
Raloxifene
| Contato
Página Inicial
Elizabeth B. Yerkes, MD
- Assistant Professor of Urology, Northwestern University,
- Feinberg School of Medicine
- Attending Urologist,
- Children's Memorial Hospital, Chicago, Illinois
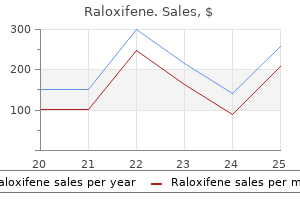
Systemic administration of the vectors has the disadvantage of systemic toxicity including viral hepatitis and encephalitis women's reproductive health issues and controversies order raloxifene 60 mg line. Several techniques of intracochlear vector delivery have been developed and their efficacy and safety have been compared and contrasted breast cancer 5k atlanta 2014 60 mg raloxifene visa. The first three methods have the advantage of a controlled steady intracochlear perfusion women's health center eureka ca purchase raloxifene 60 mg, but have the disadvantage of potentially physically damaging the architecture of the cochlea womens health diet pill 60 mg raloxifene amex. Gelfoam soaked with the vector solution applied to the round window is noninvasive and nondestructive womens health imaging generic 60 mg raloxifene free shipping, and does not cause disruption to the anatomy of the inner ear. It has also been shown that transgene expression in the contralateral, noninjected cochlea occurs, suggesting that systemic dissemination could potentially be associated with direct delivery methods. Hair cells in the cochlea are very vulnerable to disruption of their homeostasis and tend to die if they cannot function normally. One approach to treating deafness could be to trigger regeneration of cochlear hair cells. However, there is no point in stimulating the regeneration of hair cells that are unable to function because of a genetic defect. Accurate diagnosis combined with dual treatment of stem cell insertion and gene transfer would be vital for this approach to succeed. Over recent times, the potential of somatic stem cells for therapeutic applications has become almost infinite, limited only by the ingenuity of investigators in the manipulation of their genomes and culture conditions. However, demonstration of transgene expression in tissues outside the treated cochlea raises concerns about the safety of its application regarding systemic dissemination of the vectors used. It may be more feasible to treat post-natal progressive deafness and/or vestibular disorders by using this approach, but the exact pattern of expression and functions of the genes involved must be understood prior to such intervention. In addition, the attitudes of the patients and their families and their views on such intervention must be respected. The deaf community in the United Kingdom is very advanced, with its own culture and there has been anecdotal evidence that deaf couples do not necessarily want their children to be able to hear if it means that they will be excluded from the deaf community to which their parents belong (see Chapter 69, Investigation and management of the deaf child). Drug therapy An alternative approach is based on drugs, which, by definition, are small molecules with ready access to the target cells. We may be able to exploit alternative pathways to carry out the task that is affected by a mutation. For example, connexin 26 mutation is thought to the most common cause of nonsyndromic deafness in the Caucasian population. Another connexin may be capable of substituting for connexin 26 in forming gap junctions, but its gene may not normally be expressed in the cochlea. A drug might therefore be developed to activate expression of the alternative connexin gene in the cells needing to form gap junctions. Clues about which alternative pathways might be worth exploiting will come from investigations of interacting genes. Prenatal tests for congenital abnormalities including Down syndrome, cystic fibrosis and spina bifida are performed by the end of the first trimester and it would be too late if interventions were to be implemented to the developing ear at this stage. The rudimentary pinna has formed by 60 days and in the fourth month convolutions have attained their adult form, although further enlargement continues during the remaining months of gestation and also in the post-natal period. Direct gene transfer or stem cell insertion into the inner ear at the embryonic stage would involve some form of intrauterine surgery and surgical intervention on the human foetus has been performed for more than two decades in the United States. Genetic abnormalities cause not only congenital deafness; several genes have been found that, when mutated, either cause or predispose to progressive hearing loss. Understanding the molecular biology of the auditory system may be the key to the future development of genetic counselling and treatment for congenital deafness. Surgical intervention involving inner ear gene transfer on human embryos seems a good idea, but is still rather far-fetched with the technology currently available. Chapter 66 Molecular otology, development of the auditory system and recent advances in genetic manipulation] 819 Deficiencies in current knowledge and areas for future research Genetic testing for deafness is now a reality and has changed the paradigm for evaluating deaf patients. It will be used by surgeons for diagnostic purposes and as a basis for treatment and management options. Mutation screening is currently available for only a limited number of genes, such as connexin 26. In these cases, diagnosis, carrier detection and reproductive risk counselling can be provided. In the future, there will be an expansion of the role of genetic testing and counselling will not be limited to reproductive planning. Treatment and management decisions will be made based on specific genetic diagnoses. New discoveries and technologies will expand and increase the complexity of genetic testing options. Otolaryngologists will therefore have to familiarize themselves with current discoveries and accepted protocols for genetic testing. Prevalence of permanent childhood hearing impairment in the United Kingdom and implications for universal neonatal hearing screening: Questionnaire based ascertainment study. A clinically relevant article explaining the incidence of congenital deafness and the need for universal neonatal hearing screening 2. Hoxa1 and Hoxb1 synergize in patterning the hindbrain, cranial nerves and second pharyngeal arch. Goosecoid cell acts autonomously in mesenchyme-derived tissues during craniofacial development. Targeted mutation of the murine goosecoid gene results in craniofacial defects and neonatal death. Elevated blood pressure and craniofacial abnormalities in mice deficient in endothelin-1. Dual genetic pathways of endothelin-mediated intercellular signaling revealed by targeted disruption of endothelin converting enzyme-1 gene. Signaling pathways crucial for craniofacial development revealed by endothelin-A receptor-deficient mice. Null mutation of Dlx-2 results in abnormal morphogenesis of proximal first and second branchial arch derivatives and abnormal differentiation in the forebrain. Formation of the middle ear: Recent progress on the developmental and molecular mechanisms. A homeotic transformation is generated in the rostral branchial region of the head by disruption of Hoxa-2, which acts as a selector gene. Descriptive and experimental analysis of the epithelial remodellings that control semicircular canal formation in the developing mouse inner ear. A beautifully written account of the science behind the various modes of possible gene therapy. A good summary of experiments that have been carried out in cochlear gene transfer in the world literature. Expression of adeno-associated virus integrated transgene within the mammalian vestibular organs. Safety of adeno-associated virus as cochlear gene transfer vector: Analysis of distant spread beyond injected cochleae. An interesting and easy to follow article on current issues in stem cell/ gene therapy in general. Thus, this chapter starts with an outline of the key definitions and principles of screening, before proceeding to review evidence on the prevalence of different types of childhood hearing loss. The case for newborn screening is summarized and evidence for current performance of newborn screens reviewed. Other approaches to screening and surveillance in the preschool years are also reviewed (the eight-month screen, the school entry screen) and the position with regard to temporary childhood hearing loss discussed. Traditionally health service professionals have considered surveillance essentially as secondary prevention through early detection. However, the concept that child health depends upon continuous vigilance and supervision by health professionals is fairly narrow and supervisory; child health surveillance is now regarded as just one component of child health promotion programmes which aim to promote partnership between parents, children and health professionals, in which parents are empowered to make use of services and expertise according to their needs. Accurate early diagnosis of serious conditions offers the opportunity to initiate treatment before the disease progresses (or to intervene to mitigate the consequences of the impairment). Even though screening can potentially help to save lives or improve the quality of life through early diagnosis of serious conditions, it is not an infallible process. Screening can potentially reduce the risk of developing a disease (or impairment) or its complications (or consequences). However, in all screening programmes there are inevitably individuals who are referred as having the condition but do not (false positives), and who are not referred but do have the condition (false negatives). From an ethical viewpoint, screening differs from responsive clinical practice, since screening is targeting individuals who appear healthy and is offering to help individuals make an informed choice about their health or the health of their children. It is particularly important