
Omeprazole
| Contato
Página Inicial
Evelyn Mai, MD
- Whitney Sleep Center, Plymouth, MN, USA
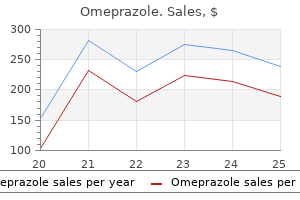
Fibers with low and medium spontaneous rates have thin dendrites that terminate on the side of the inner hair cell facing the modiolus juice diet gastritis buy 10 mg omeprazole visa. In other words gastritis migraine order omeprazole 10 mg without a prescription, spontaneous activity of nerve fibers is not random but is proving to be anatomically and functionally significant (13-16) gastritis symptoms breathing cheap omeprazole 20 mg on line. The tuning curve of a single auditory nerve fiber is perhaps the most basic measure of auditory nerve function gastritis zwieback generic omeprazole 40 mg buy line. The level is adjusted until a criterion change (one or two spikes per second) in firing rate is detected gastritis diet breakfast order cheap omeprazole on line. Tone bursts covering a wide range of frequencies are used, and the lowest level of signal is recorded for a given frequency that produces a specific rate of discharge. Units with low characteristic frequency innervate inner hair cells in the apical region of the cochlea. Thning curves are described according to the frequency of the tip or characteristic frequency. Fibers with a higher characteristic frequency have an obvious tip at the characteristic frequency and a tail that extends to the low frequencies. The high side of a tuning curve is the frequency region greater than the characteristic frequency. As characteristic frequency increases, the high side of the tuning curve becomes steeper with a slope or rejection rate that can exceed 500 dB per octave. Fiber numbers given In sequence during 1he experiment are at the tips of the curves. Tuning and suppnasslon In auditory nerve fibers of aged gerbils raised In quiet or noise. The high-frequency side no longer has a steep slope, and the low-frequency side becomes slightly more sensitive, or hypmensitive. The characteristic frequency of the fiber appealS to be much lower in frequency, and the band width of the fiber appecu:s broader. A threshold shift of approximately 30 dB occw:s, but a short, sharply tuned tip remains, and the low-frequency tail is again hypmensitive. Irregularities in this tuning auve may explain monaural displacusis; that is, a tone in one ear (800 Hz) has two pitches, for example, one at 800 Hz and a second at approximately 2. The threshold of the unit is elevated approximately 30 dB, but the tuning curve is approximately normal. Although thresholds of auditory nerve fibers are related to the rate of spontaneous di. One way is with low-spontaneous fibers; another is recruitment offibers of characteristic frequency. Diversity of charac· teristlc frequency rate-Intensity functions In guinea pig auditory nerve fibers. In the case of sensorineural hearing loss, the tips of the tuning cwves are missing. Perhaps the most studied nonlinearities are combination tones, described herein in relation to cochlear emissions, and two-tone rate suppression, as recorded in auditory nerve fibers. Two-tone rate suppression is the reduction in firing rate produced by one tone when a second tone is introduced. Tones presented in the dotted or suppression areas in the figure reduce the firing rate caused by the probe tone. Both the excitor and suppressor tones are presented simultaneously, and because little or no time lag is associated with this phenomenon nor is any evidence available that it is neurally produced, the effect is called suppre. Two-tone suppression in single units is reflected in the compound action potential. In this case, the amplitude of the compound action potential is altered by the suppressing signal, whereas in the singleunit case (left), the firing rate of a neuron is reduced by an a! In the presence of sensorineural hearing loss caused by exposure to noise or to ototoxic drugs, two-tone rate suppression is sarerely affected. Tones pre9ented in the suppression areas deaea9e the firing rate to the excitatory tone. The most prominent of all these intermodulation distortion products is the cubic distortion tone, 2F1-F2. Five major cell types are found within the cochlear nucleus, each with distinct morphologic and physiologic features, such as response to stimulus onset, stimulus offset, and frequency modulation. From the cochlear nucleus, most fibers cross the brainstem to the contralateral superior olivary complex; a much smaller number of fibers run to the ipsilateral superior olivary complex. The superior olivary complex is considered the first center in the ascending auditory system, where inputs from both ears converge. Auditory nuclei above the superior olivary complex can be excitatory or inhibitory with inputs from each ear. Although many functions have been attributed to the efferent auditory system, especially protecting the cochlea from loud sounds, the functions of the system are unknown; those that have been proposed are easily debated (26,27). The inferior colliculus is a complex nucleus with at least 18 major cell types and at least five areas of specialization. It is involved in probably all forms of auditory behavior, including differential sensitivity for frequency and intensity, loudness, and binaural hearing. The medial geniculate body of the thalamus sends projections to the auditory cortex. The auditory cortex is located in the sylvian fissure of the temporal lobe; many secondary auditory areas are clustered around the primary area. The cells in one column can have different tuning at a similar characteristic frequency, whereas another column can be associated with intensity encoding, another with providing inhibitory responses to stimulation of one ear and excitatory responses of the other ear, and so on. As is common for thalamic connections with the cortex, nuclei within the medial geniculate body that send fibers to the auditory cortex also receive fibers from the same area of the cortex. Bilateral lesions of the temporal lobe have been shown to produce wide-ranging effects (cortical deafness, in which several auditory behaviors are severely affected, including speech discrimination, localization of sound, temporal processing of information, and the detection of faint, short-duration signals) (28). Each place on the basilar membrane responds best to a specific frequencyhigh-frequency sounds are localized to the base, and lowfrequency sounds, to the apex. The:field of clinical objective audiometty has recendy gained an additional technique in the auditoty evoked response battery. Processing of neural information probably involves both parallel and serial processing. Serial processing involves a fiber going to one target, which in tum goes to another taiget, and so forth. The combined effect of the acoustic properties of the head, atemal e~ and middle eat and the input impedance of the cochlea determine the frequency range of human hearing. The