
Vasotec
| Contato
Página Inicial
Melissa Anne Daubert, MD
- Associate Professor of Medicine
- Member in the Duke Clinical Research Institute
https://medicine.duke.edu/faculty/melissa-anne-daubert-md
These effects underlie the mechanism by which bacteria induce a proinflammatory cascade in platelets blood pressure medication cialis cheap vasotec 5 mg free shipping, suggesting that bacteria can directly activate platelet-dependent thrombotic responses radial pulse blood pressure 90 5 mg vasotec buy fast delivery. Their role in atherosclerosis has recently been attributed to their release of reactive oxygen species blood pressure chart by time of day discount vasotec 5 mg amex. This development continues to be driven by scientific discovery hypertension in dogs buy generic vasotec 5 mg line, the growing number of patients prehypertension thyroid vasotec 5 mg on line, and the increasing indications for antithrombotics. Targets for antiplatelet drugs continue to be defined, leading to novel therapies and the development of additional agents in existing successful classes. Risk of a first venous thrombotic event in carriers of a familial thrombophilic defect. Genetic polymorphisms associated with venous and arterial thrombosis: an overview. Hyperhomocysteinemia: no longer a consideration in the management of venous thromboembolism. Caution in interpreting results from imputation analysis when linkage disequilibrium extends over a large distance: a case study on venous thrombosis. Association between the Glu298Asp polymorphism in the endothelial constitutive nitric oxide synthase gene and brain infarction. Plasma fibrinogen explains much of the difference in risk of coronary heart disease between France and Northern Ireland. Polymorphisms in coagulation factor genes and their impact on arterial and venous thrombosis. Functional analysis of the fibrinogen Aalpha Thr312Ala polymorphism: effects on fibrin structure and function. Association of laboratory-defined aspirin resistance with a higher risk of recurrent cardiovascular events: a systematic review and metaanalysis. Aspirin "resistance" and risk of cardiovascular morbidity: systematic review and meta-analysis. Antithrombotic effect of crotalin, a platelet membrane glycoprotein Ib antagonist from venom of Crotalus atrox. Pharmacological characterization and antithrombotic effect of agkistin, a platelet glycoprotein Ib antagonist. The humanized anti-glycoprotein Ib monoclonal antibody h6B4-Fab is a potent and safe antithrombotic in a high shear arterial thrombosis model in baboons. Anticoagulation in pulmonary embolism: update in the age of direct oral anticoagulants. Possible reflection of T lymphocyte and platelet involvement in the pathogenesis of acute coronary syndromes. Potential link between Helicobacter pylori and ischemic heart disease: does the bacterium elicit thrombosis. Immune versus thrombotic stimulation of platelets differentially regulates signalling pathways, intracellular protein-protein interactions, and alpha-granule release. Despite the relevance of vascular fibrosis to pulmonary arterial hypertension, cardiomyopathy, coronary artery disease, and many other common cardiovascular diseases, treatments targeting the process directly are lacking. In this article, we provide a comprehensive review of key topics relating to fibrosis in cardiovascular disease, including collagen biochemistry; the role of fibrosis in the pathogenesis of disease affecting the systemic, coronary, and pulmonary vasculature, as well as cardiomyocytes; diagnostic tools to detect fibrosis in patients clinically; and avenues of ongoing research aiming to develop treatments that affect or prevent cardiovascular fibrosis. The functional consequences of fibrosis are diverse and hinge, in part, on the involved tissue subtype. For example, activation of preprogrammed mechanisms in response to dermal injury results in a highly coordinated series of molecular and histological events that causes the formation of a discrete collagen plug. In this scenario, fibrosis is physiological by generating an adaptive response to trauma that regulates hemostasis and decreases the probability of infection. Pathogenic fibrosis is solely detrimental and therefore contradistinctive to maladaptive fibrosis, which may have favorable and unfavorable consequences. For example, replacement fibrosis following myocardial infarction maintains the structural integrity of the myocardium but also serves as a nidus for unstable reentry tachyarrhythmia and progression to heart failure. Understanding the nuances of vascular fibrosis requires appreciation for its pathobiology, because classifying fibrosis based only on its distribution without regard to collagen biofunctionality is an incomplete paradigm. In turn, a contemporary understanding of the molecular mechanisms that regulate fibrosis is an important step toward potentially identifying novel treatment targets for fibrotic cardiovascular diseases. The classification of fibrosis must consider collagen distribution and biofunctionality. Fibrosis contributing to cardiovascular disease is generally maladaptive or pathogenic. In maladaptive fibrosis, collagen deposition occurs in response to necrosis, such as following myocardial infarction or other injury, and increases the probability of adverse cardiovascular events through, for example, malignant arrhythmias. Thus the most common triplet sequence is glycine-proline-hydroxyproline (predicted denaturation enthalpy G° = -1. Size and complexity are increased by posttranslational modifications and self-assembly. Oxidation of lysine side chains leads to the spontaneous formation of hydroxylysyl pyridinoline and lysylpyridinoline cross-links. Each of three polypeptide -chains (662 to 3152 amino acids)13 is labeled by an Arabic numeral that indicates unique structural properties. By contrast, the Col1A gene encodes the heterotrimer collagen I, which may have either two 1-chains and one 2-chain (1[I]2, 2[I]), or, alternatively, three 1chains (1[I])3 (Table 9. Collagen structure, properties, and relevance to human biology Proline is derived from the amino acid L-glutamate and synthesized by cyclization of glutamate-5-semialdehyde into its biosynthetic precursor 1-pyrroline-5carbyoxylic acid. Owing to its secondary amino group, proline may exist in the cis or trans conformation. However, the beneficial effect of proline on thermodynamic stability of collagen requires isomerization from the cis to trans orientation. Posttranslational modification of proline residues by prolyl 4hydroxylase results in hydroxylation of its -carbon to form hydroxyproline, which provides a thermodynamic and mechanical advantage of this modification when in the Yaa position. The C-propeptides are enzymes that coordinate selection, alignment, and organization of -chains, which is required for formation and elongation of the triple helix to generate procollagen in the endoplasmic reticulum. The fundamental hallmarks of the fibrosis phenotype are increased cellular stiffness and impaired tissue compliance. For example, vascular inflammation and thrombotic remodeling promote synthesis, release, and recruitment of growth factors, angiogenic simulators, and vasoactive cytokines. If unopposed or sustained, injury to the endothelial basement membrane occurs and results in the initiation of a larger cascade characterized by increased vascular permeability, platelet degranulation, and clot formation. Ultimately, activation of fibroblasts, myofibroblasts, macrophages, and endothelial or epithelial cell phenotype switching to profibrotic cells of mesenchymal origin. Under pathogenic circumstances, tonic upregulation of this pathway promotes excessive fibrillar collagen synthesis and deposition. Thus these are bona fide treatment targets by which to prevent or attenuate cardiovascular fibrosis. Aldosterone inactivates the endothelin-B receptor via a cysteinyl thiol redox switch to decrease pulmonary endothelial nitric oxide levels and modulate pulmonary arterial hypertension. A list of some profibrotic miRs and their putative targets are provided in Table 9. In particular, cardiac fibroblasts exert a range of transcellular communication capabilities through miR signaling involving exosomes, apoptotic bodies, and microvesicles, which are important for propagation of fibrotic remodeling beyond the site of initial cardiovascular injury. The initiation of collagen degradation generally involves mechanical strain on the fibrils, which facilitates their physical dissociation and breakdown. Executing these functions is a dynamic process that involves continuous collagen deposition and breakdown. Cardiac fibroblasts secrete procollagen chains that organize into fibrils and undergo posttranslational cross-linking, which maintains tissue strength. Pathological fibrosis arises when there is aberrant healing or response to injury in which collagen deposition exceeds clearance. Overall, myocardial fibrosis results in increased tissue stiffness, decreased cardiac compliance, and, ultimately, impaired contractility with increased susceptibility to malignant arrhythmias and sudden cardiac death. Two characteristic patterns of fibrosis occur in the myocardium: replacement fibrosis and interstitial fibrosis. Replacement fibrosis occurs in response to injury in which myocytes die and are "replaced" by fibrotic scar. The most common example of replacement fibrosis occurs as a result of myocardial infarction and is observed in the blood flow distribution of the involved coronary artery. Contrast-enhanced cardiovascular magnetic resonance images in four patients with hypertrophic