
Finast
| Contato
Página Inicial
Malcolm V Brock, M.D.
- Director of Clinical and Translational Research in Thoracic Surgery
- Professor of Surgery
https://www.hopkinsmedicine.org/profiles/results/directory/profile/0005064/malcolm-brock
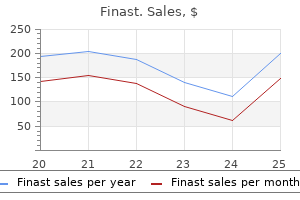
Subclavian steal syndrome may occur if the first part of the subclavian artery is occluded hair loss talk 5 mg finast with mastercard. Arm exercise causes syncope because of reversed flow in the vertebral artery leading to cerebral ischaemia hair loss 6 months postpartum discount finast 5 mg buy on-line. Treatment of gangrene How much of a limb or digit can be salvaged depends on the blood supply proximal to the gangrene hair loss jacksonville cheap finast 5 mg buy on-line. Poor circulation can sometimes be improved by radiological or surgical intervention and this may allow a more conservative debridement or distal amputation hair loss nioxin finast 5 mg buy. Macrovascular disease is atherosclerotic and typically affects the crural vessels with relative sparing of the pedal vessels hair loss treatment uae finast 5 mg otc, whereas increased microcirculatory shunting causes microvascular dysfunction. Motor involvement causes an imbalance between flexors and extensor muscle groups of the foot, promoting altered foot biomechanics and abnormal pressure loading and resulting in thick callosities developing on the sole of the foot. Superadded infection due to poor wound care can spread rapidly and proximally in subfascial planes leading to fulminant foot sepsis, gangrene and death. Treatment depends on the degree of arterial involvement, which should be investigated and treated rapidly with angioplasty or surgery. The gangrene is treated by drainage of pus, liberal debridement of dead tissue and antibiotics. Unfortunately, a number of patients present with life-threatening systemic upset and should undergo primary amputation. They can appear and extend rapidly in immobile patients and in those with debilitating illness. Prophylactic measures must be taken, including the avoidance of pressure over bony prominences by the use of foam blocks or similar, regular turning and nursing on specially designed beds that reduce the pressure to the skin. Skilled nursing and the use of appropriate dressings must prevent maceration of the skin by sweat, urine, faeces or pus. A bedsore can be expected if erythema appears that does not change colour on pressure. Advice from a plastic surgeon should be sought for major lesions; vacuum dressings and rotation flaps can be effective. Cold injury damages the wall of the blood vessel, which causes swelling, and leakage of fluid together with severe pain. When the pain disappears, a waxy appearance remains; blistering and then gangrene follow. Treatment is gradual rewarming, analgesics and delayed conservative amputation after demarcation of devitalised tissue. It may also happen when thrombosis occurs on an atherosclerotic plaque, although the outcome is usually less dramatic because collaterals are likely to have developed in chronic arterial stenosis. Embolic occlusion An embolus is an object that has become lodged in a vessel causing obstruction having been carried in the bloodstream from another site. It is often a thrombus that has become detached from the heart or a more proximal vessel. Sources include the left atrium in atrial fibrillation, a left ventricular mural thrombus following myocardial infarction, vegetations on heart valves in infective endocarditis, thrombi in aneurysms and on atheroscerotic plaques. It is essential to differentiate between the two, as they require different management. The fifth feature, anaesthesia, is often stated to be paraesthesia (the fifth P) but, in truth, complete loss of sensation in the toes and feet is characteristic. No source of embolus but previous claudication worsens but there are no sudden features of distal ischaemia. Mesenteric vessels possible gangrene and perforation of the corresponding loop of intestine. The limb is cold and the toes cannot be moved, which contrasts with venous occlusion when muscle function is not affected. The diagnosis can be made clinically in a patient who has no history of claudication and has a source of emboli, who suddenly develops severe pain or numbness of the limb, which becomes cold and mottled. Pulses are absent distally but the femoral pulse may be palpable, even thrusting, as distal occlusion results in forceful expansion of the artery with each pressure wave despite the lack of flow. Treatment Because of the ensuing stasis, a thrombus can extend distally and proximally to the embolus. The immediate administration of 5000 U of heparin intravenously can reduce this extension and maintain patency of the surrounding (particularly the distal) vessels until the embolus can be treated. Embolectomy and thrombolysis are the treatments available for patients with limb emboli. An angiogram may be performed in the operating theatre at the end of the procedure to ensure that flow to the distal leg has been restored. Postoperatively, heparin therapy is continued until long-term anticoagulation with warfarin is established to reduce the chance of further embolism. At arteriography of the ischaemic limb (usually via the common femoral artery) a narrow catheter is passed into the occluded vessel and left embedded within the clot. The method should be abandoned if there is no progression of dissolution of clot with time. There are several contraindications to thrombolysis, the most important of which are recent stroke, bleeding diathesis and pregnancy; results in those over 80 years old are poor. The artery (usually the femoral), bulging with clot, is exposed and held in silastic vessel loops. The catheter, with its balloon tip, is introduced both proximally and distally until it is deemed to have passed the limit of the clot. The balloon is inflated and the catheter withdrawn slowly, Compartment syndrome In limbs that have been