
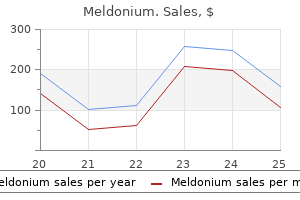
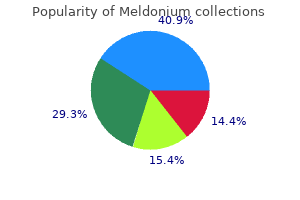
Meldonium
| Contato
Página Inicial
Paul Berkowitz, MD
- Medical Director, Inpatient Services
- Department of Psychiatry
- Desert Vista Behavioral Health Center
- Mesa, Arizona
ExoU expression by Pseudomonas aeruginosa correlates with acute cytotoxicity and epithelial injury abro oil treatment purchase meldonium us. Exoproduct secretions of Pseudomonas aeruginosa strains influence severity of alveolar epithelial injury treatment zoster ophthalmicus order meldonium cheap. Pseudomonas aeruginosa ExoT induces atypical anoikis apoptosis in target host cells by transforming Crk adaptor protein into a cytotoxin symptoms uterine cancer purchase meldonium amex. Mortality factor 4 like 1 protein mediates epithelial cell death in a mouse model of pneumonia symptoms 6dpo discount meldonium 250 mg buy. Evolution of bronchoalveolar cell populations in the adult respiratory distress syndrome symptoms ulcer stomach 500 mg meldonium purchase free shipping. Transepithelial migration of neutrophils: mechanisms and implications for acute lung injury. Recruitment of neutrophils into the alveolar spaces without a change in protein permeability. Neutrophil recruitment and increased permeability during acute lung injury induced by lipopolysaccharide. Regulation of neutrophilic inflammation by proteinase-activated receptor 1 during bacterial pulmonary infection. Neutrophil depletion suppresses pulmonary vascular hyperpermeability and occurrence of pulmonary edema caused by hantavirus infection in C. Acid aspiration-induced lung injury in rabbits is mediated by interleukin-8-dependent mechanisms. Neutrophils and their Fc gamma receptors are essential in a mouse model of transfusion-related acute lung injury. The effects of neutrophil depletion on a completely noninvasive model of acute pancreatitis-associated lung injury. Neutrophils and neutrophil products do not mediate pulmonary hemodynamic effects of endotoxin on oleic acid-induced lung injury. Dissociation between alveolar transmigration of neutrophils and lung injury in hyperoxia. Mice lacking neutrophil elastase reveal impaired host defense against gram negative bacterial sepsis. Degradation of outer membrane protein A in Escherichia coli killing by neutrophil elastase. Plasma elastase levels and the development of the adult respiratory distress syndrome. Elastolytic activity in pulmonary lavage fluid from patients with adult respiratory-distress syndrome. The presence of neutrophil elastase and evidence of oxidation activity in bronchoalveolar lavage fluid of patients with adult respiratory distress syndrome. Alpha-1 antitrypsin reduces severity of pseudomonas pneumonia in mice and inhibits epithelial barrier disruption and pseudomonas invasion of respiratory epithelial cells. Elastase inhibition reduced death associated with acid aspiration-induced lung injury in hamsters. Na) and neutrophil depletion using a granulotrap (G-1) column on lung reperfusion injury in dogs. Delayed neutrophil elastase inhibition prevents subsequent progression of acute lung injury induced by endotoxin inhalation in hamsters. Impaired immunity and enhanced resistance to endotoxin in the absence of neutrophil elastase and cathepsin G. Neutrophil elastase is needed for neutrophil emigration into lungs in ventilatorinduced lung injury. Neutrophil transmigration triggers repair of the lung epithelium via beta-catenin signaling. Unopposed cathepsin G, neutrophil elastase, and proteinase 3 cause severe lung damage and emphysema. Internalization of proteinase 3 is concomitant with endothelial cell apoptosis and internalization of myeloperoxidase with generation of intracellular oxidants. Neutrophil defensins mediate acute inflammatory response and lung dysfunction in dose-related fashion. Neutrophil alpha-defensins cause lung injury by disrupting the capillary-epithelial barrier. Pulmonary surfactant protein A protects lung epithelium from cytotoxicity of human beta-defensin 3. Differential effects of alpha- and beta-defensin on cytokine production by cultured human bronchial epithelial cells. Higher concentrations of matrix metalloproteinases in bronchoalveolar lavage fluid of patients with adult respiratory distress syndrome. Gelatinases in epithelial lining fluid of patients with adult respiratory distress syndrome. Matrix metalloproteinases and matrix metalloproteinase inhibitors in acute lung injury. Matrix metalloproteinase inhibitor prevents acute lung injury after cardiopulmonary bypass. Inhibition of matrix metalloproteinase-9 prevents neutrophilic inflammation in ventilator-induced lung injury. Tissue inhibitor of metalloproteinase-1 deficiency amplifies acute lung injury in bleomycin-exposed mice. Requirement for macrophage elastase for cigarette smoke-induced emphysema in mice. Matrix metalloproteinase-8 inactivates macrophage inflammatory protein-1 alpha to reduce acute lung inflammation and injury in mice. Matrix metalloproteinases in acute lung injury: mediators of injury and drivers of repair. Epilysin (matrix metalloproteinase-28) contributes to airway epithelial cell survival. Migration and gelatinases in cultured fetal, adult, and hyperoxic alveolar epithelial cells. High concentrations of alpha-defensins in plasma and bronchoalveolar lavage fluid of patients with acute respiratory distress syndrome. Defensins reduce the barrier integrity of a cultured epithelial monolayer without cytotoxicity. Increased hydrogen peroxide in the expired breath of patients with acute hypoxemic respiratory failure. Nitric oxide and nitrotyrosine in the lungs of patients with acute respiratory distress syndrome. Increased levels of nitrate and surfactant protein a nitration in the pulmonary edema fluid of patients with acute lung injury. Quantitation of nitrotyrosine levels in lung sections of patients and animals with acute lung