cardiomyopathy. The composition of interstitial fibrosis is disproportionately type I collagen, which increases collagen crosslinking leading to myocardial stiffness. The underlying triggers for fibroblast activation and the factors that contribute to individual variation in the development of interstitial fibrosis are unknown. Processes implicated in interstitial fibrosis include inflammation, immune response, infection, and metabolic diseases, among others. The relative contributions of these molecular mediators and specific diseases in which they exert their effects are incompletely understood. Nonetheless, these factors represent potential targets to prevent or reverse myocardial fibrosis by virtue of their involvement in fibroblast activation. Interstitial fibrosis increases with age and is observed in patients with systemic hypertension, heart failure with preserved ejection fraction, and systemic sclerosis. Importantly, interstitial fibrosis is reversible and thus an important target for intervention to improve cardiovascular outcomes. Methods of Detection the "gold standard" for detection of myocardial fibrosis is endomyocardial biopsy. Biopsy is typically performed on the interventricular septal surface of the right ventricle because of increased thrombosis and systemic embolism risk when performed in the left ventricle. The extent of fibrosis is assessed by Masson trichrome and picrosirius red staining, among other collagen stains. Major limitations of endomyocardial biopsy include the invasive nature of the procedure, with limited access to left ventricular tissue, and sampling error, in which patchy areas of fibrosis may be missed. Both methods require administration of gadolinium-based contrast, which is cleared more slowly in tissues with expanded extracellular space and reduced capillary density. Myocardial gadolinium accumulation shortens the longitudinal relaxation time, which increases signal intensity and can be quantified. T1 mapping allows identification of interstitial fibrosis that cannot be seen with the "naked eye. Precontrast or "native" T1 time is longer in areas of interstitial fibrosis, whereas postcontrast T1 is decreased in fibrotic areas. Similar to other conditions, fibrosis in hypertrophic cardiomyopathy is associated with increased risk of malignant arrhythmias and sudden cardiac death,45 including in subjects without other high-risk features. Atrial Myopathy in Atrial Fibrillation Fibrosis of the myocardium may also involve the atria and contribute to the risk of persistent atrial fibrillation and thromboembolic stroke. Fibrotic atrial cardiomyopathy results from fibroblast activation by atrial injury and stretch from atrial fibrillation risk factors. The risk of stroke appears to persist after restoration of sinus rhythm in patients with atrial fibrosis, suggesting that fibrotic substrate may contribute directly to the risk of thrombosis. Preventing atrial fibrosis has thus emerged as an additional therapeutic target to reduce stroke risk. Endomyocardial Fibrosis Endomyocardial fibrosis most commonly affects young adults in low-income tropical areas. It is characterized by an acute febrile illness, myocardial inflammation, and eosinophilic infiltration leading to subendocardial myocardial fibrosis. In the chronic phase, endomyocardial fibrosis typically involves the apices of both ventricles and manifests clinically as a restrictive cardiomyopathy with congestion, edema, and ascites. Myocardial fibrosis is also observed in genetic cardiomyopathies (arrhythmogenic right ventricular cardiomyopathy), autoimmune conditions (systemic sclerosis, Churg-Strauss syndrome), and infectious diseases (Lyme disease, Chagas disease). Lack of specificity limits the diagnostic potential of these potential biomarkers of fibrosis. Both markers correlate well with the fibrosis fraction on histology, are higher in patients with known heart disease, and decline in response to heart failure therapies. Replacement or "scar" fibrosis is thought to be irreversible, whereas interstitial fibrosis is modifiable. Although absolute reductions in collagen were modest, regression correlated with improved cardiac function, providing important proof of principle. The relative abundance of these collagen types determines the vascular biomechanical properties, arterial stiffness, and hemodynamics. Imbalance of collagen and elastin in a proinflammatory milieu leads to vascular fibrosis. Fibrosis in small vessels contributes to endothelial dysfunction, increased vascular tone, and reduced tissue perfusion. The latter can lead to replacement of parenchymal tissue with fibrosis, ultimately resulting in organ damage. Fibrosis in large vessels leads to hemodynamic changes such as systemic arterial hypertension. The clinical consequence of macrovascular fibrosis is increased arterial stiffness. Stiffening is caused by dysregulated collagen deposition and elastin degeneration, medial calcification, and cross-linking of collagen by advanced glycation end products. Arterial stiffening and vascular fibrosis precede the development of overt clinical hypertension. Therefore hypertension is both a cause and a consequence of increased arterial stiffening.
The middle rectal arteries are generally very small-calibcr vessels and may be absent arrhythmia recognition 10 mg vasotec purchase with mastercard. The two most important direct branches of the aorta that contribute to pelvic organ blood supply are the superior rectal and ovarian arteries blood pressure for stroke order vasotec amex. The mperior m:tlll artery blood pressure fluctuations cheap 10 mg vasotec amex, which is the terminal branch of the inferior mcscnteric artery blood pressure chart boy 5 mg vasotec order with mastercard, anastomoses with the middle rectal arteries blood pressure high in the morning purchase 10 mg vasotec visa, thus contributing blood to the rectum and vagina. The ovarian arteries anastomose with the ascending branch of the uterine ancry and contribute blood to the uterus and adnaa. Pelvic Blood Supply Internal mac Artery" Ant·rlor Division Parietal Branches Obturator Internal pudenda! Inferior gluteal Posterior Division Parietal Branches lliolumbar Lateral sacral Superior gluteal Vlsa! Thi& plems primarily contains sympathetic fihcn and sensory affermit fihcn from the uterus. These nerves join parasympathetic dfcrcnts from the second through the fourth sacral nerve roots (pelvic splanchnic nerves) to form the inftribr hypagmtric plncus, also known as the pelvic plncus. In addition, the inferior hypogastric plexus generally receives contributions from the sacral sympathetic trunk. With variability, 6bers of the inferior hypogastric plexus accompany the distal branches of the intcmal iliac artery to the pelvic viscera. Accordingly, they are divided into three portions: the vcsical, utcrovaginal (Frankcnhii. Clinically, the sensory afferent 6bcrs contained within the superior hypogastric plexus are targeted in presacral neurectomy, a surgical procedure performed to treat central pelvic pain (Chap. Although visceral and sexual dysfunction may follow complete interruption of the superior hypogastric plexus, contributions from the sacral sympathetic trunk can offset interruption of this sympathetic component to the inferior hypogasuic plexus. Injury to the branches of the inferior hypogastric plexus during cancer debulking, lymphadenectomy, or other extensive pelvic surgeries can lead to varying dcgrccs of voiding, sexual, and defccatory dysfunction. Similar dysfunction is also possible during incontinence or prolapse procedures that pass sutures or trocars through the paravaginal or paraurethral tissue, which contain fiber extensions of the inferior bypogastric plexus. The portion of the body that enends above the entty levd of the uterine (fallopian) tubes into the endomettial cavity is known aa the fundua. Befure menarche and after menopause, the body and cervix are approximately equal in size, but during the reproductive years, the uterine body is significantly larger than the cervix. In the adult, nonpregnant woman, the uterus measures apptmdmatdy 7 cm in length and 5 cm in width at the fundus. Interlacing myometrial 6bers surround myometrial veuels and contract to compress these. Second, the lateral ponions of the body and cervix attach to the broad and cardinal ligaments. Endometrium and Serosa 1he uterus consists ofan inner mucosal layer called the endometrium, which surrounds the endometrial cavity and is described in Chapter 8. The myometrium surrounds the endometrial cav· ity and contains smooth muscle bundles united by connective Cervix the uterine cervix begins caudal to the uterine isthmus and is approximately 3 cm long. The wall of the cervix, especially its distal segment, contains primarily 6brous tissue and approxi· matdy 10 percent smooth muscle. The smooth muscle is found on the cervical wall periphery and serves as the anachmcnt point for the cardinal and uterosacral ligaments and for the 6bromuscular walls of the vagina. This smooth muscle is easily dissected from the underlying, denser 6brous cervix core and is the layer rcftected during intrafascial hysterectomy. This tissue that attaches lateral to the uterus and cervix on each side is called the µrametrium and continues caudally along the vagina as the jJllTll&O/pium. The cardinal ligaments, also termed transvme mvka1 /igammts or Mackmrotit ligammts, primarily consist of vessels and connective tissue and contain some pelvic autonomic nctvc:s in their lower portion (Ramanah, 2012; Range. Tuey attach to the pomrolatcral pelvic walls near the origin of the internal iliac artery and contain