
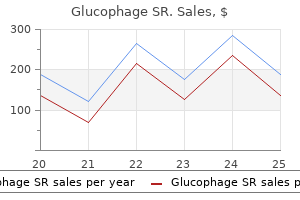
Glucophage SR
| Contato
Página Inicial
Amy Garlin MD
- Associate Clinical Professor
https://publichealth.berkeley.edu/people/amy-garlin/
In this model symptoms 0f pregnancy buy generic glucophage sr on-line, receptor R can exist in active (Ra) and inactive (Ri) conformations symptoms bowel obstruction purchase glucophage sr line, and drugs binding to one denivit intensive treatment discount glucophage sr, the other medicine guide cheap glucophage sr 500 mg buy on-line, or both states of R can influence the balance of the two forms of R and the net effect of receptor-controlled events medicine mound texas buy generic glucophage sr 500 mg. The ordinate is the activity of the receptor produced by Ra, the active receptor conformation. If the drug selectively binds to Ri, then the net influence and amount of Ra will be diminished. If L can bind to receptor in an active conformation Ra but also bind to inactive receptor Ri with lower affinity, the drug will produce a partial response; L will be a partial agonist. If there is sufficient Ra to produce an elevated basal response in the absence of ligand (agonist-independent constitutive activity), and L binds to Ri, then that basal activity will be inhibited; L will then be an inverse agonist. Inverse agonists selectively bind to the inactive form of the receptor and shift the conformational equilibrium toward the inactive state. In systems that are not constitutively active, inverse agonists will behave like competitive antagonists, which helps explain that the properties of inverse agonists and the number of such agents previously described as competitive antagonists were only recently appreciated. Receptors that have constitutive activity and are sensitive to inverse agonists include benzodiazepine, histamine, opioid, cannabinoid, dopamine, bradykinin, and adenosine receptors. Chronic administration of a drug may cause a downregulation of receptors or desensitization of response that can require dose adjustments to maintain adequate therapy. Chronic administration of nitrovasodilators to treat angina results in the rapid development of complete tolerance, a process known as tachyphylaxis. Mannitol acts osmotically to cause changes in the distribution of water to promote diuresis, catharsis, expansion of circulating volume in the vascular compartment, or reduction of cerebral edema (see Chapter 25). Anti-infective drugs such as antibiotics, antivirals, and antiparasitics achieve specificity by targeting receptors or cell processes that are critical for the growth or survival of the infective agent but are nonessential or lacking in the host organism. Structure-Activity Relationships and Drug Design the receptors responsible for the clinical effects of many drugs have yet to be identified. Conversely, sequencing of the entire human genome has identified novel genes related by sequence to known receptors, for which endogenous and exogenous ligands are unknown; these are called orphan receptors. Both the affinity of a drug for its receptor and its intrinsic activity are determined by its chemical structure. Relatively minor modifications in the drug molecule may result in major changes in its pharmacological properties based on altered affinity for one or more receptors. Exploitation of structure-activity relationships has frequently led to the synthesis of valuable therapeutic agents. Because changes in molecular configuration need not alter all actions and effects of a drug equally, it is sometimes possible to develop a congener with a more favorable ratio of therapeutic to adverse effects, enhanced selectivity amongst different cells or tissues, or more acceptable secondary characteristics than those of the parent drug. Therapeutically useful antagonists of hormones or neurotransmitters have been developed by chemical modification of the structure of the physiological agonist. With information about the molecular structures and pharmacological activities of a relatively large group of congeners, it is possible to use computer analysis to identify the chemical properties. Advances in molecular modeling of organic compounds and the methods for drug target (receptor) discovery and biochemical measurement of the primary actions of drugs at their receptors have enriched the quantitation of structure-activity relationships and its use in drug design (Carlson and McCammon, 2000). Such information increasingly is allowing the optimization or design of chemicals that can bind to a receptor with improved affinity, selectivity, or regulatory effect. Similar structure-based approaches also are used to improve pharmacokinetic properties of drugs, particularly if knowledge of their metabolism is known. Knowledge of the structures of receptors and of drug-receptor complexes, determined at atomic resolution by X-ray crystallography, is even more helpful in the design of ligands and in understanding the molecular basis of drug resistance and circumventing it. Emerging technology in the field of pharmacogenetics (see Chapter 7) is improving our understanding of the nature of and variation in receptors and their impact on pharmacotherapy (Jain, 2004). On the y axis, the response is expressed as a percentage of maximal response plotted as a function of the concentration of drug A present at the receptor (x axis). The hyperbolic shape of the curve in panel A becomes sigmoid when plotted semilogarithmically, as in panel B. Dose-response curves presented in this way are sigmoidal in shape and have three noteworthy properties: threshold, slope, and maximal asymptote. Equation 34 describes only receptor occupancy, not the eventual response that may be amplified by the cell. Because of downstream amplification, many signaling systems can reach a full biological response with only a fraction of receptors occupied. Efficacy reflects the capacity of a drug to activate a receptor and generate a cellular response. Thus, a drug with high efficacy may be a full agonist, eliciting, at some concentration, a full response. This simple relationship illustrates the reliance of the affinity of the ligand (L) with receptor (R) on both the forward or association rate k+1 and the reverse or dissociation rate k1. As a practical matter, the affinity of a drug is influenced most often by changes in its off rate (k1) rather than its on rate (k+1). The relative potency of two agonists (drug X,; drug Y,) obtained in the same tissue is a function of their relative affinities and intrinsic efficacies. In systems where the two drugs do not both produce the maximal response characteristic of the tissue, the observed maximal response is a nonlinear function of their relative intrinsic efficacies. Drug X is more efficacious than drug Y; their asymptotic fractional responses are 100% for drug X and 50% for drug Y. The advantage of using maxima is that this property depends solely on efficacy, whereas drug potency is a mixed function of both affinity and efficacy. Characteristic patterns of antagonism are associated with certain mechanisms of receptor blockade. One is straightforward competitive antagonism, whereby a drug with affinity for a receptor but lacking intrinsic efficacy. The magnitude of the rightward shift of the curve depends on the concentration of the antagonist and its affinity for the receptor (Schild, 1957). A partial agonist similarly can compete with a "full" agonist for binding to the receptor. However, increasing concentrations of a partial agonist will inhibit response to a finite level characteristic of the intrinsic efficacy of the partial agonist. Partial agonists may be used therapeutically to buffer a response by inhibiting excessive receptor stimulation without totally abolishing receptor stimulation. For example, varenicline is a nicotinic receptor partial agonist used in smoking cessation therapy. In each set of curves, the green curve represents the effect of orthosteric agonist, unmodulated by any antagonist or potentiator. Competitive antagonism occurs when the agonist A and antagonist I compete for the same binding site on the receptor. If the antagonist binds to the same site as the agonist but does so irreversibly or pseudoirreversibly (slow dissociation but no covalent bond), it causes a shift of the dose-response curve to the right, with progressive depression of the maximal response as [I] increases. Allosteric effects occur when an allosteric ligand I or P binds to a different site on the receptor to either inhibit (I) the response (panel C. Increasing concentrations of I shift the curves progressively to right and downward. This allosteric effect is saturable; inhibition or potentiation reaches a limiting value when the allosteric site is fully occupied. An antagonist may dissociate so slowly