
Unisom
| Contato
Página Inicial
David Burt, MD
- Assistant Professor, Medical Director, Chest Pain Center, Department of
- Emergency Medicine, University of Virginia, Charlottesville, VA, USA
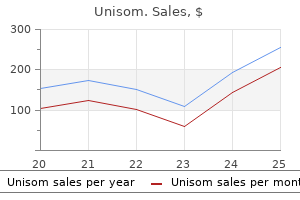
Bacteria are cultured from the bile in approximately one-half of patients with gallstones, and unrelieved obstruction in the presence of this infected bile may produce an empyema insomnia 58 order unisom in united states online. The persistently obstructed gallbladder becomes intensely inflamed and oedematous sleep aid 25mg review cheap unisom 25 mg free shipping. If the obstruction fails to resolve the transmural pressure in the wall of the gallbladder can result in venous ischaemia, leading to gangrene and or perforation insomnia history purchase 25 mg unisom. Perforation may be contained by the liver or surrounding viscera leading to localised abscess formation or may result in biliary peritonitis insomnia 8 months pregnant buy unisom online. Common clinical syndromes associated with gallstones the majority of individuals with gallstones are asymptomatic or have only vague symptoms of distension and flatulence insomnia music buy 25 mg unisom fast delivery. Less than a fifth of such patients develop symptoms or complications from their gallstones within 10 years. The imprisoned bile is absorbed, but clear mucus continues to be secreted into the distended gallbladder. Biliary colic Biliary colic is due to transient obstruction of the gallbladder from an impacted stone. There is severe gripping pain, often developing after meals or in the evening, which is maximal in the epigastrium and right hypochondrium with radiation to the back. Despite being continuous, the pain may wax and wane in intensity over several hours, and vomiting and retching are common. Resolution occurs when the stone falls back into the gallbladder lumen or passes onwards into the common bile duct. In some patients, the obstruction does not resolve and the patient develops acute cholecystitis. Chronic cholecystitis Repeated bouts of transient gallbladder obstruction (biliary colic) or acute cholecystitis culminate in fibrosis, contraction of the gallbladder and chronic inflammatory change with marked thickening of the wall. Chronic inflammatory change may be present in the absence of gallstones, as is the case in the gallbladders of typhoid carriers. The incidence of carcinoma of the gallbladder is increased in patients with longstanding gallstones. Acute cholecystitis Fistulation When large gallstones are present for a long time they can erode by the effect of pressure through the wall of the gallbladder into surrounding structures. Those eroding into the duodenum can pass into the small bowel, resulting in mechanical small bowel obstruction known as gallstone ileus. It usually begins with an attack of biliary colic, although its onset may be more gradual. There is severe right hypochondrial pain radiating to the right subscapular region, and occasionally to the right shoulder, together with tachycardia, pyrexia, nausea, vomiting and leucocytosis. The pain in acute cholecystitis is usually constant and continues for 24 hours or more, differentiating this from biliary colic where pain is short-lasting. Abdominal tenderness and rigidity may be generalised but are most marked over the gallbladder. In the remainder, tenderness may spread and pyrexia and tachycardia Choledocholithiasis When gallstones (usually small) enter the common bile duct via the cystic duct, they may pass spontaneously or give rise to obstructive jaundice, cholangitis or acute pancreatitis. Gallstone pancreatitis most commonly occurs when a small stone becomes temporarily arrested at the ampulla of Vater. The development of a tender mass, associated with rigors and marked pyrexia, signals empyema formation. The gallbladder may become gangrenous and perforate, giving rise to biliary peritonitis. Usually, this is associated with stones in the common bile duct, but compression of the bile ducts due to surrounding inflammation may be responsible. Acute cholecystitis must be differentiated from perforated peptic ulcer, high retrocaecal appendicitis, acute pancreatitis, myocardial infarction and basal pneumonia. Acute cholecystitis can develop in the absence of gallstones (acalculous cholecystitis), although this is rare. Chronic cholecystitis Chronic cholecystitis is the most common cause of symptomatic gallbladder disease. The patient gives a history of recurrent flatulence, fatty food intolerance and right upper quadrant pain. The pain is worse after meals and is often associated with a feeling of distension and heartburn. The differential diagnosis includes duodenal ulcer, hiatus hernia, myocardial ischaemia, chronic pancreatitis and gastrointestinal neoplasia. Symptoms for mucocoele are the same as those for chronic cholecystitis but a nontender