the vessels supplying the uterus and vagina. The uterosacral ligaments insert broadly into the posterior pelvic walls and 5aa1m and form the lateral boundaries of the posterior cul-de-sac of Douglas. These ligaments originate from the posterior inferior surfu:e of the cervix but may also originate, in pan, from the proximal posterior vagina (Umck, 2004). Clinically, during pelvic reconstructive surgeries that use the utcrosacral ligaments as attachment sites fur the vaginal apex, surrounding structures are especially vulnerable (Wieslander, 2007). The ureter, pelvic sidewall vessels, and sacral nerves run 1atcral to and close to these ligaments. They enter the retroperitoneal space and pass 1atcral to the infuior epigasttic vessels before entering the inguinal canal through the deep inguinal ring. They receive their blood supply from a small branch of the uterine or ovarian artery known as the Sampson artery. Within the upper portion of these two layers, the fullopian tube, ovarian ligament, and round ligament are found. Each of these has its separate mesentery, called the mesosaipinx, mesovarium, and mesotm:s, respectively, which carry nerves and vessels to these structures. At the lateral border of the fullopian tube and the ovary, the broad ligament ends where the suspensory ligament of ovary (infundibulopelvic ligament), described earlier, blends with the pdvic wall. The cardinal and uterosacral ligaments lie within the lower portion or "base" of the broad ligament. Several uterine veins run along the side of the artery and are variably found over or under the ureter. The uterine artery then divides into a larger ascending and a smaller descending branch that course alongside the uterus and cervix, respectively. Clinically, because the uterus receives dual blood supply from both ovarian and uterine vessels, some surgeons during myomectomy place tourniquets at both the infundibulopdvic ligament and uterine isthmus. The medullary portion of the ovary primarily consists of fibromuscular tissue and blood vessels. Laterally, each ovary is attached to the pelvic wall by the suspensory ligament of the ovary, clinically known as the infandibulopelvic ligament, which contains the ovarian vessels and nerves. Lymphatic drainage of the ovaries follows the ovarian vessels to the lower abdominal aorta, where they drain into the paraaortic nodes. For their innervation, the ovaries are supplied by extensions of the renal plexus that course along the ovarian vessels in the infundibulopelvic ligament. The uterine part, also known as the intramural or interstitial portion, passes through the body of the uterus at the region known as the cornua. The infandibulum of the uterine tube is the distal continuation of the ampullary segment and contains the fimbriated portion at its distal end. The venous plexus, lymphatic drainage, and nerve supply of the fallopian tubes follow a similar course to those of the ovaries. However, some lymphatic channels from the uterine body may pass along the round ligaments to the superficial inguinal nodes, and others may extend along the uterosacral ligaments to the lateral sacral nodes. In the standing or anatomic position, the apex of the vagina is directed posteriorly toward the ischial spines, and the upper two thirds of the vaginal tube lie almost parallel to the plane of the levator plate. The average length of the anterior vaginal wall is 7 to 8 cm and that of the posterior wall is 9 cm. The recesses within the vaginal lumen · Ovaries and Uterine (Fallopian) Tubes Ovaries the ovaries and fullopian tubes constitute the uterine adnexa. The size and hormonal activity of the ovaries are dependent on age, stage ofthe menstrual cycle, and exogenous hormonal suppression. A nonkeratinized squamous epithdium and its adjacent lamina propria line the vaginal lumen. The vagina is separated from the bladder anteriorly and the rectum posteriorly by the vaginal adventitia. The continuation of this adventitial layer laterally contributes and blends into the paracolpium. Similar to microscopic findings of the anterior vaginal wall, histologic studies have failed to show a separate layer between the posterior wall of tbe vagina and the rectum except in the distal 3 to 4 cm (Maldonado, 2019). Here, the dense fibromuscular tissue of the perincal body separates the vaginal from the anal walls (DeLancey, 1999). Because there is no true histologk "fascial" layer between the vagina and the bladder and between the vagina and the rectum, some recommend that terms such as "pubocervicalJpubovesical fascia" or "rectovaginal fascia" be abandoned. Veslcovaglnal space (filled with loose connective tissue) Perineal body Fused distal segment of urethra a. Vesicocervical and Vesicovaginal ·Potential" Spaces the vesicocervical space begin& below the ve&icouterine peritoneal fuld or re8cction. This fold represents the loose attach· ments of the peritoneum in the wdcouterine pouch, also known as the anterior cul·d. The vcsiccccrvical space continues down u the vesicovagintd space, which extends to the junction of the proximal and middle thirds of the urethra. Clinically, during an abdominal hysterectomy or ccsarcan delivery, surgeons easily lift and incise the ve&icouterine peri· toncal fold to create a "bladder:8ap" and then develop the vcsicoccrvical and vesicovaginal spaces. I ligament 6bers, also known as rectal pillars, are fibcrs of the posterior parametrium that atend down from the cervix. Vilginal Support Although the connective tissue in the pelvis is continuous and interdependent, Delancey (1992) has described three levels of vaginal connective tissue support. These atcachments are known as level I support or suspmsory axis and provide connective tissue support to the vaginal apex: after hysterectomy. In the standing position, level I support 6bcrs are both vertically oriented (cardinal ligaments) and posteriorly oriented (utcrosacral ligaments) (Chen, 2013). RectovaglnalSpace this potential space is immediately adjacent to the posterior surf. These grooves run along tbe vaginal sidewalls and give tbe vagina an "H" shape when viewed in cross section. The re8ection of tbe bladder onto the abdominal wall is triangular, and the triangle apex is continuoua with the median umbilical ligament. Tue mucosa of the bladder consista of transitional epithelium and underlying lamina propria. The bladder is divided into a hotly (dome) and a fontlru (base) apprmimatdy at the level of the ureteric orifices. These loops are two U-shaped bands of6bers found at the Vaginal Blood Supply, Lymphatics, and Innervation Tue main blood supply to the vagina ar. These veasels fonn an anastomotic arcade along the lateral sides of the vagina at the levd of the vaginal sulci, and they anastomose with the contralatenl vessels on the anterior and pcmerior walls of the vagina. Additionally, the middle rectal artery from the internal iliac artery contributes to tbe posterior vaginal wall supply. The distal walls of the vagina also receive contributions from the internal pudendal artery. Other contributors arc the middle and inferior vesical arteries, which, when present, often arise from either the internal pudenda! Its proximal lumen begins at the internal urethral orifice (meatus) within the bladder. The urethra then courses through the bladder base for less than a centimeter, and this region is called the bladder n«lt. Approximately at the junction of the middle and lower third of the urethra, and just above or deep tD the perineal membrane, two strap skeletal muscles called the sphincter umhrovagina/is and compressor um/mu arc found. These mwcles were previously known as the tlup transvnuptrinelli muscles in fcmalcs. Together with the sphincter ureduac, they constitute the striated urogmilal sphincter complex. Together, these three mwcles function as a unit and have an intricate innervation that is not universally agreed upon. This complex supplies constant mnus and provides cmcrgcnqr reflex activity mainly in the distal half of the urethra to sustain continence. Distal to the depth of the perincal membrane, the walls of the urethra consist of fibrous tissue, serving as the nozzle that directs the urine stream. Duct openings of the two most prominent glands, termed Skene glands, are seen on the inner surface of the external urethral orifice. The urethra rcccivcs its blood supply &om branches of the inferior vesical/vaginal and internal pud. The peritoneum is then rc:8cctcd onto the posterior vaginal wall to form the rtctoutnint pouch. In women, this culdc-sac is located approximately 5 to 6 cm from the anal orifice and can Sphincter urethrae m. At its comsphincter mencement, the rectal wall is similar campiex to that of the sigmoid. Clinically, in the empty state, the transverse the inferior hypogastric plexus variably innervate the sphincter rectal folds overlap. An additional discwsion of lower urinary tract innercontinence by supponing fecal matter above the anal canal. It descends Below the anorectal junction, the gut extends as the anus, which on the anterior surface of the sacrum for approximately 12 cm has a series of anal valves to aid its closure. Here, the mucosa of the colon lhe posterior sur&cc of the rectum is rctroperitoncal. Anatomy 21 gives way to a transitional layer of non-hair-bearing squamous epithelium before becoming the hair-bearing perineal skin at the anocutaneous line. Next, the rectum and ampulla above the pelvic Boor receive a direct branch from the middle rectal. In the pelvis, it lies in a special connective tissue sheath that is attached to the peritoneum of the lateral pelvic wall and "medial leaf" of the broad ligament.
