
Trecator SC
| Contato
Página Inicial
Hiep T. Nguyen, MD
- Assistant Professor of Surgery, Harvard Medical School
- Assistant in Urology, Children? Hospital Boston, Boston,
- Massachusetts
Biofilms were more frequently observed in the apical portion of canals of teeth with large lesions medications j-tube trecator sc 250 mg purchase mastercard, especially those associated with a cyst medicine nausea generic 250 mg trecator sc visa. Apical periodontitis seems to fulfill most of the established criteria used to determine whether a given infectious disease can be classified as being caused by biofilm communities treatment kitty colds cheap trecator sc master card. A persistent intraradicular infection is caused by bacteria associated with the primary infection medications just for anxiety discount 250mg trecator sc otc, which had survived intracanal antimicrobial procedures medications made easy cheap 250mg trecator sc fast delivery. A secondary intraradicular infection is caused by microorganisms that were not present in the primary infection but were introduced in the root canal system at some stage after intervention, so called because it is secondary to intervention. A secondary infection is usually a contamination problem caused either by a breach in the aseptic chain, or by coronal leakage. Persistent and secondary infections are, for the most part, clinically indistinguishable. Exceptions include infection-related complications, for example, acute exacerbations arising after the treatment of noninfected teeth and emergent posttreatment apical periodontitis lesions which were absent at the time of treatment but appeared on the follow-up radiograph. Both persistent and secondary infections can be responsible for several clinical problems, including persistent exudation, persistent symptoms, interappointment flare-ups and treatment failure, characterized by posttreatment apical periodontitis. Enterococcus faecalis is a facultative bacteria most frequently detected in root canaltreated teeth. The number of microbial species present in adequately treated canals with posttreatment disease is lower than in inadequately treated or untreated canals. Extraradicular infections are characterized by bacterial invasion of the inflamed periradicular tissues and are a sequel to intraradicular infection. Extraradicular infections may be dependent on or independent of intraradicular infection; the existence of the latter condition remains to be proven. Except for acute and chronic apical abscesses, it is still controversial whether asymptomatic apical periodontitis lesions can harbour bacteria for very long, beyond the initial tissue invasion. The Need to Enhance Disinfection Culture-dependent or culture-independent (molecular) and histobacteriological studies have revealed that bacteria can persist in the root canal system after chemomechanical preparation in 40% to 60% of cases. Irrigant solutions, such as sodium hypochlorite and chlorhexidine, have pronounced antimicrobial activities and generally are effective against a large spectrum of microbial species found in infected root canals. However, the effectiveness is mostly observed when contact between irrigant and microbial cells are optimal. In clinical practice, the irrigant needs to diffuse to reach the aforementioned areas, but the short duration they remain in the canal during preparation procedures is a major limiting factor. Antimicrobial irrigating solutions usually remain in the root canal system for a shorter time period (1030 minutes) compared with an interappointment intracanal medicament (7 or more days). The substantial time difference can alter the effectiveness of bacterial elimination, especially if the antimicrobial agent is expected to reach areas distant from the main root canal by diffusion. Popular medications at that time included formaldehyde-containing substances99 and phenolic100 and iodoform-based pastes. Of the substances currently recommended for intracanal medication, calcium hydroxide is most widely accepted and commonly used. Chlorhexidine and antibiotics have also been suggested for some situations (Table 8-2). Most of its biological effects are related to its alkaline pH and due to the hydroxyl ions. Although some clinicians have developed methods of placing calcium hydroxide powder into the canal, placement is easier, more reliable and the canal better filled when calcium hydroxide is mixed with a liquid, gel, creamy carrier or vehicle. Since the effects of calcium hydroxide are pH-dependent, the ideal vehicle should enable the ionic dissociation of calcium hydroxide, which will vary depending on the type of vehicle used. Calcium hydroxide vehicles have been classified, according to consistency and ability to permit its dissociation, into aqueous, viscous and oily vehicles (Table 8-3). As the effects of calcium hydroxide are dependent on the pH reached around where it has been placed, if the ionic release is slow, it may be unable to exert its intended effects. Vehicles for calcium hydroxide may also be classified as being inert, or biologically active, from an antimicrobial standpoint (see Table 8-3). On the other hand, biologically active vehicles may provide additional effects to the calcium hydroxide, including improved or additive antimicrobial properties; these vehicles include camphorated paramonochlorophenol, chlorhexidine and iodine potassium iodide. In laboratory studies, most endodontic bacteria are eliminated after a short period of exposure to calcium hydroxide, as a result of its high pH level. In clinical practice, such conditions are not easy to achieve because direct contact between calcium hydroxide and bacteria is not always possible. In addition to the difficulties of achieving optimal contact between medicament and bacteria colonizing the intricacies of the root canal system, the medicament has to diffuse to areas distant from the main root canal; these may help explain the limitations of calcium hydroxide in predictably disinfecting the root canal system. Calcium hydroxide owes its biocompatibility to its low water solubility and diffusibility8; hence, its cytotoxic effect is limited to the tissue area in which it is in direct contact. On the other hand, the same low solubility and diffusibility make it difficult for calcium hydroxide to promote a rapid and significant increase in pH to eliminate bacteria present in dentinal tubules, tissue remnants, ramifications and isthmuses. The killing of bacteria by calcium hydroxide depends on the availability of hydroxyl ions in solution, which is much higher in the main root canal, where it is placed. As calcium hydroxide diffuses to other areas in the root canal system, the concentration of hydroxyl ions decreases as a result of the action of tissue buffering systems (bicarbonate and phosphate), acids, proteins and carbon dioxide. Saline Distilled water Dental anaesthetic solution Glycerine Propyleneglycol Polyethyleneglycol al. Long-term use, preferably with changes of the calcium hydroxide, is necessary to maximize disinfection of the root canal system. Another factor that may interfere with calcium hydroxide antimicrobial effectiveness is the presence of resistant species in the root canal system. Resistance to calcium hydroxide has been reported for some microbial species, such as E. Although camphorated paramonochlorophenol exhibits high toxicity when used alone, satisfactory biocompatibility results have been observed in animal studies with this combination. Chlorhexidine has also been proposed as a biologically active vehicle in combination with calcium hydroxide. In vitro studies have shown conflicting results for this combination, with some reporting that the antimicrobial effects were higher than calcium hydroxide alone,136 whereas others found no significant difference. At a higher pH, it precipitates and may not be available to act as an antimicrobial agent. However, studies have demonstrated that when Ledermix or Odontopaste is mixed with calcium hydroxide, it resulted in a significant loss of antibiotic activity144 and rapid destruction of the steroid component. Most are toxic to host tissues, some are allergenic and may even be carcinogenic; some are ineffective in clinical practice. Consequently, the use of most of these substances has been discontinued, and they are no longer recommended. Apart from calcium hydroxide, other medicaments in use include chlorhexidine and antibiotics. Chlorhexidine bacterial cytoplasmic membrane resulting in leakage of cytoplasmic components, a bacteriostatic effect. At higher bactericidal concentrations, chlorhexidine enters the bacterial cytoplasm via the damaged membranes and interacts with phosphated entities to form irreversible precipitates,147,155 killing the cell. As an