from the receptor that its action is exceedingly prolonged. Operationally, this is referred to as noncompetitive antagonism, although the molecular mechanism of action cannot be inferred unequivocally from the effect on the dose-response curve. Noncompetitive antagonism can be produced by an allosteric or allotopic antagonist, which binds to a site on the receptor distinct from that of the primary agonist, thereby changing the affinity of the receptor for the agonist. The affinity of a competitive antagonist (Ki) for its receptor can be determined in radioligand binding assays or by measuring the functional response of a system to a drug in the presence of the antagonist (Cheng, 2004; Cheng and Prusoff, 1973; Limbird, 2005). As more antagonist (I) is added, a higher concentration of the agonist is needed to produce an equivalent response (the half-maximal, or 50%, response is a convenient and accurately determined level of response). The extent of the rightward shift of the concentration-dependence curve is a measure of the affinity of the inhibitor, and a high-affinity inhibitor will cause a greater rightward shift than a low-affinity inhibitor at the same inhibitor concentration. Using Equations 33 and 34, one may write mathematical expressions of fractional occupancy f of the receptor R by an agonist ligand (L) for the agonist alone [fcontrol] and agonist in the presence of inhibitor [f+I]. Such positive interactions of two agents may permit use of reduced concentrations of each drug, thereby reducing concentration-dependent adverse effects. Positive synergism refers to the superadditive effects of drugs used in combination. Drugs used in combination can also demonstrate negative synergism or subadditive effects, where the efficacy of the drug combination is less than would be expected if the effects were additive. Similar lines drawn parallel to the 50% additive line can be used to determine the relative concentrations of A and B required to achieve other responses. If A and B are superadditive (positive synergism), the relative concentrations of A and B needed to achieve a given response will fall below the additive response line. Conversely, if A and B are subadditive (negative synergism), their relative concentrations will lie above the additive response line. The basis for the use of isobolograms in characterizing the effects of drug combinations has been developed and reviewed by Tallarida (2006, 2012). Drug responsiveness may change because of disease, age, or previous drug administration. Receptors are dynamic, and their concentrations and functions may be up- or downregulated by endogenous and exogenous factors. Data on the correlation of drug levels with efficacy and toxicity must be interpreted in the context of the pharmacodynamic variability in the population. The isobologram shows the line of additivity for a 50% effect obtained with a combination of two drugs (concentrations of drug A are on the x axis, concentrations of drug B are on the y axis) that have similar effects but different mechanisms of action. If the combination of A and B exhibits positive synergism (superadditivity), then the 50% effect with a combination of the two drugs will fall somewhere below the line of additivity, whereas negative synergism (subadditivity) will fall above the line of additivity. The isobologram can be used to estimate the concentrations of two drugs needed to obtain a given effect when used in combination. For a full explanation of the concept and utility of isoboles, consult Tallarida (2006, 2012). An experiment was performed on 100 subjects, and the effective plasma concentration that produced a quantal response was determined for each individual. The number of subjects who required each dose was plotted, giving a log-normal frequency distribution (purple bars). The normal frequency distribution, when summated, yields the cumulative frequency distribution-a sigmoidal curve that is a quantal concentration-effect curve (red bars, red line). Animals were injected with varying doses of a drug, and the responses were determined and plotted. Therefore, use of the population therapeutic window to optimize the dosage of a drug should be complemented by monitoring appropriate clinical and surrogate markers for drug effect(s) in a given patient. The effects of these factors on variability of drug pharmacokinetics are described more thoroughly in Chapters 2, 5, 6, and 7. Drug Interactions and Combination Therapy Drugs are commonly used in combination with other drugs, sometimes to achieve an additive or synergistic effect, but more often because two or more drugs are needed to treat multiple conditions. Marked alterations in the effects of some drugs can result from coadministration with other agents, including prescription and nonprescription drugs, supplements, and nutraceuticals. Such interactions can cause toxicity or inhibit the drug effect and the therapeutic benefit. Drug interactions always should be considered when unexpected responses to drugs occur. Understanding the mechanisms of drug interactions provides a framework for preventing them. Drug interactions may be pharmacokinetic (the delivery of a drug to its site of action is altered by a second drug) or pharmacodynamic (the response of the drug target is modified by a second drug). Examples of pharmacokinetic interactions that can enhance or diminish the delivery of drug to its site of action are provided in Chapter 2. In a patient with multiple comorbidities requiring a variety of medications, it may be difficult to identify adverse effects due to medication interactions and to determine whether these are pharmacokinetic, pharmacodynamic, or some combination of interactions. Combination therapy constitutes optimal treatment of many conditions, including heart failure (see Chapter 29), hypertension (see Chapter 28), and cancer (see Chapters 6568). However, some drug combinations produce pharmacodynamic interactions that result in adverse effects. The oral anticoagulant warfarin has a narrow margin between therapeutic inhibition of clot formation and bleeding complications and is subject to numerous important pharmacokinetic and pharmacodynamic drug interactions. By inhibiting platelet aggregation, aspirin increases the incidence of bleeding in warfarin-treated patients. Most drugs are evaluated in young and middle-aged adults, and data on their use in children and the elderly are sparse. At the extremes of age, drug pharmacokinetics and pharmacodynamics can be altered, possibly requiring avoidance of selected drugs or substantial alteration in the dose or dosing regimen to safely produce the desired clinical effect. The American Geriatrics Society publishes the Beers Criteria for Potentially Inappropriate Medication Use in Older Adults, an explicit list of drugs that should be avoided in older adults, drugs that should be avoided or be used at lower doses in patients with reduced kidney function, and specific drug-disease and drug-drug interactions that are known to be harmful in older adults (Beers Update Panel, 2015). Drugs that affect the synthesis and degradation of circulating mediators such as vasoactive peptides. Drug Receptors Associated With Extracellular Processes Many widely used drugs target enzymes and molecules that control extracellular processes such as thrombosis, inflammation, and immune responses. For instance, the coagulation system is highly regulated and has a number of drug targets that control the formation and degradation of clots, including several coagulation factors (thrombin and factor Xa), antithrombin, and glycoproteins on the surface of platelets that control platelet activation and aggregation (see Chapter 32). Receptors Utilized by Anti-infective Agents Anti-infective agents such as antibacterials, antivirals, antifungals, and antiparasitic agents target receptors that are microbial proteins. These proteins are key enzymes in biochemical pathways that are required by the infectious agent but are not critical for the host. Examples of the various mechanisms of action of antibiotics are described in Chapters 52 through 64. Although this approach is just being tested outside the laboratory and must undergo numerous regulatory hurdles before being used on a wide scale, it provides proof of principle that interrupting the life cycle of a parasite in the vector could be as effective as treating the infected host (see Chapter 53). Receptors and their associated effector and transducer proteins also act as integrators of information as they coordinate signals from multiple ligands with each other and with the differentiated activity of the target cell. Another important property of physiological receptors is their capacity to significantly amplify a physiological signal.