Overall blood pressure upper number generic vasotec 10 mg online, this risk of conversion is low blood pressure medication and zyrtec buy generic vasotec from india, and logically heart attack 4sh vasotec 10 mg on line, rates decline as surgeon experience accrues arrhythmia ultrasound cheap vasotec 5 mg. Minor complications of laparoscopy include port site infection or hematoma blood pressure medication causes nightmares cheap 10 mg vasotec with mastercard, subcutaneous emphysema from C02 infiltration, vulvar edema, and postoperative peritoneal irritation from retained intraahdominal C02· Irritation stems from conversion of C02 to carbonic acid, which can be a direct irritant. For other types of laparoscopic procedures, data do not support antibiotic prophylaxis for clean surgical cases, that is, those that do not enter the vagina, bowel, or urinary tract (Chap. For thromboprophylaxis, the same principles used for other abdominal surgeries are currently recommended for laparoscopic cases until further data accrues (American College of Obstetricians and Gynecologists, 2018h). Specific to laparoscopy, pneumoperitoneum pressure may decrease venous return from the lower extremities (Caprini, 1994; ldo, 199 5). Balanced against this is the rapid postoperative mobility achieved by most patients. Puncture Injuries Because sharp tools are used during laparoscopic entry, vessels and abdominal organs may be punctured. Risk factors are intraabdominal adhesions, incomplete gastric emptying, full bladder, insufficient pneumoperitoneum, poor muscle relaxation, thin patient habitus, and inappropriate force of tool insertion. As discussed later, several authors advocate an open entry method as a means to lower puncture injury rates (Catarci, 2001; Hasson, 2000; Long, 2008). Organ Injury the organ most frequently injured during laparoscopy is bowel, and rates of 0. Women with previous laparotomy have a higher incidence of abdominal adhesions and are at greatest risk for this complication (see Table 41-1). Unfortunately, bowel injury sustained during laparoscopy is often missed intraoperatively. In one study, nearly 50 percent of both small and large bowel injuries were unrecognized for 24 hours or longer (Chandler, 2001). Typically, these patients 876 Aspects of Gynecologic Surgery present with fever, abdominal pain, nausea, and vomiting within 48 hours of swgery (Li, 1997). In laparoscopic cases, decompression of the stomacb with an orogastric tube prior to obtaining laparoscopic access can lower the stomach punctwe risk. Moreover, in those with sU&pected abdominal adhesive di&ease, several preventative steps can help avoid bowel injury. These include: (1) an alternative site for primary trocar entry, for aample in the left hypocbondtiwn (Palmer point), rather than at the umbilicus; (2) introduction of a microlaparoscope to scout for adhesions; and (3) preoperative sonography using the visce. These occw at the same surgical steps associated with urinary tract injury during abdominal hysterectomy. Uncommonly, air embolism from gas insufllation following vessel puncture may occur. Although rare, deaths have resulted from large vessel injury (Baadsgaard, 1989; Munro, 2002). Prevention may include use of the open entry technique or awareness of the angle and force of trocar entry. Despite these steps, if a large vessel is punctured, the wounding instrument is not removed boc:ausc it may act as a vascular plug. In most cases, laparotomy, direct manual pressure on the vessel, steps for bemodynamic resuscitation, and notllication of a vascular surgeon should follow expeditiously. In contrast, if the inferior epigastric artery is injwcd, several simple techniques can control hemorrhage. If unsuccessful, a 14F Foley catheter can be threaded through the cannula of the wounding trocar or through the defect created by this trocar. The Foley balloon then is inflated and pulled upward to create direct pressure against the posterior surfu:c of the anterior abdominal wall. At the skin surfu:e, a Kelly damp is placed pcrpcndic:ular across the Foley catheter and paralld to the skin to hold the balloon firmly in place. Similarly, the Carter-Thomason tool can be used to ligate both ends of this vcssd. Nerve injury can follow in patients placed for extended pcri· ods in the dorsal lithotomy position with arms abducted. A, Suture with an attached straight Keith needle Is driven through the anterior abdominal wall lateral and caudal to the bleedlng artery. The needle is then driven upward and through the anterior abdominal wall on the other side of the vessel. Attention paid to patient position and surgery duration prevent many of these complications. Thermal Injury Accidental bwns may follow direct instrument contact or stray dectric current. Pott sites hernias develop less frequently than incisional hernias after laparotomy (Schiavone, 2016). The incidence approximates 1 percent but may rise with gR:atcr use of larger trocars and single-port umbilical techniques (Clark, 2013). With Minimally Invasive Surgery Fundamentals 877 the latter, hernia rates nearing 6 percent have been reported, and older age. A major risk fur incisional hernia is use of large trocars measuring ~ 10 mm in diameter or pon sites from which larger specimens arc extracted. Finally, peritoneal tissue is ideally not drawn into the superficial layers of the wound when removing the cannulas (Bougbcy, 2003; Montz, 1994). Surgeon Primary Surgeon Scrub Nurse Trocar-Site Metastasis Rates of trocar-site cancer metastasis arc low and complicate the clinical course of approltlmatdy 1 percent of patients in whom gynecologic maligvm. Similarly, port-site seeding atop equipment · of other tissues such as endomctriosis is possible. Currently, no evidence-based consensus below eye lc:vd to prevent neck strain (van Det, 2009). In laparoscopy, tool movement is limited compared with lapaA dedicated cabinet or "tower" houses the laparoscopic light rommy, secondary to instrument angle restrictions and fixed source, gas insufllator, and image capture equipment. Also that he or she has an unobstructed view of equipment display preoperatively, all instruments are checked and tested to conpanels. Similarly, dectrosurgical equipment and preference, the following is suggested to optimize efficiency and pedals are organized so that all these cords are aligned in one safety. Pedals arc oriented appropriately fur the primary gery, the bed is checked to ensure it moves up and down and surgeon to comfortably reach without adjusting his body or into steep Trendel. One monitor may suffice for simple procedures, however, two monitors provide easy viewing by the surgeon and as&Utant. To 878 Aspects of Gynecologic Surgery aid proper leg positioning, the stirrup b~, which holster the stirrups, are attached to the table at the level of the patient hips. To prevent femoral nerve injury, the hips are positioned without sharp flexion or marked abduction or external hip rotation. The knees are not flexed more than 90 degrees and are positioned and padded to avoid common fibular (peroneal) nerve compression. To avert slipping when in steep T rendelenburg position and to minimize lower back pressure, a patient can be placed directly on an antiskid material such as egg-crate or gel pad. With these, patient skin directly contacts the padding for traction Klauschie, 2010; Lamvu, 2004). If uterine manipulation is needed, the buttocks are placed slightly past the edge of the table. This allows improved patient access and prevents upper extremity hyperextension, which can injure the brachial plexus. The arms may be tucked using an extended draw sheet, which is placed under the gel pad. This relationship limits arm slippage, which can generate pressure against the brachial plexus. Moreover, in obese patients, antiskid material and arm tucking can help prevent slippage when in Trenddenburg position Klauschie, 2010). Fingertips are facing the thighs, well-padded, and positioned away from the moving foot of the bed to prevent unintentional amputation. During arm positioning, finger oxygen monitors and intravenous access should not be dislodged. Their goal is to brace the shoulder and prevent the head from slipping off the bed when in T rendelenburg position. However, due to the risk of nerve injury, the use of shoulder braces in general should be limited. When shoulder braces are used, compression over