intracanal medicament, chlorhexidine has been shown in vitro to be more effective than calcium hydroxide in disinfecting dentinal tubules. It has been widely used as a topical antiseptic solution, and effective concentrations range from 0. Chlorhexidine is highly effective against several gram-positive and gram-negative oral bacterial species as well as yeasts. At lower concentrations, chlorhexidine penetrates and disrupts the Antibiotics are naturally occurring substances of microbial origin, or synthetic, or semisynthetic, substances that exhibit antimicrobial activity in low concentrations by killing, or inhibiting the growth of, selective microorganisms. Antibiotics exert their actions on specific groups of microorganisms, and its range of effectiveness is termed its spectrum. The spectrum is broad when the antibiotic is effective against a wide variety of grampositive and gram-negative bacteria; the spectrum is small when it acts against a reduced number of susceptible species. Since antibiotics used systemically, or topically, are usually successful in treating infections in the body, their use as topical antimicrobial agents in root canal treatment was suggested. The main concerns about using antibiotics as intracanal medicaments include the possibility of: 8 Intracanal Medication 139 · Sensitization. The patient is sensitized to that drug and becomes predisposed to further allergic reactions when in contact with the same drug for another purpose. This is more critical with penicillins, cephalosporins and sulphonamide, for which severe and common allergic reactions have been reported. The inappropriate use of antibiotics is to be discouraged and avoided because of the risks of developing resistant bacterial strains that may cause diseases that are difficult or even impossible to treat. Bacterial strains carrying antibiotic resistance genes in endodontic infections have been detected. From a therapeutic standpoint, if a persistent infection caused by antibiotic resistant strains becomes acute, it may render ineffective, when required the use of systemic antibiotics. Endodontic infections are characterized by multispecies communities with a large interindividual variability in the bacterial species composition. Tetracycline is widely used in periodontics and has been included in some formulations for endodontic use. For instance, Ledermix contains a tetracycline derivative (demeclocycline) and a corticosteroid (triamcinolone). It has been tested as an interappointment dressing,176 but its effects were limited and not better than calcium hydroxide. Odontopaste is a zinc oxidebased preparation containing a corticosteroid (triamcinolone) and an antibiotic (clindamycin); it has been marketed as an alternative to Ledermix. Endodontic Treatment in Single or Multiple Visits Single-visit treatment implies performing chemomechanical procedures and placing a permanent root canal filling at the very same appointment. The decision as to whether the root canal treatment can be completed in one, or more, visits depends primarily on the condition of the pulp and the periradicular tissues. Infected teeth, especially if apical periodontitis is present, should be approached differently. As discussed earlier, it is questionable whether chemomechanical procedures alone will 140 8 Intracanal Medication predictably achieve adequate disinfection in all cases; especially, if infection is present in anatomic areas inaccessible to instruments and irrigants. A debatable issue in clinical endodontic practice is whether a medicament that remains in the root canal between appointments will significantly improve disinfection and enhance periradicular tissue healing. Chemomechanical procedures are highly effective, and therefore, of crucial importance in the control of root canal infection. A study192 using a large sample size composed of teeth treated by only one operator indicated that treatment performed in two, or more, visits using calcium hydroxide for intracanal medication resulted in a significantly higher favourable outcome rate compared with cases treated in a single visit; this is consistent with studies showing that the best protocol for infection control involves the use of an intracanal medication in a two-visit treatment approach. Contamination might occur as a result of microleakage or breakage of the temporary restoration. Therefore, pain control using intracanal medicaments is related to infection control. Antiinflammatory drugs can also be used for the prevention of pain in cases where it is most anticipated. Examples included a vital tooth that had not been completely instrumented, or had been overinstrumented. Teeth with persistent symptoms after chemomechanical procedures are usually associated with persistent infection and should be managed similar to cases with persistent exudation. Intracanal medication is used in these cases to act indirectly on the inflammatory process by helping to eliminate its primary cause, i. Topical intracanal use of antiinflammatory drugs, such as corticosteroids, which act directly on inflammation, are not generally recommended in these cases because their action is on the effect rather than the cause, usually microorganisms involved in persistent, or secondary, infections. Ultrasonic activation of the sodium hypochlorite irrigant can also improve cleaning of these less easily accessible areas. Inflammatory resorption of the root surface may progress rapidly and lead to significant tooth tissue loss in a matter of months if left untreated. If this is not possible, calcium hydroxide paste in an inert vehicle should be placed and root canal filling scheduled for the next visit. With these cases, efforts should always be made to complete chemomechanical cleaning and shaping early, preferably at the first visit. Where it was not possible to complete instrumentation, in selected cases, a corticosteroid medicament may be placed to prevent postoperative pain. At the first appointment, the root canals should be completely cleaned and shaped in the presence of copious and frequent irrigation of 0. Passive ultrasonic activation of the sodium hypochlorite irrigant (Chapter 7) or a final rinse with chlorhexidine may be carried out to improve canal disinfection. The use of an additive medicament with calcium hydroxide is especially relevant in retreatment cases, because of the increased risk of the presence of microbial species, such as E. At the second appointment, the calcium hydroxide dressing is removed and the root canal filled. If canal preparation cannot be completed at the first visit, there may be no room for placement of calcium hydroxide; tissue remnants can significantly dampen its effects anyway. With these cases, following final irrigation with sodium hypochlorite, excess solution is removed by aspiration and the root canal is then coronally sealed. Root canal preparation will have to be completed at the second appointment, followed by placement of calcium hydroxide intracanal medication. Instead, the good results with calcium hydroxide medication, in cases of external inflammatory root resorption, are related to its antimicrobial effects on bacteria located within dentinal tubules and other anatomical irregularities, which induce and maintain inflammation and the resorptive process. It also serves as a long-term dressing to maintain the environment free of microorganisms until repair of the periradicular tissues ensues and an apical barrier is achieved by the formation of a cementum-like hard tissue. However, a Lentulo spiral filler is an efficient instrument for the placement of calcium hydroxide paste. Operated in a low-speed handpiece, two or three applications of calcium hydroxide paste are placed into the canal. Learning Outcomes After reading this chapter, the reader should be able to explain and discuss the: · indications for using intracanal medication in endodontic treatment; · properties and modes of action of different intracanal medicaments; · different types of endodontic infections and cite the most important associated microbial species; · way bacteria colonize the root canal system; · different clinical conditions based on presence or absence of infection and how to manage them properly; · clinical antimicrobial effectiveness during the different phases of endodontic treatment and the need for enhanced canal disinfection to achieve a favourable treatment outcome. Fate of the tissue in lateral canals and apical ramifications in response to pathologic conditions and treatment procedures. Histologic investigation of root canal-treated teeth with apical periodontitis: a retrospective study from twenty-four patients. Biofilms and apical periodontitis: study of prevalence and association with clinical and histopathologic findings.
