
Zofran
| Contato
Página Inicial
Alex Ho, MD
- Bixler Emergency Center
- Tallahassee Memorial Hospital
- Formerly, Resident,
- Department of Emergency Medicine
- University of North Carolina
- Chapel Hill, North Carolina
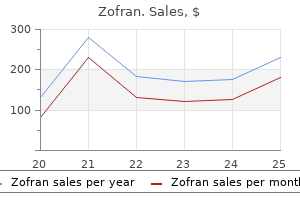
Anti-E antibodies potentiate the effect of the anti-c medicine 369 cheap zofran 4 mg on-line, so a lower threshold for beginning ultrasound surveillance should be adopted treatment of tuberculosis zofran 8 mg purchase line. All other red cell antibodies are still quantified using the dilutional method medications similar to cymbalta buy cheap zofran 4 mg, and the level of these will be given as a titer symptoms 1 week before period zofran 4 mg purchase mastercard. Anti-Kell1 antibodies are the second most common cause of fetal immune-mediated hemolysis treatment 7 order generic zofran canada, and early onset anemia and hydrops have been well documented. Nine out of 10 of the general population are Kell1 negative and only 1 in 20 babies of Kell1 negative women are Kell1 positive. The Kell antigen is expressed on red cell progenitors in the bone marrow and it is via these cells that anti-Kell1 antibodies are able to suppress hematopoiesis, as well as causing hemolysis. In approximately half of all cases of Kell isoimmunization the cause is a previous blood transfusion where cross-matching did not take account of Kell status of the woman, or donor. Absolute levels of anti-Kell antibodies are less useful in the prediction of disease severity. Fetal surveillance using middle cerebral artery Doppler studies should be offered irrespective of the anti-Kell level if the fetus is Kell positive. Women who have the blood group O quite commonly have antibodies to the A- and B-antigens, although these are more likely to be of the IgM class which does not cross the placenta. Anti-A and anti-B IgGs can reach the fetal circulation, but only mild hemolysis is the general rule for two reasons. Firstly, these antigens are expressed on a wide variety of cell types, effectively diluting their effect on red blood cells. Secondly, cell-surface expression is incomplete during gestation and develops gradually, thus limiting the risk before birth. The Future the successes of recent years have not prevented further research and progress in the prevention and management of RhD hemolytic disease. Although polyclonal anti-D is a safe product, it is pooled from various donors and anxieties about viral and prion disease transfection remain. The anti-D for these women is unnecessary, unpleasant, expensive, and not without a degree of risk. Limiting the administration of anti-D to only those RhD negative women carrying a RhD positive fetus is a worthy goal. The techniques used for non-invasive prenatal fetus RhD testing (see above) are time consuming and expensive, although very accurate. Mass screening requires an automated test, and robotic systems have been developed and tested recently with very promising results. These false positives represent a group of RhD negative women who would continue to receive anti-D unnecessarily, but this is a tiny number compared with the 40% of RhD negative women currently receiving unnecessary anti-D prophylaxis. Although these women would be at a threefold greater risk of isoimmunization because they would not receive antenatal prophylactic anti-D (they would still. There are strong ethical arguments, if not financial ones, in support of this[22,23]. An alternative approach to improve on the safety of anti-D prophylaxis is to use recombinant monoclonal antibodies (mAb) produced from hybridoma or human B-cell lines, instead of polyclonal antibodies collected from human serum. A number of these cell lines exist and progress to date has recently been summarized by Kumpel[24]. Results with some of the mAb are encouraging and D-immunization can be prevented in RhD negative volunteers transfused with RhD positive cells. A "clean" and effective recombinant anti-D mAb may be on the horizon, but hurdles still exist, not least obtaining ethical approval for large-scale trials. Mutated recombinant anti-D monoclonal antibodies have been designed and produced that are able to bind to the RhD antigen but have a much lower affinity for the Fc receptor on macrophages than normal anti-D [26]. These mutated antibodies would displace endogenous anti-D from its binding sites on the RhD antigen. The lifespan of these antibodies is limited and very high and frequent maternal administrations might be needed for transplacental transfer to maintain sufficient levels in the fetus. A welcome move in neonatal care would be the avoidance altogether of exchange transfusion. This structural analog of heme competitively blocks heme-oxygenase, a ratelimiting enzyme in bilirubin production. It does not pass through the bloodbrain barrier and does not accumulate in tissues. Several randomized trials have confirmed that these substances can prevent and block jaundice progression in the newborn. Two years later, in her second pregnancy, her routine screening bloods identified anti-K antibodies. Her third pregnancy, with a new partner, occurred 8 years later, during which her anti-K titer was found to be 1 in 4 at booking, and 1 in 8 at 28 weeks. Review by a fetal medicine specialist found the middle cerebral artery peak systolic velocity to be elevated at 76 cm s-1. Fetal blood sampling the following day gave a fetal Hb of 29g/L and found the baby to be K positive. An intrauterine transfusion was performed into a fetal intrahepatic vein, with a post-transfusion value of 115g/L. The newborn Hb was 131 g/L and a mild rise in the bilirubin level settled with only 24 hours of phototherapy. This case emphasizes the importance of ascertaining paternal and fetal red cell antigen status when there are maternal antibodies, instituting appropriate surveillance for fetal anemia, and the poor relationship between anti-K titer and fetal hemoglobin. Case Study 2 A 34-year-old woman in her first pregnancy was found to have developed low level RhD antibodies by the time of the delivery of her RhD positive baby, despite giving no history of potentially isoimmunizing events. The newborn had a positive direct Coombs test but required only 1 day of phototherapy. In her second pregnancy, the anti-D levels rose sharply during the second and early third trimester. Labor was induced at 34 weeks and the neonate did well following a single exchange transfusion and prolonged phototherapy. Fetal blood sampling and attempted intrauterine transfusion were complicated by fetal bradycardia and intrauterine fetal death at 23 weeks. Guidance on the Use of Routine Antenatal Anti-D Prophylaxis for RhD-negative Women. Techniques of intrauterine fetal transfusion for women with red cell isoimmunization for improving health outcomes (Review). Guidelines for pre-transfusion compatibility procedures in blood transfusion laboratories. Non-invasive diagnosis by Doppler ultrasonography of fetal anemia due to maternal red-cell alloimmunization. Conventional management of maternal red cell alloimmunization compared with management by Doppler assessment of middle cerebral artery peak systolic velocity. Combined plasmapheresis and intravenous immune globulin for the treatment of severe maternal red cell alloimmunization. Targeted routine antenatal anti-D prophylaxis in the prevention of RhD immunization: outcome of a new antenatal screening and prevention program. Efficacy of RhD monoclonal