the acromion may apply pressure that stretches the plexus. Moreover, lateral compression by braces may compress the humerus against the plexus. With a single-action jaw, one tip is fixed, lies in the same axis as the shaft, and offers greater stability during the action performed. Double-action jaws have tips that move synchronously, and this jaw offers a wider angle in which to perform its function. Some jaws are now modified by a compression feature that allows scissor blades to secure the tissue first in the crux of the jaws and then cut tissue with greater stability and precision. Important instrument qualities are comfort and ease of use, which stem primarily from the hand grip shape, the instrument length, and its locking capability. Although permitting better access, these longer instruments are often more difficult to manipulate due to altered operating angles caused by the extended length. In the hand grip, a locking feature allows a surgeon to hold tissue without maintaining constant pressure against the grip, and this decreases hand fatigue. This versatility allows access to additional anatomic spaces and lessens the need for uncomfortable surgeon hand or arm rotation. Analyses demonstrate that disposable instnunents add significant cost compared with reusable ones (Campbell, 2003; Morrison, 2004). The main advantage to disposable instruments is the consistent tool sharpness and avoidance of lost instrument parts. For example, dull scissors may lead to longer operating times and ineffectual surgical technique. Corson and associates (1989) showed that reusable trocars, although sharpened at regular intervals, still required twice the force for entry compared with disposable trocars. As a compromise, modified trocar systems combine the strength of these two features. Namely, the cannula is reusable, whereas a disposable inner trocar offers a consistently sharper tip. Most surgeons have designated preferences for certain types of graspers, dissectors, and cutting instruments. Additionally, 3-mm, 8-mm, and 15-mm instrument diameters are available for many tips. However, as with the alligator clamp, its ability to retraa or grasp during applied tension is poor due to slippage. Ideally, all of these clamps are included in a general laparoscopic surgical tray for most laparoscopic procedures. Generally, such tissues are placed minimize organ trauma yet allow dfcctivc manipulation. In addition, a locking these, the blunt probe has an end that is modified to decrease hand grip is typically preferred to keep grasped tissues secured. It is wed for exploration Most of these insoumcnts have double-action jaws to allow a and retraction and is a preferred tool during diagnostic laparoswide grasp around the tissue. Most blunt probes arc staiclcs, steel and arc conductive and tension strength is required, however, a tip with a singleof dcctric: airrcnt. However, disposable probes constructed of action jaw and locking hand grip may be preferred. Atraumatic graspers are used for exploration, gentle traction, and delicate tissue handling. Most of these graspcrs have a double-action jaw, and the hand grip is typically nonlocking. The Maryland clamp is an example of a curved blunt tip used for dissection and grasping. The alligator clamp is a blunt grasper with a long, wide tip that handles delicate tissues with minimal crush-injury risk. Single-tooth and double-tooth tenaculwns are both available and effectively bold and rettact dense, heavy tissue. The single-tooth tenaculum usually has a double-action jaw, whereas the double-tooth tenaculum is available with either a single- or double-a. A tenaculwu is traumatic and thus is generally used only on tissue to be resected or. It has short teeth on each side and is excellent for tissue retraction due to iu strong grip strength. For enmple, ovarian biopsy forceps provide adequate gwp with minimal tissue crushing. An appropriate setting might be ovarian cyst resection and subsequent ovarian repair. An Allis grasper has blunter teeth for grasping and holding tissue during resection. Serrated graspers are considered traumatic but are less damaging than toothed graspers. They offer a secure grip with minimal tissue damage and generally are used in repairs or tiasue approximation. Because of their variety, a surgeon should be funiliar with their grips and tissue effects to selei:t the one that best fits the planned procedure. Serrated graspers may be fenestrated or nonfenertrated, may offer a locking hand grip, and may have singie.
J Minim Invasive Gynccol 23(5):719 blood pressure kit reviews vasotec 10 mg with amex, 2016 Salim S blood pressure up heart rate down buy generic vasotec pills, Won H arrhythmia 1 order 10 mg vasotec fast delivery, N csbitt-Hawcs E hypertension 6 weeks postpartum order vasotec 5 mg without a prescription, et al: Diagnosis and management of endomctrial polyps: a criti· cal review of the literature blood pressure app for iphone order discount vasotec on line. Dian D, et al: Comparison of total laparoscopic, vaginal and abdominal hysterectomy. Arch Gynccol Obstct 277(4):331, 2008 Schmidt T, Ercn Y, Breidenbach M: Modifications of laparoscopic supraccrvical hysterectomy technique significantly reduce postoperative spotting. Hauge B, et al: Preoperative ttansccrvical analgesia for laparoscopic sterilization with Filshie clips: a doublcblind, randomized trial. Malzoni M, et al: Italian multiccnter study on complications of laparoscopic myomectomy. Obstct Gynccol 121(1):189, 2013 Sttowitzki T, von WolffM: Laparoscopic ovarian drilling (I. Fcrtil Steril 110(3):364, 2018 Tcduckdharry B, Gilmour D, Flowerdew G: Urinary tract injury at benign gynccologic surgery and the role of cystoscopy. Gynccol Obstet Invm 61(2):106, 2006 Tulandi T, Bcique F, KimiaM: Pulmonary edcma: a complication of local injection of vasopressin at laparoscopy. Fertil Steril 55:53, 1991 Tulandi T, Murray C, Guralnick M: Adhesion formation and reproductive outcome after myomcctomy and second-look laparoscopy. Obstet Gynccol 82:213, 1993 Tunitsky E, Citil A, Ayu R, et al: Docs surgical volume influence short-term outcomes of laparoscopic hysterectomy Soncja H, Samud N, et al: Outpatient Thcrmachoicc cndometrial balloon ablation: long-term, prognostic and quality-of-life measures. Gynccol Obstet Invest 70(3):145, 2010 Vcrccllini P, Zaina B, Yaylayan L, et al: Hystcroscopic myomcctomy: long-term effects on menstrual pattern and fertility. Additionally, operative cystoscopy is within the scope of many gynccologists for the passage of urctcral catheters or stcnts, bladder biopsy, and foreign-body removal. Both rigid and flexible cystoscopes are available, although in gynecology, a rigid scope offers advantages. Rigid scopes also have larger working channels, which allow a wider variety of instruments to pass. Of components, a cystoscope contains an outer sheath, bridge, endoscope (optical lc:ns), and obturator. The sheath contains one: port for fluid infusion and a second port for fluid egress. However, fur operative cases, a 21F or wider-diameter sheath is preferred to allow rapid fluid infusion and easier instrument and stent passage. The end of the sheath tapers, and in women with a narrow urethral meatus, an obturator can be placed inside: the sheath to create a rounded tip for smooth introduction. In selected instances, gentle dilation of the external urethral opening using narrow cervical dilators is needed prior to sheath introduction. To ensure adequate media flow, an infusion bag is dented signifu:andy above the level of the sympbym pubis. If the bladder is distended beyond iu capacity, c:m:a fluid will leak out the urethral mcatus and arowid the cystoscope rather than rupture the bladder, which is rare. When intnopcradvc c:ystosoopy is performed to docwncnt lower urinary tract patency, intravenous dye administration colon the urine a. In addition, the speclalized Albarnan bridge conmins a lever, which can ddlect wires at1d ca. For cystoscopy, a 70-degree endotcope i& superior fur providing the most comprchcmivc view of the lateral, anterior, and posterior walls; ttigonc; and uretcral orifices. With 0- and 70-dcgrce cndoacopi=s, operative instruments generally Ue outside the optic:al fi. Routine use of antibiotic prophylam to prevent the lus than 5-pcrccnt mean risk ofsymptomatic urr after diagnostic cystote0py is c:ontrc>Yerlial (Zeng. The American College of