
Detrol
| Contato
Página Inicial
Lucy Kean DM FRCOG
- Consultant Obstetrician Subspecialist in Maternal and
- Fetal Medicine, University Hospitals, City Campus,
- Nottingham
They are responsible for 21% of perinatal mortality and the outcome may involve physical and/or mental disability treatment 21 hydroxylase deficiency cheap detrol 2 mg on-line. Most congenital abnormalities are in low-risk patients with uncomplicated pregnancies treatment depression buy detrol 2 mg cheap. Prenatal identification of problems allows decision-making for timing medicine 031 order detrol 1 mg online, mode medicine ball abs proven 4 mg detrol, and place of delivery; meeting the neonatal team; ongoing fetal surveillance; time for the parents to come to terms with having an affected child; and in cases in which the problem would have a major impact on the child symptoms high blood sugar discount detrol 4 mg, termination of pregnancy may be offered. These are not routinely carried out unless there is bleeding, pain, or hyperemesis gravidarum (to exclude a molar pregnancy or twins). To date a pregnancy, crownrump length between 6 and 12 weeks is most accurate-the growth is constant across the population. Taking the 99th percentile as a cut off for cardiac screening enables 33% of heart abnormalities to be detected antenatally. Of all chromosomally normal fetuses (euploid) with significant nuchal thickening, 7090% have normal outcome, 2. Obstetrics Anomaly scan requirements · Skull shape and internal structures including the cerebellum, ventricular size, and nuchal fold · Spine in longitudinal and transverse views · Abdomen for shape and content at the level of the stomach, kidneys, umbliicus/abdominal wall, and bladder · Arms and legs for three bones and a hand or foot · Heart in four-chamber view, with outflow tracts, and lungs · Face and lips. Some anomalies have better survival rates than others and counselling must be supportive and informative no matter what the decision. Soft markers are findings on the anomaly scan that are in themselves of little significance, but are slightly more common in chromosomally abnormal fetuses. Others include 2-vessel umbilical cord, echogenic intracardiac foci and mild renal pelvic dilatation. Scans should be at least 2 weeks apart and used when there is increased risk of growth abnormality eg previous growth restriction, pre-eclampsia, measuring small for dates. In an unselected population, it has not been shown to be of value but it is useful in high-risk pregnancies. High resistance increases risk of maternal pre-eclampsia and fetal growth restriction and requires extra maternal and fetal surveillance during pregnancy. High resistance indicates placental failure, and these fetuses are at higher risk of intrauterine death. In absent or reversed end-diastolic flow, delivery by caesarean section should be considered, depending on gestation. Dopplers of fetal vessels (middle cerebral artery and ductus venosus) may be used for gestations <32 weeks to time delivery. A risk of 1:150 or less is high risk and the woman is offered invasive testing eg amniocentesis. Prevalence increases 35 years 1:380 with increasing maternal age, and most occur secondary to non-disjunction of chromosome 21 40 years 1:110 at meiosis. Features include microcephaly, holoprosencephaly, exomphalos and cleft lip and palate. It achieves detection rates of 90% of all aneuploides, 86% trisomy 21, and higher for trisomy 18 and trisomy 13. Use between 15 weeks + 0 days and 20 weeks + 0 days, so useful for women presenting in the 2nd trimester. Karyotyping takes 2 days, enzyme and gene probe analysis 3 weeks, so termination for abnormality is earlier, safer, and is done before the pregnancy is apparent, compared with amniocentesis. Amniocentesis is undertaken from 16 weeks onwards and involves the aspiration of fluid containing fetal cells shed from skin and gut. There are good data to show that detection of trisomy 18 and 21 have sensitivity and specificity rates approaching 100%. Increased venous distensibility and pelvic congestion predispose to haemorrhoids and varicose veins. Cigarettes and spices should be avoided, cold, small meals, and antacids and H2- receptor antagonists may be used. Treatment Admit to hospital if unable to keep anything down despite oral anti-emetics, for rehydration and correction of metabolic disturbance. I was admitted 5 times for fluid rehydration and that was whilst taking 4 different types of anti-emetics. I had a MalloryWeiss tear at 7 weeks and developed hyperemesis-induced hyperthyroidism. There are increased risks of painful crises, perinatal mortality, premature labour, and fetal growth restriction. Most prevalent in those of African descent it is also prevalent in the Caribbean, Middle East, Mediterranean, parts of India, and South and Central America. Screen for red cell antibodies (if present risk of haemolytic disease of newborn). Progestogenic contraception is first choice; oestrogencontaining contraceptives are used as second-line agents. Examine the heart in all pregnancies, but especially in those from an immigrant population. Never ignore even asymptomatic cases of Marfan syndrome, pulmonary hypertension, and mitral stenosis. Marfan syndrome: Autosomal dominant with 80% cardiac involvement with mitral valve prolapse, regurgitation, and/or aortic root dilatation. Ischaemic heart disease is increasingly common with rising maternal age and obesity. Peripartum cardiomyopathy is rare and defined as heart failure without known cause and no previous history of heart disease. Manage with elective delivery if antenatal, anticoagulants, conventional treatment for heart failure, and may require intra-aortic balloon pumps/left ventricular assist devices and/or cardiac transplantation. Use the lowest effective dose and consider drugs which have previously been effective. With severe depression, bipolar affective disorder, schizophrenia, or other mental health diagnoses requiring specialist input, do not stop or change medication without their help. Remember the high risk of rapid postpartum relapse with significant associated risks to mother and infant, particularly in women with bipolar disorder (up to 50%). Try to wait until the 2nd trimester before prescribing but do not delay if severe symptoms. There is a very small risk of persistent fetal pulmonary hypertension and neonatal withdrawal (breastfeeding can ease this). Avoid paroxetine (1st trimester use may be associated with cardiac malformations, and increased risk of neonatal withdrawal). Fluoxetine and citalopram are present in relatively high concentrations in breast milk. Valproate and carbamazepine should not be prescribed to women of childbearing age and urgent advice sought with a view to stopping them if a woman taking them is pregnant. Iron and folate supplements (and prevention