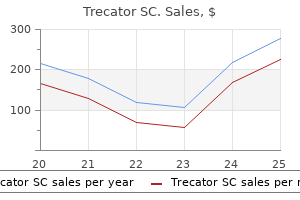
In patients with bacterial meningitis medications j-tube purchase 250 mg trecator sc with amex, di use meningeal enhancement is of en seen af er the administration o gadolinium treatment arthritis order genuine trecator sc. It progresses to a petechial rash treatments yeast infections pregnant buy trecator sc no prescription, then to a purpuric rash symptoms 0f yeast infectiion in women buy discount trecator sc online, and i untreated medicine reminder trecator sc 250 mg buy on line, to skin necrosis or gangrene. Anaplasma phagocytophilum causes human granulocytic ehrlichiosis (anaplasmosis), and Ehrlichia cha eensis causes human monocytic ehrlichiosis. The principal causes include Mycobacterium tuberculosis, Cryptococcus neo ormans, Histoplasma capsulatum, Coccidioides immitis, and reponema pallidum. Ce epime is a broad-spectrum ourth-generation cephalosporin with in vitro activity similar to that o ce otaxime or cef riaxone against S. In clinical trials, ce epime has been demonstrated to be equivalent to ce otaxime in the treatment o penicillin-sensitive pneumococcal and meningococcal meningitis, and it has been used success ully in some patients with meningitis due to Enterobacter species and P. Metronidazole is added to the empirical regimen to cover gram-negative anaerobes in patients with otitis, sinusitis, or mastoiditis. In hospital-acquired meningitis, and particularly meningitis ollowing neurosurgical procedures, staphylococci and gram-negative organisms including P. In these patients, empirical therapy should include a combination o vancomycin and cef azidime, ce epime, or meropenem. The number o patients with bacterial meningitis enrolled in clinical trials o meropenem has not been su cient to de nitively assess the e cacy o this antibiotic. A 7-day course o intravenous antibiotic therapy is adequate or uncomplicated meningococcal meningitis. Methicillin-sensitive Methicillin-resistant Listeria monocytogenes Haemophilus in uenzae Streptococcus agalactiae Bacteroides ragilis Fusobacterium spp. Close contacts are de ined as those individuals who have had contact with oropharyngeal secretions, either through kissing or by sharing toys, beverages, or cigarettes. Pneumococcal meningitis Antimicrobial therapy o pneumococ- intravenous vancomycin therapy, then either intraventricular or intrathecal vancomycin, 20 mg once daily, can be added. A 3-week course o intravenous antibiotic therapy is recommended or meningitis due to gram-negative bacilli. G ram-negative bacillary meningitis cal meningitis is initiated with a cephalosporin (ce triaxone, ce otaxime, or ce epime) and vancomycin. Once the results o antimicrobial susceptibility tests are known, therapy can be modi ied accordingly (able 46-3). Ri ampin can be added to vancomycin or its synergistic e ect but is inadequate as monotherapy because resistance develops rapidly when it is used alone. A 2-week course o intravenous antimicrobial therapy is recommended or pneumococcal meningitis. The intraventricular route o administration is pre erred over the intrathecal route because adequate concentrations o vancomycin in the cerebral ventricles are not always achieved with intrathecal administration. Vancomycin is the drug o choice or methicillin-resistant staphylococci and or patients allergic to penicillin. A prospective European trial o adjunctive therapy or acute bacterial meningitis in 301 adults ound that dexamethasone reduced the number o un avorable outcomes (15 vs. Dexamethasone (10 mg intravenously) was administered 1520 min be ore the rst dose o an antimicrobial agent, and the same dose was repeated every 6 h or 4 days. These results were con rmed in a second trial o dexamethasone in adults with pneumococcal meningitis. T erapy with dexamethasone should ideally be started 20 min be ore, or not later than concurrent with, the rst dose o antibiotics. One o the concerns or using dexamethasone in adults with bacterial meningitis is that in experimental models o meningitis, dexamethasone therapy increased hippocampal cell injury and reduced learning capacity. Patients of en have mild lethargy or drowsiness; however, pro ound alterations in consciousness, such as stupor, coma, or marked con usion, do not occur in viral meningitis and suggest the presence o encephalitis or other alternative diagnoses. Moderate or severe sequelae occur in ~25% o survivors, although the exact incidence varies with the in ecting organism. Common sequelae include decreased intellectual unction, memory impairment, seizures, hearing loss and dizziness, and gait disturbances. Headache is almost invariably present and of en characterized as rontal or retroorbital and requently associated with photophobia and pain on moving the eyes. Nuchal rigidity is present in most cases but may be mild and present only near the limit o neck ante exion. Constitutional signs can include Herpesviruses Cytomegalovirusa Herpes simplex virus 1 b Herpes simplex virus 2 Human herpesvirus 6 Varicella-zoster virus Epstein-Barr virus Arthropod-borne viruses La Crosse virus West Nile virus c St. In temperate climates, there is a substantial increase in cases during the nonwinter months, re ecting the seasonal predominance o enterovirus and arthropod-borne virus (arbovirus) in ections in the summer and all, with a peak monthly incidence o about 1 reported case per 100,000 population. During enteroviral in ections, viral shedding in stool may persist or several weeks. The presence o enterovirus in stool is not diagnostic and may result rom residual shedding rom a previous enteroviral in ection; it also occurs in some asymptomatic individuals during enteroviral epidemics. The typical pro le is a pleocytosis, a normal or slightly elevated protein concentration (0. As a rule, a lymphocytic pleocytosis with a low glucose concentration should suggest ungal or tuberculous meningitis, Listeria meningoencephalitis, or nonin ectious disorders. For viruses with low seroprevalence rates, diagnosis o acute viral in ection can be made by documenting seroconversion between acute-phase and convalescent sera (typically obtained af er 24 weeks) or by demonstrating the presence o virus-speci c IgM antibodies. Oligoclonal bands also occur commonly in certain nonin ectious neurologic diseases. A variety o clinical algorithms or di erentiating bacterial rom aseptic meningitis have been developed. One such prospectively validated system, the bacterial meningitis score, suggests that the probability o bacterial meningitis is 0. Enteroviruses are the most likely cause o viral meningitis in the summer and all months, especially in children (<15 years), although cases occur at reduced requency year round. Although the incidence o enteroviral meningitis declines with increasing age, some outbreaks have pre erentially a ected older children and adults. Patients present with sudden onset o ever; headache; nuchal rigidity; and of en constitutional signs, including vomiting, anorexia, diarrhea, cough, pharyngitis, and myalgias. The physical examination should include a care ul search or stigmata o enterovirus in ection, including exanthems, hand- ootmouth disease, herpangina, pleurodynia, myopericarditis, and hemorrhagic conjunctivitis. Chronic and severe in ections can occur in neonates and in individuals with hypo- or agammaglobulinemia. Arboviral meningitis should be considered when clusters o meningitis and encephalitis cases occur in a restricted geographic region during the summer or early all. Mumps should be considered when meningitis occurs in the late winter or early spring, especially in males (male-to- emale ratio 3:1). With the widespread use o the live attenuated mumps vaccine in the United States since 1967, the incidence o mumps meningitis has allen by >95%; however, mumps remains a potential source o in ection in nonimmunized individuals and populations. Rare cases (10100:100,000 vaccinated individuals) o vaccine-associated mumps meningitis have been described, with onset typically 24 weeks af er vaccination. The presence o parotitis, orchitis, oophoritis, pancreatitis, or elevations in serum lipase and amylase is suggestive o mumps meningitis; however, their absence does not exclude the diagnosis. Clinical meningitis was previously estimated to occur in 1030% o patients with mumps parotitis; however, in a recent U. Mumps in ection con ers li elong immunity, so a documented history o previous in ection excludes this diagnosis. Hypoglycorrhachia, occurs in 1030% o patients and may be a clue to the diagnosis when present. Some patients have an associated rash, pulmonary in ltrates, alopecia, parotitis, orchitis, or myopericarditis. Patients with suspected bacterial meningitis should receive appropriate empirical therapy pending culture results (see above). Seriously ill patients should probably receive intravenous acyclovir (1530 mg/kg per day in three divided doses), which can be ollowed by an oral drug such as acyclovir (800 mg ve times daily), amciclovir (500 mg tid), or valacyclovir (1000 mg tid) or a total course o 714 days. Patients with viral meningitis who are known to have de cient humoral immunity. Intraventricular administration o immunoglobulin through an Ommaya reservoir has been tried in some patients with chronic enteroviral meningitis who have not responded to intramuscular or intravenous immunoglobulin. Vaccination is an e ective method o preventing the development