
Sildigra
| Contato
Página Inicial
Amy Mackey, MD
- Department of Obstetrics and Gynecology
- Abington Memorial Hospital
- Abington, Pennsylvania
If compliance is unlikely impotence from diabetes 50 mg sildigra buy, as judged by medical erectile dysfunction 45 year old male 25 mg sildigra purchase, psychiatric erectile dysfunction treatment in thailand 100 mg sildigra for sale, psychological erectile dysfunction treatment mayo clinic 25 mg sildigra order overnight delivery, and social work assessment erectile dysfunction treatment fruits sildigra 120 mg order without a prescription, transplantation should not proceed. Patients with psychiatric illnesses including depression, bipolar affective disorder, and psychosis require assessment by a psychiatrist to determine transplant suitability and to devise a management plan to cope with possible consequences of immunosuppressive medications such as corticosteroids. Presence of Multiple Comorbidities Increasingly patients with multiple comorbidities are referred for consideration of transplantation as the boundaries for acceptance onto transplant programs broaden. Alternatively, arrest occurs in hospital and patient is unable to be resuscitated. Alternatively, this occurs during brain death testing and the patient is not or cannot be successfully resuscitated. Category V: Unexpected cardiac arrest in a critically ill patient Example: Unsuccessful resuscitation after unexpected cardiac arrest in intensive care. Controversially, some societies have suggested that patients must have specified long-term survival prospects-for example, an 80% chance of surviving 5 years-to be accepted for transplantation from a deceased donor. In addition, risk calculators have been devised based on registry data to allow such predictions. A targeted reassessment of waiting-list patients therefore should be conducted at regular intervals (Table 102-3). Surgical reassessment may be needed in patients with peripheral vascular disease, if patients gain weight, or if a complication such as peritonitis occurs while the patient awaits transplantation. Patients should be temporarily removed from the waiting list if they develop a serious infection or other illness until it is resolved. Donation after brain death donors can be further divided into standard criteria donors and extended-criteria donors. The definition of extended-criteria donor varies; in the United States it refers to heart-beating donors older than 60 years or 50 to 59 years old with two or three of the following criteria: a history of hypertension; elevated serum creatinine at donation (>1. In some jurisdictions, the term marginal donor is loosely used to describe donors who are less than optimal for some reason-usually the presence of significant underlying disease (hypertension, diabetes, vascular disease, renal impairment) or advanced age (older than 65 years). The Maastricht classification separates these types of donors into controlled and uncontrolled categories (Box 102-3). Uncontrolled donors are those who are deceased on arrival to the hospital or who have a failed cardiopulmonary resuscitation. From a practical point of view, a system that uses controlled donors is easier to implement than one using uncontrolled donors. This is largely related to factors surrounding ethical considerations and the consent process involving relatives of the donor. Evaluation of the Deceased Donor In most circumstances, organ donor coordinators screen potential deceased donors after referral from hospital intensive care units or emergency departments. The assessment focuses on general health (including history of infections and cancer), social history (especially drug use and sexual history), and laboratory evidence of renal impairment or other diseases (Box 102-4). In some patients a biopsy (often performed at retrieval) may provide useful information, particularly with extended-criteria donors. Donors younger than 5 or 6 years are generally associated with high risk of failure, especially from vascular thrombosis. The use of pressor agents, volume resuscitation, and other conditioning strategies is complex and has been the subject of several guideline documents (see the Intensive Care Society website, In this category of donor, the kidneys are generally not subject to significant warm ischemia at the time of organ retrieval unless the donor suffers prolonged hemodynamic compromise. Surgical retrieval can then take place after a period of delay to variably allow one or more of the following: family counseling, donor assessment, or relocation from one hospital area to another. This is responsible for the higher rate of delayed graft function that is seen in this group. The need for dialysis support after transplantation is approximately 50% but varies from 30% to 90%, depending on the Maastricht category of donor. Living donors may be related, unrelated, altruistic, or part of a donor exchange or list-exchange program. In many countries with well-established transplant programs, half or more of all transplants are now performed with living donors. In Japan, Brazil, and the Middle East, more than 80% of transplants use living donors. The superior outcomes of transplantation from living donors compared with that from deceased donors has supported the development of living donor paired exchange and living donordeceased donor exchange. Registry data and institutional surveys suggest the perioperative risk of donor death is approximately 3 in 10,000. In open surgery, the risks are related to perioperative complications, including pulmonary emboli, pneumonia, and ischemic events. With laparoscopic surgery, complications are largely a result of catastrophic intraoperative events or postoperative bleeding related to securing of the vascular pedicle. Numerous series report early operative complications after laparoscopic and open donor nephrectomy with rates of 3% to 38%. This enormous variability relates to both definition of complication and accuracy of reporting. Case series report that physical and psychological function in living donors is higher than the community norm. Physical issues reported by donors after donation frequently include a temporary decrease from baseline in energy; some note a longer time to full recovery than anticipated and incision pain (after open nephrectomy) that lasts longer than expected. Longerterm psychological morbidity appears minimal; however, some series have reported an association with anxiety, depression, or other psychological issues in a small proportion of the patients. Psychological evaluation before donation is therefore extremely important, as is the need to provide support and counseling after donation. This issue is particularly important when the transplant does not go as well as anticipated. Several groups have developed guidelines for the evaluation of the living donor, including the Amsterdam forum47 and consensus guidelines published by several U. The survival of living related donors is similar to the expected survival derived from the general population. Error bars at 5-year intervals indicate 95% confidence intervals for the probability of survival among kidney donors. Borderline elevated levels should be further evaluated with ambulatory blood pressure monitoring. If elevated blood pressure is detected and the prospective donor is still under consideration, echocardiography (looking for left ventricular hypertrophy), ophthalmologic evaluation (looking for hypertensive retinal changes), and assessment for microalbuminuria (suggesting hypertensive renal damage) should be undertaken. Guidelines typically exclude from donation those with urine protein higher than 300 mg/24 h (with or without hypertension). It is our view that the presence of microalbuminuria (with or without hypertension) should also lead to exclusion, given the likely underlying renal and systemic microvascular pathology this signifies, particularly in those with other cardiovascular risk factors. Hypertension and Proteinuria in the Living Donor assessment of the kidneys and vessels. An assessment of the anatomy may be achieved by computed tomographic angiography or magnetic resonance angiography, depending on the particular center. Formal renal arteriography, although informative, is no longer necessary, given the anatomic detail obtainable noninvasively with modern radiologic techniques. It is accepted that this is an overgeneralization, potentially representing too low a limit for the younger donor. This method has been recommended by the British Transplantation Society (guidelines available at These include the impact of obesity on perioperative complications, future renal function, and cardiovascular health. In addition to close assessment of those who are overweight, prospective donors with an abnormal fasting glucose concentration, a history of gestational diabetes, or a first-degree relative with diabetes should be evaluated with an oral glucose tolerance test. Patients often lose weight and otherwise change their lifestyle (exercise, diet), leading to an improvement in their results and eventual acceptance as donors. It is important that these lifestyle and risk modifications be sustained after donation occurs. Isolated hematuria in a prospective donor necessitates consideration of thin basement membrane nephropathy, Alport syndrome (carrier status in women may cause minor or moderate abnormalities), and IgA nephropathy as well as urinary tract infection, malignant disease, and nephrolithiasis. Microhematuria is a relatively common problem, with persistent microhematuria evident in approximately 3% of the general population. If persistent isolated asymptomatic microhematuria is detected during living donor evaluation, a workup should include cystoscopy and