subject to sudden ischaemia followed by revascularisation, oedema is likely. Muscles swell within confined fascial compartments and this can itself be a cause of tissue ischaemia, with both local muscle necrosis and nerve damage due to pressure, and systemic effects such as renal failure secondary to the liberation of muscle breakdown products. Liberal concomitant usage of fasciotomy following revascularisation of a prolonged ischaemic limb is advisable. Air embolism Air may be accidentally injected into the venous circulation or sucked into an open vein during head and neck surgery or a cut throat. If a large volume of air reaches the right side of the heart it may form an air lock within the pulmonary artery and cause acute right heart failure. The treatment of air embolism is to put the patient in a head-down (Trendelenburg) position to encourage the air to enter the veins in the lower part of the body. The patient should also be placed on the left side to help the air to float to the ventricular apex, away from the ostium of the pulmonary artery. In extreme cases, air may be aspirated from the heart through a needle introduced below the left costal margin. Arterial embolisation requires accurate selective catheterisation using the Seldinger technique. A variety of materials may be used, including gelfoam sponge, plastic microspheres, balloons, ethyl alcohol, quick-setting plastics and metal coils. The patient often complains of numbness/paraesthesia in the distribution of nerves running within the compartment (non-myelinated type C sensory fibres are most sensitive to hypoxia). Examination of the limb reveals a tense compartment with passive flexion and extension of muscles causing pain. The usual site for fasciotomy is the calf (especially the anterior tibial compartment), but compartment syndrome may occasionally affect the thigh and the arm. Acute mesenteric ischaemia Acute mesenteric occlusion may be either thrombotic (following atheromatous narrowing) or embolic. Embolic occlusion results in sudden, severe abdominal pain, with bowel emptying (vomiting and diarrhoea) and a source of emboli present (usually cardiac). Unfortunately, the diagnosis is often only made at laparotomy with widespread infarction of the small and large bowel present; in this situation, it is often fatal. Occasionally, the degree of bowel infarction is more limited; resection of the dead bowel and embolectomy of the superior mesenteric artery or bypass surgery can reduce the otherwise high mortality rate in these patients. Other forms of embolism Infective emboli of bacteria or an infected clot may cause mycotic aneurysms, septicaemia or infected infarcts. Parasitic emboli, caused by the ova of Taenia echinococcus and Filaria sanguinis hominis, may occur in some countries. Gabrielle Falloppio (Fallopius), 15231563, Professor of Anatomy, Surgery and Botany, Padua, Italy. Friedrich Trendelenburg, 18441924, Professor of Surgery successively at Rostock, Bonn and Leipzig, Germany. A limb is dead when arterial occlusive disease is severe enough to cause infarction of macroscopic portions of tissue, i. If the obstruction cannot be reversed and the symptoms are severe, amputation is required. A limb is deadly when the putrefaction and infection of moist gangrene spreads to surrounding viable tissues. Other life-threatening situations for which amputation may be required include gas gangrene (as opposed to simple infection), neoplasm (such as osteogenic sarcoma) and arteriovenous fistula. A limb may be deemed a dead loss in the following circumstances: first, when there is relentless severe rest pain without gangrene and reconstruction is not possible amputation will improve quality of life; second, when a contracture or paralysis makes the limb impossible to use and renders it a hindrance; and third, when there is major unrecoverable traumatic damage. For less extensive gangrene, if amputation is taken through a joint, healing is improved by removing the cartilage from the joint surface. A transmetatarsal amputation may be required when several toes are affected but the proximal circulation is adequate. Major amputation Choice of operation the major choice is between an above- and below-knee operation. A below knee amputation preserves the knee joint and gives the best chance of walking again with a prosthesis. However, an above knee amputation is more likely to heal and may be appropriate if the patient has no prospect of walking again. Unfortunately, the presence of a femoral pulse does not guarantee healing of a below-knee amputation, and sometimes a failed below-knee amputation may require revision to an above-knee procedure. For above- or below-knee amputations with a good stump shape, it is possible to hold a prosthesis in place simply by suction, without any cumbersome and unsightly straps. Gangrene Deadly limb Wet gangrene Spreading cellulitis Arteriovenous fistula Other. However, if the metatarsophalangeal joint region is involved, a ray excision is required, taking part of the corresponding metatarsal bone and cutting tendons back. Maurice Raynaud, 18341881, physician, Hospital Lariboisière, Paris, France, described this condition in 1862. For both methods, the total length of flap must be at least one and a half times the diameter of the leg at the point of bone section. The long posterior flap technique is the older method and remains the more popular, probably because of its relative simplicity. The proposed incision should be marked carefully: the tibial tuberosity identified and a distance 10 cm measured distally and marked with a sterile marker pen; this is the anterior landmark. The circumference is measured at this landmark with a long suture tie and this length divided into two thirds. The suture is centred over the anterior landmark so that there is one-third either side. The line of incision is now extended transversely around the back of the limb to join the distal extent of the longitudinal incisions. An