
Priligy
| Contato
Página Inicial
Assistant Professor, Department of Otolaryngology
- Medical Director, OHSU-Northwest Clinic for Voice and Swallowing
- Oregon Health and Science University
- Portland, Oregon
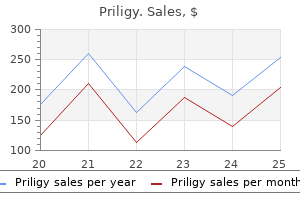
Outcome for patients with fibromyalgia Factors that can help predict the outcome for an individual patient are as yet unknown doctor for erectile dysfunction in bangalore discount priligy 90mg visa. It is generally accepted that symptoms of fibromyalgia will be present to a greater or lesser degree for years impotence in the bible priligy 90 mg buy without a prescription. Response to treatment in the clinical setting is most commonly identified by subjective patient report of change in symptoms and improved function erectile dysfunction at the age of 17 purchase 60 mg priligy with amex. Measurement scales impotence testicular cancer order generic priligy pills, used in the research setting erectile dysfunction utah discount 60mg priligy visa, are not routinely used in clinical practice to follow patients with fibromyalgia. Treatments for fibromyalgia require constant re-evaluation to ensure continued efficacy and absence of side effects. In the absence of a good therapeutic relationship between the patient and the healthcare team, adherence to treatment recommendations is generally poor. Therefore, healthcare professionals should work towards patient partnership in order to achieve realistic outcome goals and optimal health status. The quality of life and functional status of patients with fibromyalgia can be severely affected and even impact on ability to work. Patients should however be encouraged to remain in as normal a pattern of life as possible and should be discouraged from excessive illness focus. Sleep disturbance and fatigue Management of sleep disturbance should incorporate principles of sleep hygiene with attention to negative effects of drugs such as opioids or substances such as alcohol or caffeine. Drug categories showing a positive impact on sleep such as gabapentinoids or cannabinoids may be selected. Use of tranquillizers should be discouraged as there is a danger of continued lifelong use with potential for abuse. Other agents that have been examined in small studies for some effect on sleep in fibromyalgia are cyclobenzaprine, quetiapine, a second-generation antipsychotic agent, and melatonin. A common trend for all of the aforementioned agents is the lack of concrete evidence, either for or against use in fibromyalgia. Fatigue remains a constant challenge in fibromyalgia management, with limited evidence for appreciable effect of pharmacotherapy with the exception of Conclusions Fibromyalgia is an illness seen mostly in women and characterized by widespread body pain with abnormality located in the nervous system. Important 213 Section 5: the Specific Condition: Other Causes of Neuropathic Pain features associated with pain include fatigue, sleep, and mood disturbance. Numerous factors have been proposed as contributing to the onset of this condition, although the exact cause is not yet clarified. Even in the absence of complete understanding of cause and pathogenesis, treatments are directed to alleviate symptoms with the goal to improve functional status, although treatments remain imperfect. In the absence of a cure, fibromyalgia can be expected to persist over time with fluctuations in intensity of complaint. Patients should be strongly encouraged to continue to function at home, in the workplace and in society as normally as possible and should refrain from dependence on a sickness role. Efficacy of multicomponent treatment in fibromyalgia syndrome: a meta-analysis of randomized controlled clinical trials. Efficacy of hypnosis/ guided imagery in fibromyalgia syndromea systematic review and meta-analysis of controlled trials. Comorbid depression and anxiety in fibromyalgia syndrome: relationship to somatic and psychosocial variables. The relationship between fibromyalgia and major depressive disorder: a comprehensive review. The role of psychosocial factors in predicting the onset of chronic widespread pain: results from a prospective population-based study. Ottawa Panel evidence-based clinical practice guidelines for aerobic fitness exercises in the management of fibromyalgia: part 1. Efficacy of hydrotherapy in fibromyalgia syndromea meta-analysis of randomized controlled clinical trials. Evidence for the efficacy of complementary and alternative medicines in the management of fibromyalgia: a systematic review. Efficacy of acupuncture in fibromyalgia syndromea systematic review with a meta-analysis of controlled clinical trials. Chiropractic management of fibromyalgia syndrome: a systematic review of the literature. Tramadol and acetaminophen combination tablets in the treatment of fibromyalgia pain: a double-blind, randomized, placebo-controlled study. Preference for nonsteroidal antiinflammatory drugs over acetaminophen by rheumatic disease patients: a survey of 1,799 patients with osteoarthritis, rheumatoid arthritis, and fibromyalgia. Cannabinoids for treatment of chronic non-cancer pain; a systematic review of randomized trials. Amitriptyline in the treatment of fibromyalgia: a systematic review of its efficacy. A systematic review on the effectiveness of treatment with antidepressants in fibromyalgia syndrome. Treatment of fibromyalgia syndrome with gabapentin and pregabalin a meta-analysis of randomized controlled trials. Systematic review of the comparative effectiveness of antiepileptic drugs for fibromyalgia. Serotonin norepinephrine reuptake inhibitors are a good option for neuropathic pain with concomitant depression or anxiety disorder. For an individual patient, the treatment algorithm is tailored on the basis of the etiology of neuropathic pain, concomitant chronic medical conditions and their medications, individual risks, costs of treatment, and personal preferences. Anatomically, it is divided in to central and peripheral neuropathic pain, the lesion being in the brain or spinal cord, or in the peripheral nervous system, respectively [3]. For moderate and severe neuropathic pain, pharmacotherapy is the most important treatment. In meta-analyses, patients with at least 50% pain relief are classified as responders. The etiology of neuropathic pain, concomitant chronic medical conditions and their medications, individual risks. In addition to pain relief, medication may provide better sleep, improved mood, or relief of anxiety. Although this may indicate the importance of the noradrenergic uptake, this is not entirely clear. Tricyclic antidepressants Evidence of efficacy Tricyclic antidepressants became a mainstay in the management of neuropathic pain before their mechanisms were elucidated and before the advent of systematic ways to evaluate their efficacy. Amitriptyline is the most extensively studied drug in this group, but there is also evidence of the efficacy of clomipramine, desipramine, and imipramine for neuropathic pain [10]. Amitriptyline is the first-line agent for central post-stroke pain, and is recommended also for central neuropathic pain caused by spinal cord injury [5,9,17]. In addition to pain relief, better sleep and anxiolytic effect are helpful in treatment of patients with chronic neuropathic pain. Most