
Baycip
| Contato
Página Inicial
Carl Bouchard, DMD, MSc, FRCD (C)
- Clinical Professor, Department of Oral and
- Maxillofacial Surgery
- Laval University
- Centre Hospitalier Affili? Universitaire de Qu?bec
- Quebec, Canada
In this article medications that cause hyponatremia discount 500 mg baycip, we explore the application of tractography to the study of white matter neuroanatomy medications removed by dialysis purchase 500 mg baycip. We further discuss tractographic contributions to the understanding of the anatomy of major white matter systems (projection symptoms 4dp5dt fet cheapest baycip, association symptoms 9dpiui buy baycip overnight delivery, limbic treatment xerostomia order baycip toronto, commissural, and cranial nerves). When compared to the traditionally used method of post-mortem white matter dissection, tractography confers several notable advantages: firstly, it does not involve the removal of overlying cortex or white matter, thus completely preserving hemispheric architectural integrity. Secondly, it allows for observation of white matter cortical terminations, giving direct insight into connectivity. Thirdly, white matter volumetry may be calculated, allowing determination of the hemispheric lateralization of white matter systems. It involves the calculation of a single directional tensor per voxel, derived from the diffusion properties of protons confined to axons. Tractographic visualization is subsequently achieved by stepwise connection of similarly oriented directional tensors (or equivalent for nontensor techniques). Shortcomings of tensor-based tractography are its inability to accurately trace crossing fibers and the inability to demonstrate cortical terminations with accuracy. Tractography has addressed some of these controversies by allowing in vivo studies in large groups of healthy and diseased subjects. Nevertheless, because of the variance in tractographic modalities and methodologies, new controversies regarding the structure, subdivision, connectivity, and even existence of white matter systems have arisen. Short projections, known as the anterior thalamic radiations, then project from the thalamus to the cingulum. The cingulum travels around and dorsal-to the parasagittal corpus callosum, before terminating within the entorhinal cortex and completing the circuit. Fornix the fornix is the primary efferent hippocampal pathway and is readily visualized using tractographic algorithms. It originates from the subiculum and entorhinal cortex of the hippocampus as the fimbria. Each hemispheric fimbria passes superomedially along the medial border of the posterior pulvinar in a forward-looping course. It is joined by its antihemispheric counterpart at the junction of the atrium and body of the lateral ventricle, to form the forniceal body, which lies beneath the splenium of the corpus callosum. The two hemispheric components of the body communicate via the hippocampal commissure, or psalterium. The body continues anteriorly, along the superomedial surface of the posterior aspect of the pulvinar before separating again into antihemispheric continuations above the anterior surface of the foramen of Monro. These anterior divisions each further subdivide into anterior and posterior columns. The anterior column terminates within the hypothalamus, accumbens nucleus, and septal region. Anteriorly, it originates below the genu of the corpus callosum from the subcallosal gyrus and paraolfactory area. It courses around the genu and splenium of the corpus callosum, traveling posteriorly within the white matter of the cingulate gyrus, assuming its sagittal contour. The posterior (ventral) component continues as cingulate fibers travel via the medial temporal lobe to terminate within the uncus, parahippocampal gyrus, and amygdala. Along its course, short fibers interconnect cortical areas over both long and short distances. Thalamic Radiations the thalamic radiations are short fibers that project radially from the gray matter of the thalamus to end points within the frontal, parietal, temporal, and occipital lobes. Postthalamic fibers travel further dorsally, becoming interspersed with fibers from the anterior limb of the internal capsule, to terminate within the cingulum and cingulate gyrus. Projection System the projection system subserves both cortical sensory input and motor output. The motor projection pathways include geniculate and cerebrospinal fibers traversing within the genu and posterior aspect of the internal capsule and the corticopontine fibers. Extrathalamic Serotonergic Projections the dorsal longitudinal fasciculus is the primary extrathalamic serotonergic afferent. It originates from the dorsal raphe nuclei as two smaller bundles (dorsal and ventral), which ascend in the paramedian brain stem and merge at the caudal diencephalon before separating again. One group of fibers ascends within the internal capsule and terminates within lateral cerebral cortex. The other group curves ventrally, traveling to the hypothalamus via the medial forebrain bundle. They originate at the ventroposteromedial and ventroposterolateral nuclei of the thalamus together with components of the corona radiata. Toward their terminations within the postcentral cortex the thalamocortical sensory projections are said to "rotate" posteriorly. Research concerning their anatomy has been limited largely to nonhuman immunohistochemical tracer studies; however their pathway from the locus coeruleus nuclei is suggested to travel to frontal cortical areas via the brainstem, before sweeping rostrocaudally through the hemisphere via the cingulum and giving off widespread connections throughout its course. Extrathalamic Projections There are four types of extrathalamic afferent projections traversing between subthalamic nuclei and cortical areas. They convey serotonergic, noradrenergic, dopaminergic, and cholinergic afferents from the mesencephalic raphe nuclei, pontine nucleus locus coeruleus, substantia nigra/ventral tegmental area complex, and nucleus basalis of the substantia innominata, respectively. These pathways remain obscure to cadaveric Extrathalamic Dopaminergic Projections Extrathalamic dopaminergic afferents arise from the substantia nigra, within the ventral tegmental area of the midbrain. There is otherwise limited information regarding the trajectory of these projections within humans. The medial pathway originates from Ch4 nuclei and travels via the gyrus rectus and medial orbital gyrus to the callosal rostrum, before entering the cingulum. As part of the cingulum course, it gives off radiations to orbitofrontal, subcallosal, cingulate, pericingulate, and retrosplenial cortex. A capsular division ascends from Ch4 via the medial external capsule adjacent to the putamen, terminating within the dorsal frontoparietal cortex, middle and inferior temporal gyri, inferotemporal cortex, and the parahippocampal gyri. Individual capsular fibers travel via the uncinate fasciculus to the amygdala (this is potentially disputed, see below). The second lateral component is a perisylvian division also traveling within the claustrum, before turning laterally to terminate within the inferior frontal and superior temporal gyri. Individual perisylvian fibers radiate to the frontoparietal operculum, Optic Radiations the optic radiations arise from the lateral geniculate nucleus of the ventral thalamus. Fibers first travel anteriorly within the temporal lobe, medial to the medial wall of the anterior horn of the lateral ventricle, before turning acutely and continuously fanning out around the supero-anterior aspect of the anterior horn. The radiations, now lateral to the lateral ventricle, continue posteriorly to the occipital lobe. They course within the sagittal stratum, lying superficial to the tapetum, which forms the lateral wall of the lateral ventricle. The optic radiations terminate at the superior and inferior cortical margins of the calcarine fissure. Despite potential clinical benefit, accurate tractographic representation of the optic radiations proves difficult for most tractographic modalities. Algorithms may be unable to trace the gradated and acute trajectory of the optic radiations as they turn around the slanted superior aspect of the anterior horn. The close proximity of the optic radiations