Obstetriciam and Gynccologists (2018b) and othC3 recommend ag;diut prophyfui· fur routine diagnottk cystoKopy in healthy adults at low risk fur surgial site infections (Wolf, 2008). Opy may be performed in low or 1tandard lithoaimy poiition with the legs positioned in stinups. For office cp1D1copy, a lubricating gel is applied to the endoscope tip or 2-percent lid. For operative procedures, an additional 50 mL of 4-pcra:nt lidocainc solution may be instilled. The perineum and urethral meanu are surgic:ally prcpaml prior to un:thral manipulation. Of vital-dye optinm, indigo QnDinc dion:ap have prompted a search fur safe alu:matives. In women, this angle is direcud slightly upward but i& more pronounced with anterior vaginal wall prolapse. The c:ystosoope ill advanc:cd toward the bladder, while the provider views the video screen. To maintain orientation during rotation, the camera is hdd static, while the light cord and cymsc. First, to view the entire left side of the bladder, the cystosccpe and light cable are rowed approzimately 90 degrees in a clockwise fashion. Once the left orifice is noted, further subtle clockwise rotation of the cy;toccope along the interuretcric ridge permits identification of the right orifice. While horizontal to the floor, the c:ysto· scope is withdrawn to the bladder neck and then angled downw. Semantically, most are designed to remain indwelling for prolonged ureteral drainage. Stents are used to relieve obsttuction, treat w:eteral injury, or protcc:t a urctc. Both are hollow to permit radiopaque medium injec:tion and to allow urine egress through or around it. First, these maight narrow tubes may be inserted at the beginning of surgery and left through its duration to define ureteral anatomy. Last, urologists may use c:athcters to collect sclec:tive ureteral urine for cytology. Generally, open-ended or whi6tle-tip typcs are used to dellneate anatomy or exclude obstruction. For this, a 4 to 6F open-ended or whistle-tip catheter is threaded through the operating channel of a 30-degree cystoscope and into the field of view. By advancing both the catheter and cysroscope toward the ureteral orifice, the catheter is passed into the opening. The corresponding catheter distance from the ureteral orifice to the brim approximates 13 cm Qackson, 2019). Once the renal pelvis is reached, the length of the ureter can be measured and is reflected by the catheter marking seen at the ureteric orifice. If resistance is encountered, catheter advancement is stopped, and retrograde pyclography is completed to guide catheter placement. If ureteral transection or stricture is suspected from the just-described steps, a cone tip urcteral catheter is inserted. Through it, radiographic contrast is injected into the distal ureter to locate extravasation or point of narrowing. If conuast flows easily up to the renal pelvis and no extravasation noted, ureteral injury is unlikely. Still, if thermal-injury concerns persist, a double- scent is placed for 2 to 4 weeks to maintain ureteral patency while the edema and inflammation of normal healing subside. If gross blood issues from an orifice prior to uretera1 manipulation, the ureter may be partially transected, severely crushed, or coagulated. Even if suitable urine dHux from a urereral orifice is noted, many insert and maintain a double- stent fur approximately 2 to 4 weeks. In addition, a er urogram or renal sonogram is completed 4 to 6 weeks after stent removal to exclude stricture. After these interrogations, persistently absent cffiux from one orifice may uncommonly reflect a long-standing unilateral nonfunctioning kidney. For this purpose, a ureceral catheter is advanced until gentle resistance is met, which indicates that the renal pelvis has been reached. The ureteral catheter is tied securely to the transurethral catheter and drains into the cystoscopy drape. At the conclusion of surgery, the catheter is removed if there arc: no concerns for ureteral injury. If concerns for injury are prc:sc:nt, a guide wire can be placed through the catheter, the catheter is removed, and a double- stent is threaded over the wire. Stents vary in length from 20 to 30 cm, and a 24-crn or 26-cm length is appropriate for most adults. Double-pigtail or double- stents describe their tip shape, and the ends coil within the renal pelvis and bladder, respectively, to prevent stent migration. For placement, a guide wire is first threaded into the ureteral orifice and passed to the renal pelvis with fluoroscopic guidance. The wire is removed, and retrograde pyelography is performed to obtain a nephrostogram (Linder, 2019). After this study, some of the radiopaque deposited contrast remains in the renal pelvis. This catheter also aids ureteral length measurement and thereby stent length selection. For this, markings on the catheter at the level of the ureteral orifice arc noted. Next, the double-pigtail scene is threaded over the same guide wire and advanced by a pusher device until its distal end enters the bladder. The guide wire is partially removed, allowing the upper curl to form in the renal pelvis. Correct upper coil positioning, indicated by a full curl of at least 180°, is confirmed intraoperatively using fl. Evaluation of the distal coil or curl, which also should be at least 180°, is done cysroscopically. To help avoid patient discomfort and irritative voiding symptoms, the coil should not cross the sagittal midline of the bladder (Al-Kandari, 2007). Longer duration may lead to greater patient discomfort, pyclonephritis, and stent encrustation. However, pyclonephritis may occur in patients with stems, and diagnosis = requires prompt mmauon of intravenous antibiotics (Table 3-14, p. Although not generally recommended, we then continue daily antibiotic prophylaxis after treating pyelonephritis until the stent is removed. Stent-related suprapubic pain or bladder spasm is common and can be treated with an anticholincrgic agent (Table 23-5, p. One aample of the latter is tamsulosin hydrochloride (Flomax), which is prescribed as a 0. The physiologic rationale for these both drug groups is outlined in Chapter 23 p. Notably, pain or obstructive symptoms may reflect stent migration, which is reported in approximately 4 percent of cases (Breau, 2001). If displacement is suspected, a plain abdominal radiograph will display stent position. In this study, the symphysis pubis serves as a general marker of the midsagittal plane. In pregnant patients, coil position can be verified sonographically to avoid radiation exposure. For malpositioning, the stent can be exchanged over a guide wire in an outpatient setting. The lower pigtail of the scent is identified, grasped, and pulled out concurrently with the cystoscope. Small mucosal lesions can be biopsied with minimal risk or discomfort to the patient. Large lesions highly suspicious for bladder cancer should be referred to a urologic oncologist. Biopsy is performed, and the cystoscope and instrument are withdrawn through the urethra together. In this way, a biopsy specimen is not pulled through the sheath and possibly lost. For brisk bleeding, electrosurgical coagulation can be used if a nonconducting solution such as water or glycine was selected as the distention medium. Electrolyte solutions such as saline cannot be used with monopolar electrosurgcry. These solutions conduct current, dissipating the energy, and thereby rendering the instrument useless. Foreign bodies, such as small stones that can pass transurethrally, arc removed using the same technique as biopsy. The instrument is used to grasp the foreign body and then removed together with the cystoscope. Surgeries for Pelvic Floor Disorders 2-0 absorbable suture then is cttated at the bladder dome, with $titcha placed deeply into the bladder mu. The two suture ends are pulled upward and held tightly to prevent dimnding fluid escape. To allow viNalharlon of the trlgone and ureteral orifices, die Foley bulb is ddlatcd but left in place. Ifthe ureteral orifice$ still cannot be visuilizcd, the bladder incision is enended inferiorly into the rca:opubic portion to allow direct trigone visualization. A wfde purse-string U$ing Office cym>scopy does not require specific postoperative management. Instead, anteroinferiorly and laterally, the bladder abuts the loose connective tissue that fills the retropubic space, and here, the bladder lacks a peritoneal covering.