urinary cytology if the hematuria is not clearly glomerular in origin. A renal biopsy should be considered when there is glomerular hematuria or the possibility of familial disease. An asymptomatic potential donor with a current single stone is suitable if the donor does not have a high risk of recurrence, if the stone is smaller than 1. Atherosclerotic renal vascular disease is a relative contraindication to living donation. If it is discovered, the donor should be normotensive, have normal renal function, and have only unilateral disease. The age of the prospective donor should also be considered, with the outcome in donors older than 50 years more predictable and benign than in younger donors. These include melanoma, testicular cancer, renal cell carcinoma, bronchial and breast cancer, choriocarcinoma, hematologic malignant neoplasm, and multiple myeloma. A history of malignant disease may be acceptable if the specific cancer is curable and transmission of the cancer can reasonably be excluded; consultation with an oncologist may be required. Examples of cancers considered to have low risk for transmission include early prostatic and early low-grade bladder and cervical malignancies. Consent to receive a renal transplant must include a discussion with the donor and the recipient regarding the fact that risk of transmission of malignant disease cannot be completely excluded. Malignant Disease Renal Abnormalities in the Living Donor Cardiovascular and Pulmonary Disease In prospective donors, the cardiac assessment should be based on the history, risk factors, examination, and electrocardiographic findings. An exercise or pharmacologic stress test and echocardiography may be warranted in certain circumstances. Individuals with myocardial dysfunction or coronary ischemia are at increased anesthetic risk and should generally not donate. Pulmonary contraindications to donation include chronic lung diseases that significantly increase the anesthetic risk. If indicated by history and examination, pulmonary function testing, echocardiography, or sleep studies should be performed. In all cases, donors should cease smoking for at least 8 to 12 weeks before surgery to minimize the risk of postoperative pneumonia. This involves removal of blood group antibodies by plasma exchange or immunoadsorption to achieve target titers. With use of this protocol, patient and graft survival appears to be equivalent to that of blood groupcompatible transplantation for the short to medium term (up to 9 years). In this example, the A3 antigen is the only antigen present in the two lysed cell populations and absent from the nonlysed samples. Prior treatment of sera with dithiothreitol can remove IgM antibodies and aid in the interpretation of the test (Table 102-4). Autoantibodies (such as may occur in lupus) may also give falsepositive results and can be determined by prior absorption with autologous lymphocytes. Crossmatching of donor lymphocytes with recipient serum allows screening for this possibility. The sensitivity of the assay can be augmented by the addition of antihuman globulin. Binding of antibody from donor serum is detected by flow cytometry after probing with a fluorescein-labeled anti-immunoglobulin antibody. In most centers, it is not routinely performed before deceased donor transplants, but it is commonly performed in a living donor transplant workup. Graft persistence effectively induces and maintains donor-specific unresponsiveness. Predicting potential survival benefit of renal transplantation in patients with chronic kidney disease. Follow-up after renal transplantation with organs from donors after cardiac death. Risk factors for vascular thrombosis in pediatric renal transplantation: A special report of the North American Pediatric Renal Transplant Cooperative Study. Utilizing list exchange and nondirected donation through "chain" paired kidney donations. Living-donor kidney transplantation: A review of the current practices for the live donor. Morbidity and mortality after living kidney donation, 1999-2001: Survey of United States transplant centers. A Report of the Amsterdam Forum on the Care of the Live Kidney Donor: Data and medical guidelines. Influence of obesity on the appearance of proteinuria and renal insufficiency after unilateral nephrectomy. The decision on whether to proceed with transplantation in the context of this information is complex. Recommendations for detection and characterization of clinically relevant antibodies in solid organ transplantation are summarized by the British Society of Histocompatibility and British Transplantation Society and are available at A more recent set of guidelines was also published after a Consensus Conference on Antibodies in Transplantation, held in 2012. Practice variations in the evaluation of adult candidates for cadaveric kidney transplantation: A survey of the European Transplant Centers. Canadian Society of Transplantation: Consensus guidelines on eligibility for kidney transplantation. Risk-stratified screening for ischemic heart disease in kidney transplant candidates. Prognostic value of myocardial perfusion studies in patients with end-stage renal disease assessed for kidney or kidney-pancreas transplantation: A meta-analysis. Stroke in renal transplant recipients: Epidemiology, predictive risk factors and outcome. Peripheral arterial disease as a predictor of outcome after renal transplantation. Identifying high risk groups and quantifying absolute risk of cancer after kidney transplantation: A cohort study of 15,183 recipients.
In addition erectile dysfunction los angeles generic 100 mg sildigra fast delivery, short and more frequent dialysis treatments are recommended with use of small surface area dialyzers and reduced blood flow rates treatment of erectile dysfunction in unani medicine purchase sildigra 50 mg visa. An extension of this syndrome may be one that mimics osmotic demyelination syndrome-similar to that seen with rapid correction of hyponatremia zma impotence purchase sildigra cheap online. Several cases have been reported in association with dialysis initiation do erectile dysfunction pills work generic sildigra 120 mg online, with clinical manifestations similar to the locked-in pontine picture of central demyelination erectile dysfunction treatment costs purchase sildigra online from canada. The difference is that with the dialysis-related condition, the patients appear to recover over the ensuing 5 to 7 days and the condition seems to be related to edema rather than demyelination. The typical complaint is of crawling sensations in the legs that occur with inactivity, and symptoms may worsen during dialysis. The etiology, prevention, and management of restless legs syndrome are discussed in Chapter 86. Intradialytic seizures occur in less than 10% of patients and tend to be generalized but easily controlled. However, focal or refractory seizures warrant evaluation for focal neurologic disease, particularly intracranial hemorrhage. Treatment of established seizures requires cessation of dialysis, maintenance of airway patency, and investigation for metabolic abnormalities. Intravenous 50% dextrose in water should be administered promptly if hypoglycemia is suspected. It is usually aggravated by the supine position, but there are no visual disturbances. Preventive measures include slow dialysis with reduced blood flow rates, change to bicarbonate dialysate, sodium and ultrafiltration modeling, coffee ingestion during dialysis, and use of reprocessed dialyzers. Attention should also be paid to adequate flushing of the lines and dialyzer before commencement of dialysis. Changing the dialysis membrane, especially to a synthetic membrane or an alternative synthetic membrane, sometimes is useful in patients with refractory cases. Complement activation and neutropenia have also been detected with other more widely used dialyzer membranes, including cellulose acetate and polysulfone, but to a lesser degree. Although the long-term clinical relevance of this phenomenon remains speculative, its contribution to acute intradialytic morbidity is discussed later. Acute hemolysis can be caused by faulty dialysis equipment, chemicals, drugs, toxins, or patient-related factors. Furthermore, during dialyzer reprocessing, formaldehyde retention can result in hemolysis by inducing formation of cold agglutinins or inhibiting red cell metabolism. The diagnosis of acute hemolysis is evident when grossly translucent hemolyzed blood is observed in the tubing. Patients with methemoglobinemia have nausea, vomiting, hypotension, and cyanosis, and oxygen therapy does not improve the black blood present in the extracorporeal circuit. Copper contamination should be suspected in the presence of skin flushing and abdominal pain or diarrhea. Evaluation should include reticulocyte count, haptoglobin, lactate dehydrogenase, blood smear, Coombs test, and measurement of methemoglobin. Chromium 51 (51Cr)labeled red blood cell survival and bone marrow examination may occasionally be indicated if there is recurrent hemolysis. More important, analysis of tap water for chloramines and metal contaminants and thorough analysis of the dialysis equipment for clues of increased blood turbulence are recommended. Intradialytic Hemolysis Bleeding complications are commonly related to the use of intradialytic anticoagulation, which further confounds the uremic bleeding diathesis (see Chapter 84). Despite its limitations, the bleeding time remains the best indicator of hemorrhagic tendency. In addition to specific measures directed to the site of hemorrhage, reversal of uremic platelet dysfunction is imperative. Strategies include the use of erythropoiesis-stimulating agents or red blood cell transfusions to achieve a