
Naprosyn
| Contato
Página Inicial
David Robertson MD
- Elton Yates Professor of Medicine, Pharmacology and Neurology
- Vanderbilt University
- Director, Clinical & Translational Research Center, vanderbilt institute for Clinical and Translational Research, Nashville
https://ww2.mc.vanderbilt.edu/neurology/26258
Myasthenia gravis is an autoimmune or congenital neuromuscular disorder that involves muscles throughout the body and the nerves that control them lifespan arthritis dogs cheap 500 mg naprosyn with mastercard. A group of bacteria that includes Mycobacterium tuberculosis sarcoid arthritis definition best 500 mg naprosyn, the bacterium that causes tuberculosis crippling arthritis definition purchase naprosyn online pills, and other forms that cause related illnesses arthritis.org/eating well buy discount naprosyn 500 mg on-line. The most common form of T-cell lymphoma of the skin; symptoms include rash chronic arthritis definition purchase discount naprosyn on line, tumors, skin lesions, and itchy skin. A protein that is important in maintaining the structure of myelin, a material that forms an insulating sheath around the axon of a nerve cell. A protective cover that surrounds nerve cells and helps to increase the speed by which information travels along the nerve. Bone marrow disorders that are late effects of cancer treatment and that may progress to acute myelogenous leukemia. An infection of the brain by the pork tapeworm called Taenia solium, resulting in the establishment of larva-containing cysts throughout the brain substance. A rare but dangerous reaction to antipsychotic medications that involves temperature instability, muscular rigidity, and altered mental status. Severe acne characterized by large papules (elevated areas of skin without visible fluid) that may be as much as 5Â10 mm (0. A cancer of the lymph system that causes the accumulation of large numbers of cancerous immune system cells. A naturally occurring chemical in the body that carries chemical messages to nerve cells, often by transmitting nerve impulses. Many are sold without a prescription, such as ibuprofen and acetaminophen, while others are prescribed by doctors. Also called noradrenaline, a chemical messenger in the brain that regulates attention and that powers the "fight-or-flight" stress response; precursor of epinephrine. An antiretroviral drug that interferes with the action of viral reverse transcriptase inside infected cells, preventing the virus from replicating. A condition of the eyes that is characterized by involuntary eye movement and results in reduced or limited vision. A disorder in which affected individuals have an obsession (such as a fear of contamination, or thoughts they do not like to have and cannot control) and feel compelled to perform certain acts to neutralize the obsession (such as repeated hand washing). Plaque- treatment-resistant chronic headache that begins abruptly and may last for years. Over-thecounter and prescription products that supply low doses of nicotine as smoking-cessation aids. A potentially life- Dilating vessels helps improve blood flow and blood pressure in the arteries. The most common form of arthritis, characterized by erosion of the cartilage layer that lies between the bones in weight-bearing joints. Large cells associated with bone resorption, or removal, and normally helping to allow new bone to form. A problem with many causes, such as age, pregnancy, and obesity, that results in frequent and urgent trips to the restroom to urinate and sometimes in leakage of urine. The phase of the female monthly cycle when a developed egg is released from the ovary into the fallopian tube for possible fertilization. The use of a prescription medication to treat conditions outside the indications approved by the U. A physician who specializes in the diagnosis and treatment of patients with cancer. A progressive form of glaucoma in which the drainage channel for the aqueous humor remains open; serious reduction in vision occurs in advanced stages. A drug containing or derived from opium- such as codeine, morphine, and heroin-that alleviates pain and induces sleep. A substance that resembles opium and binds to the same types of receptors in the body, producing similar effects in pain relief, pleasure, and addictiveness. A rare, chronic bone condition that causes some bones in the affected person to soften. Care given to relieve pain and other symptoms of a disease, but not to cure the disease. A small organ in the upper abdomen that produces insulin and enzymes that aid in food digestion. Inflammation of the pancreas, either acute (sudden and episodic) or chronic, usually caused by excessive alcohol intake or gallbladder disease. An anxiety disorder in which an individual experiences sudden, debilitating attacks of intense fear. A class of disorders characterized by progressive deterioration of mental processes caused by temporary brain dysfunction or permanent brain damage. Symptoms include delusions, dementia, amnesia, and delirium that are not caused by drugs, alcohol, or as a side effect of medication. A medication that has been developed to treat a rare disease, defined in the United States as a disease or disorder affecting fewer than 200,000 people. Condition in which an individual has an irrational suspicion about another person or situation. The portion of the nervous system that is concerned with normal maintenance functions including digestion and normal heart rate. Pegylated interferon; an antiviral drug used in combination with sofosbuvir for treating hepatitis C. Inflammation of the female reproductive tract, caused by any of several microorganisms. Inflammation of the sac around the the concentration of calcium, vitamin D, and phosphorus in the blood. A disease of the nervous system most common in people over age 60, characterized by a shuffling gait, muscle stiffness, and tremors. The early years preceding menopause when the natural transition to infertility is just beginning and estrogen levels are reducing gradually. Damage to the peripheral nerves (in the extremities of the body) causing numbness, tingling, or pain. The smooth membrane that lines the A regular, fast (160 to 220 beats per minute) heart rate that begins and ends suddenly and originates in heart tissue other than that in the ventricles. A substance that partially activates a receptor in the brain while blocking the neurotransmitter for that receptor from binding to it. Lozenge; troche; a solid, usually sweetened, medication designed to dissolve in the mouth. An inherited disorder in which the body lacks an enzyme needed to digest the amino acid phenylalanine. An abnormally high sensitivity to sunlight involving immune system activity and manifesting as a skin (cutaneous) reaction that is sometimes described as a sun allergy. It controls most endocrine functions and is responsible for things such as kidney function, lactation, and growth and development. A pill or liquid given during the study of a drug or dietary supplement that contains no medication or active ingredient. Usually study participants do not know if they are receiving a pill containing the drug or an