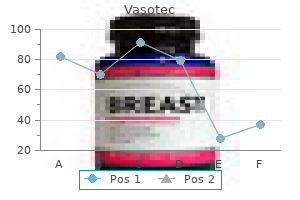
Infrapopliteal intervention procedural success is commonly defined as the re-establishment of direct "in-line" pulsatile flow to the foot hypertension treatment guidelines 2013 5 mg vasotec with mastercard. It is currently unknown whether healing rates are improved when in-line flow to the foot is established through more than one artery pulse pressure significance purchase 10 mg vasotec with mastercard, but maximizing blood flow through more than one artery is particularly attractive in patients with inadequate collateral circulation blood pressure chart according to age and weight purchase vasotec 5 mg free shipping, disease of the plantar arch vessels pulse pressure meaning generic 10 mg vasotec overnight delivery, or limb-threatening ischemia prehypertension jnc 8 vasotec 10 mg buy fast delivery. This evidence supports the contention that angioplasty of the tibioperoneal vessels should not necessarily be reserved for limb salvage situations. However, caution is still advised in patient selection, since the surgical options are limited if angioplasty fails. At present, there have been no clinical breakthroughs, but ongoing basic science activity appears to be promising. However, their role in infrainguinal revascularization is not established so their use should be limited to bailout situations after failed or failing angioplasty. Adjunctive high-cost niche devices, such as atherectomy, lasers, cryotherapy, and cutting balloons, have a very limited role, if any, in the treatment of lower-extremity ischemic lesions. Endovascular revascularization and supervised exercise for peripheral artery disease and intermittent claudication: a randomized clinical trial. Stent placement for chronic iliac arterial occlusive disease: the results of 10 years experience in a single institution. Intraarterial pressure gradients after randomized angioplasty or stenting of iliac artery lesions. Long-term cardiovascular morbidity, mortality, and reintervention after endovascular treatment in patients with iliac artery disease: the Dutch Iliac Stent Trial Study. Dutch Iliac Stent Trial: long-term results in patients randomized for primary or selective stent placement. Meta-analysis of the results of percutaneous transluminal angioplasty and stent placement for aortoiliac occlusive disease. A comparison of covered vs bare expandable stents for the treatment of aortoiliac occlusive disease. Endovascular treatment of the common femoral artery in the Vascular Quality Initiative. Paclitaxel-coated balloons in the femoropopliteal artery: it is all about the pharmacokinetic profile and vessel tissue bioavailability. Endovascular brachytherapy after femoropopliteal balloon angioplasty fails to show robust clinical benefit over time. Endovascular brachytherapy for prophylaxis of restenosis after femoropopliteal angioplasty: five-year follow-upprospective randomized study. Endovascular brachytherapy: restenosis in de novo versus recurrent lesions of femoropopliteal arterythe Vienna experience. High dose-rate brachytherapy for the treatment of lower extremity in-stent restenosis. External beam radiation to prevent restenosis after superficial femoral artery balloon angioplasty. Results of a randomized clinical trial of external beam radiation to prevent restenosis after superficial femoral artery stenting. Directional atherectomy versus balloon angioplasty in segmental femoropopliteal artery disease: two-year follow-up with colorflow duplex scanning. Subintimal angioplasty is superior to Silverhawk atherectomy for the treatment of occlusive lesions of the lower extremities. Excimer laserassisted recanalization of long, chronic superficial femoral artery occlusions. Percutaneous transluminal laser angioplasty versus balloon dilation for treatment of popliteal artery occlusions. Excimer laser assisted angioplasty for complex infrainguinal peripheral artery disease: a 2008 update. Using 6-mm cutting balloon angioplasty in patients with resistant peripheral artery stenosis: preliminary results. Cryoplasty versus conventional balloon angioplasty of the femoropopliteal artery in diabetic patients: long-term results from a prospective randomized single-center controlled trial. Percutaneous transluminal angioplasty of infrapopliteal arteries in patients with intermittent claudication: acute and one-year results. Randomized comparison of everolimus-eluting versus bare-metal stents in patients with critical limb ischemia and infrapopliteal arterial occlusive disease. Sirolimus-eluting stents for treatment of infrapopliteal arteries reduce clinical event rate compared to bare-metal stents: long-term results from a randomized trial. Drug-coated balloons for revascularization of infrapopliteal arteries: a meta-analysis of randomized trials. Lotto; Michael Belkin Abstract the clinical manifestations and complications of atherosclerosis are the most common therapeutic challenges encountered by vascular surgeons. Tremendous advances both in the understanding of atherosclerosis biology and in the ability to treat arterial occlusive disease percutaneously have dramatically impacted the treatment algorithms for arterial insufficiency in recent years. This article will review the current role for open surgical management of aortoiliac and infrainguinal arterial occlusive disease. Keywords aortoiliac; infrainguinal; peripheral vascular disease; open surgical management the clinical manifestations and complications of atherosclerosis are the most common therapeutic challenges encountered by vascular surgeons. The tendency for lesions to develop at specific anatomic sites and to follow recognizable patterns of progression was appreciated as long ago as the late 1700s by the extraordinary British anatomist and surgeon John Hunter. Considered one of the forefathers of vascular surgery, his dissections of atherosclerotic aortic bifurcations remain on view at the Hunterian Museum in London and presage the disease process that Leriche would give name to 150 years later. Cid dos Santos successfully endarterectomized a heavily diseased common femoral artery. It would be another 10 years before synthetic grafts were being regularly used for aortic bypass grafting and the first efforts to extend vein grafting to the tibial level were described by McCaughan. This article will review the current role for the surgical management of aortoiliac and infrainguinal arterial occlusive disease. Aortoiliac occlusive disease Chronic obliterative atherosclerosis of the distal aorta and iliac arteries commonly manifests as symptomatic arterial insufficiency of the lower extremities. Disease in this location is seen often in combination with occlusive disease of the femoropopliteal arteries, producing a range of symptoms from mild claudication to more severe levels of tissue loss and critical ischemia. Patients with hemodynamic impairment limited to the aortoiliac system may have intermittent claudication of the calf muscles alone or involvement of the thigh, hip, and/or buttocks. If the disease distribution also targets the hypogastric vessels, patients may additionally suffer from difficulty in achieving and maintaining an erection, resulting from inadequate perfusion of the internal pudendal arteries. A wellcharacterized constellation of symptoms and signs, known as the Leriche syndrome, which is associated with aortoiliac occlusive disease in the male, includes thigh, hip, or buttock claudication, atrophy of the leg muscles, impotence, and reduced femoral pulses. A meta-analysis did demonstrate fewer complications in women compared to men when one or more hypogastric arteries was disrupted by embolization, coverage, or ligation. The authors attributed this to the fact that most of the female patients in the study had obstetric-related pathologies, while more men had trauma, vascular, or oncologic indications for treatment. The authors further speculated that the younger age and the increased levels of estrogen in the female cohort may have contributed to the gender- related differences that were seen. A well-recognized exception to this general observation arises in the situation of embolic disease. The so-called blue toe syndrome represents a situation where atherosclerotic debris breaks free from an aortic or iliac plaque and embolizes to the distal vessels (see Chapter 45). The terminal target of the microembolic particles, be they cholesterol crystals, calcified plaque, thrombus, or platelet aggregates, is typically the small vessels of the toes. Here the left hypogastric artry is reconstituted via prominent distal lumbar collaterals and the right hypogastric artery. If, on the other hand, aortoiliac occlusive disease is found in combination with femoropopliteal occlusive disease, ischemic rest pain, or even more severe perfusion impairment leading to ischemic tissue loss or gangrene is not uncommon. Approximately one-third of patients operated on for symptomatic aortoiliac occlusive disease have orificial profunda femoris occlusive disease, and more than 40% have superficial femoral artery occlusions. Aortoiliac disease typically begins at the distal aorta and common iliac artery origins, and slowly progresses proximally and distally over time. A particularly virulent form of atherosclerotic arterial disease is often found in young women smokers. While the diminutive size of the aorta and iliac vessels has led to compromised durability when treated endovascularly, ongoing improvements in percutaneous technology have resulted in better