piriform swelling may be palpable in the right hypochondrium. Management of acute cholecystitis Patients with acute cholecystitis are admitted to hospital to be monitored; analgesics, intravenous fluid and a broad-spectrum antibiotic such as a cephalosporin are prescribed. The duration of the illness and hospitalisation is reduced, and further attacks of acute cholecystitis during the waiting period for elective surgery are averted. In hospitals serving populations with a high burden of disease, dedicated processes, access to appropriate investigations and facilities alongside experienced surgical staff are key requirements for successfully managing these patients via an acute pathway. Choledocholithiasis Stones may be present in the common bile duct of some 510% of patients with gallstones. There is little muscle in the wall of the bile duct, and pain is not a symptom unless the stone impedes flow through the sphincter of Oddi. Impaction of a stone at the sphincter obstructs the flow of bile, producing jaundice, pale stools and dark urine. Obstruction commonly persists for several days but may clear spontaneously, as a result either of passage of the stone or of its disimpaction. In longstanding obstruction the bile ducts become markedly dilated and the diameter of the common bile duct may exceed its upper limit of 7 mm. Long-standing intermittent biliary obstruction may lead to secondary biliary cirrhosis. Obstructive jaundice due to stones in the common bile duct has to be distinguished from other causes of obstructive jaundice, notably malignant obstruction and cholestatic jaundice. Acute viral or alcoholic hepatitis may occasionally be confused with obstructive jaundice. Acute pancreatitis may be associated with a stone in the common bile duct (Chapter 15). Simply stated, if the gallbladder is palpable in the presence of jaundice, the jaundice is unlikely to be due to stone and one should think of a malignant cause of the lower extrahepatic biliary tree. However, exceptions to the law are due to double impaction of the cystic duct and the common bile duct due to stone, pancreatic duct calculi, and worm-induced obstruction (ascaris or clonorchis). Distended gallbladders are not always easy to feel but can be detected readily by ultrasound. If the patient is unfit for surgery, has a delayed presentation or disease severity suggests surrounding inflammation, this will make identification of the relevant anatomical structures difficult. Ultrasound-guided percutaneous drainage of the gallbladder may be performed as an interim measure. Adenomyomatosis this rare condition is characterised by mucosal diverticula (RokitanskyAschoff sinuses) that particularly affect the fundus and penetrate the muscular layers to the serosa. Clinical presentation can mimic chronic cholecystitis while radiologically it may raise concern about the presence of a gallbladder tumor. The diagnosis may be made on careful imaging but is often only made following cholecystectomy, as the gallbladder normally contains stones. Acute acalculous cholecystitis Few patients with acute cholecystitis have acalculous inflammation. The condition may be precipitated by major surgery, bacteraemia, trauma, pancreatitis or other serious illness, and may complicate parenteral nutrition. The inflammatory reaction in the gallbladder wall may be intense and severe, leading to gangrene and perforation. In ill patients, percutaneous drainage (cholecystostomy) under ultrasound guidance may be considered, but urgent cholecystectomy is often advisable. Complications occur in up to 7% of patients and may include cholangitis, bleeding and acute pancreatitis. Patients with asymptomatic gallstones are treated expectantly, particularly if they are elderly or suffering from medical conditions likely to increase the risk of surgery. In younger patients, there may be a stronger case for surgery despite the absence of symptoms, particularly if the stones are multiple and likely to cause complications, such as acute pancreatitis or there is a high underlying prevalence of gallbladder cancer within the population being treated. Investigation of patients with suspected gallstones Blood tests A full blood count may reveal a neutrophilia in acute cholecystitis or its complications. An elevated serum bilirubin or alkaline phosphatase may signify the presence of common duct stones. Plain abdominal x-ray As only 15% of gallstones contain enough calcium to be seen on a plain radiograph, this investigation is not used in diagnosis. Gas is rarely seen outlining the biliary tree if there is a fistula between the biliary tract and the gut, as in gallstone ileus or following endoscopic sphincterotomy. Stones reflect the ultrasonic wave and are thrown into prominence by the acoustic shadow they produce. As it does not depend on hepatic excretion of contrast, it can be used in both jaundiced