hematocrit above 30% to improve rheologic plateletvessel wall interactions, intravenous conjugated estrogens at 0. For patients experiencing severe bleeding, it is advisable to consider heparin-free dialysis with use of normal saline flushes every 15 to 30 minutes with ultrafiltration adjustments. Other alternatives may include regional heparin or citrate anticoagulation, and in the long term the use of low-molecularweight heparin, heparin modeling, or prostacyclin may be considered. Tranexamic acid, a potent fibrinolytic inhibitor, has occasionally been used as an adjuvant treatment to control hemorrhage in dialysis patients. This decrease is usually of no clinical significance to patients unless there is preexisting chronic cardiopulmonary disease. Hypoventilation is the main implicated factor and is primarily central in origin as a result of a decrease in carbon dioxide production after acetate metabolism (specific to acetate dialysate), loss of carbon dioxide in the dialyzer (with both acetate and bicarbonate dialysate), and rapid alkalinization of body fluids (particularly with large surface area dialyzers). Furthermore, a commonly observed ventilationperfusion mismatch may be caused by pulmonary leukocyte agglutination (in part resulting from complement activation) or impaired cardiac output (resulting from acetate-induced myocardial depression). In high-risk patients with fluid overload, preventive measures consist of using intradialytic oxygen supplementation, conventional bicarbonate dialysate, and biocompatible membranes. However, other sources need to be considered, including intravenous infusion circuits especially with glass bottles, air bubbles from the dialysate, and (especially uncuffed) Thrombocytopenia An increasingly important cause of thrombocytopenia in dialysis patients is heparin-induced thrombocytopenia. High blood flow rates may allow rapid entry of large volumes of air despite small leaks. The acute onset of seizures and coma in the absence of precedent symptoms such as chest pain and dyspnea is highly suggestive of air embolism. In the supine position, air introduced through a central venous line will be trapped in the right ventricle, where it forms foam, interferes with cardiac output, and, if it is large enough, leads to obstructive shock. Dissemination of microemboli to the pulmonary vasculature results in dyspnea, dry cough, chest tightness, or respiratory arrest. In the left Trendelenburg position, air emboli migrate to the lower extremity venous circulation, resulting in ischemia as a result of increased outflow resistance. Foam may be visible in the extracorporeal tubing, and cardiac auscultation may reveal a peculiar churning sound. Prevention depends primarily on dialysis machines that are equipped with venous air bubble traps and foam detectors located just distal to the dialyzer and a venous pressure monitor at the venous end. The detector is attached to a relay switch that simultaneously activates an alarm, shuts off the blood pump, and clamps the venous blood line if air is detected. Therefore, dialysis should never be performed in the presence of an inoperative air detection alarm system. Glass bottles should be avoided because they create vacuum effects that can permit air entry into the extracorporeal system. Dialyzer rinsing, before use, should expand all compartments to remove residual air bubbles. Incorrect Dialysate Composition Incorrect dialysate composition results from technical or human errors. Because the primary solutes constituting the dialysate are electrolytes, the dialysate concentration will be reflected by its electrical conductivity. Therefore, proper proportioning of concentrate to water can be achieved by the use of a meter that continuously measures the conductivity of the dialysate solution as it is being fed to the dialyzer. Therefore, if conductivitycontrolled systems are used, it is safer to also check the dialysate pH before dialysis. Therefore, it is important to add human monitoring of dialysate composition before every treatment, whenever a machine has been sterilized or moved about, or whenever a new concentrate is used. Therefore, it is also essential that the supplies match the machine-proportioning ratio for which they were prepared for the appropriate final dialysate composition to be obtained. Management of Clinically Suspected Air Embolism Clamp the venous blood line Hypernatremia Stop the blood pump Place the patient in the left Trendelenburg position Hypernatremia occurs when concentrate or the ratio of concentrate to water is incorrect and the conductivity monitors or the alarms are not functioning properly. Clinical manifestations include thirst, headache, nausea, vomiting, seizures, coma, and death. Dialysis should be resumed with a different machine; the dialysate sodium level should be 2 mmol/l lower than the plasma level, and isotonic saline should be concurrently infused. Dialysis against a sodium level 3 to 5 mmol/l lower than the serum level may increase the risk of disequilibrium. Ultrafiltration with equal volume replacement with normal saline is another option. Failure to add concentrate, inadequate concentrate-water ratio, or conductivity monitor or alarm malfunction can cause hyponatremia. Hyponatremia can also occur during the course of dialysis with a proportioning system if the concentrate container runs dry and the conductivity set limits are inappropriate. Acute hypo-osmolality causes hemolysis with hyperkalemia and hemodilution of all plasma constituents. Symptoms include restlessness, anxiety, pain in the vein injected with the hypotonic hemolyzed blood, chest pain, headache, nausea, and occasional severe abdominal or lumbar cramps. Treatment consists of clamping the blood lines and discarding the hemolyzed blood in the extracorporeal circuit. Dialysis should be restarted with a new dialysate batch containing low potassium, and high transmembrane pressure should be applied to remove excess water. Correction of serum sodium concentration should be achieved by no more than 1 to 2 mmol/l/h. Anticonvulsants are indicated for seizures and blood transfusions for severe anemia. Blood Loss Although acute intradialytic metabolic acidosis can be a manifestation of improper mixing of concentrates or failure of pH monitors, other causes need to be ruled out, including diabetic or alcoholic ketoacidosis, lactic acidosis, toxic ingestions, and dilutional acidosis. In most circumstances, correction of the underlying cause and use of bicarbonate dialysate at the appropriate concentration (32 to 35 mmol/l) are adequate measures. Metabolic Acidosis Intradialytic blood loss can result from arterial or venous needle disengagement from the access, separation of the venous or arterial line connections, femoral or central line dialysis catheter perforation or dislodgment, or rupture of a dialysis membrane with or without malfunction of the blood leak detector. In addition, after traumatic insertion of a dialysis catheter, blood loss can result in pain or mass from a rapidly expanding hematoma; chest, shoulder, or neck pain from intrapericardial blood loss; back, flank, groin, or lower abdominal pain or distention from retroperitoneal bleeding; or hemoptysis from pulmonary bleeding. Clotting of Dialysis Circuit Severe intradialytic metabolic alkalosis is rare and may be caused by error in dialysate concentrates, reversed connection of bicarbonate and acid concentrate containers to the entry ports of the dialysis machine, pH monitor malfunction, or use of regional citrate anticoagulation. The most common cause, however, is hydrochloric acid loss as a result of vomiting or nasogastric suction. Removal of the alkali source is usually sufficient, and H2 antagonists or proton pump inhibitors may be successful if there is gastric acid loss. The administration of sodium chloride to anephric patients with chloride-sensitive alkalosis will not repair the alkalosis. If a more rapid reduction in serum bicarbonate is desired, modification of the dialysate bath by replacement of alkali with chloride, substitution of bicarbonate with acetate dialysate, use of acid dialysate, and infusion of hydrochloric acid are effective but cumbersome measures. The use of conventional or low-bicarbonate (25 to 30 mmol/l) dialysate is probably as effective. Metabolic Alkalosis Clotting of the extracorporeal circuit during dialysis is a common practical problem, has many underlying causes, and warrants a thorough investigation. Technical factors include an inadequate or poor priming technique, resulting in retention of air in the dialyzer, and lack of or inadequate priming of the heparin infusion line. Such operator-induced errors are corrected through ongoing staff education and competency assessment. Incorrect heparin loading dose, insufficient time lapse after loading dose of heparin for systemic anticoagulation to occur, incorrect pump setting for constant heparin infusion, delayed start of the heparin pump, and failure to release the heparin line clamp are important correctible causes of clotting that should also be considered. Low-molecular-weight heparin is often used as a single bolus at the commencement of dialysis but may not maintain anticoagulation for extended hours of treatment. Vascular accessrelated problems from inadequate blood flow caused by needle or catheter positioning or clotting, excessive access recirculation, and frequent interruption of blood flow resulting from inadequate delivery or machine alarm situations are additional causes that can result in clotting. Immediate management requires prompt recognition of the underlying cause and implementation of corrective actions, including ongoing heparin dose adjustment and, if indicated, vascular access revision. Whereas cool dialysate