for individuals who consent to be screened or have their child screened to be aware of the risks involved and have reasonable expectations of a screening programme. Assessing programmes in this way is intended to ensure that they are more beneficial than harmful, and can be implemented at reasonable cost. When research has shown screening to be effective in reducing mortality and morbidity from a particular condition, the National Screening Committee may decide to pilot the proposed screening programme. This provides valuable information on the effectiveness, feasibility and public acceptability of screening when performed in an ordinary health service setting rather than a specialist research site. The cost of case finding (including all consequential costs of the screening programme) should not be disproportionate to overall healthcare costs of care for the hearing-impaired child. There should be guidelines on how to explain results to parents with appropriate support. All hearing screening arrangements should be reviewed in the light of changes in demography, epidemiology and other factors. Cost and effectiveness of hearing screening should be examined on a case-type basis to maximize the effectiveness and benefit for each type before considering overall costs, effectiveness and benefits. There are a number of key definitions relevant to screening programmes which should be used in the quality assurance and audit of any screening programme: Coverage is the proportion of the target population who undergo the screen. Screen positive result is a screening result that is greater than or equal to a specified cut-off level. This level is based upon evidence for the benefits of early intervention in moderate or greater hearing loss. A truepositive is an individual with a screen-positive result who has the condition (impairment). A false-positive is an individual with a screen-positive result who does not have the target condition (impairment). Screen negative result is a screening result that is less than the specified cut-off level. A true-negative is an individual with a screen-negative result who does not have the condition (impairment). A false-negative is an individual with a screen-negative result who does in fact have the condition (impairment). Effective screening programmes attempt to reduce false-negatives to the irreducible minimum, while keeping false-positives within manageable service levels. The aim of a screen is to refer on a manageable proportion of the population for further (diagnostic) tests, that proportion being likely to contain as many of the true cases in the population as possible. Sensitivity is the rate of true-positives or the proportion of individuals with the target condition in Chapter 67 Hearing loss in preschool children: screening and surveillance] 823 the population who are correctly identified by the screen. The term can be applied to a screening test, if (as is the case with newborn hearing screening) the screen consists of more than one test, or to the screen as a whole, or indeed to the screening programme. Test sensitivity is the proportion of individuals who were given the test, have the condition (impairment) and were detected by the test. Screen sensitivity is the proportion of individuals who completed the screen who have the condition (impairment) and who were detected by the screen (which may consist of more than one test with conditional pass/refer rules). Programme sensitivity is the proportion of the subjects in the whole population with the specified condition (impairment) who are detected by the screening programme. It is a product of the screen sensitivity and the coverage achieved by the screen programme. Specificity is the rate of true-negatives or the proportion of individuals free of the target condition in the population who are correctly identified as such by the screen. As with sensitivity, the term specificity may be applied at the level of test, screen or programme. Positive predictive value is the proportion of individuals with a positive test result who have the target condition. The yield is sometimes expressed as the number of cases identified via the screen per 1000 individuals screened, thus allowing comparison with published prevalence figures, and acting as a surrogate for sensitivity (since sensitivity can only be established in retrospect, once all false-negative and missed cases have been found). The yield of a screen is affected by coverage and sensitivity, and affects the cost per case identified. Finally, the incremental yield is the number of true cases referred by a screen when any true cases that would have been or were identified by preceding screening, surveillance programmes or responsive services are excluded. Incidence is the number of new instances of the condition (impairment) occurring during a certain period. Thus, in an average-sized health community with 5000 births per year, an incidence of between five and ten cases of congenital permanent moderate or greater bilateral hearing loss might be expected. Prevalence is the total number of individuals who have a given disease or condition (impairment) at a given point in time per population figure. The extended Wilson and Junger screening criteria identify costs and effectiveness as important issues for screening programmes (points 9 and 14 above). Considerable effort was put into the ascertainment process such that the authors believe that over 90 percent of all known cases were found. Based on the birth cohorts for 19851990, the prevalence of moderate-to-profound congenital permanent bilateral hearing loss was 1. Data were collected in years 19981999 within a strict ethical framework from both health (audiology) and education (support services for hearing impaired children). Once duplicate data had been excluded, there were 17,160 cases, giving an overall prevalence of 1.
None of the following had any discernible influence on the outcome of surgery in comparative studies: perforation size (less versus greater than 50 percent) women's health questions online purchase raloxifene with visa, prior or concurrent adenoidectomy 100 Spontaneous healing of chronic tympanic membrane perforations is uncommon triple negative breast cancer raloxifene 60 mg order mastercard, and medical interventions are not effective in promoting perforation closure womens health partners st louis cheap raloxifene 60 mg buy online. Surgical intervention is the treatment of choice to effect closure of the perforation women's health center of york order raloxifene 60 mg amex. The medical literature provides ample evidence that when this is performed in an adept manner women's health gcb x discount raloxifene line, a high rate of closure is possible in adults, in the short to medium term at least. Chapter 74 Chronic otitis media in childhood] 939 (yes/no), status of the contralateral ear (normal/not normal) or Eustachian tube test result (good/poor) (see Table 74. They also compared variables between studies which had not been quantitatively assessed within any existing paper: infection at the time of surgery (yes/ no) and surgical technique (overlay/underlay) and, again, found no significantly discernible influence on outcome. Subsequent papers Since the tympanoplasty metaanalysis, there have been a number of papers describing tympanoplasty with cartilage repair of the tympanic membrane. It should be remembered that the same claims were made about fascia repair of the tympanic membrane in small children. Until such time as rigorous analysis of sufficient numbers with age-related data is performed then such can claims cannot be regarded as proven. Indeed, histological analysis of temporal bones not infrequently identifies the presence of middle ear inflammation behind an intact tympanic membrane. Detailed analysis of hearing outcomes in paediatric tympanoplasty is restricted because of the lack of raw data from existing studies. Elimination of middle ear pathology Sheehy and Shelton have suggested that tympanoplasty should eradicate pathological conditions from the middle Table 74. Long-term follow-up data which do not use such probabilistic techniques are often meaningless and possibly misleading. The only paper using life-table analysis to study tympanoplasty in children has shown a deterioration over time of the repaired tympanic membrane due to increasing perforation and myringitis. Even at one year following surgery, untreated middle ear inflammation has caused, through effusion, perforation and myringitis, the disease free rate to drop to 0. The decision to offer surgical treatment in a child with a tympanic membrane perforation should therefore not be a reflex initiated by sighting the perforation. A planned delay in surgical treatment prolongs the period during which infection may enter from the ear canal so diligent use of prophylactic manoeuvres must be employed to maintain a dry ear. For the patient with no interest in swimming the extra care required to control infections may be very small. When washing the hair or face, a water-resistant barrier should also be used to exclude any stray drops. Maintaining a dry ear requires extra care when the child takes an interest in swimming. The options for care include banning swimming or permitting limited surface swimming with the use of a barrier in the ear canal. Since most children greatly enjoy swimming, provision of swim plugs and advice about avoiding diving below the surface of the water should be routinely provided while awaiting surgical closure of the perforation. It will rarely be possible for the surgeon to confidently offer a discernible improvement in hearing. Some patients with no ear discharge, minimal hearing loss and no compromise of daily activity may justifiably prefer to decline an offer of surgical intervention. Tympanosclerosis, atelectasis and myringitis may all be found accompanying a perforation on the same eardrum. The aim of tympanoplasty is to restore the middle ear