o meningitis and other neurologic complications associated with poliovirus, mumps, measles, rubella, and varicella in ection. Clinical studies indicate an e ectiveness rate o 7090% or this vaccine, but a booster may be required af er ~10 years to maintain immunity. Rare patients complain o persisting headache, mild mental impairment, incoordination, or generalized asthenia or weeks to months. The outcome in in ants and neonates (<1 year) is less certain; intellectual impairment, learning disabilities, hearing loss, and other lasting sequelae have been reported in some studies. Despite comprehensive diagnostic e orts, the majority o cases o acute encephalitis o suspected viral etiology remain o unknown cause. Hundreds o viruses are capable o causing encephalitis, although only a limited subset is responsible or most cases in which a speci c cause is identi ed (able 46-4). Epidemics o encephalitis are caused by arboviruses, which belong to several di erent viral taxonomic groups including Alphaviruses. Louis encephalitis virus, Japanese encephalitis virus, Powassan virus), and Bunyaviruses. Historically, the largest number o cases o arbovirus encephalitis in the United States has been due to St. States reporting >200 cases included exas (1868 cases), Cali ornia (479), Louisiana (335), Illinois (290), Mississippi (249), South Dakota (203), and Michigan (202). States reporting >100 cases included Cali ornia (357 cases), Colorado (315), Nebraska (213), exas (157), South Dakota (148), North Dakota (123), and Illinois (106). Many patients with encephalitis also have evidence o associated meningitis (meningoencephalitis) and, in some cases, involvement o the spinal cord or nerve roots (encephalomyelitis, encephalomyeloradiculitis). Patients with encephalitis may have hallucinations, agitation, personality change, behavioral disorders, and, at times, a rankly psychotic state. Virtually every possible type o ocal neurologic disturbance has been reported in viral encephalitis; the signs and symptoms re ect the sites o in ection and in ammation. The most commonly encountered ocal ndings are aphasia, ataxia, upper or lower motor neuron patterns o weakness, involuntary movements. Ideally at least 20 mL should be collected with 510 mL stored rozen or later studies as needed. These tests help identi y or exclude alternative diagnoses and assist in the di erentiation between a ocal, as opposed to a di use, encephalitic process. Note the area o increased signal in the right temporal lobe (le t side o image) con ned predominantly to the gray matter. This patient had predominantly unilateral disease; bilateral lesions are more common but may be quite asymmetric in their intensity. Autoimmune encephalitis may also be associated with speci c cancers (paraneoplastic) and onconeuronal antibodies. In ection caused by the ameba Naegleria owleri can also cause acute meningoencephalitis (primary amebic meningoencephalitis), whereas that caused by Acanthamoeba and Balamuthia more typically produces subacute or chronic granulomatous amebic meningoencephalitis. In ection has typically occurred in immunocompetent children with a history o swimming in potentially in ected water. There have been an increasing number o cases o Balamuthia mandrillaris amebic encephalitis mimicking acute viral encephalitis in children and immunocompetent adults. This organism has also been associated with encephalitis in recipients o transplanted organs rom a donor with unrecognized in ection. Clues to the diagnosis include a history o raccoon exposure, especially o playing in or eating dirt potentially contaminated with raccoon eces. Signi cant involvement o deep gray matter structures, including the basal ganglia and thalamus, should also suggest possible avivirus in ection. These patients may present clinically with prominent movement disorders (tremor, myoclonus) or parkinsonian eatures. The complete eradication o polio remains an ongoing challenge despite a continuing World Health Organization poliovirus elimination campaign. T ree hundred orty-one cases o polio (almost all due to serotype 1) have been reported in 2013 rom eight countries (Somalia 183 cases, Pakistan 63, Nigeria 51, Kenya 14, Syria 13, A ghanistan 9, Ethiopia 6, and Cameroon 2). There have been small outbreaks o poliomyelitis associated with vaccine strains o virus that have reverted to virulence through mutation or recombination with circulating wild-type enteroviruses in Hispaniola, China, the Philippines, Indonesia, Nigeria, and Madagascar. Epidemiologic actors may provide important clues to the diagnosis o viral meningitis or encephalitis. Particular attention should be paid to the season o the year; the geographic location and travel history; and possible exposure to animal bites or scratches, rodents, and ticks. The classic clinical presentation o encephalitic (urious) rabies is ever, uctuating consciousness, and autonomic hyperactivity. Phobic spasms o the larynx, pharynx, neck muscles, and diaphragm can be triggered by attempts to swallow water (hydrophobia) or by inspiration (aerophobia). Patients may also present with paralytic (dumb) rabies characterized by acute ascending paralysis. Patients present with ocal neurologic de cits, myoclonus, seizures, and hallucinations; phobic spasms are not a typical eature. Diagnosis can be made by nding rabies virus antigen in brain tissue or in the neural innervation o hair ollicles at the nape o the neck. No speci c therapy is available, and cases are almost invariably atal, with isolated survivors having devastating neurologic sequelae. Vital unctions, including respiration and blood pressure, should be monitored continuously and supported as required. In the initial stages o encephalitis, many patients will require care in an intensive care unit. Seizures should be treated with standard anticonvulsant regimens, and prophylactic therapy should be considered in view o the high requency o seizures in severe cases o encephalitis. As with all seriously ill, immobilized patients with altered levels o consciousness, encephalitis patients are at risk or aspiration pneumonia, stasis ulcers and decubiti, contractures, deep venous thrombosis and its complications, and in ections o indwelling lines and catheters. Host cell enzymes then phosphorylate this compound to orm a triphosphate derivative.
He returned to the hospital the next day because of shortness of breath and pleuritic chest pain medicine ketorolac best 250 mg trecator sc. A chest X-ray and findings of a ventilationperfusion scan confirmed the presence of a pulmonary embolism medicine 031 order 250mg trecator sc overnight delivery. Additional laboratory studies for protein C symptoms 9 days after ovulation buy trecator sc 250 mg free shipping, protein S medications without doctors prescription order on line trecator sc, Factor V Leiden and antithrombin were normal treatments for depression buy generic trecator sc 250mg on-line. A peripheral blood smear demonstrates no schistocytes, giant platelets or satellitosis. Activated protein C resistance due to Factor V Leiden is caused by which of the following Which of the following thrombotic disorders is the most common inherited cause of venous thromboembolism Which of the following statements is true of the Prothrombin Gene G20210A mutation The presence of Factor V Leiden mutation in combination with the prothrombin gene mutation confers a twofold thrombotic risk above the risk of a single defect D. Plasma prothrombin concentrations can be used to screen for the prothrombin gene mutation 95. Which is the best treatment option for the hemorrhagic tendency in primary fibrinolysis Which of the following statements is true regarding acquired disorders of fibrinolysis A greater degree of hyperfibrinolysis in severe trauma patients confers a greater risk of survival C. Patients with amyloidosis and hyperfibrinolysis do not respond well to antifibrinolytic therapy 100. Type 1 plasminogen deficiency is associated with the development of ligneous conjunctivitis B. Type 1 plasminogen deficiency is associated with a high risk of recurrent deep venous thromboembolism D. The secondary wave of aggregation is represented by platelet degranulation with recruitment of additional platelet aggregates. E Von Willebrand disease and Bernard-Soulier syndrome are similar in that only ristocetin induced aggregation will be affected. B Scott syndrome is a rare hemorrhagic bleeding disorder characterized by a defective scramblase mechanism that does not expose procoagulant phosphatidylserine to the outer surface of activated platelets. Consequently, coagulation factor complexes cannot assemble without binding to phosphatidylserine. C Glanzmann thrombasthenia is a rare genetic disorder affecting the fibrinogen receptor 23. Fibrinogen is required for normal platelet function, and without fibrinogen, platelets cannot aggregate. Therefore, in a platelet aggregation study, platelets would not aggregate to any of the agonists. Agglutination of platelets can, however, occur in response to ristocetin since fibrinogen is not required for the action of ristocetin. As a result, the only platelet agonist that would show a defect in aggregation would be ristocetin. D the k and angle represent the rate of clot formationthe faster the rate of fibrin generation, the larger the angle. If there are clotting factor deficiencies, it would take longer to form the initial fibrin clot so