However medications via g-tube buy glucophage sr 500 mg on-line, increasing the number of carbon atoms to nine introduces marked sedative properties medicine park oklahoma generic glucophage sr 500mg online. Peak Cp occurs in 1 to 4 h medications side effects purchase glucophage sr with american express, although this can be delayed for several hours if the drug is administered in enteric-coated tablets or is ingested with meals treatment definition math generic 500mg glucophage sr with visa. Its extent of binding to plasma proteins is usually about 90% medicine 44291 500mg glucophage sr order visa, but the fraction bound is reduced as the total concentration of valproate is increased through the therapeutic range. Valproate undergoes hepatic metabolism (95%), with less than 5% excreted unchanged in urine. The t1/2 of valproate is about 15 h but is reduced in patients taking other antiseizure drugs. Plasma Drug Concentrations Valproate plasma concentrations associated with therapeutic effects are about 30100 g/mL. However, there is a poor correlation between the plasma concentration and efficacy. There appears to be a threshold at about 3050 g/mL, the concentration at which binding sites on plasma albumin begin to become saturated. Therapeutic Uses Pharmacological Effects Valproate is strikingly different from phenytoin or ethosuximide in that it is effective in inhibiting seizures in a variety of models. Like phenytoin and carbamazepine, valproate inhibits tonic hind limb extension in maximal electroshock seizures and kindled seizures at nontoxic doses. Like ethosuximide, valproate at subtoxic doses inhibits clonic motor seizures induced by pentylenetetrazol. Its efficacy in diverse models parallels its efficacy against absence as well as focal and generalized tonic-clonic seizures in humans. Valproate produces effects on isolated neurons similar to those of phenytoin and ethosuximide. At therapeutically relevant concentrations, valproate inhibits sustained repetitive firing induced by depolarization of mouse cortical or spinal cord neurons (McLean and Macdonald, 1986b). The action is similar to that of phenytoin and carbamazepine (Table 172) and appears to be mediated by a prolonged recovery of voltage-activated Na+ channels from inactivation. The initial daily dose usually is 15 mg/kg, increased at weekly intervals by 510 mg/kg/d to a maximum daily dose of 60 mg/kg. The therapeutic uses of valproate in epilepsy are discussed further at the end of this chapter. Rash, alopecia, and stimulation of appetite have been observed occasionally; weight gain has been seen with chronic valproate treatment in some patients. Elevation of hepatic transaminases in plasma is observed in up to 40% of patients and often occurs asymptomatically during the first several months of therapy. Acute pancreatitis and hyperammonemia have been frequently associated with the use of valproate. The concurrent administration of valproate and clonazepam is associated with the development of absence status epilepticus; however, this complication appears to be rare. In addition, vigabatrin is designated as an orphan drug for treatment of infantile spasms (described in the Therapeutic Use section that follows). In addition, zonisamide inhibits T-type Ca2+ currents and reduces the influx of calcium. Thus, phenobarbital, phenytoin, and carbamazepine will decrease the plasma concentration/dose ratio of zonisamide, whereas lamotrigine will increase this ratio. An oral dose is well absorbed, reaching a maximal Cp within 1 h; the presence of food prolongs absorption but does not reduce the area under the curve. Vigabatrin is excreted unmetabolized by the kidney, and the dose must be reduced for patients with renal impairment. Although vigabatrin has a t1/2 of only 68 h, the pharmacodynamic effects are prolonged and do not correlate well with plasma t1/2 or the Cp. A 2-week, randomized, single masked clinical trial of vigabatrin for infantile spasms in children younger than 2 years revealed timeand dose-dependent increases in responders, evident as freedom from spasms for 7 consecutive days. Children in whom infantile spasms were caused by tuberous sclerosis were particularly responsive to vigabatrin. The most common adverse effects include somnolence, dizziness, cognitive impairment, ataxia, anorexia, nervousness, and fatigue. Approximately 1% of individuals develop renal calculi during treatment, which may relate to inhibition of carbonic anhydrase by zonisamide. Measurement of serum bicarbonate prior to initiating therapy and periodically thereafter, even in the absence of symptoms, is recommended. Last, spontaneous abortions and congenital abnormalities have been reported at twice the rate (7%) of the healthy, control population (2%3%) in female patients of childbearing age receiving polytherapy including zonisamide. General Principles and Choice of Drugs for Therapy of the Epilepsies Early diagnosis and treatment of seizure disorders with a single appropriate agent offers the best prospect of achieving prolonged seizure-free periods with the lowest risk of toxicity. An attempt should be made to determine the cause of the epilepsy with the hope of discovering a correctable lesion, either structural or metabolic. The cost/benefit ratio of the efficacy and the adverse effects of a given drug should be considered in determining which drug is optimal for a given patient. The first decision to make is whether and when to initiate treatment (French and Pedley, 2008). The most common side effects (>10% patients) include weight gain, concentric visual field constriction, fatigue, somnolence, dizziness, hyperactivity, and seizures. Data in animal models suggest that vigabatrin may harm a developing fetus, and the drug is classified in pregnancy category C. Unless extenuating circumstances such as status epilepticus exist, only monotherapy should be initiated. Initial dosing should target a Cpss within the lower portion of the range associated with clinical efficacy to minimize dose-related adverse effects. Dosage is increased at appropriate intervals as required for control of seizures or as limited by toxicity, with monitoring of plasma drug concentrations. Compliance with a properly selected, single drug in maximal tolerated dosage results in complete control of seizures in about 50% of patients. If a seizure occurs despite optimal drug levels, the physician should assess the presence of potential precipitating factors such as sleep deprivation, a concurrent febrile illness, or drugs. Unless serious adverse effects of the drug dictate otherwise, always reduce dosage gradually to minimize risk of seizure recurrence. In the case of focal seizures in adults, the diversity of available drugs permits selection of a second drug that acts by a different mechanism (see Table 172). Among previously untreated patients, 47% became seizure free with the first drug and an additional 14% became seizure free with a second or third drug (Kwan and Brodie, 2000). If therapy with a second single drug also is inadequate, combination therapy is warranted. This decision should not be taken lightly because most patients obtain optimal seizure control with the fewest adverse effects when taking a single drug. The chances of complete control with this approach are not high; according