and nonjaundiced patients. However, it cannot accurately assess the common bile duct with regard to the presence or absence of stones. Once a patient with gallstones becomes symptomatic, elective day case laparoscopic cholecystectomy is indicated. For those patients with common bile duct stones duct clearance and cholecystectomy should be considered irrespective of symptoms. Common bile duct stones can be removed by the principles of surgical treatment involve removal of the gallbladder and the stones it contains, while ensuring that no stones remain within the ductal system. Conversion from a laparoscopic procedure to open cholecystectomy should be seen as a limitation of the minimally invasive technique and not as a failure of the surgeon. Injury to the bile duct during cholecystectomy requires immediate referral to a surgeon or service specialised in the management of such a complication. Open cholecystectomy the gallbladder is usually approached through a right subcostal incision. The peritoneal layer can gently be incised with minimal diathermy and then blunt dissected to expose the contents of the hepatobiliary triangle; this can be repeated for the posterior surface. With the cystic duct and artery clearly identified and skeletonised, intraoperative cholangiography is performed under image intensification by cannulating the cystic duct and following the injection of contrast. The cholangiogram displays the anatomy of the duct system, identifies ductal stones, and confirms that contrast passes freely into the duodenum. The cystic duct and artery are ligated and divided and the gallbladder is removed. The surgeon must be very aware of the possibility of fibrosis having drawn in the right portal structures such that they are easily damaged during such dissection. Here the peritoneal surface of the gallbladder is incised well clear of any potential portal structures, all stones evacuated and the cystic duct orifice identified from within the gallbladder and safely oversewn. Some surgeons pursue a policy of selective cholangiography, obtaining a cholangiogram only in patients at high risk of having ductal stones. The intra- and extrahepatic ducts are seen and there is flow of contrast into the duodenum. A small radiolucent calculus is present at the lower end of the common bile duct (arrow). This is a warning sign of severe fibrosis and this situation presents a high risk of duct injury if attempts are made to dissect the hepatobiliary triangle or perform fundus-first cholecystectomy. A safer option is to open the gallbladder as seen here and extract the stones and drain the gallbladder remnant. In event of biliary fistula it can be controlled by endoscopic retrograde cholangiopancreatography and stenting. The value of routinely placing an abdominal drain has been questioned although its use in difficult surgery may prevent the development of a collection and identify leakage of bile. The gallbladder and bile ducts · 227 Laparoscopic cholecystectomy Laparoscopic cholecystectomy is now the treatment of choice for symptomatic gallstones, despite having a significantly higher risk of major bile duct injury. Thus it is crucial surgeons performing such surgery create a culture of safety by understanding the steps required for safe cholecystectomy and understanding factors that contribute to bile duct injury. This posterior dissection is a key difference to the open approach to cholecystectomy. This peritoneal surface is released and any loose areolar tissue cleared from the hepatobiliary triangle including up to the base of the liver. The key to avoiding bile duct injury is recognising when it is not safe to persist in trying to obtain the critical view. Opinions vary as to whether intraoperative cholangiography should be undertaken routinely to detect such stones · In the era of laparoscopic cholecystectomy, there is a growing tendency not to perform routine operative cholangiography, and to extract symptomatic duct stones by nonoperative means. At open or laparoscopic surgery, if stones are detected in the main duct system a decision with regard to definitive management needs to be made. In a small nondilated duct a choledochotomy (opening common bile duct) is to be avoided due to risk of postprocedure stricture. Options include flushing the duct with saline after administration of pharmacological smooth muscle relaxants such as glucagon. Transcystic exploration can also be performed using baskets or balloons under radiological guidance or via a fine choledochoscope. In situations where the common bile duct is dilated, a choledochotomy can be performed. Following exploration, a further check cholangiogram or direct inspection with a fibreoptic choledochoscope should be performed to confirm clearance. A small lateral injury can be managed by biliary decompression with either placement of a T-tube or antegrade stent.