antibodies in clinical trails as replacement therapy for prophylactic anti-D immunoglobulin: more questions than answers. Noninvasive approaches to the management of RhD hemolytic disease of the fetus and newborn. In vitro assessment of recombinant, mutant anti-D immunoglobulin G devoid of hemolytic activity for treatment of on-going hemolytic disease of the fetus and newborn. The cause for this is unclear: some consider that the increased prevalence of obesity and the rising average age of mothers may be factors that have not been counterset by an increased use of thromboprophylaxis. The changes in both blood flow velocity and coagulation factors may persist for up to 6 weeks after delivery. This may reflect compression of the left iliac vein by the right iliac artery and the ovarian artery, which cross the vein only on the left side. This is an important consideration as fewer than 2% of all scans performed are positive and therefore the majority of women with suspected pulmonary emboli will be exposed to potentially unnecessary radiation. Currently it is considered that if there is a delay in obtaining objective tests, the woman should be commenced on anticoagulant therapy, unless contraindicated, until testing can be performed[7]. For the diagnosis of iliac vein thrombosis, which may present with back pain and/or swelling of the entire limb, pulsed Doppler, magnetic resonance direct thrombus imaging or venography or conventional contrast venography should be considered[7]. This may identify other pulmonary disease such as pneumonia, pneumothorax, or lobar collapse. During pregnancy, the ventilation component of the V/Q scan can often be omitted, thereby minimizing the radiation dose for the fetus. At the time, this technique had potential advantages over radionuclide (V/Q) imaging including better sensitivity and specificity (in non-pregnant patients) and a lower radiation dose to the fetus. This is particularly relevant when it is known that only around 5% at most of such investigations will have a positive result. Further, bismuth breast shields can substantially reduce the radiation exposure[20]. Furthermore, Ddimer levels are increased if there is a concomitant problem such as pre-eclampsia, preterm labor, and placental abruption. Thus, the probability of a negative result is lower and objective testing is more often required. In contrast, the European Society of Cardiology[21] recommends 04:26:48 131 Thromboembolism and Anticoagulation that D-dimer levels should be measured, as a proportion of patients will have a normal result and be able to avoid unnecessary imaging. The prevalence rates for inherited thrombophilias in European populations are shown in Table 17. The risk for protein C, S, and antithrombin deficiencies may be underestimated due to the low prevalence of these conditions, as data are drawn from inadequately sized populations. Performing thrombophilia testing in the acute stages of thrombosis gives misleading results and is not recommended. Levels of antithrombin, protein C, and protein S may fall, particularly if thrombus is extensive. The value of thrombophilia testing is in providing information that can influence the duration and intensity of anticoagulation, such as when antiphospholipid syndrome is identified. However, modern management is changing and even those with persistent antiphospholipid syndrome would not usually be offered long-term anticoagulation where their first thrombotic event is in pregnancy, because outside of pregnancy they will be less prothrombotic. Urea, electrolytes, and liver function tests should also be checked to exclude renal or hepatic dysfunction, which are cautions for anticoagulant therapy. Vitamin K antagonists are rarely employed in this setting as they cross the placenta and are associated with increased pregnancy loss, a specific embryopathy, and other abnormalities in the first trimester, as well as fetal hemorrhagic complications and central nervous system anomalies at any stage of pregnancy. However, there are increasing data supporting once daily dosing and it is uncertain whether once daily or twice daily dosing is most appropriate for treatment as pharmacokinetic and observational data suggest similar efficacy and safety[7,15]. Once full anticoagulation has been commenced, the woman should be encouraged to mobilize while wearing compression hosiery as this has been shown to reduce pain and swelling in the affected leg. Outwith pregnancy in patients with underlying malignancy, a reduction in dose has been shown to be safe after 4 weeks of therapeutic anticoagulation. Although there have been no studies directly comparing these two types of dosing strategies in pregnant women, this type of modified dosing regimen may be useful in pregnant women at increased risk of bleeding or osteoporosis[26]. For this reason, wound drains should be considered at cesarean section, and the skin incision should ideally be closed with staples or interrupted sutures to allow easy drainage of any hematoma. If the thrombosis occurred in the last week of pregnancy, consideration should be given to the use of unfractionated heparin (since it can be relatively easily reversed using protamine sulfate and has a short duration of action). Subcutaneous unfractionated heparin should be discontinued 12 hours before and intravenous unfractionated heparin stopped 6 hours before induction of labor or regional anesthesia. It is characterized by chronic persistent leg swelling, pain, a feeling of heaviness, dependent cyanosis, telangiectasis, chronic pigmentation, eczema, associated varicose veins and in some cases lipodermatosclerosis, and chronic ulceration. Symptoms are made worse by standing or walking and improve with rest and recumbency. Graduated elastic compression stockings were thought to improve the microcirculation by assisting the calf muscle pump, reducing swelling and reflux, and reducing venous hypertension[4]. Oxygen should be administered and the circulation supported using intravenous fluids and inotropic agents if required. After thrombolytic therapy has been given, an infusion of unfractionated heparin can be given. There are now a large number of published case reports on the use of thrombolytic therapy in pregnancy, streptokinase being the agent most frequently employed. Streptokinase does not cross the placenta; this is also thought to be true for other thrombolytics. The maternal bleeding complication rate is approximately 6%, which is consistent with that in non-pregnant patients receiving thrombolytic therapy. Most bleeding events occur around catheter and puncture sites and, in pregnant women, from the genital tract. If the patient is not suitable for thrombolysis or is moribund, a discussion with the cardiothoracic surgeons with a view to urgent thoracotomy or extracorporeal life support should be had [7,28,29]. She developed hyperemesis in the eleventh week of pregnancy and was unable to keep any fluids down and so was admitted for intravenous fluids and antiemetics and was given thromboprophylaxis with 5000 units of dalteparin. The hyperemesis settled on conservative management and she was discharged home after 3 days. However, 2 days later she developed pain in the left calf and returned for review. She was sent for a Duplex ultrasound scan, which showed a popliteal thrombus extending into the calf. She was anticoagulated with 1 mg/kg dalteparin twice daily and the calf pain settled within 48 hours.