antidepressants exert activity on one or both of these monoamines, and each drug has a unique profile with respect to the dominant neurotransmitters affected. Amitriptyline, imipramine, and clomipramine cause a balanced inhibition of serotonin and noradrenaline reuptake in vivo. The serotonin reuptake inhibition is exerted by the compounds themselves whereas the noradrenaline reuptake inhibition comes from their respective metabolites nortriptyline, desipramine, and desmethylclomipramine. Serotonergic processes and noradrenergic processes are integral parts of endogenous pain-inhibition mechanisms; they are involved in the descending modulatory influence on pain. It is proposed that noradrenaline reuptake inhibition is required for an analgesic effect, and that this mechanism is augmented by serotoninergic activity. Antidepressants have also been shown to produce antinociceptive effects in the spinothalamic tract and dorsal horn by inhibiting N-methyl-D-aspartate-induced neural sensitization [23]. Tricyclic antidepressants also possess postsynaptic -adrenergic, H1-histaminergic and muscarine cholinergic receptor-blocking effects (Table 18. Postsynaptic -adrenergic effect may lead to tachycardia and orthostatic hypotension, H1-histaminergic effect can cause sedation, and anticholinergic effect causes dry mouth, urinary retention, accommodation disturbances, constipation, and memory disturbances. The dose is uptitrated with 1025 mg steps every 37 days until relevant pain relief is achieved or intolerable side effects appear. Safety monitoring Electrocardiogram screening is recommended in adults aged over 40 years as well as electrocardiogram follow-up with doses over 150 mg/day. Heart rate and blood pressure follow-up (both supine and standing measurement) is recommended with dose escalation to detect possible tachycardia and orthostatic hypotension. Due to substantial pharmacokinetic variability, monitoring of serum drug concentration may be helpful in treatment, especially when a high dose is needed for therapeutic effect or when adverse effects appear at a low dose. Because amitriptyline may cause weight gain, follow-up of weight is recommended, especially in diabetic patients [25]. Contraindications, precautions, and adverse effects Tricyclic antidepressants cannot be used in the recovery phase of myocardial infarction, or in patients with cardiac conduction disturbances, cardiac incompensation, or porphyria. The most common side effects are dry mouth, constipation, sweating, dizziness, blurred vision, drowsiness, palpitation, orthostatic hypotension, sedation, urinary retention, and sexual dysfunction. Tricyclic antidepressants can also cause cognitive disorders or confusion, gait disturbance, and falls, particularly in elderly patients. A pharmacokinetic interaction involves the effect of one drug on the absorption, distribution, metabolism, or excretion of another drug. Pharmacokinetic interactions can result in changes in serum drug concentrations and might change clinical response. If concomitant use cannot be avoided, consider use of gastroprotection with a proton pump inhibitor. Concomitant use of tramadol and other serotoninergic drugs may cause serotonin syndrome. Choose an alternative analgesic that does not increase serotonin activity Duloxetine Concomitant use may increase the risk for upper gastrointestinal bleeding. In chronic concomitant use, monitor blood counts and consider use of gastroprotection. Concomitant use of duloxetine and tramadol may predispose to serotonin overactivity and serotonin syndrome. Choose an analgesic other than tramadol Duloxetine may impair thrombocyte function and thus increase the risk of bleeding. Careful monitoring of signs and symptoms of acute and/or chronic bleeding is recommended in concomitant use the risk for bleeding may be increased in concomitant use. Individuals with two non-functional alleles are classified as "poor metabolizers," individuals with one functional allele as "intermediate metabolizers," and individuals with two functional alleles as "extensive metabolizers. Serotonin syndrome A well-established pharmacodynamic drugdrug interaction in the management of neuropathic pain is serotonin syndrome. Symptoms include mental-status changes, autonomic hyperactivity, and neuromuscular abnormalities. Typical first symptoms are agitation, tremor, tachycardia, hypertension, diarrhoea, and sweating. Mild cases of serotonin syndrome resolve within 24 hours after the discontinuation of serotoninergic drugs. Duloxetine has been officially labeled for treatment of painful diabetic polyneuropathy. As both venlafaxine are indicated for treatment of major depressive disorders and generalized anxiety disorders, they should be considered in neuropathic pain patients with these psychiatric comorbidities. Duloxetine is not recommended in patients with prostatic hypertrophy and/or urinary retention, whereas it is a tempting choice for patients with overactive bladder. Venlafaxine at dose 150225 mg/ day was effective for painful polyneuropathy [3032] whereas a dose of 75 mg/day was ineffective [30]. In a head-to-head comparative study of 33 patients, venlafaxine (225 mg/day) was less effective than imipramine (150 mg/day) on the proportion of responders [32]. The efficacy of duloxetine (at dose 60120 mg/ day) has been established by three large-scale trials in painful diabetic polyneuropathy [3436]. In the three studies, the safety of duloxetine was not found to be significantly different between patients with and without historical or comorbid cardiovascular conditions [38]. Mechanisms of action Venlafaxine is a strong serotonin and a weak noradrenaline reuptake inhibitor, but with increasing drug doses noradranaline reuptake inhibition will increase mainly due to increasing concentrations of the metabolite O-desmethylvenlafaxine [23]. It weakly inhibits dopamine reuptake, with no significant affinity for histaminergic, dopaminergic, cholinergic, and adrenergic receptors. Dosing the recommended starting dose for controlledrelease venlafaxine is 75 mg given once daily. Patients not responding to the initial 75 mg/day dose may benefit from dose increases up to a maximum dose of 225 mg/day (or up to 300 mg/day in North America). No specific dose adjustments of venlafaxine are considered necessary based on patient age alone. However, caution should be exercised in treating the elderly (due to the possibility of renal impairment and the potential for changes in neurotransmitter sensitivity and affinity occurring with aging). The lowest effective dose should always be used, and patients should be carefully monitored when an increase in the dose is required. The starting and recommended maintenance dose for duloxetine is 30 and 60 mg daily respectively. Dosages above 60 mg once daily, up to a maximum dose of 120 mg/day administered in evenly divided doses, have been evaluated from a safety perspective in clinical trials. The plasma concentration of duloxetine displays large interindividual variability. Hence, some patients that respond insufficiently to 60 mg may benefit from a higher dose. In patients with inadequate initial response, additional response after this time is unlikely. No dosage adjustment is recommended for elderly patients solely on the basis of age.