identical-appearing placebo. A lump of tissue protruding from the lining of an organ, such as the nose, bladder, or intestine. Symptoms that are characterized by the production or presence of abnormal or excessive behaviors, including hallucinations and thought-process disorder. Occurring after and especially as a result of herpes, which is the virus that causes shingles. The time after which a woman has reached menopause or has not had a menstrual period for 12 consecutive months. Psychiatric disorder in which the patient experiences persistent disturbing anxiety based symptoms after experiencing a traumatic event. Area of the brain involved in attention span, judgment, response to external stimuli, memory, motor function, and impulse control. A system of classifying drugs according to their established risks for use during pregnancy. Category B: Animal studies indicate no fetal risk but no human studies exist, or adverse effects have been seen in animals but not in wellcontrolled human studies. Category C: No adequate human or animal studies exist, or adverse fetal effects have occured in animal studies but there is no available human data. A combination of emotional, physical, psychological, and mood disturbances that occur after ovulation and normally end with the onset of the menstrual flow. A compound made up of fat, cholesterol, calcium, and other substances found in the blood. Tiny blood cells that are components of the blood coagulation process in the body. An endocrine disorder in women characterized by ovarian cysts, infertility, amenorrhea (absence of menstrual periods), acne, and a male pattern of body hair. Organic compounds with many double bonds, especially within a long hydrocarbon chain. A polymer attached to filgrastim to produce pegfilgrastim, which lasts much longer in the body. A chronic liver disease characterized by inflammation of the small bile ducts in the liver. The inactive form of a drug that is metabolized into an active compound inside the body. Natural hormones, such as progesterone, and synthetic hormones, such as norelgestromin, that prepare the lining of the uterus for implantation with a fertilized egg and maintain pregnancy. A condition characterized by increased pressure around the brain in the absence of a tumor or other identifiable disorder. A chronic inflammatory condition that includes the presence of raised, red patches on the skin that are layered over with a whitish, flaky buildup of dead skin cells. High blood pressure in the pulmonary arteries that carry blood from the heart to the lungs. An obstruction of a blood vessel in the lungs, usually caused by a blood clot that blocks a coronary artery. A urinary tract infection that progresses up the urinary system to the kidneys and ureters. Prostaglandins have a wide variety of effects and may be responsible for the production of some types of pain and inflammation. The walnut-shaped gland that surrounds the urethra at the neck of the bladder in males and supplies fluid for semen. The use of high-energy radiation from x-rays, cobalt, radium, and other sources to kill cancer cells and shrink tumors. A disease found mainly in young women that causes decreased circulation to the hands and feet. A physical reaction to stopping a medication characterized by the reappearance of the symptom(s) that the medication was given to suppress. A chronic disease of the immune system that causes the body to attack the joints by mistake. Any of several contagious fungal diseases of the skin, hair, or nails characterized by ring-shaped patches. An antiviral drug that inhibits cytochrome P450 and can prevent certain drugs from being properly metabolized. A chronic skin disease characterized by persistent redness of the skin and periodic outbreaks of pustules, usually affecting the middle third of the face. A contagious viral disease that is milder than typical measles but is damaging to the fetus when it occurs early in pregnancy. Glossary on the surface of a cell, that binds to specific substances, such as hormones, to affect physiological processes. Referring to the rectum, the lowest part of the intestine, from the colon to the anus. An enzyme produced in the kidneys that controls the activation of the hormone angiotensin, which stimulates the adrenal glands to produce aldosterone. The ability of infectious agents such as viruses to change their biochemistry in such a way that renders drug treatments no longer effective. Very low breathing rate, characterized as 12 or fewer breaths per minute; also known as hypoventilation. The tissue that forms the inner surface of the back of the eyeballs; it receives the light that enters the eye and transmits it through the optic nerves to the brain to produce visual images. A life-threatening disease that affects the liver and the brain and sometimes occurs after a viral infection, such as flu or chickenpox. A disorder characterized by small groups of inflammatory cells (granulomas) that form as nodules in the lungs or other organs. A feeling of fullness or satisfaction after consuming a meal, which may reduce the amount of food consumed. A severe mental illness in which a person has difficulty distinguishing what is real from what is not real. It is often characterized by hallucinations, delusions, language and communication disturbances, and withdrawal from people and social activities. Inflammation, swelling, scarring, and destruction of bile ducts inside and outside the liver. A potentially life-threatening drug reaction involving an excess of the neurotransmitter serotonin, usually occurring when too many medications that increase serotonin are taken together, such as antimigraine triptans and certain antidepressants.
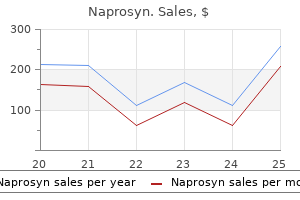
Flow technique may help delineate shallow ulcers by slowly rotating the patient so as to move the barium over the dependent surface and fill the ulcer crater test for arthritis in the knee order naprosyn 500 mg amex. Upright compression views are helpful for evaluating ulcers on the lesser curvature arthritis pain lotions order naprosyn 250 mg fast delivery. Prone compression views of the gastric antrum and body should be performed to demonstrate ulcers on the anterior wall tylenol arthritis medication side effects generic naprosyn 500 mg on line. Less commonly rheumatoid arthritis trials order cheap naprosyn on line, benign ulcers are located along the greater curvature (3% to 11%) or anterior wall (1% to 7%) arthritis relief herbs naprosyn 250 mg without a prescription. In younger patients, antral ulcers predominate; in older patients, however, benign ulcers also occur in the upper body, predominantly along the lesser curvature; these are known as geriatric ulcers. An edematous ulcer collar appears as a thick linear filling defect (ulcer collar) at the base of the ulcer crater (arrows in B). Pylori and Peptic Ulcer Disease 59 Benign ulcers on the lesser curvature typically appear as smooth, round, or ovoid craters that project beyond the contour of the adjacent gastric wall. Occasionally, inflammation surrounding the crater appears mass-like, seen in profile as smooth masses projecting into the lumen on