against hookworm and malaria) are recommended in many developing countries. Parenteral iron may be given (to those with iron deficiency anaemia not tolerating oral iron) as iron dextran or iron sucrose. Hb rises by 8g/L /week over 6 weeks, so late severe anaemia (Hb <90g/L) may need blood transfusion. Prenatal diagnosis is possible by chorionic villus sampling (p15) for thalassaemias anticipated by parental blood studies. They are still susceptible to sickling crises in pregnancy and the puerperium, so antenatal diagnosis is essential. Transmission also with viral load >400 copies/mL, seroconverision during pregnancy, advanced disease, preterm labour, hepatitis C. Premature labour If membranes rupture >34wks expedite delivery, whatever the maternal viral load. Assess renal function; refer to nephrologist if creatinine >120mol/L, protein excretion >2g/24h (use thromboprophylaxis if >5g/24h). Postnatal · Encourage breastfeeding (insulin, metformin, and glibenclamide are compatible with breastfeeding) · Encourage pre-pregnancy counselling before next pregnancy · If preproliferative retinopathy review ophthalmologically for 6 months · Discuss contraception. Withdraw treatment after 612 months for 4 weeks to see if long-term therapy is required. Hypothyroidism may be associated with postpartum depression, so check thyroid status of women with postpartum depression. Viral hepatitis and gallstones may cause jaundice in pregnancy and investigation is similar to the non-pregnant. Bile acids are a test usually only requested in pregnancy and if raised, diagnose obstetric cholestasis. Acute fatty liver of pregnancy Incidence: 1:660013,000 deliveries-so it is rare but extremely serious. Plasmodium falciparum malaria is dangerous (and complicated) in pregnancy, particularly in those with no malaria immunity. Other associations between falciparum malaria and pregnancy are anaemia, miscarriage, stillbirth, low birth weight, and prematurity. Non-resistant vivax, ovale, and malariae are treated with chloroquine orally over 3 days with weekly dose to prevent relapse during pregnancy. If infection peripartum, anticipate fetal distress, fluid-balance problems, and hypoglycaemia in labour. Mothers living in endemic areas Chemoprophylaxis improves birthweight (by ~250g, with fewer very low birthweight babies). Glycosuria in pregnancy usually reflects altered renal physiology rather than hyperglycaemia. Trimethoprim and nitrofurantoin are safe alternatives but avoid trimethoprim in the 1st trimester (antifolate action) and nitrofurantoin in the 3rd (neonatal haemolytic anaemia). Acute cystitis affects 1%, characterized by urinary frequency, urgency, dysuria, haematuria, and lower abdominal pain. Pyelonephritis Affects 12% of pregnant women and is more common due to dilatation of upper renal tract in pregnancy. Chronic renal disease With mild renal impairment (pre-pregnancy creatinine <125mmol/L) without hypertension there is little evidence that pregnancy accelerates renal disorders. Patients with marked anaemia, hypertension, retinopathy, or heavy proteinuria should avoid pregnancy as further deterioration in renal function may be expected. Pregnancy for those on dialysis is fraught with problems (fluid overload, hypertension, pre-eclampsia, polyhydramnios). Outcome is better for those with renal transplants, but up to 10% of mothers die within 7 years of giving birth. It is categorized according to seizure type: primary generalized epilepsy (tonicclonic seizures, absences, myoclonic jerks), and partial or focal seizures which may progress to secondary generalization (complex partial seizures) of which temporal lobe epilepsy is a part. Those with poorly controlled epilepsy are most likely to experience a deterioration (check drug compliance). Obstetrics Respiratory disease in pregnancy Oxygen demand increases significantly in pregnancy, due to raised metabolic rate and consumption. Asthma is common, affecting up to 7% of women in pregnancy and is due to reversible bronchoconstriction of airways from smooth muscle spasm, along with inflammation and increased mucous production. For most women asthma remains unchanged or improved, but it may worsen (especially if poorly controlled to start with). Severe and/ or poorly controlled asthma may result in fetal growth restriction and preterm labour. Pneumonia is no more common than in non-pregnant women, but has a higher mortality rate, especially with varicella zoster pneumonia. Onset is insidious, with cough, haemoptysis, weight loss, and night sweats, and may cause coarse crackles in the upper lobes and lymphadenopathy. Treat with rifampicin, isoniazid (plus pyridoxine), and pyrazinamide and/ or ethambutol. Non-steroidal antiinflammatories can be used in the first and second trimesters but are not recommended in the third as they can cause premature closure of the ductus arteriosus and late in pregnancy have been associated with renal impairment in the newborn. Most are mild to moderate involving skin, but those with renal involvement and hypertension may deteriorate and are prone to pre-eclampsia. Aspirin 75mg daily should be started prior to conception and continued throughout pregnancy, and the fetus should be carefully monitored. Postpartum, use either heparin or warfarin (breastfeeding contraindicated with neither) as risk of thrombosis is high. It tends to fall again after delivery (often leading to an improvement and tricking doctors into stopping antihypertensives too early) peaking again at day 34 postpartum. Remember to use the correct cuff size-using a small cuff on a large arm leads to a falsely elevated reading. These women have a higher risk of developing pre-eclampsia (double if on treatment), fetal growth restriction, and placental abruption. If hypertension is secondary to another disorder involve a specialist in hypertensive disorders. Change methyldopa to another antihypertensive post delivery as risk of postnatal depression. Avoid diuretics if breastfeeding (labetalol, atenolol, metoprolol, captopril, and enalapril are safe). There is an increased risk of developing pre-eclampsia (1526%) especially with earlier onset of hypertension. Management: Assessment in secondary care, with urine testing for proteinuria with automated reagent strip readings or urine protein/creatinine ratio testing to rule out pre-eclampsia. If treatment is still needed at 6 weeks arrange review with specialist in hypertensive disorders. Other postpartum risk factors include mid-cavity or rotational instrumental delivery, postpartum haemorrhage and blood transfusion. Postnatally, enoxaparin can be given as soon as possible as long as no ongoing postpartum haemorrhage, and >4h since epidural sited or removed. Obstetrics Thrombophilia in pregnancy Thrombophilia is the tendency to increased clotting and there are many underlying causes.