The overall 5-year survival rate remains low (<10%), although 5-year survival figures of 2030% are reported when resection is feasible all natural sleep aid 3 ingredients order unisom 25 mg line. Multimodal therapy involving perioperative chemotherapy and surgery is the standard of care when the treatment intent is curative insomnia band unisom 25 mg buy overnight delivery. A multidisciplinary team (consisting of surgeons, endoscopists, radiation and medical oncologists, pathologists, palliative care physicians and nutritional therapists) must be involved in the management in a high volume cancer centre quick sleep aid quality unisom 25 mg. Surgical resection Oesophagectomy with palliative intent is not appropriate as few patients recover enough to gain any benefit before they die of their disease insomnia got me like purchase unisom on line amex. Palliative oesophagectomy may have to be offered if stenting is not available in developing countries if the patient is fit sleep aid quetiapine purchase 25 mg unisom with mastercard. A right thoracotomy is carried out to resect the oesophagus, and the mobilised stomach is brought up into the chest and anastomosed to the proximal oesophagus. Once the oesophagus is removed, the stomach is brought up into the neck and anastomosed to the cervical oesophagus. This technique is appropriate for tumours of the lower third where adequate lymphadenectomy is possible. Clinical features Progressive dysphagia to solids, then liquids, is the most common presentation along with regurgitation and weight loss. The average duration of symptoms at the time of presentation is between 3 and 9 months, and as a result, around 70% of patients are not operable at the time of diagnosis. The advantages are avoidance of an anastomosis in the chest with its potential complications, and the ability to tackle mid- and upper-oesophageal malignancies due to the high proximal clearance achieved along with adequate lymphadenectomy. Increasingly surgeons are using laparoscopic and thoracoscopic techniques to mobilise the oesophagus. Alternatively, both the abdominal and chest phase of the surgery can be done using minimally invasive techniques. Current randomised clinical trials will determine the most effective combination of agents. Chemoradiotherapy can also be used preoperatively, particularly for squamous carcinoma of the oesophagus although postoperative complications for these patients may be higher. Up to a third of patients will have a complete pathological response (no residual tumour when resected) and this has prompted trials of chemoradiotherapy as definitive treatment in squamous cell carcinoma. Postoperative care Uncomplicated recovery after oesophagectomy hinges on good surgical technique, good pain relief (often by epidural analgesia), avoidance of excess intravenous fluid, early mobilisation and effective chest physiotherapy. Many surgeons place a feeding jejunostomy at the time of oesophagectomy to allow early enteral feeding. Palliation the majority of patients (about 70%) will have palliative rather than curative treatment. A full range of palliative treatments must be available and an experienced hospital clinician with good specialist nurse support should coordinate care, working closely with community services. Diagnosis and management: gastroduodenal · 193 Diagnosis and management: gastroduodenal Peptic ulceration Peptic ulceration affects areas of mucosa exposed to acidic gastric contents. The main pathology is an imbalance between the acidpepsin system and the mucosal ability to resist digestion. Pathology Duodenal ulcers usually occur in the first part of the duodenum and 50% occur on the anterior wall. The majority of gastric ulcers develop on the lesser curvature in the distal half of the stomach. Malignancy was once thought to be a complicating factor of benign gastric ulceration but malignant change in a benign ulcer is rare, and such ulcers are probably malignant from the outset. Best supportive care: Some patients are too frail for any interventional treatment and require a holistic approach to their symptoms involving medication to counter nausea, vomiting and pain. Endoscopic stent: Patients with significant dysphagia should be considered for a palliative stent as this is a safe and effective method of relieving the distress of not being able to swallow. These are inserted under intravenous sedation endoscopically but can also be screened into position by interventional radiologists. Complications include perforation during insertion, migration of the stent, blockage and tumour ingrowth. Stents cannot be used for very proximal tumours involving the cervical oesophagus. Palliative radiotherapy and brachytherapy: Intraluminal radiotherapy (brachytherapy) has been shown to provide a better quality of life for patients with incurable oesophageal cancer than a stent. External beam radiotherapy can provide good palliative care for squamous oesophageal carcinoma but requires more visits by the patient to hospital. It is more prevalent in developing countries, where poor and crowded living conditions are commonplace, and here the infection is probably acquired in early life via the faecaloral or oraloral route. It infects the antral mucosa of the stomach, where it causes an inflammatory response. This gastritis stimulates the gastrinproducing (G) cells of the antrum to increase gastrin production. The subsequent hypersecretion of acid provides an ideal environment for gastric metaplasia of the duodenal mucosa to occur. It may be that the gastritis facilitates the access of acid and pepsin to the stomach mucosa. It seems that the key factor is decreased mucosal resistance, with excess acid having less of a role. Most patients with gastric ulceration have a normal or decreased secretory capacity. Ulcers resulting from hypersecretion are usually single and, in common with other forms of peptic ulceration, may be complicated by perforation and bleeding. Clinical features Recurrent well-localised epigastric pain is typical of peptic ulcer disease. Classically, the pain of a gastric ulcer occurs during eating and is relieved by vomiting. Patients with duodenal ulceration characteristically describe pain when they are hungry. Often, however, these well-defined features are not present, and it is usually impossible to differentiate between the symptoms of gastric and duodenal ulceration. Other symptoms associated with peptic ulcer disease include heartburn, anorexia, waterbrash (a sudden flow of saliva into the mouth) and intolerance of certain foods. Where persistent vomiting is troublesome, the possibility of gastric outlet obstruction should be considered. Such vomiting may be projectile and contain recognisable undigested food eaten