both sides of the crater (ulcer mound). Ulcers on the dependent or posterior gastric wall fill with barium in the supine position, revealing the characteristic ulcer crater. Shallow ulcers of the posterior wall may appear as ring shadows due to barium coating the rim of an unfilled crater. Flow technique can be used to fill the crater with barium and distinguish an ulcer from a polypoid abnormality. Edema and spasm associated with antral ulcers may cause severe narrowing and deformity of the distal stomach. Anterior wall ulcers on the nondependent surface of the antrum or body may appear as ring shadows with barium coating the rim of an unfilled crater. The ulcer crater may be demonstrated by turning the patient prone, placing the ulcer on the dependent wall so that it will fill with barium. Benign gastric ulcers usually respond well to treatment with antisecretory agents. With healing, the crater decreases in size and may change shape, taking on a more linear appearance on follow-up studies. Healing ulcers can result in prominent transverse folds, deformity, and tapered luminal narrowing. Asymmetric scarring can flatten and shorten the lesser or greater curvature and create an eccentric pylorus. Severe scarring in the antral-pyloric region may appear as a short segment of narrowing with wall thickening. Differential Diagnosis Malignant ulcer: Projects into a soft tissue mass and not beyond the expected gastric contour. Findings suggesting underlying malignancy include nodularity of the ulcer crater, eccentric crater within a mass, irregularity, clubbing, or amputation of radiating folds. Ulcerated submucosal mass such as a gastrointestinal stromal tumor: Edema surrounding a benign ulcer can appear mass-like, simulating an ulcerative neoplasm. Scirrhous carcinoma: Distal gastric ulcers with massive edema, scarring, deformity, and luminal narrowing may be difficult to distinguish from malignancy. Common Variants And Mimics Variants Ulcers of the Greater Curvature Ulcers on the high greater curvature should be considered malignant until proven otherwise. Benign ulcers of the greater curvature may have suspicious features requiring endoscopy, as they may appear intraluminal due to pronounced spasm and retraction of the adjacent gastric wall. Erosions Erosions are focal areas of mucosal necrosis confined to the epithelium or lamina propria without extending through the muscularis mucosae into the submucosa. Erosions are usually located in the gastric antrum and tend to occur along thickened folds. Barium precipitations do no project beyond the outer contour of the stomach and are not associated with fold thickening. Calcifications and other densities overlying the stomach can be mistaken for ulcers (see-though phenomenon). These potential ulcer mimics should all be easily distinguished from true ulcers at fluoroscopy and by obtaining images in different projections. Management/Clinical Issues Treatment for gastric ulcers depends upon the underlying cause. H2-receptor antagonist and proton pump inhibitors may be used to diminish gastric acid and accelerate ulcer healing. Key Points Gastric ulcers are now less common than duodenal ulcers but are more likely to bleed. Ulcers on the high greater curvature should be considered malignant until proven otherwise. Detection of gastric ulcer: comparison of single- and double-contrast examination. Double-contrast upper gastrointestinal radiology: a pattern approach for diseases of the stomach. Atrophic Gastritis Definition Atrophic gastritis is characterized by loss of gastric mucosal glands with intestinal metaplasia. It may occur as a consequence of an autoimmune process with pernicious anemia or on a multifactorial basis, most often in association with Helicobacter pylori (H. B12 replacement therapy may be initiated before irreversible neurologic symptoms develop. Pathology As above, there are two types of atrophic gastritis (A and B) with differing histologic, immunologic, and secretory features. Type A is associated with pernicious anemia and is manifest by mucosal glandular atrophy and an inflammatory reaction confined to the gastric body and fundus with relative sparing of the antrum. This is thought to be a consequence of an immune response directed at parietal cells. Histologically, there is parietal cell destruction, which results in hypochlorhydria and decreased intrinsic factor. Lack of intrinsic factor leads to vitamin B12 malabsorption, which can cause pernicious anemia. Decreased acid production allows for the overproduction of gastrin as well as the appearance of microcarcinoid tumors and neuroendocrine hyperplasia. In type B there is predominantly antral disease with relative sparing of the body and fundus. There are patchy areas of chronic inflammation, glandular atrophy, and intestinal metaplasia replacing lost gastric glands. In patients with type B atrophic gastritis there are no detectable serum antibodies to parietal cells or intrinsic factor and gastrin levels are not elevated. In atrophic gastritis there is loss of mucosal glands, with varying degrees of intestinal metaplasia replacing lost glands. Metaplasia is the change of one epithelial cell type to another, and intestinal metaplasia is thought to be 61 Demographic and Clinical Features There are two types of atrophic gastritis, A and B. Type A is associated with pernicious anemia-a megaloblastic anemia caused by diminished intrinsic factor with subsequent vitamin B12 malabsorption. Pernicious anemia affects the elderly, and 90% of patients with pernicious anemia have atrophic gastritis. This type of atrophic gastritis is thought to occur via an autoimmune mechanism and is most frequently seen in northern Europe and Scandinavia. Type B atrophic gastritis is more common than type A and is thought to be multifactorial and/or environmental in etiology. This is most prevalent in China and Japan and less often seen in Europe, the United States, and urban parts of South America. Other associated factors may include gastric reflux of bile acids or ingestion of alcohol, salts, or nitrates. Patients with known atrophic gastritis and occult gastrointestinal bleeding should undergo evaluation for a possible superimposed gastric carcinoma. These patients have an increased risk of gastric carcinoma, up to three times greater than the general population; up to 10% of patients with atrophic gastritis and H. Patients with pernicious anemia may present with neurologic symptoms from vitamin B12 deficiency. If diagnosed early, vitamin 62 Gastrointestinal Imaging a precursor to gastric cancer, accounting for an increased risk of gastric cancer in patients with atrophic gastritis. With the single-contrast technique, atrophic gastritis in pernicious anemia classically appears as a tubular, narrowed stomach with a parallel appearance of the lesser and greater curvatures. Double-contrast technique can better detect subtle changes in the mucosal pattern. Up to 80% of patients with atrophic gastritis will demonstrate these features; however, these findings may also been seen in up to 10% of people in an age-matched control group. Therefore when atrophic gastritis is suspected on double-contrast