is not dangerous and may have beneficial hemodynamic effects (see discussion regarding intradialytic hypotension), overheated dialysate can cause immediate hemolysis and life-threatening hyperkalemia, particularly if the dialysate temperature increases to more than 51° C. In such an event, dialysis must be stopped immediately and blood in the system discarded. Dialysis should be resumed to cool the patient by use of a dialysate temperature of 34° C to treat hyperkalemia and to allow blood transfusions if Temperature Monitor Malfunction Anaphylactic and Anaphylactoid Reactions Clinical Presentation Anaphylaxis is the result of an IgE-mediated acute allergic reaction in a sensitized patient, whereas anaphylactoid reactions result from the direct release of mediators by host cells. Symptoms vary from subtle to severe and include burning or heat throughout the body or at the access site; dyspnea, chest tightness, and angioedema or laryngeal edema; paresthesias involving the fingers, toes, lips, or tongue; rhinorrhea, lacrimation, sneezing, or coughing; skin flushing; pruritus; nausea or vomiting; abdominal cramps; and diarrhea. The etiology of dialysis reactions is diverse, and a thorough investigation is required. These agents include formaldehyde, glutaraldehyde, and peracetic acidhydrogen peroxide (Renalin); in allergic patients, specific IgE antibodies against formaldehyde are occasionally detectable. Significantly higher rates of anaphylactoid reactions have been observed among users of higher molecular weight compared with lower molecular weight iron dextran. Hypersensitivity to heparin formulations is rare and usually responds to substitution of beef with pork heparin, or vice versa. Whereas high-flux dialyzers have larger pores that may potentially allow larger fragments to cross from the dialysate to the patient, the synthetic high-flux membranes have a thick wall that tends to be very adsorptive for endotoxin fragments, thus mostly preventing this phenomenon. If the patient is hypotensive, administration of fluids, cessation of ultrafiltration, and discontinuation of dialysis are often required, and refractory hypotension suggesting severe sepsis should trigger hospitalization. If a non vascular accessrelated infectious source is identified, specific therapy should be instituted on the basis of the working diagnosis. Use appropriate germicide: 4% formaldehyde* 1% formaldehyde heated to 40° C* Glutaraldehyde Hydrogen peroxideperacetic acid mixture (Renalin)* Heat sterilization (105° C for 20 hours) for reprocessing of polysulfone membranes Wash and rinse the vascular access arm with soap and water. Scrub the skin with povidone-iodine or chlorhexidine and allow to dry for 5 minutes before cannulation. Mild Reactions Mild reactions particularly occur 20 to 40 minutes after initiation of dialysis, predominantly with unsubstituted cellulosic dialyzers, and consist of chest or back pain. Dialysis can be continued because symptoms usually abate after the first hour, suggesting a relation to the degree of complement activation. Indeed, these reactions decrease with the use of substituted and reprocessed unsubstituted cellulose membranes.
Purchase sildigra with visa. Erectile Dysfunction Surgical Options | Erection Problems.
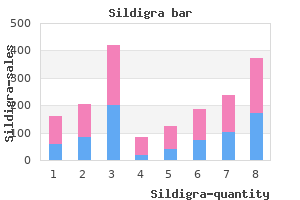
Increase of proteinuria after conversion from calcineurin inhibitor to sirolimus-based treatment in kidney transplant patients with chronic allograft dysfunction muse erectile dysfunction wiki 50 mg sildigra order otc. The influence of native nephrectomy on the incidence of recurrent disease following renal transplantation for primary glomerulonephritis erectile dysfunction treatment fruits discount sildigra 120 mg buy line. Renal allograft survival in transplant recipients with focal segmental glomerulosclerosis best erectile dysfunction pills at gnc buy 120 mg sildigra. Long-term outcome of renal transplantation patients with Henoch-Schönlein purpura erectile dysfunction treatment natural remedies buy sildigra 120 mg with mastercard. Recurrence of membranous nephropathy after renal transplantation: Probability erectile dysfunction 30s purchase sildigra from india, outcome and risk factors. Recurrence of focal segmental glomerulosclerosis in transplanted kidneys: Analysis of incidence and risk factors in 59 allografts. Recurrence of disease in patients retransplanted for focal segmental glomerulosclerosis. Recurrence of steroid resistant nephrotic syndrome in kidney transplants is associated with increased acute renal failure and acute rejection. Antihuman immunoglobulin affinity immunoadsorption strongly increases proteinuria in patients with relapsing nephrotic syndrome. Recurrent focal glomerulosclerosis: Natural course and treatment with plasma exchange. Apheresis treatment of recurrent focal segmental glomerulosclerosis after kidney transplantation: Re-analysis of published case-reports and case-series. Beneficial effect of rituximab in the treatment of recurrent membranous nephropathy after kidney transplantation. Hepatitis C virusassociated membranoproliferative glomerulonephritis in renal allografts. Recurrence of type 1 membranoproliferative glomerulonephritis after renal transplantation: Analysis of the incidence, risk factors, and impact on graft survival. Renal transplantation in patients with dense deposit disease: Morphological characteristics of recurrent disease and clinical outcome. Recurrence of nephrotic syndrome in kidney grafts of patients with congenital nephrotic syndrome of the Finnish type: Role of nephrin. Recurrent lupus nephritis after kidney transplantation: A surveillance biopsy study. Renal transplantation in systemic amyloidosis-importance of amyloid fibril type and precursor protein abundance. Clinical features, predictors of disease progression and results of renal transplantation in fibrillary/ immunotactoid glomerulopathy. Retransplantation in patients with graft loss caused by polyoma virus nephropathy. Long-term follow-up of kidney transplant patients with posttransplant lymphoproliferative disorder: Duration of posttransplant lymphoproliferative disorderinduced operational graft tolerance, interleukin-18 course, and results of retransplantation. The long-term prognosis of renal transplantation in patients with lupus nephritis. Renal transplantation for systemic lupus erythematosus and recurrent lupus nephritis. Recurrence of hemolytic-uremic syndrome in renal transplant recipients: A meta-analysis. Renal transplantation in patients with hemolytic uremic syndrome: High rate of recurrence and increased incidence of acute rejections. Outcome of renal transplantation in patients with non-Shiga toxin-associated hemolytic uremic syndrome: Prognostic significance of genetic background. Differential impact of complement mutations on clinical characteristics in atypical hemolytic uremic syndrome. Managing and preventing atypical haemolytic uremic syndrome recurrence after transplantation. Predictors and risk factors for recurrent scleroderma renal crisis in the kidney allograft: Case report and review of the literature. If there were not objective and relevant data on outcomes that are meaningful to the patient, then few would take on trust the benefits of a procedure that has the risk of multiple adverse events. The field of renal transplantation is rich with data, and increasingly sophisticated outcome measures and analyses are available to inform patient decisions. Nevertheless, when a patient is faced with a particular clinical problem, it is still common that the evidence base is insufficient to inform a specific decision. Thus it may be important to show "adjusted" results-for example, adjusted for age and gender- to get appropriate comparisons-for example, between the results in different transplant programs. A multivariate analysis will provide the opportunity to adjust the results for all of the factors that, on their own, appear to affect the outcome. In the 1000-patient example, it may be that there are statistically significant differences in death rates if the group is divided based on age, the presence or absence of diabetes, gender, or the center where the patients underwent transplantation. It may be that one transplant center that appears to have worse results performs transplants mostly on older patients and those with diabetes, whereas another center with excellent results selects only young nondiabetic recipients for transplantation. The multivariate analysis may indicate that both centers would likely achieve the same results if they performed transplants in similar patients. They may die because of the transplant, they may have an accident, or some other intervention may lead to death. The most conventional method is to use a Kaplan-Meier plot that yields an actuarial estimate of outcome, as opposed to an actual measure. The Kaplan-Meier method then uses the time of follow-up for each individual to contribute to the analysis, resulting in a better estimate of what will happen to the entire group of patients and not just the small group of patients who have reached a particular time point. For example, if one group had an average age of 30 years and the other 60 years, differing death Types of Outcome Analyses the half-life analysis is the second type of analysis that is used to extrapolate results beyond where the data stop. In the 1000-patient example it may be that no one has passed the 10-year mark, yet patients seek an estimate of how long their kidney may last. Actuarial analysis may indicate an 80% chance of a transplant lasting 10 years but does not provide information about what happens after 10 years. There are two different half-life calculations in the literature: the median survival, which is the time for which the middle patient