outcomes in this patient population in more recent years. The diagnosis of aortoiliac occlusive disease is generally made based on patient symptomatology, physical examination, and noninvasive tests such as segmental pressure measurements and pulse volume recordings (see Chapter 18). Following the diagnosis of aortoiliac disease and the decision to pursue intervention, further imaging is warranted. Should a lesion amenable to percutaneous therapy be identified, catheter-based angiography is then pursued. In the minority of cases necessitating digital subtraction angiography for preoperative planning, a retrograde femoral approach is typically utilized, while the transbrachial approach serves as a useful alternative in patients with particularly challenging anatomy (see Chapter 15). Finally, full runoff views of the lower extremities are needed to assess the presence or absence of femoropopliteal or crural disease. In ambiguous cases, pullback pressure measurements, both before and after the administration of a systemic vasodilator, such as papaverine or nitroglycerine, or the application of a tourniquet to induce reactive hyperemia, can be useful in documenting the hemodynamic significance of a particular stenotic zone. Management Considerations Risk factor modification remains a cornerstone of the management of aortoiliac occlusive disease (see Chapter 19). Smoking cessation, blood pressure control, and aggressive efforts at cholesterol lowering should be addressed with every patient with atherosclerotic disease. Strong evidence exists supporting the benefit of a structured walking program23 in increasing the walking distance of patients with claudication; it is hoped that utilization of this important treatment strategy will increase now that it is a reimbursable therapeutic option. Interestingly, studies have failed to identify any exercise components; for example, intensity, duration, or content, which independently predict improvements in maximum walking distance and pain-free walking distance. Anyone suffering from disabling claudication, rest pain, or ischemia-related tissue loss continues to warrant serious consideration for arteriography and either percutaneous or surgical intervention. Previously, such aggressive treatment would have been considered inappropriate for claudication that was not clearly disabling. However, as percutaneous treatment has become increasingly safer and more effective, and its application has spread to increasingly more arterial beds, the indications for transluminal angioplasty have correspondingly increased (see Chapter 20). Such a sea change in the overall management approach to aortoiliac disease has had a dramatic impact on the numbers of patients now proceeding to open surgery. The rising popularity and success of aortic and iliac balloon angioplasty and stenting as first-line therapy has noticeably reduced the volume of aortoiliac reconstructive procedures performed in this country. When medical therapy or percutaneous treatment has proven inadequate or is technically inadvisable, open surgical revascularization remains indicated for those patients with aortoiliac disease and disabling claudication, ischemic rest pain, and ischemic ulceration or gangrene. Patients with nighttime foot rest pain or tissue loss usually have multisegment disease and the decision whether to perform both supra- and infra-inguinal revascularization procedures or to perform only an inflow procedure is guided by the severity of the ischemia. The numerous surgical options available to the trained vascular surgeon allow tailoring of the approach to the particular overall and anatomic situation of each patient. Historically, the reconstructive options for aortoiliac occlusive disease include aortoiliac endarterectomy, aortobifemoral bypass, and so-called extraanatomic revascularization in the form of iliofemoral, femorofemoral, or axillofemoral grafting. Endarterectomy Aortic endarterectomy was commonly performed in the early era of aortoiliac reconstruction. The long-term patency of limited endarterectomy is excellent and on par with bypass procedures. Aortobifemoral Bypass Aortobifemoral bypass remains the mainstay of operative treatment for aortoiliac occlusive disease. During the last 20 years, the procedure has supplanted both aortic endarterectomy and aortoiliac bypass procedures. In the latter case, this change was largely driven by the recognition of subsequent graft failure due to progression of native iliac arterial disease. Current early patency rates for aortobifemoral bypass grafting are excellent, approaching 100% in many reporting institutions. Five-year patency rates are greater than 80%36,38,39,43 while 10-year rates are near 75%. The current graft material used by most surgeons for aortoiliac reconstruction is a knitted Dacron prosthesis, which has enhanced hemostatic properties and which tends to have a more stable pseudointima than the earlier used woven grafts. Grafts are more routinely extended beyond the iliac level to the femoral vessels, which not only improves exposure and makes for a technically easier distal anastomosis, but is also associated with less graft thrombosis from unanticipated progression of atherosclerotic disease in the external iliac vessels. For example, patients with hostile groin creases from prior surgery or radiation therapy, or obese, diabetic patients with an intertriginous rash at the inguinal crease will all likely be better served by performing the distal anastomosis at the external iliac level if their anatomy for such a procedure is suitable. The increased awareness of the critical role played by the deep femoral artery in preserving the long-term patency of aortobifemoral grafts36,47,48 has also undoubtedly contributed to the better results seen. This awareness parallels a better overall appreciation for the importance of establishing adequate outflow at the femoral level in achieving higher early and late graft patency rates and sustained symptom relief. The true impact of concomitant superficial femoral artery disease is unclear from the literature. Some reports have indicated similar patency rates between those patients with and without superficial femoral artery occlusion,29,31 while others have suggested that late patency rates are reduced in this setting. In these circumstances, it is preferable to close the endarterectomized recipient bed with a vein, bovine pericardial or Dacron patch, onto which the distal anastomosis can then be attached, rather than creating a long femoris patch with the graft limb. There are several technical considerations related to aortobifemoral bypass grafting, which are the subject of considerable and passionate debate. Advocates of an endto-end configuration claim that it facilitates a more comprehensive thromboendarterectomy of the proximal stump and allows for a direct, more inline flow pattern, with less turbulence and more favorable flow characteristics. Certainly, with concomitant aneurysmal disease or complete aortic occlusion extending up to the level of the renal arteries, end-to-end grafting is indicated. Creation of an end-toside anastomosis can, at times, be technically challenging in a heavily diseased aorta partially occluded by a side-biting clamp. A lower rate of proximal suture line pseudoaneurysms and better long-term patency rates have been found in some series. Finally, those in favor of this approach claim that the ability to more effectively close the retroperitoneum, particularly after resection of a short segment of the infrarenal aorta, results in a lower rate of late graft infection and aortoenteric fistulae, although there is no direct evidence to support this assertion. There are certain circumstances, on the other hand, when an end-to-side proximal anastomotic configuration is advantageous. The most common indication involves those patients with occluded external iliac arteries, in whom interruption of forward aortic flow may result in loss of perfusion to an important hypogastric or inferior mesenteric artery and consequent significant pelvic ischemia.
Discount vasotec 5 mg. Blood Pressure Monitor HYLOGY Digital Wrist Blood Pressure Monitor unboxing and instructions.
References
- Unger AH, Sklaroff HJ: Fatalities following intravenous use of sodium diphenylhydantoin for cardiac arrhythmias, JAMA 200:335, 1967.
- Coeytaux RR, Williams JW Jr, Gray RN, Wang A. Percutaneous heart valve replacement for aortic stenosis: state of the evidence. Ann Intern Med 2010;153:314-324.
- Ohnishi K, Ohyama N, Ito S, Fujiwara K. Small hepatocellular carcinoma: treatment with US-guided intratumoral injection of acetic acid. Radiology. 1994;193:747-752.
- Slemenda C, Hui SL, Longcope C, Conran Johnston C. Sex steroids and bone mass. A study of changes about the time of the menopause. J Clin Invest. 1987;80:1261-8.
- Bradley EH, Nallamothu BK, Herrin J, et al. National efforts to improve door-to-balloon time results from the Door-to-Balloon Alliance. J Am Coll Cardiol 2009;54(25): 2423-2429.
- Lerario AM, Moraitis A, Hammer GD. Genetics and epigenetics of adrenocortical tumors. Mol Cell Endocrinol 2014;386(1-2):67-84.
- Talbot E, Munseri P, Teixeira P, et al. Test characteristics of urinary lipoarabinomannan and predictors of mortality among hospitalized HIV-infected tuberculosis suspects in Tanzania. PLoS One 2012; 7: e32876.
- Rost NS, Masrur S, Pervez MA, Viswanathan A, Schwamm LH. Unsuspected coagulopathy rarely prevents IV thrombolysis in acute ischemic stroke. Neurology. 2009;73(23):1957-1962.