Coats disease is generally a progressive process and often leads to complications such as retinal detachment and visual loss erectile dysfunction pills review discount priligy express. In the absence of retinal detachment erectile dysfunction pump for sale priligy 60mg free shipping, conservative therapy such as photocoagulation or cryoablation of aberrant vessels is used erectile dysfunction no xplode purchase priligy 90mg on-line. Toxocara endophthalmitis may occur in the absence of systemic infection and usually presents with unilateral visual loss erectile dysfunction heart disease priligy 30mg lowest price. The inflammatory response often is complicated by vitreous membranes or tractional retinal detachment erectile dysfunction pills that work buy priligy with a visa, which generally leads to blindness when untreated. Acute infection may be treated with systemic corticosteroids and albendazole, whereas lesions associated with vitreous membranes may require a vitrectomy to repair tractional retinal detachments. Congenital toxoplasmosis often manifests with bilateral chorioretinitis, causing symptoms in more than 90% of those affected. Partial volume averaging, vessel tortuosity, or ectesia may also make a portion of the vessel appear denser than the other parts. It should be also kept in mind that the sensitivity of the dense vessel sign is relatively low. In other words, absence of dense artery sign does not exclude vessel occlusion or brain infarct. Similarly, thrombosis of the other intracranial vessels, including the veins and dural sinuses, can be diagnosed on the basis of dense clot present within the vessel. Teaching points the dense basilar artery sign indicates basilar artery thrombosis, basilar artery territory infarcts, and a poor outcome. In the appropriate clinical setting, the specificity of this finding is high although sensitivity is only moderate. Using thinner slices, comparing the density of the vessel in question to that of other vessels of similar size, helps to differentiate intraluminal clot from mimickers such as atherosclerosis, hemoconcentration, and vessel tortuosity. Increased density in the middle cerebral artery by nonenhanced computed tomography: prognostic value in acute cerebral infarction. Endovascular therapy of acute vertebrobasilar occlusion: early treatment onset as the most important factor. Multidetector computed tomography of the head in acute stroke: predictive value of different patterns of the dense artery sign revealed by maximum intensity projection reformations for location and extent of the infarcted area. Early initiation of treatment is the most important factor in achieving improved outcomes in the setting of basilar occlusion [3]. Basilar artery territory infarcts, on the other hand, may lack localizing features and are associated with varying degrees of alteration in consciousness that require a broader clinical differential diagnosis than anterior circulation infarcts. Differential diagnosis Increased attenuation in a vessel can result from increased attenuation of the blood or the vessel wall in addition to intraluminal clot formation. Atherosclerosis results in focally increased attenuation in vessel wall that can mimic thrombus. Decreased gray/white differentiation in the left insular ribbon and putamen (short arrow) is compatible with acute infarct. These scans are frequently misinterpreted, particularly when radiologists are not aware of the clinical circumstances. The underlying pathophysiologic processes leading to differences in pattern are not clearly understood, although essentially all types of global anoxicischemic injury portend a very poor prognosis. Differential diagnosis In the proper clinical setting there is no differential diagnosis. One important clue is the difference in attenuation/signal of the supratentorial brain and cerebellum. Because the supratentorial structures are preferentially affected there is usually a stark difference between cerebellum and brain. Only white matter involvement may be confused with leukoencephalopathies radiologically. Patterns of accentuated grey-white differentiation on diffusion-weighted imaging or the apparent diffusion coefficient maps in comatose survivors after global brain injury. Early detection of global cerebral anoxia: improved accuracy by high-b-value diffusion-weighted imaging with long echo time. Importance Anoxicischemic injury, particularly when it is severe, often results in brain death, which has enormous implications for cessation of life support, family counseling, and organ harvesting. Note the attenuation of the cerebellum, which appears prominent relative to diffusely decreased attenuation of the brain. Postprocessing is relatively more cumbersome, and thresholds vary based on post-processing techniques. Central to the idea of advanced imaging is to obtain a precise measure of the area of ischemic core versus ischemic but still viable tissue that is at risk for infarction in the absence of early recanalization (penumbra). It can be argued that patients can only benefit from recanalization if there is a relatively modest area of already infarcted tissue and significant (ideally >20% of area of core infarction) ischemic tissue that can be potentially salvaged. Ideally, imaging would provide an assessment (or confirmation) of occlusion of a major cerebral artery, a precise measure of the area of irreversible infarction, and assessment of the surrounding perfusion abnormality. Typical clinical scenario Stroke is characterized by a sudden, acute neurologic deficit that is referable to the involved vascular territory. Common presentations include hemiparesis, facial droop, aphasia, and loss of consciousness, although a myriad of possible combinations of neurologic signs and symptoms are possible. Common causes of diffusion abnormalities other than stroke include encephalitis, traumatic lesions, acute demyelination, brain abscess, and highly cellular neoplasms. Moreover, such recanalization is potentially harmful, since it would restore blood flow to an already infarcted area. Additionally, the right-sided sulci are effaced and there is early parenchymal hypoattenuation, in comparison with the normal left side. Traumatic and iatrogenic dissections are predominantly due to blunt/ penetrating injuries, chiropractic manipulation, or catheter angiography. In some cases, however, the lumen many be enlarged due to development of dissecting aneurysm. They argue that in some cases of V3 dissections, the only imaging abnormality is the vertebral artery wall thickening, and the lumen appears normal in caliber. Nearly 10% of vertebral artery dissections extend intracranially, with the potential to form dissecting aneurysms, thereby presenting with subarachnoid hemorrhage. In contrast, atherosclerotic disease has a predilection for the vertebral artery origin. Note that the vertebral origin is spared, differentiating it from atherosclerotic disease. Note the focal narrowing of vertebral artery and an associated small dissecting aneurysm (arrow). Likewise, patients with multiple small infarcts occasionally present late, as they may not have any significant neurologic deficits. The non-specific symptoms they have, such as headache, dizziness, drowsiness, and weakness, may be attributable to other