R time would be prolonged. Fibrinogen is required for platelet aggregation and for construction of the fibrin network. When fibrinogen is low, clot formation is slow, and this is reflected in the low angle and slightly prolonged K time. A Hyperfibrinolytic states occur when there is an increased activation of the fibrinolytic system, which results in or sustains bleeding. Primary fibrinolysis is characterized by excessive fibrinolytic activity that is not associated with thrombotic complications. To perform the test, venous blood is collected into chilled tubes containing trisodium citrate. After centrifuging, the plasma portion of the sample is collected and incubated with acetic acid. A precipitate forms, which is the euglobulin fraction containing, plasminogen, plasminogen activators and fibrinogen, while the supernatant is discarded. The euglobulin precipitate is redissolved in buffer and thrombin is added to form a clot. The time to clot lysis is variable from lab to lab, but for a reference range of 90240 minutes, hyperfibrinolysis. A patient sample is mixed with either calcium or thrombin and the resulting clot is incubated in 5M urea (or 1% monochloracetic acid) for 24 hours. However, if antiplasmin is deficient, the clot can be dissolved by plasmin, and a false positive result will occur. C the thrombin time measures the amount of time it takes for a plasma sample to clot after the addition of thrombin. Elevation of the thrombin time typically implies a quantitative or qualitative defect in fibrinogen. Instead, reptilase, an enzyme derived from the snake Bothrops atrox, is used as a replacement for thrombin. Reptilase cleaves fibrinogen to release fibrinopeptide A only while thrombin releases both fibrinopeptides A and B. A A neonate may have elevated reptilase and thrombin times because neonatal fibrinogen differs from adult fibrinogen in its sialic acid content. In this case, the patient developed an antibody to bovine Factor V, which cross-reacted with human Factor V. There have been many reports associated with factor inhibitor formation after the use of topical bovine thrombin. D the following tests are used to distinguish among the many types of Von Willebrand diseases based on quantitative versus qualitative measurements. A Differentiating between these two entities is tricky because they have similar phenotypic parameters and clinical symptoms. C the activated clotting time is a point-of-care clotting test where whole blood is collected into a tube with a coagulation activator (kaolin, celite or glass particles) and magnetic stir bar. It is used in situations where high-dose heparin therapy is needed like cardiopulmonary bypass. D the anti-Factor Xa assay is typically chromogenic but clotting-based assays are also available. In the chromogenic version, a standard curve is produced by combining known amounts of heparin to Factor Xa substrate with chromophore attached. The basic principle of the test is that Factor X cleaves the Factor Xa substrate, releasing chromophore and undergoing a color change that can be quantified. By comparing the results to the standard curve, the heparin concentration in the plasma can be calculated. In contrast, a person with the Factor V Leiden mutation will not have as prolonged a clotting time. Thus, a normal patient will have a higher ratio compared to those with Factor V Leiden mutations. In antithrombin deficiency, there is rapid thrombin generation, leading to faster overall clot development. Other diseases demonstrating enzymatic hypercoagulability include activated protein C resistance and a Factor V Leiden defect. Seroconversion after an initially negative test is almost always associated with clinically irrelevant antibodies. A There are two classes of assays for detecting antiphospholipid antibodies: immunoassays and coagulation assays. The two immunoassays used for the detection of antiphospholipid antibodies are anti-2glycoprotein I and anticardiolipin IgG and IgM assays. The dilute Russell viper venom test is a coagulationbased test to detect lupus anticoagulant. D the most sensitive test for the detection of antiphospholipid antibodies is the anticardiolipin IgG/IgM assay while lupus anticoagulant assays are the most specific but least sensitive. A Platelets have alpha granules, delta (dense) granules, lysosomes and peroxisomes. The defect may result in hemolytic anemia, immune thrombocytopenic purpura, neutropenia, arthritis and vasculitis of large and small vessels and damage to kidneys. C May-Hegglin anomaly, Epstein syndrome, Fechtner syndrome and Sebastian syndrome are autosomal dominant macrothrombocytopenias that are all part of a single disorder with a continuous clinical spectrum, ranging from sensorineural hearing loss, cataracts, nephritis and polymorphonuclear Dohle-like bodies. Paris-Trousseau syndrome is caused by an 11q chromosome deletion resulting in congenital anomalies, a mild bleeding tendency, mental retardation, dysmegakaryopoiesis and platelet inclusion bodies. C Von Willebrand disease is the most common inherited bleeding disorder and has an estimated prevalence of 1% in the population. B Post-transfusion purpura is a rare cause of severe thrombocytopenia that typically occurs 512 days after transfusion. It results in microangiopathic hemolytic anemia, thrombocytopenia and acute renal failure. C Uremic platelet dysfunction is often falsely thought to be caused by increased uremia levels. Patients with familial azotemia, an autosomal dominant disorder resulting in high plasma urea levels, have normal in vitro platelet function. A the platelet "function defect" associated with cardiopulmonary bypass is not an intrinsic defect. It occurs because the heparin used during bypass results in inhibition of endogenous thrombin. Aside from the congenital abnormalities, these syndromes are known to cause a mild macrothromboctyopenia. A Platelet-type disorders will generally manifest as mucosal bleeding (petechiae, purpura), moderate bleeding from small wounds and heavy menses. The remaining answer choices represent physical findings caused by coagulation disorders. B Acquired Factor X deficiency classically occurs in amyloidosis and is thought to occur from adsorption of Factor X to amyloid fibrils. That is why it is important to perform testing for protein S at least 10 days after the event. Oral contraceptives, estrogen use, warfarin and vitamin K all decrease the level of protein S. This increase in free protein S, however, does not have an increased predilection for bleeding. A definitive diagnosis is established by using high molecular weight kininogen deficient plasma. Bacterial infection induces coagulation directly via induction of tissue factor on endothelial cells and mononuclear cells. There can be either bleeding or thrombosis but this is not common as nearly 55% have no symptoms. B Heparin inhibits thrombin and Factor Xa indirectly by binding to and enhancing the activity of antithrombin. The typical course in heparin naïve patients is a platelet count drop of >50% or <150 × 109/L beginning 514 days after heparin exposure. Thrombocytopenia may be isolated or in conjunction with arterial and/or venous thrombosis. In this patient, physical examination did not exhibit splenomegaly so (A) is incorrect. However, the platelet count typically drops to less than 10 ×109/L and bleeding often occurs. Mechanical destruction of platelets from the cardiopulmonary bypass circuit typically occurs intraoperatively and reaches the platelet nadir by the second or third day after surgery (answer E) 87. Suitable alternatives include direct thrombin inhibitors, danaproid (an antithrombin-dependent Factor Xa inhibitor) and fondaparinux (a low molecular weight heparin). Thrombotic events typically appear before a tumor would otherwise be detected, therefore, the clinician should focus on investigating an occult malignancy. This defect is known as Factor V Leiden, which occurs in more than 95% of cases and is caused by a point mutation at one of the three arginine cleavage sites in the Factor V gene. E Homocysteinemia is the only one of the listed disorders that is inherited in an autosomal recessive fashion. B the Prothrombin Gene G20210A mutation occurs rarely in nonwhite populations and the highest prevalence is seen in Southern European populations. The occurrence of double heterozygosity of the prothrombin mutation and Factor V Leiden increases the thrombotic risk 35-fold above the risk of a single defect. Although close to 87% of patients with the prothrombin mutation have high plasma prothrombin values, plasma prothrombin concentrations cannot be used to screen for the prothrombin gene mutation since there is significant overlap. The most common site for venous thrombosis is in the deep veins of the lower limbs, while the most common site for arterial thrombosis is the cerebral arterial circulation. Only a small subgroup of patients develop catastrophic antiphospholipid syndrome where clots in multiple vascular beds leads to multiorgan failure and death. On the basis of retrospective control studies, there is an association with increased risk of arterial and venous thrombosis and elevations in homocysteine. D Antifibrinolytics such as aminocaproic acid and tranexamic acid are the best treatment choices during primary hyperfibrinolysis.
Buy trecator sc 250 mg cheap. Go Go Govinda Lyrical Video | OMG (Oh My God) | Sonakshi Sinha Prabhu Deva.