to the fluid-filled ventricles may also affect signal intensity, and close proximity to other sagittal stratum systems. Tractography of the auditory radiations is preferably suited to , and has been successfully implemented with nontensor techniques. Within the middle cerebellar peduncle, the corticopontine projections are arranged superiorly, with respect to the extrapontine projections, and project to all areas of the cerebellar cortex, Auditory Projections the auditory projections subserve transmission of auditory information from the medial geniculate nucleus to the primary auditory cortex. At this level the pathway decussates and continues to the contralateral cerebellum. Though they have been visualized using tensor-based methods,33 these pathways have received negligible attention in the literature and their hemispheric white matter trajectory, including decussation, remains obscure. They ascend through the ipsilateral pons, adjacent to the dorsolateral wall of the fourth ventricle and decussate to pass through the contralateral red nucleus within the midbrain. From here, they terminate within the ventrolateral nucleus of the contralateral thalamus. The thalamocortical projections are to all cortical areas via the internal capsule, however, specifically concerned with movement are those to the precentral cortical areas, which are postulated to be somatotopically arranged, mirroring the organization of the cortex,15 and which can be tractographically visualized. Corticospinal fibers subserve somatic motor function of the contralateral body half, following their decussation in the upper one-third of the medullary pyramids. A somatotopic arrangement of the corticospinal projections, mirroring the functional topography of the precentral gyrus was historically conjectured. These pathways have also been visualized and differentiated using tractographic means. The more radially oriented precentral fibers must traverse the centrum semiovale, a white matter area superolateral to the lateral ventricle, consisting of crossing projection, association, and commissural fibers. It subserves the consensual light reflex, connecting nuclei within the bilateral pretectal areas. Its multifunctional roles include cognition, perception, decision making, and learning. It can be grossly divided into three regions: the genu, body, and splenium; however, contemporary tractographic research has suggested alternative subdivisional arrangements based on its connectivity. As the bulk of callosal white matter is arranged perpendicularly to the majority of projection (superoinferior) and association (anteroposterior) bundles, tractography of the corpus callosum may be preferentially suited to tractographic methods unconstrained by crossing fibers; the study of Jarbo et al42 used diffusion-spectrum imaging to define callosal connectivity, finding predominant homotopic connection within the frontal, parietal, and occipital association areas, with minimal temporal connectivity. Commissural Fibers Commissural fibers are telencephalic white matter structures permitting interhemispheric communication. There are three generally accepted commissural systems: the anterior commissure, corpus callosum, and psalterium (see 24. The posterior commissure has not been extensively studied in humans and is therefore not classically included in descriptions. Anterior and Posterior Commissures the anterior and posterior commissures are compact telencephalic fiber pathways, crossing the midline, connecting gray- and white-matter structures within the hemispheres. Within each hemisphere, the lateral body bifurcates into anterior and posterior crura. The anterior crus passes within the medial orbitofrontal white matter to terminate within the olfactory bulb, anterior perforated substance, and anterior olfactory nucleus. The posterior crus continues superolaterally toward the temporal and occipital lobes. The temporal extension continues toward the temporal pole and terminates within the hippocampus and amygdala. The occipital extension merges with the sagittal stratum to terminate within the occipital cortex. In concordance with evolutionary theory, the human association systems demonstrate a greater degree of differentiation relative to nonhuman species. Studies into the cortical connectivity of association tracts are therefore paramount to anatomo-functional understanding. The "gold standard" technique of immunohistochemical tracing to define connectivity necessitates sacrifice of the study subject and is therefore limited to nonhuman species. Likewise, the limitations of human post mortem white matter dissection have been discussed above. Tractography potentially reconciles these differences, allowing human connectivity to be studied in vivo. Nevertheless, differences in data acquisition parameters, tractographic modality, and tracking methods have introduced significant variability between studies. Because of these issues, controversies persist regarding their anatomy and function. It lies deep to the cortico-cortical U-fibers and is the most superficial large white matter system. This lateralization is thought to underpin the evolution of complex language functionality unique to humans, particularly in the domains of phonological and semantic processing. The dorsal segment interconnects ventral precentral and caudal middle frontal gyri with caudal middle and inferior temporal gyri. The ventral segment connects the superior and rostral middle temporal gyri with the pars opercularis. The right-sided arcuate does not demonstrate the same extent of volumetric or connective differentiation; the ventral segment connects superior temporal gyrus with the pars triangularis. It assumes a "bow-tie" arrangement at its anterior and posterior extremities, interconnected by a compact stem. The inferior fronto-occipital fasciculus lies deep to the arcuate fasciculus within the white matter of the external and extreme capsules, with the external capsular portion traversing within the white matter of the temporal stem. At its frontal origins, the inferior fronto-occipital fasciculus lies dorsal to the uncinate fasciculus, with both systems traveling into the temporal stem together. Relevant to human evolution, this fascicle is not found within the subhuman primates, and along with other ventral fiber tracts is thought to subserve lexicosemantic processing among other complex functions. Its exact subdivision, connectivity, and lateralization in the literature have been subject to considerable debate; however, both tensor-48 and nontensor-based49 studies generally concur that it consists of superficial and deep layers, which can be further subdivided. Finally, though most groups agree upon its terminations within the frontal pole and occipital cortex, separate tractographic studies have demonstrated varying connectivity to dorsomedial and dorsolateral. It originates ventral to the inferior fronto-occipital fasciculus within the orbitofrontal cortex and frontal pole (see below) and terminates within the temporal pole. There is general consensus regarding its connectivity, with some exception; the majority of tractographic research has demonstrated bifurcating frontal connectivity with the medial and lateral orbitofrontal, rectus, and ventrolateral frontal gyri. Temporal connectivity is with the temporal pole, uncus, and parahippocampal gyrus. It connects the superior, middle, inferior, and fusiform temporal gyri to the cuneus, lingula, and occipital poles. It is thought to lie between the caudal extension of the arcuate fasciculus and the postcapsular portion of the inferior fronto-occipital fasciculus, approximating the lateral contour of the lateral ventricle during its posterior course. The existence of the inferior longitudinal fasciculus has been called into question, with suggestions that ventral temporo-occipital connectivity is in fact subserved by corticocortical U-fibers. It has been studied using both tensor and nontensor tractography, which have demonstrated it as lying within the white matter between the arcuate fasciculus and inferior fronto-occipital fasciculus, running obliquely, in a posterosuperior course to the latter. It is generally agreed that the middle longitudinal fasciculus connects superior temporal gyrus to the precuneus and cuneus.