including the sound transformer. Thus, the extent of surgery deemed to be adequate varies according to the severity of the disease. More severe disease may require attention to the middle ear space and tympanic membrane, as well as the perforation. The tympanic membrane may be entirely healthy apart from the presence of a small perforation. In this circumstance the intervention required to close the hole may be no more than excision of the rim of the perforation with the placement of a small graft to close the defect. This procedure also requires secure reinforcement of the entire tympanic membrane around the defect so that the graft obturates the perforation and is in contact with the entire rim of the perforation. Although reabsorbable materials are sometimes inserted into the middle ear to support this tissue, it is possible to support the graft on the annulus and manubrium. Because of extensive coexisting tympanic membrane disease, reinforcement of the entire tympanic membrane with temporalis fascia, tragal perichondrium or cartilage is frequently necessary. It is also possible to reduce thickened mucosa that physically impedes placement of a graft. Injury to the mucosa of the medial surface of the middle ear may cause adhesions to the tympanic membrane graft during healing. In addition, factors that narrow the slender middle ear cleft, such as thickened middle ear mucosa or retraction of the umbo increase this risk. Under any of the preceding circumstances, it is prudent to insert a barrier to prevent contact between the medial and lateral surfaces during healing. Umbo retraction is particularly common in perforations with extensive loss of the inferior part of the tympanic membrane. If the umbo retraction is particularly marked, it may be necessary to disarticulate the ossicular chain to lateralize the manubrium satisfactorily. The malleus head is excised and a malleus to stapes assembly is performed in addition to the tympanic membrane repair. Amputation of the umbo should not be performed as this greatly diminishes acoustic transmission through the middle ear. It should be that this figure is gleaned from case series proffered by motivated individuals with a special interest in otology in children. More typical figures for success rate by British surgeons seems to be between 74 percent (small Chapter 74 Chronic otitis media in childhood] 941 perforation) and 56 percent (large perforation). The surgical repair of the tympanic membrane is a difficult procedure requiring considerable skill. It is debatable whether any surgeon should continue to offer this treatment if his/her success rate for the procedure is as low as 56 percent. Following the loss of this stiff structural element, the thinned area of tympanic membrane can be more easily displaced by the pressure difference across the tympanic membrane. Should the middle ear pressure be raised, as after sleep, the tympanic membrane may bulge laterally. The posterosuperior pars tensa is more vascular than other areas of the tympanic membrane and may be subject to more marked inflammatory reactions. Some cases of tympanic membrane collapse are Chronic otitis media and the pathology of atrophy of the pars tensa of the tympanic membrane Atrophy of the pars tensa of the tympanic membrane occurs through loss of the collagenous fibrous layer. In the presence of an open Eustachian tube, sniffing results in a sharp reduction in Eustachian tube and middle ear pressure. An unwanted consequence of the sharp drop in middle ear pressure is retraction of the tympanic membrane. The benefit resulting from sniffing is closure of the tube and cessation of the unpleasant symptoms. The fundus of the retraction pocket is not wholly visible and there is some accumulation of skin in the retracted area. These have largely followed the original, using an ordinal scale largely based on anatomical features of the retraction pocket. For the most advanced stage of most of these classifications, the definition reflects the role of retraction pockets in the genesis of cholesteatoma by including a nonanatomical feature such as adherence of the pocket or keratin accumulation within the pocket. A recent, innovative classification has also reflected the tendency of retraction pockets to damage the ossicular chain by including an audiometric parameter. Definitions and classification Thus, pars tensa retraction includes not only a range of appearances, but also a clinically important minority which will insidiously deteriorate. Terminology and classifications were specifically designed to attempt to distinguish the high-risk subgroup, which progresses to cholesteatoma. In this ear there is erosion of the manubrium, the incus, the scutum and the posterior annulus as well as the development of a cholesteatoma. The tympanic membrane of this young man is almost entirely atrophic and retracted. The fundus of the retraction pocket is not entirely visible but the pocket remains selfcleaning. The manubrium, the long process of the incus and the stapes superstructure have all been eroded. Although there is air in the protympanum, the atrophic tympanic membrane is draped over the facial nerve and the stapes footplate. The last feature has resulted in elevation of the hearing threshold being restricted to 30 dB hearing loss. This is his better hearing ear and the hospital notes indicate his ear has remained unchanged for over a decade. The age distribution of patients whose retracted tympanic membranes cause sufficient concern to prompt surgery is not necessarily the same as the prevalence of retracted tympanic membranes in the community. This strikingly confirms that intervention for tympanic membrane retraction is predominantly a paediatric problem. Retraction without atrophy (grade I atelectasis) is usually a transitory condition. It rarely progresses to more advanced stages and frequently reverts to a normal tympanic membrane. This behaviour is discernibly different to more advanced stages of this disease (see Table 74. This is significantly different to the behaviour of the other stages of the disease (see Table 74. As a result, the results of the quantitative analysis of the behaviour of retraction towards the promontory has been freely interchanged with that of retraction towards the attic. Although the Sade grade remains the most widely accepted adopted means of monitoring disease progression, the risk of deterioration from one grade to the next is low and the classification provides a low predictive value for disease progression. These result not just from the atrophy of the tympanic membrane itself, but also from the underlying chronic otitis media, as well as Eustachian tube phenomena. Furthermore, complications of the retraction such as erosion of the ossicles or infection of keratin accumulating within the retraction pocket also contribute to the melange of symptoms. Variable hearing loss due to chronic inflammation with accumulation of a middle ear effusion may occur. Persistent hearing loss may result if the tip of the long process of the incus has been eroded. In general, hearing loss is mild when there is a contact between the retracted tympanic membrane and an intact stapes. Erosion of the stapes superstructure results in a larger and more clinically significant conductive hearing loss. These may be due to episodes of acute otitis media or infection of debris within the pocket. They find that sniffing, which reduces the middle ear pressure and locks the Eustachian tube, eases this sensation. Care is required to differentiate a retraction pocket from a perforated tympanic membrane and the two-dimensional view provided by a hand-held otoscope may not be sufficient. The otological microscope will help determine if the retracted area is perforated, if other tympanic membrane disease is present and whether there is any evidence for acute or chronic middle ear inflammation. If keratin is accumulating within the retraction pocket, some authorities would consider that the pathology is better considered a cholesteatoma. However, a minor accumulation of dry keratin, associated with streaming of the keratin out of the retraction pocket, usually remains asymptomatic and is not always associated with disease progression. It is important to attempt to identify the margins and entire fundus of the retraction pocket. It may disappear behind the posterior annulus, the manubrium or the chorda tympani. The structures under the floor of the retracted tympanic membrane should be carefully inspected. The promontory and round window and ossicles are readily identifiable when the inferior pars tensa is retracted. If there is retraction of the posterior tympanic membrane, the abnormality is readily recognized because the long process of the incus will be clearly visible. The retraction may be in contact with the long process of the incus only or may envelop the incus and stapes like clingfilm. The lenticular process of the incus may be eroded so that the capitulum is partly visible. The long process may be eroded so that it no longer makes contact with the stapes. There may be erosion of the posterior annulus so that the stapedius tendon and pyramid are clearly visible. An early sign of this accumulation is a stream of wax emanating from the pocket around the posterior annulus and along the posterior canal wall. Keratin accumulation may be focal and associated with areas where the fundus of the pocket is no longer visible. There may be granulation tissue associated with the retraction if this accumulating keratin becomes infected. Surgical elevation of the collapsed tympanic membrane from the ossicles carries some risk of cochlear injury. Failure of the tympanic membrane to heal after surgery may result in an iatrogenic perforation. There is also a risk of spawning an iatrogenic cholesteatoma by leaving epithelium capable of generating keratin in the mesotympanum in those cases with adherence of the tympanic membrane to the walls of the middle ear.