incision is then made along the previously measured and marked lines through skin, subcutaneous fat and deep fascia. Anteriorly, the incision is deepened to bone and the lateral and posterior incisions are fashioned to leave the bulk of the gastrocnemius muscle attached to the flap, muscle and skin being transected together at the same level. Nerves are not clamped but pulled down gently and sharply transected as high as possible. The fibula is divided 2 cm proximal to the level of tibial division using bone cutters. The tibia is cleared and transected at the desired level, the anterior aspect of the bone being sawn obliquely before the cross-cut is made. This, with filing, gives a smooth anterior bevel, which prevents pressure necrosis of the flap. The area is washed with saline to remove bone fragments and the muscle and fascia are sutured with an absorbable material to bring the flap over the bone ends. The skew flap amputation makes use of anatomical knowledge of the skin blood supply. After division of bone and muscle in a fashion similar to that described above, the gastrocnemius myoplastic flap is sutured over the cut bone end to the anterior tibial periosteum with absorbable sutures. Finally, drainage and skin sutures are inserted and the limb dressed as for the long posterior flap operation. Through-knee amputation More recently through-knee or knee disarticulation has regained popularity as an alternative to above-knee amputation if soft-tissue viability permits. This amputation preserves the full length of the femur and patella, providing a long mechanical lever that is controlled by stronger muscles as the line of muscle transection is distal and occurs through fascial tissue, as opposed to thick muscular bellies as is the case with an above-knee amputation. The bulbous nature of the amputation end, initially thought a hindrance for subsequent prosthetic fitting, is now seen as beneficial as it allows for a self-suspending prosthetic that is less likely to rotate compared to an above-knee amputation prosthetic. The line of incision is marked preoperatively: equal anterior and posterior semicircular flaps are constructed, with the proximal extent of incision being the joint line laterally and medially, and the distal extent of the anterior flap being 3 cm below the tibial tuberosity and directly posterior to this level for the posterior flap. The anterior incision is carried down to the tibia and the patellar tendon insertion into the tibial tuberosity is identified and released. The patellar tendon is followed proximally to the patella, releasing it from surrounding fascial structures. The anterior knee capsule is entered and the lateral and medial capsule divided along with the collateral knee ligaments. The knee is flexed to 90° and the dense posterior capsule divided, paying attention to identify the popliteal artery and vein located immediately behind the capsule. The medial head of the gastrocnemius muscle along with its vascular pedicle is transected 3 cm below the tibial plateau.
Diseases
- Meacham Winn Culler syndrome
- Cholestasis, progressive familial intrahepatic 3
- Hypotonic sclerotic muscular dystrophy
- Meningitis
- Neuroleptic malignant syndrome
- Exudative retinopathy familial, autosomal dominant
- Urea cycle enzymopathies
- Radiation syndromes
- Uniparental disomy of 2
Once inserted hair loss in men quilted cheap finast 5 mg with visa, the gastric balloon is inflated with 300 mL of air and retracted to the gastric fundus hormonal hair loss cure finast 5 mg purchase with amex, where the varices at the oesophagogastric junction are tamponaded by the subsequent inflation of the oesophageal balloon to a pressure of 40 mmHg hair loss cure israel buy discount finast 5 mg line. Over a short period hair loss treatment viviscal buy cheap finast online, this has become the main treatment of variceal haemorrhage that has not responded to drug treatment and endoscopic therapy hair loss 4 year old buy discount finast on-line. The shunts are inserted under local anaesthetic, analgesia and sedation, using fluoroscopic guidance and ultrasonography. A satisfactory drop in portal venous pressure is usually associated with good control of the variceal haemorrhage. The main early complication of this technique is perforation of the liver capsule, which can be associated with fatal intraperitoneal haemorrhage. Post-shunt encephalopathy is a confusional state caused by the portal blood bypassing the detoxification of the liver. It occurs in about 40% of patients, a similar incidence to that found after surgical shunts. It is rarely considered for the acute management of variceal haemorrhage, as the morbidity and mortality in these circumstances are high. Long-term -blocker therapy and chronic sclerotherapy or banding are the main alternatives. Surgical shunts are an effective method of preventing rebleeding from oesophageal or gastric varices, as they reduce the pressure in the portal circulation by diverting the blood into the low-pressure systemic circulation. There is no evidence that prophylactic shunting is beneficial in patients with varices that have not bled. Injection of contrast into the portal vein flows through the metallic stent and outlines the right hepatic vein. Pressure measurements are taken from within the portal vein before and after insertion. Management of recurrent variceal bleeds secondary to splenic or portal vein thrombosis Treatment is by splenectomy and gastro-oesophageal devascularisation, in which the blood supply to the greater and lesser curve of the stomach and lower oesophagus is divided. Surgical shunts for portal hypertension involve shunting portal blood into the systemic veins. This commonly involves a side-to-side portocaval anastomosis (a) or end-to-side portocaval (b), mesocaval (c) or splenorenal (d) anastomoses. The management of variceal bleeding should always take into account the possibility of liver transplantation when this is available. Previous