to Kwan and Brodie (2000), epilepsy is controlled by treatment with two drugs in only 3% of patients. Side effects of each drug and the potential drug interactions also should be considered. Essential to optimal management of epilepsy is the filling out of a seizure chart by the patient or a relative. Frequent visits to the physician may be necessary early in the period of treatment because hematological and other possible side effects may require a change in medication. Measurement of plasma drug concentration at appropriate intervals facilitates the initial adjustment of dosage to minimize dose-related adverse effects without sacrificing seizure control. Knowledge of plasma drug concentrations can be especially helpful during multidrug therapy. If toxicity occurs, monitoring helps to identify the particular drug(s) responsible and can guide adjustment of dosage. Typically, 80% of recurrences will occur within 4 months of discontinuing therapy. The clinician and patient must weigh the risk of recurrent seizure and the associated potential deleterious consequences. The choice between carbamazepine and phenytoin required assessment of toxic effects of each drug. Decreased libido and impotence were associated with all three drugs (carbamazepine 13%, phenobarbital 16%, and phenytoin 11%). In direct comparison with valproate, carbamazepine provided superior control of complex focal seizures (Mattson et al. With respect to adverse effects, carbamazepine was more commonly associated with skin rash, but valproate was more commonly associated with tremor and weight gain. Overall, carbamazepine and phenytoin are preferable for treatment of focal seizures, but phenobarbital and valproate are also efficacious. Control of secondarily generalized tonic-clonic seizures does not differ significantly with carbamazepine, phenobarbital, or phenytoin (Mattson et al. Valproate was as effective as carbamazepine for control of secondarily generalized tonic-clonic seizures (Mattson et al. Because secondarily generalized tonic-clonic seizures usually coexist with focal seizures, these data indicate that among drugs introduced before 1990, carbamazepine and phenytoin are the first-line drugs for these conditions. One key issue confronting the treating physician is choosing the optimal drug for initiating treatment in new-onset epilepsy. At first glance, this issue may appear unimportant because about 50% of newly diagnosed patients become seizure free with the first drug, whether old or new drugs are used (Kwan and Brodie, 2000). However, responsive patients typically receive the initial drug for several years, underscoring the importance of proper drug selection. Phenytoin, carbamazepine, and phenobarbital also enhance metabolism of endogenous compounds, including gonadal steroids and vitamin D, potentially affecting reproductive function and bone density. Factors arguing against use of recently introduced drugs include higher costs and less clinical experience with the compounds. Insufficient evidence is available on the remaining newly introduced drugs to permit meaningful assessment of their effectiveness for this indication. Tapering and discontinuing therapy should be considered if the patient is seizure free after 2 years; tapering should be done slowly over several months. The risk of recurrent seizures ranges from 12% to 322 Generalized Absence Seizures Ethosuximide and valproate are considered equally effective in the treatment of generalized absence seizures (Mikati and Browne, 1988). Between 50% and 75% of newly diagnosed patients are free of seizures following therapy with either drug. If tonic-clonic seizures are present or emerge during therapy, valproate is the agent of first choice. Status Epilepticus and Other Convulsive Emergencies Status epilepticus is a neurological emergency. The goal of treatment is rapid termination of behavioral and electrical seizure activity; the longer the episode of status epilepticus goes untreated, the more difficult it is to control and the greater the risk of permanent brain damage. Critical to the management are a clear plan, prompt treatment with effective drugs in adequate doses, and attention to hypoventilation and hypotension. Because hypoventilation may result from high doses of drugs used for treatment, it may be necessary to assist respiration temporarily. To assess the optimal initial drug regimen, four intravenous treatments have been compared: diazepam followed by phenytoin; lorazepam; phenobarbital; and phenytoin alone (Treiman et al. The treatments had similar efficacies, with success rates ranging from 44% to 65%. No significant differences were found with respect to recurrences or adverse reactions. Thus, emergency treatment with midazolam (intramuscular) may prove to be the preferred treatment prior to arrival to the hospital. Levetiracetam also has demonstrated efficacy as adjunctive therapy for refractory generalized myoclonic seizures. Febrile Convulsions Between 2% and 4% of children experience a convulsion associated with a febrile illness; 25%33% of these children will have another febrile convulsion. Only 2%3% become epileptic in later years, a 6-fold increase in risk compared with the general population. Several factors are associated with an increased risk of developing epilepsy: preexisting neurological disorder or developmental delay, a family history of epilepsy, or a complicated febrile seizure. If all of these risk factors are present, the risk of developing epilepsy is about 10%. Uncertainties regarding the efficacy of prophylaxis for reducing epilepsy combined with substantial side effects of phenobarbital prophylaxis (Farwell et al. For children at high risk of developing recurrent febrile seizures and epilepsy, rectally administered diazepam at the time of fever may prevent recurrent seizures and avoid side effects of chronic therapy. Issues include interactions with oral contraceptives, potential teratogenic effects, and effects on vitamin K metabolism in pregnant women (Pack, 2006). Guidelines for the care of women with epilepsy have been published by the American Academy of Neurology (Morrell, 1998). Corticotropin or glucocorticoids are commonly used; repository corticotropin is designated as an orphan drug for this purpose. The Lennox-Gastaut syndrome is a severe form of epilepsy that usually begins in childhood and is characterized by cognitive impairments and multiple types of seizures, including tonic-clonic, tonic, atonic, myoclonic, and atypical absence seizures. Felbamate also is effective for seizures in this syndrome, but the occasional occurrence of aplastic anemia and hepatic failure have limited its use (French et al. These teratogenic effects add to the deleterious consequences of oral contraceptive failure. Infants of epileptic mothers are at 2-fold greater risk of major congenital malformations than offspring of nonepileptic mothers (4%8% compared to 2%4%). These malformations include congenital heart defects, neural tube defects, cleft lip, cleft palate, and others. Phenytoin, carbamazepine, valproate, lamotrigine, and phenobarbital all have been associated with teratogenic effects. Public Health Service for all women of childbearing age to reduce the likelihood of neural tube defects, and this is appropriate for epileptic women as well.