many hours previously. In the stomach, prostaglandins are responsible for the production of mucus and bicarbonate, which both help to protect the stomach mucosa from acid by maintaining an alkaline buffer zone. Smoking this aetiological factor is more important in gastric than duodenal ulceration. Diagnosis As already described, endoscopy and biopsy is essential in the diagnosis of peptic ulceration. Biopsy of gastric ulcers is particularly important, as malignancy needs to be excluded. Genetic factors First-degree relatives of patients with a duodenal ulcer are at increased risk of developing a duodenal ulcer themselves. This risk is further increased if ulcers develop in patients under 20 years of age. First-degree relatives of patients with gastric ulcers are also at increased risk of developing gastric ulcers. ZollingerEllison syndrome this rare syndrome is caused by a gastrin-secreting tumour (gastrinoma) that is normally found in the pancreas but may occasionally be found in the duodenum or stomach. Diarrhoea may be a prominent feature, owing to large volumes of acid being secreted into the small intestine. The diagnosis of ZollingerEllison is problematic, but ulceration in unusual sites, at an early age, or ulcers persisting despite medical treatment should be reviewed with a high index of suspicion and serum gastrin measured. Eradication rates of greater than 90% occur with good compliance, although reinfection following successful eradication is possible. Without eradication therapy, approximately 80% of ulcers will recur within 1 year. Other factors Other patients at risk of peptic ulceration include those with blood group O and those with hyperparathyroidism. Hyperparathyroidism causes elevated calcium levels, thus stimulating acid secretion. With treatment of the underlying condition, spontaneous ulcer healing usually occurs. Severe illness, trauma, prolonged mechanical ventilation, multiple organ failure, sepsis and major surgery may give rise to stress ulceration. In preventing duodenal ulcer recurrence, eradication therapy was similar to maintenance acid-lowering drugs, but eradication therapy was superior to no treatment. In preventing gastric ulcer recurrence, eradication therapy was superior to no treatment. Benign distal ulcers may be treated by a Billroth I gastrectomy, whereby the distal part of the stomach is removed and the proximal stump anastomosed to the duodenum. More proximal ulcers usually necessitate a Polya-type reconstruction involving anastomosis of the gastric remnant to the jejunum. Many patients who had surgery for ulcer disease in the 1960s and 70s are still alive today and suffer long-term side effects similar to those experienced by patients having a gastrectomy for cancer such as dumping syndrome, abdominal pain after eating and diarrhoea. Without eradication, the relapse rate is in the region of 50%, but this falls to less than 10% with successful eradication therapy. Endoscopic surveillance of a treated ulcer should continue until healing is complete. Complications of peptic ulceration requiring operative intervention the complications that necessitate surgery include: · perforation · bleeding · obstruction. Perforation Duodenal ulcers Up to 50% of patients will have had no previous ulcer symptoms and for this reason duodenal ulcer perforation remains a common surgical emergency. The overall incidence of duodenal ulcer perforation is decreasing, probably due in part to improvements in the medical management of duodenal ulcers. Surgical management Duodenal ulceration Surgery for uncomplicated duodenal ulceration is now extremely rare. Operations such as a truncal vagotomy, highly selective vagotomy, or gastric resectional surgery have had little role since the introduction of eradication therapy. When combined they had the lowest recurrence rates at the cost of increased morbidity and mortality. Definitive procedures for peptic ulcer in the setting of perforated peptic ulcer are not recommended today. Gastric ulcers Gastric ulcer perforation is less common than duodenal ulcer perforation. It has a peak incidence in the elderly, and consequently the associated morbidity and mortality are higher. Gastric ulceration Failure of conservative therapy to heal a gastric ulcer is an indication for surgical intervention. Where malignancy cannot be excluded or is suspected, resection of the ulcer is the treatment of choice. The extent and type of resection will be determined by the position of the ulcer within the stomach and its suspected malignant potential. Clinical features the acute onset of severe unremitting epigastric pain is strongly suggestive of the possibility of perforation. Irritant stomach contents in the peritoneal cavity may give rise to shoulder-tip pain, resulting from diaphragmatic irritation. The abdomen does not move freely with respiration, and marked tenderness, guarding, fear of movement and board-like rigidity may be found on examination. Shock is frequently seen in patients presenting late in a moribund state, especially in the developing world. Generalised peritonitis does not occur in some patients because the perforation seals over with omentum. In others, the fluid tracks down the right paracolic gutter, simulating acute appendicitis. Silent perforations may also occur, and are only found incidentally on a chest x-ray. Omentum Diagnosis In 60% of cases of perforation, an erect chest x-ray will demonstrate free air under the diaphragm, although the absence of free air does not exclude a perforation. A lateral decubitus film can be useful where an erect chest x-ray is not feasible. Moderate hyperamylasaemia may be found with a perforated duodenal ulcer but high amylase levels are more suggestive of acute pancreatitis. Management the initial management, as for other causes of peritonitis, consists of resuscitation, oxygen therapy, intravenous fluids, broadspectrum antibiotics, and the passage of a nasogastric tube. Operative management is usually indicated although patients who do not have generalised peritoneal signs or systemic sepsis may be successfully managed conservatively so long as frequent reassessment shows no deterioration in their condition. Surgeons are increasingly using a laparoscopic approach to treatment but open surgery should not be considered inferior. Acute haemorrhage the differential diagnosis of upper gastrointestinal bleeding is summarised in Table 13. Upper gastrointestinal bleeding presents with haematemesis (vomiting blood) and/or melaena (the passage of black tarry stool that has a very characteristic smell). Melaena results from the digestion of blood by enzymes and Duodenal ulcers Surgery involves simple closure, whereby the ulcer is plugged using a pedicled omental patch.