in the series has survived; and the conditioned half-life, which is the median survival of the patients who have survived 1 year or more. One of the problems in the field is that many graft survival analyses do not make clear which is being used. Assume that 100 patients have died with their transplant still functioning at the time of death and 80 have lost their grafts from rejection and other causes. If one counts death as a cause of graft loss, then 180 of the 1000 patients have lost their grafts; if one ignores death as a cause, then only the 80 have lost their grafts. The latter calculation is best described as deathcensored graft survival, whereas the inclusive analysis is described as patient and graft survival. For example, in the illustrative analysis, the actual patient survival would be 90% (100 deaths in 1000 patients) and the death-censored graft survival would be 92% (80 grafts lost in 1000 transplants), so it might be concluded that 2% or 20 kidneys somehow survive in the absence of the recipient! Both approaches are of course relevant to different situations-on the one hand to understand what causes kidneys to fail, and separately to understand what causes patients to die-but there must be methodologic clarity. Collaborative Transplant Study analysis of actuarial survival of deceased donor renal transplants 1985 to 2011 by recipient graft number (1, 2, 3, and >3). In cardiovascular studies, in contrast, it is often possible to randomize many thousands of patients and detect differences in meaningful outcomes other than death; and in cancer studies it is possible to use shortterm evidence of tumor response as a surrogate for longer-term outcomes. In an earlier era of renal transplantation, relatively small studies could be highly informative. This was because the survival rates in the control arm were susceptible to large improvements-5-year graft and patient survival improved by 20% from a baseline around 47% to 67% with the addition of cyclosporine. Today the results of standard of care therapy are so high that recruitment of sufficient patients to detect either graft or patient survival differences at 1 or 2 years is not only extremely expensive but, unless the trials are very large, likely to founder on small random variations in such issues as surgical complications. The composite end point includes patient death, graft loss, acute rejection episodes, and loss to follow-up (the last index conservatively defaults the patients who are lost to follow-up as having failed the therapy). Which short-term surrogates provide good predictors of long-term outcomes has yet to be determined. Acute cellular rejection was, in the 1990s, a short-term measure of importance for long-term results, but perhaps not when current immunosuppressive regimens are used. All too often a cohort study is selected from a convenience sample and thus has critical systematic flaws. A typical convenience sample is "all patients being followed by a particular transplant unit. The cohort has been distorted, the flaw being that the patients not being followed, because of death or graft failure, may be crucial to the analysis. This issue is approached by meta-analysis of available studies and exemplified by the work of the International Cochrane Collaboration. The methodology requires searching for all studies of the question and especially capturing unpublished studies. The problem of publication bias plagues the field; studies with a positive finding for the intervention are more likely to be published than negative studies. However, it is still important to understand whether the risks change between dialysis and transplantation and thus to understand whether there is any action that can increase or decrease death from cancer after transplantation. A cumulative meta-analysis showing the effect of increasing numbers of trials on the confidence intervals of the outcome of death and graft loss in patients receiving interleukin-2 receptor blockers compared with placebo in all randomized controlled trials published from 1989 to 2005. Can a case report provide valuable information about outcomes after transplantation There are some instances of rare events where the knowledge from a case report has proved important. The surveillance and vigilance strategy for the safety of cells, tissues, and organs of human origin is based on this concept- identifying and publicizing the rare cases so that the problems can be recognized (see Case Reports Expert Opinion Guidelines the final type of analysis that is pervasive in the transplantation literature is expert opinion, sometimes leading to clinical practice guidelines. The clinician is faced with unanswered questions in day-to-day clinical decision making. Guidelines rate the available evidence on particular questions from good to nonexistent. Qualitative Studies Some questions are not amenable to quantitative data collection yet are of great importance to the field. These questions are amenable to qualitative research and can be assessed and measured, not to produce proof related to a particular question, but to generate testable hypotheses. Qualitative studies create insights into behaviors and attitudes and do not assume that there is a single reality to be discovered; people have different views on organ donation, and any system of measurement that expects everyone to be driven by the same perspectives is going to be disappointed. A guide to the approach of qualitative studies in transplantation has been published to assist scientists familiar mostly with quantitative studies. The completeness of data is related to the amount collected, the frequency with which it is updated, and the methods used. Incompleteness of follow-up data is a weakness of many transplant registries and depends on the ability of transplant programs to follow their patients and to report outcomes. Many patients move among physicians and thus lose contact with the transplanting center; and of course, many transplant centers are pressed for resources, so the voluntary and unpaid activity of completing data returns receives minimal attention. Regrettably, successful outcomes can be artificially inflated by centers that assume patients are alive and well unless they have heard otherwise: bad data thus produces apparently good results. Registries usually seek at least one data point annually that confirms the patient has been seen and the graft is still functioning; failing that, they define the patient as lost to follow-up at the point of last contact. This technique yields the most benefit from the data that are known about any one individual but does not allow uncertain data to contribute to analyses. Registries International Statistical Collections Types of Data Collection All analyses of data are dependent on the methodology of data collection and completeness of the data. Clearly if the data entered into an analysis are flawed in some way, then the analysis will simply embed those flaws and provide spurious confidence in the outcomes of the analysis. Once the flaws of data collection have been hidden by an analysis, it is all too often that they are never again identified and clinical practice is influenced on the basis of a false assumption. It is thus essential that the reader of any analysis verify for himself or herself whether the data were collected in a manner that is trustworthy and relevant to the question. There are many ways to collect data, all of which have their usefulness when applied in the right manner. These data are contributed by all national governments and represent probably the best estimates of global transplantation activity, but little or nothing regarding outcomes is available from that source. These three elements-primary data source, predefined information, and auditing-deliver the most trustworthy data. There are also two transplantation-specific databases of published clinical trials in the Cochrane Collaboration14 and the Transplantation Library. The final source of data for questions related to registered therapeutic products is pharmaceutical companies. Relative risk of graft failure with expanded-criteria donors in the United States, 1999 and 2000. Relative risk is compared with graft failure with donors aged 10 to 39 years with no adverse factors: relative risk = 1. These were the donors with which the majority of transplant programs commenced and which have become increasingly rare as road safety, accident retrieval, and neurosurgical interventions have all improved. The older recipient with previous medical conditions who finally dies from a cerebrovascular accident after many years of uncontrolled hypertension has had organs transplanted warily and somewhat reluctantly, usually into an older recip- ient. An analysis in the United States demonstrated that these extremes yield a twofold difference in graft survival. These criteria provide a matrix of relative risk of graft failure that ranges from 1. Percentage of actuarial nondeath-censored graft survival after living and deceased donor transplantation, 1985 to 1989. In a separate analysis it has been shown that the mean creatinine clearance 6 months after transplantation declines from approximately 65 ml/min if the donor was 20 to 25 years old to only 35 ml/min for donors older than 70 years. Impaired renal function and significant donor hypertension and diabetes are, for example, usually exclusion criteria based on donor safety rather than recipient outcomes. The cumulative data from almost all studies show that transplantation of a living donor kidney offers superior outcomes to deceased donation, though the precise reason for this is probably a mixture of recipient and donor factors including the ability to perform preemptive transplants with living donors.