Sensitivity pregnancy leg pain discount raloxifene 60 mg on-line, specificity and predictive value of tympanometry in predicting a hearing impairment in otitis media with effusion menstrual odor treatment cheap 60 mg raloxifene. Towards the validation of aural acoustic immittance measures for diagnosis of middle ear effusion in children womens health hudson ny order raloxifene online now. Microtympanometry menopause 8 months no period raloxifene 60 mg order with mastercard, microscopy and tympanometry in evaluating middle ear effusion prior to myringotomy womens health total body transformation purchase raloxifene amex. Identification of middle ear dysfunction in young children: a comparison of tympanometric screening procedures. Tympanometry, stapedius reflex and hearing impairment in children with otitis media with effusion. Sonotubometry: Eustachian tube ventilatory function test; A state-of-the art review. Otitis media with effusion in children with congenital or early-onset hearing impairment. Could the presence of a Carhart notch predict the presence of glue at myringotomy Evidence assessment of the accuracy of methods of diagnosing middle ear fluid in children with otitis media with effusion. Tympanometry in the detection of hearing impairments associated with otitis media with effusion. Screening in the first four years of life to undergo early treatment for otitis media with effusion. Pure-tone hearing thresholds in otologically healthy 5-year-old children in Finland. Hearing deficits in young adults who had a history of otitis media in childhood: Use of personal stereos had no effect on hearing. Does early detection of otitis media with effusion prevent delayed language development Otitis media; hearing loss, and language learning: controversies and current research. Effect of early middle ear effusion on child intelligence at three, five, and seven years of age. Randomised controlled trial of early surgery versus watchful waiting for glue ear: the effect on behavioural problems in pre-school children. Treatment of persistent Eustachian tube dysfunction with aerosolized nasal dexamethasone phosphate versus placebo. Oral or topical nasal steroids for hearing loss associated with otitis media with effusion in children. Use of antibiotics in preventing recurrent acute otitis media and treating otitis media with effusion. Otitis media with effusion and S-carboxymethylcysteine and/or its lysine salt: a critical overview. The role of Mucodyne in reducing the need for surgery in patients with persistent otitis media with effusion. A randomised comparison of homeopathy and standard care for treatment of glue ear in children. A comparison of performance of Shepard and Sheehy collar button ventilation tubes. Is aspiration of middle ear effusions prior to ventilation tube insertion really neccesary Grommets (ventilation tubes) for hearing loss associated with otitis media in children. Early surgery compared with watchful waiting for glue ear and effect on language development in preschool children: a randomised trial. A randomised study of the surgical management of children with persistent otitis media with effusion associated with a hearing impairment. Otoscopic, impedance and audiometric findings in glue ear treated by adenoidectomy and tonsillectomy; a prospective randomised trial. The role of ventilation tube status in the hearing levels in children managed for bilateral persistent otitis media with effusion. Effect of early or delayed insertion of tympanostomy tubes for persistent otitis media on developmental outcomes at the age of three years. Chapter 72 Otitis media with effusion effect of ventilation tubes (grommets) on quality of life at age 12 years. Per-operative antibiotic/steroid prophylaxis of tympanostomy tube otorrhoea; Chemical or mechanical effect Randomized trial of the efficacy of trimethoprim-sulfamethoxazole and prednisolone in preventing post-tympanostomy tube morbidity. A costbenefit analysis of the post-operative use of antibiotic ear drops following grommet insertion. Tympanic membrane abnormalities and hearing levels at the ages of 5 and 6 years in relation to persistent otitis media and tympanostomy tube insertion in the first 3 years of life: A prospective study incorporating a randomised controlled trial. Spontaneous resolution of severe chronic glue ear in children and the effect of adenoidectomy, tonsillectomy and insertion of ventilation tubes (grommets). The role of adjuvant adenoidectomy and tonsillectomy in the outcome of the insertion of tympanostomy tubes. Adenoidectomy and adenotonsillectomy for recurrent acute otitis media: parallel randomised clinical trials in children not previously treated with tympanostomy tubes. Efficacy of tympanostomy tube insertion for otitis media with effusion in children with Down syndrome. Reference lists were reviewed for further articles, and authors of recent presentations contacted personally for their reference lists. It is hard to diagnose accurately and on existing evidence, as opposed to custom and tradition, there is still a high level of uncertainty over how it should best be treated. Even a metanalysis, the supposed gold standard of evidence, is only as good as the studies it covers. It normally develops behind an intact tympanic membrane, but may include acute infections arising in the presence of ventilation tubes or existing tympanic membrane perforations. The requirement to confirm a middle ear effusion, and the nature of the symptoms and signs, vary between authors. Sporadic episodes occurring as infrequent isolated events, typically occurring with upper respiratory tract infections. Groups two and three appear similar at first glance and this distinction may be questioned. Grading of the severity of an episode has been attempted and has merit both clinically and for research. The otalgia will settle within 24 hours in two-thirds of children without treatment. Symptomatic relief is obtained without treatment in 88 percent by day four to seven. The hearing loss, caused by the middle-ear effusion, occurs early in the illness and may persist at greater than 20 dB for one month in over 30 percent, and two months in 20 percent of children. The diagnosis is often confirmed, rightly or wrongly, by an attempt at otoscopic assessment of the tympanic membrane. Since trained observers have been shown to have only an 85 percent accuracy in otoscopic diagnosis,10 it would not be surprising for a sensible primary care physician to rely more on history and the general aspect of a child than on otoscopic findings. There may well not be a clear history of a crescendo of otalgia in a coryzal child, followed by rapid symptomatic relief associated with tympanic membrane perforation and associated blood-stained otorrhoea. A large multinational study rated clinicians diagnostic certainty in children under