If severe gastritis develops medicine buddha cheap zofran 4 mg on line, as in the present case medicine 72 order zofran online pills, the intravenous route can be used for administering the bisphosphonate drug treatment 1860 neurological purchase zofran 8 mg line. It is usually recommended in severe cases of osteoporosis when other drugs fail to achieve the desired therapeutic effects medications kosher for passover buy zofran 4 mg lowest price. Their efficacy is thought to be due to their effect on serotonin and norepinephrine levels symptoms jock itch generic 8 mg zofran. Two agents, venlafaxine and paroxetine, have been most studied for this indication and are considered the drugs of choice from this class of drugs. These drugs have therapeutic effects only in controlling vasomotor symptoms; they do not have any protective effect on bone mineral density or urogenital mucosa. The doses of these agents used for controlling the vasomotor symptoms of menopause are much lower than what is used for their antidepressant effects. Some of the common adverse effects of venlafaxine are dry mouth, decreased appetite, nausea, constipation, and increased blood pressure. A, B, C, D All these drugs have no therapeutic role in controlling vasomotor symptoms of menopause. The patient noticed that they were often precipitated by bending or by other movements that compressed the abdomen. Occasionally the episodes were accompanied by nausea, anxiety, and a sense of impending doom. After 2 weeks of therapy, her blood pressure was somewhat reduced (165/105 mm Hg), but she was still hypertensive. The patient did not smoke, denied the use of illicit drugs, and drank alcohol occasionally. Physical examination showed a well-developed and nourished black female who looked her age and was in no acute distress. Vital signs were as follows: Blood pressure while lying: 182/112 mm Hg (left arm), 178/110 mm Hg (right arm) Blood pressure while standing: 160/92 mm Hg (left arm), 154/96 mm Hg (right arm) Heart rate: 88 bpm and regular Respirations: 16/min and regular the remainder of the physical examination was unremarkable. The results were the following: 24 hours urinary catecholamine excretion Epinephrine: 90 µg/dL (normal 1. She was free of headaches and was no longer having palpitations or episodes of sweating. She was scheduled for surgery to remove the left adrenal mass, and 5 days before the operation she was given metyrosine. Initially, with manipulation of the adrenal mass, her blood pressure rose to 200/100 mm Hg and her heart rate was 92 bpm. Which of the following triad of symptoms, when occurring during paroxysmal attacks, strongly suggests the diagnosis of pheochromocytoma The physician thought that the intake of this medication most likely triggered the paroxysmal episode. Which of the following statements best explains the reason for this modest effect Activation of which of the following adrenoceptors most likely contributed to the increase in E. Which of the following actions on brain autonomic receptors most likely mediates the diagnostic activity of this drug Which of the following pairs of adrenoceptors represent the molecular targets of this drug Two days after initiating therapy with phenoxybenzamine, propranolol was added to E. The primary reason for this addition was to counteract which of the following pheochromocytoma-induced effects Which of the following sets of action depicted in the attached table most likely occurred shortly after the administration of this drug Answer: D Pheochromocytoma is a tumor of chromaffin cells that secrete catecholamines. In 90% of cases pheochromocytomas are found in the adrenal medulla, but they may also be found in other tissues derived from neural crest cells (paraganglia of the sympathetic chain, carotid body, genitourinary system, brain). Chromaffin cells appear malignant upon microscopic examination, but the tumor is considered benign in 90% of cases (no metastases) and is curable if correctly diagnosed and properly treated. Learning objective: Describer the triad of symptoms that strongly suggest the diagnosis of pheochromocytoma. By activating 1 (and to a lesser extent 2) receptors in the heart catecholamines increase myocardial contractility, conduction, excitability, frequency, and oxygen consumption. Catecholamines produce a prompt increase in the metabolic rate (likely due to cutaneous vasoconstriction and increased muscular activity) and then a delayed increase probably due to oxidation of lactate in the liver. The sudden release of catecholamines causes a sharp increase of blood pressure, which is the most likely cause of the severe headache in these patients. A, B, D, E, F All these items contain at least one symptom that is absent in pheochromocytoma patients. Learning objective: Identify the drug that can trigger paroxysmal symptoms in a patient with from pheochromocytoma. It is a component of some over-the-counter preparations used as nasal decongestants. The drug acts, at least in part, by releasing catecholamines from postganglionic sympathetic terminals. In pheochromocytoma, catecholamine stores within sympathetic nerve endings are increased because the catecholamines produced by the tumor are, in part, taken up by the sympathetic terminals. Therefore the intake of a medication containing pseudoephedrine can trigger a paroxysmal episode in a patient with pheochromocytoma. The drug could counteract, not trigger, some symptoms of pheochromocytoma (tachycardia). Atropine could trigger some symptoms of pheochromocytoma (tachycardia), but could counteract other symptoms (sweating). Answer: C Paroxysmal attacks of headache, sweating, and tachycardia are so common that the lack of all three would virtually exclude the diagnosis of pheochromocytoma. Hypertension, the most prominent feature, may be paroxysmal (45%) or persistent (50%) and is rarely (5%) absent. Other common symptoms include tachypnea, angina, nausea and vomiting, epigastric pain, paresthesias, constipation, and a sense of impending doom. Epinephrine, norepinephrine, and dopamine are secreted by the adrenal medulla, and most of the symptoms of pheochromocytoma are due to the exces- 313 35 Pheochromocytoma E Prazosin is an 1-adrenoceptor antagonist. The drug could counteract, not trigger, some symptoms of pheochromocytoma (hypertension). The drug could trigger some symptoms of pheochromocytoma (tachycardia) but could counteract other symptoms (headache). Learning objective: Explain why a calcium channel blocker is usually not fully effective in decreasing the