The zymogen granules are membranebound sacs which fuse with the plasma membrane and are then released into the lumina of the acini erectile dysfunction causes psychological buy genuine sildigra on-line. Occasionally erectile dysfunction filthy frank discount sildigra 100 mg line, the proximal part of the dorsal duct persists as the duct of Santorini impotence treatment after prostate surgery purchase 120 mg sildigra otc. The disease has an autosomal recessive inheritance but clinical features are apparent in homozygotes only with apparent clinical features in homozygotes only erectile dysfunction gene therapy purchase sildigra with american express. The acini are atrophic and many of the acinar ducts contain laminated erectile dysfunction doctor kolkata discount sildigra 100 mg visa, eosinophilic concretions. Liver the bile canaliculi are plugged by viscid mucous which may cause diffuse fatty change, portal fibrosis and ductular proliferation. Sweat glands Hypersecretion of sodium and chloride in the sweat observed in these patients may be reflected pathologically by diminished vacuolation of the cells of eccrine glands. The onset of acute pancreatitis is sudden, occurring after a bout of alcohol or a heavy meal. The patient presents with abdominal pain, vomiting and collapse and the condition must be differentiated from other diseases producing acute abdomen such as acute appendicitis, perforated peptic ulcer, acute cholecystitis, and infarction of the intestine following sudden occlusion of the mesenteric vessels. Characteristically, there is elevation of serum amylase level within the first 24 hours and elevated serum lipase level after 3 to 4 days, the latter being more specific for pancreatic disease. The activation and release of these enzymes is brought about by one of the following mechanisms: i) Acinic cell damage caused by the etiologic factors such as alcohol, viruses, drugs, ischaemia and trauma result in release of intracellular enzymes. Familial hereditary pancreatitis, though uncommon, is more frequently chronic than the acute form. Other rare causes of chronic pancreatitis are hypercalcaemia, hyperlipidaemia and developmental failure of fusion of dorsal and ventral pancreatic ducts. Foci of calcification and tiny pancreatic concretions to larger visible stones are frequently found. Microscopically, depending upon the stage of development, the following changes are seen. There is evidence of preceding haemorrhage and necrosis in the form of deposits of haemosiderin pigment, calcium and cholesterol crystals. Chronic pancreatitis may be complicated by diabetes mellitus, steatorrhoea and pancreatic pseudocysts. Diet and obesity: Diet with high total caloric value and high consumption of animal proteins and fats is related to higher incidence of pancreatic cancer. Diabetes mellitus: Patients of long-standing diabetes mellitus have a higher incidence. Out of all these, only two pancreatic lesions- pseudocyst and carcinoma of the pancreas, are common and are discussed below. The patients generally present with abdominal mass producing pain, intraperitoneal haemorrhage and generalised peritonitis. Abdomen is distended, the liver is palpable 4 cm below costal margin, tender and has a nodular feel. The tumour of the head extends into the ampulla of Vater, common bile duct and duodenum, producing obstructive biliary symptoms and jaundice early in the course of illness. Carcinomas of the body and tail of the pancreas, on the other hand, are fairly large and irregular masses and frequently infiltrate the transverse colon, stomach, liver, spleen and regional lymph nodes. Rarely, peculiar tumour giant cell formation is seen with marked anaplasia, pleomorphism and numerous mitoses. Acinar cell carcinoma occurs rarely and reproduces the pattern of acini in normal pancreas. Obstructive jaundice More often and early in the course of disease in cases with carcinoma head of the pancreas (80%), and less often in cancer of the body and tail of the pancreas. She gives history of intermittent dull pain in the upper abdomen and bloating for the last 6 months, lasting for 1-2 days and gets relieved after taking some home remedies but she did not consult any physician for this. He is also passing high coloured urine and clay coloured stools for the same duration. On further inquiry, he is found to have lost 10 kg weight during the last 2 months. From point of view of diseases of the kidneys, 4 components of renal parenchyma require further elaboration: renal vasculature, glomeruli, tubules and interstitium. Renal vasculature Each kidney is supplied with blood by a main renal artery which arises from the aorta at the level of the 2nd lumbar vertebra. The anterior and posterior divisions divide into segmental branches from which interlobar arteries arise which course between the lobes. The arcuate arteries, in turn, give off interlobular arteries which lie in the cortex perpendicular to the capsular surface in the part overlying the pyramids and, therefore, are also called straight arteries. It is from the interlobular arteries that the afferent arterioles take their origin, each one supplying a single glomerulus. Cut surface of the kidney shows 3 main structures: welldemarcated peripheral cortex, inner medulla and the innermost renal pelvis. This latter part of the cortex forms faint striations called medullary rays, a misnomer since theses structures are located in the cortex but are destined for medulla. The capillary tuft is covered by visceral epithelial cells (podocytes) which are continuous with those of the parietal epithelium at the vascular pole. The transition to proximal tubular cells occurs at the urinary pole of the glomerulus. Subdivisions of capillaries derived from the afferent arterioles result in the formation of lobules (up to 8 in number) within a glomerulus. The mesangium is continuous at the hilum with the lacis cells of the juxtaglomerular apparatus. Besides their role as supportive cells, mesangial cells are involved in the production of mesangial matrix and glomerular basement membrane; they function in endocytosis of leaked macromolecules and also possibly in the control of glomerular blood flow through contractile elements present in these cells. The major function of glomerulus is complex filtration from the capillaries to the urinary space. The barrier to filtration of macromolecules of the size and molecular weight of albumin and larger depends upon the following: a) A normal lamina densa. The juxtamedullary glomeruli, however, give off a series of parallel vessels called vasa recta which descend to the inner medulla supplying the loop of Henle and collecting ducts and anastomose at all levels throughout the medulla with the ascending vasa recta. Lymphatic drainage likewise occurs through lymphatics associated with the intrarenal vasculature leaving the kidney at the hilum and draining to lateral aortic lymph nodes. The following important inferences can be drawn from the peculiarities of the renal vasculature: i) the renal cortex receives about 90% of the total renal blood supply and that the pressure in the glomerular capillaries is high. The mechanism of the release of renin and its role in hypertension are discussed on page 676. Tubules the tubules of the kidney account for the greatest amount of the renal parenchyma. The structure of renal tubular epithelium varies in different parts of the nephron and is correlated with the functional capacity of that part of the tubule. Interstitium In health, the renal cortical interstitium is scanty and consists of a small number of fibroblast-like cells. Cut surface of the kidney shows peripheral cortex, inner medulla and the innermost renal pelvis. Histologically, renal parenchyma is composed of 4 main components: renal vasculature, glomeruli, tubules and interstitium. Glomeruli have lobules having central stalk containing mesangial cells and matrix. Lobules have tuft of capillaries lined by endothelial cells and supported by visceral epithelial cells (podocytes). Regulation of acid-base balance by excretion of H+ ions (acidification) and bicarbonate ions. Specific gravity is used to measure the concentrating and diluting power of the kidneys. These consist of paper strips impregnated with appropriate reagents and indicator dyes. They are the result of precipitation of proteins in the tubule that includes not only albumin but also the tubular secretion of the Tamm Horsfall protein. Casts may be hyaline type consisting of only proteins indicating a non-inflammatory etiology of glomerular filtration of proteins, leucocyte casts inflammatory in origin, or red cell casts from haematuria. The tubular disease can be diagnosed in its early stage by water deprivation (concentration) or water excess (dilution) tests. However, if the tubular cells are nonfunctional, the solute concentration of the urine will remain constant regardless of stress of water deprivation. High levels of creatinine are associated with high levels of 2-microglobulin in the serum as well as urine, a lowmolecular weight protein filtered excessively in the urine due to glomerular disease or due to increased production by the liver. A clearance test is employed to assess the rate of glomerular filtration and the renal blood flow. Tubular diseases: these are more likely to be caused by toxic or infectious agents and are often acute. Vascular diseases: these include changes in the nephron as a consequence of increased intra-glomerular pressure such as in hypertension or impaired blood flow. The pathophysiological aspects of acute and chronic renal