scalae tympani and vestibuli contain perilymph and are connected through the helicotrema at the apex: of the cochlea. Deflection of stereocilia (hairs) of the sensory cells by a mechanical traveling wave starts transduction. The traveling wave has a sharply tuned peak at the base for high-frequency sound that progresses toward the apex: as frequency decreases. The potassium flux arises from the +80 mV endocochlear potential added to the negative intracellular potential of inner and outer hair cells. The resulting depolarization causes an enzyme cascade that releases chemical transmitters and activates afferent nerve fibers. Approximately 1,800 efferent fibers project to the sensory cells from the ipsilateral and contralateral superior olivary complexes. Tuning curves of single fibers of the nerve are strikingly similar to tuning curves of the mechanical traveling wave. Injury to sensory cells and stereocilia alters the features of tuning curves, including sensitivity and sharp tuning. These properties allow the inner ear to respond to a wide range of intensities and provide the basis for suppression phenomena. It may have a role in the cochlear transduction and in protecting the cochlea from overexposure to intense sound. Cholinergic and purinergic neurohumoral signaling in the inner ear: a molecular physiological analysis. Onset of cholinergic efferent synaptic function in sensory hair cells of the rat cochlea. Afferent and efferent innervation of the cat cochlea: quantitative analysis with light and electron microscopy. Thning and suppression in auditory nerve fibers of aged gerbils raised in quiet or noise. Probst R Otoacoustic emissions: new aspects of cochlear mechanics and inner ear pathophysiology. The olivocochlear efkrent bundle and susceptibility of the inner ear to acoustic injury. Steady state evoked potential and behavioral hearing thresholds in a group of children 2273 33. Swanepoel D, Hugo R, Roode R Auditoiy steady state responses for children with severe to profound hearing loss. Establishing normal hearing with the dichotic multiple-frequency auditory steady state response wmpared with auditory brainstem response protocol. Using multistimuls suditory steady-state responses to predict hearing thresholds in high risk infants. Antonelli New techniques and strategies for assessment of the audit01y function in adults have been introduced in recent years. Puretone audiometry, immittance measurement (tympanometry and acoustic reflexes), and calwlation of word recognition scores continue to be important for hearing assessment. Clinical audiology, however; now also includes other behavioral and electrophysiologic test procedures. This article summarizes current techniques and strategies for hearing assessment among adults. The emphasis is on use of a test batteey that maximizes diagnostic accuracy and efficiency and minimizes test time and cost. A glossary of common audiologic terms and abbreviations is provided at the end of the chapter. Interoctave hearing loss is a characteristic of commonly encountered problems, such as noise-induced cochlear dysfunction. High-frequency audiometry for stimulus frequencies greater than 8,000 Hz (up to 20,000 Hz) is technically feasible and clinically useful to certain populations, such as patients at risk for ototoxicity. All audiograms include at the minimum a graph for plotting hearing threshold levels as a function of the frequency of pure-tone signals, although the exact format and symbols vary. Stimuli are pure tones (sinusoids) at octave frequencies typically from 250 Hz up to 8,000 the unit of stimulus intensity is the decibel (dB), a logarithmic unit. The intensity of any sound is defined by the ratio of its sound pressure or sound intensity to a reference sound pressure or sound intensity. The reference sound pressure is the amount of pressure against the eardrum, caused by air molecules when a sound is present, that vibrates the eardrum and can just be detected by a normal human ear. Briefly, the relation for sound intensity is described as dB= 10 log10 (sound intensity/reference intensity) or for sound pressure as dB = 20 log10 (sound pressure/reference pressure). This is the standard for the intensity level that corresponds to the mean normal hearing threshold level, the minimal detectable intensity for each test frequency for young adults with normal hearing. A: the separate ear fonn has sections for reporting results for pure-tone audiometry top), speech audiometry (center), and aural immittance measurement (bottom). Categories of hearing loss of shown on Ute right ear graph, whereas typical findings for a conductive hearing lo" are shown in Ute left ear graph. B: the traditional audiogram form utilizes symbols (see audiogram legend for each of 13 signal presentation types. In audiologic assessment of cooperative children and adults, hearing thresholds for tonal or speech signals are measured separately for each ear with earphones (air-conduction stimulation). They offer distinct advantages over traditional supraaural earphones, including increased comfort. Pure-tone audiometry can be performed with stimuli presented with a bone-conduction oscillator or vibrator placed on the mastoid bone. Testing is conducted according to clinical adaptations of psychoacoustic methods (1). Patients are instructed to listen carefully for the tones and to respond, usually by pushing a button that activates a response light on the audiometer or by raising a hand, every time they believe they hear a tone. The most important frequencies for understanding speech are 500 through 4,000 Hz, although higher frequencies can contribute to discrimination between certain speech sounds. A four-frequency PfA including 3,000 Hz is required by the American Academy of OtolaryngologyHead and Neck Surgery. The main mechanism of crossover is presumed to be bone-conduction stimulation caused by vibration of the earphone cushion against the skull at high stimulus intensity levels. The amount of sound intensity needed before crossover occurs is a reflection of interaural attenuation, that is, the sound insulation between the two ears provided by the head. In clinical circumstances, the examiner needs to assume conservatively that interaural attenuation for bone-conducted signals is 0 dB. In other words, even a very faint sound presented to the mastoid bone of one ear by a bone-conduction vibrator can be transmitted through the skull to either or both inner ears. Masking is the audiometric technique used to eliminate participation of the ear not being tested whenever air- and bone-conduction stimulation exceeds interaural attenuation. An appropriate noise (narrow-band noise for pure-tone signals and speech noise for speech signals) is presented to the ear not being tested when the stimulus is presented to the test ear. With adequate masking, any signal crossing over to the ear not being tested is masked by the noise.