injury. Liposomal antioxidants provide prolonged protection against acute respiratory distress syndrome. Vitamin E reduces transendothelial migration of neutrophils and prevents lung injury in endotoxin-induced airway inflammation. Evidence for extracellular superoxide dismutase as a mediator of hemorrhage-induced lung injury. Extracellular superoxide dismutase in the airways of transgenic mice reduces inflammation and attenuates lung toxicity following hyperoxia. Identification of oxidative stress and Toll-like receptor 4 signaling as a key pathway of acute lung injury. The effects of hyperoxic injury and antioxidant vitamins on death and proliferation of human small airway epithelial cells. Reactive oxygen species and extracellular signal-regulated kinase 1/2 mitogen-activated protein kinase mediate hyperoxia-induced cell death in lung epithelium. Acute Respiratory Distress Syndrome Chapter 10 203 [194] Carvalho H, Evelson P, Sigaud S, Gonzalez-Flecha B. Mitogen-activated protein kinases modulate H(2)O(2)-induced apoptosis in primary rat alveolar epithelial cells. Activation of hypoxia-inducible factor-1 protects airway epithelium against oxidant-induced barrier dysfunction. Claudins: control of barrier function and regulation in response to oxidant stress. Inhibition of regulatory-associated protein of mechanistic target of rapamycin prevents hyperoxia-induced lung injury by enhancing autophagy and reducing apoptosis in neonatal mice. Oxidants spontaneously released by alveolar macrophages of cigarette smokers can inactivate the active site of alpha 1-antitrypsin, rendering it ineffective as an inhibitor of neutrophil elastase. N-Acetylcysteine treatment to prevent the progression of multisystem organ failure: a prospective, randomized, placebo-controlled study. Treatment with N-acetylcysteine during acute respiratory distress syndrome: a randomized, double-blind, placebo-controlled clinical study. Platelets induce neutrophil extracellular traps in transfusion-related acute lung injury. Excessive neutrophils and neutrophil extracellular traps contribute to acute lung injury of influenza pneumonitis. Extracellular histones are essential effectors of C5aR- and C5L2-mediated tissue damage and inflammation in acute lung injury. Extracellular histones play an inflammatory role in acid aspiration-induced acute respiratory distress syndrome. Neutrophil extracellular traps directly induce epithelial and endothelial cell death: a predominant role of histones. Circulating nucleosomes are associated with mortality in pediatric acute respiratory distress syndrome. Platelet depletion and aspirin treatment protect mice in a two-event model of transfusion-related acute lung injury. Complete reversal of acid-induced acute lung injury by blocking of platelet-neutrophil aggregation. Hyperoxia causes angiopoietin 2-mediated acute lung injury and necrotic cell death. Inhibition of prolyl hydroxylase attenuates fas ligand-induced apoptosis and lung injury in mice. ResolvinD1 reduces apoptosis and inflammation in primary human alveolar epithelial type 2 cells. Pathogenicity of influenza viruses with genes from the 1918 pandemic virus: functional roles of alveolar macrophages and neutrophils in limiting virus replication and mortality in mice. Alveolar macrophages are indispensable for controlling influenza viruses in lungs of pigs. Innate immunity in the lung: how epithelial cells fight against respiratory pathogens. Respiratory epithelial cells regulate lung inflammation in response to inhaled endotoxin. Human Toll-like receptor 2 mediates induction of the antimicrobial peptide human beta-defensin 2 in response to bacterial lipoprotein. Pulmonary surfactant protein D in first-line innate defence against influenza A virus infections. Surfactant proteins A and D inhibit the growth of Gram-negative bacteria by increasing membrane permeability. Innate immune collectin surfactant protein D simultaneously binds both neutrophil extracellular traps and carbohydrate ligands and promotes bacterial trapping. Pulmonary surfactant phosphatidylglycerol inhibits respiratory syncytial virus-induced inflammation and infection. Expression of functional toll-like receptor-2 and -4 on alveolar epithelial cells. Lung epithelial cells are essential effectors of inducible resistance to pneumonia. Pulmonary stromal-derived factor-1 expression and effect on neutrophil recruitment during acute lung injury. Chemokine expression during hepatic ischemia/reperfusioninduced lung injury in the rat. The role of alveolar epithelial cells in initiating and shaping pulmonary immune responses: communication between innate and adaptive immune systems. Macrophage tumor necrosis factor-alpha induces epithelial expression of granulocyte-macrophage colony-stimulating factor: impact on alveolar epithelial repair. Sessile alveolar macrophages communicate with alveolar epithelium to modulate immunity. Pathogenesis and reversibility of the pulmonary lesions of oxygen toxicity in monkeys. Multiple stromal populations contribute to pulmonary fibrosis without evidence for epithelial to mesenchymal transition. Keratinocyte growth factor accelerates wound closure in airway epithelium during cyclic mechanical strain. Keratinocyte growth factor enhances barrier function without altering claudin expression in primary alveolar epithelial cells. Keratinocyte growth factor promotes epithelial survival and resolution in a human model of lung injury. A randomized trial of recombinant human granulocytemacrophage colony stimulating factor for patients with acute lung injury. Endothelial-derived angiocrine signals induce and sustain regenerative lung alveolarization. Foxp3 1 Regulatory T Cell Expression Of Keratinocyte Growth Factor During Acute Lung Injury Resolution. Beta-catenin/T-cell factor signaling is activated during lung injury and promotes the survival and migration of alveolar epithelial cells.