If our patient were focused on a goal of pain elimination sleep aid for 9 month old discount 25 mg unisom, chances are he would never experience total success insomnia movie review 25 mg unisom purchase fast delivery. However insomnia night sweats cheap unisom 25 mg online, he can learn how to not suffer in response to the pain and experience success in a different way insomnia yoga 25 mg unisom for sale. Helping him understand that he is responsible for the hands-on management of his pain under the direction of his physician is critical xanax sleep aid dose buy unisom 25 mg amex. Just as the individual with diabetes is responsible for proper blood testing, administration of insulin, and adherence to nutritional guidelines, so must the patient with persistent pain learn to be responsible for managing his condition as well. The fourth focus is threshold management, helping our patient understand how to pace himself, conserve energy, and build stamina and endurance. Many individuals believe that they should pace activity by monitoring pain and stopping what they are doing when the pain increases. In any event, we know, given his condition, that he has to learn how to vary the biomechanical demands on his body and avoid extended periods of holding patterns and immobility. The fifth focus of treatment concerns the arena of performance enhancement, helping the patient identify life goals, work tasks, and activities of daily living that he wants to engage in and helping him problem-solve how to accomplish them. Sometimes this is through making accommodations, using assistive devices, or maintaining and adhering to his exercise regimen program. An ergonomic assessment of his workstation may be helpful in maintaining neutral postures and providing good postural alignment. Given how much writing an attorney does, it would be very useful to ensure that he is dictating with a wireless headset so that he can stand while working or even to get a flexible workstation desk that can accommodate standing as well as sitting. In addition, our patient can be taught mental practice techniques 91 to assist with flexibility and increased range of motion. Enthesitis and ankylosis in spondyloarthropathy: what is the target of the immune response? Van Tubergen A, Coenen J, Landewe R, Spoorenberg A, Chonis A, Boonen A, van der Linden s, van der Heijde D. Assessment of fatigue in patients with ankylosing spondylitis: a psychometric analysis. Fatigue inpatients with ankylosing spondylitis: a comparison with the general population and associations with clinical and self-reported measure. Estimates of the prevalence of arthritis and other rheumatic conditions in the United States. Identifying patients with axial spondyloarthritis in primary care: how useful are items indicative of inflammatory back pain? A comparison of patients with spondyloarthropathy seen in specialty clinics with those identified in a communitywide epidemiologic study. The European Spondyloarthropathy Study Group preliminary criteria for the classification of spondyloarthropathy. Relative value of erythrocyte sedimentation rate and C-reactive protein in assessment of disease activity in ankylosing spondylitis. Prospective evaluation of sacroiliac scintigraphy in chronic inflammatory back pain. Investigation of sacroiliac disease: comparative evaluation of radiological and radionuclide techniques. Early detection of sacroiliitis on magnetic resonance imaging and subsequent development of sacroiliitis on plain radiography. Baseline relationships between psoriasis and psoriatic arthritis: analysis of 221 patients with active psoriatic arthritis. Peripheral manifestations in spondyloarthritis: relevance for diagnosis, classification and follow-up. Diagnosing reactive arthritis: role of clinical setting in the value of serologic and microbiologic assays. Peripheral arthropathies in inflammatory bowel disease: their articular distribution and natural history. Diffuse idiopathic skeletal hyperostosis may give the typical postural abnormalities of advanced ankylosing spondylitis. Abnormalities of the sacroiliac joints in diffuse idiopathic skeletal hyperostosis: demonstration by computed tomography. Genetic basis for individual variations in pain perception and the development of a chronic pain condition. Catechol-Omethyltransferase gene polymorphisms are associated with multiple pain-evoking stimuli. A functional polymorphism in the catechol-O-methyltransferase gene is associated with osteoarthritis-related pain. Exercise in ankylosing spondylitis: discrepancies between recommendations and reality. Benefits and risks of ankylosing spondylitis treatment with nonsteroidal anti-inflammatory drugs. Nonsteroidal anti-inflammatory drugs reduce radiographic progression in