underlying conditions. Imaging description Brain infarcts in the subacute stage demonstrate enhancement and may mimic enhancing tumors or infectious processes. Enhancement of the infarcted brain parenchyma is different than "luxury perfusion," which involves enhancement of the vessels around the infarct in the acute phase. Infarcted tissue enhancement usually starts approximately 45 days after the insult and may increase in the following week [1]. Edema associated with infarcts peaks around the fourth day and starts dissipating afterwards, although some level of swelling of the infarcted tissue is usually present for approximately 2 weeks. Differential diagnosis Most infarcts have specific clinical and radiologic features and therefore require no differential diagnosis. A gyral pattern of enhancement is seen in subacute infarcts, with a greater degree of enhancement of the cortex compared to white matter. Multiple small infarcts in the subacute phase may mimic metastases or other enhancing lesions. The distribution within a vascular territory or in the watershed zones is helpful in differential diagnosis. Short-term follow-up imaging may be very helpful in problem cases, as evolving infarcts show significant changes and often improve over a short interval, in contrast to mass lesions. Importance Enhancing mass-like lesions of the brain usually require extensive work-up that frequently involves invasive procedures which may be harmful. Misdiagnosing an infarct leads not only to unnecessary work-up but also to delay in identifying and treating the underlying cause of the infarct for secondary stroke prevention. Typical clinical scenario Most infarcts, particularly of the anterior circulation, present with acute symptoms that are easily recognized by the patient and healthcare personnel. Infarcts that lack motor or sensory deficits, however, may be relatively asymptomatic or have symptoms that are nonspecific, which may lead to delayed clinical presentations and delayed imaging. This was initially interpreted as possible metastasis but later confirmed to be a subacute infarct. Patients should receive a prompt work-up and timely intervention to prevent the secondary mortality from aneurysm rebleeding. Imaging description Acute hemorrhage in the subarachnoid space appears as areas of hyperdensity in the basal cisterns, cerebral sulci, and/or the ventricles. There are several imaging findings that can help locate the site of a ruptured aneurysm. The distribution of blood in the subarachnoid space and thickness of a localized clot can often help with such localization. Additionally, the presence of a parenchymal hematoma is one of the most significant predictors for evaluating the location of the ruptured aneurysm. Preoperative knowledge of these aneurysm characteristics significantly aids in therapeutic decisions. The advantages include its very high spatial resolution and its ability to demonstrate small vessels and their relationship with the neck of the aneurysm, as well as yielding information for planning endovascular repair. However, it is not uniformly available and has an associated risk of ischemic complications due to its invasive nature. Typical clinical scenario Most patients experience a sudden, worst headache of their life. However, higher-grade patients may experience altered level of consciousness or focal neurological deficits, or become comatose. A location centered around the anterior aspect of the midbrain, absence of large amounts of intraventricular blood, and potential extension to the posterior interhemispheric fissure are characteristic imaging features of this condition. There is lack of parenchymal hematoma and a 4-vessel angiogram is negative for aneurysm. The infundibulum is typically conical in shape, measures 3mm or smaller, and has a vessel that arises from its apex. Also, venous contamination may result in false positive diagnosis of aneurysm when venous structures abut the arterial bifurcation. Noninvasive imaging techniques in the diagnosis and management of aneurysmal subarachnoid hemorrhage. These include patients with polycystic kidney disease, Marfan syndrome, coarctation of the aorta, fibromuscular dysplasia, family history of intracranial aneurysms, and EhlersDanlos syndrome. These patients should receive screening with a highly sensitive and specific technique. Imaging description Intracranial saccular (berry) aneurysms are common intracranial vascular lesions with an estimated prevalence in the general population ranging from 2% to 6% [1]. The sensitivity and specificity are reported to be as high as 90%, but depend on the size of the aneurysm. The advantages include its non-invasive nature, the lack of radiation exposure, and the high sensitivity. The characteristic features of infundibula that separate these from aneurysms are their conical shape, diameter less than 3mm, and a vessel arising from the apex. Detection of intracranial aneurysms with 64 channel multidetector row computed tomography: comparison with digital subtraction angiography. Importance Rupture of intracranial aneurysm results in subarachnoid hemorrhage, a condition with significant morbidity and mortality. Therefore, the screening techniques used for detection of unruptured aneurysms should have very high sensitivity as well as specificity to be useful. Typical clinical scenario There is no evidence to support screening the general population for intracranial aneurysms. Imaging description Giant intracranial aneurysms present unique challenges in diagnosis, characterization, and management. By definition, aneurysms that exceed 25mm in greatest diameter are termed giant aneurysms. Giant aneurysms are appreciated as round or oval masses that are slightly hyperdense compared to the gray matter. Calcification is a frequent occurrence and can be seen either in the periphery in an "egg shell" fashion or scattered within the thrombosed portion of the lumen. Administration of contrast allows the identification of the patent lumen of the aneurysm. However, as a sole imaging study, it is insufficient in precise characterization of these complex aneurysms. Because it only demonstrates the patent lumen, it may sometimes grossly underestimate the size or the extent of the aneurysm. Partially thrombosed giant aneurysms appear as extra-axial masses that consist of areas of mixed signal intensities representing clot of varying ages [1]. Giant aneurysms may also result in ischemic symptoms, due to embolic phenomenon occurring from intraluminal thrombus that these lesions frequently harbor. Differential diagnosis Differential considerations include other intracranial masses. Clues to the correct recognition include demonstrating the continuity of the mass with the carotid artery, identification of a flow void, and pulsatility artifacts. Hemorrhagic primary neoplasms and large cavernous malformations can simulate giant aneurysm on account of blood products of varying ages. However, these lesions are intraaxial, whereas giant aneurysms are located in the subarachnoid space. The aneurysm has variegated thrombus that is better seen on T1-weighted image and a smaller, patent lumen seen as a flow void (thin arrow).
Generic priligy 60 mg with amex. Dr. Bar-Chama: Understanding Erectile Dysfunction - What You Need to Know.