A patient with rontal lobe disease raises potential dilemmas in di erential diagnosis: the abulia and blandness may be misinterpreted as depression medications knee buy trecator sc 250mg online, and the disinhibition as idiopathic mania or acting out medicine park ok discount trecator sc 250mg online. I neuroleptics become absolutely necessary or the control o agitation treatment 4 stomach virus purchase trecator sc 250 mg with visa, atypical neuroleptics are pre erable because o their lower extrapyramidal side e ects symptoms 0f low sodium cheap trecator sc 250mg free shipping. Spontaneous improvement o cognitive de cits due to acute neurologic lesions is common treatment for depression order cheap trecator sc on-line. It is most rapid in the rst ew weeks but may continue or up to 2 years, especially in young individuals with single brain lesions. Some o the initial de cits appear to arise rom remote dys unction (diaschisis) in parts o the brain that are interconnected with the site o initial injury. Improvement in these patients may re ect, at least in part, a normalization o the remote dys unction. Other mechanisms may involve unctional reorganization in surviving neurons adjacent to the injury or the compensatory use o homologous structures. Cognitive rehabilitation proces dures have been used in the treatment o higher cortical de cits. Determining driving competence is challenging, especially in the early stages o dementing diseases. An on-the-road driving test and reports rom amily members may help time decisions related to this very important activity. Some o the de cits described in this chapter are so complex that they may bewilder not only the patient and amily but also the physician. It is imperative to carry out a systematic clinical evaluation to characterize the nature o the de cits and explain them in lay terms to the patient and amily. An enlightened approach to patients with damage to the cerebral cortex requires an understanding o the principles that link neural networks to higher cerebral unctions in health and disease. Mille r Gil Ra b in o vici Ma ria Ca rm e la Ta rta g lia Language and memory are essential human unctions. For the experienced clinician, the recognition o di erent types o language and memory disturbances of en provides essential clues to the anatomic localization and diagnosis o neurologic disorders. This video illustrates classic disorders o language and speech (including the aphasias), memory (the amnesias), and other disorders o cognition that are commonly encountered in clinical practice. More than one-hal o adults in the United States experience at least intermittent sleep disturbance, and only 30% o adult Americans report consistently obtaining a su cient amount o sleep. The Institute o Medicine has estimated that 5070 million Americans su er rom a chronic disorder o sleep and wake ulness, which can adversely a ect daytime unctioning as well as physical and mental health. Over the last 20 years, the eld o sleep medicine has emerged as a distinct specialty in response to the impact o sleep disorders and sleep de ciency on overall health. Sleep deprivation increases the rapidity o sleep onset and both the intensity and amount o slow-wave sleep. N3 sleep is most intense and prominent during childhood, decreasing with puberty and across the second and third decades o li. N3 sleep declines during adulthood to the point where it may be completely absent in older adults. It is the increased requency o awakenings, rather than a decreased ability to all back asleep, that accounts or the increased wake ulness during the sleep episode in older people. In the United States, adults tend to have one consolidated sleep episode each night, although in some cultures sleep may be divided into a mid-a ernoon nap and a shortened night sleep. This pattern changes considerably over the li e span, as in ants and young children sleep considerably more than older people. The continuous recording o these electrophysiologic parameters to de ne sleep and wake ulness is termed polysomnography. Characteristic eatures o sleep in older people include reduction o N3 slow-wave sleep, requent spontaneous awakenings, early sleep onset, and early morning awakening. Sleep deprivation degrades cognitive per ormance, particularly on tests that require continual vigilance. Paradoxically, older people are less vulnerable to the neurobehavioral per ormance impairment induced by acute sleep deprivation than young adults, maintaining their reaction time and sustaining vigilance with ewer lapses o attention. However, it is more di cult or older adults to obtain recovery sleep a er staying awake all night, as the ability to sleep during the daytime declines with age. Because several disorders (see below) also cause sleep ragmentation, it is important that the patient have su cient sleep opportunity (at least 8 h per night) or several nights prior to a diagnostic polysomnogram. There is growing evidence that sleep de ciency in humans may cause glucose intolerance and contribute to the development o diabetes, obesity, and the metabolic syndrome, as well as impaired immune responses, accelerated atherosclerosis, and increased risk o cardiac disease and stroke. For these reasons, the Institute o Medicine declared sleep de ciency and sleep disorders "an unmet public health problem. The ascending arousal neurons use monoamines (norepinephrine, dopamine, serotonin, and histamine), glutamate, or acetylcholine as neurotransmitters to activate their target neurons. Additional arousal-promoting neurons in the hypothalamus use the peptide neurotransmitter orexin (also known as hypocretin, shown in blue) to rein orce activity in the other arousal cell groups. Damage to the arousal system at the level o the rostral pons and lower midbrain causes coma, indicating that the ascending arousal in uence rom this level is critical in maintaining wake ulness. Damage to the hypothalamic branch o the arousal system causes proound sleepiness, but usually not coma. Speci c loss o the orexin neurons produces the sleep disorder narcolepsy (see below). Many sleep-promoting neurons are themselves inhibited by inputs rom the arousal system. This mutual inhibition between the arousal- and sleep-promoting systems orms a neural circuit akin to what electrical engineers call a " ip- op switch. Neurons in the ventrolateral preoptic nucleus, one o the key sleep-promoting sites, are lost during normal human aging, correlating with reduced ability to maintain sleep (sleep ragmentation). The arousal system in the brain (green) includes monoaminergic, glutamatergic, and cholinergic neurons in the brainstem that activate neurons in the hypothalamus, thalamus, basal orebrain, and cerebral cortex. Orexin neurons (blue) in the hypothalamus, which are lost in narcolepsy, rein orce and stabilize arousal by activating other components o the arousal system. The neurochemistry o sleep homeostasis is only partially understood, but with prolonged wake ulness, adenosine levels rise in parts o the brain. Adenosine may act through A1 receptors to directly inhibit many arousal-promoting brain regions. In addition, adenosine promotes sleep through A2a receptors; inhibition o these receptors by ca eine is one o the chie ways in which people ght sleepiness. Other humoral actors, such as prostaglandin D2, have also been implicated in this process. Both adenosine and prostaglandin D2 activate the sleep-promoting neurons in the ventrolateral preoptic nucleus. Allostasis is the physiologic response to a threat that cannot be managed by homeostatic mechanisms. For example, insomnia is very common in patients with anxiety and other psychiatric disorders. Stress-induced insomnia is even more common, a ecting most people at some time in their lives. The limbic areas are not only targets or the arousal system, but they also send excitatory outputs back to the arousal system, which contributes to a vicious cycle o anxiety about wake ulness that makes it more di cult to sleep. However, behavioral approaches (cognitive behavioral therapy and sleep hygiene) that may reduce orebrain limbic activity at bedtime are o en equally or more success ul. Prominent daily variations also occur in endocrine, thermoregulatory, cardiac, pulmonary, renal, immune, gastrointestinal, and neurobehavioral unctions. At the molecular level, endogenous circadian rhythmicity is driven by sel -sustaining transcriptional/translational eedback loops. In evaluating daily rhythms in humans, it is important to distinguish between diurnal components passively evoked by periodic environmental or behavioral changes. While it is now recognized that most cells in the body have circadian clocks that regulate diverse physiologic processes, most o these disparate clocks are unable to maintain the synchronization with each other that is required to produce use ul 24-h rhythms aligned with the external light-dark cycle. The genetically determined period o this endogenous neural oscillator, which averages ~24. Humans are exquisitely sensitive to the resetting e ects o light, particularly the shorter wavelengths (~460500 nm) o the visible spectrum. Small di erences in circadian period contribute to variations in diurnal pre erence in young adults (with the circadian period shorter in those who typically go to bed and rise earlier compared to those who typically go to bed and wake up later), whereas changes in homeostatic sleep regulation may underlie the age-related tendency toward earlier sleep-wake timing. The timing and internal architecture o sleep are directly coupled to the output o the endogenous circadian pacemaker. Paradoxically, the endogenous circadian rhythm or wake propensity peaks just be ore the habitual bedtime, whereas that o sleep propensity peaks near the habitual wake time. These rhythms are thus timed to oppose the rise o sleep tendency throughout the usual waking day and the decline o sleep propensity during the habitual sleep episode, respectively. Misalignment o the endogenous circadian pacemaker with the desired wake-sleep cycle can, there ore, induce insomnia, decreased alertness, and impaired per ormance evident in night-shi workers and airline travelers. During the transitional state (stage N1) between wakeulness and deeper sleep, individuals may respond to aint auditory or visual signals. A er sleep deprivation, such transitions may intrude upon behavioral wake ulness notwithstanding attempts to remain continuously awake (see "Shi Work Disorder," below). Certain disorders may occur during speci c