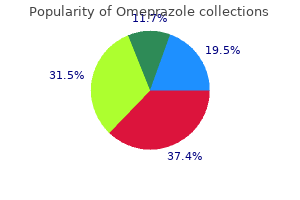
The factors that are assessed in predicting recovery of facial function include timing of onset (delayed vs gastritis symptoms in telugu 20 mg omeprazole visa. The delay of onset of paralysis following temporal bone fracture is the most important of the predictive factors gastritis cats 20 mg omeprazole buy mastercard. McKennan and Chole (53) described their experience with 17 patients with immediate-onset facial paralysis and 19 patients with delayedonset paralysis gastritis flare up cheap 20 mg omeprazole with amex. Complete spontaneous recovery of facial function occurred in 94% of the patients with delayedonset paralysis gastritis ct proven 40 mg omeprazole. In contrast the gastritis diet order discount omeprazole line, B out of the 17 immediate-onset paralysis patients had facial nerve transections. Chapter 150: Middle Ear and Temporal Bone Trauma 2417 Turner reviewed a large series of traumatic facial paralysis treated conservatively (54). Complete recovery occurred in 94% of the delayed-onset cases and 75% of immediate-onset palsies. The one patient with delayed-onset paralysis who had no recovery of function developed the facial palsy coincident with acute otitis media. Similarly, in a recent systematic review, the outcomes of 25 patients with immediate paralysis and 20 patients with delayed paralysis treated with conservative management were assessed. Eighty percent of the delayed paralysis patients had complete recovery of facial function while less than 40% of those with immediate paralysis recovered complete facial function (55). However, 44 out of 45 of their patients (including both immediate and delayed onset) had satisfactory recovery. Review of the above literature argues strongly against surgical exploration and decompression of delayed posttraumatic and facial paralysis. There are no convincing data in the literature that demonstrate that surgical intervention in delayed-onset paralysis will increase the probability of complete recovery of function. May describes the difficulty in differentiating immediate- from delayed-onset facial paralysis. He explored reportedly "delayed-onset" palsies and found on occasion a severed nerve (57). This observation highlights the necessity of careful examination in the emergency room prior to chemical paralysis. Even in comatose patients, painful stimuli will generally induce a symmetric grimace when both facial nerves are intact; unilateral weakness of all facial branches implies a peripheral-that is, facial nervelesion, whereas selective weakness of the lower branches with bilateral temporal branch sparing implies a central lesion, proximal to the facial nucleus. Admittedly, information regarding facial nerve function immediately following an injury is not always available. Sometimes the exam is omitted due to attention to other life-threatening complications or because the patient has already received muscle relaxants with intubation. If facial function is present in the emergency room and subsequently deteriorates, our experience is that the patient will recover without surgical treatment. The degree of facial nerve injury is also a critical factor in guiding the management algorithm. Incomplete paresis rarely fails to completely resolve spontaneously unless an additional insult to the nerve. Consequently, only patients with complete paralysis of immediate or unknown onset are considered for surgical exploration. The role of electrodiagnostic testing is to assist the clinician in differentiating a neuropraxic injury from a neural degenerative injury and to assess the proportion of degenerated axons. Nerves sustaining a neuropraxic injury proximal to the stimulated portion of the nerve maintain electrical stimulability at all times following the injury. Partial or complete disruption of the nerve results in Wallerian degeneration and consequent decrease or loss of stimulability. However, Wallerian degeneration occurs in a delayed fashion, and the distal segment of the nerves maintains electrical stimulability for 3 to 5 days postinjury (58). Consequently, electrodiagnostic testing cannot reliably differentiate a neuropraxic injury from a laceration of the nerve for up to 3 to 5 days. The first-degree injury is an anatomically intact nerve fiber with a conduction blockade (neuropraxia). The seconddegree injury transects the axons but maintains an intact endoneurium (axonotmesis). The third-degree injury transects the axon and endoneurium but maintains an intact perineurium (neurotmesis). Aberrant regeneration can occur with third-degree injuries, leaving patients with some weakness and synkinesis. Fourth-degree injuries transect the entire nerve trunk but maintain an intact epineural sheath (neurotmesis). Loss of the conduit of the epineural sheath allows regenerating axons to cross into adjacent fascicles, resulting in a loss of topographic organization. A proportion of the regenerating fibers are also lost due to the healing process and scarring. These lesions result in a high incidence of residual weakness, synkinesis, and hyperkinesis. Complete transection of the entire nerve trunk and epineurium is classified as a fifth-degree injury (neurotmesis) and is associated with poor spontaneous recovery, if any, depending on the degree of diastasis of the nerve stumps. Some authors have advocated a sixth-degree injury classification in which different fascicles of the facial nerve have sustained different degrees of injury of the five traditional injury types described by Sunderland. The current used is incrementally increased just until threshold is reached, manifested by facial twitching, and this threshold level is recorded for each side individually. The test is most useful between 2 and 14 days postinjury in patients with dense facial paralysis to differentiate between neuropraxic and neurodegenerative injuries. The testing is unnecessary in incomplete paralysis in which there is almost always 100% recovery. The difference in contraction is expressed as equal, mildly decreased, markedly decreased, or no response. Again, any volitional movement of the face would indicate an intact nerve trunk and supercede any electrical testing. The stimulating bipolar electrodes are placed adjacent to the stylomastoid foramen, and the recording bipolar electrodes in the nasolabial crease. If voluntary activity is present in the acute postinjury period, the patient has a very high probability of good recovery (64). Fibrillation potentials result from denervation of the muscle but are delayed 2 to 3 weeks following the injury and consequently offer little additional information to guide therapy in the acute setting (66). Turner in 1944 reported on 69 patients with varying degrees of facial paralysis following temporal bone trauma (54). Thirty of these patients had complete facial paralysis, all of which were treated nonoperatively. This group of patients was unbiased in that none of his series underwent surgical decompression. Good recovery occurred in 63% of the patients, incomplete recovery with synldnesis in 23%, and poor recovery in 13 o/o. Brodie and Thompson (2) had eight patients with complete paralysis who met criteria for facial nerve decompression who, for a variety of reasons, did not undergo surgical exploration. Seven of the eight patients had good recovery of function