hypertension of a patient suffering from pheochromocytoma. A A positive family history for myocardial infarction is known to be a major risk factor for cardiovascular disease but not for pheochromocytoma. D A positive family history for lymphoma can be a risk factor for blood cancers but not for pheochromocytoma. Learning objective: Explain the reason for chest pain in a patient with pheochromocytoma. Even if only 1 out of 1,000 hypertensive patients turn out to be affected by this disease, pheochromocytoma should always be suspected in patients with hypertension, and this diagnosis should be excluded only after appropriate investigation. Nifedipine is a calcium channel blocker that, at therapeutic doses, blocks only L-type calcium channels on the smooth muscle membrane. By reducing calcium entry the drug provokes a vasodilation, mainly on the arterioles. Therefore it antagonizes the vasoconstricting action of catecholamines by acting on receptors different from those activated by catecholamines. In conclusion, it can be defined as a functional antagonist of norepinephrine and epinephrine. A general rule in pharmacology is that a functional antagonist is less effective than a pharmacological antagonist, in most cases. Answer: B Catecholamine-induced tachycardia requires an increased amount of oxygen, but, in spite of coronary vasodilation, oxygen demand is higher than oxygen supply, causing a relative heart ischemia. A Catecholamines cause coronary vasodilation, not vasoconstriction, because the heart relies primarily on metabolic mechanisms to adapt the caliber of its coronary vessels to the need of oxygen. D Only extremely high tachycardia can increase pulmonary artery pressure, due to the increased left diastolic volume. Learning objective: Describe a common cardiovascular effect in a patient with pheochromocytoma. Answer: B Up to 25% of pheochromocytomas are considered to be inherited and associated with other endocrine tumors. Answer: B An excessive fall in blood pressure that occurs on assuming the upright position 314 Answers and Explanations is called postural (or orthostatic) hypotension. It occurs primarily for two reasons: the baroreceptor reflex cannot function properly, because there is an impairment of the afferent, central, or efferent portion of the autonomic reflex arc. Under normal conditions, the gravitational stress of sudden standing normally causes pooling of blood in the venous capacitance vessels of the legs and trunk. The subsequent transient decrease in venous return and cardiac output results in reduced blood pressure, which, in turn, decreases the stretching of baroreceptors located in the carotid sinus and in the aortic arch. This leads to the removal of the inhibitory influences on vasomotor centers in the brain, resulting in a compensatory reflex increase in sympathetic drive. Therefore heart rate, myocardial contractility, and total peripheral resistance increase, thereby restoring the blood pressure to normal. Even if the ultimate cause is uncertain, it is likely that the two main causes of postural hypotension are operative. Pheochromocytoma can cause volume depletion because of chronic vasoconstriction and profuse sweating. Pheochromocytoma can impair the baroreceptor function because of chronic activation of sympathetic receptors. C Coronary vasodilation, not vasoconstriction, occurs in pheochromocytoma because the increased heart work needs an increased oxygen supply. D Pheochromocytoma usually causes a decrease, not an increase, in cardiac output due to volume depletion. Learning objective: Identify the adrenoceptor that most likely contributed to the hyperglycemia in a patient with pheochromocytoma. Answer: A Catecholamines have several different actions that can increase blood glucose. These include the following: Inhibition of insulin secretion (the activation of 2-receptors in pancreatic cells, which inhibits the secretion, predominates over the activation of 2-receptors, which stimulates the secretion). Stimulation of glycogenolysis in the liver (through activation of 2adrenoceptors). Glycogenolysis is stimulated also in muscle, but the glucose is used by the muscle cells to provide energy. Stimulation of gluconeogenesis in the liver (though activation of 2-adrenoceptors). Stimulation of glucagon secretion (through activation of 2adrenoceptors), which in turn stimulates liver glycogenolysis. By decreasing oxygen supply to the liver the glucose output should be decreased, not increased. D, E Activation of dopamine D1- and D2-adrenoceptors does not affect blood glucose. Answer: A Clonidine is an 2-adrenoceptor agonist that acts mainly on presynaptic receptors in the rostral ventrolateral medulla (the vasomotor center). This action reduces the efferent sympathetic discharge, thereby decreasing the catecholamine release from the adrenal medulla in a normal person. This action also contributes to the reduction of the efferent sympathetic discharge. Learning objective: Explain why clonidine cannot significantly decrease catecholamine secretion in a patient with pheochromocytoma. By blocking 1-adrenoceptors the drug lowers the blood pressure and is the first-line agent for the preoperative management of pheochromocytoma. Learning objective: Identify the pheochromocytoma/symptom that is best antagonized by phenoxybenzamine. Answer: D Unlike normal chromaffin cells, pheochromocytoma cells are not innervated and therefore not susceptible to manipulation by drugs that decrease central sympathetic outflow. In a patient without pheochromocytoma, plasma norepinephrine should fall to < 400 pg/mL after clonidine. The modest decrease in the present case supports the diagnosis of pheochromocytoma. Since it causes a sympathetically mediated vasoconstriction, the central sympathetic outflow should be decreased, not increased. D Unlike the normal adrenal medulla, which secretes ~ 85% epinephrine, most pheochromocytomas secrete predominantly norepinephrine. Learning objective: Explain the molecular mechanism of action of phenoxybenzamine. This activation decreases insulin secretion, leading to hyperglycemia, a well-known effect of pheochromocytoma. By blocking 2-adrenoceptors, phenoxybenzamine counteracts the epinephrine-induced decrease of insulin secretion. A Sweating is a sympathomimetic effect, but the receptors involved are mainly cholinergic; therefore sweating cannot be blocked by an -antagonist. Moreover, in patients with pheochromocytoma the effect is most likely indirect, related to the hypermetabolism induced by catecholamine excess.