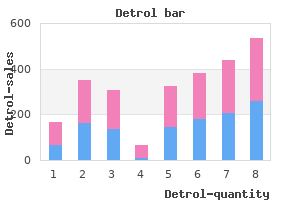
Other precipitants include menstruation symptoms 2dp5dt buy detrol toronto, caffeine withdrawal medicine vials cheap detrol 4 mg buy on-line, hunger medicine 6 year detrol 1 mg order without a prescription, estrogen exposure (typically via oral contraceptives) symptoms yellow eyes discount detrol 2 mg without a prescription, sleep deprivation treatment of ringworm buy 1 mg detrol free shipping, stress, heat, and exertion. Migraine without aura is the most common migraine phenotype in pediatric patients. Criteria assist in the diagnosis of migraine without aura and are based on the number and duration of episodes, as well as symptoms and associated findings (Table 28. It has been recognized that children may have shorter-duration headaches, so an allowance has been made to reduce the duration to 2-72 hours or 1-72 hours with diary confirmation. At times, though, the pain of an episode may be sudden and severe, prompting concern for a thunderclap headache. More typically, pain increases in severity over the course of an individual episode and becomes throbbing. Because most patients are sensitive to motion, light, and noise during a migraine attack, they search for a dark and quiet place to sleep. Aura consisting of visual, sensory, and/or speech/language symptoms, each fully reversible, but no motor, brainstem, or retinal symptoms C. In migraine with aura, the headache is preceded by sensory signs or symptoms termed an aura, which is caused by vasoconstriction and diminished blood flow to the affected region of the brain. Sensory auras are less common than visual auras and may consist of numbness or tingling. Diplopia, vertigo, and vomiting should prompt evaluation for a posterior fossa abnormality, such as a mass or a vascular malformation. Hemiplegic migraine has an aura that consists of unilateral motor weakness and visual, sensory, and/or speech/language symptoms that are fully reversible. Aura consisting of visual, sensory, and/or speech/language symptoms, each fully reversible, but no motor or retinal symptoms C. At least 1 aura symptom spreads gradually over 5 or more min, and/ or 2 or more symptoms occur in succession 2. Severe or very severe unilateral orbital, supraorbital, and/or temporal pain lasting 15-180 min (when untreated)* C. At least 1 of the following symptoms or signs, ipsilateral to the headache: a) Conjunctival injection and/or lacrimation b) Nasal congestion and/or rhinorrhea c) Eyelid edema d) Forehead and facial sweating e) Forehead and facial flushing f) Sensation of fullness in the ear g) Miosis and/or ptosis 2. Attacks have a frequency between 1 every other day and 8 per day for more than half of the time when the disorder is active E. This migraine subtype is extremely rare, and other causes of the vision disturbance should be investigated prior to designating this diagnosis. The childhood periodic syndromes, or episodic syndromes that may be associated with migraine, are a group of potentially related symptoms that occur with increased frequency in children with migraine. Some of these have included gastrointestinalrelated symptoms (motion sickness, recurrent abdominal pain, recurrent vomiting including cyclic vomiting, and abdominal migraine), sleep disorders (sleepwalking, sleeptalking, and night terrors), unexplained recurrent fevers, and even seizures. Confusional migraine and Alice in Wonderland syndrome are rare migraine with aura variants that occur primarily in children. Confusional migraine begins after 5 years of age and usually converts to typical migraine as the patient gets older. Episodes begin with an alteration in consciousness, which may include varying degrees of lethargy, agitation, and stupor. The aura of Alice in Wonderland syndrome is characterized by perceptual disturbances in which the sense of proportion or distance, particularly with respect to the body, is distorted. Patients with migraine may have neurologic deficits that persist during and after the headache. These deficits include hemisensory symptoms, hemiparesis, aphasia, visual loss, and alteration in consciousness. These symptoms usually last for the duration of the headache but may remain for days following headache abatement. Permanent neurologic deficits are rare but may occur if the vasoconstriction is severe and causes infarction. This prolonged headache is usually associated with protracted vomiting and dehydration. Some disorders that feature migraine with aura episodes have an identified genetic etiology. This diagnosis must be considered in children with coexisting epilepsy, mental retardation or regression, and myopathy. Cluster headaches are characterized by episodes of pain interspersed between long periods of remission (Table 28. Pain is unilateral and localized to the eye and temple but may spread to other parts of the head. Lacrimation, rhinorrhea, sweating, and nasal stuffiness usually accompany the headache. Patients find it impossible to rest, and they become agitated and restless during an attack. This is in sharp contrast to a migraine, in which the patient is quiet and withdraws to a dark cool room for sleep. Episodic cluster headaches occur in a series that may last for weeks or months, separated by remission periods of months to years, whereas chronic cluster headaches are defined as occurring for more than 1 year without such a remission period, or with remission periods that last less than 1 month. Aneurysms and Arteriovenous Malformations Arterial aneurysms may be congenital (berry) or caused by an infectious process (mycotic). The pain is acute in onset and associated with nuchal rigidity, emesis, and changes in sensorium. In half of the cases, patients report having previous headaches before having the headache associated with the rupture. If the clinician suspects a leaking or ruptured aneurysm, rapid neurologic and neurosurgical care is mandatory. Paroxysmal Hemicrania Paroxysmal hemicrania is characterized by shorter attacks (2-30 minutes) and absolute prevention with and response to indomethacin. Chronic paroxysmal hemicrania consists of frequent and intense unilateral headaches. Although it usually begins in adulthood, chronic paroxysmal hemicrania may affect older children and adolescents. Patients have at least 20 attacks a day, and the pain may awaken the patient from sleep. Because the symptoms of chronic paroxysmal hemicrania are similar to those of vascular malformations of the brain, a neuroimaging study should be performed to rule out malformation before the diagnosis of chronic paroxysmal hemicrania is made. Secondary Headaches Arteritis, Cerebral Venous Thrombosis, and Vascular Dissection Vascular dissection may present with a headache that precedes ischemic symptom development by hours to days. These headaches are typically persistent, nonthrobbing, and unilateral but may be throbbing, thunderclap, and steadily worsening. Infection, coughing, vomiting, and connective tissue disorders such as Ehlers-Danlos disease are risk factors. The headache is generally constant and may have qualities of both chronic tension-type and