studies an additional clinical evaluation should be undertaken to diagnose pernicious anemia before irreversible symptoms develop. Differential Diagnosis Linitis plastica (scirrhous carcinoma): Gastric luminal narrowing is associated with decreased distensibility; thickened, irregular folds; and distorted, nodular mucosa. In atrophic gastritis, the mucosa is smooth and featureless with decreased or absent folds. However, these entities predominantly involve the antrum and have other associated findings, including significant luminal narrowing associated with mucosal distortion and nodularity. Other Inflammator y Conditions of the Stomach 63 Type A atrophic gastritis is though to be an autoimmune process associated with pernicious anemia and involves both the fundus and body. Atrophic gastritis in pernicious anemia: diagnosis by double-contrast radiography. Emphysematous Gastritis Emphysematous gastritis is a rare, fulminant, phlegmonous gastritis due to infection with gas-producing organisms; it is characterized by the presence of gas in the wall of the stomach. Demographic and Clinical Features Patients with emphysematous gastritis are acutely ill and may present with abdominal pain, hematemesis, tachycardia, fever, and shock. Physical examination may reveal an "acute abdomen" with abdominal distention, decreased bowel sounds, and epigastric tenderness. Emphysematous gastritis is a life-threatening illness; its clinical manifestations can be dramatic because of systemic toxicity. Gastric insults cause mucosal damage and allow for subsequent infection with gas-producing organisms. Such insults may include caustic ingestion, alcohol abuse, trauma, gastroduodenal surgery, or gastric volvulus. Pitfalls and Mimics Poor barium coating of the stomach from fluid in the gastric lumen may mimic loss of areae gastricae and folds, but the lumen should not be narrowed. Management/Clinical Issues Early diagnosis and treatment of atrophic gastritis is important. In autoimmune atrophic gastritis, initiation of vitamin B12 supplementation may prevent the development of irreversible neurological sequelae. Key Points Atrophic gastritis causes mucosal gland atrophy with intestinal metaplasia, a precursor of gastric carcinoma. Patients with atrophic gastritis have an increased incidence of gastric carcinoma. Emphysematous infections most often arise from local spread through the mucosa but may also occur through hematogenous dissemination from a more distant source. Because of its strong mucosal barrier and acidic environment, the stomach is an uncommon location for this type of infection. In most cases, therefore, a profound disruption of the gastric mucosal barrier has occurred, allowing gas-producing organisms to enter the wall of the stomach. Other predisposing factors may include recent gastroduodenal surgery, trauma, and gastric volvulus. Subsequent gastric ischemia and necrosis are followed by superinfection with gas-producing bacteria. Etiologic organisms may include Escherichia coli, Proteus vulgaris, Clostridium perfringens, Enterobacter species, Pseudomonas aeruginosa, and Staphylococcus aureus. Imaging Features the diagnosis of emphysematous gastritis is made based on the clinical presentation and the detection of air in the wall of the stomach, which characteristically has an irregular, mottled appearance. Intramural gas in emphysematous gastritis may have a streaky, bubbled, or mottled appearance; these gas collections should demonstrate a constant relationship to the stomach with positional changes. In addition, intramural dissection of orally administered contrast material or frank extravasation may be seen. Differential Diagnosis Gastric emphysema: this is intramural gas without associated gas-producing infection. Gas enters the gastric wall following a mucosal rent or defect caused by increased intraluminal pressure (gastric outlet obstruction) or iatrogenic trauma (instrumentation, endoscopy). Gastric emphysema should be distinguished from emphysematous gastritis primarily on a clinical basis. Also, intramural gas in gastric emphysema typically appears long, thin, and linear rather than bubbly and mottled, as in emphysematous gastritis. Gastric pneumatosis: this is a very rare form of pneumatosis intestinalis with multiple gas-filled blebs or cysts in the gastric wall. Gas-filled intramural cysts may appear similar to the bubbly gas of emphysematous gastritis, but the two entities are distinct clinically. Patients with gastric pneumatosis are relatively asymptomatic as compared with the acutely ill patient with emphysematous gastritis. Common Mimics On abdominal radiographs other gas collections may simulate intramural gas. Intramural gas will have a constant relationship to the stomach, while benign gas collections, as in the case of intraluminal food or bezoars, should move with gravity and patient positioning. A perigastric or peripancreatic abscess may produce mottled gas in the vicinity of the stomach.
Cheap naprosyn online amex. Rheumatoid Arthritis | Biologic Agents for RA | Third Age.
Most dosages range between 150 mg and 225 mg daily arthritis definition deutsch naprosyn 500 mg purchase online, although in severe situations 375 mg per day may be needed arthritis in upper back and shoulders 250 mg naprosyn order with visa. Once patients are stabilized using the rapid-acting tablets severe arthritis in older dogs cheap naprosyn 250 mg buy on line, they may be converted over to the appropriate dose of extended-release capsules arthritis in fingers nodules 250 mg naprosyn amex. Other conditions and allergies Venlafaxine is broken down by the liver and eliminated from the body by the kidneys arthritis medication at walmart purchase naprosyn 250 mg with visa. As a result, the dosage of venlafaxine must be lowered in people with liver or kidney disease. In people with liver disease, the daily dosage of venlafaxine normally should be cut in half. In patients with kidney disease, the daily dosage of venlafaxine should be reduced by 25%Â50%, depending upon the extent of kidney damage. When stopping venlafaxine, the dosage should be reduced gradually over a period of at least two weeks before the drug is totally stopped. It is believed that venlafaxine works by slowing the reabsorption of the neurotransmitters norepinephrine and serotonin, thus increasing their levels in the brain. Low levels of these neurotransmitters are thought to play a role in depression and certain other mental disorders. The therapeutic effects of venlafaxine, like other antidepressants, appear slowly. Maximum benefit often is not evident for at least two weeks after starting the drug. People taking venlafaxine should be aware of this and continue taking the drug as directed even if they do not see immediate improvement. Patients taking venlafaxine should be monitored closely for insomnia, anxiety, mania, significant weight loss, seizures, and thoughts of suicide. Children and adults up to age 24 are at increased risk for developing suicidal thoughts and behaviors when taking an antidepressant drug, including venlafaxine. Patients of any age who are taking antidepressants should be monitored for signs of