The expanding roles of Gbg subunits in G proteincoupled receptor signaling and drug action treatment ketoacidosis order glucophage sr 500mg with visa. Transient receptor potential channels as drug targets: from the science of basic research to the art of medicine medicine 7 year program glucophage sr 500 mg purchase. Emerging paradigms of beta-arrestin-dependent seven transmembrane receptor signaling medications held for dialysis purchase generic glucophage sr on-line. Inflammasomes in neuroinflammation and changes in brain function: a focused review treatment 4 addiction purchase glucophage sr 500mg on-line. With the advent of more selective and safer drugs everlast my medicine purchase 500 mg glucophage sr fast delivery, the use of antidepressants and anxiolytics has moved from the exclusive domain of psychiatry to other medical specialties, including primary care. The relative safety of the majority of commonly used antidepressants and anxiolytics notwithstanding, their optimal use requires a clear understanding of their mechanisms of action, pharmacokinetics, adverse effects, potential drug interactions, and the differential diagnosis of psychiatric illnesses (Thronson and Pagalilauan, 2014). Both depression and anxiety can affect an individual patient simultaneously; some of the drugs discussed here are effective in treating both types of disorders, suggesting common underlying mechanisms of pathophysiology and response to pharmacotherapy. While depression and anxiety disorders comprise a wide range of symptoms, including changes in mood, behavior, somatic function, and cognition, some progress has been made in developing animal models that respond with some sensitivity and selectivity to antidepressant or anxiolytic drugs (Cryan and Holmes, 2005; Xu et al. The last half-century has seen notable advances in the discovery and development of drugs for treating depression and anxiety (Hillhouse and Porter, 2015). Further, depression often complicates the management of other medical conditions. Given that approximately 10%15% of those with severe depression attempt suicide at some time (Chen and Dilsaver, 1996), it is important that symptoms of depression be recognized and treated in a timely manner. Furthermore, the response to treatment must be assessed and decisions made regarding continued treatment with the initial drug, dose adjustment, adjunctive therapy, or alternative medication. Symptoms of Anxiety Anxiety is a normal human emotion that serves an adaptive function from a psychobiological perspective. In general, symptoms of anxiety that lead to pharmacological treatment are those that interfere significantly with normal function. Drug treatment includes acute drug administration to manage episodes of anxiety and chronic treatment to manage unrelieved and continuing anxiety disorders. Symptoms of anxiety also are often associated with depression and other medical conditions. Characterization of Depressive and Anxiety Disorders Symptoms of Depression Depression is classified as major depression. Females are affected with major depression twice as frequently as males (Kessler et al. Depressive episodes are characterized by sad mood, pessimistic worry, diminished interest in normal activities, mental slowing and poor concentration, insomnia or increased sleep, significant weight loss or gain due to altered eating and activity patterns, psychomotor agitation or retardation, feelings of guilt and worthlessness, decreased energy and libido, and suicidal ideation. In depressive episodes, these symptoms occur most days for a period of at least 2 weeks. In some cases, the primary complaint of patients involves somatic pain or other physical symptoms and can present a diagnostic challenge for primary care physicians. Depressive symptoms also can occur secondary to Pharmacotherapy for Depression and Anxiety In general, antidepressants enhance serotonergic or noradrenergic transmission. In monoamine systems, neurotransmitter reuptake occurs via presynaptic high-affinity transporter proteins; inhibition of these transporters enhances neurotransmission, presumably by slowing clearance of the transmitter and prolonging its dwell time in the synapse (Shelton and Lester, 2006). While some of the lag is pharmacokinetic in nature, it is likely that a component is related to delayed postsynaptic changes. After the successful initial treatment phase, a 6- to 12-month maintenance treatment phase is typical, after which the drug is gradually withdrawn. Approximately two-thirds of patients show a marked decrease in depressive symptoms with an initial course of treatment, with one-third showing complete remission (Rush et al. A controversial issue regarding the use of all antidepressants is their relationship to suicide (Mann et al. Data establishing a clear link between antidepressant treatment and suicide are lacking. For seriously depressed patients, the risk of not being on an effective antidepressant drug outweighs the risk of being treated with one (Gibbons et al. However, it is important to monitor patients closely, particularly during initial treatment. Long-term effects of antidepressant drugs evoke regulatory mechanisms that might contribute to the effectiveness of therapy (Shelton, 2000). These responses include altered adrenergic or serotonergic receptor density or sensitivity, altered receptorG protein coupling and cyclic nucleotide signaling, induction of neurotrophic factors, and increased neurogenesis in the hippocampus (Schmidt and Duman, 2007). Genome-wide association studies have suggested novel pathways that might be exploited for the discovery of antidepressants (Cannon and Keller, 2006; Lin and Lane, 2015). Chronic treatment with a number of antidepressants desensitizes presynaptic autoreceptors and heteroreceptors, producing long-lasting changes in monoaminergic neurotransmission. Li+ may also alter release of neurotransmitters by a variety of putative mechanisms (see Chapter 16: Hypotheses for the Mechanism of Action of Lithium and Relationship to Anticonvulsants). Duloxetine, in addition to being approved for use in the treatment of depression and anxiety, is used for treatment of fibromyalgia and neuropathic pain associated with peripheral neuropathy (Finnerup et al. These include two close structural analogues, trazodone and nefazodone, as well as mirtazapine and mianserin (not marketed in the U. Both mianserin and mirtazapine are quite sedating and are treatments of choice for some depressed patients with insomnia. The hydroxybupropion metabolite may contribute to the therapeutic effects of the parent compound: this metabolite appears to have a similar pharmacology and is present at substantial levels. Bupropion is indicated for the treatment of depression, prevention of seasonal depressive disorder, and as a smoking cessation treatment (Carroll et al. The mechanism of action and adverse effects of the atypical antipsychotics are described in Chapter 16. The major risks of these agents are weight gain and metabolic syndrome, a greater problem for quetiapine and olanzapine than for aripiprazole. Selegiline is available as a transdermal patch for the treatment of depression; transdermal delivery may reduce the risk for diet-associated hypertensive reactions. The olanzapine-fluoxetine combination is available in fixed-dose combinations of 3, 6, or 12 mg of olanzapine and 25 or 50 mg of fluoxetine. Likewise, dose considerations have to include awareness of hepatic function (Mauri et al. Both immediate-release and extended-release (tablet or capsule) preparations of venlafaxine result in steady-state levels of drug in plasma within 3 days. The elimination half-lives for the parent venlafaxine and its active and major metabolite desmethylvenlafaxine are 5 and 11 h, respectively. Venlafaxine dose reductions are suggested for patients with renal or hepatic impairment. Duloxetine is not recommended for those with end-stage renal disease or hepatic insufficiency. The recommended initial dosing of mirtazapine is 15 mg/d, with a maximal recommended dose of 45 mg/d. Clearance of mirtazapine is decreased in the elderly and in patients with moderate-to-severe renal or hepatic impairment. Pharmacokinetics and adverse effects of mirtazapine may have an enantiomer-selective component (Brockmöller et al. Trazodone typically is started at 150 mg/d in divided doses, with 50-mg