polygenic influences such as diabetes, certain types of glomerulonephritis and hypertension for which no additional genetic testing or screening is required above that recommended for routine donor evaluation (3). Where the diagnosis is a known genetic disease or the family history is suggestive of a monogenic (Mendelian) disease, the pedigree will aid in the identification of the mode of inheritance (typically autosomal dominant, autosomal recessive or X-linked) and the identification of at risk relatives. This information is important to clarify the lifetime risk to a genetically related potential donor of developing significant renal disease.
Therapy durations longer than 2 weeks appear to be associated with these effects infection on face buy genuine fucidin, with thrombocytopenia being more likely to occur than anemia or neutropenia antibiotic susceptibility testing generic 10 gm fucidin with amex. Delayed neutrophil recovery and worsening thrombocytopenia have been documented in patients with baseline marrow suppression antimicrobial vinyl chairs buy fucidin on line. In a single case treating uti holistically purchase fucidin 10 gm line, a postsurgical cerebral abscess caused by penicillin-susceptible S infection 6 weeks after giving birth purchase cheapest fucidin. In small numbers of patients with infection caused by resistant and extremely resistant strains, the addition of linezolid to failing regimens led to sterilization of sputum after 4 to 6 months of therapy. Similarly, blood pressure monitoring is recommended for patients taking adrenergic agents such as pseudoephedrine and phenylpropanolamine. Optic neuropathy causes gradual onset of blurring and if the drug is not discontinued can lead to permanent loss of useful 409 visual acuity. In a recent randomized, double-blind, double-dummy, multicenter trial, oral tedizolid, 200 mg once daily for 6 days, was noninferior to oral linezolid, 600 mg twice daily for 10 days, in the treatment of acute bacterial skin and skin structure infections. Whether all members of this class are immune modulators has not been demonstrated. Other notable yet rare postmarketing reports of adverse effects include posterior reversible leukoencephalopathy syndrome, seizures, tooth and tongue discoloration, black hairy tongue (lingua villosa nigra), and hypoglycemia among diabetic patients receiving insulin or oral hypoglycemic agents. Oxazolidinones, a new class of synthetic antibacterial agents: in vitro and in vivo activities of DuP105 and DuP721. Vancomycinresistant Enterococcus faecium meningitis successfully managed with linezolid: case report and review of the literature. Efficacy and tolerability of prolonged linezolid therapy in the treatment of orthopedic implant infections. Linezolid for the treatment of multidrug-resistant, gram-positive infections: experience from a compassionate-use program. Determination of risk factors associated with isolation of linezolid-resistant strains of vancomycin-resistant Enterococcus. Multicity outbreak of linezolid-resistant Staphylococcus epidermidis associated with clonal spread of a cfr-containing strain. Increasing incidence of linezolid-intermediate or -resistant vancomycin-resistant Enterococcus faecium strains parallels increasing linezolid consumption. Transferable plasmidmediated resistance to linezolid due to cfr in a human clinical isolate of Enterococcus faecalis. Complicated skin and skin-structure infections and catheter-related bloodstream infections: noninferiority of linezolid in a phase 3 study. Linezolid is a specific inhibitor of 50S ribosomal subunit formation in Staphylococcus aureus cells. Crosslinking in the living cell locates the site of action of oxazolidinone antibiotics. Bacteriostatic or bactericidal effect of linezolid against multiresistant Streptococcus pneumoniae. Clinical update on linezolid in the treatment of gram-positive bacterial infections. In vitro activity of linezolid (U-100766) against Haemophilus influenzae measured by three different susceptibility testing methods. Oxazolidinones, a new class of synthetic antituberculosis agent: in vitro and in vivo activities of DuP-721 against Mycobac terium tuberculosis. Successful treatment of vancomycin-resistant Enterococcus faecium meningitis with linezolid: case report and literature review. Penetration of linezolid into bone, fat, muscle and haematoma of patients undergoing routine hip replacement. Unexpected effect of rifampin on the pharmacokinetics of linezolid: in silico and in vitro approaches to explain its mechanism. Therapeutic drug monitoring may improve safety outcomes of long-term treatment with linezolid in adult patients. Efficacy of linezolid in treatment of experimental endocarditis caused by methicillin-resistant Staphylococcus aureus. The clinical significance of vancomycin minimum inhibitory concentration in Staph ylococcus aureus infections: a systematic review and metaanalysis. Is it time to replace vancomycin in the treatment of methicillin-resistant Staphylococcus aureus infections Successful treatment of vancomycin-resistant Enterococcus faecium bacteremia with linezolid after failure of treatment with