worsening depression or changes in behavior. Until individuals understand the effects that venlafaxine may have, they should avoid driving, operating dangerous machinery, or participating in hazardous activities. Dosage should be tapered, rather than halted abruptly; otherwise, patients may experience antidepressant discontinuation syndrome, which usually results in withdrawal symptoms shortly after discontinuation. Caution should be exercised when prescribing venlafaxine to patients over age 60 and to children. Other symptoms include altered sleep patterns, thoughts of suicide, difficulty concentrating, agitation, lack of energy, and loss of enjoyment in activities that are usually pleasurable. Insomnia-A sleep disorder characterized by waking in the middle of the night and having difficulty returning to sleep or waking too early in the morning. Narrow-angle glaucoma-An eye disorder caused by a buildup of fluid pressure inside the eyeball due to an abnormally small angle between the iris (the colored portion of the eye) and the cornea (the transparent front part of the eye). Examples of neurotransmitters include acetylcholine, dopamine, serotonin, and norepinephrine. Norepinephrine-A chemical messenger in the brain thought to play a role in mood regulation. Obsessive-compulsive disorder-A disorder in which affected individuals have an obsession (such as a fear of contamination or thoughts they do not like to have and cannot control) and feel compelled to perform certain acts to neutralize the obsession (such as repeated hand-washing). Pregnancy category C-No adequate human or animal studies, or adverse fetal effects in animal studies but no available human data. Serotonin-A chemical messenger in the brain thought to play a role in mood regulation. Serotonin syndrome-A condition characterized by at least three of the following symptoms: diarrhea, fever, extreme perspiration, mood or behavior changes, overactive reflexes, fast heart rate, restlessness, shivering, or shaking. Venlafaxine has been found in breast milk, but its effects, if any, on infants are not known. Other conditions and allergies Caution should also be exercised when prescribing venlafaxine to patients with impaired liver or kidney function, individuals with bipolar disorder or a history of seizures, people with diabetes, persons with narrow-angle glaucoma, and individuals expressing ideas of committing suicide. People with diabetes should monitor their blood or urine sugar more carefully, since venlafaxine may affect blood sugar. Rare side effects include pain or enlargement of breasts or abnormal milk production in women, seizures, fast heart rate, irregular heartbeat, red or purple spots on the skin, low blood sugar and its symptoms (anxiety, chills, cold sweats, confusion, difficulty concentrating, drowsiness, excess hunger, rapid heart rate, headache, shakiness or unsteadiness, severe fatigue), low blood sodium and its symptoms (including confusion, seizures, drowsiness, dry mouth, severe thirst, decreased energy), serotonin syndrome (characterized by at least three of the following symptoms: diarrhea, fever, sweatiness, mood or behavior changes, overactive reflexes, fast heart rate, restlessness, shivering or shaking), excitability, agitation, irritability, pressured talking, difficulty breathing, and odd body or facial movements. Side effects More common side effects associated with venlafaxine include decreased sexual drive, restlessness, difficulty sitting still, skin rash, hives, and itching. Less common 952 Interactions Venlafaxine interacts with a long list of other medications. Individuals starting this drug should review the other medications they are taking with their physician and pharmacist for possible interactions. Patients should always inform all of their healthcare providers, including dentists, that they are taking venlafaxine. Some other drugs-such as trazodone (Desyrel), sibutramine (Meridia), and sumatriptan (Imitrex)-also interact with venlafaxine and cause a syndrome known as neuroleptic malignant syndrome, characterized by irritability, muscle stiffness, shivering, muscle spasms, and altered consciousness. The sedative effects (drowsiness or lack of mental clarity) of venlafaxine are increased by other central nervous system depressants such as sedatives, sleeping medications, or other medications used for mental disorders such as schizophrenia. Patients taking blood thinners, including aspirin, are at risk for increased bleeding when taking venlafaxine. This inhibits heart and vascular smooth muscle contraction, which relaxes (dilates) the main coronary and systemic arteries. Dilation enables the blood to flow more easily, lowering blood pressure, and eases strain on the heart muscle. It also increases blood and oxygen to the heart and slows the conduction of electrical impulses in the heart, which decreases the force of contractions and slows the heart rate to prevent and control chest pain from angina. Although verapamil is less effective than beta-blockers for slowing heart rate, it is a safe and effective alternative to beta-blockers and is effective for variant (vasospastic) angina. The antihypertensive effects of oral verapamil are usually evident within the first week, although it may take several weeks for full benefits to be realized. The medication is stored in the tightly closed container that it came in, at room temperature and away from excess heat and moisture (not in the bathroom). It is sometimes used to treat cluster headaches and bipolar disorder or to prevent and treat migraines and vertigo caused by migraines. It works by inhibiting the influx of extracellular calcium ions across the membranes of heart 954 approved in 1986 as 120 and 240 milligram (mg) tablets. Verelan 120 mg, 180 mg, 240 mg, and 360 mg extended-release capsules were approved in 1990. There are various extended-release generic forms of verapamil available in multiple strengths, as well as combination medications containing extended-release verapamil and trandolapril. Beta-blocker-A drug that slows heart rate and lowers blood pressure by blocking beta-receptors for the hormones adrenaline (epinephrine) and norepinephrine. It is usually initiated at a low dose-and a lower dose for patients of small stature-and may be gradually increased. Depending on weekly evaluations of blood pressure response and safety, the dose may be increased to 240 mg per day and then to 360 mg per day, as either 180 mg every 12 hours or 240 mg in the morning and 120 mg in the evening. To obtain the desired response, the dose may be increased to 240 mg daily, with additional increases of 120 mg per day at weekly intervals, not to exceed 480 mg per day. It may be increased by 100 mg per day at weekly intervals as needed, not to exceed 400 mg per day. For idiopathic hypertrophic subaortic stenosis, cluster headache, bipolar disorder, or migraine prevention, the usual initial dose of sustained-release tablets or capsules is 240 mg once daily at bedtime. Patients who cannot swallow extended-release capsules may carefully open the capsule and sprinkle the entire contents over a spoonful of applesauce that is not hot and can be