one year of age at only 58 percent, rising to 73 percent in those over 31 months. Diagnostic confusion may occur with acute mastoiditis, otitis media with effusion, otitis externa, trauma, Ramsey Hunt syndrome and bullous myringitis. Hypomobility of the drum demonstrated by pneumatic otoscopy has been shown to aid diagnosis10 and is felt essential in some countries,1 although others including the Dutch2 take a more pragmatic view and do not include this in their diagnostic criteria. Should the drum have perforated, or a ventilation tube be in situ, mucopurulent otorrhoea will be seen. Investigations Tympanometry may be used to establish the presence of a middle ear effusion, but is not usually available. Tympanocentesis and culture of middle ear effusion have been used in a number of studies assessing diagnostic accuracy of clinical signs, and establishing the organisms prevalent in a community. Taking a bacterial swab of persistent otorrhoea following perforation is recommended. Nasopharyngeal swabbing for bacterial culture has been assessed but the correlation with middle ear organisms has been too weak to recommend it clinically. Immunoglobulin assay may be appropriate: Ig A, G (with subclasses) and M are typically assessed. This heterogeneity is important when considering vaccination against viruses as a prophylactic measure. These alternative routes of entry are suggested by the wide variation in rates of isolation of specific viral strains in the middle ear during systemic infection, ranging from 4 to 74 percent of cases dependent upon the specific virus. This implies some viruses may be actively invading the middle ear cleft, and may be contributing directly to mucosal inflammation. There is good clinical and animal evidence that viral infection affects Eustachian tube function. Ciliated epithelial cells numbers decline, mucus production increases in the Eustachian tube and negative middle ear pressure results. Alteration of host immunity has been documented after viral infections, increasing susceptibility to bacterial infections. The ability of bacteria to colonize and adhere to the nasopharyngeal epithelium appears to be increased by certain viral infections. This is important as clinical studies show that children who have both viruses and bacteria in their middle ear are very much more likely to have a poor response to antibiotics when compared to those with bacteria only (33 versus 3 percent failure respectively, in one study14). Why this should be is unclear, but may be related to the greater concentrations of inflammatory mediators in ears in which both bacteria and viruses are present. Incidence (%) 1637a 1123 Up to 13 Up to 5 Haemophilus influenzae Moraxella catarrhalis Streptococcus pyogenes Staphylococcus aureus a There are some 90 serotypes. The Eustachian tube is traditionally assumed to be the main route by which organisms reach the middle ear, though there are relatively few studies to confirm this. It is speculated that negative middle ear pressure may facilitate the movement of bacteria up the Eustachian tube. Studies of Native Americans, who are prone to otitis media, suggest their Eustachian tubes are shorter, straighter and more patulous than in whites, but also that they have a low passive tubal resistance. Specifically, otitis-prone children have been shown to have significantly poorer active tubal function (muscular opening function). Pathogen entry through tympanic membrane perforations or ventilation tubes is most commonly associated with water exposure. It was shown that the wide variation in rates of identification of specific viral strains from the middle ear could not be explained by passive Eustachian tube transport alone. Limited evidence is beginning to emerge that over-expression may alter the mucociliary transport system. However, environmental factors, such as poor economic status, may contribute to the increased risks in these groups. Maternal blood group A is reported to an independent risk factor (relative risk 2. However, a number of specific associations have been identified which suggest that certain defective or immature pathways may predispose to infection. Low levels of IgG2 subclasses have been reported in several studies to be more common in otitisprone children. Those with IgG2 deficiency were shown to be three times more likely to develop post-ventilation tube insertion otorrhoea for example. This may be particularly important in infancy when the antibody repertoire is limited. The most important is almost invariably stated to be day-care attendance outside the home. Certainly Eustachian tube dysfunction in these groups predisposes to middle ear effusion, but it is not clear whether it is this dysfunction or an increase in risk secondary to subtle immunological factors that predisposed to infection. No increase is found in children with primary ciliary dyskinesia if grommets are not inserted, or cystic fibrosis. Its incidence appears highest in the first year of life, more specifically the second six months of life in most studies, and gradually reduces with increasing age. Epidemiological studies have been compromised by difficulty in achieving accuracy in diagnosis when large numbers of children are being assessed, hence there are wide variations in reported numbers. Incidences of over 60 percent are stated in some reports of infants up to age one year. Possible reasons include increased day nursery attendance and changes in diagnostic awareness. Others have reported that by age three, half of children will have had at least three episodes. Current debate questions whether and for whom treatment is required, and the role of prophylactic strategies. There is limited experimental animal evidence showing that ibuprofen provides additional benefit by reducing mucosal inflammation when taken in combination with amoxicillin. A recent metanalysis9 has addressed the question of whether antibiotics should be given at initial consultation. Two-thirds of children recovered within 24 hours of the start of treatment, and 80 percent by days two to seven, with or without antibiotics. Antibiotics did lead to 5 percent fewer children overall having pain between days two and seven. That equates to 17 children needing to be treated to prevent one child experiencing pain during days two to seven. Relatively few data were available on hearing loss at one and two months post-infection, but no differences were found between those who received antibiotics and those who did not. However, those taking antibiotics suffer nearly double the side effects, such as diarrhoea, than those who do not, and run a greater risk of developing antibiotic resistant bacteria. At 819 days the weighted mean failure rate in the short course was 19 percent and 13. It implied that 17 children would need to receive the long course to avoid one treatment failure.