and one patient had a poor outcome. The combined rate of good recovery of function with conservative, nonsurgical management, in the above three studies is 63%. In contrast analysis of six case series studies of patients undergoing surgical decompression for complete facial nerve paralysis revealed a combined rate of good recovery of facial function of 51%. It is difficult to compare the recovery rates of facial nerve function in patients undergoing surgical and nonsurgical management the patients included in the observation studies did not necessarily meet the same criteria as those included in the surgical decompression studies, thereby potentially artificially inflating the positive outcomes in patients treated nonsurgically. Since Wallerian degeneration is not documented on electrodiagnostic testing for 3 to 5 days following the axonotmesis or neurotmesis, surgical intervention is delayed until several days after the nerve has degenerated. Although decompression of the facial nerve prophylactically in acoustic neuroma surgery has been proven efficacious, the decompression is performed prior to Wallerian degeneration having occurred (72). Demonstrating that decompression of a posttraumatic nonsevered nerve is efficacious remains to be proven in a randomized prospective study. The key factor in the decision to surgically explore a facial nerve is whether the nerve is suspected of being severed, crushed, or impaled with bone fragments. The incidence of transected nerves in the largest series ranges from 6% to 45% (52,67 -69,73). The high frequency ofsevered nerves in some of these reports is biased by patient selection, as discussed previously. Patients are referred to the tertiary centers performing nerve explorations when they fail to spontaneously recover. However, the vast majority of patients do not have a transected nerve and therefore recover spontaneously and are not referred to tertiary centers. The probability of severing the facial nerve is actually quite low, but the outcome of a transected nerve following observation alone is poor. Therefore, an attempt should be made to identify patients with crushed, impaled, or otherwise transected nerves, as these are the patients who would most benefit from surgical intervention. Electrodiagnostic testing of nerves with complete paralysis can only differentiate injuries that have undergone Wallerian degeneration from those that have not, that is, Sunderland 11-V- versus Sunderland! Since one cannot differentiate a Sunderland fifth-degree injury (severed nerve) from a second-, third-, or fourth-degree injury on the basis of electrodiagnostic testing, exploration is warranted only in patients with complete, immediate-onset paralysis in whom electrical stimulability is lost; it is these patients who are at greatest risk for crushed, partially severed, or transected nerves. The site of injury to the facial nerve in temporal bone fractures is in the perigeniculate region in 80% to 93% of patients (33,67,68). Lambert and Brackmann (67) found a second lesion in 4 out of 21 patients in the mastoid segment Accordingly, the approach utilized for the nerve exploration must expose these two regions. Fisch advocates a translabyrinthine approach for transverse fractures and a combined transmastoid/middle cranial fossa approach for longitudinal fractures (63). May described a transmastoidf supralabyrinthine approach to the region of the geniculate ganglion for facial nerve decompression (74). Goin studied this approach in cadaveric temporal bones and found that he could consistently expose the distal labyrinthine segment and geniculate ganglion (75). Yanagihara (76) applied the transmastoid/supralabyrinthine approach in 36 patients. Only five temporal bone fractures in his series of 41 patients required a middle cranial fossa approach to expose the geniculate region. The translabyrinthine approach is advocated for facial nerve exploration in patients with profound hearing loss. The approach provides excellent exposure for decompression, nerve rerouting with direct reanastomosis, and cable grafting. In otic capsule-sparing fractures with ossicular discontinuity, the nerve is explored via a transmastoid/ supralabyrinthine approach. This approach generally requires dislocation of the incus and ossicular reconstruction at the completion of the operation. If the patient has any contralateral hearing loss or the anatomy is not conducive for supralabyrinthine exposure, a middle cranial fossa approach is utilized. This recommendation was based on the observation that regeneration and axoplasmic flow were greatest at 3 weeks postinjury. Barrs studied the timing of facial nerve repair in micropigs and found no advantage of waiting the 3 weeks until the neuronal cell body metabolic activity was maximal (78). Tills animal model did not show a statistically significant difference in electrophysiologic testing between nerves grafted throughout various times within 3 months of transection. He argues that decompression should be performed early to minimize further degeneration. His series demonstrated a correlation between better results and shorter interval between injury and repair. The question as to whether these patients would have recovered spontaneously to the same degree remains unanswered. Six patients had nerve edema and two had bony impingement of the nerve at the time of operation. Again, the question remains whether these patients would have had spontaneous recovery to the same degree. Fifty-nine percent of facial palsies that recover spontaneously do so within 1 month, and 88% recover by 3 months postinjury (2). Summary of Facial Nerve Treatment Algorithm Patients with delayed-onset facial paralysis are placed on a 2-week course of systemic corticosteroids (unless medically contraindicated) and observed. Patients with complete paralysis of immediate onset are tested with the Hilger nerve stimulator between days 3 and 7 postinjury. If stimulability is present to any degree (implying a physically intact nerve), the patients are observed. If the nerve loses all stimulability within 1 week of the injury, facial nerve exploration is performed. Facial nerve injuries occurring in an otic capsuledisrupting fracture are typically explored via a translabyrinthine approach: the translabyrinthine approach affords the most direct, complete access to the entire length of the intratemporal facial nerve, and in fractures that cause a profound sensorineural hearing loss, the approach does not engender any significant morbidity than that already sustained. In patients in whom excellent intrinsic exposure of the intratemporal facial nerve can be achieved, that is, with well-aerated mastoid air cell systems or with ossicular discontinuity, a transmastoid/supralabyrinthine approach is chosen. If a severed facial nerve is encountered using the transmastoid/supralabyrinthine approach and inadequate exposure for cable grafting occurs, a middle cranial fossa approach is performed. The transmastoid facial nerve decompression begins with a complete mastoidectomy skeletonizing the tegmen mastoideum superiorly, the sigmoid sinus posteriorly. The antrum is opened, exposing the short process of the incus and the lateral semicircular canal. The facial recess is opened and the facial nerve is skeletonized from the second genu to the stylomastoid foramen.