With additional multisystem organ dysfunction medicine rap song order 500 mg meldonium mastercard, systemic inflammatory response symptoms white tongue purchase 500 mg meldonium free shipping, hemodilution from the circuit 4 medications at target 250 mg meldonium free shipping, and acute renal failure that is associated with critically ill patients medicine rheumatoid arthritis purchase meldonium with paypal, drug responses can be difficult to predict medications in carry on luggage buy cheap meldonium 250 mg on line, and possibilities range from drug toxicity to lack of effect. Video-assisted thoracoscopic repair was performed in a postpneumonectomy patient who was not a candidate for one-lung ventilation. A relatively shorter setup time with the smaller portable circuits allows use outside the operating room and interhospital transport. Lower levels of systemic anticoagulation and percutaneous Seldinger-guided access contribute to its relatively greater use recently. This is best monitored by an arterial catheter and pulse oximeter in the right upper extremity to detect proximal arterial desaturation. Tsushima and colleagues suggested that the annual incidence of acute lung failure was approximately 190,000 cases per year in the United States alone. All patients underwent peripheral cannulation, predominantly femoral-jugular, and the Cardiohelp system was used for 20. The overall survival rate was 56%, with 33% of patients dying during mechanical support and 11% dying after weaning. Risk factors that did affect survival included renal failure, advanced age, and multiple organ failure. The past decade has witnessed a dramatic increase in the number of lung transplantations and a significant improvement in 1-year survival rates, increasing from 75% to more than 80%. Stern and coworkers reported a 90% mortality rate for patients with idiopathic pulmonary fibrosis on mechanical ventilation. Some recent case series have reported encouraging short- and medium-term survival rates for the bridge-to-lung transplantation group. Garcia and colleagues120 described use of the jugular, bicaval, double-lumen, 23-Fr Avalon Elite cannula. The clots can disrupt the function of the membrane oxygenator, inhibit pump function, and embolize to vital organs. Clinicians can use heparin-bonded circuits to reduce the risk of thrombus formation and lower the level of anticoagulation needed in the immediate period after circuit implementation. In addition to reducing the risk of thrombus formation, heparinbonded circuits reduce inflammation by decreasing complement and granulocyte activation. Patients with heparin-induced thrombocytopenia should avoid contact with heparin-bonded circuits, and the circuit should be changed to a nonheparin-bonded circuit. It allows patients to be maintained on low levels of anticoagulation for prolonged periods. The test result is reported as the duration in seconds, with longer times reflecting higher degrees of anticoagulation. In the case of flow abnormalities, pump head thrombosis must be ruled out, and it can be suggested by a sudden change in the sound from the pump, hemolysis, or thrombocytopenia. More than 50% of cases showed preceding, significant alterations in gas exchange, laboratory values (ie, increased D-dimers, decreased fibrinogen, decreased platelet count, lactate dehydrogenase level elevation, and an increase in plasma free hemoglobin), or increased resistance to blood flow through the circuit. If they are on the venous side of the circuit, air aspiration and gas embolism can occur. Immediate replacement of the affected portion of the circuit or the entire apparatus may be indicated. It is usually caused by creation of a significant negative pressure and air entrainment in the circuit. Treatment must be immediate, with prompt circuit shutoff and clamping, simultaneous full ventilator support, and circuit de-airing. Longterm functional neurologic outcome data for adults and children need more study. In this group, chromosomal abnormalities, time to lactate normalization, and high inotrope scores predict poor cognitive outcomes. Other than cannulation site bleeding, mucosal bleeding can occur from the airway to stomach, colon or rectum, and bladder with minor, repeated trauma or instrumentation. Anemia can be an issue because the circuit is usually primed with a crystalloid solution that causes dilution of blood cells. Extracorporeal membrane oxygenation for pediatric respiratory failure: history, development and current status. Contemporary extracorporeal membrane oxygenation for adult respiratory failure: life support in the new era. Prolonged extracorporeal oxygenation for acute post-traumatic respiratory failure (shock-lung syndrome): use of the Bramson membrane lung. Extracorporeal membrane oxygenation in severe acute respiratory failure: a randomized prospective study. Extracorporeal life support for 100 adult patients with severe respiratory failure. Joint statement on mechanical circulatory support in children: a consensus review from the Pediatric Cardiac Intensive Care Society and Extracorporeal Life Support Organization. Recommendations for the use of mechanical circulatory support: device strategies and patient selection. Extracorporeal membrane oxygenation for 2009 influenza A(H1N1) acute respiratory distress syndrome. Extracorporeal membrane oxygenation for severe influenza A (H1N1) acute respiratory distress syndrome: a prospective observational comparative study. Rescue therapy in adult and pediatric patients with pH1N1 influenza infection: a tertiary center intensive care unit experience from April to October 2009. Influenza A pandemics: clinical and organizational aspects: the experience in Chile. Extracorporeal lung support for patients who had severe respiratory failure secondary to influenza A (H1N1) 2009 infection in Canada. The first novel influenza A (H1N1) fatality despite antiviral treatment and extracorporeal membrane oxygenation in Hong Kong. Extracorporeal membrane oxygenation use has increased by 433% in adults in the United States from 2006 to 2011. Extracorporeal membrane oxygenation for treating severe cardiac and respiratory disease in adults. Early experience with a polymethyl pentene oxygenator for adult extracorporeal life support. Poly-methyl pentene oxygenators have improved gas exchange capability and reduced transfusion requirements in adult extracorporeal membrane oxygenation. Attenuation of changes in leukocyte surface markers and complement activation with heparin-coated