Surgical the surgical treatment of patients with complications of rhinosinusitis can be conveniently divided into that necessary for the treatment of the rhinosinusitis and that necessary for the treatment of the complication women's health clinic buffalo ny order raloxifene with mastercard. These are likely to be carried out at the same time women's health issues contraception discount 60 mg raloxifene free shipping, but may involve more than one team of surgeons pregnancy early signs raloxifene 60 mg mastercard. The principles of draining any pus and establishing ventilation of the sinuses remain exactly the same and are described elsewhere breast cancer 7 cm cheap raloxifene 60 mg without prescription. Where the complication has arisen from acute rhinosinusitis women's health big book of exercises app order raloxifene online from canada, it is likely that the operative field will be very haemorrhagic, making endoscopic surgery much more difficult than in the presence of chronic rhinosinusitis alone. Contraindications for an endoscopic approach include any intracranial complication, osteomyelitis of the frontal bone or orbital complications with an acute visual problem. Some surgeons suggest that endoscopic ethmoidectomy together with removal of the lamina papyracea and perinasal drainage of the orbital abscess is sufficient treatment. However, unless the surgeon is extremely familiar with endoscopic nasal surgery, it is probably easier and wiser to use an external approach. This has the advantage of allowing an assistant to help keep the operative field clear. If an external approach is used, the conventional LynchHowarth Chapter 120 Complications of rhinosinusitis] 1545 or externally through the medial canthal incision. The former, endonasal, siting is likely to result in less cosmetic deformity than leaving an external drain. As far as the otorhinolaryngologist is concerned, discussion needs to take place as to whether the neurosurgical approach is going to be done at the same time as any sinus surgery. There is little evidence to help decide whether these should be done as separate procedures, but as with orbital cellulitis, it is probably better to undertake the surgery for the complication at the same time as undertaking surgical treatment for the underlying rhinosinusitis. However, intracranial complications are most likely to arise from frontal rhinosinusitis rather than disease of the other paranasal sinuses, and definitive surgery on the frontal sinus is difficult at the best of times. In these circumstances, it is probably better to undertake a temporary drainage procedure at the time of surgery for the intracranial complication, rather than attempt a formal sinus reventilation procedure or obliteration. A frontal sinus trephine procedure with placement of an external drain is likely to give the best immediate result, leaving the decision about any definitive surgical procedure until the patient has fully recovered from treatment of the complication. Other concurrent complications of rhinosinusitis should be excluded prior to theatre. Following surgery, a prolonged course (six weeks) of culture-directed antibiotic therapy should be given. Occasionally the orbital abscess will lie away from the lamina papyracea, especially if there is a frontal rhinosinusitis. The major complications of rhinosinusitis are orbital and intracranial infection, of which orbital complications are the more common. A more recent study of 219 patients showed an overall mortality rate of 16 percent. Chapter 120 Complications of rhinosinusitis] 1547 [Surgical treatment is normally required for resolution in patients with abscess formation. Ã Deficiencies in current knowledge and areas for future research $ $ $ the numbers of patients presenting with complications of rhinosinusitis is very small, and the symptomatology often very varied. This makes it very difficult to design studies in any particular area that would result in level 1 or 2 evidence. The evidence presented here is, therefore, mostly based on the results of retrospective case series reviews. A number of the widely quoted series cover periods that must now be considered the medical past, particularly with regard to the development and widespread availability of imaging techniques and therefore diagnosis. However, much of the data they provide with regard to populations at risk, organisms isolated and prognosis for outcome are still generally comparable with modern series. A large centre, perhaps in a country where the condition is seen more frequently, would be the optimal setting to investigate this. However, extrapolation of results to other centres with varying experience of endoscopic surgery would, as ever, be difficult. There is also little information to suggest why some individuals should develop complicated sinus disease when similar organisms are isolated from patients with uncomplicated disease. Further investigation of factors, including host and bacterial genetics, may suggest potential reasons. In addition, the use of techniques such as polymerase chain reaction for the detection of bacterial sequences may be helpful in gaining more information on otherwise culturenegative specimens. Preseptal (periorbital) cellulitis, subperiosteal abscess and orbital cellulitis due to rhinosinusitis. Infectious intracranial complications of rhinosinusitis, other than meningitis, in children: 12-year review. The role of computed tomography and magnetic resonance imaging in patients with rhinosinusitis with complications. Intracranial complications of paranasal rhinosinusitis: A combined institutional review. Simultaneous intracranial and orbital complications of acute rhinosinusitis in children. The patient will experience nasal polyps to be an unpleasant disease, which severely interferes with the quality of life. Finally, a disease characterized by the occurrence of multiple polyps is most correctly named nasal polyposis and, strictly speaking, it is not a nasal but a sinonasal disease. The surface is smooth and the colour is more yellow than the pink mucous membrane. Nasal polyps originate in the upper part of the nose around the openings to the ethmoidal sinuses. The polyps protrude into the nasal cavity from the middle and superior meatus, resulting in nasal blockage and abolishing airflow to the olfactory region. Nasal polyposis, consisting of multiple, bilateral polyps, is part of an inflammatory reaction involving the mucous membrane of the nose, the paranasal sinuses and often the lower airways. Polyps are easily accessible for histological and immunological studies and an increasing number of publications have appeared in recent years. Nasal polyposis occurs with a high frequency in groups of patients having specific airway diseases (Table 121. It is noteworthy that nasal polyps are very rare in allergic children in contrast to children with cystic fibrosis and that the disease is more frequent in nonallergic than in allergic adult patients with rhinitis and asthma. Although the disease, nasal polyposis, is rare, isolated nasal polyps occur in one third of examined nasoethmoidal blocks from cadavers. In a follow up of patients in an otology practice, the median time from the first to the second polypectomy was six years, indicating that many cases of nasal polyposis are mild. In this disease, the tissue inflammation is typically eosinophil-dominated,9 as in the aspirin triad. As most polyps are characterized by tissue eosinophilia, it has been the belief for decades that allergy is a significant cause of nasal polyposis. However, this view has been challenged because most studies have failed to show a higher occurrence of positive skin tests to inhaled allergens in patients with polyps than in the general population. In striking contrast to nasal polyposis, which is a disease of middle-aged people, allergic rhinitis occurs with its highest prevalence in children and young adults. Children with perennial allergic rhinitis, who can have markedly swollen nasal mucous membranes, almost never develop polyps (Table 121. Even the pathogenic contribution of allergic reactions in patients with coincidental occurrence of the two conditions can be questioned. Keith and coworkers13 were unable to show any deterioration of nasal symptoms or eosinophilia during the pollen season in polyp patients having a positive skin test to pollen. Thus, it appears that allergy is not a well-documented cause or aggravating factor in nasal polyposis. It consists of recurrent respiratory disease with chronic rhinosinusitis, nasal polyps, bronchiectasis and azoospermia. This is misleading and may result in futile attempts at identifying a causative allergen in air, food or beverages. It was recently shown that, in a number of cases, it is caused by IgG autoantibodies to the receptor for IgE on mast cells. Although tempting to hypothesize, a similar process has not been identified in nasal polyposis. There is experimental evidence that cytotoxic proteins from eosinophils can damage the respiratory epithelium and induce bronchial hyperreactivity in asthma. This area, so critical for sinus pathology, is also referred to as the ostiomeatal complex. It is remarkable that polyps exclusively develop from a few square centimetres of an airway mucous membrane which often is universally inflamed. Another possibility is an influence of special airflow, air current and pressure in the upper part of the nose. Finally, it may be of significance that the nerve