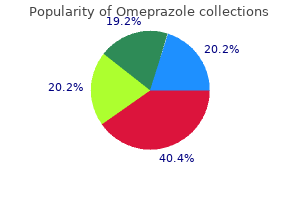
The paramedian strip of mucosa will be later Imbricated over the bony edge of the hard palate to facilitate the flttlng of a prosthesis chronic gastritis leads to discount 20 mg omeprazole amex. C; the orbital contents are dissected from the medial Inferior and lmral walls gastritis diet 8 plus 10 mg omeprazole purchase with amex, exprulng the lacrimal sac gastritis diet kencing cheap omeprazole amex, the anterior and posterior ethmoid arteries gastritis chronic erosive order omeprazole in united states online, and the Infraorbital flssure gastritis sintomas buy generic omeprazole from india. The maxilla Is severed from the nasal bones with the saw, and the osteotomy Is extended superlorty to the frontoethmoldalsuture. A superior osteotomy Is carried out posteriorly to a point 3 to 4 mm posterior to the posterior ethmoid artery. An osteotomy Is performed connecting the lateral and medial wall osteotomies across the Inferior orbital flssure. The maxilla Is detached from the skull by tapping a chisel placed Into the pblrygomaxillary flssure In a posterosuperior direction. The obturator or denture is wired to the remaining dentition or suspended from Ute zygomaic arch and pirifonn aperture or leg screwed to the remaining hard palate. The anterior half is used for Ute reconstruction, and the posterior half is transposed to the anterior temporal fossa to obliterate the defect. Ethmoid Sinus Tumors originating in the ethmoid sinuses produce symptoms at early stages, leading to earlier diagnosia and better prognosis. Combined therapy with radiation is recommended for advanced stages, positive surgical ma! Sphenoid Sinus Primary malignancies of the sphenoid sinus are extremely rare, making up less than 1% of malignant sinonasal tumoa. These incisions allow the preservauon of the lids, which can be used to line the remaining orbital cavity. If the eyelids are involved by the tumor, the incisions are modified to include their resection en bloc. The upper eyelid is retracted superiorly, and the periorbita is incised over the superior orbital rim. The orbit is dissected from the superior wall, identifying optic: foramen and superior orbital fissure. These are infiltrated with lidocaine to block the autonomic innerv«tion and prevent cardiac arrhythmias. The neural and vascular structures traveling through these foramina are transec:ted after hemostasis with bipolar cautery or damping. Inferior traction on the globe allows further visualization of tha orbital floor and Inferior orbital fissure. The roof oftha orbit may be lined with a skin graft or left to granulate and mucosalize. In tha case of axtanslon through the anterior wall of the antrum, tha facial ftap may be alevatad In a subcutaneous plane, Including the facial musculature In the specimen. The dissection Is carried out along the lataral wall of the maxilla and tha Internal maxillary artery Is ldentlfled at the pt:erygomaxlllary flssure and dipped. Tumors confined to the ftoor of the antrum may be managed by partial maxlllectomy. The nasal septum may be sacrlfload or praserved for suspension of the prosthesis or reconstructive ftaps. Usually requires surgical drai nag e/debri dement (+)margins, perineural, perivascular invasion (+)lymph nodes, recurrent tumor Palliative role Clinical research (controlled protocols) Combination therapy Chemotherapy sinus. Gross total removal and postoperative radiation therapy is the treatment of choice for most of these tumors. Although the benefits of surgical debulking are debatable, at the very least it will provide a wide sphenoidotomy for drainage and debridement during radiation therapy. Frontal Sinus Tumors arising in the frontal sinus, like sphenoidal tumors, are rare. As great as 26% of patients with sinonasal malignancies have orbital invasion at the time of presentation (23). Patients with orbital invasion rapidly develop ocular symptoms, such as proptosis, diplopia, decreased visual acuity, diminished motility, chemosis, lid edema, and epiphora. Bone erosion does not constitute an absolute indication for orbital exenteration (24). The prognosis of patients with invasion of the periorbita is dismal; therefore, palliation is a more realistic goal (Table 129. Adjunctive radiation therapy, before or after surgery, does not seem to yield an improved prognosis. Resection of the medial and inferior orbital walls produces severe enophthalmos and hypophthalmos, which is aggravated by resection of the periorbita. Rigid reconstruction of the bony orbit using titanium mesh with or without calvarial bone grafts is recommended; which is then covered with local, regional, or microvascular flaps. To better restore the orbital anatomy and to prevent lagophthalmos, due to ectropion, the lateral canthus should be reattached to the corresponding anatomical site of insertion. The low incidence of nodal metastasis from sinonasal malignancies does not justify the use of elective neck dissection or radiation. The trend toward worst survival in those patients who required exenteration illustrates the aggressiveness of tumors that invade the periorbita. However, an isolated rerurrence to cervical nodes is rare; usually it is accompanied by rerurrent disease at the primary site. The presence of tumor in this area is considered a risk factor for local rerurrence. Despite the difficulty of an en bloc resection of this area, several authors have designed approaches with sound oncologic principles, obtaining variable results. Infratemporal Fossa and Skull Base the skull base may be involved by tumor by direct invasion and bone erosion, by preformed pathways. The overall incidence of skull base invasion by sinonasal malignancies appears to be about 15%. Absolute contraindications for craniofacial resection are medical or nutritional problems that would eliminate the patient as a surgical candidate. Resection of these areas is associated with an unacceptable morbidity and mortality rate. Relative contraindications include invasion of the dura and intracranial involvement of neural structures. These situations have a poor prognosis, but in selected cases craniofacial resection may offer significant palliation or local control. A dacryocystorhinostomy at the time of definitive resection is an effective way to prevent this complication. Limitation of movement of the extraocular muscles may occur after trauma to the muscle or its motor innervation or upon entrapment in the craniofacial osteotomies. The