migraine headaches. Other features of this syndrome are fatigue, dizziness, vertigo, poor memory, decreased reaction times, and inability to concentrate. About 70% of patients recover within a year, but 15% are still symptomatic after 3 years. Post-traumatic headache is considered acute if duration is less than 3 months and chronic if over 3 months. Even though postconcussive syndrome is more common in persons with a history of psychologic or psychosomatic illness, a neuroimaging study may be necessary to exclude the rare possibility of a chronic subdural hematoma. Vasculitis Vasculitis is an important cause of headaches in adults; however, in children, headache is rarely the presenting manifestation of this disorder and is instead a less frequent associated finding. Because of the increased risk of systemic hypertension in patients with vasculitis, it is important to include a blood pressure measurement as part of the complete history and physical examination. When systemic lupus erythematosus and mixed connective tissue disorders affect the central nervous system, children may present with seizures and mental status changes. More commonly experienced symptoms are focal neurologic deficits such as weakness of the limbs and face or speech abnormalities; as such, every child presenting with a focal neurologic deficit must undergo evaluation for stroke. If papilledema is present, neuroimaging should be obtained prior to lumbar puncture to evaluate for other causes of papilledema, such as a tumor or hydrocephalus (see Table 28. If the patient does not have a sixth cranial nerve palsy, then the diagnosis may be suggested (but not confirmed) if 3 of the following imaging requirements are met: empty sella, flattening of the posterior aspect of the globe, distention of the perioptic subarachnoid space with or without a tortuous optic nerve, and transverse venous sinus stenosis. Ongoing observation with recurrent exams, imaging, and studies is indicated to confirm the diagnosis. All patients with pseudotumor cerebri should be monitored closely with special attention to ocular findings, as they are at risk for development of permanent visual impairment. Headache in pseudotumor cerebri may be intermittent or constant and may resemble a migraine. Pseudotumor cerebri may be either primary or secondary to a variety of medical conditions. In idiopathic intracranial hypertension, a subset of primary pseudotumor cerebri, the typical patient is postpubertal, obese, and female. Pseudotumor cerebri may also be due to obstructive, toxic, metabolic, or hormonal causes that may often be revealed through a thorough history and physical examination (Table 28. In addition to headache and papilledema, signs and symptoms may include sixth and seventh cranial nerve palsies and visual field changes. In severe cases, the retinal blind spot may enlarge, and the visual fields may become constricted. Diagnosis in most cases is based on the historical presentation and the demonstration of an elevated cerebrospinal fluid opening pressure on a lumbar puncture obtained in the lateral position. Slowly developing hydrocephalus initially causes mild pain, whereas rapidly developing hydrocephalus causes severe pain. Most patients with hydrocephalus have morning headaches that lessen after they arise, though pain may also be constant. Physical examination reveals signs of increased intracranial pressure, such as papilledema or tenderness of the neck. Macrocephaly is present in young children with unfused cranial sutures and in those with long-standing hydrocephalus. The head growth chart is especially important in the evaluation of children with hydrocephalus. Head growth is abnormal if the plot of sequential head circumferences crosses percentile lines. The pain is maximum and severe at the onset of the activity and then resolves in seconds. Cough headaches, which are much shorter than are exercise-induced vascular headaches, may be caused by both benign and life-threatening conditions. Structural causes of cough headache include brain tumors, cysts, and Chiari malformations. The results of the physical examination are usually normal, even when structural lesions cause this syndrome. The etiology of the headache is due to traction on the dura and vessels at the base of the brain. The headache associated with intracranial hypotension typically improves while the patient is recumbent and worsens upon sitting or standing. The most common cause of a headache from intracranial hypotension is a persistent cerebrospinal fluid leak following lumbar puncture. Patients describe a severe headache within seconds after assuming an upright position. Intracranial Masses Brain neoplasms are the second most common type of childhood malignancy, though the overall incidence is low. Headaches caused by hydrocephalus may develop rapidly, whereas traction on dural or vascular structures from tumor growth causes a slow and progressive headache. At the time of presentation, most patients with tumors or hydrocephalus have chronic and progressive headaches, with a history of increasing frequency and severity of pain over time. For example, patients with posterior fossa tumors usually have occipital pain, but if hydrocephalus is also present, the pain may be generalized. Headache secondary to tumor typically demonstrates a slow increase in the severity and frequency of painful episodes; initially, pain may be mild, and over-the-counter analgesics provide adequate pain relief. However, it is important to note that many patients with brain tumors have no particular pattern to their headaches. Patients with brain tumors near the optic chiasm may have visual disturbances, endocrine deficiencies, or galactorrhea. Diplopia may be present if the third or sixth cranial nerve is compressed; ptosis may also be present. Other historical features concerning for intracranial neoplasm include changes in school performance, reported motor or balance disturbances, personality or behavior changes, or seizures. Physical examination often reveals abnormal findings, including papilledema and neurologic deficits. Focal neurologic findings may include eye movement abnormalities, anisocoria, facial weakness, ptosis, swallowing difficulties, hemiparesis, sensory deficits, cranial nerve deficits, altered mental status, and ataxia. Papilledema may be absent in children with posterior fossa tumors (with or without hydrocephalus) or in children with open fontanels. Nonlateralizing signs include increased motor tone as well as third and sixth nerve palsies. Increased motor tone may not be a constant finding and may manifest as transient shivering. The Parinaud syndrome is the triad of upward-gaze paresis, poor pupillary reaction to light, and retraction nystagmus on convergence. This constellation of physical findings is seen in patients with hydrocephalus or tumors in the pineal region. Increased intracranial pressure secondary to hydrocephalus and/or a brain tumor should be suspected in any child with chronic progressive headaches, abnormal neurologic examination findings, nuchal rigidity, or abnormal head growth.