A Activation of D2-adrenoceptors in the chemoreceptor trigger zone is usually caused by high doses treatment quad strain purchase 4 mg zofran, not intermediate doses symptoms constipation zofran 8 mg order visa, of dopamine symptoms concussion purchase zofran 8 mg overnight delivery. C By activating D1-adrenoceptors in the proximal tubule medications lisinopril purchase zofran 4 mg amex, dopamine decreases rather than increases Na+ reabsorption treatment receding gums buy zofran 8 mg fast delivery. D By activating 1-adrenoceptors in the macula densa, dopamine increases rather than decreases renin secretion. E the systemic vascular resistance is not much affected by an intermediate dose of dopamine because the D1-mediated vasodilation of the splanchnic and renal beds is counteracted by the vasoconstriction caused by the release of norepinephrine. Dopamine is not effective when given orally because it is completely metabolized by the liver. It defines the ranges of doses with a high chance of efficacy and a low chance of adverse effects, that is, the range of doses which have a high probability of therapeutic success. A the therapeutic index is the ratio between a harmful dose and an effective dose of a drug. C Drug efficacy is the maximal effect a drug can produce, irrespective of the dose given. D the median therapeutic dose is the dose of a drug that can produce a given effect in 50% of the population under study. A Dopamine can cause nausea and vomiting, but this is related to the dose, not to the administration procedure. For every drug that follows a first-order elimination kinetics and is administered at fixed intervals, the time needed to achieve the steady-state plasma concentration (exactly 94% plasma concentration) is equal to 4 half-lives. This time is independent of the dose and the dosing 55 7 Cardiogenic Shock intervals (provided that this interval is less than 4 half-lives). B Opening of ligand-gated K+ channels would cause hyperpolarization of the cardiac muscle membrane, adversely affecting heart contractility. C Increased synthesis of diacylglycerol can follow the activation of 1-adrenoceptors, not of 1-adrenoceptors. Learning objective: Identify the hemodynamic parameter that mediates the increase in urine output after dopamine infusion in a patient with cardiogenic shock. Answer: D A widely used index of cardiac oxygen consumption is the so-called double product (also called the pressure-rate product), which is the product of systolic blood pressure and heart rate. This suggests that dopamine has likely affected adversely the myocardial oxygen supply/demand ratio. Answer: A Dobutamine is a selective 1-adrenoceptor agonist and therefore is expected to increase the stroke volume. Selectivity is not absolute, and at higher doses the drug may also activate 2- and 1-adrenoceptors. By improving cardiac contractility dobutamine offsets this activation and therefore decreases, not increases, these hemodynamic parameters. He tried to control diarrhea with an over-the-counter preparation of loperamide, with little success. The patient also reported that he had lost 16 pounds and that 3 days ago he became feverish (100°F, 37. The patient denied alcohol or illicit drug use, but he had been smoking one pack of cigarettes daily for the past 15 years. His physical examination was essentially normal except for an abdominal tenderness on palpation on the right lower quadrant. Pertinent lab results on admission were as follows: Blood hematology Hematocrit 28% (normal 3648%) Hemoglobin (Hgb) 8. Endoscopy A cobblestoned-appearing terminal ileum and ascending colon, with areas of normal tissue separated by areas of ulcerated mucosa. Intestinal biopsy A patchy acute and chronic inflammatory infiltrate, crypt abscesses, and several noncaseating granulomas. One week later he was dismissed from the hospital with the same postdischarge therapy. He had fewer bowel movements (34 each day), but his appetite and weight were not increased, and he still had intermittent abdominal pain and a low-grade fever. The gastroenterologist decided to add methotrexate and metronidazole to the therapy. Five weeks into the new therapy all the symptoms disappeared, and the prednisone dosage was tapered to 10 mg/daily. The patient also noticed that his feces had an oily appearance and were especially foul smelling. Direct activation of which of the following receptors most likely mediated the therapeutic effect of the drug in this patient Which of the following molecular actions most likely contributes to the therapeutic effect of prednisone in G. The killing of which of the following cells primarily mediates the therapeutic effect of methotrexate in G. The inhibition of which of the following enzymes most likely mediates the therapeutic effect of methotrexate in G. Which of the following molecular actions on bacterial cells most likely mediated the therapeutic effect of metronidazole in G. Which of the following is a potentially lethal adverse effect that can occur soon after infliximab administration Because infliximab was no longer effective, the gastroenterologist decided to substitute it with another monoclonal antibody. Which of the following molecular actions most likely mediated the prophylactic effect of the drug in this patient The blockade of which of the following endogenous compounds most likely mediated the therapeutic effect of the drug in this patient The distinguishing feature of the disease is that the inflammation is transmural. E Disease involving the rectum only (proctitis) usually results from infection or radiation. Answer: D In up to 50% of cases noncaseating granulomas are detected in the bowel wall by an intestinal biopsy. These symptoms, however, are not specific, and many patients are first seen with an acute abdomen that simulates acute appendicitis. Activation of serotoninergic receptors in the gastrointestinal system would increase intestinal peristalsis, an adverse effect in patients with diarrhea. D Activation of 2-adrenoceptors can cause relaxation of intestinal smooth muscle, but 2-adrenoceptor agonists are not used to treat diarrhea. Activation of these receptors in the gastrointestinal system would increase intestinal peristalsis, an adverse effect in patients with diarrhea. Answer: E Loperamide is the most common overthe-counter preparation to treat diarrhea. The drug is an opioid agonist that directly activates -receptors in the enteric nervous system. This activation of both enteric neurons and smooth muscles ultimately causes a decrease in