optic nerve may be compressed during the mobilization of the specimen or during craniofacial resection. Enophthalmos or hypophthalmos usually develop due to the loss of the inferior orbital and/or medial support. Radiation Therapy the incidence of radiation complications in patients with orbit preservation is close to 100% (Table 129. The field included in the radiation portals for sinonasal tract tumors usually includes the anterior and posterior orbital segment. When the orbit is involved by the tumor, irradiation of the entire eye is usually necessary. A dry eye will decompensate rapidly, leading to severe keratitis, panophthalmitis, and blindness within 1 year. If the anterior segment can be spared, patients will most likely experience delayed (3 to 5 years) loss of vision secondary to post-radiation retinopathy or optic neuropathy. Although the retina and optic nerve are radio resistant, their microvasrulature is not. Although they are rare below 3,500 cGy, their incidence is 50% to 65% with 6,000 to 7,000 cGy and above 85% with 8,000 cGy. Nevertheless, the degree of visual impairment cannot be acrurately predicted and has been reported with doses considered within the safe limits. The incidence of unilateral blindness can range around 35%, while the incidence of bilateral blindness, although rarely reported, may be as high as 8% and is related to the irradiation of the contralateral posterior segment. Blindness is felt to be due to ipsilateral radiation retinopathy and contralateral optic neuropathy. However, the dose should not be compromised to diminish the complication rate if the attempted goal is rure. Conformal radiation therapy reduces the percentage of radiation received by normal tissue and may decrease the incidence of optic nerve and optic chiasm complications. Chapter 129: Neoplasms of the Nose and Paranasal Sinuses 2059 Wound Complications Wound complications include bleeding, infection, and loss of reconstructive flaps or skin grafts Table 129. Severe osteoradionecrosis can be secondary to poor dentitia or recently atracted dentitia. We recommend the routine emaction of poor dentitia with time to recover prior to postoperative radiation to avoid this complication. D: Orbital, cranial, and zygomatic osteotomies are performc~d according to the required exposure. The aaniotomy and orbital bone grafts are replaced above the pericranial flap which separates the aanial cavity from Ute upper aerodigestive tract. Formation of austs within the nasal cavity is a common problem and may lead to infection. A secondary reconstruction must be postponed until the defect is free of infection. Treatment oflocal infection and debridement of neaotictissue, followed by regmfting with internal and exwnal splinting of the skin graft may remedy this problem. Ocular and orbital complications following radiation therapy of paranasalsinus malignancies and review of literature. Mild to moderate bleeding is managed using the principles of treatment for anterior and posterior epistaxis. In the case of a massive tumor that completely occludes the nasal passages, angiography and embolization should be considered. If circumstances preclude the use of this technique, a transantral ligation of the internal maxillary artery and transotbitalligation of the ethmoidal arteries may control the bleeding. Ligation of the external carotid artery, although not as effective as internal maxillary artery ligation, may be necessary if the transantral approach is impossible. One should remembe~; however, that ligation of the external carotid artery will eliminate the possibility of embolization. Uncontrollable hemostasis from a known malignancy may require emergency maxillectomy. Emergent treatment of the tumor with radiation or surgery may be necessary to prevent blindness, although it will be a moot point if the eye is going to be ultimately sacrificed. Treatment includes empiric intravenous antibiotics with broad spectrum coverage, including the skin and aerodigestive flora. Further contamination or exposure of the intracranial contents to the sinonasal tract should be curtailed by the use of vascularized flaps. Free bone grafts that become infected during the early postoperative period should be removed. Late osteomyelitis or osteoradionecrosis may be managed with antibiotics and debridement limited to the affected bone. Hyperbaric oxygen treatment may be beneficial in patients with osteoradionecrosis. Tension pneumocephalus is treated by percutaneous aspiration and diversion of the nasal airway. The latter may be accomplished with the use of an endotracheal tube, nasal trumpets, or a tracheotomy. Lymph node metastases in malignant tumors of the paranasal sinuses: prognostic value and treatment. Endonasal endoscopic medial maxillectomy with preservation of the inferior turbinate. Long-term single-center results of management ofethmoid adenocarcinoma: 95 patients over 28 years. Primary mucosal melanoma of the sinonasal tract: report of 18 patients and anal~is of 1077 patients in the literature. Mucosal melanoma of the nose and paranasal sinuses, a contemporary experience from the M. When, how and why to treat the neck in patients with esthesioneuroblastoma: a review. Benign schwannoma in paranasal sinuses: a clinico-pathological study of five cases, emphasizing diagnostic difficulties. Lymphoma ofthe nasal cavity and paranasal sinuses: improved outcome and altered prognostic factors with combined modality therapy. Endoscopic surgery for malignant tumors of the sinonasal tract and adjacent skull base: a 10-year experience. Intra-arterial cisplatin and concomitant radiation therapy followed by surgery for advanced paranasal sinus cancer. Patterns and incidence of neural invasion in patients with cancers of the paranasal sinuses. They may seem indicated in the presence of a necrotic tumo~ but prolonged treatment may lead to colonization with resistant flora that will be more difficult to eradicate in case of meningitis. The response of sinonasal tract tumors to radiation therapy varies with the stage and histology of the tumor. This article outlines the most common categories of orbital tumors and other common orbital pathologic processes. We discuss various classifications of the pathologies presented, as well as the most common associated signs/symptoms, radiographic findings, and recommended workup and treatment for these lesions.
Buy omeprazole american express. What causes chemical gastritis ? | Healthy LIFE.