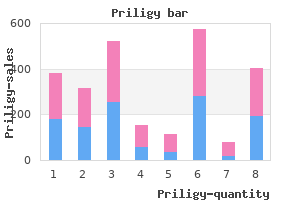
Hemorrhages due to anticoagulation are usually large erectile dysfunction blood pressure medications side effects buy discount priligy line, lobar hemorrhages erectile dysfunction questions priligy 30 mg purchase online, and hypertensive hemorrhages typically are located in the deep gray nuclei impotence natural treatments order 60mg priligy, brainstem erectile dysfunction drugs patents priligy 30 mg buy with amex, and cerebellum impotence hypertension medication order priligy without a prescription. Amyloid angiopathy is characterized by a lobar hemorrhage with associated gray/white matter junction microhemorrhages and/or leptomeningeal hemosiderosis on susceptibility-weighted sequences. Neoplasms that produce intraparenchymal hemorrhage include high-grade gliomas and metastatic tumors, such as melanoma and renal cell carcinoma. Cavernous malformations may be the cause of acute intraparenchymal hemorrhage in young children and young adults. They typically have a heterogenous "popcorn" appearance with a complete hemosiderin rim on T2-weighted images and no surrounding edema. Clues to the etiology are age and associated classic cavernous malformations in other brain locations (particularly in the familial form). Intraparenchymal calcifications are nonspecific and can be seen in a variety of etiologies, including normal deposition in the basal ganglia, prior cerebral insult. Primary intraaxial central nervous system neoplasms that show calcifications include astrocytomas, oligodendrogliomas, or, rarely, glioblastomas. Low-grade oligodendrogliomas are slowly growing neoplasms typically located in a cortical/subcortical location, most commonly in the frontal lobe. Differentiation from other neoplasms is not definitively possible with imaging alone. Lymphoma is characteristically located in the deep white matter and deep gray nuclei. Lymphoma typically demonstrates avid homogenous enhancement in immunocompetent patients. In immunocompromised patients, lymphomas may demonstrate rim enhancement with nonenhancing regions of central necrosis. These lesions usually show dense, homogeneous enhancement and restricted diffusion and do not have susceptibility. Calcifications have little to no blooming on susceptibility-weighted images, in contrast with hemorrhage, which has marked blooming. The findings are consistent with a late subacute hem orrhage in a patient with a known history of amyloid angiopathy. The postcontrast T1weighted image demonstrates an avidly enhanc ing mass consistent with a pathologically proven hemorrhagic renal cell carcinoma metastasis. There are fat fluid levels in the frontal horns of the lateral ventricles with chemical shift arti fact on the T2weighted images as well as multiple small T1 hyperintense foci consistent with fat within the bilateral sylvian fissures. The location and imaging characteristics of this lesion are consistent with a proteinaceous colloid cyst. These findings are consistent with melanocytic deposits in a patient with neurocutaneous melanosis. Subacute phase methemoglobin (both intracellular and extracellular) has intrinsic T1 hyperintense signal. Intracellular meth emoglobin also demonstrates blooming on susceptibilityweighted sequences. A history of recent trauma or anticoagulation makes the diagnosis of T1 hyperintense intracranial hemorrhage straightforward. Patients with a history of hypertension may have deep gray nuclei and brainstem or cerebellar T1 hyper intense subacute hemorrhages. Lobar T1 hyperintense lesions with associated gray/ white matter junction foci of susceptibility suggest amyloid angiopathy in older patients. Furthermore, in the appropriate clinical set ting, intraparenchymal T1 hyperintense lesions should raise the concern for meta static disease. Intrinsic T1 hyperintensity associated with metastatic melanoma may be due to either hemorrhagic components or intrinsic T1 shortening from melanin. In many cases, an underlying mass can be identified on contrastenhanced sequences. If an underlying mass is not identified, it is important to obtain followup imaging to rule out an underlying enhancing lesion initially obscured by the hemorrhage. In younger patients, T1 hyperintense hemorrhages may result from underlying vascular lesions such as cavernous malformations (a "popcorn" appearance with complete hemosiderin rim on gradient echo and T2weighted sequences) or arteriovenous malformations. Melanincontaining lesions, such as neuro cutaneous melanosis, also should be con sidered in the differential diagnosis of T1 shortening when the clinical setting is appro priate. Its intracranial imaging characteristics are due to the proliferation of melanocytes in the leptomeninges or paren chyma. Because symp toms usually manifest by 2 to 3 years of age, a pediatric patient with cutaneous lesions and these imaging characteristics should sug gest this diagnosis despite its rarity. Fatcontaining lesions, such as lipomas or dermoid cysts, also should be considered in the differential diagnosis of T1 shortening. Dermoid cysts often are midline in sellar/ parasellar, frontal, and posterior fossa loca tions and are believed to be due to inclusion of surface ectoderm early during embryo genesis. Dermoid cyst rupture can present with disseminated foci of intracra nial T1 hyperintensity due to spillage of lipid contents into the subarachnoid space or intra ventricular compartment. Because of density differences, lipid droplets or fat fluid levels are antidependent. Dermoid rupture can cause chemical meningitis due to meningeal irritation from the internal contents, which can result in leptomeningeal enhancement. Proteincontaining lesions also should be considered in the differential diagnosis of T1 hyperintense lesions. The location of a proteincontaining lesion is the most impor tant clue to diagnosis. For instance, colloid cysts, which arise from the inferior aspect of the septum pellucidum, typically are pres ent in the region of the foramen of Monro. These lesions are wellcircumscribed, nonen hancing cystic lesions that are hyperintense on T1weighted images when the protein/ mucin content is relatively high. Axial T1 precontrast image (A) demonstrates a T1 hyperintense lesion centered in the left caudate nucleus. Susceptibility blooming is not associated with the intrinsically T1 hyperintense lesion; the signal characteristics could be secondary to extracellular methemoglobin or melanin. The imaging characteristics of metastatic melanoma may vary from patient to patient depending on whether the lesions represent melanotic melanoma metastasis, amelanotic melanoma metastasis, or hemorrhagic metastasis. The imaging interpreter should closely compare T1 precontrast and T1 postcontrast sequences to avoid this pit fall. Stendel R, et al: Ruptured intracranial dermoid cysts, Surg Neurol 57(6):391398, 2002. There also are periventricular T2 hyperintensity and bilateral deep gray nuclei lacunes. There is restricted diffusion in the genu and splenium of the corpus callosum as well as the right corona radiata. Typically, chronic microbleeds are