Synercid (quinupristin/dalfopristin). Vancomycinresistant Enterococcus faecalis endocarditis: linezolid failure and strain characterization of virulence factors. Failure of linezolid therapy for post-neurosurgical meningitis due to Enterococ cus faecium. Early and extended early bactericidal activity of linezolid in pulmonary tuberculosis. Successful treatment of disseminated Mycobacterium chelonae infection with linezolid. Successful treatment of refractory disseminated Mycobacterium avium complex infection with the addition of linezolid and mefloquine. Intensive care unit dissemination of multiple clones of linezolid-resistant Enterococcus faecalis and Enterococcus faecium. Resistance to linezolid in a porcine Clostridium perfringens strain carrying a mutation in the rplD gene encoding the ribosomal protein L4. Efficacy and safety of linezolid compared with vancomycin in a randomized, double-blind study of febrile neutropenic patients with cancer. Adverse effects of antimicrobials via predictable or idiosyncratic inhibition of host mitochondrial components. Rhabdomyolysis in a patient treated with linezolid for extensively drug-resistant tuberculosis. Safety and Efficacy Study of Oxazolidinones to Treat Uncomplicated Skin Infections. In vitro activity of cadazolid against Clostridium difficile strains isolated from primary and recurrent infections in Stockholm, Sweden. A nonantibacterial oxazolidinone derivative that inhibits epithelial cell sheet migration. The modern era of antimicrobial chemotherapy began in 1932 with the first reports by Domagk of the protective activity of sulfachrysoidine (Prontosil) against murine streptococcal infections. This drug was developed initially by the German dye industry and had been available commercially since the early 20th century. Sulfachrysoidine exerted its antibacterial activity through the release in vivo of paraaminobenzenesulfonamide (sulfanilamide). This was the first antibacterial agent used in the United States, in July 1935, in an unsuccessful attempt to treat a 10-year-old girl late in the course of meningitis and sepsis caused by Haemophilus influenzae. Trimethoprim is a 2,4-diaminopyrimidine and, as such, inhibits the enzyme dihydrofolate reductase, resulting in interference in folic acid and subsequent pyrimidine synthesis in the bacterial cell. Trimethoprim is one of several such compounds synthesized and studied by Hitchings and co-workers in the 1950s and 1960s. The use of trimethoprim as a potentiator of sulfonamide activity was introduced by Bushby and Hitchings2 in 1968. These agents, available in a fixed-drug combination, show true antibacterial synergism against a wide variety of organisms. DerivationandNomenclature Since the introduction of sulfonamides into clinical medicine, dozens of compounds have been used. The various compounds can be classified as (1) short-acting or medium-acting sulfonamides, (2) long-acting sulfonamides, (3) sulfonamides limited to the gastrointestinal tract, or (4) topical sulfonamides. Many branded sulfonamide preparations have been discontinued or replaced by generic products. Sulfisoxazole and sulfamethoxazole have been combined with phenazopyridine, a urinary analgesic. The nature of these substitutions determines other pharmacologic properties of the drug, such as absorption, solubility, and gastrointestinal tolerance. Substitutions at the 4-amino group result in decreased absorption from the gastrointestinal tract. Neither sulfadimethoxine nor any other long-acting sulfonamides other than sulfadoxine is currently available in the United States. Sulfadoxine, originally known as sulformethoxine (N-[5,6dimethoxy-4-pyrimidyl] sulfanilamide) is a very long-acting sulfonamide that, combined with pyrimethamine, was formerly available in the United States. Sulfadoxine has a half-life of 100 to 230 hours and reaches a peak serum level of 51 to 76 µg/mL 2. Although resistance is noted, this combination is still used in malaria prophylaxis during pregnancy in some countries. The in vitro antimicrobial sensitivity of sulfonamides is influenced strongly by the size of the inoculum and the composition of the test medium. Resistance to sulfonamides is widespread and increasingly common in community-acquired and nosocomial strains of bacteria, including streptococci, staphylococci, Enterobacteriaceae, Neisseria spp. In recent decades, sulfonamide resistance in Enterobacteriaceae and gram-positive bacteria has increased substantially. Plasmid transfer can occur in the gastrointestinal tract and in vitro and has been seen especially with multiple species of Enterobacteriaceae. Salmonella resistance to sulfonamides has also increased, often in conjunction with resistance to other antibiotic classes. They have been used in the past to suppress the susceptible bowel flora before surgery. Salicylazosulfapyridine (sulfasalazine, Azulfidine) is a sulfonamide derivative used to treat ulcerative colitis. This drug is absorbed in its parent form as sulfapyridine, and significant blood levels of this compound are measurable. Mafenide acetate (para-aminomethylbenzene sulfonamide) is available for use in the topical treatment