Preservation of hearing and facial nerve function is paramount in many otologic and neurotologic procedures gastritis healing process omeprazole 40 mg buy fast delivery. Although the preservation of hearing has yet to reach the same level of success achieved in preservation of the facial nerve function gastritis diet ���� omeprazole 20 mg low price, the technology and our understanding of the neurophysiologic basis of hearing is advancing gastritis lemon buy omeprazole with a visa, and further improvement seems likely gastritis diet ������� omeprazole 20 mg buy otc. Intraoperative monitoring of the facial and auditory nerves is now in increasing use around the world lymphocytic gastritis definition order discount omeprazole line. Efficacy has been established in improving functional outcomes in cerebellopontine angle tumors and many experts favor its routine use in a wide array of both otologic and neurotologic surgeries, especially when the risk of nerve injury is considered to be high. As we expand neurophysiologic monitoring to other cranial nerves, its role in the preservation of these nerves may prove useful in quality of life outcomes and likely will play a larger role in neurotologic surgery in the future. Regardless, intraoperative neurophysiologic monitoring should serve only as an adjunct to , not a replacement for, enensive preoperative planning, a thorough knowledge of temporal bone anatomy and its common variants, and meticulous technique. Improved preservation of hearing and facial nerve function in vestibular schwannoma swgezy via the retrosigmoid approach in a series of 200 patients. Intraoperative neurophysiological monitoring in vestibular schwannoma surgery: advances and clinical implications. Evaluation of three intraoperative auditozy monitoring techniques in acoustic neuroma swgezy. Intraoperative cochlear nerve monitoring in vestibular schwannoma surgery-does it really affect hearing outcome Hearing preservation and intraoperative auditozy brainstem response and cochlear nerve compound action potential monitoring in the removal of small acoustic neurinoma via the retrosigmoid approach. Management of vestibular schwannomas (acoustic neuromas): the value of neurophysiology for evaluation and prediction of auditory function in 420 cases. Acoustic neuroma surgery: use of cochlear nerve action potential monitoring fur hearing preservation. Delayed sensorineural hearing loss following uncomplicated neurovascular decompression of the trigeminal root entzy zone. Results of auditory brainstem response monitoring of microvascular decompression: a prospective study of 22 patients with hemifacial spasm. Brainstem auditory evoked potential monitoring during microvascular derompression fur hemifacial spasm: intraoperative brainstem auditory evoked potential changes and warning values to prevent hearing loss-prospective study in a consecutive series of 84 patients. Intraoperative monitoring ofbrainstem auditory evoked potentials during microvascular decompression of cranial nerves in cerebellopontine angle. Operative strategies fur minimizing hearing loss associated with microvascular decompression fur trigeminal neuralgia. Microvascular decompression for hemifacial spasm: long-term results from 114 operations performed without neurophysiological monitoring. Electrocochleography: a review of recording approaches, clinical applications, and new findings in adults and children. Succinylcholine can be used for induction because of its short duration of effect with complete recovery from neuromuscular blockade within 15 minutes. Intraoperative monitoring of facial and cochlear nerves during acoustic neuroma swgezy. Late failure rate of hearing preservation after middle fossa approach fur resection of vestibular schwannoma. Hearing preservation in retrosigmoid approach of small vestibular schwannomas: prognostic value of the degree of internal auditozy canal filling. Hearing preservation in acoustic neuroma surgery: value of monitoring oochlear nerve action potentials. Hearing preservation after acoustic neuroma surgery using intraoperative ctirect eighth cranial nerve monitoring. Electmcochleogram after transection of vestibulo-cochlear nerve in a patient with a large acoustic neurinoma. Intraoperative electrooochleography of endolymphatic hydrops surgery using clicks and tone bunts. Compound action potentials recorded intracranially from the auditory nerve in man. Intraoperative auditory assessments as predictors of hearing preservation after vestibular schwannoma surgery. Advances in monitoring of seventh and eighth cranial nerve function during posterior fussa surgery. A oomparison of direct eighth nerve monitoring and auditory brainstem response in hearing preservation surgery fur vestibular schwannoma. The learning curve in post-operative hearing results in vestibular schwannoma surgery. Transtragal, transtympanic electrode placement for intraoperative electmcochleographic monitoring. Intraoperative monitoring of cochlear nerve oompound action potential in cerebellopontine angle tumour removal. Intraoperative brainstem auditory evoked potential pattern and perioperative vasoactive treatment fur hearing preservation in vestibular schwannoma surgery. Intraoperative monitoring of cochlear function using distonion product oto- 2331 53. Intraoperative monitoring of facila muscle evoked responses obtained by intracranial stimulation of the facila nerve: a more accurate technique forfacila nerve dissection. Technical and instrumental improvements in the surgical treatment of acoustic neurinomas. New development in intraoperative video monitoring of facial nerve: a pilot study. Continuous electromyography monitoring of motor cranial nerves during cerebcllopontine angle surgery. Video-based system for intraoperative facial nerve monitoring: oomparison with electromyography. Does electrode placement influence quality of intraoperative monitoring in vestibular schwannoma surgery Four-channel electromyography of the facial nerve in vesttbular schwannoma surgery: sensitivity and prognostic value fur short-term facial function outcome. Electroneurography and intraoperative facial monitoring in contemporary neurotology. Microsurgical instruments and nerve stimulatormonitor fur retrolabyrinthine vestibular neurectomy. Intraoperative monitoring of facial nerve antidromic potentials during acoustic neuroma surgery. Intraoperative monitoring of the facial nerve during decompressive surgery for hemifacial spasm. Improved preservation of facial nerve function in the infratemporal approach to the skull base. Intraoperative facial nerve monitoring in chronic ear surgery: a resident training experience. Cost-effectiveness of intraoperative facial nerve monitoring in middle ear or mastoid surgery. Congenital auricular atresia: update on options for intervention and timing of repair. Intraoperative monitoring of lower cranial nerves in skull base surgery: technical report and review of 123 monitored cases. Electmphysiologic recurrent laryngeal nerve