contraction of intestinal longitudinal muscles but a marked increase in contraction of circular muscles. Therefore propulsive peristaltic waves are diminished and tone is increased, thus relieving diarrhea. The drug cannot cross the blood brain barrier and is therefore free of central properties and potential for addiction. A Activation of 2-adrenoceptors can cause relaxation of smooth muscle, but 2-adrenoceptor agonists are not used to treat diarrhea. Activation of these receptors would increase both sympathetic and parasympathetic firing. Because the parasympathetic is predominant in the gastrointestinal system, its activation would increase intestinal peristalsis, an adverse effect in patients with diarrhea. The second cause is decreased oral intake since patients with bowel strictures feel better when they do not eat. Aminosalicylates are believed to work topically in areas of injured gastrointestinal mucosa. These drugs likely act by inhibiting cyclooxygenases, thus decreasing prostaglandin synthesis. In support of prostaglandins as the mediators for inflammatory bowel disease are reports of disease exacerbation after oral administration of misoprostol, a prostaglandin derivative. However, specific inhibitors of prostaglandins are less effective than mesalamine and related compounds. Other potential mechanisms of aminosalicylates are related to their inhibition of the production of proinflammatory cytokines. Mesalamine is well absorbed through the small intestine and does not reach the distal small bowel or colon in appreciable quantities. To overcome this problem a number of pharmaceutical formulations (sulfasalazine, olsalazine, etc. Mesalamine itself is formulated in various ways (time-release granules, tablets with a pH-dependent coating, etc. The gene expressionmediated induction of synthesis of anti-inflamma- tory cytokines contributes to the antiinflammatory effect of glucocorticoids. E Lipocortin is an enzyme that acts as an inhibitor of phospholipase A2, the enzyme that catalyzes the synthesis of eicosanoids. Glucocorticoids increase the synthesis of lipocortin, thereby inhibiting the synthesis of eicosanoids. Answer: E Glucocorticoids inhibit the synthesis of almost all known proinflammatory cytokines and can stimulate the synthesis of some anti-inflammatory cytokines. A Glucocorticoids inhibit prostaglandin biosynthesis but have no effect on the metabolism of prostaglandins. B, C Glucocorticoids increase, not decrease, the biosynthesis of lipocortin, which in turn inhibits, not enhances, the activity of phospholipase A2. D the complement system is an important mediator of host defense and has proinflammatory activity. Answer: C Methotrexate is an antineoplastic drug often used as an immunosuppressive. Many agents that kill proliferative cells appear to work at a similar level in immune response. Methotrexate can reduce only the pain related to neoplastic or immunological disorders. Answer: C T-helper cells are the major effector cells in several autoimmune diseases. Killing these cells represents an important goal of any immunosuppressive treatment. A, B, D these cells are not dividing and therefore are not the target for methotrexate. These cells are killed because they are rapidly proliferating, and this explains myelosuppression, which is a major toxic effect of methotrexate. Metronidazole has a potent bactericidal activity against obligate anaerobes, including Bacteroides, the most common anaerobes of normal intestinal flora. The fact that in the normal adult colon 96 to 99% of bacterial flora consists of anaerobes explains why metronidazole is especially useful in reducing this flora. A Mycoplasmas are facultative anaerobes and therefore not sensitive to metronidazole. Answer: A Metronidazole is an antibiotic active against most microaerophilic and anaerobic bacteria and anaerobic protozoa. These microorganisms, unlike their aerobic counterparts, contain electron transport components, called ferredoxins, that can donate electrons to metronidazole. B Inhibition of cell wall synthesis would be the mechanism of action of betalactam antibiotics. D Synthesis of abnormal proteins would be part of the mechanism of action of aminoglycoside antibiotics. E Inhibition of purine synthesis would be the mechanism of action of trimethoprim-sulfamethoxazole. Answer: E Methotrexate inhibits dihydrofolate reductase, the enzyme that catalyzes the reduction of folate to dihydrofolate and the reduction of dihydrofolate to tetrahydrofolate. The decreased synthesis of tetrahydrofolate, which is a one-carbon-unit carrier, inhibits the synthesis of purines and pyrimidines, which are essential for the synthesis of ribonucleotides. Inhibitors of topoisomerase of bacterial cells are the fluoroquinolone antibiotics. C Immunosuppressive drugs such as cyclosporine and tacrolimus are inhibitors of calcineurin enzyme. Short-term benefits after a single infusion may persist for up to 12 weeks, but a number of serious adverse effects can occur. C Granulocyte colony stimulating factor is a cytokine used primarily in stem cell transplantation. Learning objective: Describe a potentially lethal adverse effect that can occur soon after infliximab administration. Both reactions can be lethal and can be minimized by pretreatment with a high dose of glucocorticoids. Acute infusion reactions occur in about 20% of patients treated with monoclonal antibodies and represent the most serious adverse effect of these drugs. A, B, C, D, F All these adverse effects have been associated with infliximab administration in postmarketing reports, but their frequency is very low, and often a causal relationship to infliximab cannot be established. Answer: E All infusion reactions involve the immune system; however, some (anaphylactic, caused by subsequent exposure) are allergic in nature and usually mediated by immunoglobulin E (IgE). Symptoms and signs include rash, coughing, sneezing, wheezing, difficulty breathing, urticaria, angioedema, abdominal cramping, hypotension, and palpitations. Other reactions (anaphylactoid, caused by first exposure) are not true allergic reactions and are mediated by cytokine release (the so-called cytokine-release syndrome). Symptoms and signs include high fever, chills, myalgia, joint pain, tremor, confusion, hallucinations, and seizures. The clinical manifestations of both syndromes are almost the same, and in nontypical cases differentiation between the two syndromes can be 17.
Buy discount zofran line. Meningitis - causes symptoms diagnosis treatment pathology.