of burns. Its use has been limited, however, by metabolic acidosis caused by carbonic anhydrase inhibition. Silver sulfadiazine has fewer side effects and is used for burns,4 although newer silver compounds are being introduced. Outbreaks of silver-resistant infections in burn units ultimately may limit its usefulness. Although a wide variety of chemical modifications of the sulfonamides have been synthesized, all basically share the same mechanism of action. The sulfonamides are bacteriostatic in that they inhibit bacterial growth by interfering with microbial folic acid synthesis. Richmond9 has suggested that sulfonamides may act on bacterial repressor genes or by feedback inhibition to decrease formation of new enzymes. The ultimate result of decreased folic acid synthesis is a decrease in bacterial nucleotides, with subsequent inhibition of bacterial growth. Topical Sulfonamides Pharmacology Routes of Administration Sulfonamides are usually administered orally. Sulfacetamide is available as ophthalmic preparations; silver sulfadiazine and mafenide acetate are applied topically in burn patients and are associated with significant absorption of sulfonamide percutaneously. Absorption MechanismsofAction Most of the short-acting and medium-acting sulfonamides are absorbed rapidly and almost completely in the nonionized state from the small intestine and stomach. Compounds with N-1 substitutions are absorbed poorly, as are more acidic compounds. Distribution the sulfonamides are generally well distributed throughout the body, entering the cerebrospinal fluid and synovial, pleural, and peritoneal fluids with concentrations approaching 80% of serum levels. Blood and tissue levels are related to the degree of protein binding (Table 33-1) and lipid solubility. Sulfonamides administered in pregnancy readily cross the placenta and are present in the fetal blood and amniotic fluid. Metabolism and Excretion Acetylation and glucuronidation occur in the liver, and free and metabolized drug appears in the urine. Plasma half-lives vary widely; they are related inversely to lipid solubility and directly to pKa values but are not related clearly to the degree of protein binding. Small amounts of sulfonamides are found in bile, human milk, prostatic secretions, saliva, and tears. Levels obtainable in cerebrospinal fluid and other body fluids are related inversely to the degree of protein binding. Sulfonamides can cause nausea, vomiting, diarrhea, rash, fever, headache, depression, jaundice, hepatic necrosis, drug-induced lupus,22 and a serum sicknesslike syndrome. Sulfadiazine used in excessively high doses is associated with crystalluria and tubular deposits of sulfonamide crystals. These complications can be minimized by maintenance of high urine flow and alkalinization of the urine. Tubular necrosis, interstitial nephritis, and necrotizing angiitis may be associated rarely with sulfonamide sensitivity. Sulfonamides administered during the last month of pregnancy compete for bilirubin-binding sites on plasma albumin and may increase fetal blood levels of unconjugated bilirubin, increasing the risk of kernicterus. Also, because of the immature fetal acetyltransferase system, blood levels of free sulfonamide may be increased, further adversely affecting the risk of kernicterus. Significant hypersensitivity reactions can occur with sulfonamides administered via any route. The most important of these reactions are erythema nodosum, erythema multiforme (including Stevens-Johnson syndrome), fixed-drug eruption, vasculitis similar to periarteritis nodosa, and anaphylaxis. One report has suggested that cutaneous reactions, including toxic epidermal necrolysis, may be related to an inherited constitutional defect in detoxification of metabolites. Sulfonamides also displace methotrexate from its bound protein, increasing methotrexate toxicity.
Fucidin 10 gm buy free shipping. Anadolu Agency - Antimicrobial fabric from chinaberry tree.
References
- Morgan T, Anderson J, Jorden M, et al. Pulmonary glial heterotopia in a monoamniotic twin. Pediatr Pulmon 2003;36:162-6.
- Gottschalk A, Ochroch EA: Preemptive analgesia: What do we do now [Correspondence]? Anesthesiology 98:280, 2003.
- Rodrigues NR, Owen N, Talbot K, Ignatius J, Dubowitz V, Davies KE. Deletions in the survival motor neuron gene on 5q13 in autosomal recessive spinal muscular atrophy. Hum Mol Genet. 1995;4:631-634.
- St-Jacques B, Hammerschmidt M, McMahon AP. Indian hedgehog signaling regulates proliferation and differentiation of chondrocytes and is essential for bone formation. Genes Dev 1999;13(16):2072-2086.
- Aldara package insert. Graceway Pharmaceuticals. Revised 10/2010.
- Seitz, M., Reich, O., Gratzke, C. et al. High-power diode laser at 980 nm for the treatment of benign prostatic hyperplasia: ex vivo investigations on porcine kidneys and human cadaver prostates. Lasers Med Sci 2009;24:172-178.
- McGraw T, Kosek P: Erythromelalgia pain managed with gabapentin, Anesthesiology 86:988, 1997.
- Gleason DF, Mellinger GT: Prediction of prognosis for prostatic adenocarcinoma by combined histological grading and clinical staging, J Urol 111(1):58n64, 1974.