cardiopulmonary bypass. Hemolysis during cardiac extracorporeal membrane oxygenation: a case-control comparison of roller pumps and centrifugal pumps in a pediatric population. Hemolytic characteristics of three commercially available centrifugal blood pumps. Extracorporeal membrane oxygenation for treating severe cardiac and respiratory failure in adults. Trans-diaphragmatic left ventricular venting during peripheral venous-arterial extracorporeal membrane oxygenation. Impella to unload the left ventricle during peripheral extracorporeal membrane oxygenation. Combination use of a TandemHeart with an extracorporeal oxygenator in the treatment of five patients with refractory cardiogenic shock after acute myocardial infarction. Balloon atrial septostomy for left ventricular decompression in patients receiving extracorporeal membrane oxygenation for myocardial failure. Percutaneous left-heart decompression during extracorporeal membrane oxygenation: an alternative to surgical and transeptal venting in adult patients. Extracorporeal life support devices and strategies for management of acute cardiorespiratory failure in adult patients: a comprehensive review. Venovenous extracorporeal membrane oxygenation in adults: practical aspects of circuits, cannulae, and procedures. Insertion of bicaval dual lumen extracorporeal membrane oxygenation catheter with image guidance. Initial experience with single cannulation for venovenous extracorporeal oxygenation in adults. Pharmacokinetic changes in patients receiving extracorporeal membrane oxygenation. In vitro evaluation of sedative drug losses during extracorporeal membrane oxygenation. Congenital diaphragmatic hernia requiring extracorporeal membrane oxygenation: does timing of repair matter Outcome analysis of neonates with congenital diaphragmatic hernia treated with venovenous vs venoarterial extracorporeal membrane oxygenation. Use of extracorporeal membrane oxygenation during resection of tracheal papillomatosis. Extra corporal membrane oxygenation in general thoracic surgery: a new single veno-venous cannulation. Post-pneumonectomy video-assisted thoracoscopic bullectomy using extra-corporeal membrane oxygenation. The need for thoracic surgery in adult patients receiving extracorporeal membrane oxygenation: a 16-year experience. Cardiac arrest in special circumstances: electrolyte abnormalities, poisoning, drowning, accidental hypothermia, hyperthermia, asthma, anaphylaxis, cardiac surgery, trauma, pregnancy, electrocution. Prolonged extracorporeal membrane oxygenationassisted support provides improved survival in hypothermic patients with cardiocirculatory arrest. Successful use of venovenous extracorporeal membrane oxygenation in accidental hypothermic cardiac arrest. Extracorporeal membrane oxygenation as a bridge to emergency heart-lung transplantation in a patient with idiopathic pulmonary arterial hypertension. Venovenous extracorporeal life support after pulmonary endarterectomy: indications, techniques, and outcomes. Veno-venous extracorporeal membrane oxygenation bridging to pharmacotherapy in pulmonary arterial hypertensive crisis. Use of venovenous extracorporeal membrane oxygenation and an atrial septostomy for pulmonary and right ventricular failure. Mechanical support for pulmonary veno-occlusive disease: combined atrial septostomy and venovenous extracorporeal membrane oxygenation. First experiences with a new miniaturised life support system for mobile percutaneous cardiopulmonary bypass. First experience with the ultra compact mobile extracorporeal membrane oxygenation system Cardiohelp in interhospital transport. The Registry of the International Society for Heart and Lung Transplantation: 29th adult lung and heart-lung transplant report-2012. Prognosis of patients with advanced idiopathic pulmonary fibrosis requiring mechanical ventilation for acute respiratory failure. Primary lung transplantation after bridge with extracorporeal membrane oxygenation: a plea for a shift in our paradigms for indications. Should lung transplantation be performed for patients on mechanical respiratory support Extracorporeal membrane oxygenation as a bridge to lung transplant: midterm outcomes. Physiotherapy for patients on awake extracorporeal membrane oxygenation: a systematic review. Extracorporeal membrane oxygenation in nonintubated patients as bridge to lung transplantation. Organ allocation waiting time during extracorporeal bridge to lung transplant affects outcomes. Ambulatory veno-venous extracorporeal membrane oxygenation: innovation and pitfalls. Outcome of extracorporeal membrane oxygenation as a bridge to lung transplantation: an institutional experience and literature review. Ambulatory extracorporeal membrane oxygenation: a new approach for bridge-to-lung transplantation. Interventional lung assist: a new concept of protective ventilation in bridge to lung transplantation. The Novalung interventional lung assist as bridge to lung transplantation for self-ventilating patients: initial experience. Bridge to thoracic organ transplantation in patients with pulmonary arterial hypertension using a pumpless lung assist device. Modified technique using Novalung as bridge to transplant in pulmonary hypertension. Extracorporeal pumpless interventional lung assist in clinical practice: determinants of efficacy. The use of helmets to deliver non-invasive continuous positive airway pressure in hypoxemic acute respiratory failure. Up to 151 days of continuous animal perfusion with trivial heparin infusion by the application of a long-term durable antithrombogenic coating to a combination of a seal-less centrifugal pump and a diffusion membrane oxygenator. Quantitative measurement of heparin in comparison with conventional anticoagulation monitoring and the risk of thrombotic events in adults on extracorporeal membrane oxygenation. Efficiency in extracorporeal membrane oxygenation: cellular deposits on polymethylpentene membranes increase resistance to blood flow and reduce gas exchange capacity. Technical complications during veno-venous extracorporeal membrane oxygenation and their relevance predicting a system-exchange: retrospective analysis of 265 cases. Extracorporeal membrane oxygenation cannulation trends for pediatric respiratory failure and central nervous system injury. Two-year survival, mental, and motor outcomes after cardiac extracorporeal life support at less than five years of age.
Purchase meldonium us. Tropic Thunder - Best of Jeff Portnoy / Jack Black / Hot LZ.