associated with hypertension, amyloid angiopathy, and other causes of small vessel vasculopathy. Microhemorrhages resulting from chronic hypertension typically are located in the deep gray nuclei, deep white matter, brainstem, and cerebellum. Approximately 56% of patients with an acute hypertensive hemorrhage have associated microbleeds. Microhemorrhages resulting from amyloid angiopathy typically occur in patients older than 60 years, in a cortical/subcortical distribution with sparing of the deep white matter, basal ganglia, brainstem, and cerebellum. Approximately 75% of patients with a lobar hemorrhage resulting from amyloid angiopathy have associated microbleeds at gray/ white matter junctions. Patients with the rarer inflammatory form of amyloid angiopathy have associated vasogenic edema and leptomeningeal enhancement. The diagnosis of hemorrhagic metastases should be considered when additional enhancing lesions with susceptibility and surrounding edema are seen. The most common hemorrhagic cerebral metastases are melanoma and renal cell carcinoma. Breast carcinoma and lung carcinoma hemorrhage less frequently but are the most common cerebral metastases and should be considered. Thyroid carcinoma and choriocarcinoma also produce hemorrhagic lesions, but they rarely metastasize to the brain. Lobar or deep acute hemorrhage in young patients with additional foci of susceptibility can suggest the diagnosis of multiple cavernous malformations, especially if there is a classic heterogeneous lesion with a complete hemosiderin ring and no surrounding edema. In patients with a family history of this condition, an autosomal dominant inheritance pattern is seen. It is noteworthy that these familial lesions are not associated with developmental venous malformations. Microhemorrhage associated with diffuse axonal injury is most often seen at gray/white matter junctions and in the corpus callosum, subcortical and deep white matter, and dorsolateral brainstem. In addition to punctate foci of susceptibility, diffusion restriction may be seen at sites of diffuse axonal injury. Lastly, any cause of vasculitis, whether infectious or inflammatory, should be considered. In particular, septic emboli, fungal infections, and radiation and chemotherapy changes should be considered in the appropriate clinical setting. In addition, causes of small vessel vasculopathy, such as sickle cell disease or cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy, should be considered. Patients with amyloid angiopathy and numerous microhemorrhages may present with dementia. Of note, the ring of peripheral enhancement is slightly thicker toward its cortical margin. Despite the size of this lesion, a paucity of surrounding edema and mass effect is noted. There is restricted diffusion in the periphery of the lesion but not in the center. Of note, there is an enhancing internal septation as well as irregularity, nodularity, and varying thickness of the enhancing wall. Subtle ependymal enhancement is noted along the walls of the temporal horn of the right lateral ventricle. There is mildly restricted diffusion in the rim of the lesion but not in the center. There is minimal surrounding linear enhancement along perivascular spaces as well as overlying dural enhancement. The degree of perilesional edema A solitary ring-enhancing lesion is usually due to a neoplastic process, infection, or demyelination. In decreasing order of frequency, solitary ring-enhancing lesions represent gliomas, metastases, abscesses, or demyelinating lesions. Multiplicity, on the other hand, in decreasing order of frequency, suggests metastases, pyogenic abscesses, demyelinating lesions, or opportunistic infections. In an adult patient, a heterogeneous lesion with a thick, irregular, and nodular rim of enhancement suggests a necrotic neoplastic lesion, such as glioblastoma multiforme or metastasis. An abscess often presents with specific clues to the diagnosis, including homogeneous central restricted diffusion, an often T2 hypointense peripherally enhancing rim, considerable surrounding edema, and a thicker wall toward the cortex/periphery. Because abscesses tend to grow away from the wellvascularized gray matter, thinning of the medial wall is seen. Hematogenous abscesses (in the setting of endocarditis, cardiac shunts, and pulmonary arteriovenous malformations) Ring-Enhancing Lesions 25 are usually multiple and present at gray/ white matter junctions. Nevertheless, because of the higher incidence of neoplasms and infection, these entities still remain considerations with this pattern of enhancement. Further support for this diagnosis comes in the form of multiple white matter lesions seen in a typical distribution, such as at the callosal-septal interface, and oriented perpendicularly to the ventricular surface. Masses are commonly hyperdense to isodense on computed tomography and demonstrate dense homogeneous enhancement. Although avid homogenous enhancement is usually seen in immunocompetent patients, imaging tends to be more variable in immunocompromised patients, and lesions may be heterogeneously enhancing or ring enhancing. Importantly, linear enhancement at the margins of the lesion tracking along Virchow-Robin perivascular spaces is highly specific. In immunocompetent patients, intracranial lesions are solitary 70% of the time, whereas in immunocompromised patients, lesions are equally likely to be multiple versus solitary. Approximately 85% of lesions are supratentorial, with more than 60% of intracranial lesions occuring in a periventricular location and 12% of lesions involving the corpus callosum. Trans-spatial lesions typically have intraparenchymal enhancement with adjacent dural enhancement. There is associated cortical atrophy, ipsilateral choroid plexus hypertrophy, and a prominent medullary vein. The easiest is determined first by attempting to differentiate infectious from noninfectious entities, a prospect often aided by a suggestive clinical history or imaging findings suggesting the source of infection. Uncomplicated bacterial meningitis typically demonstrates thin, smooth leptomeningeal enhancement. Entities classically presenting with thick, nodular, basal predominant enhancement include tuberculous meningitis, fungal meningitis, neurosarcoidosis, pyogenic meningitis, and neurosyphilis. Entities with more diffuse nodular leptomeningeal enhancement include meningeal carcinomatosis, lymphomatous meningitis, and leukemia. Very thick, smooth, basilar leptomeningeal enhancement can suggest the unlikely diagnosis of leptomeningeal gliomatosis in the setting of a chronic aseptic meningitis pattern of presentation. Infectious meningitis results in leptomeningeal enhancement because of the breakdown of the blood-brain barrier. Tuberculous and fungal forms of meningitis are often basilar predominant and confluent. In addition, fungal and tuberculous meningitis may produce thicker nodular enhancement in contrast to the typical bacterial meningitis enhancement pattern. Less common etiologies include vasculitis, gliomatosis, Sturge-Weber syndrome, and moyamoya disease.