endings near the borderline between the nose and paranasal sinuses are thin23 and may easily become damaged by cytotoxic proteins, released by eosinophils. As mentioned, nasal polyps develop in areas where the lining of the nasal cavity joins that of the sinuses, and these marginal zones contain thin nerve fascicles,23 which may have increased sensitivity to damaging factors. While the exact cause and mechanism of the denervation of the nasal polyps is unknown, there is little doubt that the complete loss of autonomic innervation is an important pathogenetic factor in the formation of polyps. While nasal mucosa glands are small branched tubuloalveolar glands, those in the polyps are long, tubular and of varying shape, size and type. The nasal glands are evenly distributed over the mucous membrane, while the glands in the polyps are very unevenly distributed. Many cell junctions have the appearance of a web of villous processes and are incompletely sealed, while others are wide open,23 promoting oedema formation. Inflammation Nasal polyposis is the ultimate form of inflammation of the upper airways, which, for unknown reasons, preferentially develops in subtypes of inflammatory diseases. Although IgE-mediated allergy is not an important aetiological factor, recent data indicate that both mast cells and histamine are involved in the inflammation and in the pathogenesis of polyps. Eosinophil infiltration and activation is caused by cytokines, chemokines and adhesion molecules. Involvement of the paranasal sinuses, the mucosa of which has many goblet cells but few seromucous glands, contributes to the viscosity of the discharge. The disease can vary in severity from a single episode of nasal blockage, relieved by a short course of treatment, to a life-long disease, requiring continuous and combined treatment. They should be told that these factors are not the cause of the disease, although they can provoke symptoms from an irritable mucous membrane. There is hyperplasia of the maxillary mucous membrane and the ethmoidal cells are filled with polypoid mucous membrane. This pathology may not necessarily result in symptoms, but it can cause a feeling of congestion and may also increase the tendency to bacterial infection, especially following a common cold. It is indicated when there is a suspicion of malignancy or meningocoele, and also in all cases before endoscopic surgery. These three disease manifestations usually start within months or a few years in 40- to 50-year-old patients. Asthma patients have polyps which are sensitive to corticosteroid treatment, but they usually require continuous intranasal therapy and surgery as well. As a rule, the asthma is chronic, severe and persistent, requiring continuous inhaled corticosteroid treatment. Questioning about adverse reactions to acetylsalicylic acid is obligatory in patients with nasal polyps. It starts with a low dosage (10 mg) and it must be performed by a specialist in a hospital setting. Other examinations Any child with nasal polyps needs an evaluation for cystic fibrosis. In general, allergy testing is not indicated but it is often expected by the patient. Nasal bleeding, pain and unilateral polyps should alert the physician to other conditions, such as malignant tumours, inverted papillomata and, in a child, meningocoeles, all of which may masquerade as simple polyps. For that reason, microscopy is always necessary when polyps are removed for the first time, and when polyps are unilateral. Endoscopic appearance No polyps Restricted to middle meatus Below middle turbinate Massive polyposis Reprinted from Ref. In contrast to a hyperplastic turbinate, a polyp can be made to move by touching with a probe. Endoscopy with a rigid scope is the preferred examination, as it can diagnose small polyps in the middle meatus and give a superior assessment of the extent of the disease and of anatomical abnormalities. The examination is performed after simple spraying of the nose with a local anaesthetic and a vasoconstrictor. Endoscopy is useful, not only for the diagnosis, but also for follow-up examination after Table 121. Right Maxillary Anterior ethmoid Posteriod ethmoid Sphenoid Frontal Ostiomeatal complex Total 02 02 02 02 02 0/2 012 Left 02 02 02 02 02 0/2 012 0, no opacity; 1, some opacity; 2, total opacity. The aetiology is unknown and treatment consists of surgical removal, which cures the disease. Possibly, leukotriene antagonists may have an additional effect in selected patients. Score 2 Intranasal corticosteroids Intranasal corticosteroids are by far the best documented type of treatment for nasal polyposis. This may be due to inadequate intranasal distribution of the spray in a very blocked nose. Pressure from polyps may have changed the normal slitlike cavity to a wide tube in the lower part of the nose, at the same time as there may be considerable pathology and blockage in the upper part of the nose. Clinical experience indicates that the effect of topical steroids, in contrast to systemic administration, is poor. The total glucocorticoid dose in a depot-injection corresponds to about 100 mg prednisolone. Clinical experience confirms that the beneficial effect, in many cases, will outlast the medication for a variable period. In severe disease, requiring endoscopic surgery, preoperative use of a systemic steroid will considerably facilitate surgery.
Increasing prevalence of hay fever and atopy among children in Leipzig pregnancy journal generic raloxifene 60 mg amex, East Germany menstrual yearly calendar raloxifene 60 mg amex. The first large epidemiologic survey showing an association between rhinitis and asthma women's health nurse practitioner salary by state order raloxifene 60 mg with amex. Moreover womens health 60 years raloxifene 60 mg otc, this study is the first to show that nonallergic rhinitis is strongly associated with asthma women's health clinic nambour purchase raloxifene with a visa. Seasonal increase of carbachol airway responsiveness in patients allergic to grass pollen. Long-term risk factors for developing asthma and allergic rhinitis: a 23year follow-up study of college students. Onset and remission of allergic rhinitis and asthma and the relationship with atopic sensitization and smoking. Journal Deficiencies in current knowledge and areas for future research $ $ $ $ $ $ $ $ $ More prospective studies should assess the relationship between rhinitis and asthma and confirm that rhinitis is a risk factor for asthma. In occupational diseases, the recognition of rhinitis may detect patients early during the course of the disease in order to prevent the onset and progression of persistent asthma in subjects exposed to known risk factors. More studies are needed to appreciate the relationships between the upper and lower airways and the systemic nature of allergic diseases. Large pivotal clinical trials should be started to assess whether the treatment of one target organ may improve outcome measures of the other target organ. Large pivotal trials should be started to show that oral or systemic treatments improve outcome measures of the entire airway. Prospective studies should confirm the protective role of nasal treatment on asthma exacerbations and emergency department visits. This paper reports a World Health Organization workshop highlighting the relationships between asthma and rhinitis. Ã Chapter 122 the relationship between the upper and lower respiratory tract of Allergy and Clinical Immunology. Association between rhinitis and asthma are well known and many studies have been published within the past five years. Comparison between nasal and bronchial inflammation in asthmatic and control subjects. The first study in which nasal and bronchial mucosal biopsies have been carried out in the same patients. Eosinophils are a feature of upper and lower airway pathology in non-atopic asthma, irrespective of the presence of rhinitis. Relationship of computed tomographic findings to allergy, asthma, and eosinophilia [published erratum appears in Journal of the American Medical Association 1994 Sep 21;272(11):852]. Association between sinusitis and asthma are well known and many studies have been published. However, this study shows that the more severe asthma, the more extensive sinusitis. Bronchial mucosal manifestations of atopy: a comparison of markers of inflammation between atopic asthmatics, atopic nonasthmatics and healthy controls. Cytokine expression in the lower airways of nonasthmatic subjects with allergic rhinitis: Influence of natural allergen exposure. Pulmonary inflammation after segmental ragweed challenge in allergic asthmatic and nonasthmatic subjects. The authors have demonstrated for the first time that allergen trigger of one site of the airways induces inflammation in the other site of the airways. Nasal allergen provocation induces adhesion molecule expression and tissue eosinophilia in upper and lower airways. Allergen-induced increase in airway responsiveness, airway eosinophilia, and bone-marrow eosinophil progenitors in mice. Contribution of basophil/mast cell and eosinophil growth and differentiation to the allergic tissue inflammatory response. Treatment of allergic rhinitis with intranasal corticosteroids in patients with mild asthma: effect on lower airway responsiveness. Nasal inhalation of the glucocorticoid budesonide from a spacer for the treatment of patients with pollen rhinitis and asthma. Efficacy and safety of loratadine plus pseudoephedrine in patients