Unfortunately medications that cause high blood pressure purchase online detrol, these tests are nonspecific and not necessarily diagnostic of vascular thrombosis symptoms crohns disease detrol 1 mg order without prescription. Studies in adults have indicated that a negative assay for D-dimer has a strong negative predictive value for pulmonary embolus medications during breastfeeding discount detrol 2 mg buy online, especially when combined with an algorithm for risk assignment symptoms nausea headache fatigue detrol 4 mg. The diagnostic approach to a patient with suspected venous thrombosis is presented in treatment quinsy generic detrol 4 mg with amex. Specific Diagnostic Studies Compression ultrasonography is generally used to assess for the presence of a lower extremity thrombosis and many episodes of upper extremity thrombosis. Magnetic resonance imaging and magnetic resonance venography can be useful in diagnosis of venous dural sinus thrombosis. Pulmonary embolism may be present without significant respiratory distress, and should be considered in patients with chest pain or hemoptysis, particularly following surgery and immobilization. Thrombophilia Testing In children, the diagnosis of venous thrombosis in the setting of risk factors, such as surgery, immobilization, or catheter placement, does not generally warrant any additional work-up. Adult guidelines specifically recommend against thrombophilia testing in thrombosis in the setting of major transient risk factors. An unprovoked thrombosis merits work-up for a congenital or acquired thrombophilic condition. Neck trauma that is often mild can cause carotid or vertebral artery dissection or aneurysms. A history of neck trauma should be sought in older children who present with arterial stroke. Abnormal Anticoagulant Therapy Heparin Heparin is the most commonly used agent for the initial treatment of venous or arterial thrombosis. Although most studies of heparin pharmacokinetics have been performed in adults, there are important differences in the pharmacologic features of heparin in children and especially neonates. In contrast, most children older than 1 year are satisfactorily maintained on 20 U/kg/hr of heparin. The heparin dose should be adjusted every 4-6 hours until a satisfactory level is attained. Reports in adults suggest that the heparin level is superior for monitoring heparin therapy. Studies have documented an increased risk for recurrent thrombi in patients who failed to achieve adequate anticoagulant levels promptly. For long-term anticoagulant therapy, warfarin can be started after the institution of heparin therapy. Total length of therapy for provoked clots should not exceed 3 months, while therapy for unprovoked clots may extend to 6-12 months or indefinitely, depending on the presence of other prothrombotic conditions. Although rare, these are associated with a higher relative risk for thrombosis than the more common thrombophilias. If low levels are found, studies should be performed on the parents to establish the inheritance of the deficiency because all these are inherited as autosomal co-dominant traits. Less severe, but more common, thrombophilias include factor 5 Leiden and the prothrombin gene mutation. Testing of asymptomatic family members is not generally required, although affected females should be counseled to avoid estrogencontaining oral contraceptives due to a higher risk for thrombosis. The lupus anticoagulant does not bind in vivo to the platelet membrane; thus, the whole blood clotting time is normal. Paradoxically, the lupus anticoagulant is associated with venous and arterial thromboembolic disease and spontaneous abortions but is usually not a cause of clinical bleeding. If these study findings are negative, the thrombin time should be measured or a comparison of functional and antigenic levels of fibrinogen should be done to detect a dysfibrinogenemia. Fibrinolytic Therapy Fibrinolytic therapy is indicated for serious and potentially lifethreatening thrombosis because it provides a more rapid lysis of clots than standard anticoagulant treatment with heparin and is clinically effective in both arterial and venous clots. Because bleeding complications are many times higher than those with heparin in older individuals, the clinical severity of the clot must justify the use of lytic therapy. For smaller thrombi or those in nonvital locations, heparin is safe and effective. If the clot has been long-standing, it is unlikely that fibrinolytic therapy will be efficacious. The presence of any intracranial process, recent major surgery, or recent significant bleeding is an absolute contraindication to fibrinolytic therapy and a relative contraindication to heparin treatment. Patients with protein C or protein S deficiency are at risk for warfarin-induced skin necrosis when warfarin therapy is initiated, particularly if high doses are used. These individuals should be given heparin before warfarin is started, and they should not receive a loading/high dose of warfarin. Fibrinolytic therapy appears to result in a more rapid return of pulmonary artery flow after pulmonary emboli and may decrease the likelihood of postphlebitic syndrome after deep vein thrombosis. Warfarin acts by blocking the vitamin Kdependent post-translational modification of factors 2, 7, 9, and 10 and of protein C and protein S. If warfarin therapy is started early in the course of heparin therapy for thrombotic disease, effective oral anticoagulant effect is often achieved by day 5, at which time levels of all the vitamin Kdependent factors should be depressed by warfarin. A family history and personal history that quantitate bleeding episodes are of utmost help in planning an evaluation. Red flags include anemia; signs of end-organ bleeding or vascular occlusion, particularly the central nervous system; signs of a systemic disorder (pancytopenia, hypotension, rash, weight loss, chronic fever, liverrenal-pulmonary system involvement); and signs of hemorrhagic shock. Inherited thrombophilia in children with venous thromboembolism and the familial risk of thromboembolism: an observational study. Thromboprophylaxis in a pediatric hospital: a patient-safety and quality-improvement initiative. Bleeding in the heritable connective tissue disorders: mechanisms, diagnosis, and treatment. Guidance for diagnosis and treatment of disseminated intravascular coagulation from harmonization of the recommendations from three guidelines. Antithrombotic therapy in neonates and children: antithrombotic therapy and prevention of thrombosis. Management of stroke in infants and children: a scientific statement from a special writing group of the American Heart Association Stroke Council and the Council on Cardiovascular Disease in the Young. Direct oral anticoagulants compared with vitamin K antagonists for acute venous thromboembolism: evidence from phase 3 trials. Production of acute-phase reactants and alterations in metabolism and endocrine function are examplesofthesechanges. This increases oxygen consumption, carbon dioxide production, and fluid and caloric needs. Heat illness must be distinguished