patients with ankylosing spondylitis: a randomized clinical trial. Efficacy of methotrexate in ankylosing spondylitis: a randomized, double-blind, placebo controlled trial. Infliximab in combination with methotrexate and Infliximab in patients with ankylosing spondylitis: a clinical and imaging study. Recombinant human tumor necrosis factor receptor (etanercept) for treating ankylosing spondylitis: a randomized, controlled trial. Magnetic resonance imaging examinations of the spine in patients with ankylosing spondylitis before and after therapy with the tumor necrosis factor alpha receptor fusion protein etanercept. Efficacy and safety of up to 192 weeks of etanercept therapy in patients with ankylosing spondylitis. Efficacy and safety of adalimumab in the patients with ankylosing spondylitis: results of a multicenter, randomized placebo-controlled trial. Improvement in pain intensity, spine stiffness, and mobility during a controlled individualized physiotherapy program in ankylosing spondylitis. Measuring disease activity in ankylosing spondylitis: patient and physician have different perspectives. Are chronic low back pain outcomes improved with co-management of concurrent depression? Screening for depression in primary care with two verbally asked questions: cross sectional study. Spinal mobility in ankylosing spondylitis: reliability, validity and responsiveness. Preliminary clinical prediction rule for identifying patients with ankylosing spondylitis who are likely to respond to an exercise program: a pilot study. Mortality, course of disease, and prognosis of patients with ankylosing spondylitis. Health status of patients with ankylosing spondylitis: a comparison with the general population. Expert opinion and key recommendations for the physical therapy and rehabilitation of patients with ankylosing spondylitis. Relationship between psychological status and disease activity and quality of life in ankylosing spondylitis. Psychological correlates of self-reported functional limitation in patients with ankylosing spondylitis. Effects of psychological therapy on pain behavior of rheumatoid arthritis patients. Psychological and behavioral approaches to pain management for patients with rheumatic disease. Effect of improving depression care on pain and functional outcomes among older adults with arthritis. New treatment targets in ankylosing targets in ankylosing spondylitis and other spondyloarthritides. Abatacept in spondyloarthritis refractory to tumor necrosis factor alpha inhibition. The pain initially began while performing close-grip resisted curl-ups for the first time. Training-related activities are painful, particularly extreme shoulder internal rotation and elbow flexion. Prior treatment with ibuprofen 800 mg three times daily with meals resulted in no significant improvement. The patient demonstrates a high level of anxiety because he is concerned about his athletic scholarship and about an upcoming international tournament in Europe. He also finds that when he is stressed, such as before an upcoming examination, his pain severity worsens. He is referred to the Interdisciplinary Pain Medicine Clinic for further evaluation. Physical examination reveals a well-developed muscular male in no apparent distress. Palpation at the right biceps distal insertion at the radial tuberosity and at the antecubital fossa is positive. What are the clinical manifestations of distal biceps tendonitis pain, and how is it diagnosed? How does psychological state effect the development and presentation of physical symptoms? The differential diagnosis for this patient includes distal biceps tendinopathy, bicipital radial bursitis, distal brachialis strain, and elbow joint synovitis. Given the demographics of the patient, mechanism of injury, absence of significant past medical history, and physical examination findings, his injury is most consistent with distal biceps tendinopathy. Current histologic studies reveal degenerative changes within the involved tendon. As a result, tendinosis is the currently preferred histologic term, whereas tendinopathy is used clinically. The bundles are encased in an endotendon, and the entire tendon is wrapped in an epitendon. Tendons that curve around bony structures usually have a synovial-lined sheath (tenosynovial sheath), whereas others have only a paratendon layer. Collagen fibrils are composed of type 1 collagen (able to withstand high tensile forces) and elastin (provides flexibility). Additionally, some tendons have areas of hypovascularity or watershed regions making them potentially more prone to injury and portend a longer healing time. What little is known is based mostly on extrapolations from experimental animal models and a few human studies. Some animal models