sleep stages and are described below under "Parasomnias. N3 sleep is associated with secretion o growth hormone in men, while sleep in general is associated with augmented secretion o prolactin in both men and women. Sleep onset (and probably N3 sleep) is associated with inhibition o thyroid-stimulating hormone and o the adrenocorticotropic hormonecortisol axis, an e ect that is superimposed on the prominent circadian rhythms in the two systems. Sleep e ciency is highest when the sleep episode coincides with endogenous melatonin secretion. Administration o exogenous melatonin can hasten sleep onset and increase sleep e ciency when administered at a time when endogenous melatonin levels are low, such as in the a ernoon or evening or at the desired bedtime in patients with delayed sleep-wake phase disorder, but it does not increase sleep e ciency i administered when endogenous melatonin levels are elevated. This may explain why melatonin is o en ine ective in the treatment o patients with primary insomnia. In ormation rom a bed partner or amily member is o en help ul because some patients may be unaware o symptoms such as heavy snoring or may underreport symptoms such as alling asleep at work or while driving. Physicians should inquire about when the patient typically goes to bed, when they all asleep and wake up, whether they awaken during sleep, whether they eel rested in the morning, and whether they nap during the day. It is o en help ul or the patient to complete a daily sleep log or 12 weeks to de ne the timing and amounts o sleep. When relevant, the log can also include in ormation on levels o alertness, work times, and drug and alcohol use, including ca eine and hypnotics. Polysomnography is necessary or the diagnosis o several disorders such as sleep apnea, narcolepsy, and periodic limb movement disorder. A conventional polysomnogram per ormed in a clinical sleep laboratory allows measurement o sleep stages, respiratory e ort and air ow, oxygen saturation, limb movements, heart rhythm, and additional parameters. A home sleep test usually ocuses on just respiratory measures and is helpul in patients with a moderate to high likelihood o having obstructive sleep apnea. Sleepy students o en have trouble staying alert and per orming well in school, and sleepy adults struggle to stay awake and ocused on their work. Reaction time is equally impaired by 24 h o sleep loss as by a blood alcohol concentration o 0. First, patients may describe themselves as "sleepy," " atigued," or "tired," and the meanings o these words may di er between patients. For clinical purposes, it is best to use the term "sleepiness" to describe a propensity to all asleep; whereas " atigue" is best used to describe a eeling o low physical or mental energy but without a tendency to actually sleep. Sleepiness is usually most evident when the patient is sedentary, whereas atigue may inter ere with more active pursuits. Sleepiness generally occurs with disorders that reduce the quality or quantity o sleep or that inter ere with the neural mechanisms o arousal, whereas atigue is more common in in ammatory disorders such as cancer, multiple sclerosis (Chap. Second, sleepiness can a ect judgment in a manner analogous to ethanol, such that patients may have limited insight into the condition and the extent o their unctional impairment. Finally, patients may be reluctant to admit that sleepiness is a problem because they may have become un amiliar with eeling ully alert and because sleepiness is sometimes viewed pejoratively as re ecting poor motivation or bad sleep habits. Table 24-1 outlines the diagnostic and therapeutic approach to the patient with a complaint o excessive daytime sleepiness. Speci c areas to be addressed include the occurrence o inadvertent sleep episodes while driving or in other sa etyrelated settings, sleepiness while at work or school (and the relationship o sleepiness to work and school perormance), and the e ect o sleepiness on social and amily li. Standardized questionnaires such as the Epworth Sleepiness Scale are o en used clinically to measure sleepiness. Eliciting a history o daytime sleepiness is usually adequate, but objective quanti cation is sometimes necessary. The test is per ormed a er an overnight polysomnogram to establish that the patient has had an adequate amount o good-quality nighttime sleep. An average sleep latency across the naps o less than 8 min is considered objective evidence o excessive daytime sleepiness. For the sa ety o the individual and the general public, physicians have a responsibility to help manage issues around driving in patients with sleepiness. Legal reporting requirements vary rom state to state, but at a minimum, physicians should in orm sleepy patients about their increased risk o having an accident and advise such patients not to drive a motor vehicle until the sleepiness has been treated e ectively. Insu cient sleep is especially common among shi workers, individuals working multiple jobs, and people in lower socioeconomic groups. Most teenagers need 9 h o sleep, but many ail to get enough sleep because o circadian phase delay, or social pressures to stay up late coupled with early school start times. Late evening light exposure, television viewing, video-gaming, social media, texting, and smartphone use o en delay bedtimes despite the xed, early wake times required or work or school. As is typical with any disorder that causes sleepiness, individuals with chronically insu cient sleep may eel inattentive, irritable, unmotivated, and depressed, and have di culty with school, work, and driving. Individuals di er in their optimal amount o sleep, and it can be help ul to ask how much sleep the patient obtains on a quiet vacation when he or she can sleep without restrictions. Some patients may think that a short amount o sleep is normal or advantageous, and they may not appreciate their biological need or more sleep, especially i co ee and other stimulants mask the sleepiness. A 2-week sleep log documenting the timing o sleep and daily level o alertness is diagnostically use ul and provides help ul eedback or the patient.
Therefore medicine plies proven 250mg trecator sc, it appears that periodontal pathogens often accompany endodontic infections and support the concept that endodonticperiodontal interrelationships are a critical pathway for both diseases medications japan travel purchase generic trecator sc from india. Extrinsic foreign bodies kerafill keratin treatment discount 250 mg trecator sc with visa, including foreign lipids treatment 1860 neurological 250 mg trecator sc buy visa, cellulose granulomas and iatrogenic materials treatment herniated disc buy trecator sc, can cause a direct inflammatory response. The effects include an increase in calcifications, fibrosis and collagen resorption, as well as a direct inflammatory action. At that stage, pathogens leaking from the oral cavity through the accessory canal into the pulp may cause a chronic inflammatory reaction followed by pulpal necrosis. However, as long as the accessory canals are protected by sound cementum, necrosis does not usually occur. Additionally, if the microvasculature of the apical foramen remains intact, the pulp will retain its vitality. The effect of periodontal treatment on the pulp is similar during root surface debridement, or periodontal surgery, if accessory canals are opened to 266 13 Marginal Periodontitis and the Dental Pulp the oral environment. In such cases, pathogenic invasion and secondary inflammation and necrosis of the pulp can occur. Classification There are many ways of classifying the socalled endodonticperiodontal (endoperio) lesions. The combined lesions include: · primary endodontic lesion with secondary periodontal involvement; · primary periodontal lesion with secondary endodontic involvement; · true combined lesions. This classification is based on the theoretical pathways explaining how these lesions are formed. Therefore, it is essential that a gutta-percha cone be inserted into the sinus tract and that one or more radiographs are taken to track the origin of the lesion. The sinus tract extending into the gingival sulcus or furcation usually disappears within a few weeks, once the necrotic pulp has been treated. It is important to recognize that an attempt to provide periodontal treatment for this condition will result in failure if the necrotic pulp has not been diagnosed and treated. The prognosis in this condition depends wholly on the stage of the marginal periodontitis and the efficacy of periodontal treatment. The clinician must also be aware of the radiographic appearance of marginal periodontitis associated with developmental radicular anomalies (see later). When plaque or calculus is encountered on probing, the treatment and prognosis of the tooth are altered; the tooth now requires both endodontic and periodontal treatments. If the endodontic treatment is adequate, prognosis depends on the severity of the marginal periodontal damage and the efficacy of periodontal treatment. With endodontic treatment alone, only part of the lesion will heal to the level of the secondary periodontal lesion. Primary endodontic lesions with secondary periodontal involvement may also occur as a result of root 270 13 Marginal Periodontitis and the Dental Pulp increasing problem with molar teeth that have been treated by root resection. In a study of 100 patients, a total of 38 teeth failed during the 10-year period of observation, and 47% of the failures were a result of root fractures, with the vast majority being in mandibular molar teeth. Symptoms may be acute, with periodontal abscess formation associated with pain, swelling, pus exudation, pocket formation and tooth mobility. A more chronic response may sometimes occur without pain and involves the sudden appearance of a pocket with bleeding on probing, or exudation of pus. When the root perforation is situated close to the alveolar crest, it may be feasible to raise a flap, repair the defect with an appropriate filling material, and subsequently reposition the flap apically to expose the repaired perforation site. In deeper perforations or in the roof of the furcation, immediate internal repair of the perforation and infection control is essential for better prognosis. The signs may range from a local deepening of a periodontal pocket to more acute periodontal abscess formation. In addition, root fractures have become an the apical progression of a periodontal pocket can continue until the apex is reached. In a single-rooted tooth, the