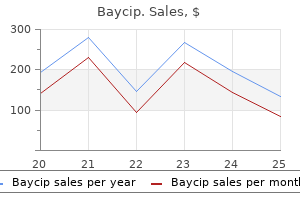
Neither the visual cortex nor the optic radiation is related to the surgical trajectory 92507 treatment code purchase 500 mg baycip, and therefore the risk of injury to these structures is minimal symptoms 5 weeks into pregnancy baycip 500mg purchase visa. Nonetheless medicine nobel prize 2015 quality 500 mg baycip, the surgeon should be aware of the location of the lateral geniculate body when opening the choroidal fissure symptoms 9 days post ovulation order line baycip. This approach may be an advantage for more successful seizure control and better neuropsychological and psychosocial outcome in patients with posteriorly located hippocampal sclerosis medicine 7 cheap 500mg baycip. With precise knowledge of surgical anatomy and microsurgical technique, many surgeons have achieved excellent results with the pterionaltranssylvian approach without visual field defects. As we gained more experience using this approach in tumor cases, however, we noticed that it is possible to remove the temporal pole. For example, the semisitting position needs special attention from the neurosurgeon, anesthesiologist, nurses, technicians, and the entire operating team. Surgical Considerations the mediobasal temporal structures, such as the amygdala, uncus, hippocampus, and parahippocampal gyrus, can vary considerably in size and form. Our experience suggests that the pterional transsylviantransamygdalar approach is superior to prevent injury to the temporal stem when compared to a standard temporal lobectomy. Furthermore, posterior transection of the hippocampusparahippocampal gyrus is generally done at the level of the posterior margin of the cerebral peduncle, where the P2P3 segment junction is located, at the level of the ascending tail of the hippocampus and 10 to 15 mm before the isthmus cinguli. Initial resection of parahippocampal gyrus directly discloses whole extent of hippocampus and faces surgical trajectory toward amygdala via its inferolateral axis. Such trajectory enables clear visualization of most superomedial border of amygdala as resected. The posterior portions of the hippocampus and parahippocampal gyrus can be removed through this approach, possibly allowing better seizure control, especially in patients with posterior hippocampal sclerosis. Furthermore, there is no danger of damage to the superficial and deep sylvian veins, the middle cerebral artery and its branches, and especially the temporal pole and temporal neocortex. In addition, patients with dominant temporal lobe epilepsy who are highly functional, or those whose preoperative Wada results suggest a risk of significant verbal memory loss with temporal neocortical resection, the selective procedure is the preferred operation. There is an increasing tendency for recommending surgical interventions to pediatric epilepsy patients in earlier ages. Seizure and memory outcome following temporal lobe surgery: selective compared with nonselective approaches for hippocampal sclerosis. In reply: the paramedian supracerebellartranstentorial selective amygdalohippocampectomy for mediobasal temporal epilepsy. Oper Neurosurg (Hagerstown) 2018;15 (3):E34E35 37 Selective Amygdalohippocampectomy 10. Selective subtemporal amygdalohippocampectomy for refractory temporal lobe epilepsy: operative and neuropsychological outcomes. Inferior temporal sulcus approach for amygdalohippocampectomy guided by a laser beam of stereotactic navigator. Subtemporal transparahippocampal amygdalohippocampectomy for surgical treatment of mesial temporal lobe epilepsy. The paramedian supracerebellar-transtentorial approach to the entire length of the mediobasal temporal region: an anatomical and clinical study. The connections of the amygdala and of the anterior temporal cortex in the human brain. Small petrosal approach to the middle portion of the mediobasal temporal region: technical case report. The insula and deep middle cerebral venous drainage system: Normal anatomy and angiography. The paramedian supracerebellar-transtentorial approach to remove a posterior fusiform gyrus arteriovenous malformation. The paramedian supracerebellar-transtentorial approach for a tentorial incisura meningioma: 3-dimensional operative video. The Vertebrate Visual System: Its Origin, Structure, and Function and Its Manifestations in Disease with an Analysis of Its Role in the Life of Animals and in the Origin of Man, Preceded by a Historical Review of Investigations of the Eye, and of the Visual Pathways and Centers of the Brain. A standardized protocol for the prevention of clinically relevant venous air embolism during neurosurgical interventions in the semisitting position. However, epileptogenic zone may frequently stretch beyond the anatomical boundaries of the lesion. Therefore, determining the extent of resection in lesional epilepsy patients is critical to optimize surgical outcome, and it may not always be feasible and certain compromises may be required in some cases. Therefore, the surgical strategy in lesional epilepsy patients is a multifaceted topic. Although there is consensus on critical significance of complete lesion resection, the importance of additional resection of adjacent cortex or the mesial temporal structures remains controversial. In this article, we will discuss the surgical strategies in children with lesional temporal epilepsy, mainly focusing on tumors and vascular malformations. The goal in neuro-oncological surgery is always total resection of the tumor when it is feasible. This is also relevant for tumor-related epilepsy cases with one significant difference; an equally important additional surgical target: the epileptogenic zone. These dual therapeutic goals can be achieved by determining both the causative relationship between lesion and seizures as well as the spatial relationship between lesion and epileptogenic zone. Although epileptogenic zone frequently corresponds to the cortex immediately adjacent to the lesion, it may also stretch beyond the anatomical boundaries of the lesion. Therefore, determining the extent of resection in lesional epilepsy patients is critical to optimize surgical outcome, and it might be quite challenging at times. Furthermore, reaching these goals may not always be feasible, and certain compromises may be required in some cases. Çataltepe et al11 reported that temporal tumor-related epilepsy patients constituted 40% of pediatric epilepsy surgery cases in their series. Among other commonly seen glioneuronal tumors are desmoplastic infantile astrocytoma, gangliocytoma or ganglioglioma, papillary glioneuronal tumor, and central neurocytoma. The factors effecting good outcome in epilepsy patients are not only dependent on the type of the lesion but also related to the location of the lesion as well as the extent of the epileptogenic zone and the area of resection. It should be defined based on the location, extent of the lesion, and epileptogenic zone, as well as the histopathological diagnosis. Determining the optimal surgical strategy in these cases is a challenging task and involves some controversy. Lesionectomy alone, lesionectomy with resection of the epileptogenic zone, or lesionectomy with resection of the ipsilateral mesial structures all have their advocates in discussions about the appropriate surgical approaches in these cases. Mechanism of Seizures the epileptogenic mechanisms involved in lesion-related epilepsy are not clear. Several mechanisms, including direct pressure and irritation of the cortical tissue, gliotic changes and disruption of vascular structures of the surrounding cortex, morphological alterations at the cellular level, changes in inhibitory and excitatory neurotransmitter levels, and denervation hypersensitivity have been proposed to play a role. Developmental tumors may even have intrinsic epileptogenicity, because they are frequently associated with cortical dysplasia and contain cells with a rich array of neurochemical properties, including altered inhibitory and excitatory local circuits. Brain tumors associated with epilepsy are often located in the cortex or in graywhite matter junction. When the lesion is located in the temporal lobe, its direct or indirect effects on hippocampus may cause seizures. The lesion location may