However medicine 60 zofran 8 mg order free shipping, families should be offered a choice of counselor since they may be more comfortable discussing complex issues medications with sulfa order zofran with a mastercard, particularly termination of pregnancy treatment laryngomalacia infant buy zofran from india, with a counselor who does not also regularly provide medical treatment to a member of their family inoar hair treatment cheap zofran 8 mg buy. Genetic counseling is a step-wise process and may require discussion about the following issues: · family diagnosis of the bleeding disorder and its clinical severity; · inheritance pattern of the disorder within the family to either exclude carriership or to identify "possible" and "obligate" carriers; · penetrance of the bleeding disorder; · pattern of transmission and consequences of the bleeding disorder in future offspring; · benefits and hazards of carrier detection techniques; and · options available for management of pregnancy x medications zofran 8 mg purchase without prescription, including prenatal diagnosis. The disorders are caused by mutations in the long arm of the X chromosome in the F8 gene (Xq28) or the F9 gene (Xq27). The two disorders represent the most common of the severe heritable coagulation disorders with a combined prevalence of around 1 in 10 000. Approximately 5060% of males with hemophilia have a positive family history, which usually provides the opportunity for informed pre-pregnancy genetic counseling and prenatal diagnosis[4]. The analysis of an accurate family pedigree is essential to establish the probability of hemophilia carriership and transmission risk. Sons of males with hemophilia will not have hemophilia unless there is also maternal hemophilia carriership. Daughters of males with hemophilia will always inherit hemophilia and will therefore be obligate hemophilia carriers. Approximately 4050% of individuals newly diagnosed with hemophilia have no family history of hemophilia. Hemophilia is highly penetrant, meaning that the severity of the disease remains constant between generations. Sporadic hemophilia in males arises because of new mutations in the F8 or F9 genes occurring during gametogenesis in either the 04:31:19 256. However, spontaneous mutations occur more readily during spermatogenesis than oogenesis. Therefore, the causative mutation in a male with sporadic hemophilia is more likely to have arisen during spermatogenesis in the maternal grandfather than in oogenesis in the mother. It follows that mothers of males with sporadic hemophilia are likely to be constitutional hemophilia carriers. Observational population studies confirm this prediction and show that approximately 90% of mothers of males with sporadic hemophilia are carriers and therefore, have significant risk of transmitting hemophilia to future male offspring[5]. For women who have a history of hemophilia in antecedent male relatives, it may be possible to rule out carriership of the familial hemophilia mutation by analysis of the family pedigree alone. However, it is essential to recognize that there is a small probability of second hemophilia mutations arising through spontaneous mutagenesis. Therefore, women in whom carriership can be ruled out by pedigree analysis should be counseled that the risk of an affected male fetus is not zero, but instead is approximately the same as that of the background population. Laboratory Detection of Hemophilia Carriership Determining the probability of hemophilia carriership by pedigree analysis is essential for the genetic counseling process. However, all women who are potential hemophilia carriers should also be offered laboratory carriership detection. Two complementary approaches are available: coagulation factor activity assays and genetic testing. However, there is wide variation in factor activity between carriers and there is significant overlap with women who are not hemophilia carriers. Therefore, measurement of coagulation factor activity may guide identification of hemophilia carriers but is insufficient for definitive diagnosis. Genetic Detection of Carriership Female hemophilia carriers are heterozygous for mutations in F8 or F9 and demonstration of a hemophiliaassociated mutation in these genes is sufficient to diagnose carriership. It is good practice to confirm hemophilia carriership with genetic testing even in women identified as obligate carriers by pedigree analysis. Definitive exclusion of hemophilia carriership in potential carriers requires demonstration that the hemophilia mutation in the family is absent. In this circumstance, prior knowledge of the causative mutation in a male with hemophilia or an obligate female carrier from the family is essential. Testing the potential for transmission of hemophilia in asymptomatic women raises complex moral issues for the individual and families undergoing testing. The full implications of genetic testing should therefore be discussed during counseling and informed written consent is mandatory. Counseling should include specific discussion about the limitations of F8 and F9 genetic analysis. These resources are invaluable for confirming that a newly identified mutation in a hemophilia family is causative and in predicting the future clinical phenotype, including inhibitor risk, of affected males. Limitations and Hazards of Genetic Diagnosis of Carriership Failure to Detect Causative Mutations Approximately 5% of hemophilia mutations are not detected by inversion analysis or analysis of the coding sequence of F8 or F9. Some mutations, such as large deletions, may be readily detected in males with standard Sanger sequencing techniques but this is not the case in heterozygous female carriers. This may not be informative in all families and, because of genetic recombination events, has lower diagnostic accuracy than direct mutation detection by sequencing. Mutations Associated with Hemophilia Although more than 1800 F8 mutations have now been identified in individuals with hemophilia A, many defects are recurrent and have been recognized in multiple affected families. A major structural rearrangement of the F8 gene resulting from an inversion involving intron 22 accounts for approximately 50% of cases of severe hemophilia A. Other recurrent mutations associated with severe hemophilia A include an inversion affecting intron 1, point mutations, nonsense mutations, deletions, or other major structural changes in F8 that prevent expression of the gene. Mild hemophilia A and hemophilia B are False-Negative Carrier Detection Because of Somatic Mosaicism An individual is a somatic mosaic for hemophilia when a spontaneous hemophilia mutation occurs in a somatic cell during early embryogenesis rather than during gametogenesis in one or other parent. This means that in an affected embryo, the hemophilia mutation is present in some cells, including germ 04:31:19 258. Normal sequence with no evidence of copy number variation (results lie between red and blue lines). Those germ cells which contain the hemophilia mutation may then go on to form gametes, potentially resulting in transmission of the hemophilia mutation to subsequent generations. Somatic mosaicism has been identified in a female proband in more than 10% of families with severe hemophilia and, in some cases, the hemophilia mutation was present in up to 25% of maternal cells[13]. This may result in mis-classification of somatic mosaic mothers as "not hemophilia carriers. Estimates of the recurrence risk for non-carrier mothers due to mosaicism for X-linked disorders are variable, with reported values ranging from 3 to 10%. For families with sporadic hemophilia B, one study estimated that women have a risk of hemophilia B in a second fetus of <6%[14]. Prenatal Fetal Sexing Fetal sexing is an important first step in the evaluation of the fetus of a pregnant hemophilia carrier since if a female fetus is identified, the probability of a significant bleeding disorder is very low and a restrictive delivery with hemostatic precautions is not necessary [15]. Prenatal Diagnosis of Hemophilia Women who have been identified as hemophilia carriers by pedigree analysis and laboratory investigation may be offered several different options for prenatal diagnosis. Involvement of healthcare professionals with expertise in fetal medicine is essential. Prenatal diagnosis in hemophilia