failure are briefly discussed below. Intra-renal causes Intra-renal disease is characterised by disease of renal tissue itself. The decline in formation of the urine leads to accumulation of waste products of protein metabolism in the blood and resultant azotaemia, metabolic acidosis, hyperkalaemia, hypernatraemia and hypervolaemia due to secondary effects of circulatory overload and pulmonary oedema. The specific gravity of the urine is low but the concentration of sodium in urine tends to be elevated. The process of healing may take up to one year with restoration of normal tubular function. Glomerular destruction results in changes in filtration process and leads to development of the nephrotic syndrome characterised by proteinuria, hypoalbuminaemia and oedema. Diseases causing tubulointerstitial pathology Damage to tubulointerstitial tissues results in alterations in reabsorption and secretion of important constituents leading to excretion of large volumes of dilute urine. The most common example is intake of high doses of analgesics such as phenacetin, aspirin and acetaminophen (chronic analgesic nephritis). Renal insufficiency At this stage, about 75% of functional renal parenchyma has been destroyed. Renal failure At this stage, about 90% of functional renal tissue has been destroyed. As a result, the regulation of sodium and water is lost resulting in oedema, metabolic acidosis, hypocalcaemia, and signs and symptoms of uraemia. Metabolic acidosis As a result of renal dysfunction, acidbase balance is progressively lost. The clinical features of hyperkalaemia are: cardiac arrhythmias, weakness, nausea, intestinal colic, diarrhoea, muscular irritability and flaccid paralysis. Azotaemia the waste-products of protein metabolism fail to be excreted resulting in elevation in the blood levels of urea, creatinine, phenols and guanidines causing biochemical abnormality, azotaemia. Anaemia Decreased production of erythropoietin by diseased kidney results in decline in erythropoiesis and anaemia. Integumentary system Deposit of urinary pigment such as urochrome in the skin causes sallow-yellow colour. Respiratory system Hypervolaemia and heart failure cause pulmonary congestion and pulmonary oedema due to back pressure. Radiologically, uraemic pneumonitis shows characteristic central, butterfly-pattern of oedema and congestion in the chest radiograph. Skeletal system the skeletal manifestations of renal failure are referred to as renal osteodystrophy (page 827). Two major types of skeletal disorders may occur: i) Osteomalacia occurs from deficiency of a form of vitamin D which is normally activated by the kidney (page 245). Since vitamin D is essential for absorption of calcium, its deficiency results in inadequate deposits of calcium in bone tissue. Decreased calcium level triggers the secretion of parathormone which mobilises calcium from bone and increases renal tubular reabsorption of calcium thereby conserving it. Abnormalities in amount of renal tissue these include: anomalies with deficient renal parenchyma. A simple classification including all cystic lesions of the kidney is given in Table 20. Renal dysplasia is the most common form of cystic renal disease in the newborn and infants. Normal renal parenchyma is almost totally obscured by the mass while calyces and pelvis may not be recognised. The renal pelvis and calyces are present but are greatly distorted by the cysts and may contain concretions. The cysts, however, do not communicate with the pelvis of the kidney-a feature that helps to distinguish polycystic kidney from hydronephrosis of the kidney on sectioned surface (page 674). Diagrammatic representation of comparison of gross appearance of the two main forms. In severe form, the gross bilateral cystic renal enlargement may interfere with delivery. Almost all cases of infantile polycystic kidney disease have associated multiple epitheliumlined cysts in the liver or proliferation of portal bile ductules. In older children, associated hepatic changes develop into what is termed congenital hepatic fibrosis which may lead to portal hypertension and splenomegaly. Medullary Cystic Disease Cystic disease of the renal medulla has two main types: A. The condition occurs in adults and may be recognised as an incidental radiographic finding in asymptomatic cases, or the patients may complain of colicky flank pain, dysuria, haematuria and passage of sandy material in the urine.
There is hyperkeratosis erectile dysfunction prescription medications sildigra 100 mg without prescription, focal hypergranulosis and irregular acanthosis with elongated saw-toothed rete ridges erectile dysfunction devices diabetes 50 mg sildigra order with amex. Common examples of genetic dermatoses are icthyosis erectile dysfunction treatment urologist cheap generic sildigra canada, xeroderma pigmentosum and urticaria pigmentosa erectile dysfunction caused by high cholesterol order sildigra with a visa. Common infectious dermatoses are impetigo erectile dysfunction creams and gels generic sildigra 100 mg on-line, verrucae, viral exanthemata, and superficial mycoses. A comprehensive list of tumours and tumour-like lesions of the skin is presented in Table 24. The subcutaneous tissue shows masses or nodules of calcium salt surrounded by foreign body giant cells. Histologically, squamous papillomas are characterised by hyperkeratosis, acanthosis with elongation of rete ridges and papillomatosis. Histologically, the cyst wall contains epidermis as well as appendages such as hair follicles, sebaceous glands and sweat glands. Histologically, the cyst walls are composed of several layers of epithelial cells and contain lobules of sebaceous glands in the cyst wall. The border of the elevated lesion at the lateral margin is in a straight line from the normal uninvolved epidermis (arrow). The condition may occur anywhere on the skin but is found more often on the trunk, buttocks and extremities. The condition is considered to be a forerunner of invasive squamous cell and/or basal cell carcinoma. The disorder may lead to multiple malignancies of the skin such as basal cell carcinoma, squamous cell carcinoma and malignant melanoma. Cancer of scrotal skin in chimney-sweeps was the first cancer in which an occupational carcinogen (soot) was implicated. Microscopically, squamous cell carcinoma is an invasive carcinoma of the surface epidermis characterised by the following features. On cutting, the growth is both exophytic and endophytic and is chalky white in colour. It is customary with pathologists to label squamous cell carcinomas with descriptive terms such as: well-differentiated, moderately-differentiated, undifferentiated, keratinising, nonkeratinising, spindle cell type etc. Overall prognosis of squmaous cell carcinoma induced by actinic keratosis is excellent. The most characteristic histologic feature is the presence of multiple horn cysts having keratinised centre and surrounded by basophilic cells resembling basal cells. Histologically, the circumscribed tumour is located in deeper dermis and subcutis. Histologically, the tumour is composed of variable-sized lobules of poorly-differentiated cells containing some sebaceous cells. The tumour cells show marked cytologic atypia such as pleomorphism and hyperchromasia. Eccrine poroma this tumour arises from intraepidermal portion of the sweat gland duct. Histologically, it consists of tumour cells arising from the lower portion of the epidermis and extending downward into dermis as broad anastomosing bands. Eccrine hidradenoma Hidradenoma originates from the intradermal portion of the eccrine sweat duct. The tumour cells are round to polygonal and may have clear or eosinophilic cytoplasm. Eccrine spiradenoma this is found as a solitary, painful, circumscribed nodule in the dermis. Papillary hidradenoma Papillary hidradenoma or hidradenoma papilliferum is usually located as a small lesion commonly in women in the skin of the anogenital area. Histologically, it is a circumscribed tumour in the dermis under a normal epidermis. The tumour cells lining these structures resemble apocrine epithelium with features of decapitation secretions. All these carcinomas are adenocarcinomas and must be distinguished from metastatic adenocarcinoma in the skin. Most naevi appear in adolescence and in early adulthood due to hormonal influence but rarely may be present at birth. Melanin pigment is abundant in the naevus cells present in the lower epidermis and upper dermis, but the cells in the mid-dermis and lower dermis hardly contain any melanin. These lesions, in addition to the junctional activity as in junctional naevi, show nests of naevus cells in the dermis to a variable depth. The lesion is mainly located in the upper dermis as nests and cords of naevus cells. Juvenile melanoma is important since it is frequently confused with malignant melanoma histologically. The common sites on the skin are the trunk (in men), legs (in women); other locations are face, soles, palms and nail-beds. Some high risk factors associated with increased incidence of malignant melanoma are as under: i) Persistent change in appearance of a mole. Malignant melanoma can be differentiated from benign pigmented lesions by subtle features as summed up in Table 24. Spread Histologically, irrespective of the type of malignant melanoma, the following characteristics are observed. At times, there may be no evidence of melanin in H&E stained sections but Fontana-Masson stain or dopa reaction reveals melanin granules in the cytoplasm of tumour cells. Depending upon the depth of invasion into the