interfere with cortical afferents and efferents and lead to relative deafferentation of a certain cortical area that has intrinsic epileptogenicity. Small hemorrhages in and around the tumors also cause hemosiderin deposits, which are highly epileptogenic. There are several conditions for optimizing seizure control in children with lesional epilepsy. Second, the epileptogenic zone should be contained within the resected area, and finally the remaining cortical and subcortical areas should not develop independent seizures after surgery. Unsuccessful results in lesional epilepsy surgery are frequently related to incomplete resection of the lesion or epileptogenic zone or the presence of additional or secondary epileptogenic foci. Lesion Lesionectomy alone is probably the most commonly used surgical approach in lesional epilepsy cases. Although there is a wide consensus regarding the significance of total tumor resection for good seizure control, the results of this surgical approach in the published epilepsy series are quite different. Khajavi et al44 reported that seizure-free outcome was only correlated with the extent of tumor resection but not with additional resection of the surrounding cortex. Conversely, Jooma et al45 reported that epilepsy patients who underwent lesionectomy procedure alone had a significantly lower seizure-free outcome rate compared with patients who had additional cortical resections of the adjacent epileptogenic zone. Sugano et al46 reported that after complete resection of mass lesions, they still found residual spikes in the mesial structures in up to 86% of the patients and recommended additional resection in these areas for better seizure control. Surgical Strategy Although the histological subtype of the lesion is always the major factor influencing clinical outcome in any given patient, 38 Surgical Management of Lesional Temporal Lobe Epilepsy 367 Epileptogenic Zone the first step in the planning lesional epilepsy surgery is to define the relationship between the localization of the seizures and the location of the lesion. If the clinical and electrophysiological characteristics of the seizures are fully correlated with the location of the lesion, then the next step would be to determine whether the epileptogenic zone exceeds the anatomical boundaries of the lesion. The surgical resection strategy is then designed based on lesion location, the extent of the epileptogenic zone, and the relative position of adjacent eloquent cortex. Mesial Temporal Structures It has been generally assumed that the primary epileptogenic activity arises in the vicinity of the lesion. However, the situation may be more complicated if the lesion is located in the temporal lobe because secondary involvement of the mesial temporal structures in seizure generation is not rare with temporal lobe lesions. It is well known that the hippocampus is a very epileptogenic structure and may even generate a separate focus for secondary epileptogenesis in these cases. This is a legitimate concern because it is possible that epileptogenic zone may not be limited to cortex adjacent to the lesion itself but may also include the mesial temporal structures. If that is the case, then resection of the mesial temporal structures along with the lesion may be needed to obtain a seizure-free outcome. The tumor was resected along with anterior temporal lobe and mesiotemporal structures. Conversely, if mesial temporal structures are not directly in the lesional zone, then the risks and benefits of the resection of mesial temporal structures should be assessed carefully. Well-defined histological and electrophysiological changes in the hippocampus are very important to determine the most appropriate surgical approach in these cases. Therefore, it may be very difficult to appreciate pathological changes, such as neuronal loss, in the hippocampus of the patients with temporal neocortical lesions using available imaging techniques. Even if the hippocampus demonstrates epileptogenic properties by intracranial monitoring techniques, imaging studies may not be grossly abnormal. Furthermore, the presence of mesial temporal onset of seizures was not associated with hippocampal neuronal loss in histological examination. Mihara and Baba48 identified independent ictal discharges arising from ipsilateral mesial structures in 47% of the patients with neocortical temporal lesions and concluded that there is independent epileptogenicity of both neocortical lesions and ipsilateral mesial structures in this subgroup of patients. Similarly, Fried et al15 published their results of 41 temporal tumors and stated that seizure-free outcome rate was 87% without any correlation with the extent of hippocampal resection. Two other series showed similar seizure control rates without resecting hippocampus of the epilepsy patients with occult vascular malformations in temporal lobe. Currently, there is no clear-cut evidence in relevant literature to devise an optimal strategy regarding resection of the mesial structures along the temporal lobe lesions. The presence of radiologically normal-appearing mesial structures along with a temporal lobe lesion presents an additional challenge because even if the mesial structures are radiologically normal appearing, they may still be histologically abnormal and capable of generating independent seizures. This may be related to abnormal synaptic reorganization of hippocampus that may be induced by seizures propagating from temporal neocortical lesions. The critical question is whether the epileptogenic capacity of the ipsilateral radiologically normal-appearing hippocampus would still continue after resection of the temporal tumor. Another avenue to assess the ipsilateral radiologically normal-appearing hippocampus is its functional status. Impaired performance on the Wada test correlates well with the extent of hippocampal neuronal loss according to Morioka et al. Conversely, if these test results show well-functioning mesial structures, then mesial structures might be preserved. Otsubo et al55 reported dual pathology in 54% of patients with epileptogenic ganglioglioma. Conversely, we found a dual pathology rate of 8% in our pediatric temporal lobe tumor series. Li et al56 demonstrated that seizure-free outcome rate was significantly low if only one of the lesions was removed in patients with dual pathology, but it was quite high (73%) when both sclerotic hippocampus and the lesion were removed. Morris et al57 also recommend resection of sclerotic hippocampus along with the temporal tumor if imaging studies are correlated with hippocampal sclerosis. This decision needs to be tailored case by case based on the electrophysiological findings and functional status of the mesial temporal structures. The accessibility of the lesion, its relationship to eloquent cortex, and mesial structures are all critical components in determining the surgical approach and extent of the resection. We prefer to classify temporal lobe lesions, mainly tumors, in three groups based on their location within the temporal lobe as we described previously. Basal temporal lobe tumors: basal part of inferior temporal gyrus and fusiform gyrus. Therefore, low-grade mesial temporal lobe tumors can be classified separately from temporal neocortical tumors. Conversely, separation between basal and lateral temporal tumors is less precise, and tumors extending to both sides are not rare. However, surgical access to basal temporal tumors has its unique challenges, and it is still helpful to use this classification to define the surgical approach and its rationale more clearly. We define our approach based not only on the tumor location in the temporal lobe but also on being in the dominant or nondominant hemisphere to provide a framework to discussion. It should be emphasized that the location-based description of our surgical approach is defined simply to provide a general perspective to our discussion and certainly should not be considered as a strict guideline. Note that collateral sulcus (arrow) is well preserved without any tumor involvement in the fusiform gyrus. The critical part of the decision-making process in these cases is defining the spatial relationship between the epileptogenic zone and the lesion itself.