support the notion of an early inflammatory response with acute tendon loading, whereas, with a more gradual loading model, only degenerative changes are found. Under normal cyclical loading conditions, tendons undergo periods of breakdown and repair, maintaining normal health within the tendon. If the tendon is overwhelmed with repetitive stress or exposed to local hyperthermic conditions during periods of strenuous exercise, microinjury of the tendon can occur. Free nerve endings accompany the ingrowth of the blood vessels, which is paralleled with increased levels of glutamate, substance P, and calcitonin gene-related peptide (nerve pain transmitters). At some point after this step, the patient may become symptomatic and present to the office for evaluation. The later part of this theory can be used to help develop a treatment approach that will be discussed later in this chapter. Reprinted with permission from Abate M, Gravare-Silbernagel K, Siljeholm C, et al. Patients will typically report an insidious onset of discomfort around the region of the involved tendon. The interviewer should elicit information about activities that may have led to the injury. Specifically, inquiries should be made about sudden changes in activity level such as starting a new job, home project, sport, or activity. If the patient is an athlete, did he or she have a sudden change or escalation in the training program? Patients who work on an assembly line or who perform heavy manual labor should be questioned about the amount of maintenance exercise performed. Elicitation of pain with palpation of the involved tendon or activation and stretching of the associated muscle is common. Differentiating pain related to the tendon compared to the adjacent joint can be difficult at times. In general, painful articular structures should be provoked with passive movement of the joint while taking care to not stretch the adjacent tendons. He likely injured the distal biceps tendon as a result of the sudden overstressing of the tendon with a new biceps curl exercise. The location of his pain, tenderness to palpation of the tendon, and ability to reproduce his pain with provocative maneuvers are all consistent with distal biceps tendinopathy. Although the Hook test may reproduce his pain, a firm end feel with lateralization of the tendon would help to confirm that at least some portion of the tendon remains intact. Several factors may play a role in which study(s) is ordered, including availability of the imaging modality and patient-specific characteristics. Ultrasound is quickly becoming the study of choice for assessing soft-tissue structures of the musculoskeletal system. Split or partial thickness tears of the tendon are not uncommon and may be associated with adjacent joint or bursa effusion. A potential limitation of ultrasound in the United States at this time includes the limited availability of qualified ultrasonographers. Fortunately, many physicians in a variety of fields (radiology, physiatry, family medicine, rheumatology, orthopedics, and others) are being trained to perform diagnostic scans of the musculoskeletal system. Also, ultrasound is not capable of adequately assessing intra-articular structures at this time.
25 mg unisom order mastercard. Baby Sleep Music - Calming - Lullaby for Babies Relaxing.
References
- Meyers MA: Dynamic Radiology of the Abdomen: Normal and Pathologic Anatomy, 5th ed. Springer, New York, 2000.
- Kroon BK, Horenblas S, Deurloo EE, et al: Ultrasonography-guided fine-needle aspiration cytology before sentinel node biopsy in patients with penile carcinoma, BJU Int 95(4):517n521, 2005. Kroon BK, Horenblas S, Lont AP, et al: Patients with penile carcinoma benefit from immediate resection of clinically occult lymph node metastases, J Urol 173:816n819, 2005. Kumar S, Ananthakrishnan P: Predicting regional lymph node metastasis in carcinoma of the penis: a comparison between fine-needle aspiration cytology, sentinel lymph node biopsy and medial inguinal lymph node biopsy, BJU Int 81:453n457, 1998.
- Smet PJ, Edyvane KA, Jonavicius J, et al: Colocalization of nitric oxide synthase with vasoactive intestinal peptide, neuropeptide Y, and tyrosine hydroxylase in nerves supplying the human ureter, J Urol 152:1292, 1994.
- Exner DV, Dries DL, Waclawiw MA, Shelton B, Domanski MJ. Beta-adrenergic blocking agent use and mortality in patients with asymptomatic and symptomatic left ventricular systolic dysfunction: a post hoc analysis of the Studies of Left Ventricular Dysfunction. J Am Coll Cardiol. 1999;33(4):916-923.
- Humar A, Asberg A, Kumar D, et al. An assessment of herpesvirus co-infections in patients with CMV disease: correlation with clinical and virologic outcomes. Am J Transplant. 2009; 9:374-381.