This water vapor would be synonymous with pulmonary exudate and medications xanax buy meldonium 500 mg without a prescription, when excessive treatment goals for depression buy generic meldonium 500 mg on line, mimics pulmonary edema associated with permeability changes of the alveolar capillary membrane medications an 627 purchase meldonium 500 mg with amex. As fluid moves through a conduit 909 treatment purchase generic meldonium online, laminae are established symptoms joint pain cheap meldonium 250 mg with mastercard, with the highest velocity of flow achieved in the center of the tube. At the same time, the outermost layers, nearest the walls of the conduit, effectively have no velocity because of the drag coefficient of the inside surface. The laminar effect can be disrupted by several techniques that produce a "secondary flow," facilitating increased gas exchange. Laminar flow is reduced in hollow-fiber oxygenators with blood flow through the fibers by the expansion and contraction of the capillaries via the movement of blood through them, gently disrupting the boundary layers. Estimating the total surface area of material necessary for gas exchange is a function of the predicted oxygen demands of the patient, the pattern of flow within the device. As the surface area of an oxygenator increases, the volume of solution necessary to prime the system increases. Contemporary designs have blood flow around hollow fibers with gas flowing through the fibers. Those with shorter blood flow paths require more fiber surface area to achieve a similar oxygen transfer. Systems that use the latter design require a lower membrane surface area for gas exchange and hence result in lower prime volumes. The oxygenator represents the largest source of nonendothelialized surface area in the extracorporeal circuit, ranging in size between 0. Dickinson and associates102 conducted an in vitro analysis that showed significant air-handling differences between the oxygenators from four different manufacturers. Venous and Cardiotomy Reservoirs There are two general categories for venous reservoirs: open and closed systems (Box 32. Filters and defoaming compartments in the venous reservoir and air-trapping ports located at the highest level of the blood flow path within the oxygenator are areas designed to allow passive removal of air. The large buoyant air migrates to the top of the reservoir and escapes through strategically placed vents on the reservoir cover. With open systems, the circulating blood is exposed to a larger and more complex surface that contains defoaming sponges and antifoam agents. It has been reported that occlusion of the vacuum source line can cause pressurization of the venous reservoir and introduction of a gas embolism to the patient through the venous line. Recently, several randomized clinical trials have found superior clinical outcomes with a system equipped with a closed reservoir and a centrifugal arterial pump. Levels of complement 3a, thromboxane B2, fibrin degradation products, and elastase were significantly greater in open reservoir patients. The authors suggested that limiting increases in these markers would be best accomplished by eliminating cardiotomy suction and routinely using heparin-bonded circuits whenever possible. All have eliminated or isolated the venous reservoir to reduce blood foreign surface contact, and all eliminated the introduction of activated blood from a cardiotomy suction system. Furthermore, shed blood at the surgical field could be readily collected and reintroduced into the circulation with conventional systems using the cardiotomy suction system without the use of an autotransfuser. With most of the minisystems, minor changes in the circuit or complete major reconfiguration of the minisystem may be necessary if excessive bleeding occurs at the surgical field (addition of a venous reservoir, addition of a cardiotomy reservoir, and transfer of a massive amount of blood from the autotransfuser collection reservoir back to the minisystem). Minisystems do not facilitate emptying of the cardiac chambers as well as do conventional systems. Safe use of these systems requires good communication among the surgeon, anesthesiologist, and the perfusion team, together with careful monitoring. These major differences have made some centers reluctant to change to these new systems. Further studies are necessary to substantiate the benefit of such systems and will likely increase the adoption of this new technology. Maquet has designed a new system aimed to improve the safety and ease of transporting patients supported with an extracorporeal live support. Early reported experience with this system has been favorable in terms of ease of set up, performance, and portability. However, in either of these scenarios, external warming blankets and ambient room temperature are controlled to restrict declines in patient temperature. Stainless steel is the most durable and chemically inert of all commercially used heat exchangers. The ideal heat exchanger must possess the following characteristics: low resistance to blood flow, freedom from defects in material that could facilitate the mixture of blood and water, low priming volume, and disposability. The effectiveness of a heat exchanger depends on several factors, including total surface area, thickness of the conductor walls, thermal conductivity, and the residence time of blood through the device. As fluid flow through a heat exchanger is increased, the performance characteristics decline, primarily as a function of decreased residence time in the device. Heat exchanger basic design consists of two separate phases, with water passing on one side and blood, or perfusate, on the other. The direction of blood flow is routinely countercurrent to the flow of water, optimizing heat transfer. The temperature of the water entering the heat exchanger is controlled by either an external cooler/heater device or a wall source, with a temperature range from 4°C to 42°C. The majority of heat transfer occurs by the process of conduction, in which thermal energy is passed from water to blood. Heat exchangers can be placed in the circuit in a variety of locations, although the most common location is on the proximal side of the oxygenator, often termed an integral heat exchanger. Increased risk would be directly proportional to the oxygen tension of blood, which would enhance the rate solubility shifts. Other potential risks of heat exchangers are associated with the type of material used for construction. Because stainless steel is relatively expensive, aluminum has been used most often as the material for heat exchangers. Aluminum, however, has a high toxicity in humans; when blood levels exceed 100 mg/L, careful patient monitoring is imperative and levels greater than 200 mg/L are toxic. This change in materials was considered to reduce manufacturing costs and aid in the disposal of used oxygenators. Miniaturized cardiopulmonary bypass improves shortterm outcome in cardiac surgery: a meta-analysis of randomized controlled studies. Eventually, a grounding cable was added to prevent such leaks, but the Forte oxygenator was taken off the market because clinicians had no confidence in it. Regardless of the material used and despite careful manufacturing, heat exchangers must be tested before use. The heat exchange coefficient can be calculated for various devices over steady-state conditions, which would provide comparative analysis data on heat exchanger efficiency. Cooler/Heater Units