surgical shunts greatly increase the morbidity associated with orthotopic liver transplantation. The fluid accumulation is usually associated with abdominal discomfort and a dragging sensation. In those considered inappropriate for liver transplantation, management is aimed at symptomatic control of ascites. Intravenous contrast enhancement will allow abdominal varices to be demonstrated and assess patency of the portal vein, as portal vein thrombosis is a common predisposing factor to the development of ascites in chronic liver disease. Aspiration of the peritoneal fluid allows the measurement of protein content to determine whether the fluid is an exudate or transudate, and an amylase estimation to exclude pancreatic ascites. Cytology will determine the presence of malignant cells, and both microscopy and culture will exclude primary bacterial and tuberculous peritonitis. As a result of venous outflow obstruction, the liver becomes acutely congested, with the development of impaired liver function and, subsequently, portal hypertension, ascites and oesophageal varices. In an acute thrombosis, the patient may rapidly progress to fulminant liver failure but, Treatment of ascites in chronic liver disease the initial treatment is to restrict additional salt intake and commence diuretics using either spironolactone or furosemide. This should be combined with advice on avoiding any precipitating factors for impaired liver function, such as alcohol intake in patients with alcoholic cirrhosis. The cause of the venous thrombosis needs to be established, and an underlying myeloproliferative disorder or procoagulant state is commonly found, such as antithrombin 3, protein C or protein S deficiency. Patients presenting in fulminant liver failure should be considered for liver transplantation, as should those with established cirrhosis and the complications of portal hypertension. Primary sclerosing cholangitis this condition often presents in young adults with mild non-specific symptoms, and biliary disease is suggested by the finding of abnormal liver function tests. The disease process results in progressive fibrous stricturing and obliteration of both the intrahepatic and the extrahepatic bile ducts. If the radiological appearances are equivocal, a liver biopsy is required to demonstrate the fibrous obliteration of the biliary tracts. There is no specific treatment that can reverse the ductal changes, and the patients usually slowly progress to progressive cholestasis and death from liver failure. Further, imaging cannot reliably differentiate between inflammatory and malignant biliary strictures. Patients with good liver function, no dominant strictures and negative biliary cytology may simply be monitored for disease progression. The only useful treatment modality is liver transplantation, which is associated with excellent results if carried out before bile duct cancer has developed. Temporary relief of obstructive jaundice due to a dominant bile duct stricture can be achieved by biliary stenting, although there is considerable risk of cholangitis from the introduction of bacteria to the biliary tract. Diagnosis is suggested by the finding of circulating antismooth muscle antibodies and, if necessary, is confirmed by liver biopsy. The condition is slowly progressive, with deterioration in liver function resulting in lethargy and malaise. It may be complicated by the development of portal hypertension and the secondary complications of ascites and variceal bleeding. The condition is a medical emergency, and delay in appropriate treatment results in multiorgan failure secondary to septicaemia. Once the diagnosis has been confirmed, the patient should be commenced on a first-line broad spectrum antibiotic and rehydrated, and arrangements should be made for urgent endoscopic or percutaneous transhepatic drainage of the biliary tree. Biliary stone disease is a common predisposing factor, and the causative ductal stones may be removed at the time of endoscopic cholangiography by endoscopic sphincterotomy. Biliary stasis and stone formation combine to predispose to biliary sepsis, which may be life-threatening. Obstructed and septic bile ducts may be drained either radiologically or surgically. Malignant change within the ductal system results in cholangiocarcinoma, which may be amenable to resection. Pyogenic liver abscess the aetiology of a pyogenic liver abscess is unexplained in the majority of patients. Common causes include biliary stone disease and other causes of intra-abdominal sepsis, including appendicitis and diverticular disease. It has an increased incidence in the elderly, diabetics and the immunosuppressed, who usually present with anorexia, fevers and malaise, accompanied by right upper quadrant discomfort. The most common organisms are Streptococcus milleri and Escherichia coli, but other enteric organisms such as Streptococcus faecalis, Klebsiella and Proteus vulgaris also occur, and mixed growths are common. First-line antibiotics to be used are a penicillin, aminoglycoside and metronidazole or a cephalosporin and metronidazole. Percutaneous drainage without ultrasound guidance should be performed with caution as an empyema may follow drainage through the pleural space. A source for the liver abscess should be sought, Simple cystic disease Simple cysts are generally solitary, and occur more frequently in women. Most are incidental findings, and have a characteristic blue hue when seen at laparoscopy. Indications for surgical intervention include symptoms, rupture, haemorrhage, infection or indeterminate diagnosis. Surgical resection typically involves laparoscopic deroofing, with oversewing of the cyst wall. It is an autosomal dominant condition, more commonly seen in women, and around half of patients will also have polycystic kidneys. Indications for surgical intervention are broadly similar to those for simple cysts, although the large number of lesions means that deroofing a single cyst