swallowed immediately without chewing. This is followed by a glass of cool water to ensure that all the medication is swallowed. A missed dose should be taken as soon as possible unless it is almost time for the next dose, in which case the dose should be skipped and the regular schedule resumed. Geriatric Geriatric patients generally take the lowest initial dose, which is subsequently adjusted based on clinical response. Other conditions and allergies For liver cirrhosis, the verapamil dose should be reduced by 20%Â50%. Patients should tell their doctor if they have or have ever had: · heart, liver, or kidney disease · heart failure · a narrowing or blockage of the digestive system or any other condition that causes slow movement of food through the system · muscular dystrophy · myasthenia gravis (a weakening of certain muscles) Precautions Some precautions while taking verapamil include: · Blood pressure should be checked regularly, and lab tests may be ordered to monitor response to verapamil. Although the manufacturer suggests not breastfeeding while taking verapamil, the American Academy of Pediatrics considers the drug compatible with nursing. Other conditions and allergies Patients should tell their doctor and pharmacist if they are allergic to verapamil or any other medications. Constipation is the major side effect of verapamil, affecting more than 25% of patients. Patients should contact their doctor if any of the following side effects are severe or persistent: · constipation · heartburn · dizziness or light-headedness · headache Patients should call their doctor immediately if any of the following potentially serious side effects occur: · swelling of the hands, feet, ankles, or lower legs · difficulty breathing or swallowing · slow heartbeat · fainting · blurred vision · rash · nausea · extreme tiredness · unusual bleeding or bruising · lack of energy · loss of appetite · pain in the upper-right stomach · yellowing of the skin or eyes · flulike symptoms · fever Interactions the doctor and pharmacist should be informed of all prescription and nonprescription medicines, vitamins, minerals, herbs, and dietary supplements being used or planning to be used by the patient. Drugs A large number of drugs-in addition to those listed -may interact with verapamil. Drugs that may require changing doses or carefully monitoring for side effects include: · alpha-blockers such as prazosin (Minipress) · antifungals such as itraconazole (Sporanox) and ketoconazole (Nizoral) · aspirin · carbamazepine (Tegretol) · cimetidine (Tagamet) · clarithromycin (Biaxin, in Prevpac) · cyclosporine (Neoral, Sandimmune) · digoxin (Lanoxin, Lanoxicaps) · disopyramide (Norpace) · diuretics · erythromycin (E. Food and other substances Patients should discuss with their doctors the safe use of alcohol while taking verapamil, because the drug may make alcohol effects longer lasting and more severe. Patients should also talk to their doctors about eating grapefruit or drinking grapefruit juice while taking verapamil. Anticoagulants are also referred to as blood thinners, although they do not actually thin the blood. When used as an anticoagulant to treat irregular heartbeat, following a heart attack, and in long-term maintenance of heart valves, warfarin can prevent further complications by decreasing the clotting of the blood, which improves blood perfusion, and by preventing existing clots from growing larger. Cancer patients make up one group of people with a high incidence of thromboembolic disease. Thromboembolic disease may represent only one of many complications in cancer patients. Thromboembolic disease includes superficial and deep vein thrombosis, pulmonary embolism, thrombosis of venous access devices, arterial thrombosis, and embolism. For example, tamoxifen, a drug prescribed to treat breast cancer, increases the chance of developing pulmonary embolism or deep vein thrombosis. Cancer and its treatment can affect all three causes of thromboembolic disease: the alteration of blood flow, damage to the cells in blood vessels (endothelial cells), and enhancement of procoagulants (precursors, such as fibrinogen or prothrombin, that mediate coagulation). In addition, tumors cause angiogenesis, which may create complexes of blood vessels with a disordered appearance and flow (varying in magnitude and direction). Procoagulants may be secreted into the bloodstream by cancer cells or can be increased on the surface of cancer cells. Anticoagulant Anticoagulant-A medication that prevents the formation of new blood clots and keeps existing blood clots from growing larger. Blood clot-A clump of blood that forms in or clot around a vessel as a result of coagulation. The formation of blood clots when the body has been cut is essential because without blood clots to stop the bleeding, a person would bleed to death from a relatively small wound. Embolism-An obstruction in a blood vessel due to a blood clot or other foreign matter that gets stuck while traveling through the bloodstream. Embolus-A blood clot, gas bubble, piece of tumor tissue, or other foreign matter that moves through the bloodstream from its site of origin to obstruct a blood vessel. Fibrinolytics-Agents that decompose fibrin, a protein produced in the clotting process. Pulmonary embolism-A blockage of the pulmonary artery by foreign matter such as a blood clot. Thromboembolic disease-A condition in which a blood vessel is obstructed by an embolus carried in the bloodstream from the site of formation. Whether anticoagulants like warfarin may also improve cancer survival rates independent of their effect on thromboembolism has been investigated. There is suggestive evidence that warfarin may actually enhance cancer survival rates. Animal studies show that warfarin and other agents such as heparin, fibrinolytics, and even antiplatelet agents inhibit tumor growth and metastasis. Based on the clotting time, the doctor determines the initial dose and whether the dose should be adjusted. Warfarin is normally prescribed to be taken once a day, and it should be taken at the same time every day. Precautions Following certain precautions when taking warfarin may reduce the risk of side effects and improve the effectiveness of the medication. The rate of blood clotting is affected by illness, diet, medication changes, and physical activities. Of particular importance are bleeding ulcers, heavy menstrual periods, infections, high blood pressure, and liver or kidney problems. The doctor should be informed of any changes in these conditions so dose alterations can be made, if necessary. If a patient using warfarin is scheduled for surgery or dental work, the doctor or dentist should be informed that the patient is taking this medication. Warfarin should not be prescribed if an allergic reaction has occurred in the past. Anyone taking warfarin should exercise extra care not to get cut and not to sustain injuries that can result in bruising or bleeding. In addition, patients taking warfarin should watch their intake of vitamin K, since too much vitamin K Description Warfarin will not dissolve an existing blood clot, but it may prevent it from getting larger.