Cooler/heater units consist of a system that provides a thermoregulated water supply and can circulate water between 40 to 420C to the heater exchanger through a 1 2 -inch internal diameter water tube. The latter design is preferable in that the pressure on the water side of the oxygenator heat exchanger will then always be lower than the pressure in blood side. There have been numerous reports of mycobacterium contamination from cooler/ heater unit water supplied to the oxygenator heat exchanger or to the cardioplegia delivery heat exchanger, resulting in endocarditis or death. Some studies suggest that 20-µm screen filtration is superior to 40-µm filtration in the reduction of cerebral embolic counts. A systematic review of the data related to arterial line filtration reported that the level of evidence supporting this practice was high (class I level of evidence A). Screen filters trap particulate and gaseous emboli that are of larger diameter than their effective pore size. The filter material is accordion pleated to provide a larger surface area within a lower prime housing. Two contemporary filter designs consist of a larger flat screen surface that is located concentrically around the oxygenator fiber bundle. The Terumo F series filter incorporates the screen material concentrically surrounding the fiber bundle. Sorin Group has incorporated a concentric filter design that surrounds the fiber bundle. This design does not effectively reduce prime volume; however, the larger housing provides an effective bubble trap (Box 32. However, as with most technologic advances, it is the combination of all component parts that function to ensure success. Besides the pump and oxygenator, a seamless array of tubing is required to connect the patient to the heart-lung machine. Monitoring lines are necessary not only to ensure patient hemodynamic management but also to assess the proper function of the pump. Manufacturers of tubing and circuit packs can attest to the large number of variations in combinations and configurations of circuit assemblies requested by different institutions, as well as by individual clinicians within the same institution. Numerous cannulae are available for all types of cardiac surgery, which may reflect the developmental philosophy that if a vessel could conceivably be perfused or drained, then a cannula could be made to facilitate insertion. In the past, cannulae were constructed of stainless steel or tapered polyvinylchloride. Subsequently, thin-walled stainless steel was used to increase effective orifice diameter and reduce cannulae pressure drop across the cannulae. Currently, most cannulae are fabricated from polyvinylchloride with composite polycarbonate thin-walled tips. The ends of the cannulae are formed to permit easy vascular entry while maintaining maximum lumen (caliber) size. According to Poiseuille mechanics, the greatest resistance, measured as pressure drop in a circuit, is found at the smallest opening for fluid flow and has an inverse exponential relation to the fourth power of the radius of the lumen. Therefore to reduce pressure drops across the circuit, cannulae are selected to facilitate the greatest flow with the least injury to the vessel because of mechanical abrasion. Several new designs of venous cannulas have recently emerged that incorporate a malleable, wire-reinforced backbone to allow for bending of the catheter without kinking the lumen. Cannulae could then be positioned out of the surgical field to provide an unobstructed view for the surgeon. The axillary or subclavian artery often is selected for arterial return for patients with severe atherosclerosis of the ascending aorta. This site offers the advantage of providing antegrade flow to the arch vessels, protection of the arm and hand, and avoidance of inadvertent cannulation of the false lumen in cases in which type A aortic dissection has occurred. Alternatively, the arterial tubing line can be connected directly to the Dacron graft with the aid of a tubing connector. Transapical aortic cannulation through a 1-cm incision on the anterior wall of the left ventricle also has been described for patients with type A dissection. Plasticizers impart flexibility into tubing and account for as much as 40% of the polymer. Perfusion during coronary and mitral valve surgery utilizing minimally invasive port-access technology. Mixed venous oxygen saturation is measured by optical or chemical fluorescence by flow through cells placed in the venous line. A stopcock is placed in the venous line to facilitate the delivery of medications and for venous sampling. Blood then enters the venous reservoir, which serves as a volume chamber for settling and acts as a safety feature, providing additional response time to the perfusionist. Hardshell reservoirs are open to the atmosphere (open systems) through a ventilation port on top of the reservoir and are effective in handling gross quantities of air that may return through the venous or cardiotomy line. The venous reservoir also has an inlet line that drains blood from a cardiotomy reservoir. A cardiotomy reservoir is simply a second chamber used for collecting and filtering blood aspirated from the surgical field via suction lines. Vented blood from the left ventricle, pulmonary artery, or aortic root also is returned to the venous reservoir through the cardiotomy device. These are hard-shell devices made of polycarbonate housing material with polyurethane and polyester filters and defoamers to reduce the risk for gas embolism into the venous reservoir. Some venous reservoirs also serve as integral cardiotomy reservoirs, obviating the need for a separate unit. From the venous reservoir, blood is pumped into the heat exchanger of a membrane oxygenator by the actions of the arterial pump. The heat exchanger is connected to an external water source that maintains the perfusate temperature according to the temperature of the water pumped from the cooler/heater. The gas blender is attached to the inlet gas port of the oxygenator via a section of 1/4-inch tubing and a bacteriostatic (0. Gas exchange across the blood and gas phases of the fiber occurs through the process of simple diffusion. Levels of high gas molecule concentration are permitted to diffuse through tiny slit pores of the oxygenator fiber strands to lower levels of gas concentration. Many circuits also have a vaporizer for the delivery of volatile, inhaled anesthetic gases placed in-line between the gas blender and the oxygenator. The oxygenator has two ports on the outflow side by which arterialized blood is accessed: a recirculation port and an arterial outlet port. The recirculation port is used both to provide a safety line for relieving overpressurization and to facilitate easy replacement in the event of device failure. It also is used as an exit port of arterialized blood for sanguineous cardioplegia or in the separate perfusion of a second arterial cannula. By incorporating both components together, the use of most integrated oxygenators results in a significant decrease in foreign surface area and resultant prime volume. The arterial filter is a screen device constructed of synthetic material, with a specific pore size effectively blocking particles greater in size than the rating of the filter (20 and 40 µm). Just distal to the arterial line filter is a bubble detector that is an essential feature for the conduct of safe perfusion. This device is controlled by a microprocessor and is used to detect microgaseous and macrogaseous emboli.