dermis, Clark has described following 5 levels: Level I: Malignant melanoma cells confined to the epidermis and its appendages. The prognosis for patients with malignant melanoma depends upon the stage at presentation. Metastatic spread of malignant melanoma is very common and takes place via lymphatics to the regional lymph nodes and through blood to distant sites like lungs, liver, brain, spinal cord, and adrenals. Just as in breast cancer, sentinel lymph node biopsy is quite helpful in evaluation of regional nodal status. All the tissue elements of the dermis such as fibrous tissue, adipose tissue, neural tissue, endothelium and smooth muscle are capable of transforming into benign and malignant tumours. The commonest sites are the lower and upper extremities, followed in decreasing frequency, by abdominal cavity and retroperitoneum. The benign variant is also known by various synonyms like dermatofibroma, histiocytoma, sclerosing haemangioma, fibroxanthoma and xanthogranuloma. Benign histiocytomas are often small but malignant fibrous histiocytomas may be of enormous size. The benign variety contains uniform spindle-shaped cells with admixture of numerous foamy histiocytes. Histologically, xanthomas are composed of dermal collections of benign-appearing foamy histiocytes. Multinucleate tumour giant cells surrounded by lipid-laden cytoplasm are often present. Lesions may affect different body surfaces but often involve the trunk, extremities, face and scalp. It may be well-differentiated, moderately-differentiated, undifferentiated, keratinising, non-keratinising, spindle cell type. Tumours arising from epidermal adnexa or appendages can differentiate towards hair follicles, sebaceous glands and sweat glands (apocrine and eccrine glands). There is a history of presence of small waxy nodule initially for about one year which slowly increased in size followed by its ulceration. This system is commonly termed hypothalamic-pituitary hormone axis for different hormones schematically illustrated in. With this brief overview of principles of physiology of hormones, we now turn to the study of diseases of the endocrine organs. Hypofunction Deficiency of hormones occurs from destruction of hormone-forming tissues from inflammation (often autoimmune), infections, iatrogenic. Neuroendocrine cells which are present in the gastric and intestinal mucosa and elaborate peptide hormones. Neuroganglia cells lie in the ganglia cells in the sympathetic chain and elaborate amines. In addition to above, other non-endocrine secretions include neurotransmitter substances such as acetylcholine and dopamine released from neural synapses, and erythropoietin and vitamin D3 elaborated from the kidney. Understanding the pathology of these endocrine organs requires the knowledge of overall framework of hormone secretions, their actions and broad principles of feedback mechanisms. These include neuroendocrine cells in gastric and intestinal mucosa, neuroganglia cells, adrenal medulla, parafollicular C cells of the thyroid, islets of Langerhans and isolated cells in the left atrium. Anatomically, endocrine system consists of 6 distinct organs: pituitary, adrenals, thyroid, parathyroids, gonads, and pancreatic islets. It is situated at the base of the brain in a hollow called sella turcica formed out of the sphenoid bone. The gland is composed of 2 major anatomic divisions: anterior lobe (adenohypophysis) and posterior lobe (neurohypophysis). The adenohypophysis has no direct neural connection but has indirect connection through capillary portal circulation by which the anterior pituitary receives the blood which has already passed through the hypothalamus. Chromophil cells with basophilic granules these cells constitute about 10% of the anterior lobe and are mainly found in the region of median wedge. Chromophobe cells without visible granules these cells comprise the remainder 50% of the adenohypophysis. These cells by light microscopy contain no visible granules, but on electron microscopy reveal sparsely granulated corticotrophs, thyrotrophs and gonadotrophs. Oxytocin It causes contraction of mammary myoepithelial cells resulting in ejection of milk from the lactating breast and causes contraction of myometrium of the uterus at term. It is obvious from the description above that pituitary, though a tiny organ, is concerned with a variety of diverse functions in the body. The pituitary gland and hypothalamus are so closely interlinked that diseases of the pituitary gland involve the hypothalamus, and dysfunctions of the hypothalamus cause secondary changes in the pituitary. The pituitary gland is involved in several diseases which include: non-neoplastic. Gigantism, therefore, occurs in prepubertal boys and girls and is much less frequent than acromegaly. The main clinical feature in gigantism is the excessive and proportionate growth of the child. These features result either from associated inhibition of gonadotropin secretion or interference in gonadotropin effects. The features include premature development of genitalia both in the male and in the female, growth of pubic hair and axillary hair. Though a number of syndromes associated with deficiency of anterior pituitary hormones have been described, two important syndromes are panhypopituitarism and dwarfism. Empty-sella syndrome Empty-sella syndrome is characterised by the appearance of an empty sella and features of panhypopituitarism. Most commonly, it results from herniation of subarachnoid space into the sella turcica due to an incomplete diaphragma sella creating an empty sella. Less often, it may be due to a pituitary adenoma or craniopharyngioma, infarction and trauma to the pituitary. The only significant clinical syndrome due to hypofunction of the neurohypophysis and hypothalamus is diabetes insipidus. The main features of diabetes insipidus are excretion of a very large volume of dilute urine of low specific gravity (below 1. Papillary pattern is composed of columnar or fusiform cells arranged about fibrovascular papillae. Functional classification of pituitary adenoma can be done by carrying out specific immunostains against the hormone products. Pressure effects these are caused by expansion of the lesion resulting in destruction of the surrounding glandular tissue by pressure atrophy. Major pituitary tumours are adenomas (micro- and macroadenomas) and craniopharyngioma. Sporadiac cases appear to be due to genetic abnormalities of signaling pathways, particularly G protein mutations. It has 2 peaks of occurrence: children and young adults in 1st to 2nd decade and then in adults past 6th decade. The fluid in the cystic cavity typically has colour and consistency of machinery oil. Histologically, craniopharyngioma closely resembles ameloblastoma of the jaw (page 513). Stratified squamous epithelium frequently lining a cyst and containing loose stellate cells in the centre. Zona fasciculata is the middle layer and constitutes approximately 70% of the cortex. It consists of cords of more compact cells than those of zona fasciculata but has similar functional characteristics of synthesis and secretion of glucocorticoids and androgens. Central or truncal obesity contrasted with relatively thin arms and legs, buffalo hump due to prominence of fat over the shoulders, and rounded oedematous moon-face. Increased protein breakdown resulting in wasting and thinning of the skeletal muscles, atrophy of the skin and subcutaneous tissue with formation of purple striae on the abdominal wall, osteoporosis and easy bruising of the thin skin from minor trauma. Systemic hypertension is present in 80% of cases because of associated retention of sodium and water. Bilateral adrenal hyperplasia, especially in children (congenital hyperaldosteronism). Adrenogenital syndrome characterised by excessive production of adrenal sex steroids.
Additional information:
References
- Eisenberg, D., Popescu, W. M., Duffy, A. J., et al. Laparoscopic treatment of subxiphoid incisional hernias in cardiac transplant patients. JSLS. 2008; 12:262-266.
- Juweid ME, Stroobants S, Hoekstra OS, et al. Use of positron emission tomography for response assessment of lymphoma: consensus of the Imaging Subcommittee of International Harmonization Project in Lymphoma. J Clin Oncol 2007;25(5):571-578.
- Wilkins RM, Pritchard DJ, Burgert EO Jr, et al. Ewing's sarcoma of bone. Experience with 140 patients. Cancer 1986;58(11):2551-2555.
- Kawakami T, Mizoguchi M, Saito R, Soma Y. Histopathological evidence of small-vessel vasculitis within the skin and lungs associated with interstitial pneumonia in an adult patient with dermatomyositis. Clin Exp Dermatol 2008;33(4):415-7.
- Curhan GC, Willett WC, Rimm EB, et al: Prospective study of beverage use and the risk of kidney stones, Am J Epidemiol 143(3):240n247, 1996. Curhan GC, Willett WC, Rimm EB, et al: A prospective study of the intake of vitamins C and B6, and the risk of kidney stones in men, J Urol 155(6):1847n1851, 1996. Curhan GC, Willett WC, Speizer FE, et al: Comparison of dietary calcium with supplemental calcium and other nutrients as factors affecting the risk for kidney stones in women, Ann Intern Med 126(7):497n504, 1997.
- Nemoy NJ, Staney TA: Surgical, bacteriological, and biochemical management of infection stones, JAMA 215(9):1470n1476, 1971.
- Nethercott SE, Strawbridge WG. Identification of bacterial residues in sarcoid lesions. Lancet 1956;271:1132-4.
- Hosteenge J, Stone JR, Donella-Deane A, et al: The effect of substituting phosphotyrosine for sulphotyrosine on the activity of hirudin. Eur J Biochem 1990;188:55-59.