from fever as a cause for elevatedbodytemperature. Thereisacorrelation between axillary and rectal temperature measurements; the axillarytemperatureisusually0. When detection of fever is critical for diagnosis and management, rectal temperatures should be used in the child 3 years of age and younger. They may show signs of shock, including weak peripheral pulses, tachycardia, poor perfusion, respiratory distress, mottling, cyanosis, or decreased mental status (Table 39. After thorough clinical and laboratory evaluation, ill-appearing children should be admitted to the hospital, and will likely need empiric antibiotic treatment. It is important to consider that infants, especially those younger than 2 monthsofage,mayhaveabluntedfebrile(orhypothermic)response toinfection. Infants younger than 3 months, malnourished, and immunocompromised individuals are exceptions. Althoughbloodcultures do not provide immediateresults,methods allow for continuous and more rapid detection of bacterial growth. Inpractice, pneumonia can often be diagnosed solely on the basis of the clinical findings of fever, tachypnea, and crackles; chest radiographs arenotalwaysnecessary. In very young infants, clinical evaluation alone is inadequate for excluding serious bacterial infections. A number of prospective studies have contributed to the development of specific low-risk screeningcriteria(Table39. Blood cultures should be obtained for all children in whom sepsis or meningitis is suspected. Riskfactorsforgirlsare:age <12months,whiterace,temperaturegreaterthan39°C,andfever for 2 or more days. For boys, the risk factors are uncircumcised status, nonblack race,temperaturegreaterthan 39°C,andfever for over 24hours. Forboyswho are circumcised, 2 or more of the other risk factors increases the risktoover1%andtheyshouldbescreened. Ifthecultureispositive for nontyphoidal Salmonella organisms and the child is younger than 3 months, full sepsis evaluation and intravenous antibiotics arerecommended. Those who appear ill or who have positive culture results should be admitted for parenteral antibiotics. If child fulfills all low-risk criteria, administer no antibiotics, ensure follow-up in 24 hr and access to emergency care if child deteriorates. If child does not fulfill all low-risk criteria, hospitalize and administer parenteral antibiotics until all cultures are final and definitive diagnosis determined and treated Reassurance that diagnosis is likely self-limited viral infection, but advise return with persistence of fever, temperatures >39°C (102. In infants, the findings are usually nonspecific and may be subtle; they includevomiting,diarrhea,irritability,lethargy,poorappetite,respiratorydistress,seizures,hypothermia,andjaundice. Itisuncommonfor affected young infants to have a stiff neck; only 30% have a bulging fontanel. Reactive arthritis caused by immune complex deposition is also seen with bacterial meningitis. A positive sign is present if this movement is limited by contraction of the hamstrings and causes pain. If signs or symptoms of increased intracranial pressure are present, the lumbar puncture should be postponed until the increased pressure is lowered with appropriate treatment. If a lumbar puncture is delayed, appropriate antibiotic therapy should be initiated without further delay. The patient lies supine, and the head is passively elevated from the table by the examiner. The patient complains of neck and low back discomfort and attempts to relieve the meningeal irritation by involuntary flexion of the knees and hips. Complaints of pain in the lower back, neck, and/or head are suggestive of meningeal irritation. L4-L5 position is determined by a vertical line drawn between the superior iliac crests. On penetration into the space, the examiner often feels a give or pop after moving through the dura. After the needle enters into the subarachnoid space, the clinician removes the stylet and collects the cerebrospinal fluid. Openingpressureislessthan5cm H2O in premature infants and less than 10cm H2O in normal newborns. Eastern equine encephalitis and lymphocytic choriomeningitis may have cell counts of several thousand. Some patients will have been treated with antibiotics before the lumbar puncture is performed. Transmissionisviathefecal-oralroute,andyoungchildren exhibit increased transmission of the viruses and more severe disease in comparison with other age groups. Louis encephalitis, Powassan and California encephalitis, West Nile virus, Colorado tick fever Herpes simplex (types 1, 2) Human herpesvirus (types 6, 7) Varicellazoster virus EpsteinBarr virus Parvovirus B19 Cytomegalovirus Adenovirus Variola (smallpox) Measles Mumps Rubella Influenza A and B Parainfluenza Rhinovirus Rabies Lymphocytic choriomeningitis Rotaviruses Coronaviruses Human immunodeficiency virus type 1 Bacteria Mycobacterium tuberculosis Leptospira species (leptospirosis) Treponema pallidum (syphilis) Borrelia species (relapsing fever) Borrelia burgdorferi (Lyme disease) Nocardia species (nocardiosis) Brucella species Bartonella species (cat-scratch disease) Rickettsia rickettsiae (Rocky Mountain spotted fever) R. Enteroviruses and arboviruses cause most cases of infectious encephalitisinchildren. Taking the history should be repeated because parents often remember important details after the initial interview. Increased temperatures after exercise and in the afternoon often represent normal variations. Saddle-back or double-humpfeverlastsafewdays,isfollowedbyanafebriledayor 2, and then returns. Doublequotidianfever(2feverspikeseachday)occurs in kala-azar, malaria, and gonococcal endocarditis. The food history should be detailed and should include water sources, use of game meats, cooking practices, and consumption of unpasteurized,rawmilk,orsoftcheese. Travel history is critically important in the establishment of a differential diagnosis. Physical Examination Whenever possible, the patient should be examined during a febrile episode. Tuberculosiscancause formation of choroidal tubercles and also ulcerative palpebral conjunctivallesions. Abdominal tenderness may be present with abdominal abscesses, hepatosplenomegaly,andinflammatoryboweldisease. Arectalexamination should be performed, and stool should be tested for occult blood. Irritability and pain on palpation over a bone or disuse pseudoparalysis may be the 1st clue to osteomyelitis. Bone pain may also result from neoplastic infiltration of the bone marrow or sickle cell anemia. Myalgias occur commonly with viral diseases such as influenza, and may be present with rickettsial diseases, polyarteritis nodosa, Takayasu arteritis, and dermatomyositis. Skin the skin must be inspected for evidence of rashes and other lesions (seeChapter40). Dermatomyositis is characterized by a heliotropic rash of the upper eyelids and an erythematouseruption(vasculitis)overtheextensorsurfaces(Gottron sign). The rash of Kawasaki disease is erythematous and may manifest in many forms; it is most commonly a diffuse maculopapular rash. Vegetations also may not be visible initially by transthoracic echocardiography; a transesophageal approach is much more sensitive.