is unlikely to relieve symptoms. Computed tomography scan showing an airfluid level and rim enhancement with intravenous contrast typical of a liver abscess. Jacques Caroli, 19021979, Professor of Medicine, St Antoine Hospital, Paris, France, described the disease in 1958. Jean-Martin Charcot, 18251893, French neurologist and Professor of Pathology at Pitié-Salpêtrière Hospital, Paris, France. Atypical clinical or radiological findings should raise the possibility of a necrotic neoplasm. Amoebic liver abscess Entamoeba histolytica is endemic in many parts of the world. It exists in vegetative form outside the body and is spread by the faecaloral route. The most common presentation is with dysentery, but it may also present with an amoebic abscess, the common sites being paracaecal and in the liver. The amoebic cyst is ingested and develops into the trophozoite form in the colon, and then passes through the bowel wall and to the liver via the portal blood. Diagnosis is by isolation of the parasite from the liver lesion or the stool and confirming its nature by microscopy. Often patients with clinical signs of an amoebic abscess will be treated empirically with metronidazole (400 800 mg t. These were removed from the bile duct of a patient presenting with obstructive jaundice due to a hydatid liver cyst communicating with the bile duct. Hydatid liver disease this is a very common condition in countries around the Mediterranean and Middle East. The causative tapeworm, Echinococcus granulosus, is present in the dog intestine, and ova are ingested by humans and pass in the portal blood to the liver. Liver abscesses are often large by the time of presentation with upper abdominal discomfort or may present after minor abdominal trauma as an acute abdomen due to rupture of the cyst into the peritoneal cavity. Liver cysts can also rupture through the diaphragm producing an empyema, into the biliary tract producing obstructive jaundice, or into the stomach. Treatment is indicated to prevent progressive enlargement and rupture of the cysts. There are many reports that percutaneous treatment of hydatid cysts is safe and effective. Failure to respond to medical treatment or percutaneous treatment usually requires surgical intervention. The surgical options range from liver resection or local excision of the cysts to deroofing with evacuation of the contents. Contamination of the peritoneal cavity at the time of surgery with active hydatid daughters should be avoided by continuing drug therapy with albendazole and adding peroperative praziquantel. This should be combined with packing of the peritoneal cavity with 20% hypertonic saline-soaked packs and instilling 20% hypertonic saline into the cyst before it is opened. The residual cavity may become infected, and this may be reduced, as may bile leakage, by packing the space with pedicled greater omentum (an omentoplasty). If doubt exists as to whether a suspected cyst is active, it can be followed on ultrasound, as active cysts gradually become larger and more superficial in the liver. Rupture of daughter hydatids into the biliary tract may result in obstructive jaundice or acute cholangitis. This may be treated by endoscopic clearance of the daughter cysts prior to cyst removal from the liver. Active hydatid disease usually produces a non-calcified liver cyst and, within the cyst, floating layers of the germinal membrane can be seen. If necessary the incision can be extended across the midline transversely in the left upper quadrant. The procedure for complete mobilisation of the liver is described, although this will not be necessary in all cases. The left triangular ligament is divided, facilitated by placing a swab in front of the oesophagogastric junction. The right triangular ligament is then divided by retraction of the diaphragm away from the right lobe. This proceeds from above the renal veins until the main named hepatic veins are reached below the diaphragm. The parenchyma is divided along this plane of demarcation, commencing by diathermy of the liver capsule. Prospective evidence suggests there is no difference in speed of transection or blood loss between these methods. As the parenchyma is divided, vessels and bile duct branches are diathermised or ligated depending on their size. Dissection continues on until the hepatic vein branches are approached from within the liver parenchyma, when they are ligated or stapled then divided. Segmental and local resections Traditionally, surgical strategy has involved removal of the entire liver segment or hemiliver containing disease, with a view to providing the largest possible negative margin. This approach has no impact on long-term oncological outcome, and preserves liver remnants, so allowing the opportunity for further resection in the case of recurrent disease. These again may be slung to allow the remaining lymphatic tissue surrounding the portal vein to be ligated and divided. The possibility of a replaced right hepatic artery should be sought arising from the superior mesenteric artery and lying posterior to the bile duct (25% of people), and an accessory left hepatic artery from the left gastric artery in the lesser omentum (25% of people). Laparoscopic liver resections Laparoscopic liver surgery aims to provide curative resection while minimising postoperative time to recovery. There are Division of the parenchyma: hemihepatectomy Once the liver has been adequately mobilised and the hilar vessels have been exposed, the main inflow vessels and bile duct to the liver to be resected can be divided. Blood loss and transfusion the reduction of blood loss during liver surgery has been one of the major achievements in the last 20 years, and resection is often possible without blood transfusion. Better understanding of the segmental anatomy of the liver, better patient selection for surgery and low central venous pressure anaesthesia (<10 mmHg) have all helped to reduce the need for blood transfusions.