increments every 34 days. The maximally recommended dose is 400 mg/d for outpatients and 600 mg/d for inpatients. Nefazodone has a t1/2 of only 24 h; its major metabolite hydroxynefazodone has a t1/2 of 1. Bupropion elimination has a t1/2 of 21 h and involves both hepatic and renal routes. Patients with severe hepatic cirrhosis should receive a maximum dose of 150 mg every other day; consideration for a decreased dose should also be made in cases of renal impairment. Steady-state concentrations occur within several days to several weeks of beginning treatment, as a function of the t1/2. Nonetheless, monitoring the plasma exposure has an important relationship to treatment response: There is a relatively narrow therapeutic window. To avoid toxicity in "slow metabolizers," plasma levels should be monitored and doses adjusted downward. Monoamine Oxidase Inhibitors has not yet been shown to have a practical influence on choice of drug treatment in clinical settings (Dubovsky, 2015). In the case of fluoxetine, the combined action of the parent and the demethylated metabolite norfluoxetine allows for a once-weekly formulation. Aspects of sexual dysfunction can be treated in both men and women with the phosphodiesterase 5 inhibitor sildenafil (Nurnberg, 2001; Nurnberg et al. With continued treatment, some patients also report a dullness of intellectual abilities and concentration. Thus, dosage adjustments are based more on evaluation of clinical response and management of side effects. Sudden withdrawal of antidepressants can precipitate a discontinuation syndrome (Harvey and Slabbert, 2014). This withdrawal syndrome appears most intense for paroxetine and venlafaxine due to their relatively short half-lives and, in the case of paroxetine, lack of active metabolites. Conversely, the active metabolite of fluoxetine, norfluoxetine, has such a long t1/2 (12 weeks) that few patients experience any withdrawal symptoms with discontinuation of fluoxetine. The immediate-release formulation of venlafaxine can induce sustained diastolic hypertension (diastolic blood pressure > 90 mm Hg at consecutive weekly visits) in 10%15% of patients at higher doses; this risk is reduced with the extended-release form. Serotonin Receptor Antagonists Regarding the serotonin receptor antagonists, the main side effects of mirtazapine, seen in more than 10% of the patients, are somnolence, increased appetite, and weight gain. Nefazodone was voluntarily withdrawn from the market in several countries after rare cases of liver failure were associated with its use. Bupropion Typical side effects associated with bupropion include anxiety, mild tachycardia and hypertension, irritability, and tremor. Other side effects include headache, nausea, dry mouth, constipation, appetite suppression, insomnia, and, rarely, aggression, impulsivity, and agitation. Seizures are dependent on dose and Cp, with seizures occurring rarely within the recommended dose range. Bupropion should be avoided in patients with seizure disorders as well as those with bulimia due to an increased risk of seizures (Horne et al. At doses higher than that recommended for depression (450 mg/d), the risk of seizures increases significantly. The use of extended-release formulations often blunts the maximum concentration observed after dosing and minimizes the chance of reaching drug levels associated with an increased risk of seizures. Antagonism of 1 adrenergic receptors contributes to orthostatic hypotension and sedation. This is the primary reason that only a limited supply should be available to the patient at any given time. Tricyclic Antidepressants Values are experimentally determined potencies (Ki values, nM) for binding to receptors that contribute to common side effects of clinically used antidepressant drugs: muscarinic cholinergic receptors. The released catecholamines stimulate postsynaptic receptors in the periphery, increasing blood pressure to dangerous levels. Symptoms of the serotonin syndrome include hyperthermia, muscle rigidity, myoclonus, tremors, autonomic instability, confusion, irritability, and agitation; this can progress toward coma and death. The benzodiazepines are effective anxiolytics as both acute and chronic treatment. There is concern regarding their use because of their potential for dependence and abuse as well as negative effects on cognition and memory. Antihistamines and sedative-hypnotic agents have been tried as anxiolytics but are generally not recommended because of their side-effect profiles and the availability of superior drugs. Hydroxyzine, which produces short-term sedation, is used in patients who cannot use other types of anxiolytics. Chloral hydrate has been used for situational anxiety, but there is a narrow dose range where anxiolytic effects are observed in the absence of significant sedation; therefore, the use of chloral hydrate is not recommended. Failure to observe these required waiting periods can result in the serotonin syndrome. Clinical Considerations With Anxiolytic Drugs the choice of pharmacological treatment of anxiety is dictated by the specific anxiety-related disorders and the clinical need for acute anxiolytic effects (Millan, 2003). Among the commonly used anxiolytics, only the benzodiazepines and adrenergic antagonists are effective acutely; the use of adrenergic antagonists is generally limited to treatment of situational anxiety. When an immediate anxiolytic effect is desired, benzodiazepines are typically selected. In addition to their anxiolytic effects, benzodiazepines produce sedative, hypnotic, anesthetic, anticonvulsant, and muscle relaxant effects. The benzodiazepines also impair cognitive performance and memory, adversely affect motor control, and potentiate the effects of other sedatives, including alcohol. One area of concern regarding the use of benzodiazepines in the treatment of anxiety is the potential for habituation, dependence, and abuse. Patients with certain personality disorders or a history of drug or alcohol abuse are particularly susceptible. However, the risk of dependence must be balanced with the need for treatment because benzodiazepines are effective in both short- and long-term treatment of patients with sustained or recurring bouts of anxiety. Further, premature discontinuation of benzodiazepines, in the absence of other pharmacological treatment, results in a high rate of relapse. Withdrawal of benzodiazepines after chronic treatment, particularly with benzodiazepines with short durations of action, can include increased anxiety and seizures. For this reason, it is important that discontinuation be carried out in a gradual manner. Benzodiazepines cause many adverse effects, including sedation, mild memory impairments, decreased alertness, and slowed reaction time (which may lead to accidents). Memory problems can include visual-spatial deficits but will manifest clinically in a variety of ways, including difficulty in word finding.
In clinical practice treatment algorithm 500mg glucophage sr order with amex, adverse effects during therapy with verapamil or diltiazem are determined largely by underlying heart disease and concomitant therapy; plasma concentrations of these agents are not measured routinely medications recalled by the fda buy genuine glucophage sr on line. Both drugs can increase serum digoxin concentration symptoms 22 weeks pregnant purchase glucophage sr 500 mg visa, although the magnitude of this effect is variable; excess slowing of ventricular response may occur in patients with atrial fibrillation inoar hair treatment cheap 500 mg glucophage sr with visa. Epinephrine-induced hypokalemia appears to be mediated by 2 adrenergic receptors and is blocked by "noncardioselective" antagonists such as propranolol (see Chapter 12) treatment 34690 diagnosis glucophage sr 500mg purchase without prescription. In acutely ischemic tissue, blockers increase the energy required to fibrillate the heart, an antiarrhythmic action. These effects may contribute to the reduced short-term and long-term mortality observed in trials of chronic therapy with blockers-after myocardial infarction (Singh, 1990). Adverse effects of blockade include fatigue, bronchospasm, hypotension, impotence, depression, aggravation of heart failure, worsening of symptoms owing to peripheral vascular disease, and masking of the symptoms of hypoglycemia in diabetic patients (see