monitoring during thyroid and parathyroid surgery: international standards guideline statement. Vagal nerve monitoring in surgery of the skull base: a comparison of efficacy of three techniques. Intraoperative monitoring of facial nerve function in cerebellopontine angle surgery. A multifactorial analysis of facial nerve results in surgery for cerebellopontine angle tumon. Intraoperative facial nerve monitoring in posterior fossa acoustic neuroma surgery. Predictive facton of longterm facial nerve function after vestibular schwannoma surgery. Assessment of real-time clinical facial function during vestibular schwannoma resection. Facial nerve monitoring parameten as a predictor of postoperative facial nerve outcomes after vestibular schwannoma resection. Intraoperative monitoring and facial nerve outcomes after vestibular schwannoma resection. Quantitative parameters of intraoperative electromyography predict facial nerve outcomes for vestibular schwannoma surgery. Thain time as a quantitative electromyographic parameter for facial nerve function in patients undergoing surgery for vestibular schwannoma. Delayed facial nerve paresis following acoustic neuroma resection and postoperative vasoactive treatment Zentralbl Neurochir 2004; 65: 103-107. Before disrussing the individual disease processes, we review the normal anatomy and physiology of the external ear. Both contain elastic cartilage derived from mesoderm and a small amount of subrutaneous tissue. During normal gestation, the cartilaginous hillocks merge to form the auricle, and with selective growth of the mandible, the auricle rises from its original position near the lateral commissure of the mouth to the temporal area. The tragus and antitragus form a partial barrier to the entrance of macroscopic foreign bodies. The process of canalization is complete by about week 12 of gestatio~ at which time the canal fills with epithelial tissue. The outer 40% of the canal in its anterior and inferior aspect is cartilaginous and contains a thin layer of subrutaneous tissue between the skin and cartilage. The inner 60% is osseous, is formed primarily by the tympanic ring, and contains very scant soft tissue between the skin, periosteum, and bone. The junction of the cartilaginous and bony portions of the canal is a narrowed section termed the isthmus. Laterally to medially, the canal rurves slightly superiorly and posteriorly in a gentle S shape. The canal can be thought of as pointing toward the nose; thus, pull the auricle gently upward, outward, and backward to straighten the canal for examination. Together, these three adnexal structures provide a protective function and are termed the apopilosebaceous unit. Glandular secretions combine with sloughed squamous epithelium to form an acidic coat of cerumen, one of the primary barriers to infection of the canal. An invagination of the epidermis forms the outer wall of the hair follicle, and the hair shaft forms the inner wall the follirular canal is the space between these two structures. The alveoli of the sebaceous and apocrine glands empty into short straight excretory ducts, which drain into follicular canals. Instrumentation and excessive cleansing of the canal distwb this primary protective barrier and may lead to infection. Individual variations in the anatomy of the canal may predispose some people to wax accumulation. Superiorly, the canal is bound by the middle cranial fossa and inferiorly by the infratemporal fossa and base of the skull. Infections mending through the roof of the canal may extend into these structures. Anteriorly, the canal is bordered by the temporomandibular joint and the parotid gland. The lymphatic drainage of the canal is an important channel for the spread of infection. Anteriorly and superiorly, the canal drains to the preauricular lymphatics in the parotid gland and the superior deep cervical nodes. The inferior portion of the canal drains into the infra-auricular nodes near the angle of the mandible. Posteriorly, the lymphatia drain into the postauricular nodes and the superior deep cervical nodes. Venous drainage from the auricle and meatus is via the superficial temporal and posterior auricular veins. The former joins the retromandibular vein, which usually divides and joins both jugular veins; the latter joins the atemal jugular but may also drain to the sigmoid sinus through the mastoid emissaJ:Y vein (1). The appearance of the canal varies according to the time cowse of infection: acute, subacute, or chronic. Later, pain ensues as the swollen soft tissues of the canal distract the periosteal lining of the bony canal. As the disease progresses, purulent discharge begins, and the auricle and periauricular soft tissues may become involved. In patients in whom the disease does not resolve after treatment, a subawte or chronic form may occur. This condition may be likened to eczema and is a spectrum of disease ranging from mild drying and scaling of the canal skin to complete obliteration of the canal by chronically infected hypertrophic skin. Pain, fullness, itching, and hearing loss are the four major symptoms of external otitis, although not every patient has each symptom (4). Typically, the preinflammatory stage begins when the stratum corneum becomes edematous due to the removal of the protective lipid layer and acid mantle from the canal, resulting in plugging of the apopilosebaceous unit. The disruption of the epithelial layer allows invasion of bacteria that either reside in the canal or are introduced on foreign objects inserted into the canal, such as a cotton swab or a dirty fingernail. This produces the acute inflammatory stage, which is accompanied by pain and tenderness of the auricle. Further progression of the inflammation in the absence of treatment produces the severe inflammatory stage.
References
- Ruskin JA, Gurney JW, Thorsen MK, et al. Detection of pleural effusions on supine chest radiographs. AJR Am J Roentgenol 1987;148(4):681-683.
- Zhang Q, Raoof M, Chen Y, et al. Circulating mitochondrial DAMPs cause inflammatory responses to injury. Nature. 2010;464:104-107.
- Oh JJ, Lee JK, Kim K, et al: Comparison of the width of peritumoral surgical margin in open and robotic partial nephrectomy: a propensity score matched analysis, PLoS ONE 11(6):e0158027, 2016.
- Saric M, Perk G, Purgess JR, et al. Imaging atrial septal defects by real-time three-dimensional transesophageal echocardiography: step-by-step approach.] Am Soc Echocardiogr. 2010;23:1128-1135.
- Jensen PA, Lambert LA, Iademarco MF, et al. Guidelines for preventing the transmission of Mycobacterium tuberculosis in healthcare settings, MMWR Recomm Rep. 2005;54(RR-17): 1-141.
- Muller MP, Hansel M, Stehr SN, Weber S, Koch T. A state-wide survey of medical emergency management in dental practices: incidence of emergencies and training experience. Emerg Med J 2008;25(5):296-300.
- Ben Q, Xu M, Ning X, et al. Diabetes mellitus and risk of pancreatic cancer: a meta-analysis of cohort studies. Eur J Cancer 2011;47(13):1928-1937.