Order discount baycip. Minecraft Mods: MONOBLOCKS MOD (1.7.10).
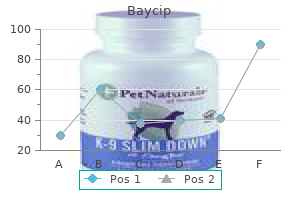
In children with an appropriate comprehension level treatment bacterial vaginosis buy generic baycip from india, this may be accomplished by using a series of simple picture sequences to teach the steps symptoms 10 dpo order baycip online pills. As an example treatment hepatitis c discount baycip 500mg on line, the modified sequence in children following airway reconstruction consists of five steps: (1) coughing to clear prior to accepting food or liquid treatment kidney cancer baycip 500 mg buy amex, (2) oral holding of the bolus prior to transferring it for the swallow treatment zenkers diverticulum buy genuine baycip online, (3) holding the breath before and during transfer for the swallow, (4) holding the breath during the swallow, and (5) gentle coughing to clear following the swallow. The use of a thickened fluid bolus has been found to assist patients in maintaining control of the bolus while learning the sequence. Once the sequence is learned, introduction of small presentations of easily managed solids as well as single sips of liquid may be introduced. Box 383 the cough serves to expel food material that has inadvertently fallen into the larynx. Head rotation toward the paralyzed side has been shown to close off this side from the bolus pathway, thereby improving clearance. These exercises include active range of motion, stretching, strength training, passive exercises, and sensory applications. Although techniques and tools for incorporating oral motor exercises into the dysphagia treatment plan for both infants and children are available, empirical evidence to support the effectiveness of specific oral motor exercises and exercise protocols is scant, with few controlled studies reporting dose, frequency, and subsequent outcomes across pediatric populations. In addition, methods for the measurement of the tone, weakness, or strength of oral motor and pharyngeal musculature are not widely available. Box 384 Sensory treatment strategies may include the use of modalities such as cold, vibration, or electrical stimulation in conjunction with active exercises. Verbal directions such as "push as hard as you can with your tongue against the roof of your mouth while you swallow," "swallow hard with all of your muscles," and "squeeze my hand as you swallow hard" can be used by the clinician to help the child exert some volitional pressure against the palate and at the tongue base. Approaches to treatment primarily comprise alterations in positioning, the use of sensory input to facilitate motor action, the use of specific feeding strategies and specialized equipment, and bolus modification using differing food textures and liquid viscosities. The therapist and the family work together to develop an overall treatment strategy appropriate for each patient. In developing individual strategies, the therapist must be sensitive to socioeconomic and cultural factors that may be a barrier to carrying out the plan in the home environment. Proper alignment of the head, neck, trunk, and extremities facilitates coordinated oral motor movements and the respiratory support needed for safe swallowing. The optimal position for infant feeding includes the head and neck being in a neutral to slightly flexed position, with neutral alignment of the trunk and orientation of the head and extremities about the body midline. Input from an occupational or physical therapist regarding underlying muscle tone and the implications for positioning is often advantageous. Variations in infant positioning may assist in facilitating coordination of respiration and swallowing during feeding. For example, the rationale for using side-lying positioning during feeding is to facilitate midline positioning of the upper and lower extremities, increase postural stability, and decrease arching of the back. Such positioning protects the airway during respiration by using gravitational forces to direct the flow of milk away from the airway. Descriptions of side-lying to relieve upper airway obstruction with feeding are primarily based on clinical expertise, with the rationale that the traditional cradle-hold position may allow gravity to pull the tongue into the pharynx. In contrast, side-lying or prone positioning may minimize the gravitational pull on the tongue. Evidence for using sidelying positioning during feeding in preterm infants is mixed. Some investigators have found that it promotes better regulation of breathing and allows infants to maintain physiologic stability throughout feeding. Others have reported that side-lying does not make an appreciable difference in the duration of time necessary to achieve full oral feedings in comparison to other positioning options. Excessive head and neck hyperextension is counterproductive to safe and efficient feeding, and slight modifications to help align the head and neck to the trunk are often necessary. Given the degree of impairment in craniocervical postural control in some patients, positioning with the head in the midline or with head flexion may not be possible or practical. Specialized adap- 472 Pediatric dysPhagia: etiologies, diagnosis, and ManageMent tive seating may therefore be necessary to establish and maintain individualized optimal positioning for feeding. The use of this approach was first proposed for the treatment of abnormal movement patterns in patients with neuromuscular disorders such as cerebral palsy. Specific sensory input is selected to influence exteroceptive (contact) sensations to assist with modifying the functional adequacy of oral movement patterns. The treatment plan incorporates optimal positioning for feeding, provision of oral tactile input prior to feedings, and hands-on interventions during a feeding activity. Components of the sensorimotor therapeutic approach have been used in clinical practice, integrating five basic treatment principles described by Sheppard. Therapeutic strategies are chosen to target a specific neuromuscular impairment following assessment of respiratory support for feeding, postural control, and oral motor manipulation skills. Optimal postural alignment and positioning is essential, with external assist provided as needed to maintain upright positioning with appropriate support for the feet and hips, and to maintain stability of the upper extremities, the shoulder girdle, and the neck and head. Treatment strategies are implemented prior to or during a functional feeding task - for example, working on tongue lateralization with presentation of food rather than within the context of an isolated tongue lateralization exercise. Consider the developmental sequence for which skills are typically acquired; for example, anteroposterior tongue motion for transfer of purees occurs prior to the emergence of the lateral tongue motion needed for manipulation of foods with 476 Pediatric dysPhagia: etiologies, diagnosis, and ManageMent increased textures and eventual biting and manipulation of solids. Continue to monitor the progress throughout treatment, with advancement of tasks as progress is demonstrated, or modification of tasks if regression or lack of progress is noted. Sensorimotor Interventions in Preterm Infants Neurologic immaturity, respiratory instability, immaturity of bowel function, abnormalities in muscle tone, and accompanying complex medical issues put premature infants at risk for feeding problems and frequently delay the introduction of oral feeding. Examples of non-nutritive oral activities include the use of perioral stimulation, intraoral stimulation to the gums and tongue, exposure to pacifiers to encourage non-nutritive sucking, oral exploration of oral sensory toys, and oral care and tooth-brushing. A wide array of nipples, bottles, cups, and utensils are also available to assist with progression to nutritive treatment. The initial sensorimotor feeding assessment should include observation of the types of feeding equipment already in use, as well as exploration of possible alternative options. For example, infants with an underlying muscle tone abnormality may present with a retracted tongue configuration that precludes efficient sucking. The choice of pacifier or nipple should meet the goal of providing proprioceptive input to the tongue to promote a more anterior position. This choice should also provide a sufficient contact area between the tongue and nipple to aid in central grooving of the