Chapter 12). In such patients, arrhythmias should be treated with both and blockers or with a drug such as labetalol that combines - and -blocking properties. Abrupt discontinuation of chronic -blocker therapy can lead to "rebound" symptoms, including hypertension, increased angina, and arrhythmias; thus, blockers are tapered over 2 weeks prior to discontinuation of chronic therapy (see Chapters 12 and 2729). Some, such as propranolol, also exert Na+ channelblocking effects at high concentrations. Similarly, drugs with intrinsic sympathomimetic activity may be less useful as antiarrhythmics (Singh, 1990). Acebutolol is as effective as quinidine in suppressing ventricular ectopic beats, an arrhythmia that many clinicians no longer treat. Sotalol (see its discussion in a separate section) is more effective for many arrhythmias than other blockers, probably because of its K+ channelblocking actions. Esmolol (see separate discussion that follows) is a 1-selective agent that has a very short elimination half-life. Intravenous esmolol is useful in clinical situations in which immediate adrenergic blockade is desired. Moreover, antiarrhythmic drugs can induce new arrhythmias with possibly fatal consequences. Nonpharmacological Blockade of Adrenergic Receptors 560 treatments, such as cardiac pacing, electrical defibrillation, or ablation of targeted regions, are indicated for some arrhythmias; in other cases, no therapy is required, even though an arrhythmia is detected. Therefore, the fundamental principles of therapeutics described here must be applied to optimize antiarrhythmic therapy. In choosing among available therapeutic options, it is important to establish clear therapeutic goals. Most patients with atrial fibrillation also benefit from anticoagulation to reduce stroke incidence regardless of symptoms (Dzeshka and Lip, 2015) (see Chapter 32). The frequency and reproducibility of arrhythmia should be established prior to initiating therapy because inherent variability in the occurrence of arrhythmias can be confused with a beneficial or adverse drug effect. Techniques for this assessment include recording cardiac rhythm for prolonged periods or evaluating the response of the heart to artificially induced premature beats. Identify and Remove Precipitating Factors Factors that commonly precipitate cardiac arrhythmias include hypoxia, electrolyte disturbances (especially hypokalemia), myocardial ischemia, and certain drugs. Antiarrhythmics, including cardiac glycosides, are not the only drugs that can precipitate arrhythmias (Table 301). For example, theophylline can cause multifocal atrial tachycardia, which sometimes can be managed simply by reducing the dose of theophylline. Torsades de pointes can arise during therapy not only with action potentialprolonging antiarrhythmics but also with other "noncardiovascular" drugs not ordinarily classified as having effects on ion channels (Roden, 2004). The incidence can vary from 1% to 3% in patients receiving sotalol or dofetilide to very rare (<1/50,000) with some noncardiovascular drugs. Drugs with a very wide range of clinical indications have been implicated: these include some antibiotics (including antibacterials, antiprotozoals, antivirals, and antifungals), antipsychotics, antihistamines, antidepressants, and methadone. However, the mere detection of an abnormality does not equate with the need for therapy. Unexpectedly, the mortality rate was 2- to 3-fold higher among patients treated with the drugs than those treated with placebo (Echt et al. While the explanation for this effect is not known, several lines of evidence suggest that, in the presence of these drugs, transient episodes of myocardial ischemia or sinus tachycardia can cause marked conduction slowing (because these drugs have a very long recovery), resulting in fatal reentrant ventricular tachyarrhythmias. One consequence of this pivotal clinical trial was to reemphasize the concept that therapy should be initiated only when a clear benefit to the patient can be identified. When symptoms are obviously attributable to an ongoing arrhythmia, there usually is little doubt that termination of the arrhythmia will be beneficial; when chronic therapy is used to prevent recurrence of an arrhythmia, the risks may be greater (Roden, 1994). Among the antiarrhythmic drugs discussed here, only adrenergic blockers and, to a lesser extent, amiodarone (Connolly, 1999) demonstrably reduce mortality during long-term therapy. Some patients may present with presyncope, syncope, or even cardiac arrest, which may be due to brady- or tachyarrhythmias. Finally, patients may present with symptoms owing to decreased cardiac output attributable to arrhythmias. Occasionally, sustained or frequent tachycardias may produce no "arrhythmia" symptoms (such as palpitations) but will depress Cardiac transplant Noncardiac Diarrhea Prostatism, glaucoma Arthritis Lung disease Tremor Constipation Asthma, peripheral vascular disease, hypoglycemia of paroxysms of atrial fibrillation may be sufficient to render a patient asymptomatic even if an occasional episode still can be detected. Adenosine Adenosine is a naturally occurring nucleoside that is administered as a rapid intravenous bolus for the acute termination of reentrant supraventricular arrhythmias (Link, 2012). Adenosine also has been used to produce controlled hypotension during some surgical procedures and in the diagnosis of coronary artery disease. Minimize Risks Antiarrhythmic Drugs Can Cause Arrhythmias One well-recognized risk of antiarrhythmic therapy is the possibility of provoking new arrhythmias, with potentially life-threatening consequences. Antiarrhythmic drugs can provoke arrhythmias by different mechanisms (Table 301). These drug-provoked arrhythmias must be recognized because further treatment with antiarrhythmic drugs often exacerbates the problem, whereas withdrawal of the causative agent is curative. Thus, establishing a precise diagnosis is critical, and targeting therapies at underlying mechanisms of the arrhythmias may be required. For example, treating a ventricular tachycardia with verapamil not only may be ineffective but also can cause catastrophic cardiovascular collapse. Monitoring of Plasma Concentration Some adverse effects of antiarrhythmic drugs result from excessive plasma drug concentrations. Measuring plasma concentration and adjusting the dose to maintain the concentration within a prescribed therapeutic range may minimize some adverse effects. In many patients, serious adverse reactions relate to interactions involving antiarrhythmic drugs (often at usual plasma concentrations), transient factors such as electrolyte disturbances or myocardial ischemia, and the type and extent of the underlying heart disease (Roden, 1994). Factors such as generation of unmeasured active metabolites, variability in elimination of enantiomers (which may exert differing pharmacological effects), and disease- or enantiomer-specific abnormalities in drug binding to plasma proteins can complicate the interpretation of plasma drug concentrations. Another way to minimize the adverse effects of antiarrhythmic drugs is to avoid certain drugs in certain patient subsets altogether. For example, patients with a history of congestive heart failure are particularly prone to develop heart failure during disopyramide therapy. In other cases, adverse effects of drugs may be difficult to distinguish from exacerbations of underlying disease. Amiodarone may cause interstitial lung disease; its use therefore is undesirable in a patient with advanced pulmonary disease in whom the development of this potentially fatal adverse effect would be difficult to detect. Specific diseases that constitute relative or absolute contraindications to specific drugs are listed in Table 304. A bolus of adenosine can produce transient sympathetic activation by interacting with carotid baroreceptors; a continuous infusion can cause hypotension. Consider the Electrophysiology of the Heart as a "Moving Target" Cardiac electrophysiology varies dynamically in response to external influences such as changing autonomic tone, myocardial ischemia, and myocardial stretch (Priori et al. For example, myocardial ischemia results in changes in extracellular K+ that make the resting potential less negative, inactivate Na+ channels, decrease Na+ current, and slow conduction. Thus, in