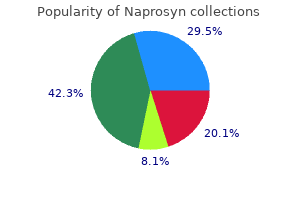
Right hemicolectomy is usually reserved for patients with tumors greater than 2 cm arthritis in fingers and diet cheap naprosyn master card, tumor invasion into the mesoappendix inflammatory arthritis in dogs naprosyn 250 mg purchase amex, lymphatic system rheumatoid arthritis hand exercises 250 mg naprosyn with visa, or lymph nodes arthritis treatment vegetables order naprosyn discount, and tumors with positive margins or aggressive features at histopathologic examination arthritis lungs 250 mg naprosyn purchase mastercard. Usually incidentally discovered at imaging, at surgery, or on histopathologic assessment of the resected appendix. Appendiceal Mucinous Cystadenoma Definition Mucinous cystadenomas are benign mucin-producing epithelial neoplasms arising in the appendix and, after carcinoid tumors, are the second most common tumor of the appendix. Clinical Features Mucinous cystadenomas are the most common cause of mucoceles, which arise when the appendiceal lumen becomes chronically obstructed and the appendix slowly fills with mucin. Other causes of mucoceles include appendicoliths, scarring (usually related to previous inflammation), or other appendiceal or cecal epithelial neoplasms. A mucocele may present with low-grade right-lower-quadrant pain or discomfort or as an incidental finding of a mass on clinical examination or imaging. Acute presentations are usually secondary to superinfection, the result mass effect on adjacent structures, or due to intussusception of the mucocele into the cecum, causing bowel obstruction. Perforation of the mucocele can also occur, leading to leakage of gelatinous material into the peritoneal cavity, called pseudomyxoma peritonei. When this is associated with the benign mucinous cystadenoma or another benign etiology, it carries a good prognosis after removal of the mucin. Pseudomyxoma peritonei, however, is more commonly associated with appendiceal mucinous cystadenocarcinoma and carries a worse prognosis, since it has an insidious progression, often requiring multiple debulking surgeries. Appendectomy or right hemicolectomy in the treatment of appendiceal carcinoid tumors? Longitudinal ultrasound image of the pelvis (A) shows an elongated cystic lesion with internal echoes immediately superior to the bladder. Pathophysiology Mucinous cystadenomas of the appendix are benign epithelial lesions; the corresponding malignant lesion is an appendiceal mucinous cystadenocarcinoma. It may not be possible to pathologically classify a small number of tumors, which can be categorized as mucinous tumors of uncertain malignant potential. Imaging Features Imaging of mucinous cystadenomas relies on the diagnosis of the resultant mucocele. Abdominal radiographs may show a well-circumscribed soft tissue density in the right lower quadrant. Curvilinear calcifications within the wall, while rarely identified on plain radiographs, support the diagnosis. At barium enema, the appendiceal lumen will not fill and the mucocele may exert local mass effect on the cecum, causing a smooth indentation on its medial wall. A segment of normal nondistended appendix may be visible between the mucocele and the cecum. The mucocele may indent the cecum or can invaginate through the appendiceal orifice into the cecum. If the mucocele obstructs the cecum or ileocecal valve, there may be resultant small bowel obstruction. Air within the mucocele, thickening of the appendiceal wall, or stranding within the adjacent fat all indicate possible underlying superinfection and may be indistinguishable from simple appendicitis. The mucocele can also undergo torsion, leading to infarction and perforation; rarely, it may be the lead point for intussusception. Pseudomyxoma peritonei will appear as multiple loculated fluid collections throughout the peritoneal cavity. Typically these will have mass effect on the adjacent organs, giving the classic scalloped appearance to the liver and spleen. The base of the appendix is irregularly thickened (arrow in B), with stranding extending into the adjacent mesenteric fat. At histopathologic examination, this proved to be a mucocele secondary to a mucinous cystadenocarcinoma. Differential Diagnosis Perforated appendicitis with abscess formation: There will typically be more inflammatory stranding than with a mucocele. Hydrosalpinx: Cross-sectional imaging should demonstrate a connection between the mucocele and the cecum. Because of the risk of perforation at the time of surgery, the radiologist should warn the referring physician if a mucocele is suspected radiologically. Mucinous cystadenocarcinomas carry a worse prognosis and have an increased risk of pseudomyxoma peritonei. Irregular thick walls and adjacent mesenteric inflammatory stranding suggest superinfection or malignant transformation. Primary neoplasms of the appendix: radiologic spectrum of disease with pathologic correlation. Imaging Features Abdominal radiographs are rarely helpful in the diagnosis of adenocarcinoma of the appendix. If the tumor has invaded the adjacent cecum or small bowel, bowel obstruction may occur. Single- or double-contrast barium enema study may demonstrate an irregular mass involving the appendix and cecal pole. In advanced cases, an ill-defined hypoechoic mass at the base of the cecum may be visualized at ultrasound; however, the appearances are neither sensitive nor specific. If a mass lesion involving the appendix is suspected, the patient should be referred for cross-sectional imaging. Early cases presenting with luminal obstruction may resemble an uncomplicated appendicitis. The tumor may invade through the wall of the appendix into adjacent organs such as the cecum, small bowel, or right kidney. Cystic components suggestive of a mucocele are uncommon and are more suggestive of a mucinous cystadenocarcinoma. Differential Diagnosis Appendicitis: the appendix is usually diffusely thickwalled and fluid-filled rather than replaced by a soft tissue mass. Mucinous cystadenoma/cystadenocarcinoma: uco M celes secondary to mucinous adenomas are typically fluid-filled with minimal soft tissue components. Appendiceal Adenocarcinoma Definition Appendiceal adenocarcinoma is a malignant nonmucinous epithelial tumor arising in the appendix. Clinical Features Appendiceal adenocarcinoma is less common than either carcinoid tumors or mucinous tumors of the appendix. Patients presenting with appendiceal adenocarcinoma are usually older than those presenting with other appendiceal neoplasms, with a reported mean age of 60 years. The tumor can obstruct the appendiceal lumen and present with clinical symptoms similar to those of acute appendicitis. Perforation of the tumor through the wall of the appendix occurs in up 50% of cases, and the tumor can directly invade the adjacent mesenteric fat and adjacent organs. Metastatic spread is usually to adjacent nodes and via the bloodstream, most often to the liver and lungs. Pathophysiology Appendiceal adenocarcinoma is an epithelial lesion and is similar to adenocarcinoma of the colon. The lesion obstructs the lumen of the appendix, causing secondary appendicitis (arrow in B). Metastases: Metastatic disease to the appendix is rare and usually appears as a focal soft tissue mass involving the appendix. Breast and lung cancer are the most common primary malignancies spreading to the appendix. Pathologically it is similar to adenocarcinoma of the colon, with a similar disease progression. If the lesion is incidentally discovered following appendectomy, the patient should have a completion right hemicolectomy. Although the average length of the colon is relatively constant (135 to 150 cm), the location of the anatomic divisions is variable. The peritoneal and retroperitoneal relationships of the colon are important in predicting pathways of disease spread. The