prognosis is usually poor, unlike the primary endodontic lesion. In molar teeth, not all roots may suffer the same loss of supporting tissues extending to the apex, in which case the possibility of root resection should be considered. The treatment of marginal periodontitis can also lead to secondary endodontic involvement. For example, a blood vessel within a lateral canal may be severed by a curette during treatment. Additionally, pulp changes resulting from marginal periodontitis were observed when the main apical foramen was involved. There is a correlation between cultivable microorganisms from the root canals of human caries-free teeth with advanced periodontitis and those from associated periodontal pockets. Support for this concept has come from research in which cultured samples obtained from the pulp tissue and radicular dentine of periodontally involved human teeth showed bacterial growth in 87% of the cases. Sometimes, there is lack of correlation between marginal periodontitis and pulp involvement. The prognosis is particularly poor in single rooted teeth, but the situation may be salvaged in molars by sectioning the tooth, if all the roots are not as severely involved. Healing of apical periodontitis may be anticipated after successful endodontic treatment. A fracture that has exposed the pulp space, with resultant necrosis, may also be labelled a true combined lesion and yet not be amenable to successful treatment. On the other hand, in a tooth with primary periodontal lesion, the pulp is vital and responsive to sensitivity testing. However, primary endodontic lesions with secondary periodontal involvement, primary periodontal lesions with secondary endodontic involvement, or true combined lesions may be clinically and radiographically very similar. The degree of healing that has taken place after root canal treatment will determine the retrospective classification. The main factors to consider, at the time of diagnosis, are pulp vitality and type and extent of the periodontal defect. Primary endodontic lesion should only be managed by endodontic treatment, and the prognosis is good. Primary endodontic lesions with secondary periodontal involvement should first be managed with endodontic treatment. The treatment results should be evaluated in 2 to 3 months and only then should periodontal treatment be considered. This sequence of treatment allows sufficient time for initial tissue healing and better assessment of the periodontal condition. In this regard, it has been suggested that during interim endodontic treatment, aggressive removal of the periodontal ligament and underlying cementum will adversely affect periodontal healing1; areas of the roots that were not aggressively treated showed unremarkable healing. Primary periodontal lesions with secondary endodontic involvement and true combined endodonticperiodontal lesions require both endodontic and periodontal treatments. It has been demonstrated that intrapulpal infection tends to promote marginal epithelial downgrowth along a denuded dentine surface. In general, assuming the endodontic treatment is adequate, the lesion of endodontic origin will heal. Thus, the prognosis of combined diseases is dependent on the efficacy of periodontal treatment. These grooves usually begin in the central fossa of maxillary central, or lateral, incisors, over the cingulum, and continue apically down the root for varying distances. Such a groove is apparently the result of an attempt by the tooth germ to form another root. This fissure-like channel may provide a nidus for biofilm formation and infection, and an avenue for the progression of marginal periodontitis. From the time the tooth develops with this anomalous root defect, the potential for isolated marginal periodontitis exists. As long as the epithelial attachment remains intact, the periodontium remains healthy. In selected cases, radicular grooves can be treated satisfactorily and maintained. The clinician must look for the groove because it may have been altered by a previous restoration on the palatal surface. The use of an operating microscope during clinical examination is advantageous because of enhanced magnification and illumination. If the condition is purely periodontal, it can be diagnosed visually by following the groove to the gingival sulcus and probing the depth of the pocket. This pocket is usually tubular and isolated, as opposed to a more generalized periodontal condition. If this entity is also associated with pulp infection, the patient may present with endodontic symptoms, and the results of pulp sensitivity testing will not be normal. Bone destruction that follows the groove longitudinally may be apparent radiographically. The appearance of a teardrop-shaped area on the radiograph should also arouse suspicion. The developmental groove may actually be visible on the radiograph; if so, it will appear as a dark longitudinal line. This condition must be differentiated from a longitudinal fracture, which may give a similar radiographic appearance. The essential problem is the need to eliminate the pathway of infection resulting from the presence of the anatomical radicular anomaly. The prognosis is improved if the condition is diagnosed and treated early, but its management remains challenging. Although the acute nature of the problem may be alleviated initially, the reason for the inflammation must be eradicated by cutting out the groove and surgical management of the tissues. This can be combined with placement of a biocompatible material in an attempt to improve success. However, if the prognosis appears poor, early extraction is advisable to avoid compromising future implant treatment. Combined management includes endodontic treatment, atraumatic extraction, groove reduction, Emdogain application and tooth reimplantation. Tooth resection involves the removal of one, or more, roots of a tooth along with their coronal part(s); it is sometimes referred to as hemisection. Bicuspidization is the separation of a multirooted tooth by a vertical cut through the furcation. Indications for root amputation or tooth resection include: · Advanced marginal periodontitis. The pattern of alveolar bone loss in marginal periodontitis may affect the different roots of a molar tooth unequally. If left untreated, the adjacent healthier root support could, eventually, become involved by direct extension of the periodontal lesion, 278 13 Marginal Periodontitis and the Dental Pulp resulting in poorer prognosis. Removal of the offending root(s) allows the well-supported part of the tooth to be retained as a functional unit, resulting in healthy tissues and a normal radiographic appearance. The morphology of the distobuccal root of the maxillary first molar and the mesiobuccal root of the second molar often tend to flare toward each other. Marginal periodontitis in these sites may lead to angular bone loss, which is difficult to treat and leaves the patient with a plaque control management problem. Indications for bicuspidization include: · Gross perforation in the furcation area. This makes periodontal treatment and home maintenance by the patient more difficult. Contraindications for anatomical redesigning include: · Poor plaque control and an unmotivated patient. This is particularly important if there was no improvement after initial periodontal treatment. This relates to all remaining roots of the involved tooth, particularly, if it serves as an abutment for fixed prosthodontics. A special clinical situation with a more favourable prognosis exists when there is only apical fusion and adequate interradicular bone, allowing for surgical root removal. The furcation area is situated so far apically that considerable supporting bone would need to be sacrificed. This may preclude the formation of a functional band of attached gingiva around the remaining roots. Coronal reshaping and buccolingual narrowing to reduce the occlusal table should also be performed to redirect occlusal forces to the remaining solid roots. The need for root removal may become apparent during diagnosis and treatment planning instead of treating roots with extensive periodontal breakdown. Root canal treatment is completed, and a permanent restorative material placed in the pulp chamber and coronal entrance of the root to be amputated, so that the root end is already sealed when the root is removed. A full-thickness mucoperiosteal flap is reflected to expose the furcation area, which is carefully explored with a periodontal probe to ensure that the furcation has not been exposed on all three surfaces. If so, tooth resection is required, leaving one root in situ; otherwise, the tooth would need to be extracted. The cut in the root is made with a long thin bur, long enough to reach from one side of the root to the other. Care must be taken to maintain the correct angulation of the bur, so as not to damage the remaining root(s) or the crown. Removal of some of the buccal cortical plate of bone may be required so that the separated root can be gently elevated out of its socket, without undue pressure being applied to the adjacent tooth or bone. Once the root has been removed, the area of the stump is reshaped with burs, so that it blends imperceptibly into the remaining tooth structure. The periodontal condition is reevaluated approximately 3 months after root removal. If the mucogingival and osseous deformities still remain, definitive periodontal surgery should be carried out. An alternative treatment modality allows for root amputation to be performed at the time of periodontal surgery; this has the advantage of combining both stages into only one surgical procedure.
References
- Serefoglu EC, Silay MS: Botulinum toxin-A injection may be beneficial in the treatment of life-long premature ejaculation, Med Hypotheses 74(1):83n84, 2010.
- Wang A, Rana S, Karumanchi SA. Preeclampsia: the role of angiogenic factors in its pathogenesis. Physiology (Bethesda) 2009;24:147-158.
- Vitiello MV, et al. Rapid eye movement sleep measures of Alzheimeris-type dementia patients and optimally healthy aged individuals. Biol Psychiatry 1984;19(5):721-34.
- Cunha R, Donjacour A: Stromal-epithelial interactions in normal and abnormal prostatic development, Prog Clin Biol Res 239:251n272, 1987.
- Hebert PC, Wells G, Blajchman MA, et al: A multicenter, randomized, controlled clinical trial of transfusion requirements in critical care. Transfusion Requirements in Critical Care Investigators, Canadian Critical Care Trials Group, N Engl J Med 340:409-417, 1999.