is currently offered to families for two different reasons: 1. This is achieved either by fetal sexing or by mutation detection to rule in or rule out an affected fetus. This option is typically performed in the third trimester when the absolute risk to the pregnancy by amniocentesis is low. For early definitive diagnosis of hemophilia in a male fetus using first trimester prenatal genetic diagnosis to enable the option of termination of an affected pregnancy. It is advised that a dating ultrasound is used to confirm gestational age, to limit the need for a repeat test. Detection of the hemophilia mutation present in the family is then performed only on cells from confirmed male fetuses. However, higher miscarriage rates and fetal talipes have been associated with amniocentesis performed before 15 weeks[21]. Cord blood sampling is unsuitable for prenatal diagnosis of hemophilia because of the risk of bleeding if the fetus is affected with hemophilia. Third Trimester Amniocentesis Amniocentesis performed at 3436 weeks enables definitive genetic diagnosis in pregnancies where the fetus is at risk of a moderate or severe bleeding disorder. Late amniocentesis carries a risk of early rupture of membranes and premature labor of approximately 1% in experienced centers[20]. Consequently, women routinely receive steroid therapy prior to the procedure to improve fetal lung maturity. Late amniocentesis can only be performed where the causal hemophilia mutation is known and results can be expected within 35 working days. All mothers should be counseled about risks of early labor which could result in delivery before the genetic test result is known. The uptake of this approach is very low in most reported series of pregnancies in hemophilia carriers. Genetic results can be expected within 35 working days of the procedure, thereby facilitating early termination, if appropriate. Genetic analysis showed five unaffected fetuses, in which delivery using routine practice in local hospitals was possible, without restrictive pro-hemostatic precautions. Preimplantation sexing with reimplantation of female or unaffected male embryos requires standard in vitro fertilization techniques, and then harvesting of cells from embryos at the 8-cell stage for analysis. These approaches are technically feasible in hemophilia and have now been performed in small numbers of successful pregnancies. Preimplantation genetic diagnosis may be the preferred option for those women who do not wish to consider termination of an affected pregnancy. However, assisted reproductive technology is stressful and requires invasive transvaginal egg collection which in some carriers may require pro-hemostatic support. Genetic Counseling for Other Severe Heritable Bleeding Disorders Genetic counseling, carrier detection, and prenatal diagnosis should also be considered in families with other rare heritable bleeding disorders which may also present a bleeding risk to an affected fetus. Since most of the rare bleeding disorders show autosomal recessive inheritance, genetic counseling requires discussion about the transmission of homozygous or compound heterozygous mutations from both parents. Affected fetuses are usually sporadic and arise in families with no bleeding history in heterozygous "carrier" ancestors. For mothers who are known heterozygous "carriers" or who themselves are homozygous or compound heterozygous for a recessive bleeding disorder, accurate prediction of fetal bleeding risk may require partner testing. This is particularly important in consanguineous partnerships where the risk of transmission of homozygous recessive mutations is high. Genetic counseling for the rare bleeding disorders should reflect that the relationship between plasma coagulation factor activity and bleeding risk in affected individuals is less predictable than in hemophilia and that some disorders show variable penetrance. Since the range of reported mutations in the rare bleeding disorders is less than for hemophilia, detection of previously undescribed mutations in affected families is common. Uncertainty about whether a candidate mutation is causal may hamper genetic carrier detection and prenatal diagnosis in some families. One emerging approach is to quantify accurately the relative concentration of mutant compared to normal gene sequences in maternal blood using. Fetal sex testing plays no part in prenatal diagnosis of the rare bleeding disorders since these disorders are autosomally inherited. Mothers may require factor concentrate therapy or other hemostatic measures such as tranexamic acid before invasive diagnostic procedures. She has previously received genetic counseling and her carriership status has been confirmed by genetic testing. She and her partner have agreed that they would consider a termination if the fetus was an affected male. In this case study, after detailed discussion and counseling, the family chose to proceed with termination of pregnancy using suction techniques, which are possible up to the end of the 12th week of gestation and are psychologically and physically less demanding than termination at a later gestation. The boy had been born at term by spontaneous vaginal delivery, with no instrumentation. His development was normal and there was no history of bleeding, except an increased propensity to bruise. Genetic testing of the F8 gene using a Southern blotting technique confirmed the inversion 22 mutation in the boy but showed only normal F8 in the mother. Therefore, the mother was informed that hemophilia in her son had arisen through a spontaneous mutation and that she was not a carrier. Three years later, the mother delivered a second son through a normal vaginal delivery. Although the second son was initially asymptomatic, he presented at 14 months old with a knee hemarthrosis. Subsequent investigations confirmed that he also had severe hemophilia A caused by the inversion 22 mutation. This case highlights that women with a male child with apparently de novo hemophilia should be counseled very carefully if they are found not to be a carrier of the familial mutation by conventional genetic testing. Somatic mosaicism should be discussed with women in this scenario and should be evaluated using specialist genetic testing techniques. A framework for genetic service provision for hemophilia and other inherited bleeding disorders. Prenatal diagnosis in hemophilia A: experience of the genetic diagnostic laboratory. Mutation rates in humans I: overall and sex-specific rates obtained from a population study of hemophilia B. Noninvasive prenatal testing for fetal sex determination: is ultrasound still relevant European Journal of Obstetrics & Gynecology and Reproductive Biology 2013; 171: 197204. Foetal sex determination in maternal blood from the seventh week of gestation and its role in diagnosing hemophilia in the foetuses of female carriers. Third trimester amniocentesis for diagnosis of inherited bleeding disorders prior to delivery. Live birth following the first mutation specific preimplantation genetic diagnosis for hemophilia A. Worldwide about 76 000 pregnant women die each year from pre-eclampsia and related hypertensive disorders. And, the number of babies who die from these disorders is thought to be in the order of 500 000 per annum[1].
References
- Yao F, Seed C, Farrugia A, et al. The risk of HIV, HBV, HCV and HTLV infection among musculoskeletal tissue donors in Australia. Am J Transplant. 2007;7(12):2723-2726.
- Asil T, Ir N, Karaduman F, et al. Combined antithrombotic treatment with aspirin and clopidogrel for patients with capsular warning syndrome: A case report. Neurologist 2012;18:68-9.
- Lassen NA. Control of cerebral circulation in health and disease. Circ Res. 1974;34(6):749-60.
- Parazzini F, Negri E, Vecchia C, et al. Hysterectomy, oophorectomy, and subsequent ovarian cancer risk. Obstet Gynecol. 1993;81:363.
- Turcotte LM, Whitton JA, Friedman DL, et al. Risk of subsequent neoplasms during the fifth and sixth decades of life in the Childhood Cancer Survivor Study cohort. J Clin Oncol 2015;33(31):3568-3575.
- Maruyama K, Takahashi A, Kobayashi T, et al: Diphallia and the VATER association, J Urol 162:2144, 1999.
- Tufro-McReddie A, Norwood VF, Aylor KW, et al: Oxygen regulates vascular endothelial growth factor-mediated vasculogenesis and tubulogenesis, Dev Biol 183(2):139-149, 1997.