tongue for efficient sucking. Non-Nutritive Oral Stimulation Non-nutritive stimulation techniques are used in preterm infants as well as in infants with medical conditions that require supporting the development of sensorimotor skills for oral feeding. The rationale for non-nutritive oral stimulation is that heightened sensory awareness facilitates motor action, helps to prevent development of oral aversion, and assists with the transition to nutritive sucking by promoting the development of the oral motor skills necessary to transition to oral feeds. For infants who are non-oral feeders, frequent opportunities for non-nutritive sucking using a pacifier may help to establish oral motor patterns needed for the eventual transition to oral feeding. Whereas some are suitable for a wide age range, others are designed for specific age ranges (eg, 6 months and younger, 6 to 18 months). Single piece pacifiers are made from a single molded piece of plastic, silicone, or latex. As in other areas, empirical research on the use of pacifiers reveals a lack of clarity as to their positive and negative effects. In preterm infants, decreased length of hospital stay and earlier transition to bottle feeds have been documented. The four primary characteristics that should be considered in the selection process include shape, size, consistency, and size and type of nipple hole. The shape of the nipple has been shown to have a significant impact on the mechanics of sucking. In contrast, a wide-base nipple with a bulblike end may encourage forward tongue thrusting and tongue protrusion during sucking, which decrease overall sucking efficiency. The use of a narrow, round nipple may decrease the tongue protrusion pattern and promote anteroposterior movements, thereby improving overall sucking efficiency. Adequate contact between the nipple and the tongue is needed for efficient sucking. The consistency of the nipple refers to its degree of firmness and compressibility. The infant must be able to exert enough sucking pressure to compress the nipple for extraction of fluid. Generally, a nipple with a soft consistency requires less compression effort and yields a higher flow compared with a nipple with increased firmness that requires more compression effort; however, studies of flow rates indicate variability among different nipple types. The variability that may exist between nipple types should be considered by the clinician during the selection process. Bottles A wide variety of bottle systems are available and these generally consist of several components, including a nipple, the collar that positions the nipple on the bottle, and a travel cover for the nipple. Many bottle brands offer several compatible nipples with differing flow rates appropriate for chronologic age. Generally, a slower flow is appropriate for young infants, whereas a faster flow is appropriate for older, more efficient feeders. Bottles are typically made from glass, plastic, or stainless steel, and may have unique internal designs. For example, some contain venting systems designed to minimize the amount of air that the infant swallows while feeding, whereas others have special silicone sleeves designed for easy gripping as the baby learns to hold the bottle for self-feeding. As discussed in Chapter 39, specialty bottles are also made for infants with cleft palate, as these patients cannot generate negative intraoral pressure or compression of the tongue against the palate. Cups with valves or spill-proof features help to minimize spills as the baby learns to drink from a cup; however, the baby is still using a sucking motion to obtain the fluid, as opposed to learning to manage the flow of liquid delivered via cup. Utensils the choice of utensils for feeding treatment is based on the developmental level and the oral motor patterns of the patient. The spoon options include those that are made from soft plastic or silicone material, having varied bowl shapes. Specific designs are available for use during the self-feeding learning period, including the weighted spoon and angled spoon. Oral Appliances Views among practitioners vary in regard to the use of oral appliances to aid feeding. For example, the use of feeding obturators to facilitate feeding in infants born with a cleft palate is not advocated in all centers, as discussed in Chapter 39. Reducing the bolus volume by offering a defined volume of fluid from a sip-control cup, modifying textures to Cups A plethora of available cups are on the market. Cup characteristics include a screw-on or snap-on lid with spill-proof internal valves, free-flowing spouts, soft pliable spouts, open cups with handles, cups with internal straws, and cups with weighted bases designed to keep the cup upright to avoid spills. Clear or transparent cups permit visualization of the level of fluid inside the cup. The rationale for this strategy is that the reduction of flow rate may facilitate oral control. It also provides increased time for patients to achieve airway closure, and thus airway protection, during swallowing. The use of starch-based or gum-based thickening products or of natural foods such as baby rice cereal, pureed fruit, and yogurt are the primary methods of increasing viscosity. The options for thickening liquid and considerations pertaining to the use of these options are summarized in Tables 384 and 385. As discussed, although altering liquid viscosity is a frequently used practice in pediatrics, evidence as to the efficacy of thickening fluids is limited. The use of thickened fluids may allow an infant or child to forgo or minimize tube feedings and may facilitate airway protection during swallowing. Nevertheless, potential physiologic impacts of this practice, such as the nutritional implications of increased caloric density, cannot be ignored. For example, using rice cereal as the thickening agent may put the infant at risk of ingesting more than the recommended amount of some nutrients, such as iron. Commercial thickening agents bind to water, preventing its absorption and leading to potential dehydration unless adjustments are made in free water intake. Box 385 the term "free water" refers to water that is available to be absorbed from the digestive tract. The viscosity of liquid varies based on the type of product used, the way the product is prepared, and the base liquid characteristics. For example, there are special considerations for breastmilk, as the amylase in human milk breaks down rice cereal and starch-based thickeners, transforming the fluid back to its original thin viscosity. The use of gum-based thickeners adds volume but no calories, thus requiring the infant to ingest more fluid volume to achieve the same caloric and nutrient intake. With this in mind, multidisciplinary clinical practice guidelines should be followed for the use of thickened liquids in pediatric patients. Clinicians should be aware of their institutional guidelines for product use and precautions. Moreover, other compensatory strategies may be used in place of thickened liquids and, in many cases, should be considered. Psychosocial and behavioral approaches to treatment Although the underlying medical condition that contributes to feeding and swallowing issues may eventually resolve, feeding avoidance and maladaptive mealtime behaviors in infants and children often persist. Persistent feeding problems often evoke stress and anxiety, both in the child and in caretakers. Behavioral interventions to restructure mealtime interactions and to ultimately increase oral intake are thus a vital component of the treatment process. Structure and support are provided by the clinicians to ensure that caregivers successfully use recommended strategies and that these strategies are applied in the home and other settings. Standardization of Viscosity Nomenclature A lack of standardized nomenclature regarding food texture and drink thickness has long been a major obstacle to research in dysphagia. Advancements in clinical research require agreement on a single standardized terminology, and international efforts to move in this direction (International Dysphagia Standardization Initiative) are described in Appendix 382. Integration of behavioral interventions in the context of multidisciplinary feeding treatment for oral sensorimotor and nutritional issues has been shown to be beneficial in children with complex feeding problems. Children with depressed appetite may benefit from appetite stimulants such as Periactin.