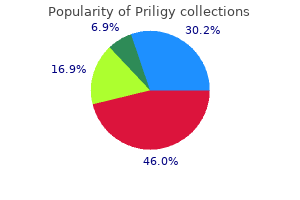
Bradycardia can be prevented or reversed by administration of an anticholinergic agent such as atropine impotence quit smoking order priligy 90 mg with visa. Activation of alpha2-adrenergic receptors produces very different responses than alpha1 activation erectile dysfunction drugs without side effects priligy 90mg purchase free shipping. The most important responses to alpha2-receptor agonists occur in the brain rather than the peripheral nervous system erectile dysfunction icd 0 buy cheap priligy. Methyldopa (Aldomet) and clonidine (Catapres zinc causes erectile dysfunction 30 mg priligy purchase overnight delivery, Duraclon) are two drugs in this class erectile dysfunction doctor dc priligy 30 mg buy on-line. Its most frequent indication is for the relief of congestion associated with the common cold and allergies. One advantage of phenylephrine, however, is that it cannot be used by illicit drug dealers to synthesize methamphetamine. Formulations containing phenylephrine are exempt from regulations in most states that require pseudoephedrine products to be kept behind the pharmacy counter. When applied intranasally by spray or drops, it reduces nasal congestion by constricting small blood vessels in the nasal mucosa. Parenteral administration of phenylephrine can prevent or reverse acute hypotension caused by spinal anesthesia or vascular shock. Unlike epinephrine, which markedly increases the heart rate, phenylephrine tends to slow the heart rate probably due to reflex bradycardia. In situations in which reflex bradycardia is undesirable, this action may be blocked by the administration of atropine. Applied topically to the eye during ophthalmic examinations, phenylephrine can dilate the pupil, without causing significant cycloplegia. Applied to swollen hemorrhoidal tissue, the drug can relieve itching and burning associated with hemorrhoids. Mechanism of Action: Phenylephrine directly activates alpha1adrenergic receptors in the peripheral nervous system. It has weak beta-adrenergic activity at high doses, but this is usually not of clinical significance. Serious adverse effects include reflex bradycardia and reduced blood flow to peripheral tissues due to severe vasoconstriction. The use of phenylephrine nasal and ophthalmic solutions is not recommended in infants or children except under the care of a health care provider. Because it causes reflex bradycardia, patients with preexisting bradycardia should not receive phenylephrine. Phenylephrine causes vasoconstriction, which can reduce coronary blood flow in patients with advanced coronary artery disease, causing angina attacks. Phenylephrine also reduces the effectiveness of nitrates such as nitroglycerin that are taken to prevent anginal episodes. Because of its effects on the eye, it should not be administered to patients with narrow-angle glaucoma. Phenylephrine should be used with caution in patients with hyperthyroidism or diabetes because these patients are more sensitive to the potential cardiac adverse effects. Drug Interactions: Phenylephrine will reduce the effectiveness of antihypertensive medications. Increased effects of phenylephrine may occur in patients taking ergot alkaloids and tricyclic antidepressants. Additive effects may occur if phenylephrine is given concurrently with other adrenergic agonists, including amphetamines or cocaine. Phentolamine is a specific alpha antagonist that can be used to lower blood pressure, and antidysrhythmic agents may be indicated. Nursing Responsibilities: Key nursing implications for patients receiving phenylephrine are included in the Nursing Practice Application for Patients Receiving Adrenergic Agonist Therapy on pages 244245. Patient and Family Education: Do not give the drug to infants and children unless directed by a health care provider because children are especially sensitive to the effects of phenylephrine. Drugs Similar to Phenylephrine (Neo-Synephrine) Most agents with predominant alpha-adrenergic agonist activity can be grouped into subclasses based on their indications: intranasal or ocular decongestants. Another drug in this class, methoxamine (Vasoxyl), is no longer available in the United States. If the drug is abruptly discontinued, congestion may worsen, a phenomenon known as rebound congestion. Although these drugs may also have some beta-adrenergic activity, they are only used for their effects on alpha-adrenergic receptors in the nasal mucosa. Pseudoephedrine is an intranasal decongestant that deserves special attention because of its potential for misuse. Most states have enacted laws to regulate the sale of solid tablet formulations containing pseudoephedrine, requiring that pseudoephedrine be placed behind the pharmacy counter so that only pharmacists can provide the product. Most states also require the pharmacist to record the name and address of the buyer. Ocular decongestants: Naphazoline (Naphcon, Clear Eyes), oxymetazoline (Afrin 12 hour), and tetrahydrozoline (Visine) are available as ophthalmic solutions to relieve redness due to minor eye irritations, such as those caused by the common cold, swimming, allergies, or contact lenses. Midodrine (ProAmatine): Approved in 1996, midodrine is converted into an active metabolite that has alpha1-agonist actions. The drug increases standing, sitting, and supine systolic and diastolic blood pressure. Because marked elevation of supine blood pressure occurs in as many as 13% of the patients taking the drug, it carries a Black Box Warning that supine and sitting blood pressures should be monitored during therapy and that it should not be used in patients with an initial supine systolic pressure greater than 180 mmHg. The most common adverse effects are paresthesia, goosebumps, dysuria, and pruritus of the scalp. Drugs used for their beta1-agonist actions are sometimes called cardiotonic drugs because they increase the force of contraction of the heart. In the treatment of heart failure or shock, they are administered to increase cardiac output. Another name applied to these drugs is inotropic agents, because they reverse the cardiac symptoms of shock by increasing the strength of myocardial contraction. Most drugs used for their strong beta1-agonist activity are nonselective and activate other receptor subtypes. For example, although epinephrine is often used for its beta1 activation of the heart following cardiac arrest, the drug has effects on all receptor subtypes. Dopamine is somewhat unique in that at low doses the drug activates dopamine receptors, and at moderate doses it stimulates both beta1 and dopamine receptors. At high doses dopamine activates all three receptor types: dopamine, alpha, and beta1. Dobutamine is selective for beta1 receptors and isoproterenol activates both beta1 and beta2 receptors. Beta2-adrenergic agonists: Beta2-adrenergic receptors are more widely distributed than beta1 receptors. Pharmacologically, the most important site is in the lung, where activation of beta2 receptors leads to relaxation of bronchial smooth muscle. Beta2adrenergic agonists, commonly referred to as bronchodilators, are used extensively in the treatment of asthma and other pulmonary disorders. The following discussion is limited to autonomic bronchodilators; information on other classes of drugs used in the pharmacotherapy of asthma is presented in Chapter 47. Autonomic drugs used as bronchodilators include nonselective adrenergic agonists, as well as those that are selective for beta2 receptors. Epinephrine is the best example of a nonselective agent that is an effective bronchodilator. Likewise, isoproterenol is