Preseptal cellulitis treatment sinus infection cheap detrol 1 mg buy, defined as infection confined to the eyelid tissues anterior to the orbital septum symptoms 10dpo buy detrol overnight delivery, is a common infection in children and needs to be distinguished from infection involving the orbit medicine cabinets surface mount cheap detrol 2 mg with amex. Preseptal infections may result from trauma and insect bites involving the eyelids medicine in ukraine order cheap detrol line, severe conjunctivitis medicine werx generic detrol 1 mg with visa, primary bacteremia, upper respiratory infection or they may spread to the eyelids from the paranasal sinuses. The affected eyelids are swollen and red, and the infection can spread further into the eyebrow, forehead, and cheek. Proptosis and limitation of eye movements do not occur in preseptal cellulitis, but confirmation of this can be problematic because of the difficulty of opening the eye. Patients with signs and symptoms of systemic toxicity should be hospitalized for intravenous antibiotics; milder cases of preseptal cellulitis may be managed with oral antibiotics as long as appropriate follow-up is ensured. Orbital cellulitis is an infection of the orbit that involves the tissues posterior to the orbital septum. Most frequently, this is a result of spread of infection from the ethmoid or frontal sinuses. Ocular signs include eyelid edema and erythema, proptosis, and inferior and lateral displacement of the globe with limited eye movements. If orbital cellulitis is suspected, computed tomography of the orbit and sinuses is indicated. Children younger than 9 years are more likely to have an infection caused by a single aerobic pathogen, whereas children older than 9 years may have complex infections with multiple pathogens. Often, orbital cellulitis begins as a subperiosteal abscess that forms in the potential space between the periorbital (analogous to the periosteum of long bones) and the orbital bones. Left untreated, this space-occupying mass can apply pressure to the optic nerve and cause permanent damage to vision. It can also spread into the intracranial space and result in a cavernous sinus thrombosis, a subdural empyema, or cerebral abscess. Most children younger than 9 years who have small to medium-sized subperiosteal abscesses can be treated successfully with broad-spectrum intravenous antibiotics (ceftriaxone and vancomycin, ampicillin/sulbactam, or piperacillin/tazobactam). Close observation with periodic checks of vision and pupillary function is important in the 1st 24-48 hours of treatment. Older children, those with large subperiosteal abscesses, and children who fail to respond to intravenous antibiotics within 48 hours require surgical drainage of 590 Section 6 NeurosensoryDisorders that the head is straighter. Congenital sensory nystagmus occurs with disorders that impair normal image formation (bilateral congenital cataracts) or image processing in both eyes (a retinal dystrophy or bilateral optic nerve atrophy or hypoplasia). Visual acuity is more severely impaired than in idiopathic congenital nystagmus (20/200 or less), and visual loss may be progressive in some instances. The evaluation of a child with congenital nystagmus entails a thorough health and family history, a general physical examination, and an eye examination by an ophthalmologist with expertise in pediatric eye disorders. A cranial magnetic resonance imaging scan is indicated when the hallmark signs of congenital motor nystagmus such as a null point and dampening of nystagmus on convergence are not yet identifiable and there are no eye findings to suggest a specific pathology such as cataract. Nystagmus that is truly acquired beyond the 1st few months of life is of concern and may represent a significant neurologic abnormality. It may be caused by central nervous system disorders, particularly of the cerebellum, brainstem, or suprasellar region. In children, the most common tumor causing acquired nystagmus is a craniopharyngioma. Emergency drainage is indicated in a patient of any age where there is compromise of the optic nerve. Horizontal nystagmus is the most common form of nystagmus, but vertical nystagmus and torsional nystagmus also occur (Table 32. Congenital nystagmus is somewhat of a misnomer because the abnormal eye movements are generally not noted until an infant is 1 or 2 months of age, when the fixation reflex becomes established. Congenital motor nystagmus is often idiopathic; in this case, visual acuity is only moderately impaired, and the fundus examination findings and the electroretinogram are normal. Usually an affected individual will have a null point or a preferred position in which the eye movements are minimized. This may affect the head position as the patient tries to keep the eyes in the null point. In patients with congenital motor nystagmus there is often dampening or quieting of the nystagmus with convergence. Spasmus nutans is a special form of acquired nystagmus with onset in the 1st 2 years of life. The usual triad of findings consists of nystagmus (often a shimmering type of nystagmus that is frequently asymmetric or even monocular), head nodding, and torticollis. This form of nystagmus is generally benign and disappears by the age of 3-4 years. In some cases, spasmus nutans can be associated with chiasmal or suprachiasmal or retinal dystrophies. Opsoclonus is a special form of eye movement abnormality that is not truly nystagmus in that the bizarre, seemingly random oscillations of the eyes are not rhythmic and are frequently multivectorial. Close follow-up is indicated to make sure that the cornea is healing and has not developed an infection that could lead to a corneal ulcer. Hyphema Any child with blunt trauma to the eye should be evaluated for blood in the anterior chamber of the eye, known as a hyphema. The anterior segment and pupillary function should be assessed if the hyphema only partially fills the anterior chamber. The nature of the traumatic injury varies by age but there is a persistent male preponderance. In school-aged children, sports-related injuries are the most common cause of ocular injury accounting for 25% of hospitalizations. For instance, the incidence of eye injuries from ice hockey are almost zero since the institution of mandatory face masks in children playing organized hockey. Projectile injuries from firearms, air guns, and fireworks are relatively frequent in the United States, however, these injuries are very rare in countries without easy access to guns or fireworks. If the circumstances of the injury suggest a high likelihood of a perforating injury (from a sharp object that could go through the cornea or sclera), the eye should not be forced open but rather, should be covered with a protective shield to prevent further injury until the child can be seen by an ophthalmologist and an exam under anesthesia can be done if necessary. The fluorescein may have linear pattern of staining that suggests a foreign body may be on the tarsal conjunctiva under the upper eyelid and during an eye blink the cornea is being abraded. Otherwise the foreign body may be removed at a slit lamp using topical anesthesia if the patient is cooperative. Management of a corneal abrasion entails relief of pain, prevention of infection, and promotion of healing of the corneal epithelium. Topical anesthesia, while used in the office, should not be used at home as it prevents epithelial healing and can be toxic to the cornea with longer-term use. A drop of a cycloplegic agent (cyclopentolate) may provide comfort by relieving ciliary spasm. It may be of benefit to refer the patient to a psychiatrist if the symptoms do not subside. The complications of hyphema include glaucoma, corneal blood staining, and rebleeding. The glaucoma may be managed initially with topical medications but the blood may need to be washed out of the anterior chamber surgically if the intraocular pressure cannot be controlled, blood is not resolving, or corneal blood staining is severe and threatening vision. Symptoms associated with reading are common and include seeing blurred print, words "swimming" together, and skipping words or lines. Uncommon visual phenomena may include seeing colored lights, objects appearing larger or smaller, seeing spots, and double vision. There may be physiologic explanations for each of the complaints, and the child is usually interested in an explanation of the reason proposed for his or her complaint. A careful history of the exact nature of the complaint and any associated concerns should be sought and a screening eye examination performed. An external eye examination may reveal a reason for eye pain (conjunctival injection, tearing, corneal abrasion, foreign body). Ocular injuries are also detected in the course of examining many other child abuse injuries. Blunt injuries to the eyelids and anterior segment of the eye from fingers, fists, or belts may cause eyelid ecchymosis, subconjunctival hemorrhage, hyphema, cataract, and lens dislocation. The finding of such an injury should alert the physician to the possibility of child abuse. Abusive head trauma is caused by forceful acceleration and deceleration motion such as shaking, which results in subdural hemorrhage and retinal or vitreous hemorrhages. The vitreous is adherent to the retina and the traction of the moving vitreous results in multiple retinal hemorrhages, often in all layers of the retina. Vitreous or retinal hemorrhage may take a long time to resolve and the child is at risk for amblyopia during the time the vision is obscured by blood. In cases of persistent hemorrhage, a vitrectomy may need to be done to clear the blood in the visual axis. Fewer than half of the patients diagnosed with abusive head trauma with retinal or vitreous hemorrhage see better than 20/40 after recovery. Functional Vision Loss Some patients complain of vision loss or blurring or other visual disturbances (seeing spots, colors, or patterns) while the eye exam is normal. The key to confirming functional vision loss is to demonstrate objective findings that indicate better vision than the subjective responses. Stereoacuity testing may demonstrate better visual acuity than the patient is reporting. There are several examining techniques that the ophthalmologist can employ to get this information. There are also objective tests available to further delineate etiologies of possible vision loss; however, these are rarely needed. If difficulty 593 reading persists despite correction of any refractive error and an otherwise normal eye exam, the child may have learning disabilities that warrant further evaluation. Behavioral vision therapy has not been proven to improve reading skills, learning disabilities, or dyslexia. Impaired visual function resulting from strabismus, cataracts, or other conditions may produce amblyopia and blindness. It is important to detect amblyopia because in most cases, amblyopia is reversible if discovered early and treated appropriately. Symptoms and signs that suggest potentially life- or vision-threatening diseases are listed in Table 32. Endoscopic treatment of intranasal abnormalities associated with nasolacrimal duct obstruction. Risk definition and management strategies in retinoblastoma: current perspectives. Guidelines for automated preschool vision screening: a 10-year, evidence based update. The critical period for surgical treatment of dense congenital unilateral cataract. Complications, adverse events, and additional intraocular surgery 1 year after cataract surgery in the Infant Aphakia Treatment Study. A suspicion index for early diagnosis and treatment of cerebrotendinous xanthomatosis. A randomized trial comparing part time patching with observation for children 3 to 10 years of age with intermittent exotropia. A randomized trial comparing part time patching with observation for intermittent exotropia in children 12 to 35 months of age. Childhood Uveitis American Academy of Pediatrics Section on Rheumatology and Section on Ophthalmology, Cassidy J, Kivlin J, et al. Expert panel recommendations for the use of anti-tumor necrosis factor biologic agents in patients with ocular inflammatory disorders. Retinopathy of Prematurity Early Treatment for Retinopathy of Prematurity Cooperative Group. Revised indications for the treatment of retinopathy of prematurity: results of the early treatment for retinopathy of prematurity randomized trial. Initiation and use of propanolol for infantil hemangioma: a report of a consensus conference. Intralesional bleomyicin: a potential treatment for refractory orbital lymphangiomas. Prophylaxis of ophthalmia neonatorum: comparison of betadine, erythromycin and no prophylaxis. Criteria for nonsurgical management of subperiosteal abscess of the orbit: analysis of outcomes, 1988-1998. Interventions for diabetic retinopathy in type 1 diabetes: systemic review and meta-analysis. Children or their parents rarely arrive in the clinic with a complaint of arthritis or patellofemoral syndrome. Instead, they have symptoms such as extremity pain, joint swelling, or limitations of activity and function. These children may have chronic inflammatory arthritis or an associated systemic rheumatic disease, a traumatic condition, a mechanical problem, or a pain syndrome, among other possible explanations. For many of these diagnoses, the history and physical examination are sufficient to confirm a diagnosis; for others, specific laboratory tests or imaging studies will confirm a suspected diagnosis. Musculoskeletal symptoms may indicate pathologic processes localized and restricted to a single extremity or joint, or localized symptoms may be a component of a systemic illness. Arthritis is a specific sign indicating objective inflammation of the joint, and can be defined as (1) swelling of the joint or (2) limitation of motion combined with 1 of the following: pain on motion, tenderness, or warmth. Arthritis is not a specific disease; there are infectious, postinfectious/reactive, hematologic, metabolic, oncologic, and rheumatic causes of arthritis. The precise diagnosis is determined by 1st establishing the characteristics of the arthritis with respect to the number and location of joints involved, severity, degree of disability, and chronicity. The clinician combines these characteristics with the history and the pattern of any associated systemic signs and symptoms to determine the specific cause of arthritis. Adolescents have a tendency to either underreport or overreport their symptoms, making the history especially challenging within this age group. If there are inconsistencies, it becomes increasingly difficult to formulate a diagnosis, and information from the physical examination, along with potential laboratory and imaging studies, may be needed to resolve the inconsistencies.
Buy genuine detrol. 2 Things Vets MUST prove to Corroborate a Non-Combat VA PTSD Stressor Event.
References
- Voci P, Bilotta F, Caretta Q, et al: Papillary muscle perfusion pattern. A hypothesis for ischemic papillary muscle dysfunction, Circulation 91:1714-1718, 1995.
- Domb BG, Stake CE, Botser IB, Jackson TJ. Surgical dislocation of the hip versus arthroscopic treatment of femoroacetabular impingement: a prospective matched- pair study with average 2- year follow- up. Arthroscopy 2013; 29(9):1506-13.
- Hauser MA, Horrigan SK, Salmikangas P, et al. Myotilin is mutated in limb girdle muscular dystrophy 1A. Hum Mol Genet. 2000;9(14):2141-2147.
- Cardona-Grau D, Bush RA, Le HK, et al: Reducing opioid prescriptions in outpatient pediatric urological surgery, J Urol 201:1-5, 2019.
- Thulesius O, Angelo-Khattar M, Sabha M: The effect of ureteral distension on peristalsis: studies on human and sheep ureters, Urol Res 17:385, 1989.
- Bamber J, Cosgrove D, Dietrich CF, et al. EFSUMB guidelines and recommendations on the clinical use of ultrasound elastography. Part 1: basic principles and technology. Ultraschall Med. 2013;34:169-184.
- Hann LE, Greatrex KV, Bach AM, et al. Cholangiocarcinoma at the hepatic hilus: sonographic findings. AJR Am J Roentgenol. 1997;168:985-989.
- Taieb D, Timmers HJ, Hindie E, et al. EANM 2012 guidelines for radionuclide imaging of phaeochromocytoma and paraganglioma. Eur J Nucl Med Mol Imaging 2012;39(12):1977-1995.