Cheap 5 mg finast with mastercard. How to GROW HAIR FAST | Japanese Hair Growth & Radiant Glowing Skin Secret | Camellia Oil |.
They typically present de novo with peak incidence in the fifth and sixth decades of life hair loss zoloft discount finast 5 mg buy on line, respectively hair loss cure coming soon finast 5 mg order fast delivery, or they may represent transformation of previously diagnosed hair loss cure in china buy genuine finast line, or clinically silent hair loss 3 months after stopping birth control discount finast 5 mg mastercard, low-grade gliomas hair loss 7 years order finast 5 mg without a prescription. Active treatment consists of maximal resection, high-dose focused radiation therapy, and chemotherapy administered locally as carmustine wafers at the time of resection and/or systemically with oral temozolomide. Meningioma Meningiomas are usually benign lesions, although anaplastic variants do occur. If the lesion is large or positioned so as to impinge on key structures, the patient may require steroids and early surgery. The degree of resection predicts recurrence, with rates of 10% at ten years for total excision with a clear dural margin and 30% at ten years for subtotal excision. Lesions that are difficult to approach surgically may be managed with radiotherapy or stereotactic radiosurgery. Microadenomas are less than 10 mm in size and usually present incidentally or with endocrine effects. Macroadenomas are larger than 10 mm, and often present with visual field deficits. Surgical resection is usually performed by a transsphenoidal approach through the nose, using a microscope or endoscope. Diabetes insipidus resulting from manipulation of the pituitary stalk is common in the immediate postoperative period and usually resolves spontaneously. Where it is suspected, the patient will require hourly measurement of urine output, and blood and urine samples for calculation of sodium concentration and osmolality. Pituitary apoplexy is the syndrome associated with haemorrhagic infarction of a pituitary tumour. It presents with sudden headache, visual loss and ophthalmoplegia with or without impaired conscious level. Endocrine resuscitation with intravenous steroids is the priority, and surgical decompression may be required. Vestibular schwannoma these are nerve sheath tumours arising in the cerebellopontine angle, which present with hearing loss, tinnitus and balance problems. Facial numbness and weakness are less common, while large tumours may present with features of brainstem compression or hydrocephalus. Baseline assessment of pituitary function should include serum prolactin, folliclestimulating hormone and luteinising hormone together with testosterone in males or oestradiol in females, thyroid function tests and fasting serum growth hormone and cortisol. Preoperative prolactin levels are crucial since prolactinomas may be managed without the need for surgery. Prolactinomas are managed initially with dopamine agonists such as bromocryptine and cabergoline. Growth hormone-secreting tumours may also respond to dopamine agonists or to somatostatin analogues such as octreotide. The cortisol level is also important, since deficiency must be corrected, especially in the perioperative period. Effective treatment requires close cooperation between the neurosurgical team and an endocrinologist. Harvey Williams Cushing, 18691939, Professor of Surgery at Harvard University Medical School, credited as the father of modern neurosurgery, and described the eponymous disease, but also pioneered new techniques in bacteriology, blood pressure measurement and electrocautery. Large lesions (>4 cm), especially with brainstem compression, will require excision and consideration of ventriculoperitoneal shunt to relieve hydrocephalus. Translabyrinthine, retrosigmoid and middle fossa approaches are possible, the latter options offering potential preservation of hearing in smaller tumours with some intact function at presentation. In removing larger tumours, it is often impossible to preserve hearing, or indeed facial nerve function. Cyst types include: Brain tumours in children Brain tumours are the most common solid tumours in children. Neural tube defects Failure of closure of the neural tube is associated with folate deficiency, family history and some anticonvulsants. Prenatal screening, using serum alphaprotein levels and ultrasound, and diagnostic testing, using amniocentesis, are possible. The spectrum of conditions associated with failed closure of the posterior neuropore includes the conditions described below. Sometimes it may be associated with tethered cord syndrome, which involves thickening of the filum terminale, resulting in traction on the cord. Presentation is with progressive deficits, spasticity, bladder dysfunction or scoliosis, and treatment involves surgical exploration and untethering of the cord. Pituitary tumours typically present with endocrinological disturbance (microadenomas) or visual deficits due to compression (macroadenomas). Some of these tumours are managed surgically, in close cooperation with endocrinologists Vestibular schwannomas (acoustic neuromas) are benign nerve sheath tumours, usually presenting with hearing loss, tinnitus and balance problems. Myelomeningocoele A herniating sac of meninges without covering skin contains spinal cord, nerves or both. Open myelomeningocoele presents a high infection risk and requires early surgical repair. In general these present with combinations of developmental delay, seizures and macrocephaly or hydrocephalus. Early fusion of one or more cranial sutures, craniosynostosis, is