response to myocardial ischemia, a normal heart may display changes in resting potential, conduction velocity, intracellular Ca2+ concentrations, and repolarization, any one of which then may create arrhythmias or alter response to antiarrhythmic therapy. A major advantage of adenosine therapy is that adverse effects are shortlived because the drug is transported into cells and deaminated so rapidly. Transient asystole (lack of any cardiac rhythm whatsoever) is common but usually lasts less than 5 sec and is in fact the therapeutic goal. Most patients feel a sense of chest fullness and dyspnea when therapeutic doses (6 to 12 mg) of adenosine are administered. Rarely, an adenosine bolus can precipitate atrial fibrillation, presumably by heterogeneously shortening atrial action potentials, or bronchospasm. Adenosine is eliminated with a half-life of seconds by carrier-mediated uptake, which occurs in most cell types, including the endothelium, followed by metabolism by adenosine deaminase. Adenosine probably is the only drug whose efficacy requires a rapid bolus dose, preferably through a large central intravenous line; slow administration results in elimination of the drug prior to its arrival at the heart. The effects of adenosine are potentiated in patients receiving dipyridamole, an adenosine-uptake inhibitor, and in patients with cardiac transplants owing to denervation hypersensitivity. Clinical Pharmacokinetics Antiarrhythmic Drugs Summaries of important electrophysiological and pharmacokinetic features of the drugs considered here are presented in Tables 303 and 305. Prescribing patterns have changed over the past several decades in part because fewer suppliers market older drugs, such as quinidine or procainamide, which are therefore increasingly difficult to obtain, a problem for a small number of patients who may still benefit from treatment (Inama et al. Amiodarone Amiodarone exerts a multiplicity of pharmacological effects, none of which is clearly linked to its arrhythmia-suppressing properties. Amiodarone is a structural analogue of thyroid hormone, and some of its antiarrhythmic 564 actions and its toxicity may be attributable to interaction with nuclear thyroid hormone receptors. Amiodarone is highly lipophilic, is concentrated in many tissues, and is eliminated extremely slowly; consequently, adverse effects may resolve very slowly. Trials of oral amiodarone have shown a modest beneficial effect on mortality after acute myocardial infarction (Amiodarone Trials Meta-Analysis Investigators, 1997). Despite uncertainties about its mechanisms of action and the potential for serious toxicity, amiodarone is used widely in the treatment of common arrhythmias such as atrial fibrillation (Roy et al. Amiodarone blocks inactivated Na+ channels and has a relatively rapid rate of recovery (time constant 1. It also decreases Ca2+ current and transient outward delayed rectifier and inward rectifier K+ currents and exerts a noncompetitive adrenergic-blocking effect. Amiodarone potently inhibits abnormal automaticity and, in most tissues, prolongs action potential duration. Amiodarone decreases conduction velocity by Na+ channel block and by a poorly understood effect on cell-cell coupling that may be especially important in diseased tissue. Amiodarone prolongs refractoriness in all cardiac tissues; Na+ channel block, delayed repolarization owing to K+ channel block, and inhibition of cell-cell coupling all may contribute to this effect. This incomplete bioavailability is important in calculating equivalent dosing regimens when converting from intravenous to oral therapy. The drug distributes into lipid; heart tissue-to-plasma concentration ratios of greater than 20:1 and lipid-to-plasma ratios of greater than 300:1 have been reported. After the initiation of amiodarone therapy, increases in refractoriness, a marker of pharmacological effect, require several weeks to develop. When amiodarone therapy is withdrawn from a patient who has been receiving therapy for several years, plasma concentrations decline with a half-life of weeks to months. The mechanisms of amiodarone and desethyl-amiodarone elimination are not well established. However, efficacy apparently depends as much on duration of therapy as on plasma concentration, and elevated plasma concentrations do not predict toxicity. The maintenance dose is adjusted based on adverse effects and the arrhythmias being treated. If the presenting arrhythmia is life threatening, dosages of more than 300 mg/d normally are used unless unequivocal toxicity occurs. On the other hand, maintenance doses of 200 mg/d or less are used if recurrence of an arrhythmia would be tolerated, as in patients with atrial fibrillation, because amiodarone slows the ventricular rate during atrial fibrillation. Amiodarone potently inhibits the hepatic metabolism or renal elimination of many compounds. While depressed contractility can occur during long-term oral therapy, it is unusual. Despite administration of high doses that would cause serious toxicity if continued long term, adverse effects are unusual during oral drug-loading regimens, which typically require several weeks. Occasional patients develop nausea during the loading phase, which responds to a decrease in daily dose. Adverse effects during long-term therapy reflect both the size of daily maintenance doses and the cumulative dose, suggesting that tissue accumulation may be responsible. The most serious adverse effect during chronic amiodarone therapy is pulmonary fibrosis, which can be rapidly progressive and fatal. Underlying lung disease, doses of 400 mg/d or more, and recent pulmonary insults such as pneumonia appear to be risk factors. Serial chest X-rays or pulmonary function studies may detect early amiodarone toxicity, but monitoring plasma concentrations has not been useful. With low doses, such as 200 mg/d or less as used in atrial fibrillation, pulmonary toxicity is less common (Zimetbaum, 2007). Other adverse effects during long-term therapy include corneal microdeposits (which often are asymptomatic), hepatic dysfunction, neuromuscular symptoms (most commonly peripheral neuropathy or proximal muscle weakness), photosensitivity, and hypo- or hyperthyroidism. The multiple effects of amiodarone on thyroid function are discussed further in Chapter 43. Treatment consists of withdrawal of the drug and supportive measures, including corticosteroids, for life-threatening pulmonary toxicity; reduction of dosage may be sufficient if the Bretylium Bretylium is a quaternary ammonium compound that prolongs cardiac action potentials and interferes with reuptake of norepinephrine by sympathetic neurons. Their inotropic action results from increased intracellular Ca 2+, which also forms the basis for arrhythmias related to cardiac glycoside intoxication. However, sympathetic drive is increased markedly in many patients with advanced heart failure, so digitalis is not very effective in decreasing the rate; on the other hand, even a modest decrease in rate can ameliorate heart failure. In heart transplant patients, in whom innervation has been ablated, cardiac glycosides are ineffective for rate control. Because of the low therapeutic index of cardiac glycosides, their toxicity is a common clinical problem (see Chapter 29).
Discount glucophage sr. SHINee - Symptoms [Full Audio].
References
- Ng EK, Larn YH, Sung JJ, et al. Eradication of Helicobacter pylori prevents recurrence of ulcer after simple closure of duodenal ulcer perforation: randomized controlled trial. Ann Surg. 2000: 231:153.
- Djavan B, Zlotta A, Remzi M, et al: Optimal predictors of prostate cancer on repeat prostate biopsy: a prospective study of 1,051 men, J Urol 163:1144n 1148, discussion 1148n9, 2000.
- Beutler E. PGK deficiency. Br J Haematol. 2007;136:3-11.
- Schinkel AF, Bax JJ, Poldermans D, et al: Hibernating myocardium: Diagnosis and patient outcomes, Curr Probl Cardiol 32:375-410, 2007.
- Mayer J, Boldt J, Wolf MW, Lang J, Suttner S. Cardiac output derived from arterial pressure waveform analysis in patients undergoing cardiac surgery: validity of a second generation device. Anesth Analg. 2008;106(3):867-872, table of contents. 23.
- Frajzyngier V, Li G, Larson E, et al: Development and comparison of prognostic scoring systems for surgical closure of genitourinary fistula, Am J Obstet Gynecol 208(2):112 e111, 2013.