with seasonal allergic rhinitis and mild asthma. Patients receiving intranasal corticosteroids have fewer emergency department visits for asthma. Allergic rhinitis in Rochester, Minnesota residents with asthma: frequency and impact on health care charges. This is achieved by complicated aerodynamics that depend on the geometry of the internal nose. The septum also supports the dorsum, columella and the tip of the nose and as such it contributes to cosmesis. The success of functional nasal surgery, as well as cosmetic nasal surgery, depends heavily on the correction of the septum. This explains why nasal surgery almost always involves both function and aesthetics as pointed out by Maurice Cottle in the 1960s. Usually this is of no consequence because due to its flexibility it can withstand limited mechanical impact. Nevertheless, from life in utero onwards there are many risks of nasal trauma in which the septum is involved. Furthermore, the septum plays a key role in the development and growth of the nose, the midface and maxilla. These lesions not only disturb the growth of the cartilage involved, but also the growth of the bones related to this cartilage. The effects of trauma in early childhood are often first noticed during the growth spurt in puberty. The cephalic part of the septum ossifies from the perpendicular plate of the ethmoidal bone. The vomer develops in the tissues covering the posteroinferior part of the septal cartilage as two bony plates with the cartilage between. The perpendicular plate forms the cephalic part of the skeleton of the septum, the vomer the posterocaudal part and the quadrilateral cartilage the anterior part. The septum sits anteriorly via the quadrilateral cartilage on the anterior nasal spine and the premaxilla. Again, more posteriorly the vomer slides between the maxillary crest and the quadrilateral cartilage. Particles over 5 mm are captured in the mucus and transported to the nasopharynx by ciliary movements. Thus, it is obvious that good function of the nose depends on healthy mucous membranes that will need a great deal of moisture and energy in the form of heat. Choanal atresia is a relatively rare condition, which is seen in one in 10,000 births. It should be noted that complete neonatal nasal obstruction can result in intermittent hypoxia, apnoea and failure to thrive and therefore constitutes a life-threatening emergency. Furthermore, the septum may be involved in rare congenital conditions, such as congenital midline nasal masses, teratomas or frontonasal dysplasia and bifid noses. The valve has the smallest cross-sectional surface of the upper respiratory tract. The maxillary and palatine processes form the palate and fuse in the midline with the septum. Consequently, in surgery a cleft can be found to the right or to the left of the septum. When there is insufficient growth of the palatine and maxillary processes from both sides, the inferior part of the septum will be free. When the maxillary process does not reach the frontonasal process, this will result in a cleft lip which can be unilateral or bilateral. Nevertheless, all nasal trauma deserve careful physical examination even when there are no serious signs, such as nose bleeding, in which case one should be aware of the possibility of a septal haematoma. If an incision in the mucosa is made to drain a haematoma, it should be a horizontal incision to avoid disruption of the mucociliary transport. Septal haematoma Septal abscess Internal nasal bleeding that cannot escape through the mucous membranes or skin will result in a haematoma. It is a serious condition that is the most common cause of a septal abscess is a septal haematoma. Three to five days after the trauma that caused the haematoma, a fever and nasal blockage may Chapter 123 the septum] 1573 occur which, at that time, will not be associated with the trauma and frequently is interpreted as flu. In fact, the septal haematoma has developed into a septal abscess and it is at this point that the patient seeks help, by which time there is already severe damage to the septal skeleton. Since this condition usually occurs in children, severe growth impairment is unavoidable, although good medical and surgical care can diminish the consequences to some extent. Septal fractures the type of fracture in nasal trauma depends on the side and magnitude of the impact. Frontal trauma will frequently result in vertical fractures, whereas lateral trauma can give horizontal fractures. The tension that is normally present in the septal cartilage can make a dislocation worse and difficult to reposition. In vertical fractures in particular, the consequent scar can impede mucociliary transport. Incomplete fractures can lead to bending of the cartilage because the balance of the stresses in the cartilaginous fibres is lost, or because of scar retraction in fibrous tissue filling up the incomplete fracture. In the former case, there is a bending away from the incomplete fracture, while in the latter the convexity is on the same side of the incomplete fracture. Although perichondrium is able to form cartilage, in general the conditions under which this can occur do not exist in fractured cartilage. In vertical fractures, there may be a luxation or subluxation of the caudal part of the quadrilateral cartilage. In case of a luxation, the caudal rim of the cartilage can be seen to the left or to the right of the columella. When there is no skeleton to prevent drying of the back of the mucosa opposite to the mucosal laceration, the mucosa on both sides of the septum will disappear and this leads to a perforation. This explains why perforations are seen in deep trauma of the septum, which not only involve the mucosa but also the underlying skeleton. In submucosal skeleton resections, such as the Killian procedure, a septum perforation is a common complication, because in the case of a mucosal defect the inner surface of the opposite mucosa is not protected against dehydration by the skeleton. In the septum, mucosa and perichondrium or periosteum are closely related to each other. Although septal perforations can be asymptomatic, they may present to the surgeon with debilitating symptoms such as nasal blockage, atrophy of the mucosa, dryness, crusting, nose bleeding, whistling and headache. The other symptoms are the result of the poor condition of the mucosa, which is worse around the perforation. Perforations in the anterior part of the septum present more symptoms than perforations in the posterior part. Closure of a septal perforation is difficult due to lack of material to reconstruct the skeleton and the mucosa and because of the poor condition of the tissues around the perforation. There are many techniques to close a septal perforation, which indicates that none of them presents the ultimate solution. Vital tissues are brought into the perforation to reconstruct the skeleton and the lining of the septum and to replace the atrophic tissues around the perforation. Anatomical limitations mean that these transplants only marginally meet the requirements of the vascularization for these types of reconstruction. The necessary mucosa can be found locally, on the turbinates or at the inside of the upper lip. It is difficult to get good access to the surgical field, especially to lay the necessary sutures in the often very delicate edges of the perforation. When closure of a perforation is difficult, conservative treatment might be an alternative. A silastic button may have a positive effect by improving the aerodynamics and protecting the edges of the perforation, although the button itself can be the cause of crusting. Vascular and bleeding disorders the function of the nose requires an extensive blood supply. The abundance of blood vessels and their relatively superficial position in the nasal septum result in epistaxis following mucosal trauma, inflammation, tumours, vascular diseases or bleeding dyscrasias. It is conceivable that septal surgery influences nose bleeding by altering the vascularization. However, there is insufficient evidence for a causal relationship between nasal bleeding and septal deviations. Nevertheless, there might be an indication for a septoplasty to make the site of the bleeding more accessible for local treatment. Branches of the anterior ethmoidal artery are divided over the anterior part of the septum. The posterior ethmoidal artery provides blood to the superior posterior part of the septum. The sphenopalatine branch of the maxillary artery enters the nose through the sphenopalatine foramen and supplies the posterior inferior part of the septum. In the region of the anterior nasal spine, it forms anastomoses with terminal branches off the greater palatine artery and the labial branch of the facial artery. Above the incisive foramen along the inferior mucocutaneous junction, capillary vessels run to the surface.
60 mg raloxifene order overnight delivery. Dr. Emily Turney - West Georgia Healthcare for Women.
References
- Schug, S. et al. (1991). Treatment principles for the use of opioids in pain of non-malignant origins. Drugs, 42, 228n239.
- Pearcy, M. J. (1990). Inferred strains in the intervertebral discs during physiological movements. Journal of Man and Medicine, 5, 68n71.
- Myobloc(R) Prescribing Information. Solstice Neurosciences, Inc. South San Francisco, CA, 2004.
- Carlo RD, et al. Steroid, prolactin, and dopamine receptors in normal and pathologic breast tissue. Ann N Y Acad Sci. 1986;464:559-562.