Multicenter preoperative stroke risk index for patients undergoing coronary artery bypass graft surgery medications used to treat ptsd order meldonium now. Association of fast-track cardiac management and low-dose to moderate-dose glucocorticoid administration with perioperative hyperglycemia medicine vs dentistry order meldonium 250 mg with visa. Perioperative glycemic control and the risk of infectious complications in a cohort of adults with diabetes inoar hair treatment meldonium 500 mg purchase. The association of diabetes and glucose control with surgicalsite infections among cardiothoracic surgery patients symptoms tonsillitis generic 500 mg meldonium amex. Nurse-administered subcutaneous morphine is a satisfactory alternative to intravenous patient-controlled analgesia morphine after cardiac surgery medicine used for anxiety cheap meldonium online mastercard. Patient-controlled versus nurse-controlled analgesia after cardiac surgery: a meta-analysis. Intrathecal morphine in the management of pain following cardiac surgery: a comparison with morphine i. Effects of intrathecal opioid on extubation time, analgesia, and intensive care unit stay following coronary artery bypass grafting. Neuraxial blockade and hematoma in cardiac surgery: estimating the risk of a rare adverse event that has not (yet) occurred. Efficacy of ketorolac tromethamine and extrapleural intercostal nerve block on post-thoracotomy pain: a prospective, randomized study. Non-steroidal anti-inflammatory drugs in treatment of postoperative pain after cardiac surgery. Saphenous vein graft patency 1 year after coronary artery bypass surgery and effects of antiplatelet therapy: results of a Veterans Administration Cooperative Study. Implications of preoperative administration of aspirin in patients undergoing coronary artery bypass grafting. Collaborative overview of randomised trials of antiplatelet therapy-I: Prevention of death, myocardial infarction, and stroke by prolonged antiplatelet therapy in various categories of patients. Effect of metoprolol on death and cardiac events during a 2-year period after coronary artery bypass grafting. Myocardial protection with prophylactic oral metoprolol during coronary artery bypass grafting surgery: evaluation by troponin I. Are beta-blockers effective in elderly patients who undergo coronary revascularization after acute myocardial infarction The effect of aggressive lowering of low-density lipoprotein cholesterol levels and low-dose anticoagulation on obstructive changes in saphenous-vein coronary-artery bypass grafts. Perioperative statin therapy is associated with a significant and dose-dependent reduction of adverse cardiovascular outcomes after coronary artery bypass graft surgery. Statin pretreatment and risk of in-hospital atrial fibrillation among patients undergoing cardiac surgery: a collaborative meta-analysis of 11 randomized controlled trials. Endorsed by the Society of Cardiovascular Anesthesiologists, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons. Reduced anticoagulation after mechanical aortic valve replacement: interim results from the prospective randomized on-X valve anticoagulation clinical trial randomized Food and Drug Administration investigational device exemption trial. Carotid artery disease and stroke during coronary artery bypass: a critical review of the literature. Postoperative atrial fibrillation is a major cause of stroke after on-pump coronary artery bypass surgery. Off-pump coronary artery bypass grafting reduces mortality and stroke in patients with atheromatous aortas: a case control study. Effects of admission hyperglycemia on mortality and costs in acute ischemic stroke. Perfusion deficit parallels exacerbation of cerebral ischemia/ reperfusion injury in hyperglycemic rats. Predictors of delirium after cardiac surgery delirium: effect of beating-heart (off-pump) surgery. Incidence and risk factors for delirium and other adverse outcomes in older adults after coronary artery bypass graft surgery. Meta-analysis of antiarrhythmic therapy in the prevention of postoperative atrial fibrillation and the effect on hospital length of stay, costs, cerebrovascular accidents, and mortality in patients undergoing cardiac surgery. Interventions on prevention of postoperative atrial fibrillation in patients undergoing heart surgery: a meta-analysis. Magnesium infusion dramatically decreases the incidence of atrial fibrillation after coronary artery bypass grafting. Effect of rate or rhythm control on quality of life in persistent atrial fibrillation. Factors that predict the use of positive inotropic drug support after cardiac valve surgery. Diagnosis and treatment of shock due to massive pulmonary embolism: approach with transesophageal echocardiography and intrapulmonary thrombolysis. Diagnostic accuracy of transesophageal echocardiography during cardiopulmonary resuscitation. Clinical and echocardiographic diagnoses disagree in patients with unexplained hemodynamic instability after cardiac surgery. The use of transesophageal echocardiography for preload assessment in critically ill patients. Assessment of ventricular function in critically ill patients: limitations of pulmonary artery catheterization. Combined inotropic effects of amrinone and epinephrine after cardiopulmonary bypass in humans. Effectiveness of intraaortic balloon pumping in patients who were not able to be weaned from cardiopulmonary bypass after coronary artery bypass surgery and mortality predictors in the perioperative and early postoperative period. Coronary artery bypass grafting in patients with severe left ventricular dysfunction: a prospective randomized study on the timing of perioperative intraaortic balloon pump support. Optimal timing of preoperative intraaortic balloon pump support in high-risk coronary patients. Effective surgical management of high-risk coronary patients using preoperative intra-aortic balloon counterpulsation therapy. Intraaortic balloon pumping for cardiac support: trends in practice and outcome, 1968 to 1995. Right ventricular function in cardiovascular disease, part I: Anatomy, physiology, aging, and functional assessment of the right ventricle. An analysis of the association between preoperative renal dysfunction and outcome in cardiac surgery: estimated creatinine clearance or plasma creatinine level as measures of renal function. The use of diuretics and dopamine in acute renal failure: a systematic review of the evidence. Efficacy of N-acetylcysteine in preventing renal injury after heart surgery: a systematic review of randomized trials. Role of N-acetylcysteine in prevention of contrast-induced nephropathy after cardiovascular procedures: a meta-analysis. Comparison of coronary bypass surgery with angioplasty in patients with multivessel disease. Five-year outcome after coronary angioplasty versus bypass surgery in multivessel coronary artery disease: results from the French Monocentric Study. A randomized study of coronary angioplasty compared with bypass surgery in patients with symptomatic multivessel coronary disease. A meta-analysis of randomized controlled trials comparing coronary artery bypass graft with percutaneous transluminal coronary angioplasty: one- to eight-year outcomes. Five-year outcome in patients with isolated proximal left anterior descending coronary artery stenosis treated by angioplasty or left internal mammary artery grafting: a prospective trial. Off-pump coronary artery bypass in patients with left ventricular dysfunction: a meta-analysis. Off-pump coronary artery bypass may increase late mortality: a meta-analysis of randomized trials. Postoperative cardiovascular dysfunction is becoming more common as older and increasingly critically ill patients undergo cardiac surgical procedures. Pharmacologic therapy with suitable monitoring and mechanical support may be needed for patients