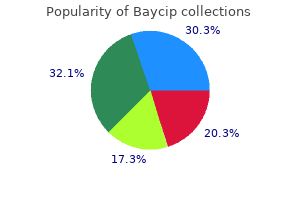
A technique preserving posterior insular cortex below the superior peri-insular sulcus has been reported; however this may result in leaving behind residual lesion and poor outcome in one of three patients operated with this technique treatment whiplash order on line baycip. A high index of suspicion for insular epilepsy is important medicine 003 order baycip mastercard, and good working knowledge of the insularperisylvian anatomy is imperative to safely navigate the intricate anatomy of the perisylvian region medicine yeast infection cheap baycip generic. Insularopercular epilepsy represents a challenging form of focal pediatric epilepsy for many reasons medicine hat baycip 500mg without a prescription. The typical subjective semiology of insular epilepsy may not be reported in younger children treatment yeast uti generic baycip 500mg line. Malformations of cortical development are the underlying pathological substrate in the majority of cases, and epileptogenic zone is almost universally multilobar, involving the insula and at least one other cerebral lobe. Despite these challenges, resective surgery offers good seizure freedom rates at low permanent morbidity profile, and the available evidence suggests that many patients experience cognitive improvement postoperatively. In upcoming years, refinement of presurgical noninvasive tests will improve our ability to identify and evaluate pediatric insular epilepsy to optimize patient selection and surgical results. Neuropsychological Outcome In spite of the cognitive functions attributable to the insula and the potential impact on the developing brain, there is very limited data on the impact of insulectomy on neurocognitive function or social or emotional problems, particularly in children. Many patients will experience improvements in cognition following insular epilepsy surgery. Dylgjeri et al reported neuropsychological improvement in 90% of patients undergoing insular epilepsy surgery, however, behavior was only improved in 20%. Clinical manifestations of insular lobe seizures: a stereo-electroencephalographic study. Perisylvian, including insular, childhood epilepsy: presurgical workup and surgical outcome. Stereotactic depth electrode investigation of the insula in the evaluation of medically intractable epilepsy. Successful surgical treatment of insular epilepsy with nocturnal hypermotor seizures. Indications, technique, and safety profile of insular stereoelectroencephalography electrode implantation in medically intractable epilepsy. Magnetic resonance imaging-guided laser interstitial thermal therapy as treatment for intractable insular epilepsy in children. Insular epilepsy masquerading as multifocal cortical epilepsy as proven by depth electrode. Nocturnal hypermotor seizures, suggesting frontal lobe epilepsy, can originate in the insula. Mental retardation in pediatric candidates for epilepsy surgery: the role of early seizure onset. Health-related quality of life before and after pediatric epilepsy surgery: the influence of seizure outcome on changes in physical functioning and social functioning. Surgical strategy to avoid ischemic complications of the pyramidal tract in resective epilepsy surgery of the insula: technical case report. Circuitry and functional aspects of the insular lobe in primates including humans. Three systems of insular functional connectivity identified with cluster analysis. Probabilistic tractography recovers a rostrocaudal trajectory of connectivity variability in the human insular cortex. Beyond the tripartite cognition-emotion-interoception model of the human insular cortex. A link between the systems: functional differentiation and integration within the human insula revealed by meta-analysis. Surgical pathologic findings of extratemporal-based intractable epilepsy: a study of 133 consecutive resections. Operculo-insular epilepsy: scalp and intracranial electroencephalographic findings. Safety and usefulness of insular depth electrodes implanted via an oblique approach in patients with epilepsy. Surgical techniques for investigating the role of the insula in epilepsy: a review. The hybrid operculo-insular electrode: a new electrode for intracranial investigation of perisylvian/insular refractory epilepsy. Risks and benefits of invasive epilepsy surgery workup with implanted subdural and depth electrodes. Part 1: surgical anatomy and morphometric analysis of the transsylvian and transcortical approaches to the insula. Anatomical configuration of the Sylvian fissure and its influence on outcome after pterional approach for microsurgical aneurysm clipping. Epilepsy surgeries requiring an operculoinsular cortectomy: operative technique and results. Seizures outcome after stereoelectroencephalography-guided thermocoagulations in malformations of cortical development poorly accessible to surgical resection. Laser ablation as treatment strategy for medically refractory dominant insular epilepsy: therapeutic and functional considerations. Neurology 2008;71(21):17191726 40 Surgical Management of InsularOpercular Epilepsy in Children 86. Responsive cortical stimulation for the treatment of medically intractable partial epilepsy. Neuropsychological performance before and after partial or complete insulectomy in patients with epilepsy. Decision-making impairments following insular and medial temporal lobe resection for drug-resistant epilepsy. J Clin Neurosci 2017;43:121125 403 41 Summary Focal Cortical Dysplasia: Histopathology, Neuroimaging, and Electroclinical Presentation Olesya Grinenko and Imad M. Seizures are usually frequent, highly stereotyped, and commonly manifest early in life. Type Ia is characterized by isolated architectural disorganization, while type Ib is defined as architectural abnormality intermixed with giant, immature neurons (but not dysmorphic neurons). In the pediatric population, it is critical to repeat the study, especially in children younger than 3 years, as brain myelination continues after birth and some lesions can become visible only after myelination is complete. These spikes could be part of network-dependent propagation patterns and therefore their localization significance is questionable. Time of seizure onset can help in some cases, although it highly depends on electrode positions. Visual characteristics of the ictal patterns also may be identical in the epileptogenic zone and regions of propagation. These include: (1) measurement of changes in energy ratio between fast and slow activities in relation to time of seizure onset ("epileptogenic index");66 (2) co-localization of fast activity with slow polarization shift and voltage depression;64 and (3) support vector machinebased classifier identifying specific timefrequency pattern. Seizures are usually frequent, highly stereotyped, and commonly manifest early in life (in the majority of patients before 5 years of age). Seizures commonly respond to antiepileptic medications at the onset of the disease or during its course as epilepsy remits for several years, but eventually become pharmacoresistant. Epileptogenicity arising from the primary visual cortex leads to complaints of colored