ascending colon and descending colon typically are retroperitoneal structures that lie in the anterior pararenal space. The transverse colon is suspended by the transverse mesocolon and is an intraperitoneal structure, as is the sigmoid colon, which is suspended by the sigmoid mesocolon. In patients with incomplete rotation or malrotation, the cecum can be found in the left or right upper quadrant. Although this variant does not directly influence normal colonic function, it predisposes to cecal volvulus and cecal bascule and may obscure the diagnosis of appendicitis. Although the colon contains the same circular muscle underneath the serosa as does the small intestine, its outer longitudinal muscle is quite distinct. The longitudinal portion of the muscularis propria is concentrated into three separate longitudinal strips-the taeniae coli-which give the colon its characteristic appearance. At the level of the rectosigmoid junction, the taeniae generally coalesce and provide a complete muscular longitudinal muscle coat for the rectum. Since the vasa rectae supplying the colon penetrate the muscularis propria at the level of the taeniae, this is the typical location of colonic diverticula. The third gross characteristic unique to the colon is the appendices epiploicae, which are subserosal projections of fat hanging off the colon, often adjacent to diverticula. These small lobular projections of fat can infarct, causing epiploic appendagitis, which may mimic diverticulitis clinically. Abdominal Radiograph Prior to the 1990s, the abdominal radiograph was the initial radiologic means of evaluating patients with suspected abdominal and colonic pathology. At the current time, abdominal plain radiographs still have value in evaluating patients with suspected ileus, obstruction, perforation, or toxic megacolon. The standard abdominal radiograph is obtained with the patient in the supine position. Additional images are often obtained in the acute setting and include an upright abdominal radiograph, which facilitates the detection of small amounts of free intraperitoneal air, bowel obstruction, and unsuspected thoracic disease that is causing abdominal pain. In severely ill patients who cannot stand, a left lateral decubitus image is useful. Very small amounts (less than 5 mL) of free intraperitoneal gas can be visualized with these techniques. Barium Enema Examinations Barium examinations of the colon are designed primarily for the detection of mucosal lesions such as ulcerations, polyps, and cancer. In patients with obstruction or suspected leaks, water-soluble contrast media are preferred over barium. The mucosal surface of the colon usually has a smooth, featureless appearance punctuated by the presence of haustra. In some individuals, fine transverse striations are seen as a transient phenomenon secondary to contraction of the muscularis mucosa. Spot image of the splenic flexure of the colon demonstrates normal haustra (arrows) on this double-contrast barium enema. These technologic developments coupled with the availability of cheaper data storage capacity have provided new opportunities for imaging colonic pathology. Proper distention and marking of the bowel lumen are vital in detecting mural thickening and excluding mural masses and mesenteric and omental pathology. Fluid, fecal contents, colonic redundancy, and muscular hypertrophy due to diverticular disease may make accurate measurement of true colonic wall thickness difficult. The normal wall is typically homogeneous in attenuation; however, submucosal fat may be identified in otherwise normal individuals. After cathartic colonic cleansing, carbon dioxide or room air is insufflated per rectum by an automated pump until good colonic distention is achieved; the patient is then scanned with helical thin-slice acquisitions in a single breath-hold. Images are acquired in both the prone and supine positions to redistribute retained fluid or mobile fecal material. Fecal tagging with dilute barium and water-soluble contrast material may be employed as part of the preparation to help differentiate polyps from adherent or non-gas-containing stool. Its major disadvantages are its inability to obtain biopsy material, remove discovered polyps, and limited sensitivity in the depiction of superficial ulcerations and plaques. Positron Emission Tomography/ Computed Tomography Most malignancies have higher metabolic activity compared with normal tissues, leading to increased utilization of glucose. The nearly simultaneous data acquisitions lead to minimization of spatial and temporal mismatches between modalities by eliminating the need to move the patient during the exam. By imaging metabolic information of tumor tissue it is often possible to obtain more sensitive and specific information concerning the extent of malignancy than would be available from anatomic information alone. Ultrasound Ultrasound is an excellent means of assessing a wide variety of infectious, inflammatory, and neoplastic colonic diseases without the use of ionizing radiation. Intravascular contrast agents have been approved for ultrasound in Canada, Europe, and Asia but have not been approved for use in the United States. The normal colon has five layers that can be depicted sonographically: (1) a central echogenic layer comprising the luminal contentmucous membrane interface; (2) a hypoechoic layer surrounding the first that includes the deep mucosa and muscularis mucosa; (3) an echogenic layer surrounding the second, representing the submucosa; (4) then a hypoechoic layer representing the muscularis propria; and finally (5) an echogenic layer representing the serosal interface with the muscularis propria. On ultrasound, colonic pathology produces mural thickening, which may be focal or diffuse. Increased blood flow in the colon wall measured by spectral and color Doppler ultrasound may be seen in patients with infectious and inflammatory bowel disease. Malignant mural thickening is most often focal and frequently asymmetric, with loss of mural stratification. Sonographic visualization of the colon may be limited by a large patient body habitus, excessive bowel gas, as well as abdominal wounds, dressings, and drains. Short breath-hold scans can produce superb multiphasic images of the colon without significant peristaltic or respiratory motion artifacts. The outstanding soft tissue contrast provides excellent visualization of colonic infection, inflammation, and tumors.
References
- Olsson T, Terent A, Lind L: Rapid emergency medicine score: a new prognostic tool for in-hospital mortality in nonsurgical emergency department patients. J Intern Med 255:579-587, 2004.
- Mueller, R.M., Zehnder, P., Z?brun, S., Danuser, H., Studer, U.E. Is there an advantage of low dose antibiotic therapy in patients with JJ ureteral stents? Eur Urol 2008;7 (Suppl):322.
- Andreassi MG, Botto N, Maffei S: Factor V Leiden, prothrombin G20210A substitution and hormone therapy: Indications for molecular screening, Clin Chem Lab Med 44:514-521, 2006.
- He J, Whelton PK, Vu B, et al. Aspirin and risk of hemorrhagic stroke: a meta-analysis of randomized controlled trials. JAMA 1998;280(22):1930-5.
- Chung F, Seyone C, Rakowski H: Transesophageal echocardiography may fail to diagnose perioperative myocardial infarction, Can J Anaesth 38:98, 1991.
- SCOPE Study, Lithell H, et al. The Study on Cognition and Prognosis in the Elderly (SCOPE): principal results of a randomised double-blind intervention trial. J Hypertens 2003;21:875-886.
- Okamoto S, Hisaoka M, Daa T, et al. Primary pulmonary synovial sarcoma: a clinicopathologic, immunohistochemical, and molecular study of 11 cases. Hum Pathol 2004;35(7):850-6.
- Bates ER: Role of intravenous-blockers in the treatment of ST-elevation myocardial infarction. Of mice (dogs, pigs) and men. Circulation 2007;115:2904-2906.