also a common neonatal presentation. Lipomyelomeningocoele Adipose tissue adherent to the spinal cord herniates through a bony defect to the sacrolumbar soft tissue. This may be associated with bladder dysfunction and require surgical relief of the resultant cord tethering. Failure of closure of the anterior neuropore produces anencephaly, which is uniformly fatal; the spectrum of spinal dysraphisms, however, is replicated in the skull. Cysts these benign fluid-filled intracranial lesions typically present incidentally or with mass effect or hydrocephalus. Type Scaphocephaly Brachycephaly Microcephaly Plagiocephaly Trigonocephaly Suture involved Sagittal suture Coronal suture All sutures involved Unilateral coronal/ lambdoid suture Metopic suture Clinical features Narrow boatshaped head Shortened/ broad forehead Small head Asymmetric skull Pointed narrow forehead Summary box 43. Imaging demonstrates a hypoplastic cerebellar vermis, with the posterior fossa occupied by a large thinwalled cyst. Epilepsy Up to 10% of the population will suffer a seizure at some point in their lives, and epilepsy, a syndrome of recurrent unprovoked seizures, represents the most common neurological disorder. About 2030% of patients fail to achieve adequate seizure control with drugs, and many of these focal epilepsies may benefit from surgery. In other cases the clinical picture, including seizure type, focal features and investigation results, can be used to identify the seizure focus. Dual pathology refers to the presence of an extrahippocampal lesion plus hippocampal atrophy, important because removal of both the lesion and the atrophic hippocampus will be necessary to achieve seizure control. Craniosynostosis Normal fusion of the coronal, lambdoidal, squamosal and sagittal sutures occurs between 6 and 12 months of age; others such as the frontal suture fuse later. Craniosynostosis is the premature fusion of one (simple craniosynostosis) or more (complex craniosynostosis) cranial sutures, preventing growth perpendicular to the suture. Syndromic craniosynostosis, often associated with abnormalities of the fibroblast growth factor receptor genes, is accompanied by developmental delay and other abnormalities. Electroencephalography entails recording from an array of scalp electrodes, and comparison between ictal and inter-ictal recordings. This is especially helpful in lateralising the focus of complex partial seizures in temporal lobe epilepsy, and is combined with video monitoring of the seizure in a videotelemetry suite. A more detailed localisation may be achieved invasively by the preoperative placement of subdural or depth electrodes or by intraoperative electrocorticography. Sodium amytal is injected into each internal carotid artery in turn, with simultaneous speech and memory testing to localise function. The aim is to confirm language laterality that resection on the side of the lesion will not significantly impair verbal memory functions. Awake craniotomy, allowing mapping particularly of speech centres, is increasingly employed. Mesial temporal epilepsy is commonly medically refractory and can be addressed surgically by amygdalohippocampectomy or resection of the temporal lobe including the mesial structures. The extent of resection is limited by the potential for damage to the optic tracts and to speech areas in the dominant hemisphere. With careful patient selection, cure rates of up to 70% or greater can be achieved. This is usually considered in the early years of life when plasticity and potential for functional recovery is greatest. Disconnection procedures include corpus callosotomy, used for patients suffering drop attacks, and subpial transections to isolate a seizure focus in eloquent brain from the surrounding cortex. Vagal nerve stimulators can be implanted in severe drug refractory epilepsy, with electrodes applied to the vagus nerve in the carotid sheath in the neck. This option can achieve effective seizure control, especially in children, although the mechanism is not clear. Inhibition of the action of these centres remains a valuable tool later in the course of the disease as the therapeutic window using levodopa narrows, but this is now generally achieved using deep brain stimulation with electrodes. This offers the advantage of an adjustable and reversible effect, and can be performed bilaterally where equivalent lesioning surgery would likely result in deficits. Deep brain stimulation is also an option for other movement disorders where less invasive approaches are ineffective. The pain is often attributable to impingement on the nerve by the superior cerebellar artery or other vessels, as first postulated by Walter Dandy. Occasionally another primary lesion is responsible; for example bilateral trigeminal neuralgia in younger patients is suggestive of multiple sclerosis. Where medications such as gabapentin and carbamazepine cannot achieve control, surgical options include: Pain syndromes Neurosurgical approaches to the relief of pain may address the underlying aetiology directly or may seek to interrupt or modulate the transmission responsible for the pain. The contrasting approaches are demonstrated in the management of trigeminal neuralgia. This manifests, generally in middle age or later, with paroxysmal lancinating pain in the distribution of one or more divisions of the trigeminal nerve. Craniotomy and microvascular decompression: this is designed to address the proposed origin of the neuropathic pain, by applying material between the nerve and adjacent vessel to prevent direct contact and stimulation. It achieves