an effective bronchodilator; however, it also affects beta1 receptors, which increases its potential for producing cardiovascular adverse effects. Selective beta2 agonists such as albuterol have become first-line drugs in the pharmacotherapy of asthma and other conditions characterized by bronchospasm. Inhalation administration of these agents relieves acute bronchospasm within minutes. Some of the inhaled beta2 agonists, such as albuterol (Proventil, Ventolin, VoSpire) and pirbuterol (Maxair), have a rapid onset; however, their duration of action is only 3 to 5 hours. Others such as formoterol (Xopenex) have longer onsets of action, but their effects can last up to 12 hours. The agent of choice and dosage schedule are individualized for the particular pattern of asthma exhibited by each patient. From what you learned in Chapter 18, would the administration of an anticholinergic such as atropine improve or worsen this condition Activation of beta-adrenergic receptors can produce a wide variety of physiological responses, depending on the location of the receptor and which subtype is stimulated. Some beta-adrenergic agonists are more selective for beta1 receptors, whereas others affect primarily beta2. Beta1-adrenergic agonists: Pharmacologically, the most significant site having beta1 receptors is cardiac muscle. Activation of beta1 receptors results in cardiac actions typical of the fight-or-flight response: increased heart rate (positive chronotropic effect), force of contraction (positive inotropic effect), and velocity of impulse conduction across the myocardium (positive dromotropic effect). A second therapeutic application of beta2 agonists is for the treatment of preterm labor contractions. Activation of beta2 receptors in the uterus relaxes uterine smooth muscle, leading to a delay in labor. This delay allows for additional maturation of the organ systems of the fetus, which increases the probability of neonatal survival. Drugs used to delay preterm labor are called tocolytics and are discussed in Chapter 72. Adverse effects of the beta2 agonists are predictable extensions of their autonomic activation. Tachycardia, palpitations, flushing, insomnia, and tremor are possible adverse effects with all beta2 agonists. The oral forms have some beta1 activity; thus systemic adverse effects are more common than the inhaled drugs, which act locally and produce few systemic adverse effects. Beta agonists should be used cautiously in patients with dysrhythmias or heart failure. The drug should be used with caution in patients with hyperthyroidism or diabetes because these patients are more sensitive to the potential cardiac adverse effects. Isoproterenol (Isuprel) Classification: Therapeutic: Bronchodilator Pharmacologic: Nonselective beta-adrenergic agonist Drug Interactions: Concurrent administration with a betaadrenergic blocker diminishes the bronchodilation effect of isoproterenol and may induce bronchospasm in patients with asthma. Use with other bronchodilators or adrenergic agonists such as epinephrine or dopamine may result in additive effects. Isoproterenol should not be concurrently administered with potassium-wasting diuretics because hypokalemia may result. Treatment of Overdose: Overdose with isoproterenol will cause tachycardia and other dysrhythmias. Due to the relatively short half-life of the drug, discontinuing the infusion is often enough to reverse symptoms, although supportive cardiac drugs may be necessary. Therapeutic Effects and Uses: Isoproterenol is a catecholamine that has been available as a drug for over 50 years. Isoproterenol activates both beta1- and beta2-adrenergic receptors, but has little effect on alpha receptors. The cardiac actions of isoproterenol are used to advantage in the pharmacotherapy of cardiogenic or bacteremic shock, cardiac arrest, Adams-Stokes syndrome, and certain types of ventricular dysrhythmias. Dobutamine has largely replaced isoproterenol as a cardiac agent, because it is more specific to beta1 receptors in the heart. Isoproterenol was once available by inhaler for asthma pharmacotherapy and was a drug of choice due to its bronchodilation effects caused by activation of beta2 receptors in the airways. The development of selective beta2 agonists with fewer cardiac adverse effects, however, led to a significant decline in the use of isoproterenol as an antiasthmatic agent. Mechanism of Action: Isoproterenol is a potent activator of both beta1- and beta2-adrenergic receptors throughout the body. Nursing Responsibilities: Key nursing implications for patients receiving isoproterenol are included in the Nursing Practice Application for Patients Receiving Adrenergic Agonist Therapy on pages 244245. Lifespan and Diversity Considerations: Assist the older adult to ambulate if blurred vision, light sensitivity, or dizziness occur from drug effects, to prevent falls. Arformoterol (Brovana), formoterol (Foradil, Performist), indacaterol (Arcapta Neohaler) and salmeterol (Serevent) are also given by inhalation, but the long onset of action of these agents makes them unsuitable for relieving acute asthma attacks. The longer acting drugs are used in combination with inhaled corticosteroids in the pharmacotherapy of chronic asthma. When given 15 minutes before exercise, albuterol may be used for the prophylaxis of exercise-induced bronchospasm. Dobutamine (Dobutrex): Dobutamine is a selective beta1adrenergic agonist that has value in the short-term treatment of certain types of shock due to its ability to cause the heart to beat more forcefully. Dobutamine is especially beneficial in cases where the primary cause of shock is related to heart failure, not hypovolemia. In fact, hypovolemia should be corrected before administering adrenergic agonists such as dobutamine. The resulting increase in cardiac output assists in maintaining blood flow to vital organs; renal blood flow is enhanced, and urine output increased. The patient should be monitored continuously during the infusion for abnormal changes in heart rate or rhythm. Tocolytics: Terbutaline and ritodrine are beta2 agonists that relax uterine smooth muscle. From what you learned in Chapter 4, which route of administration- oral, subcutaneous, or inhalation-would likely give the fastest onset of drug action for this patient Assessment throughout administration: Decreased Cardiac Output Impaired Gas Exchange Ineffective Airway Clearance Disturbed Sleep Pattern, related to adverse drug effects Deficient Knowledge (Drug Therapy) Risk for Injury, related to adverse effects of drug therapy or administration Assess for desired therapeutic effects dependent on the reason for the drug. Teach the patient to follow directions on the inhaler or autoinjection epinephrine device and to have on hand for emergency use at all times.
References
- Lindner A, Schalke B, Toyka KV. Outcome in juvenile-onset myasthenia gravis: A retrospective study with long-term follow-up of 79 patients. J Neurol. 1997;244:515-520.
- Gudmundsson J, Sulem P, Manolescu A, et al: Genome-wide association study identifies a second prostate cancer susceptibility variant at 8q24, Nat Genet 39:631n637, 2007.
- Steffens HP, Kurz S, Holtappels R, et al. Preemptive CD8 T-cell immunotherapy of acute cytomegalovirus infection prevents lethal disease, limits the burden of latent viral genomes, and reduces the risk of virus recurrence. J Virol. 1998;72:1797-1804.
- Arce J, Gaya JM, Huquet J, et al: Can we identify those patients who will benefit from prostate-sparing surgery? Predictive factors for invasive prostatic involvement by transitional cell carcinoma, Can J Urol 18(1):5529n5536, 2011.