circles or twinkling stars in one of the visual field quadrants, 79 while ictal epileptic activation of the postcentral gyrus is associated with tingling sensation in one part of the body (commonly hand or arm), and a primary motor cortex activation leads to clonic jerks that spreads somatotopically ("jacksonian march"). If an epileptogenic lesion is located in an association cortex, clinical semiology is typically expressed following the ictal involvement of multiple brain areas. The pattern of activation is commonly driven by physiologicalanatomical connections (subcortical intralobar, interlobar, and/or interhemispheric). The clinical epilepsy phenotype could be West syndrome or LennoxGastaut syndrome. Less commonly, it presents as severe epilepsy with multiple spike foci81 or Ohtahara syndrome. For example, it can initially present as West syndrome and progress to LennoxGastaut syndrome. Despite generalized clinical and electrographic characteristics, epilepsy surgery is highly effective in these cases. Moreover, shorter epilepsy duration before surgery increases the chance for improved development. Concordance of the data allows for surgical planning, but only after establishing anatomical relationships between functional and epileptogenic cortices. In these cases, additional electrocorticographic and functional mapping may be needed. In other patients, phase 2 enables the formulation of strong hypotheses for the planning of intracranial studies (phase 3). Presurgical evaluation has four essential steps: · Confirmation of epilepsy diagnosis and the exclusion of genetic and metabolic causes. The first scenario is the most desirable and leads to the greatest rate of success in postresection seizure control; it predicts seizure freedom in 60 to 80% of the children. For these reasons, invasive recordings should not be performed if clear/ testable hypotheses cannot be generated. In the last scenario, a patient is excluded from surgical treatment based on the results of phase 1, phase 2, and phase 3 evaluations. Further medical management and neuromodulation techniques such as vagus nerve stimulation, deep brain stimulation, and responsive neurostimulation should be tried (see Guerrini et al107 for review). Clinical history: 17-year-old right-handed male who presented with focal drug-resistant epilepsy since the age of 9 years. All seizures were stereotyped and would last about 30 seconds with frequency of up to 20 per day. Ictal onset pattern consisted of mixed frequency and amplitude spiking in the left frontal region associated with rhythmical delta activity over the left fronto-temporal and vertex regions. A patient management discussion led to the proposal of an anatomo-electro-clinical hypothesis pointing to the left frontal lobe: prefrontal, frontopolar and mesial frontal regions. Efforts in epilepsy prevention in the last 40 years: lessons from a large nationwide study. Clinical characteristics in focal cortical dysplasia: a retrospective evaluation in a series of 120 patients. Interobserver and intraobserver reproducibility in focal cortical dysplasia (malformations of cortical development). Prospective magnetic resonance imaging identification of focal cortical dysplasia, including the non-balloon cell subtype. Electro-clinical and imaging characteristics of focal cortical dysplasia: correlation with pathological subtypes. Temporal lobe epilepsy and focal cortical dysplasia in children: A tip to find the abnormality. Blurring in patients with temporal lobe epilepsy: clinical, high-field imaging and ultrastructural study. A distinct variant of focal cortical dysplasia type I characterised by magnetic resonance imaging and neuropathological examination in children with severe epilepsies. Standard magnetic resonance imaging is inadequate for patients with refractory focal epilepsy. The value of repeat neuroimaging for epilepsy at a tertiary referral centre: 16 years of experience. Histopathological correlates of epileptogenicity as expressed by electrocorticographic spiking and seizure frequency. Epileptogenicity of focal malformations due to abnormal cortical development: direct electrocorticographic-histopathologic correlations. Ictal patterns of neocortical seizures monitored with intracranial electrodes: correlation with surgical outcome. Local and remote epileptogenicity in focal cortical dysplasias and neurodevelopmental tumours. Seizure-onset patterns in focal cortical dysplasia and neurodevelopmental tumors: Relationship with surgical prognosis and neuropathologic subtypes. Language cortex representation: effects of developmental versus acquired pathology. Reorganization and stability for motor and language areas using cortical stimulation: case example and review of the literature. Surgical treatment of pediatric focal cortical dysplasia: Clinical spectrum and surgical outcome. Focal malformations of cortical development: a most relevant etiology of epilepsy in children. The surgically remediable syndrome of epilepsy associated with bottomof-sulcus dysplasia. Focal cortical dysplasia type 1b as a cause of severe epilepsy with multiple independent spike foci. Early seizure onset and dysplastic lesion extent independently disrupt cognitive networks. Neurology 2013;81(8): 745751 41 Focal Cortical Dysplasia: Histopathology, Neuroimaging, and Electroclinical Presentation 85. Neuropathological spectrum of cortical dysplasia in children with severe focal epilepsies. Correlating magnetoencephalography to stereo-electroencephalography in patients undergoing epilepsy surgery. Epilepsy surgery in children: evaluation of seizure outcome and predictive elements. Outcome of surgery in children with focal cortical dysplasia younger than 5 years explored by stereo-electroencephalography. Predictive factors of surgical outcome in frontal lobe epilepsy explored with stereoelectroencephalography.
References
- Fouque F, Brivet M, Boutron A, et al. Differential effect of DCA treatment on the pyruvate dehydrogenase complex in patients with severe PDHC deficiency. Pediatr Res 2003;53:793.
- Kovacs GT, Krins AJ. Female sterilisations with Filshie clips: what is the risk failure? A retrospective survey of 30,000 applications. J Fam Plann Reprod Health Care. 2002;28(1):34-5.
- Stewart C, Haitsma I, Zador Z, et al. The new Licox combined brain tissue oxygen and brain temperature monitor: assessment of in vitro accuracy and clinical experience in severe traumatic brain injury. Neurosurgery. 2008;63(6):1159-1164; discussion 1164-1155.
- Keyes M, Schellenberg D, Moravan V, et al. Decline in urinary retention incidence in 805 patients after prostate brachytherapy: the effect of learning curve? Int J Radiat Oncol Biol Phys 2006;64(3):825-834.
- Sloan MA, Duh S-H, Mayder LS, et al. Marijuana and the risk of stroke. Stroke 2000;30:57.
- Kaefer M, Diamond D, Hendren WH, et al: The incidence of intersexuality in children with cryptorchidism and hypospadias: stratification based on gonadal palpability and meatal position, J Urol 162(3 Pt 2):1003n1006, discussion 1006n1007, 1999.
- Janjan N, Miller M, Schusterman MA. Therapeutic principles and options in radiation oncology. Plast Reconstr Surg 1995;96:1463-1473.