long-lasting relief of symptoms in about 80% of patients, but is associated with the standard risks of craniotomy and a significant incidence of cranial nerve deficit. Peripheral nerve injections can achieve good short-term relief of pain restricted to small areas supplied by terminal branches of the trigeminal. This permits lesioning of the ganglion by glycerol injection, radiofrequency thermocoagulation or balloon compression, with the aim of disrupting aberrant pain transmission. Electrical stimulation is used to modulate pain transmission: for example spinal cord stimulators can be applied to a range of pain syndromes especially associated failed spinal surgery. Deep brain stimulation targeting the periaqueductal grey and sensory thalamic nuclei has a role in chronic pain arising in the context of thalamic stroke. Implanted devices may also be used for intrathecal delivery of opiates for pain control, or baclofen to alleviate spasticity. Risks of craniotomy the risks associated with craniotomy are important to appreciate in discussing operations with patients and family, and in evaluating patients who deteriorate postoperatively. Brainstem death is legally equivalent to death, and is a precondition for the harvesting of organs for transplant from heart-beating donors. Diagnosis requires: identification of the cause of irreversible coma; exclusion of reversible causes of coma; clinical demonstration of the absence of brainstem function. The causative agent seems to be a misfolded protein, a prion, which is not destroyed by conventional sterilisation techniques. These include family history, receipt of pituitary-derived human growth hormone, cadaveric dura mater grafts and previous brain or spinal surgery prior to 1997. Where risk factors are present, instruments must be quarantined or destroyed postoperatively. Clear explanations of neurological and neurosurgical pathology supported by the best illustrations available in the field. The frontalis muscle may also contribute to eyelid elevation, particularly when the levator muscle is weak. Both lids are attached to the orbital rim by the medial and lateral canthal tendons. Both have a rich vascular supply and are innervated by the V1 division of the trigeminal nerve (cranial nerve V) above and the V2 division below. It merges into the sclera at the corneoscleral junction (the limbus), the insertion of the bulbar conjunctiva. It is perforated by the long and short posterior ciliary arteries and the vortex veins and is contiguous with the optic nerve sheath. The uvea comprises iris, Choroid Sclera Superior rectus Retina Lens Lacrimal system the almond-shaped lacrimal gland lies under the upper outer orbital rim and opens into the upper conjunctival fornix through 1015 ducts. Tears are swept across the globe by the lids and evaporate or pass into the upper and lower lid puncta, and then into the canaliculi to join the common canaliculus, which passes into the lacrimal sac under the medial canthal tendon. The sac is drained by the nasolacrimal duct into the nose, opening in the inferior meatus under the inferior turbinate. Johannes Peter Müller, 18011858, Professor of Anatomy and Physiology, Berlin, Germany. Johan Friedrich Horner, 18311886, Professor of Ophthalmology, Zurich, Switzerland, described this syndrome in 1869. Photoreceptor cells in the outer retina sense light and send impulses to retinal ganglion cells in the inner retina via bipolar cells. The retinal pigment epithelium underlies the photoreceptors and is responsible for reprocessing of photopigments. The optic nerve conveys the axons of retinal ganglion cells from the eye to the brain. The most high-resolution part of the retina, the macula, lies at the posterior pole within the vascular arcade.
Carum carvi (Caraway). Finast.
- How does Caraway work?
- What is Caraway?
- Dosing considerations for Caraway.
- Are there safety concerns?
- Indigestion. appetite stimulation, increasing digestive juices, constipation, gas, bloating, spasms of stomach and intestines, infection, inducing menstruation, relieving menstrual cramps, increasing milk flow in nursing mothers, improving blood flow, and other conditions.
- Are there any interactions with medications?
- Stomach upset, when used in combination with other herbs.
Source: http://www.rxlist.com/script/main/art.asp?articlekey=96237
References
- Natvig K, Larsen TE. 1978.
- Sapino A, Bussolati G. Is detection of endocrine cells in breast adenocarcinoma of diagnostic and clinical significance? Histopathology. 2002;40(3):211-214.
- Alfonsi P. Postanaesthetic shivering: epidemiology, pathophysiology, and approaches to prevention and management. Drugs. 2001;61:2193-2205.
- Asensio JA, Demetriades D, Hoyt DB. Vascular injuries: complex and challenging injuries. Part 1: Surg Clin of North Am. 2001;81.
- Marks LS, Partin AW, Gormley GJ, et al: Prostate tissue composition and response to finasteride in men with symptomatic benign prostatic hyperplasia, J Urol 157(6):2171n2178, 1997.
- Rusch V, Baselga J, Cordon-Cardo C, et al. Differential expression of the epidermal growth factor receptor and its ligands in primary non-small cell lung cancers and adjacent benign lung. Cancer Res 1993;53(10 Suppl):2379- 2385.
- Hyland ME, Whalley B. Motivational concordance: an important mechanism in self-help therapeutic rituals involving inert (placebo) substances. J Psychosom Res. 2008;65(5):405-413.
- Eisensehr I, Linke R, Noachtar S, et al. Reduced striatal dopamine transporters in idiopathic rapid eye movement sleep behaviour disorder: comparison with Parkinsonis disease and controls. Brain 2000;123 (Pt 6):1155-60.