in the postoperative period until ventricular or circulatory dysfunction improves. This article reviews management considerations of patients with postoperative circulatory failure. As hemoglobin concentration increases, so does blood viscosity and therefore the work of the heart to eject the blood. In normal hearts (eg, athletes), increasing hemoglobin levels to supranormal increases performance, a finding suggesting that in this setting the increased viscosity is less important than the elevated oxygen-carrying capacity. Model analysis of data from animal investigations suggested that maintenance of the hematocrit between 30% and 33% provides the best balance between oxygen-carrying capacity and viscosity. Patients needing continued inotropic or mechanical support of ventricular function beyond the first few postoperative hours, especially patients in need of intravascular volume expansion, should probably be transfused to a hematocrit in this range, bearing in mind that blood transfusion has been associated with decreased organ function and increased mortality rates in critically ill patients. This study supports the concept that this is the desirable hematocrit especially in older cardiac surgical patients or in patients experiencing a complicated course. In patients with marginal arterial oxygenation, pulmonary function must be closely monitored to allow prompt therapy to be undertaken for abnormalities. Measurements of airway resistance and respiratory system compliance should be made. Patients with pulmonary disease may experience dramatic worsening of oxygenation when vasodilator therapy is started because of release of hypoxic vasoconstriction in areas of diseased lung. Reduced doses of direct-acting vasodilators or trials of different agents may be indicated. For example, sedation and paralysis may buy time to allow reversible postoperative myocardial dysfunction to improve. Previous reports found that administration of nitroprusside and the use of high flows (>2. Unless end-tidal carbon dioxide is monitored or arterial blood gases are analyzed often to show the increased carbon dioxide production and to guide increases in ventilation, hypercarbia will occur, causing catecholamine release, tachycardia, and pulmonary hypertension. Muscle relaxation may provide more stable hemodynamic conditions than meperidine, but accompanying sedation must be administered to avoid having an awake and paralyzed patient. Often, over minutes, a patient who needs vasodilators for hypertension then requires vasopressors or large volumes of fluid for hypotension. It is important to recognize when these changes result from changes in body temperature, to avoid attributing them to other processes that may call for different therapy. Assessment of the Circulation Physical Examination Surgical dressings, chest tubes attached to suction, fluid in the mediastinum and pleural spaces, peripheral edema, and temperature gradients can distort or mask information obtained by the classic techniques of inspection, palpation, and auscultation in the postoperative period. However, the physician should not be deterred from applying these basic techniques in view of their potential benefit. Physical examination may be of great value in diagnosing gross or acute disease, such as pneumothorax, hemothorax, or acute valvular insufficiency, but it is of limited value in diagnosing and managing ventricular failure. For example, in the critical care setting, experienced clinicians (eg, internists) using only physical findings often misjudge cardiac filling pressures by a large margin. That no such trials have been conducted in cardiac surgical patients probably attests to the reluctance of cardiac surgeons and anesthesiologists to manage their patients without what they consider to be important information. In one study, this decline was evident only in one-half of the patients,44 but in the other studies, more than 90% of patients showed at least a transient decrease in function. Decreased ventricular performance at normal or elevated filling pressures occurs, suggesting decreased contractility. Satisfactory myocardial protection is important to prevent postoperative dysfunction. Although little consensus exists that any one technique is preferable in all circumstances, cold intermittent crystalloid cardioplegia with systemic hypothermia is the most widely used technique clinically. Salerno and associates54 recommended continuous, warm, retrograde blood cardioplegia without systemic hypothermia, and Mullen and colleagues50 suggested that blood cardioplegia had at least a short-term benefit with less myocardial damage and better function; however, other studies of blood cardioplegia have had mixed results4752 (see Chapters 31 and 32). Other proposed factors that contribute to postoperative ventricular dysfunction include myocardial ischemia,55 residual hypothermia,46,47 preoperative medications such as -adrenergic antagonists,53 and ischemia-reperfusion injury (Box 38. Inflammatory cell activation from cytokine generation, upregulation of neutrophil adhesion molecules with neutrophil activation, oxygen free radical formation, and lipoperoxidation after ischemia-reperfusion injury may be important pathways accounting for the dysfunction. Multiple studies showed the importance of limiting myocardial ischemia-reperfusion injury. Studies evaluating complement inhibition with pexelizumab in improving outcomes described a novel strategy that unfortunately was never approved despite promising results61 (see Chapter 9). Postoperative Myocardial Ischemia Although intraoperative myocardial ischemia has often been a focus, studies showed that ischemia frequently occurs postoperatively and is associated with adverse cardiac outcomes. Surprisingly, these abnormalities most often appeared in the regions of the heart that had been revascularized. Score is defined as follows: 0, normal; 1, mild hypokinesis; 2, severe hypokinesis with myocardial thickening; 3, akinesis; and 4, dyskinesis. Prognostic importance of postbypass regional wall motion abnormalities in patients undergoing coronary artery bypass graft surgery. Early recovery, or fast-tracking, of the cardiac surgical patient has led to some concern that ischemia will occur as patients awaken early after the operation in pain, especially because Mangano and colleagues63 showed that sedation with a sufentanil infusion could reduce ischemia in this period. In most patients, pharmacologic interventions can be rapidly weaned or stopped within the first 24 hours postoperatively. Ventricular tachycardia or fibrillation Ischemia Catecholamines Postoperative Arrhythmias Patients with preoperative or newly acquired noncompliant ventricles need a correctly timed atrial contraction to provide satisfactory ventricular filling, especially when they are in sinus rhythm preoperatively. Although atrial contraction provides approximately 20% of ventricular filling, this may be more important in postoperative patients, when ventricular dysfunction and reduced compliance may be present. Rate and rhythm disorders must be corrected when possible, using epicardial pacing wires.
References
- Hung YP, Dong F, Watkins JC, et al. Identification of ALK rearrangements in malignant peritoneal mesothelioma. JAMA Oncol 2018;4(2):235-238.
- Giardini A, Khambadkone S, Taylor A, et al. Effect of abnormal pulmonary flow distribution on ventilatory efficiency and exercise capacity after arterial switch operation for transposition of great arteries. Am J Cardiol. 2010;106:1023- 28.
- Poulton TJ, Walker RA: Helicopter cooling of heat stroke victims. Aviat Space Environ Med 58:358, 1987.
- Rupp SM, Apfelbaum JL, Blitt C, et al. Practice guidelines for central venous access: a report by the American Society of Anesthesiologists Task Force on Central Venous Access. Anesthesiology. 2012;116(3):539-573.
